Power Point Lecture Slides prepared by Barbara Heard

Power. Point® Lecture Slides prepared by Barbara Heard, Atlantic Cape Community Ninth Edition College Human Anatomy & Physiology CHAPTER 17 Blood © Annie Leibovitz/Contact Press Images © 2013 Pearson Education, Inc.

Blood Composition • Blood – Fluid connective tissue – Plasma – non-living fluid matrix – Formed elements – living blood "cells" suspended in plasma • Erythrocytes (red blood cells, or RBCs) • Leukocytes (white blood cells, or WBCs) • Platelets © 2013 Pearson Education, Inc.
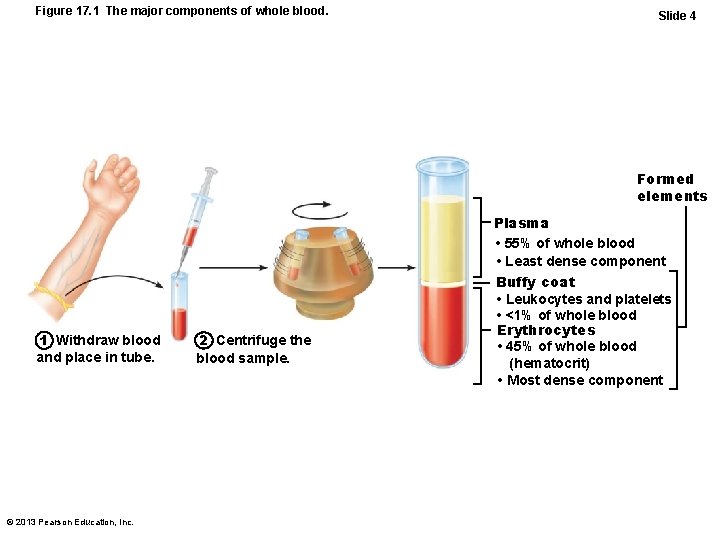
Figure 17. 1 The major components of whole blood. Slide 4 Formed elements 1 Withdraw blood and place in tube. © 2013 Pearson Education, Inc. 2 Centrifuge the blood sample. Plasma • 55% of whole blood • Least dense component Buffy coat • Leukocytes and platelets • <1% of whole blood Erythrocytes • 45% of whole blood (hematocrit) • Most dense component

Functions of Blood • Functions include – Distributing food and oxygen, carries waste to lungs and kidneys, carries hormones – Regulating body temperature, normal p. H and fluid levels – Protection from blood loss (clotting) and prevents infection (WBC) © 2013 Pearson Education, Inc.

Blood Plasma • 90% water • Over 100 dissolved solutes – Nutrients, gases, hormones, wastes, proteins, inorganic ions – Plasma proteins most abundant solutes • Remain in blood; not taken up by cells • Proteins produced mostly by liver • 60% albumin; 36% globulins; 4% fibrinogen © 2013 Pearson Education, Inc.

Formed Elements RBC WBC and Platelets • Most blood cells originate in bone marrow and do not divide © 2013 Pearson Education, Inc.
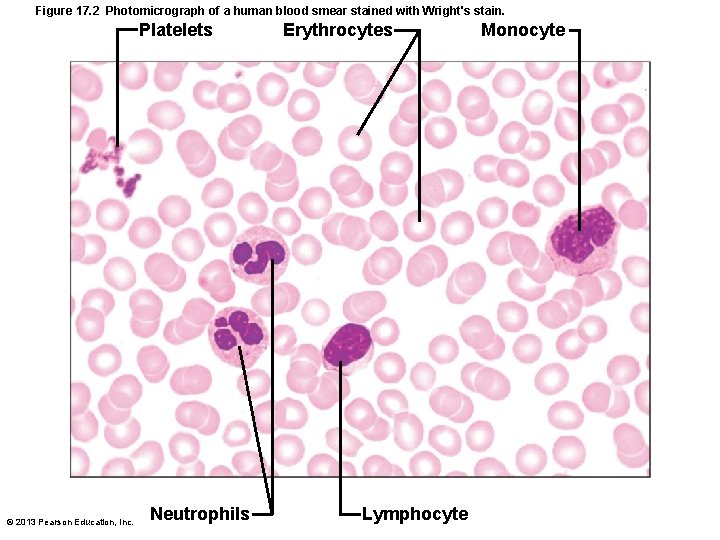
Figure 17. 2 Photomicrograph of a human blood smear stained with Wright's stain. Platelets © 2013 Pearson Education, Inc. Neutrophils Erythrocytes Lymphocyte Monocyte

Erythrocytes • Structural characteristics contribute to gas transport – Biconcave shape—huge surface area relative to volume – >97% hemoglobin (not counting water) – No mitochondria; ATP production anaerobic; do not consume O 2 they transport © 2013 Pearson Education, Inc.

Hematopoiesis • Blood cell formation in red bone marrow – Composed of reticular connective tissue and blood sinusoids • In adult, found in axial skeleton, girdles, and proximal epiphyses of humerus and femur © 2013 Pearson Education, Inc.
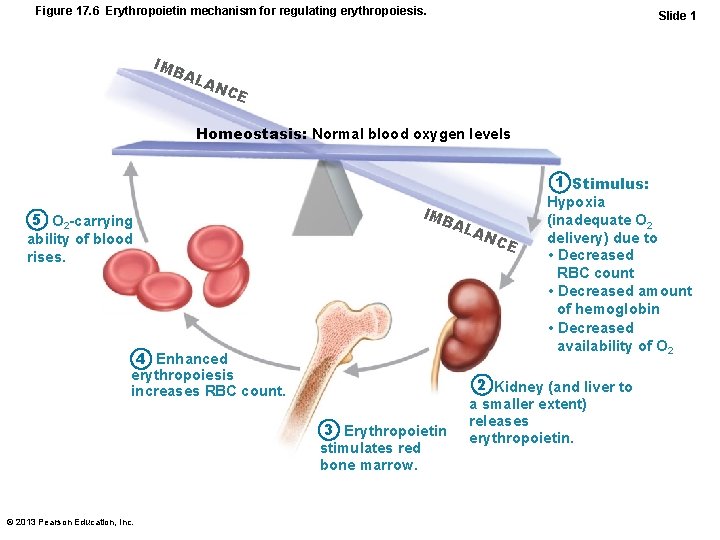
Figure 17. 6 Erythropoietin mechanism for regulating erythropoiesis. IMB AL Slide 1 AN CE Homeostasis: Normal blood oxygen levels 5 O 2 -carrying ability of blood rises. IMB AL 4 Enhanced erythropoiesis increases RBC count. 3 Erythropoietin stimulates red bone marrow. © 2013 Pearson Education, Inc. AN C E 1 Stimulus: Hypoxia (inadequate O 2 delivery) due to • Decreased RBC count • Decreased amount of hemoglobin • Decreased availability of O 2 2 Kidney (and liver to a smaller extent) releases erythropoietin.

Fate and Destruction of Erythrocytes • Life span: 100– 120 days – No protein synthesis, growth, division • Old RBCs become fragile; Hb begins to degenerate • Get trapped in smaller circulatory channels especially in spleen • Macrophages engulf dying RBCs in spleen © 2013 Pearson Education, Inc.

Fate and Destruction of Erythrocytes • Heme and globin are separated – Iron salvaged for reuse – Heme degraded to yellow pigment bilirubin – Liver secretes bilirubin (in bile) into intestines • Degraded to pigment urobilinogen • Pigment leaves body in feces as stercobilin – Globin metabolized into amino acids • Released into circulation © 2013 Pearson Education, Inc.
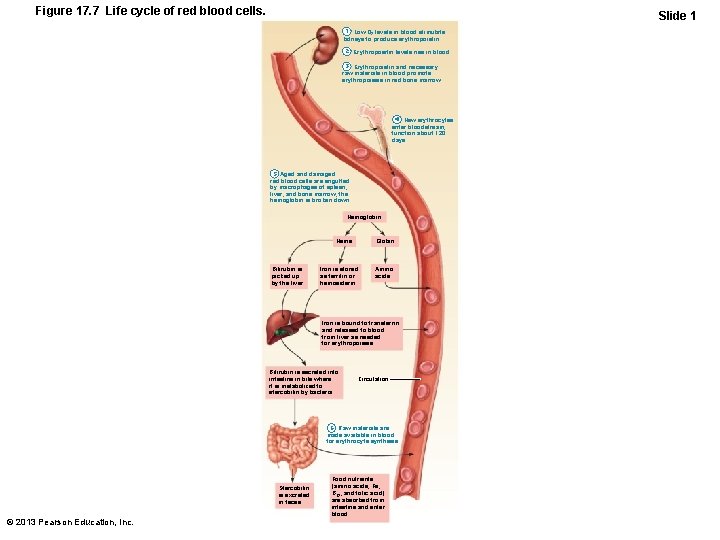
Figure 17. 7 Life cycle of red blood cells. Slide 1 1 Low O 2 levels in blood stimulate kidneys to produce erythropoietin. 2 Erythropoietin levels rise in blood. 3 Erythropoietin and necessary raw materials in blood promote erythropoiesis in red bone marrow. 4 New erythrocytes enter bloodstream; function about 120 days. 5 Aged and damaged red blood cells are engulfed by macrophages of spleen, liver, and bone marrow; the hemoglobin is broken down. Hemoglobin Heme Bilirubin is picked up by the liver. Globin Iron is stored as ferritin or hemosiderin. Amino acids Iron is bound to transferrin and released to blood from liver as needed for erythropoiesis. Bilirubin is secreted into intestine in bile where it is metabolized to stercobilin by bacteria. Circulation 6 Raw materials are made available in blood for erythrocyte synthesis. Stercobilin is excreted in feces. © 2013 Pearson Education, Inc. Food nutrients (amino acids, Fe, B 12, and folic acid) are absorbed from intestine and enter blood.

Erythrocyte Disorders • Anemia – Blood has abnormally low O 2 -carrying capacity – Sign rather than disease itself – Blood O 2 levels cannot support normal metabolism – Accompanied by fatigue, pallor, shortness of breath, and chills © 2013 Pearson Education, Inc.

Causes of Anemia: Blood Loss • Hemorrhagic anemia – Blood loss rapid (e. g. , stab wound) – Treated by blood replacement • Chronic hemorrhagic anemia – Slight but persistent blood loss • Hemorrhoids, bleeding ulcer – Primary problem treated © 2013 Pearson Education, Inc.

Causes of Anemia: Low RBC Production • Iron-deficiency anemia – Caused by hemorrhagic anemia, low iron intake, or impaired absorption – Microcytic, hypochromic RBCs – Iron supplements to treat © 2013 Pearson Education, Inc.

Causes of Anemia: Low RBC Production • Pernicious anemia – Autoimmune disease - destroys stomach mucosa – Lack of intrinsic factor needed to absorb B 12 • Deficiency of vitamin B 12 – RBCs cannot divide macrocytes – Treated with B 12 injections or nasal gel – Also caused by low dietary B 12 (vegetarians) © 2013 Pearson Education, Inc.
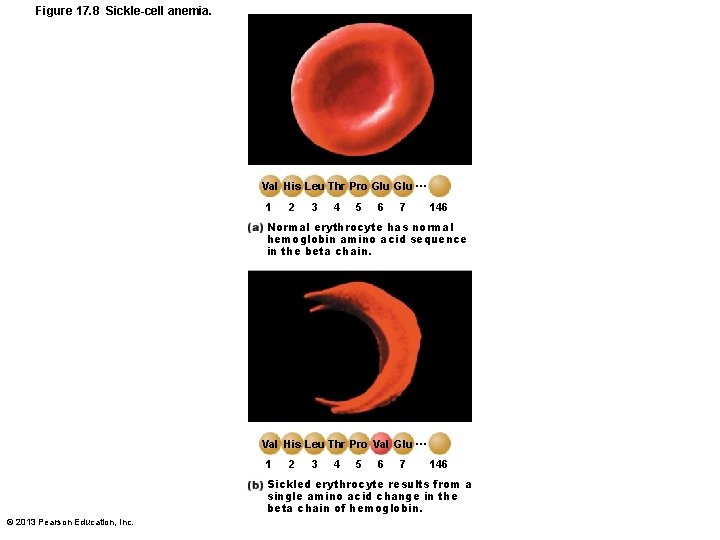
Figure 17. 8 Sickle-cell anemia. Val His Leu Thr Pro Glu … 1 2 3 4 5 6 7 146 Normal erythrocyte has normal hemoglobin amino acid sequence in the beta chain. Val His Leu Thr Pro Val Glu … 1 2 3 4 5 6 7 146 Sickled erythrocyte results from a single amino acid change in the beta chain of hemoglobin. © 2013 Pearson Education, Inc.

Leukocytes • Function in defense against disease – Can leave capillaries via diapedesis – Move through tissue spaces by ameboid motion and positive chemotaxis © 2013 Pearson Education, Inc.

Lymphocytes • Two types – T lymphocytes (T cells) act against virusinfected cells and tumor cells – B lymphocytes (B cells) give rise to plasma cells, which produce antibodies © 2013 Pearson Education, Inc.

Leukemia • Cancerous leukocytes fill red bone marrow – Other lines crowded out anemia; bleeding • Immature nonfunctional WBCs in bloodstream • Death from internal hemorrhage; overwhelming infections • Treatments – Irradiation, antileukemic drugs; stem cell transplants © 2013 Pearson Education, Inc.

Hemostasis • Fast series of reactions for stoppage of bleeding • Requires clotting factors, and substances released by platelets and injured tissues • Three steps 1. vasoconstriction 2. Platelet plug formation 3. Coagulation (blood clotting) © 2013 Pearson Education, Inc.
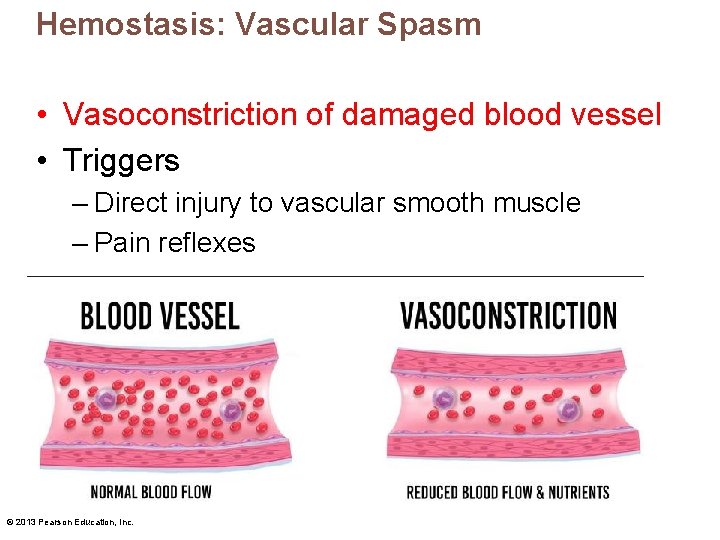
Hemostasis: Vascular Spasm • Vasoconstriction of damaged blood vessel • Triggers – Direct injury to vascular smooth muscle – Pain reflexes © 2013 Pearson Education, Inc.

Hemostasis: Platelet Plug Formation • Positive feedback cycle • Damaged endothelium exposes collagen fibers – Platelets stick to collagen fibers via plasma protein – Swell, become spiked and sticky, and release chemical messengers • ADP causes more platelets to stick and release their contents © 2013 Pearson Education, Inc.

Hemostasis: Coagulation • Reinforces platelet plug with fibrin threads • Blood transformed from liquid to gel • Series of reactions using clotting factors (procoagulants) – Vitamin K needed to synthesize 4 of them © 2013 Pearson Education, Inc.
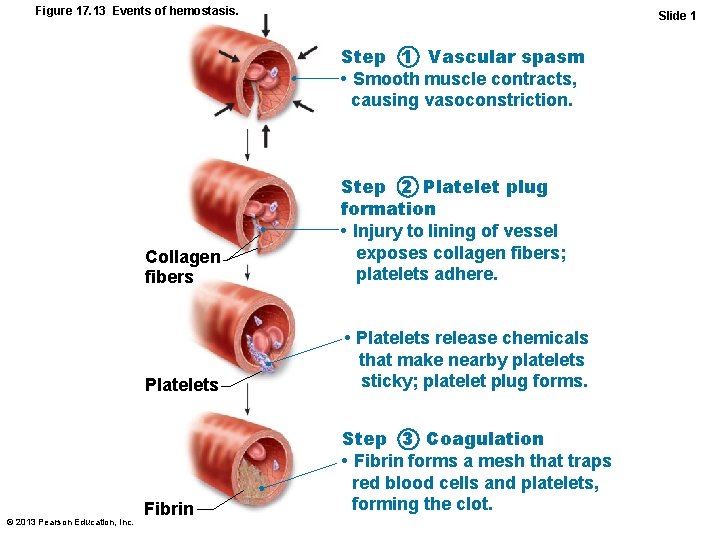
Figure 17. 13 Events of hemostasis. Slide 1 Step 1 Vascular spasm • Smooth muscle contracts, causing vasoconstriction. © 2013 Pearson Education, Inc. Collagen fibers Step 2 Platelet plug formation • Injury to lining of vessel exposes collagen fibers; platelets adhere. Platelets • Platelets release chemicals that make nearby platelets sticky; platelet plug forms. Fibrin Step 3 Coagulation • Fibrin forms a mesh that traps red blood cells and platelets, forming the clot.
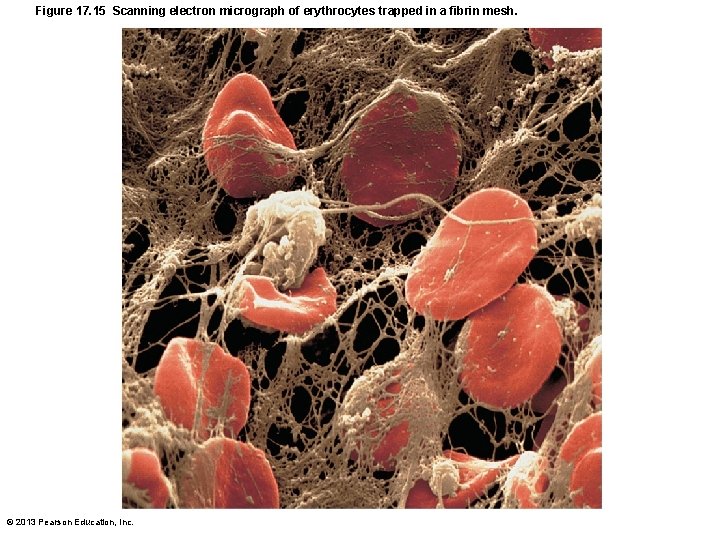
Figure 17. 15 Scanning electron micrograph of erythrocytes trapped in a fibrin mesh. © 2013 Pearson Education, Inc.

Clot Retraction • Stabilizes clot • Actin and myosin in platelets contract within 30– 60 minutes • Contraction pulls on fibrin strands, squeezing serum from clot • Draws ruptured blood vessel edges together © 2013 Pearson Education, Inc.

https: //www. youtube. com/watch? v=P 7 Kjyx. N_m 4 https: //www. youtube. com/watch? v=5 tj 4 LTU 9 Nec https: //www. youtube. com/watch? v=Rs. KZWqs. Upw&list=PL 1 A 106 F 4 D 05105663 © 2013 Pearson Education, Inc.
- Slides: 29