POWERPOINT LECTURE SLIDE PRESENTATION by LYNN CIALDELLA MBA

POWERPOINT® LECTURE SLIDE PRESENTATION by LYNN CIALDELLA, MBA, The University of Texas at Austin Additional Text by J Padilla exclusively for physiology at ECC UNIT 3 20 Integrative Physiology II: Fluid and Electrolyte Balance HUMAN PHYSIOLOGY AN INTEGRATED APPROACH DEE UNGLAUB SILVERTHORN Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings FOURTH EDITION
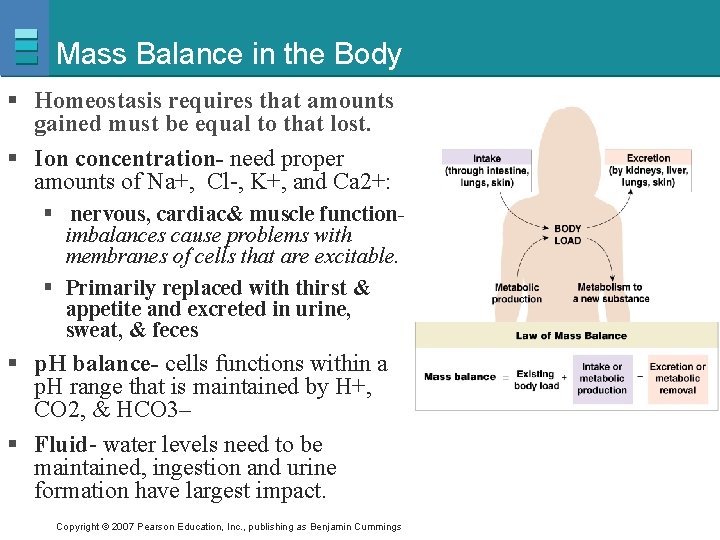
Mass Balance in the Body § Homeostasis requires that amounts gained must be equal to that lost. § Ion concentration- need proper amounts of Na+, Cl-, K+, and Ca 2+: § nervous, cardiac& muscle functionimbalances cause problems with membranes of cells that are excitable. § Primarily replaced with thirst & appetite and excreted in urine, sweat, & feces § p. H balance- cells functions within a p. H range that is maintained by H+, CO 2, & HCO 3– § Fluid- water levels need to be maintained, ingestion and urine formation have largest impact. Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings
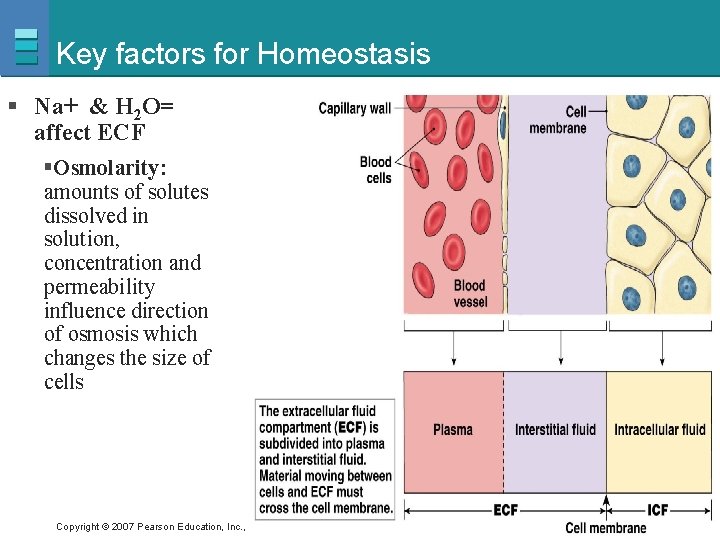
Key factors for Homeostasis § Na+ & H 2 O= affect ECF §Osmolarity: amounts of solutes dissolved in solution, concentration and permeability influence direction of osmosis which changes the size of cells Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings
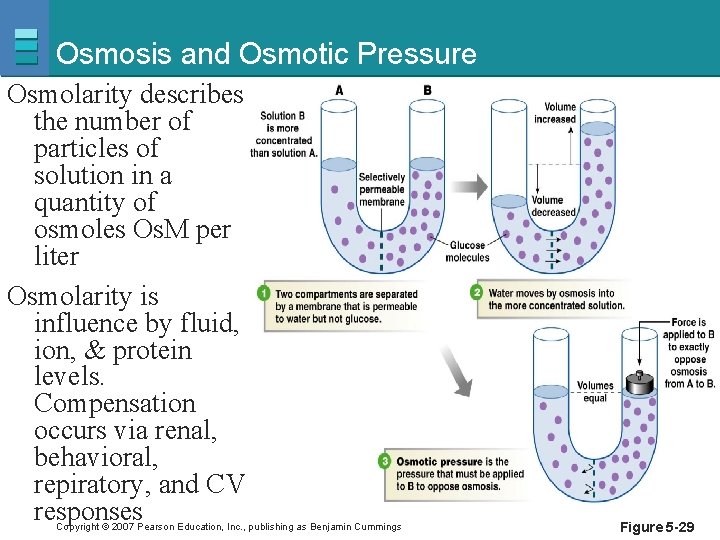
Osmosis and Osmotic Pressure Osmolarity describes the number of particles of solution in a quantity of osmoles Os. M per liter Osmolarity is influence by fluid, ion, & protein levels. Compensation occurs via renal, behavioral, repiratory, and CV responses Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 5 -29
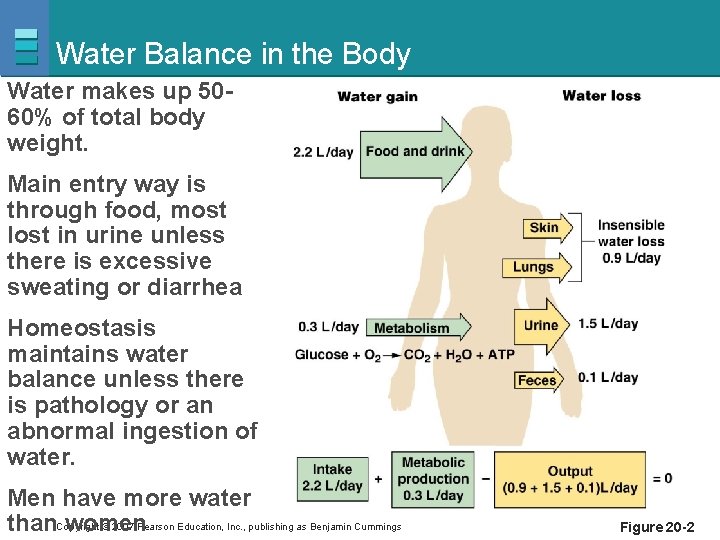
Water Balance in the Body Water makes up 5060% of total body weight. Main entry way is through food, most lost in urine unless there is excessive sweating or diarrhea Homeostasis maintains water balance unless there is pathology or an abnormal ingestion of water. Men have more water © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings than. Copyright women Figure 20 -2
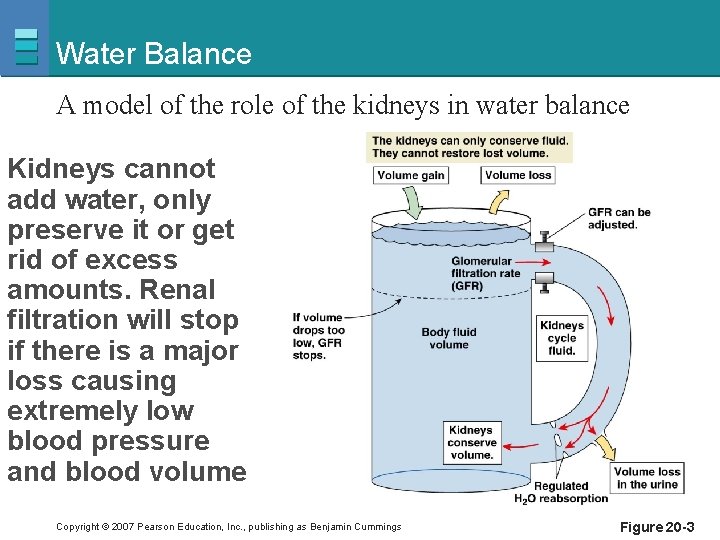
Water Balance A model of the role of the kidneys in water balance Kidneys cannot add water, only preserve it or get rid of excess amounts. Renal filtration will stop if there is a major loss causing extremely low blood pressure and blood volume Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -3
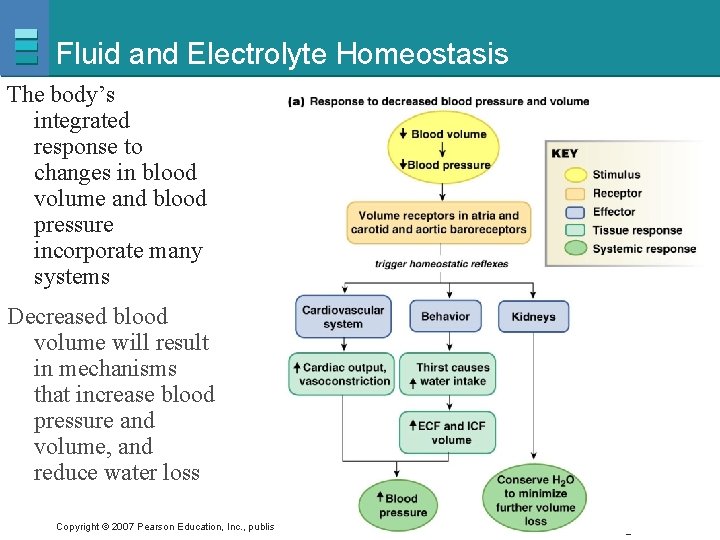
Fluid and Electrolyte Homeostasis The body’s integrated response to changes in blood volume and blood pressure incorporate many systems Decreased blood volume will result in mechanisms that increase blood pressure and volume, and reduce water loss Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -1 a
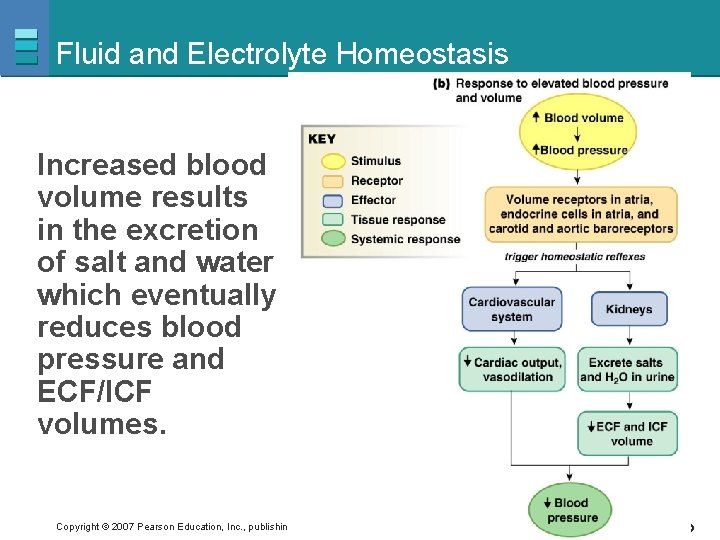
Fluid and Electrolyte Homeostasis Increased blood volume results in the excretion of salt and water which eventually reduces blood pressure and ECF/ICF volumes. Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -1 b
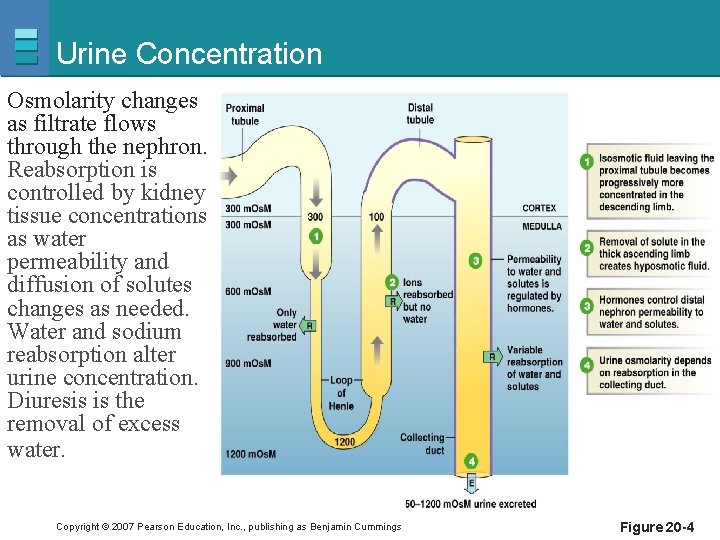
Urine Concentration Osmolarity changes as filtrate flows through the nephron. Reabsorption is controlled by kidney tissue concentrations as water permeability and diffusion of solutes changes as needed. Water and sodium reabsorption alter urine concentration. Diuresis is the removal of excess water. Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -4

Water Reabsorption Vasopression or antidiuretic hormone causes a graded effect of forming water pores on collecting duct cells. Thus permeability is increased and more water is retained making urine more concentrated. Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -5 a

Water Reabsorption If vasopressin is absent water will not move out through water pores (aquaporins)a nd the urine will be dilute. Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -5 b
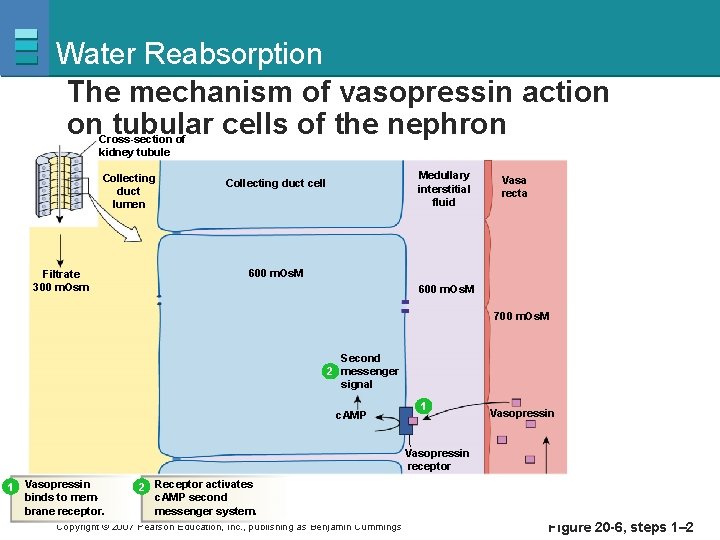
Water Reabsorption The mechanism of vasopressin action on tubular cells of the nephron Cross-section of kidney tubule Collecting duct lumen Filtrate 300 m. Osm Medullary interstitial fluid Collecting duct cell Vasa recta 600 m. Os. M 700 m. Os. M Second 2 messenger signal c. AMP 1 Vasopressin receptor 1 Vasopressin binds to membrane receptor. 2 Receptor activates c. AMP second messenger system. Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -6, steps 1– 2
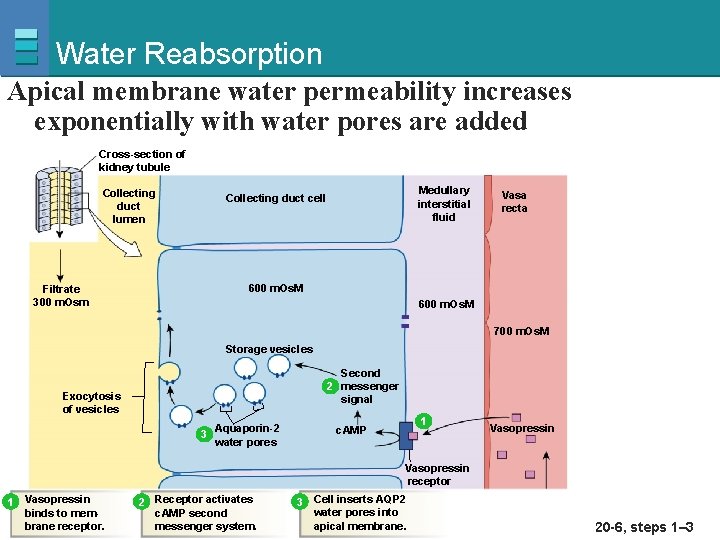
Water Reabsorption Apical membrane water permeability increases exponentially with water pores are added Cross-section of kidney tubule Collecting duct lumen Medullary interstitial fluid Collecting duct cell Vasa recta 600 m. Os. M Filtrate 300 m. Osm 600 m. Os. M 700 m. Os. M Storage vesicles Second 2 messenger signal Exocytosis of vesicles 3 Aquaporin-2 water pores 1 c. AMP Vasopressin receptor 1 Vasopressin 2 Receptor activates 3 Cell inserts AQP 2 water pores into binds to memc. AMP second apical membrane Copyright receptor. © 2007 Pearson messenger system. Education, Inc. , publishing as Benjamin Cummings Figure 20 -6, steps 1– 3
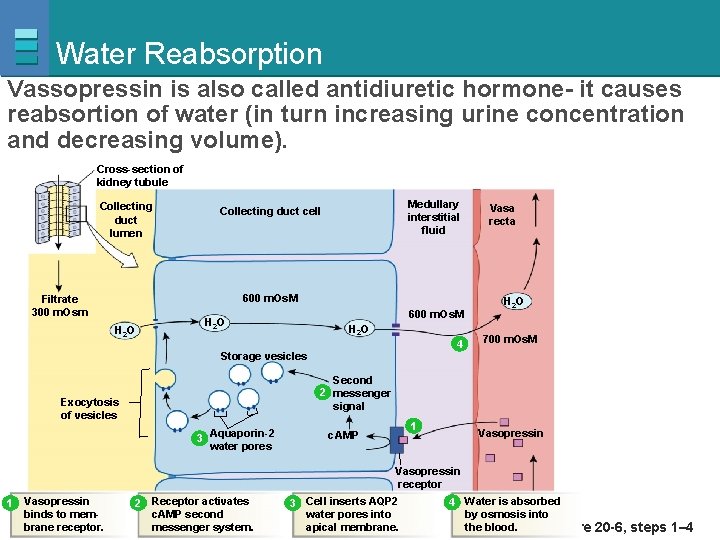
Water Reabsorption Vassopressin is also called antidiuretic hormone- it causes reabsortion of water (in turn increasing urine concentration and decreasing volume). Cross-section of kidney tubule Collecting duct lumen Medullary interstitial fluid Collecting duct cell 600 m. Os. M Filtrate 300 m. Osm H 2 O 600 m. Os. M H 2 O 4 Vasa recta H 2 O 700 m. Os. M Storage vesicles Second 2 messenger signal Exocytosis of vesicles 3 Aquaporin-2 water pores 1 c. AMP Vasopressin receptor 1 Vasopressin 2 Receptor activates 3 Cell inserts AQP 2 binds to memc. AMP second water pores into Education, Inc. , publishing asapical Benjamin Cummings brane Copyright receptor. © 2007 Pearson messenger system. membrane. 4 Water is absorbed by osmosis into the blood. Figure 20 -6, steps 1– 4
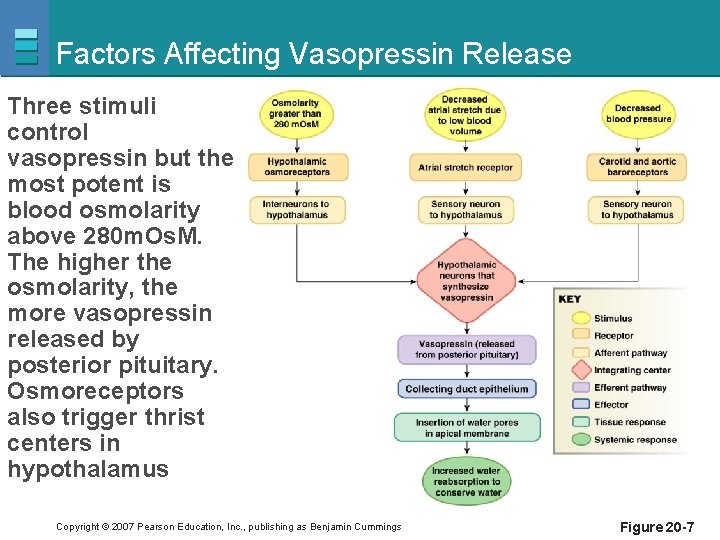
Factors Affecting Vasopressin Release Three stimuli control vasopressin but the most potent is blood osmolarity above 280 m. Os. M. The higher the osmolarity, the more vasopressin released by posterior pituitary. Osmoreceptors also trigger thrist centers in hypothalamus Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -7
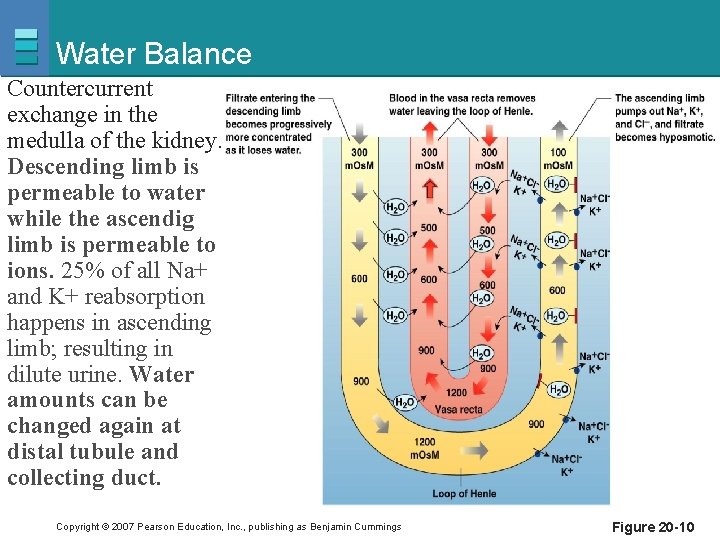
Water Balance Countercurrent exchange in the medulla of the kidney. Descending limb is permeable to water while the ascendig limb is permeable to ions. 25% of all Na+ and K+ reabsorption happens in ascending limb; resulting in dilute urine. Water amounts can be changed again at distal tubule and collecting duct. Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -10
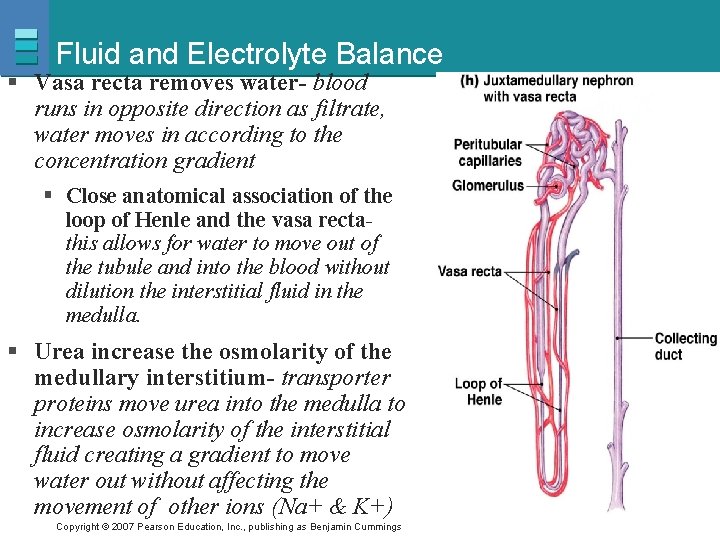
Fluid and Electrolyte Balance § Vasa recta removes water- blood runs in opposite direction as filtrate, water moves in according to the concentration gradient § Close anatomical association of the loop of Henle and the vasa rectathis allows for water to move out of the tubule and into the blood without dilution the interstitial fluid in the medulla. § Urea increase the osmolarity of the medullary interstitium- transporter proteins move urea into the medulla to increase osmolarity of the interstitial fluid creating a gradient to move water out without affecting the movement of other ions (Na+ & K+) Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings
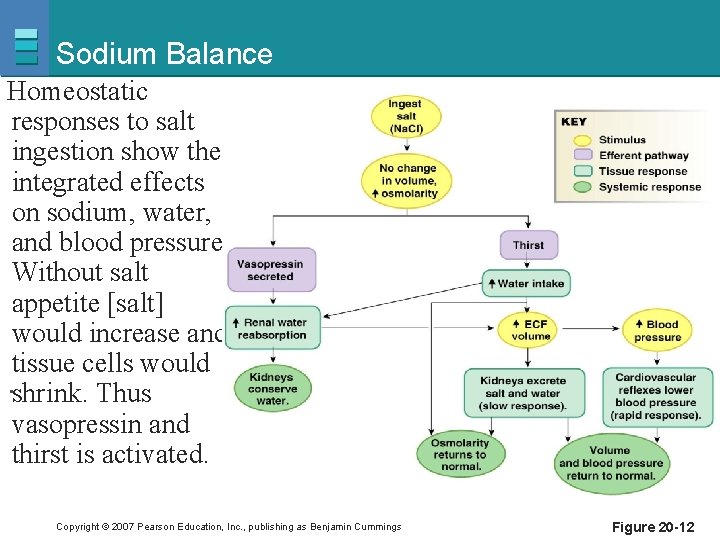
Sodium Balance Homeostatic responses to salt ingestion show the integrated effects on sodium, water, and blood pressure. Without salt appetite [salt] would increase and tissue cells would. shrink. Thus vasopressin and thirst is activated. Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -12
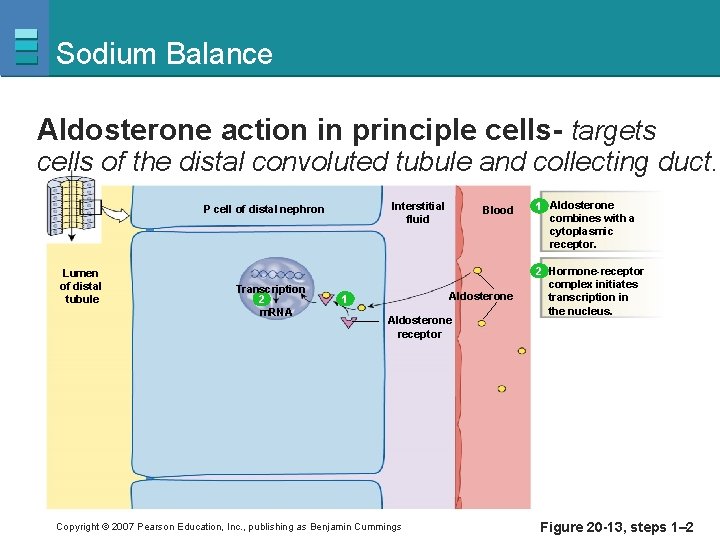
Sodium Balance Aldosterone action in principle cells- targets cells of the distal convoluted tubule and collecting duct. Interstitial fluid P cell of distal nephron Lumen of distal tubule Transcription 2 m. RNA Blood Aldosterone 1 Aldosterone receptor Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings 1 Aldosterone combines with a cytoplasmic receptor. 2 Hormone-receptor complex initiates transcription in the nucleus. Figure 20 -13, steps 1– 2
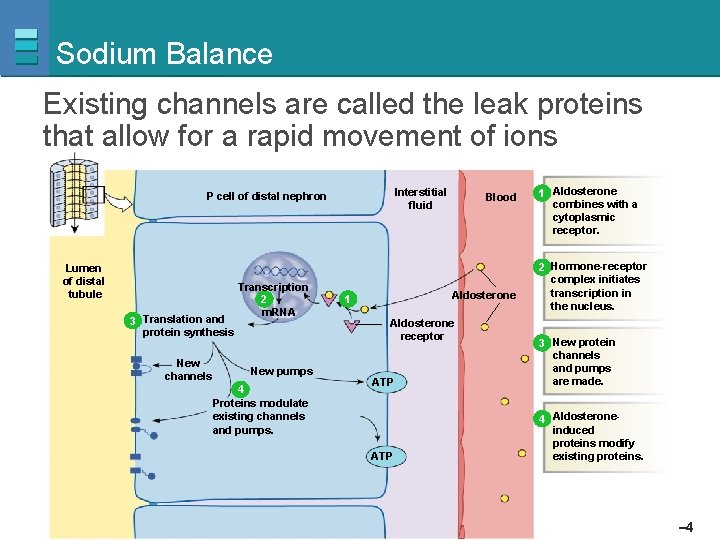
Sodium Balance Existing channels are called the leak proteins that allow for a rapid movement of ions Interstitial fluid P cell of distal nephron Lumen of distal tubule 3 Translation and protein synthesis New channels Transcription 2 m. RNA New pumps 4 Proteins modulate existing channels and pumps. Blood Aldosterone 1 Aldosterone receptor 1 Aldosterone combines with a cytoplasmic receptor. 2 Hormone-receptor complex initiates transcription in the nucleus. ATP 3 New protein channels and pumps are made. ATP 4 Aldosteroneinduced proteins modify existing proteins. Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -13, steps 1– 4
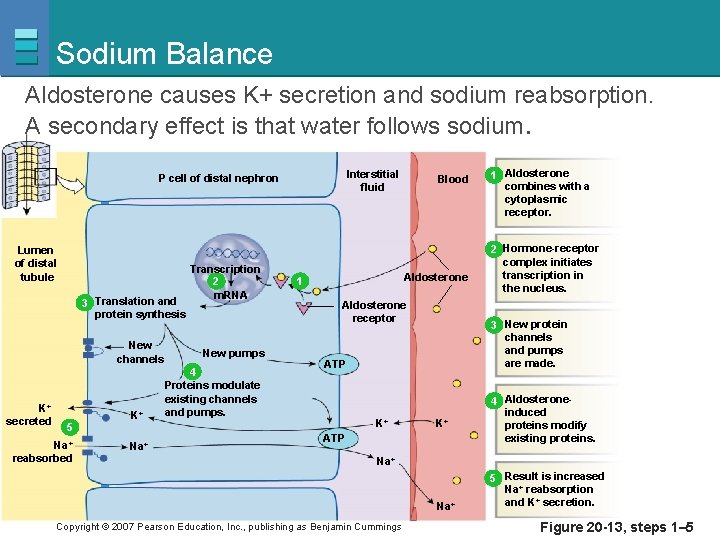
Sodium Balance Aldosterone causes K+ secretion and sodium reabsorption. A secondary effect is that water follows sodium. Interstitial fluid P cell of distal nephron Lumen of distal tubule 3 Translation and protein synthesis New channels K+ secreted 5 Na+ reabsorbed K+ Na+ Transcription 2 m. RNA New pumps 4 Proteins modulate existing channels and pumps. Blood Aldosterone 1 Aldosterone receptor 1 Aldosterone combines with a cytoplasmic receptor. 2 Hormone-receptor complex initiates transcription in the nucleus. ATP 3 New protein channels and pumps are made. ATP 4 Aldosteroneinduced proteins modify existing proteins. K+ K+ Na+ Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings 5 Result is increased Na+ reabsorption and K+ secretion. Figure 20 -13, steps 1– 5
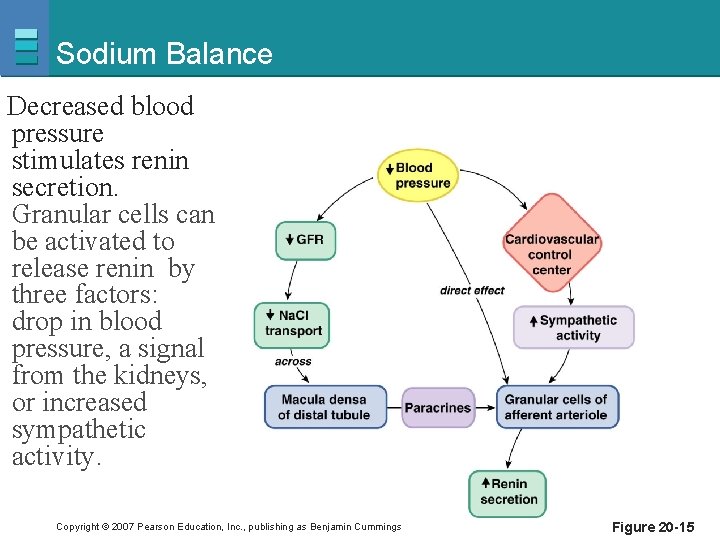
Sodium Balance Decreased blood pressure stimulates renin secretion. Granular cells can be activated to release renin by three factors: drop in blood pressure, a signal from the kidneys, or increased sympathetic activity. Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -15
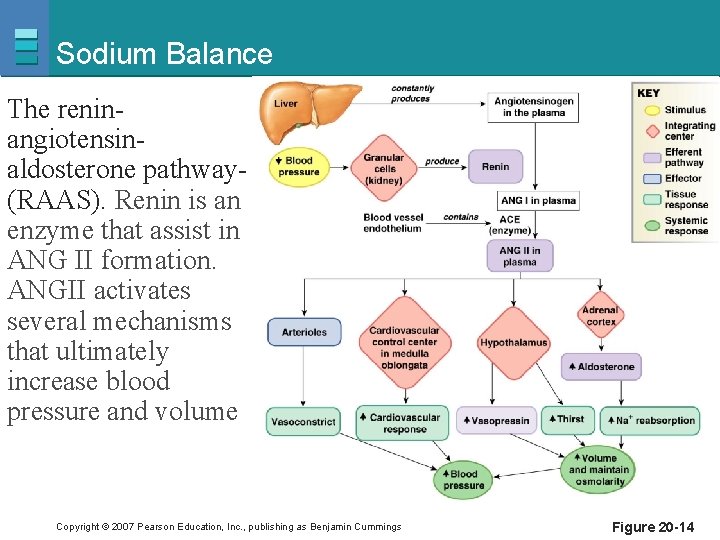
Sodium Balance The reninangiotensinaldosterone pathway(RAAS). Renin is an enzyme that assist in ANG II formation. ANGII activates several mechanisms that ultimately increase blood pressure and volume Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -14
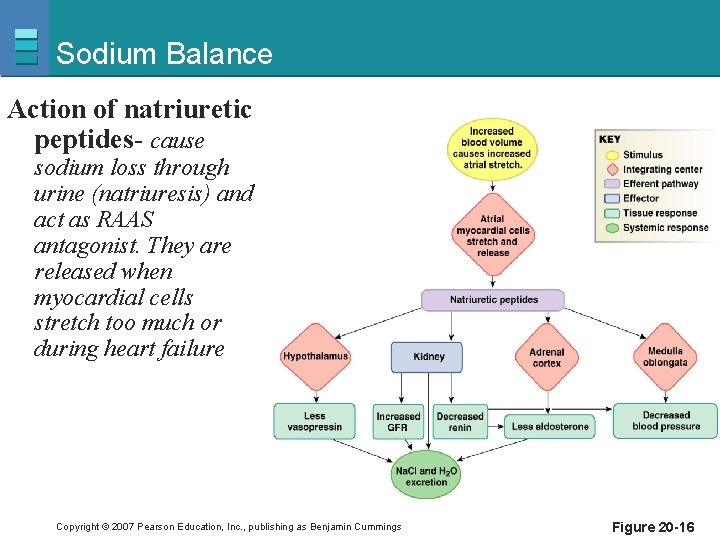
Sodium Balance Action of natriuretic peptides- cause sodium loss through urine (natriuresis) and act as RAAS antagonist. They are released when myocardial cells stretch too much or during heart failure Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -16

Potassium Balance § Regulatory mechanisms keep plasma potassium in narrow range (3. 5 -5 meq/L) § Aldosterone is released in response to excess levels, it increases permeability at distal nephron so K is moved into the urine while sodium is reabsorbed § Hypokalemia (K+ levels below 3) § In ECF levels are low, K+ leaves the cell, and resting membrane potential is more negative (hyperpolaized)= stronger stimulus § Muscle weakness and failure of respiratory muscles and the heart due to hyperpolarized neurons. § Hyperkalemia (K+ levels above 6) § In ECF levels are high, more K+ enters the cell, thus depolarizing it but then less able to repolarize thus LESS excitable § Can lead to cardiac arrhythmias § K+ irregularities include kidney disease, diarrhea, and diuretics Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings

Behavioral Mechanisms Drinking water and eating salt is the only way the body obtains these substances, therefore individuals who cannot do this must be assisted. § Drinking replaces fluid loss – when body osmolarity raises above 280 m. Os. M hypothalmic osomreceptors trigger thrist. Oropharynx receptors are stimulated by cold drink and signal thirst quench § Low sodium stimulates salt appetite – the hypothalamus also has centers for salt appetite which trigger a response when osmolarity is low. § Avoidance behaviors help prevent dehydration § Desert animals avoid the heat Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings
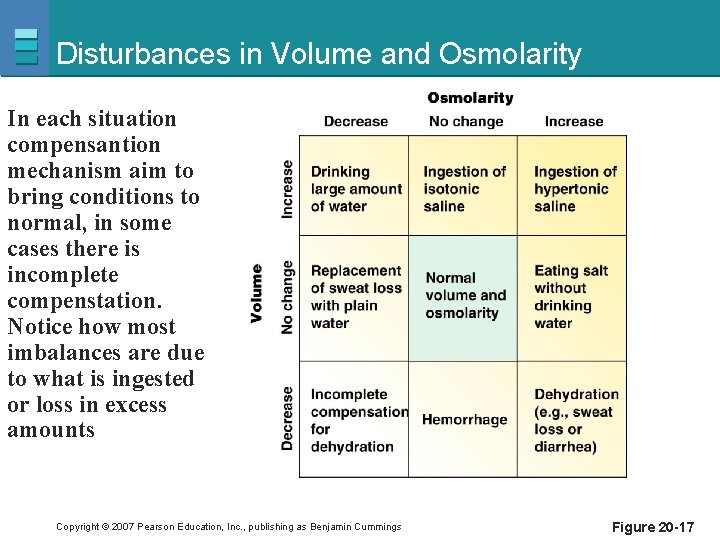

Disturbances in Volume and Osmolarity In each situation compensantion mechanism aim to bring conditions to normal, in some cases there is incomplete compenstation. Notice how most imbalances are due to what is ingested or loss in excess amounts Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -17

Severe Dehydration Compensation § Condition: low ECF volume, low blood pressure, high osmolarity § Compensation Mechanisms § Cardiovascular Responses- increase cardiac output & vasoconstriction to increase blood pressure. Vasoconstriction reduces GFR activating granular cells to release renin § Angiotensin II- produce after renin release that activates RAAS pathway to trigger thirst, vasopressin release, and vasoconstrion. (aldosterone is not release as it would increase osmolarity) § Vassopressin- increase water reabsorption to reduce loss in urine § Thrist/ IV-replacement of loss fluids and lowering of osmolarity Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings

Acid-Base Balance § Normal plasma p. H is 7. 38– 7. 42 - also resembles the p. H inside cells, its optimum for proper protein & enzyme function § H+ concentration is closely regulated- slight p. H changes indicate a 10 -fold increase/decrease in [H+] which can have damaging effects on protein structure & function. § Abnormal p. H affects the nervous system- H+ imbalances cause K+ imbalances because transporter protein in kidneys moves H+ and K+ in antiport fashion § Acidosis: neurons become less excitable and CNS depression patients can fall into a coma or have respiratory failure § Alkalosis: hyperexcitable- numbness, tingling, muscle twitches, severe cases lead to paralysis of respiratory muscles § p. H disturbances- induced by an imbalance of H+ input/output § Compensation by buffers, ventilation, or renal regulation § Greatest source is CO 2 level changes induced by metabolic or respiratory factors Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings
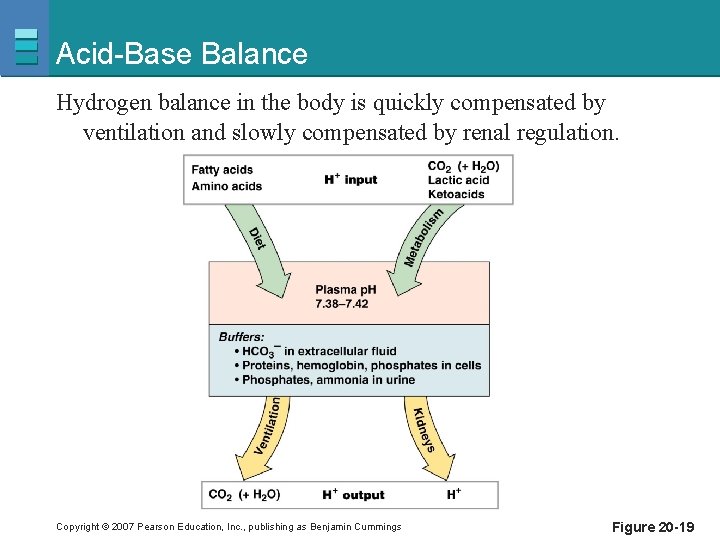
Acid-Base Balance Hydrogen balance in the body is quickly compensated by ventilation and slowly compensated by renal regulation. Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -19

Acid and Base Input Acid § Organic acids – acids produced by the body during metabolism or ingested molecules that realease H+ (acidic fruits, amino acids, fatty acids) § Under extraordinary conditions – produce more H+ than the body can normally get rid off and cause pathological effects § Metabolic organic acid production can increase Ketoacids – strong acids produced when fats & proteins are metabolized § Diabetes – metabolism disorder causes ketoacid formation § Accumulation of CO 2 - can occur as a result of anaerobic respiration, increased metabolism, or decreased ventilation § Acid production - CO 2 combines with water rapidly to make an acid and drop p. H. Respiratory system gets rid of 75% of a Base Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings
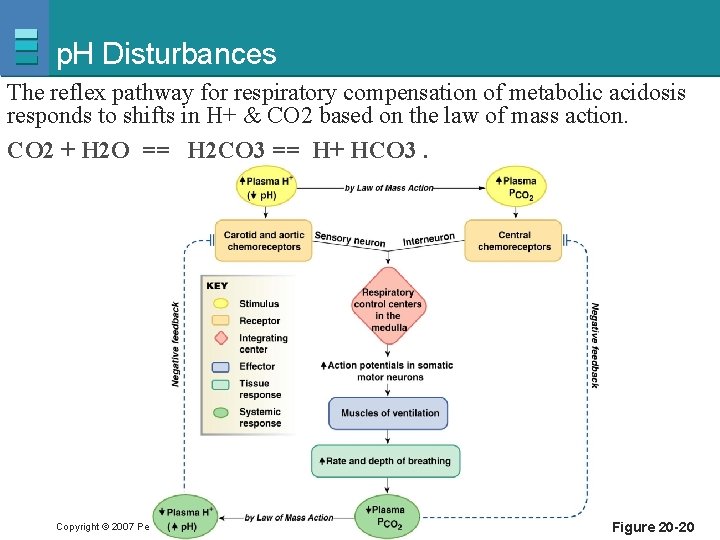
p. H Disturbances The reflex pathway for respiratory compensation of metabolic acidosis responds to shifts in H+ & CO 2 based on the law of mass action. CO 2 + H 2 O == H 2 CO 3 == H+ HCO 3. Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -20

p. H Homeostasis § Buffers moderate changes in p. H- cannot prevent changes, they absorb/release H+ § Cellular proteins, phosphate ions, and hemoglobin- serve as intracellular buffers § Ventilation § Rapid- quickly gets rid of CO 2 by increasing breathing rate § 75% of disturbances- are cleared by ventilation thanks to the central and peripheral chemoreceptors that sense changes in [H+] § Renal regulation- uses ammonia and phosphate buffers in addition to § Directly excreting or reabsorbing H+ § Indirectly by change in the rate at which HCO 3– buffer is reabsorbed or excreted Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings
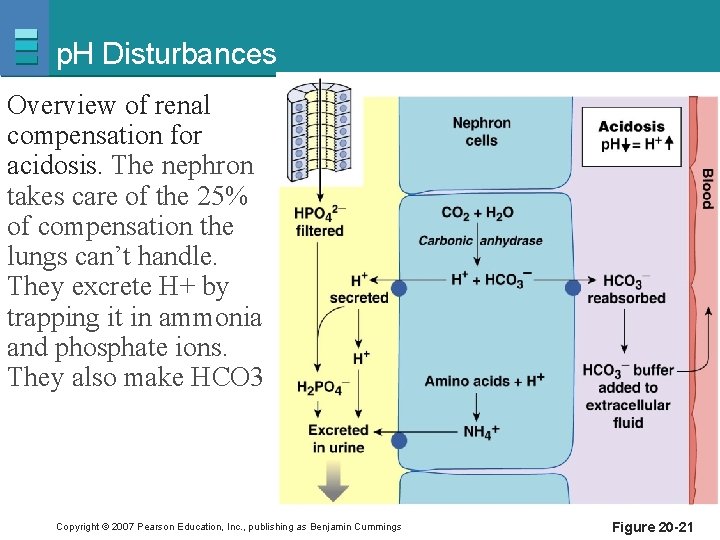
p. H Disturbances Overview of renal compensation for acidosis. The nephron takes care of the 25% of compensation the lungs can’t handle. They excrete H+ by trapping it in ammonia and phosphate ions. They also make HCO 3 Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -21
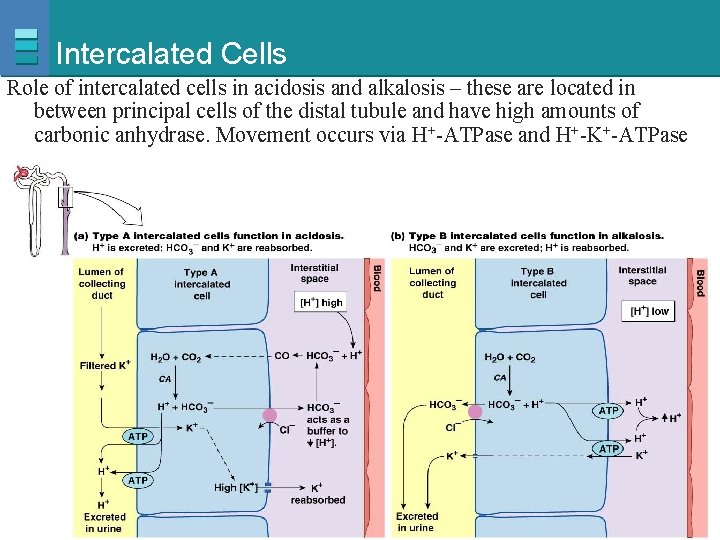
Intercalated Cells Role of intercalated cells in acidosis and alkalosis – these are located in between principal cells of the distal tubule and have high amounts of carbonic anhydrase. Movement occurs via H+-ATPase and H+-K+-ATPase Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings Figure 20 -23
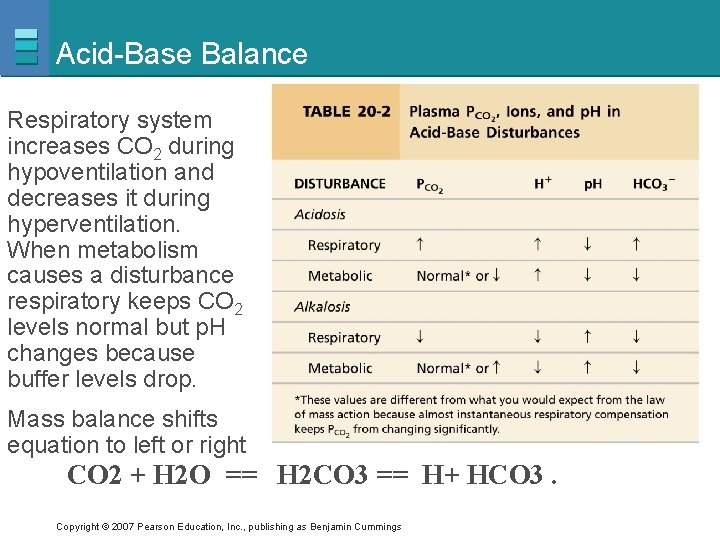
Acid-Base Balance Respiratory system increases CO 2 during hypoventilation and decreases it during hyperventilation. When metabolism causes a disturbance respiratory keeps CO 2 levels normal but p. H changes because buffer levels drop. Mass balance shifts equation to left or right CO 2 + H 2 O == H 2 CO 3 == H+ HCO 3. Copyright © 2007 Pearson Education, Inc. , publishing as Benjamin Cummings
- Slides: 36