Power Point Lecture Slides prepared by Meg Flemming

Power. Point® Lecture Slides prepared by Meg Flemming Austin Community College 9 CHAPTER The General and Special Senses © 2013 Pearson Education, Inc.

Chapter 9 Learning Outcomes • 9 -1 • Explain how the organization of receptors for the general senses and the special senses affects their sensitivity. • 9 -2 • Identify the receptors for the general senses, and describe how they function. • 9 -3 • Describe the sensory organs of smell, and discuss the processes involved in olfaction. • 9 -4 • Describe the sensory organs of taste, and discuss the processes involved in gustation. © 2013 Pearson Education, Inc.

Chapter 9 Learning Outcomes • 9 -5 • Identify the internal and accessory structures of the eye, and explain their functions. • 9 -6 • Explain how we form visual images and distinguish colors, and discuss how the central nervous system processes visual information. • 9 -7 • Describe the parts of the external, middle, and internal ear, and the receptors they contain, and discuss the processes involved in the senses of equilibrium and hearing. • 9 -8 • Describe the effects of aging on smell, taste, vision, and hearing. © 2013 Pearson Education, Inc.

Sensory Receptors (9 -1) • Can be special cell processes • Or separate cells • Monitor conditions both inside and outside the body © 2013 Pearson Education, Inc.

Free Nerve Endings (9 -1) • The simplest receptors • Are modified dendritic endings • Examples: • Touch receptors • Pain receptors • Heat receptors • Taste receptors © 2013 Pearson Education, Inc.

Separate Receptor Cells (9 -1) • Complex structures • Associated with supportive cells • Examples: • Visual receptors in the eyes • Auditory receptors in the ears © 2013 Pearson Education, Inc.

The Receptive Field (9 -1) • The area monitored by a single receptor • The smaller the field, the more precise the sensory information © 2013 Pearson Education, Inc.
Sensation and Perception (9 -1) • Sensation • Occurs in the brain • The action potential from the afferent pathway arrives in sensory cortex • Perception • Awareness and interpretation of sensory input by the integration areas of cerebral cortex © 2013 Pearson Education, Inc.

Adaptation (9 -1) • A reduction in sensitivity due to a constant stimulus • Some sensory receptors adapt quickly (e. g. , jumping into a cold lake) • Some are slow to adapt or do not adapt at all, like pain receptors © 2013 Pearson Education, Inc.

General Senses (9 -1) • Temperature • Pain • Touch • Pressure • Vibration • Proprioception (body position) • Occur throughout the body © 2013 Pearson Education, Inc.

Special Senses (9 -1) • Olfaction (smell) • Gustation (taste) • Vision • Equilibrium (balance) • Hearing • Concentrated in the sense organs and located in the head © 2013 Pearson Education, Inc.
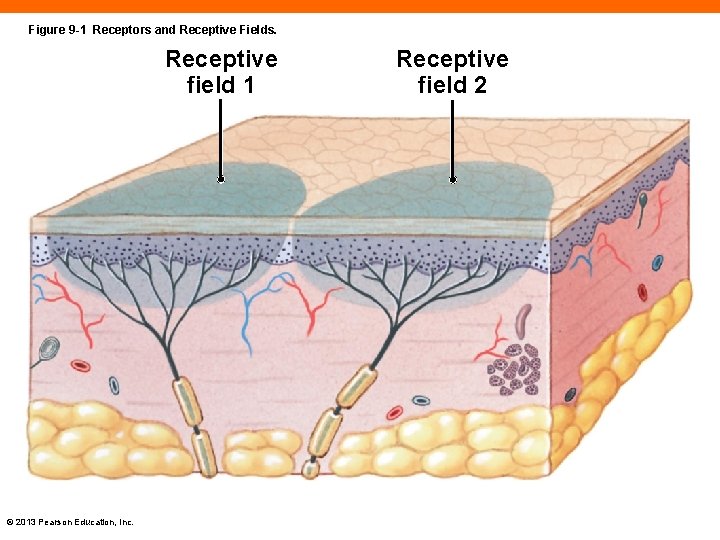
Figure 9 -1 Receptors and Receptive Fields. Receptive field 1 © 2013 Pearson Education, Inc. Receptive field 2

Checkpoint (9 -1) 1. What is adaptation? 2. Receptor A has a circular receptive field with a diameter of 2. 5 cm. Receptor B has a circular receptive field 7. 0 cm in diameter. Which receptor provides more precise sensory information? 3. List the five special senses. © 2013 Pearson Education, Inc.

Classes of General Sensory Receptors (9 -2) • Classified by type of stimulus that activates them • Nociceptors respond to pain • Thermoreceptors respond to temperature • Mechanoreceptors respond to touch, pressure, and body position • Chemoreceptors respond to chemical stimuli © 2013 Pearson Education, Inc.

Nociceptors (9 -2) • Free nerve endings that adapt very slowly • Can respond to extremes of temperature, mechanical damage, dissolved chemicals • Fast pain transmitted to CNS through myelinated axons • Slow pain transmitted by unmyelinated axons and is burning or aching • Referred pain is perception of pain in an unrelated area of the body © 2013 Pearson Education, Inc.
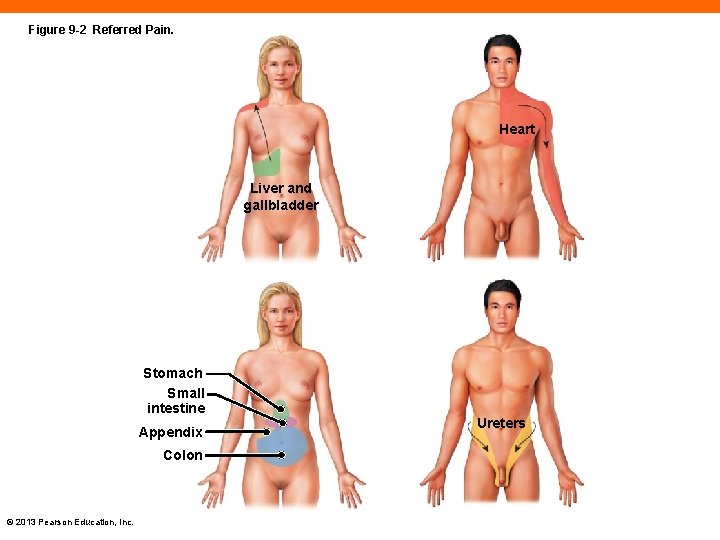
Figure 9 -2 Referred Pain. Heart Liver and gallbladder Stomach Small intestine Appendix Colon © 2013 Pearson Education, Inc. Ureters

Thermoreceptors (9 -2) • Free nerve endings • In dermis, skeletal muscles, liver, and hypothalamus • Cold receptors • More numerous than warm receptors, although there is no known difference in structure • They use the same pathway as pain receptors, but thermoreceptors are adaptive © 2013 Pearson Education, Inc.

Three Classes of Mechanoreceptors 1. Tactile receptors • Touch 2. Baroreceptors • Pressure 3. Proprioceptors • Position © 2013 Pearson Education, Inc.

Tactile Receptors (9 -2) • Include fine touch and pressure receptors and crude touch and pressure receptors • Six types of tactile receptors in the skin 1. Free nerve endings responding to temperature and pain 2. Root hair plexus 3. Tactile (Merkel) disc 4. Tactile (Meissner) corpuscle 5. Lamellated (pacinian) corpuscle 6. Ruffini corpuscle © 2013 Pearson Education, Inc.
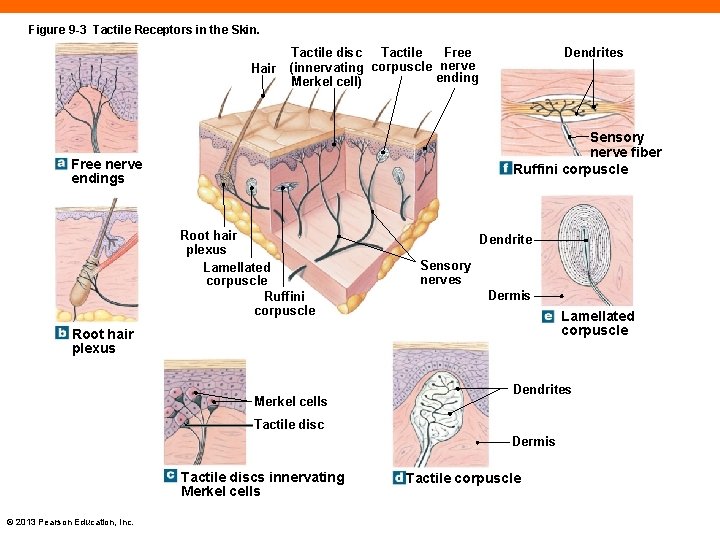
Figure 9 -3 Tactile Receptors in the Skin. Hair Free Tactile disc Tactile (innervating corpuscle nerve ending Merkel cell) Dendrites Sensory nerve fiber Ruffini corpuscle Free nerve endings Root hair plexus Lamellated corpuscle Ruffini corpuscle Dendrite Sensory nerves Dermis Lamellated corpuscle Root hair plexus Merkel cells Dendrites Tactile disc Dermis Tactile discs innervating Merkel cells © 2013 Pearson Education, Inc. Tactile corpuscle

Baroreceptors (9 -2) • Monitor changes in pressure in the viscera • Adapt readily • Found in the major blood vessels, lungs, digestive, and urinary tracts © 2013 Pearson Education, Inc.
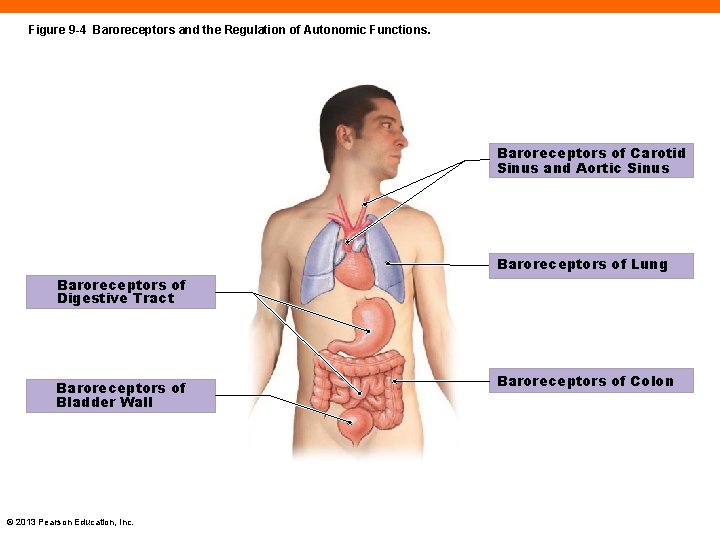
Figure 9 -4 Baroreceptors and the Regulation of Autonomic Functions. Baroreceptors of Carotid Sinus and Aortic Sinus Baroreceptors of Lung Baroreceptors of Digestive Tract Baroreceptors of Bladder Wall © 2013 Pearson Education, Inc. Baroreceptors of Colon

Proprioceptors (9 -2) • Monitor position, tension in tendons and ligaments, state of muscle contraction • Nonadaptive and include: • Free nerve endings that monitor joint capsule pressure, tension, and movement • Golgi tendon organs that monitor strain on tendons • Muscle spindles that monitor the length of a muscle © 2013 Pearson Education, Inc.

Chemoreceptors (9 -2) • Respond to chemicals in solution in body fluids • Include CNS receptors that monitor CSF, plasma concentrations of carbon dioxide, and p. H • Key peripheral chemoreceptors for plasma carbon dioxide and p. H are in the carotid bodies and aortic bodies © 2013 Pearson Education, Inc.
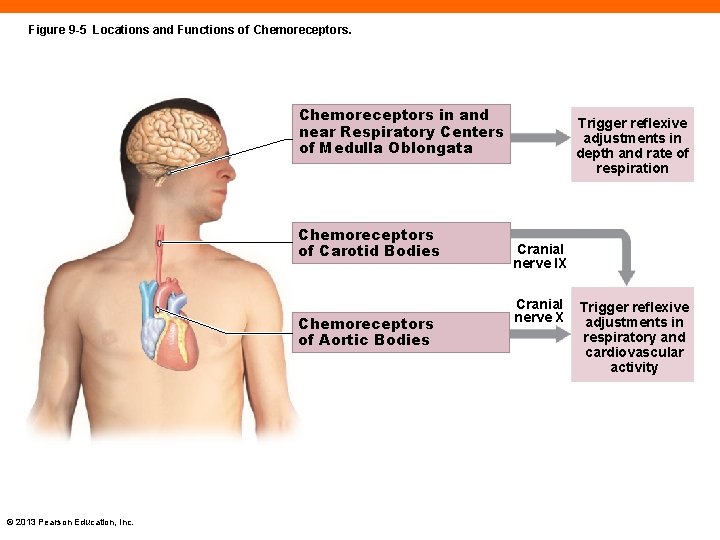
Figure 9 -5 Locations and Functions of Chemoreceptors in and near Respiratory Centers of Medulla Oblongata Chemoreceptors of Carotid Bodies Chemoreceptors of Aortic Bodies © 2013 Pearson Education, Inc. Trigger reflexive adjustments in depth and rate of respiration Cranial nerve IX Cranial nerve X Trigger reflexive adjustments in respiratory and cardiovascular activity

Checkpoint (9 -2) 4. List the four types of general sensory receptors, and identify the nature of the stimulus that excites each type. 5. Identify the three classes of mechanoreceptors. 6. What would happen if information from proprioceptors in your legs were blocked from reaching the CNS? © 2013 Pearson Education, Inc.
Special Sense of Olfaction (9 -3) • Olfactory organs found in the nasal cavity • Olfactory epithelium, containing olfactory receptor cells, supporting cells, and stem cells, lines the nasal cavity • Olfactory glands, which are deeper, secrete mucus • Air is warmed and moisturized as it is inhaled © 2013 Pearson Education, Inc.

Special Sense of Olfaction (9 -3) • Olfactory receptor cells • Modified neurons with chemical receptors called odorant -binding proteins on the cilia • Odorants are chemicals in the air that bind to the proteins • Respond to over 1000 unique smells © 2013 Pearson Education, Inc.

Olfactory Pathways (9 -3) • Axons projecting from the olfactory epithelium • Bundled and pass through the cribriform plate of the ethmoid bone and into olfactory bulb • Olfactory tracts extend back to the olfactory cortex of the cerebrum, the hypothalamus, and the limbic system • Olfaction is the only sense that is NOT routed through the thalamus © 2013 Pearson Education, Inc.
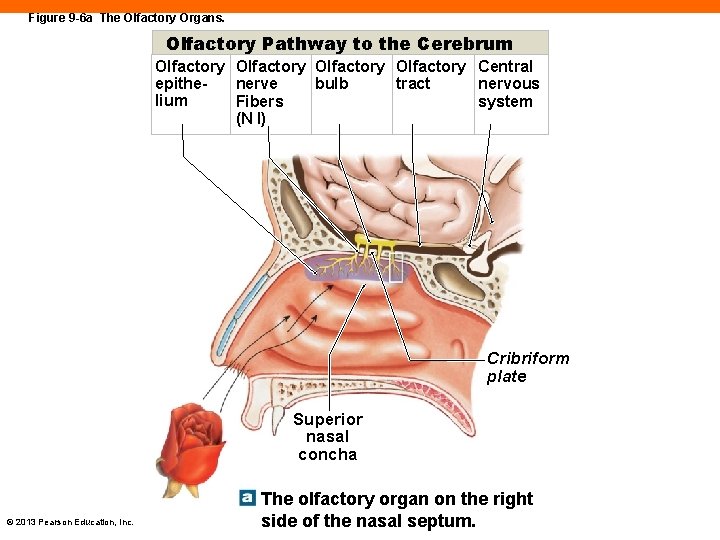
Figure 9 -6 a The Olfactory Organs. Olfactory Pathway to the Cerebrum Olfactory Central epithebulb nerve tract nervous lium Fibers system (N I) Cribriform plate Superior nasal concha © 2013 Pearson Education, Inc. The olfactory organ on the right side of the nasal septum.
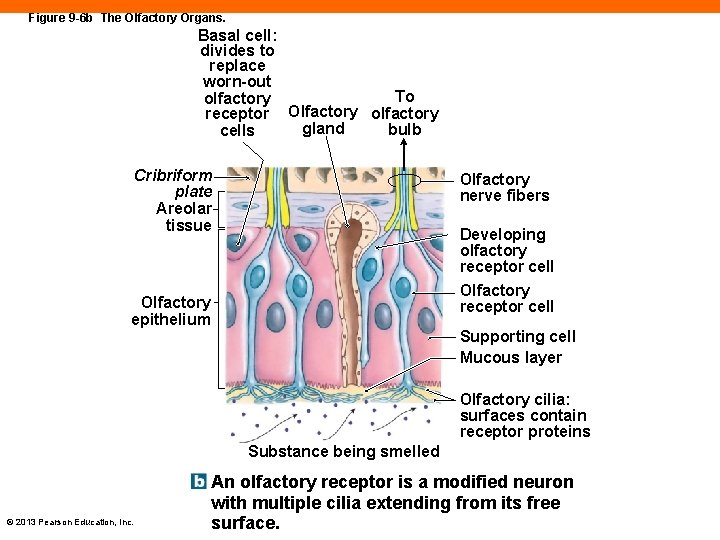
Figure 9 -6 b The Olfactory Organs. Basal cell: divides to replace worn-out To olfactory receptor Olfactory olfactory gland bulb cells Cribriform plate Areolar tissue Olfactory nerve fibers Developing olfactory receptor cell Olfactory epithelium Supporting cell Mucous layer Olfactory cilia: surfaces contain receptor proteins Substance being smelled © 2013 Pearson Education, Inc. An olfactory receptor is a modified neuron with multiple cilia extending from its free surface.

Checkpoint (9 -3) 7. Define olfaction. 8. How does repeated sniffing help to identify faint odors? © 2013 Pearson Education, Inc.

Special Sense of Gustation (9 -4) • Gustatory receptors • Found in the gustatory cells of the taste buds, which are found on the sides of the papillae • Circumvallate papillae most numerous and on the front 2/3 of the tongue • Gustatory cells have microvilli (taste hairs) that extend out through the taste pore © 2013 Pearson Education, Inc.

Special Sense of Gustation (9 -4) • Taste hairs respond to chemicals in solution • Trigger a change in the membrane potential of the taste cells • Primary taste sensations • Sweet, sour, bitter, salty, and umami • Also receptors in the pharynx for water © 2013 Pearson Education, Inc.

The Taste Pathway (9 -4) • Extends from the taste cell axons found in: • Facial nerve (N VII) • Glossopharyngeal (N IX) • Vagus (N X) • Fibers synapse in the medulla oblongata • Those neurons extend into the thalamus • Neurons project to the primary sensory cortex © 2013 Pearson Education, Inc.
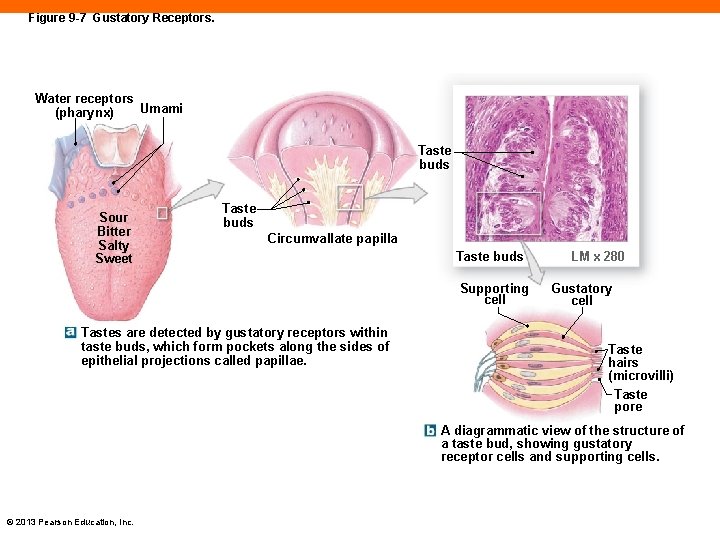
Figure 9 -7 Gustatory Receptors. Water receptors Umami (pharynx) Taste buds Sour Bitter Salty Sweet Taste buds Circumvallate papilla Taste buds Supporting cell Tastes are detected by gustatory receptors within taste buds, which form pockets along the sides of epithelial projections called papillae. LM x 280 Gustatory cell Taste hairs (microvilli) Taste pore A diagrammatic view of the structure of a taste bud, showing gustatory receptor cells and supporting cells. © 2013 Pearson Education, Inc.

Checkpoint (9 -4) 9. Define gustation. 10. If you completely dry the surface of your tongue and then place salt or sugar crystals on it, you cannot taste them. Why not? © 2013 Pearson Education, Inc.

The Accessory Structures of the Eye (9 -5) 1. Eyelids and associated exocrine glands 2. The superficial epithelium of the eye 3. Structures associated with the production, secretion, and removal of tears 4. The extrinsic eye muscles © 2013 Pearson Education, Inc.

The Eyelids (9 -5) • Also called palpebrae • Upper and lower eyelids join at the medial canthus and lateral canthus • At the medial canthus, glands that secrete gritty "sleep" are found in the lacrimal caruncle • Have sebaceous glands that can become infected, known as a sty © 2013 Pearson Education, Inc.

Conjunctiva (9 -5) • Inner surface of the eyelids • And the outer, white surface of the eye, up to the edge of the cornea • Irritation or damage to the conjunctiva is called conjunctivitis, or pinkeye © 2013 Pearson Education, Inc.

The Lacrimal Apparatus (9 -5) • Produces essential tears, distributes them across the eye, and removes them • The lacrimal gland secretes the tears and is superior and lateral to the eyeball • Tears drain through two pores at the medial canthus called the lacrimal canals and into the nasolacrimal duct PLAY ANIMATION The Eye: Accessory Structures © 2013 Pearson Education, Inc.
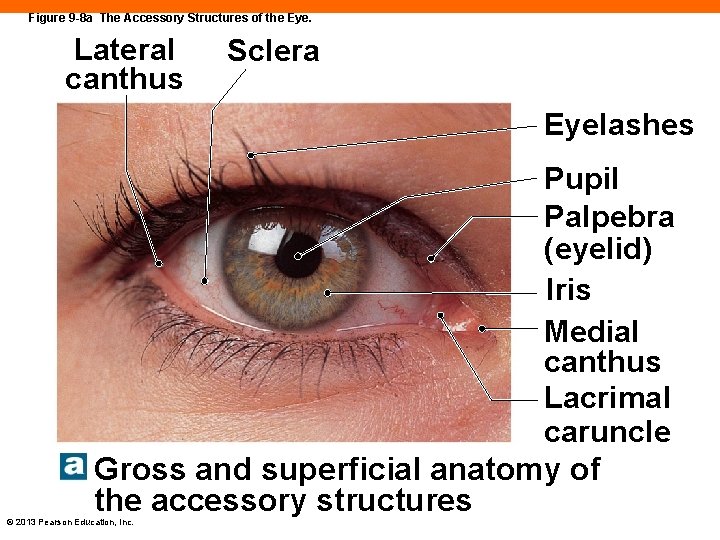
Figure 9 -8 a The Accessory Structures of the Eye. Lateral canthus Sclera Eyelashes Pupil Palpebra (eyelid) Iris Medial canthus Lacrimal caruncle Gross and superficial anatomy of the accessory structures © 2013 Pearson Education, Inc.
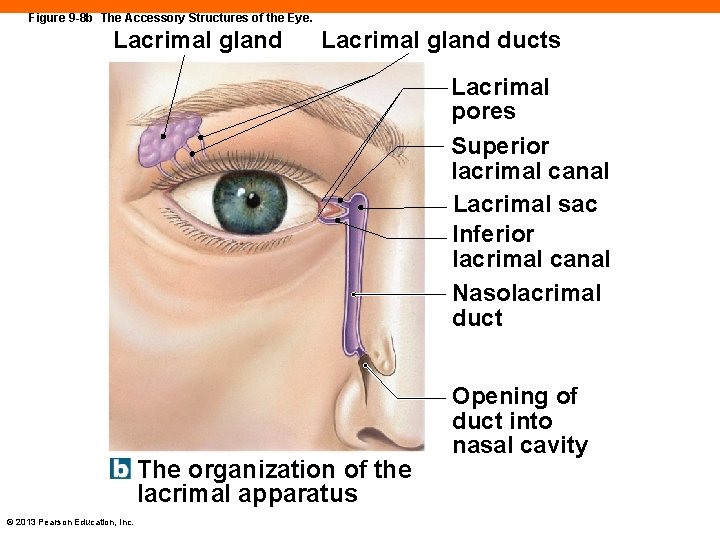
Figure 9 -8 b The Accessory Structures of the Eye. Lacrimal gland ducts Lacrimal pores Superior lacrimal canal Lacrimal sac Inferior lacrimal canal Nasolacrimal duct The organization of the lacrimal apparatus © 2013 Pearson Education, Inc. Opening of duct into nasal cavity

The Extrinsic Eye Muscles (9 -5) • Control the position of the eye and include: • Inferior rectus • Medial rectus • Superior rectus • Lateral rectus • Inferior oblique • Superior oblique © 2013 Pearson Education, Inc.
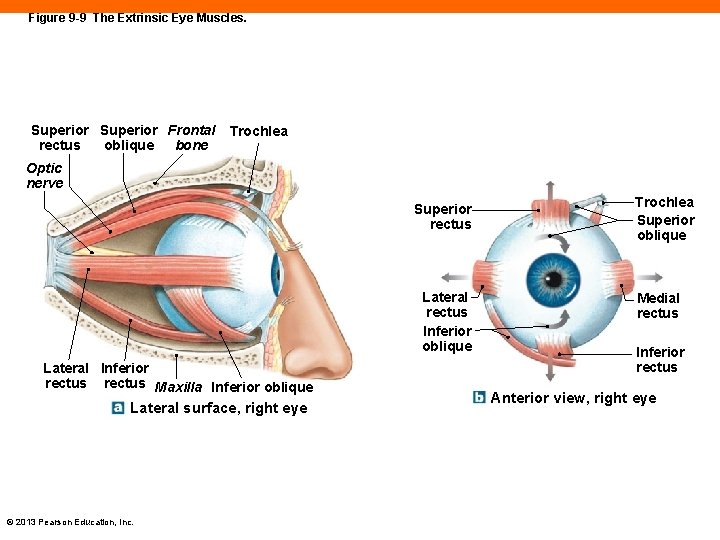
Figure 9 -9 The Extrinsic Eye Muscles. Superior Frontal rectus oblique bone Trochlea Optic nerve Superior rectus Lateral rectus Inferior oblique Lateral Inferior rectus Maxilla Inferior oblique Lateral surface, right eye © 2013 Pearson Education, Inc. Trochlea Superior oblique Medial rectus Inferior rectus Anterior view, right eye
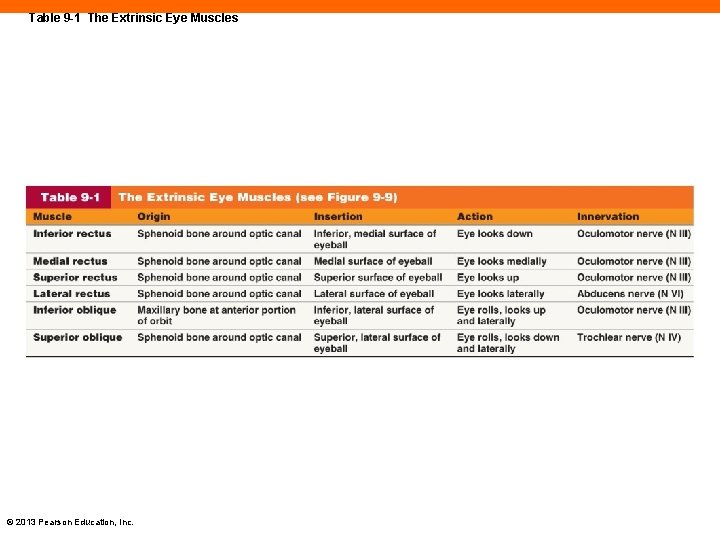
Table 9 -1 The Extrinsic Eye Muscles © 2013 Pearson Education, Inc.
The Eye (9 -5) • Found in the orbit with the: • Lacrimal glands • Extrinsic eye muscles • Cranial nerves • Blood vessels • Orbital fat cushions the eye © 2013 Pearson Education, Inc.

The Eyeball (9 -5) • The eyeball is hollow and divided into two cavities 1. Posterior cavity • Filled with jellylike vitreous body 2. Anterior cavity has two subdivisions • The anterior and posterior chambers • Filled with aqueous humor © 2013 Pearson Education, Inc.

The Fibrous Layer of the Eyeball (9 -5) • The sclera • The white of the eye • Supportive dense connective tissue • The cornea • Transparent • Allows light to enter the eye © 2013 Pearson Education, Inc.
The Vascular Layer of the Eyeball (9 -5) • Contains blood and lymphatic vessels, and the intrinsic eye muscles • Functions 1. Providing a route for vessels supplying the tissue 2. Adjusting the amount of light entering the eye 3. Providing a route for secreting and reabsorbing aqueous humor 4. Controlling the shape of the lens © 2013 Pearson Education, Inc.
The Vascular Layer of the Eyeball (9 -5) • Structures • The iris, with pupillary muscles that change the size of the pupil, the "window" into the eye • The ciliary body, which contains the ciliary muscle and ciliary processes, and the suspensory ligaments, which adjust the shape of the lens for focusing • The choroid, a highly vascular tissue PLAY ANIMATION The Eye: Cilliary Muscles © 2013 Pearson Education, Inc.
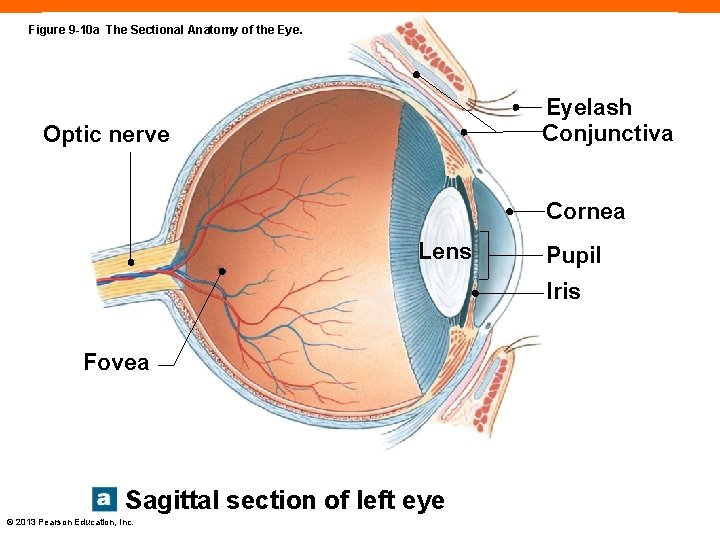
Figure 9 -10 a The Sectional Anatomy of the Eyelash Conjunctiva Optic nerve Cornea Lens Pupil Iris Fovea Sagittal section of left eye © 2013 Pearson Education, Inc.
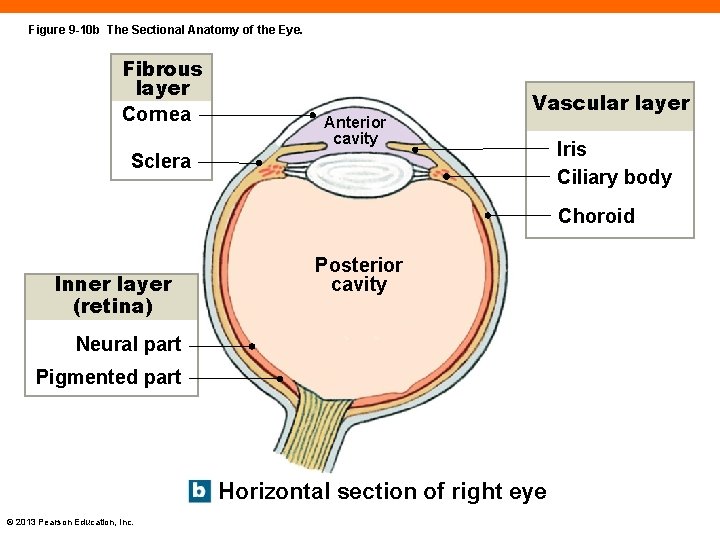
Figure 9 -10 b The Sectional Anatomy of the Eye. Fibrous layer Cornea Anterior cavity Vascular layer Sclera Iris Ciliary body Choroid Inner layer (retina) Posterior cavity Neural part Pigmented part Horizontal section of right eye © 2013 Pearson Education, Inc.
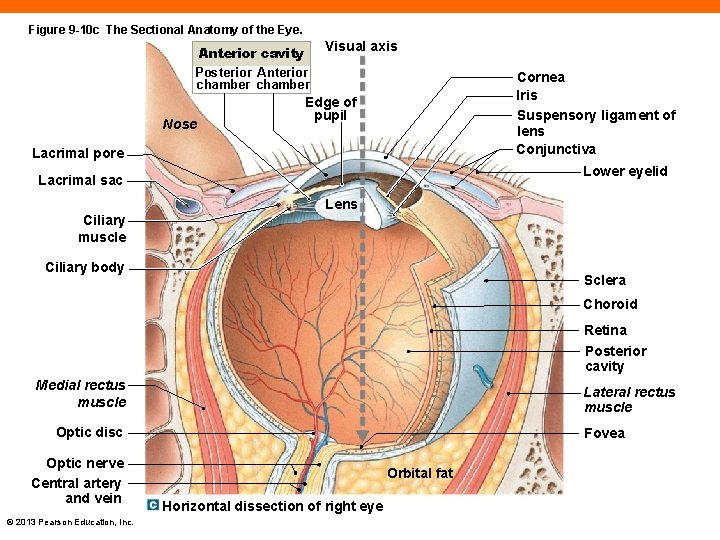
Figure 9 -10 c The Sectional Anatomy of the Eye. Anterior cavity Posterior Anterior chamber Nose Visual axis Cornea Iris Suspensory ligament of lens Conjunctiva Edge of pupil Lacrimal pore Lower eyelid Lacrimal sac Ciliary muscle Lens Ciliary body Sclera Choroid Retina Posterior cavity Medial rectus muscle Lateral rectus muscle Optic disc Optic nerve Central artery and vein © 2013 Pearson Education, Inc. Fovea Orbital fat Horizontal dissection of right eye
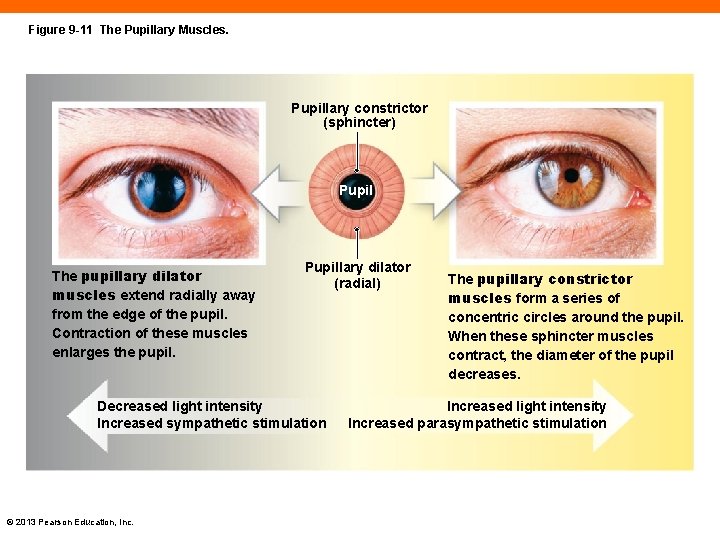
Figure 9 -11 The Pupillary Muscles. Pupillary constrictor (sphincter) Pupil The pupillary dilator muscles extend radially away from the edge of the pupil. Contraction of these muscles enlarges the pupil. . dilator Pupillary (radial) Decreased light intensity Increased sympathetic stimulation © 2013 Pearson Education, Inc. The pupillary constrictor muscles form a series of concentric circles around the pupil. When these sphincter muscles contract, the diameter of the pupil decreases. Increased light intensity Increased parasympathetic stimulation
The Inner Layer (9 -5) • Also called the retina • The inner layer includes: • A pigmented part, which absorbs light • A neural part that contains the photoreceptors • Supportive cells and neurons • Blood vessels © 2013 Pearson Education, Inc.

Photoreceptors (9 -5) • Rods • Used in dim light • Found on the periphery of retinal surface • Cones • Used in bright light and detect color • Found in the macula, the center of which is the fovea, or fovea centralis © 2013 Pearson Education, Inc.
The Inner Layer (9 -5) • Rods and cones synapse with bipolar cells, which synapse with ganglion cells • Ganglion cells • These axons leave the back of the eye through the optic disc, the origin of the optic nerve • The blind spot is where there are no photoreceptors on the retina PLAY ANIMATION The © 2013 Pearson Education, Inc. Eye: The Retina
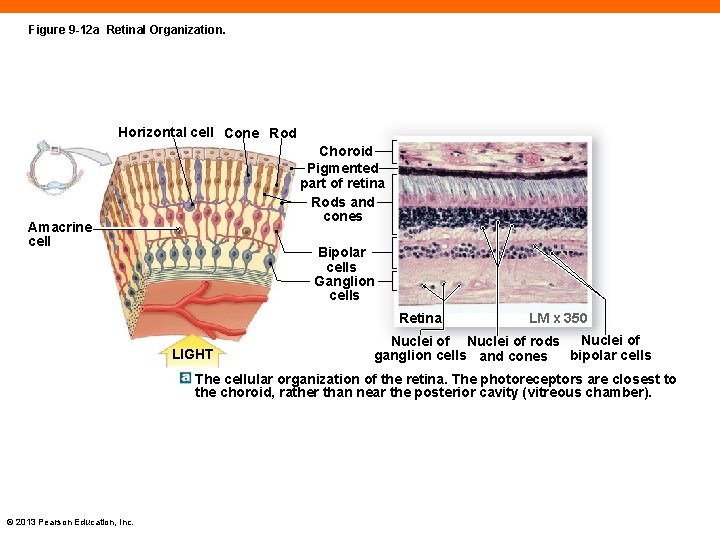
Figure 9 -12 a Retinal Organization. Horizontal cell Cone Rod Choroid Pigmented part of retina Rods and cones Amacrine cell Bipolar cells Ganglion cells Retina LIGHT LM x 350 Nuclei of rods ganglion cells and cones bipolar cells The cellular organization of the retina. The photoreceptors are closest to the choroid, rather than near the posterior cavity (vitreous chamber). © 2013 Pearson Education, Inc.
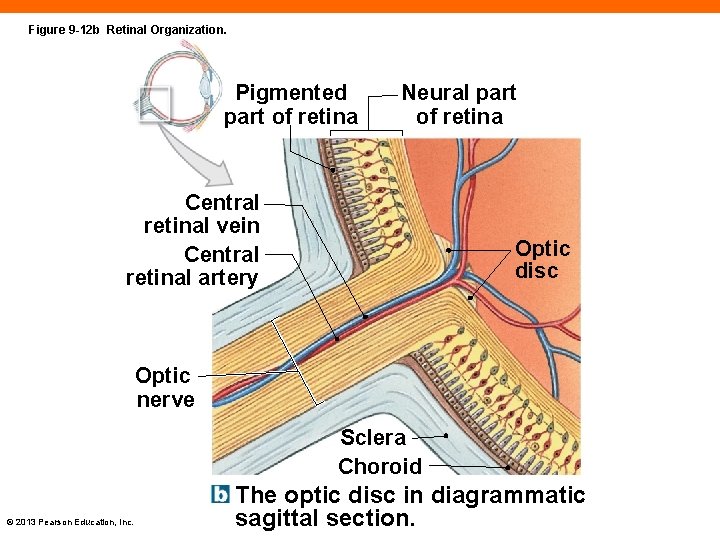
Figure 9 -12 b Retinal Organization. Pigmented part of retina Neural part of retina Central retinal vein Central retinal artery Optic disc Optic nerve Sclera Choroid © 2013 Pearson Education, Inc. The optic disc in diagrammatic sagittal section.
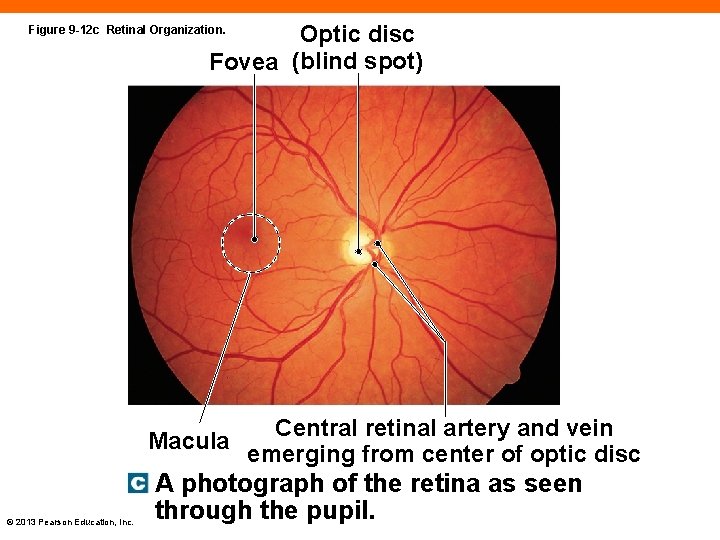
Optic disc Fovea (blind spot) Figure 9 -12 c Retinal Organization. Central retinal artery and vein Macula emerging from center of optic disc © 2013 Pearson Education, Inc. A photograph of the retina as seen through the pupil.

Figure 9 -13 A Demonstration of the Presence of a Blind Spot. © 2013 Pearson Education, Inc.
The Chambers of the Eye (9 -5) • Anterior cavity • Anterior chamber extends from the cornea to the iris • Posterior chamber between the iris and the lens • Filled with aqueous humor produced by the ciliary processes • Maintains pressure in eye • Drains out through the scleral venous sinus © 2013 Pearson Education, Inc.

The Chambers of the Eye (9 -5) • Problems with fluid and pressure is a condition called glaucoma • Posterior cavity • Filled with the vitreous body • Holds the retina in place © 2013 Pearson Education, Inc.
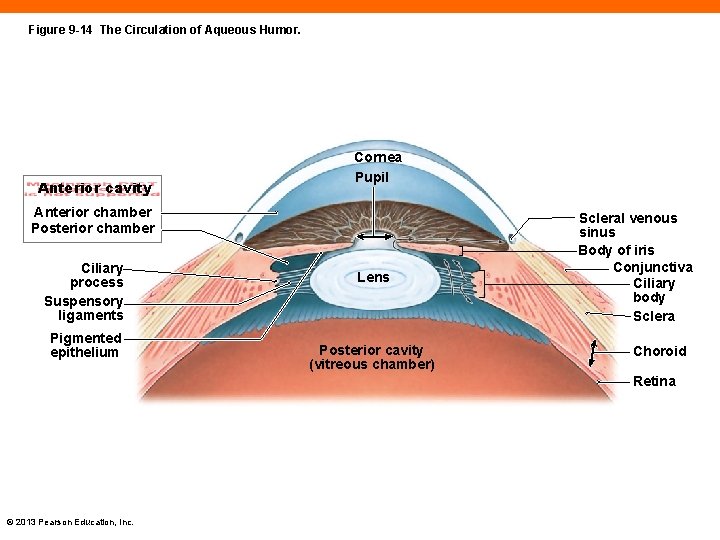
Figure 9 -14 The Circulation of Aqueous Humor. Anterior cavity Cornea Pupil Anterior chamber Posterior chamber Ciliary process Suspensory ligaments Pigmented epithelium Lens Posterior cavity (vitreous chamber) Scleral venous sinus Body of iris Conjunctiva Ciliary body Sclera Choroid Retina © 2013 Pearson Education, Inc.

The Lens (9 -5) • Posterior to cornea • Held in place by suspensory ligaments • Cells • Are wrapped in concentric circle • Elastic fibers make lens spherical • Changes shape to accommodate for focus © 2013 Pearson Education, Inc.

Light Refraction and Accommodation (9 -5) • Light is bent or refracted as it enters the cornea and lens • Light rays converge on retina at focal point • Focal distance is between lens and focal point • For far-away objects, the ciliary muscles relax, flattening the lens • For close objects, the lens accommodates by rounding when the ciliary muscles contract PLAY ANIMATION The © 2013 Pearson Education, Inc. Eye: Light Path
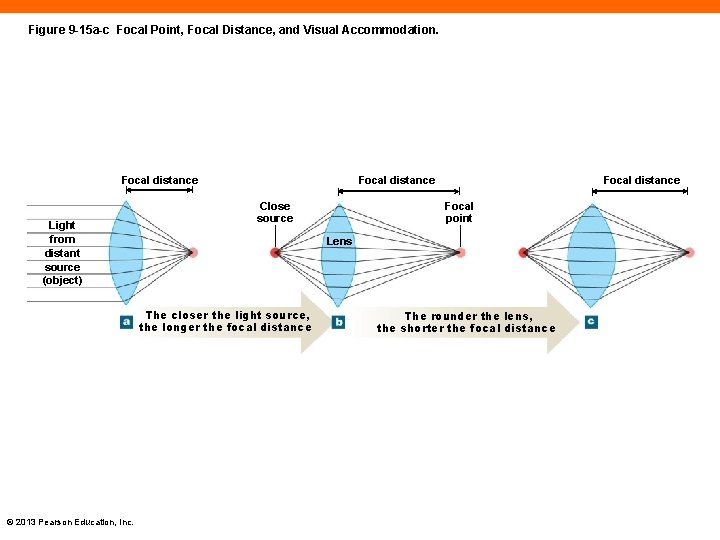
Figure 9 -15 a-c Focal Point, Focal Distance, and Visual Accommodation. Focal distance Light from distant source (object) Focal distance Close source Focal point Lens The closer the light source, the longer the focal distance © 2013 Pearson Education, Inc. Focal distance The rounder the lens, the shorter the focal distance
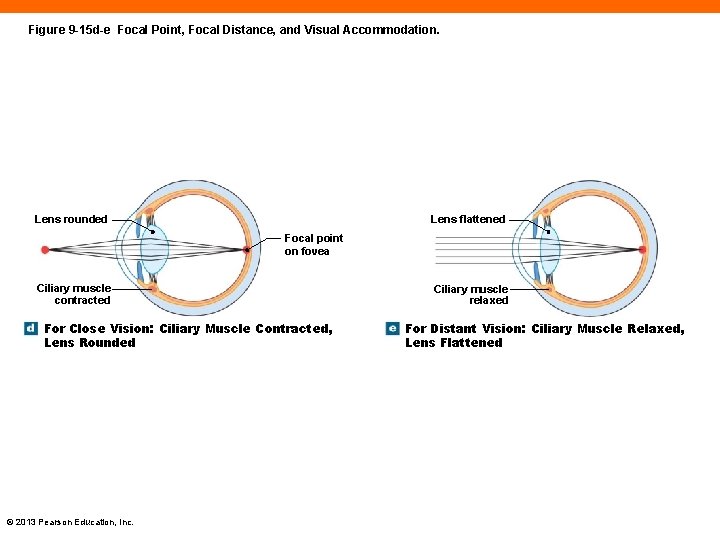
Figure 9 -15 d-e Focal Point, Focal Distance, and Visual Accommodation. Lens flattened Lens rounded Focal point on fovea Ciliary muscle contracted For Close Vision: Ciliary Muscle Contracted, Lens Rounded © 2013 Pearson Education, Inc. Ciliary muscle relaxed For Distant Vision: Ciliary Muscle Relaxed, Lens Flattened
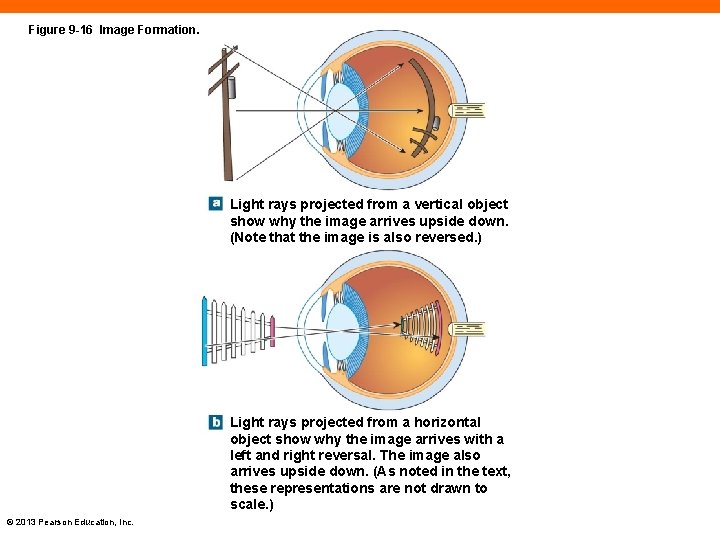
Figure 9 -16 Image Formation. Light rays projected from a vertical object show why the image arrives upside down. (Note that the image is also reversed. ) Light rays projected from a horizontal object show why the image arrives with a left and right reversal. The image also arrives upside down. (As noted in the text, these representations are not drawn to scale. ) © 2013 Pearson Education, Inc.
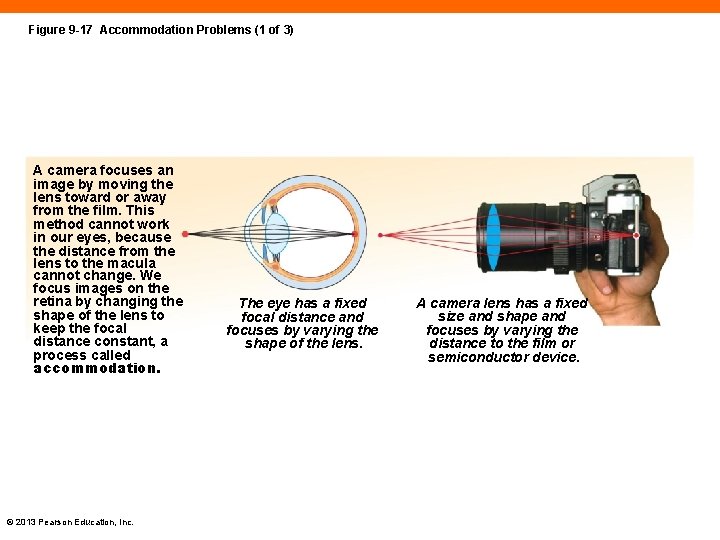
Figure 9 -17 Accommodation Problems (1 of 3) A camera focuses an image by moving the lens toward or away from the film. This method cannot work in our eyes, because the distance from the lens to the macula cannot change. We focus images on the retina by changing the shape of the lens to keep the focal distance constant, a process called accommodation. © 2013 Pearson Education, Inc. The eye has a fixed focal distance and focuses by varying the shape of the lens. A camera lens has a fixed size and shape and focuses by varying the distance to the film or semiconductor device.
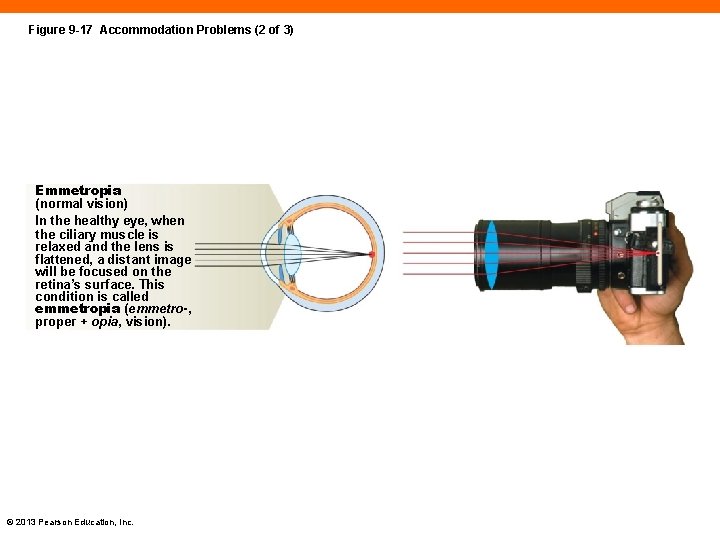
Figure 9 -17 Accommodation Problems (2 of 3) Emmetropia (normal vision) In the healthy eye, when the ciliary muscle is relaxed and the lens is flattened, a distant image will be focused on the retina’s surface. This condition is called emmetropia (emmetro-, proper + opia, vision). © 2013 Pearson Education, Inc.
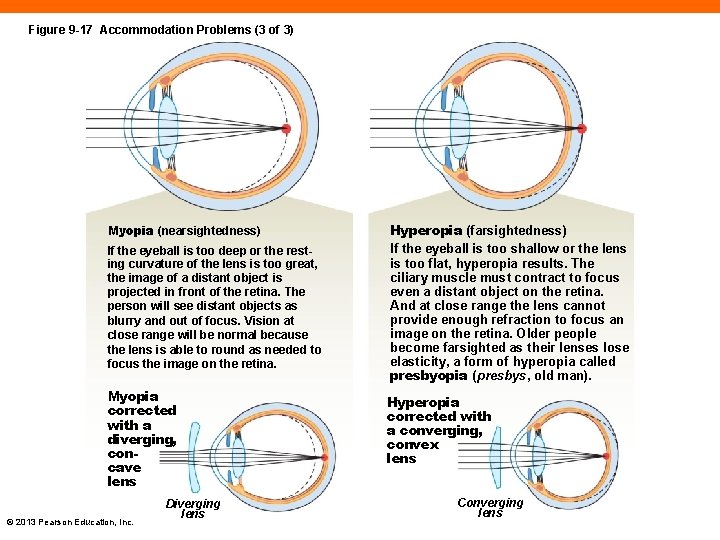
Figure 9 -17 Accommodation Problems (3 of 3) Myopia (nearsightedness) If the eyeball is too deep or the resting curvature of the lens is too great, the image of a distant object is projected in front of the retina. The person will see distant objects as blurry and out of focus. Vision at close range will be normal because the lens is able to round as needed to focus the image on the retina. Myopia corrected with a diverging, concave lens © 2013 Pearson Education, Inc. Diverging lens Hyperopia (farsightedness) If the eyeball is too shallow or the lens is too flat, hyperopia results. The ciliary muscle must contract to focus even a distant object on the retina. And at close range the lens cannot provide enough refraction to focus an image on the retina. Older people become farsighted as their lenses lose elasticity, a form of hyperopia called presbyopia (presbys, old man). Hyperopia corrected with a converging, convex lens Converging lens

Checkpoint (9 -5) 11. Which layer of the eye would be the first to be affected by inadequate tear production? 12. When the lens is more rounded, are you looking at an object that is close to you or far from you? 13. As Malia enters a dimly lit room, most of the available light becomes focused on the fovea of her eye. Will she be able to see very clearly? © 2013 Pearson Education, Inc.

Photoreceptors Respond to Photons (9 -6) • Photons are units of visible light • Red, orange, yellow, green, blue, indigo, violet • Color determined by wavelength • Photons of red have longest wavelength, least energy • Photons of violet have shortest wavelength, most energy © 2013 Pearson Education, Inc.

Photoreceptors in the Eye (9 -6) • Rods • Respond to presence or absence of photons regardless of wavelength • Very sensitive, therefore effective in dim light • Cones • Three different types • Blue cones, green cones, red cones • Contain pigments sensitive to blue, green, or red wavelengths of light • Less sensitive, therefore function only in bright light © 2013 Pearson Education, Inc.

Color Blindness (9 -6) • Occurs when one or more types of cone is not functioning or is missing • Most common is red-green color blindness where red cones are missing • More common in males (10 percent) than females percent) • Total color blindness is extremely rare (1 person in 300, 000) © 2013 Pearson Education, Inc. (0. 67

Figure 9 -18 A Standard Test for Color Vision. © 2013 Pearson Education, Inc.

The Structure of Photoreceptors (9 -6) • Outer segment contains hundreds to thousands of flattened discs • Contain visual pigments that absorb photons and initiate photoreception • Made of compound rhodopsin that contains opsin and retinal (derived from vitamin A) • Retinal is the same in rods and cones, opsin is different • Inner segment contains organelles, synapses with bipolar cells © 2013 Pearson Education, Inc.
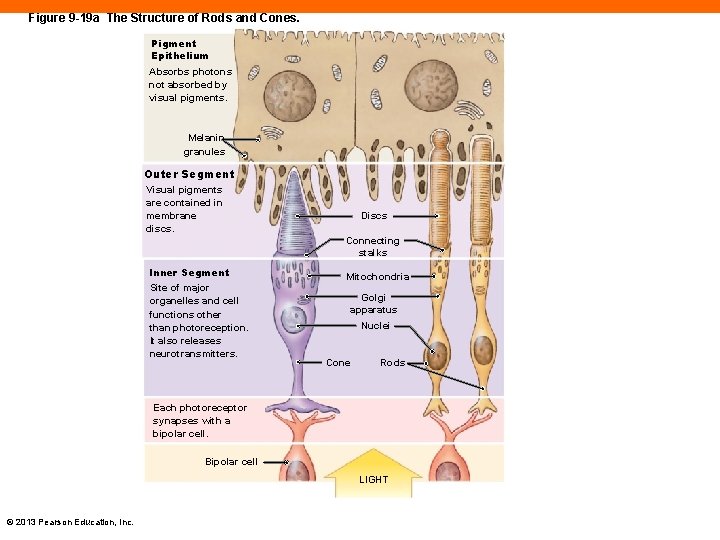
Figure 9 -19 a The Structure of Rods and Cones. Pigment Epithelium Absorbs photons not absorbed by visual pigments. Melanin granules Outer Segment Visual pigments are contained in membrane discs. Discs Connecting stalks Inner Segment Site of major organelles and cell functions other than photoreception. It also releases neurotransmitters. Mitochondria Golgi apparatus Nuclei Cone Rods Each photoreceptor synapses with a bipolar cell. Bipolar cell LIGHT © 2013 Pearson Education, Inc.
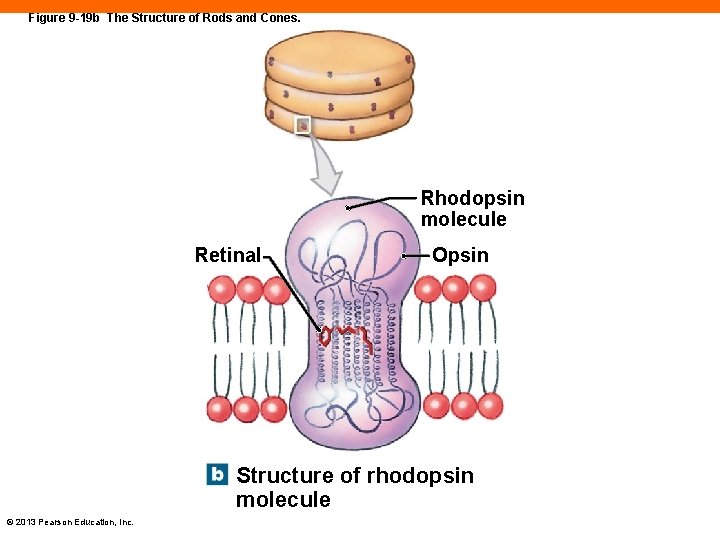
Figure 9 -19 b The Structure of Rods and Cones. Rhodopsin molecule Retinal Opsin Structure of rhodopsin molecule © 2013 Pearson Education, Inc.

Photoreception (9 -6) • Photon strikes rhodopsin • Retinal and opsin break apart, referred to as bleaching • Alters rate of neurotransmitter release into synapse with bipolar cell • For rod or cone to be able to respond to light again, the opsin and retinal must recombine © 2013 Pearson Education, Inc.
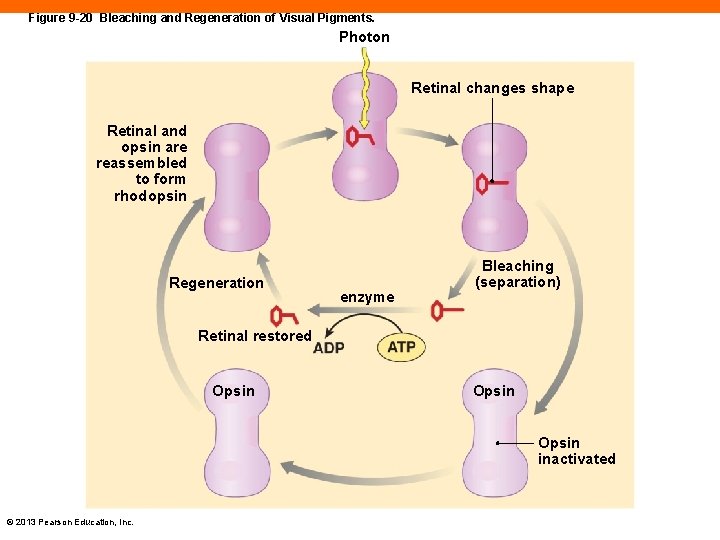
Figure 9 -20 Bleaching and Regeneration of Visual Pigments. Photon Retinal changes shape Retinal and opsin are reassembled to form rhodopsin Regeneration enzyme Bleaching (separation) Retinal restored Opsin inactivated © 2013 Pearson Education, Inc.
The Visual Pathways (9 -6) • Photoreceptor bipolar cell ganglion cell • Axons from optic nerves (N II) optic chiasm • Medial fibers cross, lateral fibers do not cross • Optic tracts thalamic nuclei • Superior colliculi of midbrain controls eye reflexes • Thalamic axons visual cortex of cerebrum © 2013 Pearson Education, Inc.
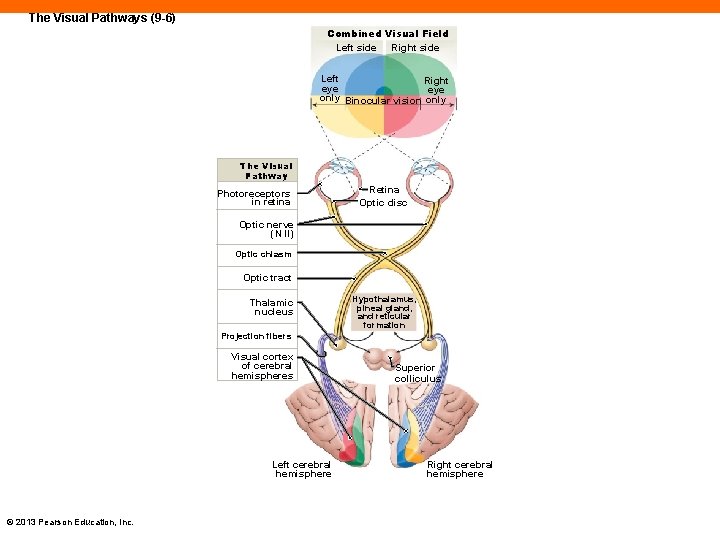
The Visual Pathways (9 -6) Combined Visual Field Left side Right side Left Right eye only Binocular vision only The Visual Pathway Photoreceptors in retina Retina Optic disc Optic nerve (N II) Optic chiasm Optic tract Thalamic nucleus Hypothalamus, pineal gland, and reticular formation Projection fibers Visual cortex of cerebral hemispheres Left cerebral hemisphere © 2013 Pearson Education, Inc. Superior colliculus Right cerebral hemisphere

Checkpoint (9 -6) 14. Are individuals born without cone cells able to see? Explain. 15. How would a diet deficient in vitamin A affect vision? © 2013 Pearson Education, Inc.
Anatomy of the Ear (9 -7) • External ear • Visible portion, collects sound waves • Middle ear • Chamber with structures that amplify sound waves • Internal ear • Contains sensory organs for hearing and equilibrium PLAY ANIMATION The Ear: Ear Anatomy © 2013 Pearson Education, Inc.
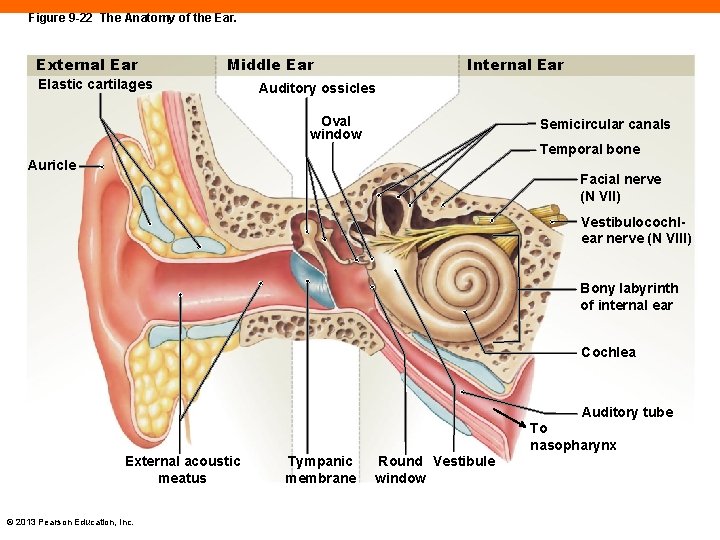
Figure 9 -22 The Anatomy of the Ear. External Ear Middle Ear Elastic cartilages Internal Ear Auditory ossicles Oval window Semicircular canals Temporal bone Auricle Facial nerve (N VII) Vestibulocochlear nerve (N VIII) Bony labyrinth of internal ear Cochlea Auditory tube To nasopharynx External acoustic meatus © 2013 Pearson Education, Inc. Tympanic membrane Round Vestibule window

The External Ear (9 -7) • Auricle or pinna is fleshy "cup" directing sound into ear • External acoustic meatus or auditory canal • Contains ceruminous glands, secreting earwax • Tympanic membrane or eardrum • Thin sheet that vibrates when sound waves strike it © 2013 Pearson Education, Inc.

The Middle Ear (9 -7) • Also called the tympanic cavity • Air-filled chamber • Auditory tube • Also called pharyngotympanic or Eustachian tube • Leads to the pharynx, making a path for microorganisms to trigger otitis media, an infection • Allows for pressure equalization on either side of eardrum © 2013 Pearson Education, Inc.

The Auditory Ossicles (9 -7) • Three small bones in middle ear that connect tympanic membrane to internal ear 1. Malleus attaches to eardrum 2. Incus attaches malleus to innermost bone 3. Stapes has a base that nearly fills the oval window into the internal ear © 2013 Pearson Education, Inc.
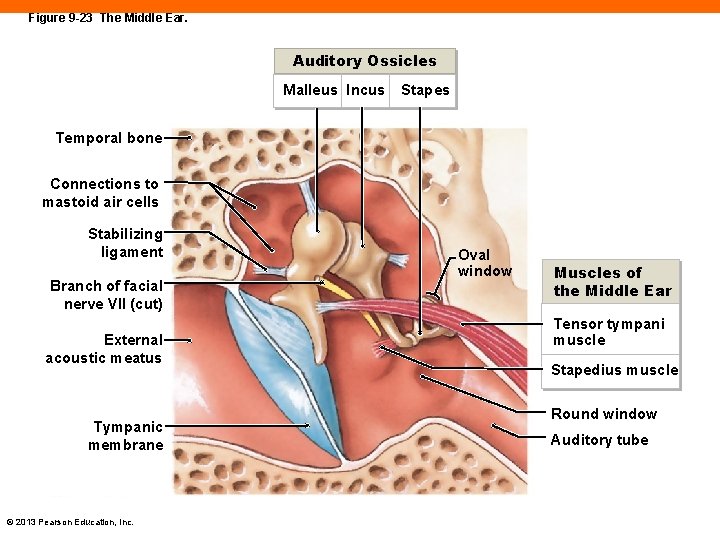
Figure 9 -23 The Middle Ear. Auditory Ossicles Malleus Incus Stapes Temporal bone Connections to mastoid air cells Stabilizing ligament Branch of facial nerve VII (cut) External acoustic meatus Tympanic membrane © 2013 Pearson Education, Inc. Oval window Muscles of the Middle Ear Tensor tympani muscle Stapedius muscle Round window Auditory tube

The Internal Ear (9 -7) • Sensory structures protected by bony labyrinth • Contains fluid perilymph between bony and membranous labyrinths • Inside bony labyrinth is membranous labyrinth • Tubes that follow contours of bony labyrinth • Filled with fluid endolymph © 2013 Pearson Education, Inc.

Three Parts of the Bony Labyrinth (9 -7) 1. Vestibule • Contains membranous saccule and utricle with receptors for gravity and linear acceleration 2. Semicircular canals • Contain membranous semicircular ducts with receptors for rotational acceleration • Vestibular complex is the combination of the first two, providing sense of balance © 2013 Pearson Education, Inc.

Three Parts of the Bony Labyrinth (9 -7) 3. Cochlea • Contains the membranous cochlear duct • Sensory receptors for hearing • Oval window is covered with thin membrane separating perilymph in cochlea from air in middle ear • Round window is opening in the bone of the cochlea © 2013 Pearson Education, Inc.

Hair Cells (9 -7) • Sensory receptors in internal ear • Surrounded by supporting cells • Synapse with dendrites of sensory neurons • Free surface covered with stereocilia • Movement of stereocilia alters neurotransmitter release • Bending stereocilia in one direction triggers depolarization; in the other direction, hyperpolarization © 2013 Pearson Education, Inc.
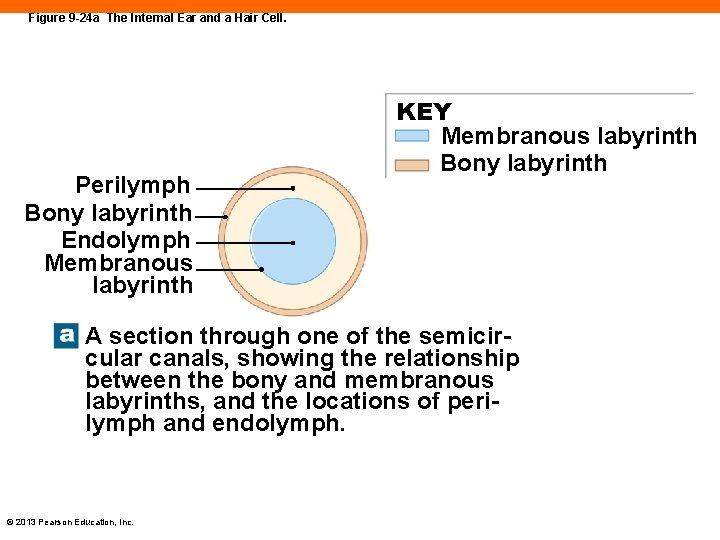
Figure 9 -24 a The Internal Ear and a Hair Cell. Perilymph Bony labyrinth Endolymph Membranous labyrinth KEY Membranous labyrinth Bony labyrinth A section through one of the semicircular canals, showing the relationship between the bony and membranous labyrinths, and the locations of perilymph and endolymph. © 2013 Pearson Education, Inc.
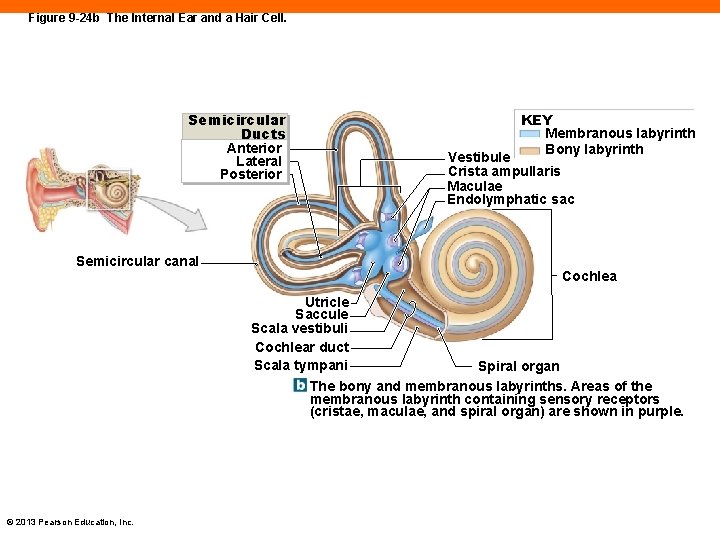
Figure 9 -24 b The Internal Ear and a Hair Cell. KEY Membranous labyrinth Bony labyrinth Semicircular Ducts Anterior Lateral Posterior Vestibule Crista ampullaris Maculae Endolymphatic sac Semicircular canal Cochlea Utricle Saccule Scala vestibuli Cochlear duct Scala tympani Spiral organ The bony and membranous labyrinths. Areas of the membranous labyrinth containing sensory receptors (cristae, maculae, and spiral organ) are shown in purple. © 2013 Pearson Education, Inc.
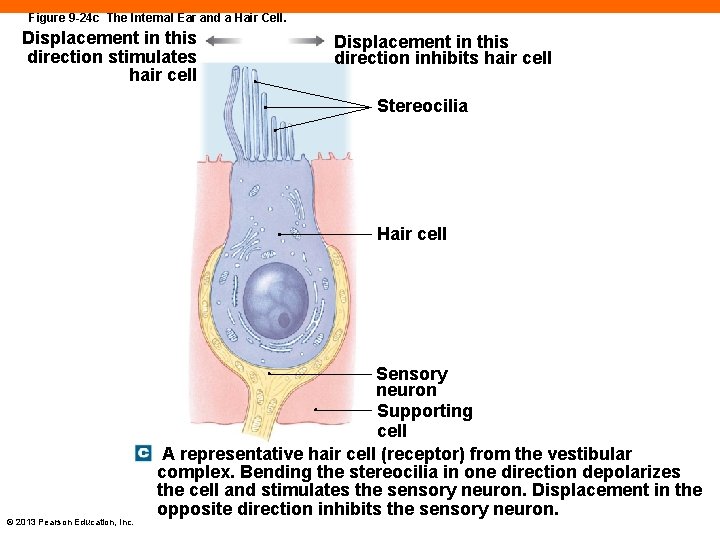
Figure 9 -24 c The Internal Ear and a Hair Cell. Displacement in this direction stimulates hair cell Displacement in this direction inhibits hair cell Stereocilia Hair cell © 2013 Pearson Education, Inc. Sensory neuron Supporting cell A representative hair cell (receptor) from the vestibular complex. Bending the stereocilia in one direction depolarizes the cell and stimulates the sensory neuron. Displacement in the opposite direction inhibits the sensory neuron.

Equilibrium (9 -7) • Dynamic equilibrium • Maintaining balance while in motion • Monitored by semicircular ducts • Static equilibrium • Maintaining balance and posture while motionless • Monitored by saccule and utricle © 2013 Pearson Education, Inc.

The Semicircular Ducts (9 -7) • Three ducts 1. Anterior 2. Posterior 3. Lateral • Organized in three planes 1. Transverse 2. Frontal 3. Sagittal © 2013 Pearson Education, Inc.

The Semicircular Ducts (9 -7) • Each contains the ampulla, which contains the sensory receptors • The crista ampullaris contains hair cells that are embedded in gelatinous structure called the cupula • When head rotates, endolymph pushes against the cristae and activates hair cells © 2013 Pearson Education, Inc.

The Vestibule (9 -7) • Saccule receptors • Respond to gravity and linear acceleration • Utricle receptors • Respond to horizontal acceleration • Hair cells clustered in maculae • Project into gelatinous membrane with otoliths • Gravity pulls on otoliths, pulling on hair cells © 2013 Pearson Education, Inc.
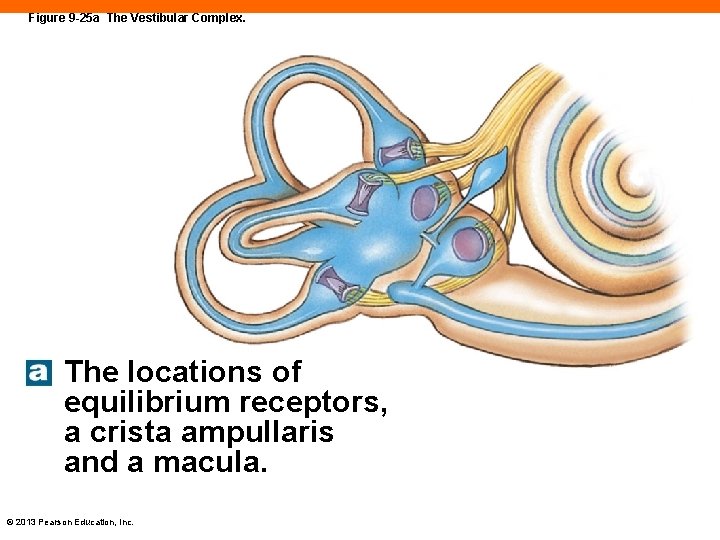
Figure 9 -25 a The Vestibular Complex. The locations of equilibrium receptors, a crista ampullaris and a macula. © 2013 Pearson Education, Inc.
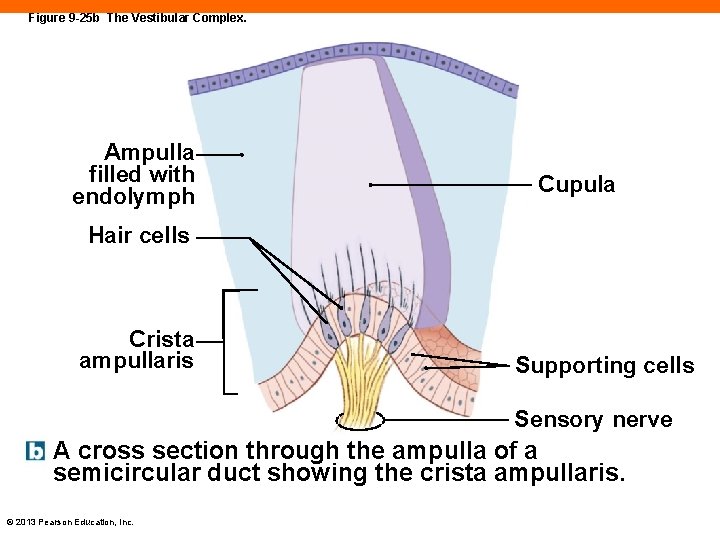
Figure 9 -25 b The Vestibular Complex. Ampulla filled with endolymph Cupula Hair cells Crista ampullaris Supporting cells Sensory nerve A cross section through the ampulla of a semicircular duct showing the crista ampullaris. © 2013 Pearson Education, Inc.
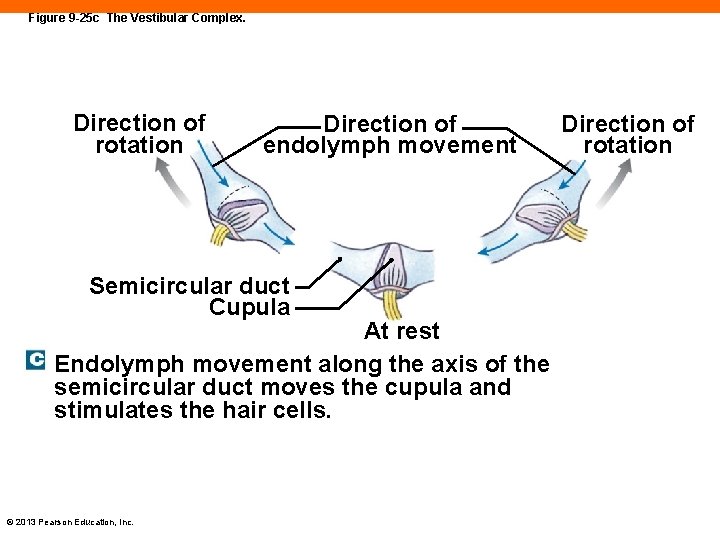
Figure 9 -25 c The Vestibular Complex. Direction of rotation Direction of endolymph movement Semicircular duct Cupula At rest Endolymph movement along the axis of the semicircular duct moves the cupula and stimulates the hair cells. © 2013 Pearson Education, Inc. Direction of rotation
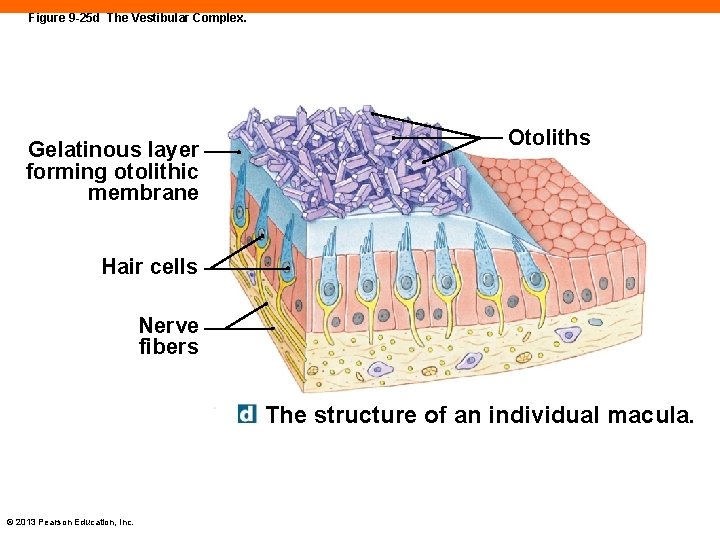
Figure 9 -25 d The Vestibular Complex. Gelatinous layer forming otolithic membrane Otoliths Hair cells Nerve fibers The structure of an individual macula. © 2013 Pearson Education, Inc.
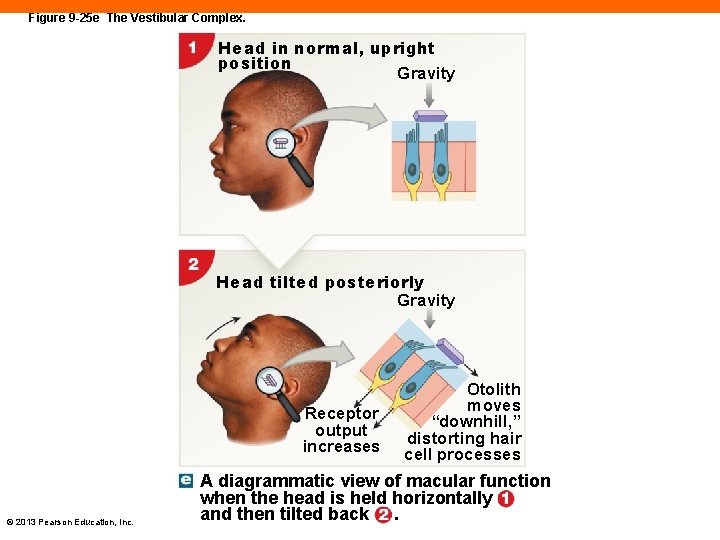
Figure 9 -25 e The Vestibular Complex. Head in normal, upright position Gravity Head tilted posteriorly Gravity Receptor output increases © 2013 Pearson Education, Inc. Otolith moves “downhill, ” distorting hair cell processes A diagrammatic view of macular function when the head is held horizontally and then tilted back.

Pathways for Equilibrium Sensations (9 -7) • Hair cells of vestibule and semicircular ducts • Synapse with neurons of vestibular branch of N VIII • These synapse with neurons in the vestibular nuclei of the pons and medulla oblongata • Information is relayed to: • Cerebellum • Cerebral cortex • Motor nuclei in brain stem and spinal cord PLAY ANIMATION The © 2013 Pearson Education, Inc. Ear: Balance

Hearing (9 -7) • Vibrations of sound waves determine stimulus • Tympanic membrane vibrates the ossicles • Pressure pulses travel through perilymph of cochlea • Pitch (frequency) determined by which part of cochlear duct is stimulated • Volume (intensity) determined by how many hair cells are activated at that site © 2013 Pearson Education, Inc.

The Cochlear Duct (9 -7) • Sectional view shows three chambers 1. Scala vestibuli (the vestibular duct) 2. Scala media (the cochlear duct) 3. Scala tympani (the tympanic duct) • Scala vestibuli and scala tympani are filled with perilymph and are a continuous chamber © 2013 Pearson Education, Inc.

The Spiral Organ of Corti (9 -7) • Located in cochlear duct on basilar membrane • Hair cell stereocilia project into tectorial membrane, attached to wall of cochlear duct • Waves strike basilar membrane, moving it up and down • Hair cells are pushed against tectorial membrane, bending stereocilia © 2013 Pearson Education, Inc.
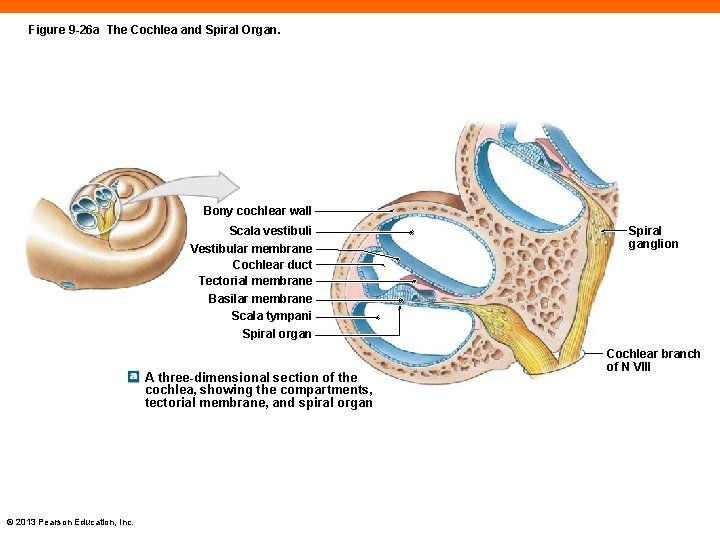
Figure 9 -26 a The Cochlea and Spiral Organ. Bony cochlear wall Scala vestibuli Vestibular membrane Cochlear duct Tectorial membrane Basilar membrane Scala tympani Spiral organ A three-dimensional section of the cochlea, showing the compartments, tectorial membrane, and spiral organ © 2013 Pearson Education, Inc. Spiral ganglion Cochlear branch of N VIII
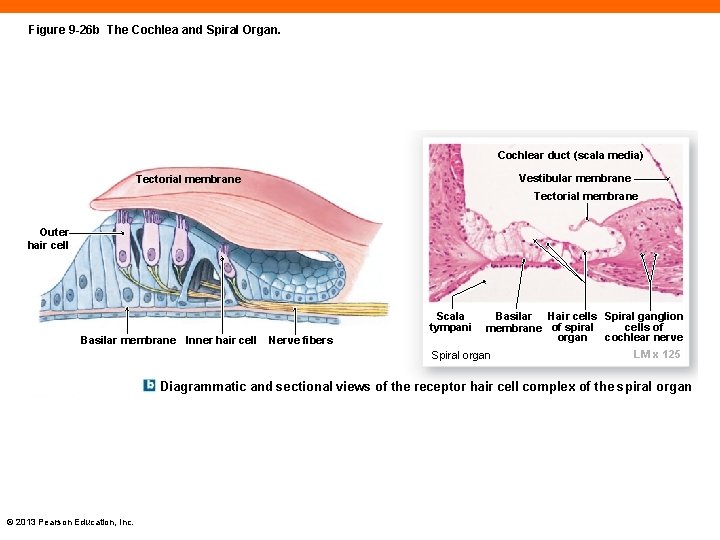
Figure 9 -26 b The Cochlea and Spiral Organ. Cochlear duct (scala media) Vestibular membrane Tectorial membrane Outer hair cell Scala tympani Basilar membrane Inner hair cell Nerve fibers Basilar Hair cells Spiral ganglion cells of membrane of spiral organ cochlear nerve Spiral organ LM x 125 Diagrammatic and sectional views of the receptor hair cell complex of the spiral organ © 2013 Pearson Education, Inc.
Six Steps of Hearing (9 -7) 1. Sound waves strike tympanic membrane 2. Tympanic membrane vibrates auditory ossicles 3. Vibration of stapes applies pressure to perilymph 4. Pressure distorts basilar membrane 5. Movement of basilar membrane distorts hair cells against tectorial membrane, altering neurotransmitter release 6. Impulses travel to CNS through N VIII © 2013 Pearson Education, Inc.
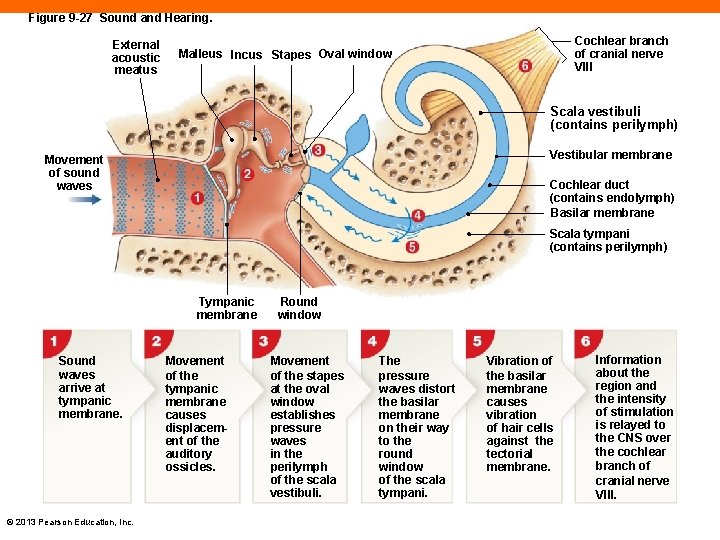
Figure 9 -27 Sound and Hearing. External acoustic meatus Cochlear branch of cranial nerve VIII Malleus Incus Stapes Oval window Scala vestibuli (contains perilymph) Vestibular membrane Movement of sound waves Cochlear duct (contains endolymph) Basilar membrane Scala tympani (contains perilymph) Tympanic membrane Sound waves arrive at tympanic membrane. © 2013 Pearson Education, Inc. Movement of the tympanic membrane causes displacement of the auditory ossicles. Round window Movement of the stapes at the oval window establishes pressure waves in the perilymph of the scala vestibuli. The pressure waves distort the basilar membrane on their way to the round window of the scala tympani. Vibration of the basilar membrane causes vibration of hair cells against the tectorial membrane. Information about the region and the intensity of stimulation is relayed to the CNS over the cochlear branch of cranial nerve VIII.

Auditory Pathways (9 -7) • Cochlear branch of vestibulocochlear nerve (N VIII) axons arise from spiral ganglion • To cochlear nuclei of medulla oblongata • To inferior colliculi of midbrain • To nuclei in thalamus • To auditory cortex of temporal lobes © 2013 Pearson Education, Inc.
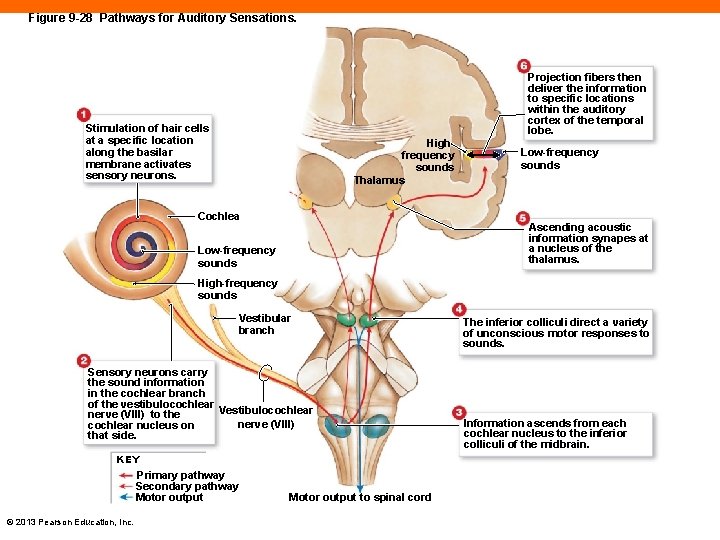
Figure 9 -28 Pathways for Auditory Sensations. Projection fibers then deliver the information to specific locations within the auditory cortex of the temporal lobe. Stimulation of hair cells at a specific location along the basilar membrane activates sensory neurons. Highfrequency sounds Thalamus Cochlea Low-frequency sounds Ascending acoustic information synapes at a nucleus of the thalamus. Low-frequency sounds High-frequency sounds Vestibular branch Sensory neurons carry the sound information in the cochlear branch of the vestibulocochlear Vestibulocochlear nerve (VIII) to the nerve (VIII) cochlear nucleus on that side. KEY Primary pathway Secondary pathway Motor output © 2013 Pearson Education, Inc. Motor output to spinal cord The inferior colliculi direct a variety of unconscious motor responses to sounds. Information ascends from each cochlear nucleus to the inferior colliculi of the midbrain.

Checkpoint (9 -7) 16. If the round window were not able to bulge out with increased pressure in the perilymph, how would sound perception be affected? 17. How would the loss of stereocilia from the hair cells of the spiral organ affect hearing? © 2013 Pearson Education, Inc.

Aging and the Special Senses (9 -8) • Olfaction and gustation decrease with decrease in number and sensitivity of receptors • Hearing decreases with age due to loss of elasticity of tympanic membrane © 2013 Pearson Education, Inc.

Checkpoint (9 -8) 18. How can a given food be both too spicy for a child and too bland for an elderly individual? 19. Explain why we have an increasingly difficult time seeing close-up objects as we age. © 2013 Pearson Education, Inc.
- Slides: 121