Powered Air Purifying Respirators Objectives Identify high hazard

Powered Air Purifying Respirators

Objectives § Identify high hazard procedures § Describe indications for a PAPR § PAPR inspection § Donning and Doffing a PAPR § Describe maintenance and storage of a PAPR

Powered Air Purifying Respirator (PAPR) § NIOSH approved Powered Air Purifying Respirator (PAPR) provides respiratory protection against aerosol transmissible pathogens during performance of high hazard procedures. § Provides an alternate means of respiratory protection against aerosol pathogens. § Fit testing is not required § Wearing glasses or a beard will not affect the performance

When is PAPR use indicated? § Emergency Preparedness (Disaster Planning) § To prevent exposure to aerosol transmissible diseases § During performance of high hazard procedures such as o Cardiopulmonary Resuscitation o Bronchoscopy o Extubation o Sputum Induction o Open airway suctioning on patients suspected or confirmed to have an Aerosol Transmissible Disease.

Indications For PAPRs Continued § Entering an airborne isolation room without an N 95 mask § Fit testing has failed § Employee has facial hair or facial deformity that would interfere with mask-to-face seal. § A higher level of protection is preferred

When is a PAPR contraindicated? § During the performance of routine patient care § If it has been determined that a PAPR will interfere with the successful performance of any required task or compromise patient safety, the user may wear an N 95. The user will make this determination as part of their assessment prior to the procedure.

Inpatients with suspected or active ATD § Provide airborne isolation room if it is suspected high hazard procedures will be performed (if not, a private room is acceptable) § Isolation protocol as appropriate for either droplet or airborne pathogens WITH the PAPR alert signage outside the patient room § A HEPA filter should be placed in the room when performing high hazard procedures (if available) DROPLET ISOLATION( (In addition to STANDARD PRECAUTIONS ) MASK: Mask covering eyes, nose AN mouth. REQUIRED when you are within 3 feet of the patient. GLOVES: REQUIRED if you will touch anythingcontaminated with respiratory secretions. GOWN: REQUIRED if clothing will contact contaminated surfaces or respiratory secretions HANDS: USE ANTIMICROBIAL SOAP & WATER OR ALCOHOL GEL IF HANDS ARE NOT VISIBLY CONTAMINATED.

Surgery on suspect / active ATD Patients § Postpone all non-urgent procedures until the patient is determined to be non-infectious. § Keep operating traffic to a minimum. § Schedule procedure time when minimum number of HCWs and patients are present (end of the day) § Place bacterial filter on patient's endotracheal tube or expiratory side of breathing circuit or anesthesia machine. § All personnel present during the procedure should wear appropriate respiratory protection N-95 respirator or higher (standard surgical masks alone do not offer sufficient protection).
Recovering Surgery Patients § If possible, patient will recover in the same OR suite that the surgery is performed in used. § Monitor patient during recovery in a room With HEPA Filter machine running. § The HEPA machine should remain on for 10 -15 minutes after patient discharge before entering the room for cleaning. § In the event that a HEPA filters was not used (i. e. , an influx of airborne infectious patients), the room should remain empty for one hour before use.

Obtaining a PAPR § Contact Central Supply when anticipating performance of a high hazard procedure § Return PAPRs to central supply for cleaning and disinfection when no longer needed

Inspection Before Use Examine the following before and after use and during cleaning: § § § § Rubber Face piece Air-purifying element holder for breaks, cracks, worn threads, missing gasket Excessive dirt, cracks, tears, holes, distortion Cracked, scratched, or loose-fitting lens (full face) Incorrectly mounted full face piece lens or broken/missing mounting clips Head strap breaks, tears, loss of elasticity Broken or malfunctioning buckles/attachments Excessively worn serrations on head piece Harness which might allow the face piece to slip Inhalation/Exhalation valves Detergent residue, dust particles, dirt, or hair on valve or valve seat. Cracks, tears, distortion in valve material or valve seat Improper insertion of the valve body in the face piece

LED Indicators The LEDs alert the user when it is time to exit the environment and re-charge or change out the battery and/or change the filter. Located inside the PAPR helmet, above the user’s line of site Green Light = Fully Functional Yellow Light = Indicates low air flow (Filter may need to be changed) Red Light = Indicates low battery Red and Yellow = low battery OR both battery and filters require changing EXIT THE ENVIRONMENT AND RETURN PAPR TO CENTRAL SUPPLY IF YOU SEE A RED OR YELLOW LIGHT!
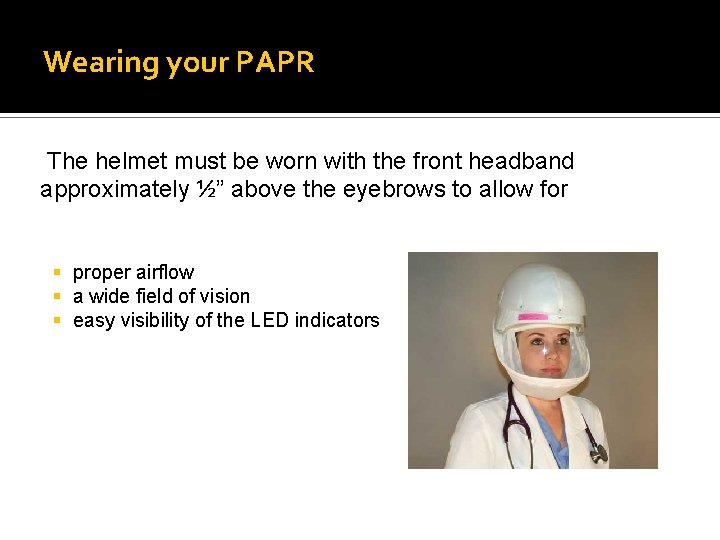
Wearing your PAPR The helmet must be worn with the front headband approximately ½” above the eyebrows to allow for § proper airflow § a wide field of vision § easy visibility of the LED indicators

Adjusting for Proper Fit Adjustment of the PAPR helmet to achieve a proper fit can be accomplished by adjusting the ratchet knob at the back of the helmet

Return PAPR to Central � For cleaning and disinfection � If battery light is red or yellow � Integrity of the unit is impaired

Designated Storage Areas PAPRs ♦ Central Supply for acute care areas ♦ Cardiopulmonary (personnel in this area frequently perform high hazard procedures) ♦ Emergency Department in case of a need to respond to a small event

References CAL-OSHA ATD Standard - http: //www. dir. ca. gov/title 8/5199. html CDC Guidelines for Preventing the Transmission of Mycobacterium tuberculosis in Health-Care Setting http: //www. cdc. gov/mmwr/preview/mmwrhtml/rr 5417 a 1. htm? s_cid= rr 5417 a 1 California Department of Public Health www. cdph. ca. gov/ Nicas et al. J Occupational Environmental Hygience 2005; 2: 143 -154
- Slides: 17