PostTraumatic Seizures and Epilepsy in the Developing Brain

Post-Traumatic Seizures and Epilepsy in the Developing Brain Michael J. Esser MD, Ph. D, FRCPC Pediatric Neurologist Alberta Children’s Hospital University of Calgary

Disclosure • Faculty/Presenter Disclosure; Michael J. Esser • Grants/Research Support: CIHR, CIMVHR, ACHF, Brain Canada

Objectives • Ascertain the epidemiology of pediatric PTS and PTE • Consider the evidence for the “need” of seizure prophylaxis in pediatric TBI • Consider the balance of seizure treatment versus drug (neuro)toxicity

Central question • Should we treat children with TBI o Is there a need? o Balance the developmental impact of seizures/epilepsy with those of seizure medications


Numbers and what they mean • PTS and PTE – measures of Incidence, epidemiology, outcomes, treatment o Incidence is dependent on “common” classification/terminology • No accepted nomenclature of seizure types and blurring of time stratification o Epidemiology is dependent on accurate capture and categorization. o Outcomes – affected by classification and treatment • Guidelines are based on adults and incomplete data o Treatment – kids are not little adults, and one-size doesn’t fit all

TBI • Leading cause of morbidity and mortality in Pediatric age group o ~>50% of childhood deaths (Mazzola and Adelson, 2002) • 1. 4 million TBIs in US, 626, 000 are in children up to age 19 (Aitken et al. , 2009)
Post-Traumatic Seizures (PTS) • Dependent on several factors o Nature of injury (NAT greatest), severe TBI, age (<2 highest), o prolonged LOC, prolonged post-traumatic amnesia, intracranial hemorrhage, depressed or open skull fracture • Aggregate incidence** of PTS is from 1. 6 - 42. 5% (1. 6 -9. 3) (Arnt et al. , 2015; Tanaka and Litofsky, 2016)) o Mild-TBI (1 -5%), moderate (10 -20%), severe (20 -42. 5%) (Tanaka and Litofsky, 2016) o NAT (33 -73%) o Recurrence risk within the first week – 35 -65% (Arnt et al. , 2015) • Most are focal (54 -80%) • Post-traumatic status epilepticus - 3 -11% o Younger children > older children o Clinical and subclinical PTSE associated with increased LOS and lower global outcome scores (Arnt et al. , 2013)

Seizure characteristics • Seizure within the first 7 days • 25% PTS <60 min, 50% PTS < 7 days, o Most are 2 o GTC – 60 -85% (Pagni and Zenga, 2005) • Focal symptoms related to region affected • In pediatrics, hypomotor is more prevalent in severe TBI (Park and Chugani, 2015) - ? Due to large number of NAT patients o The later in onset from injury the more likely it will be focal • >50% o ~ 18. 4 % PICU TBI will progress to status epilepticus (Tanaka and Litofsky, 2016) o Post traumatic epilepsy • 17 -33% with PTS will develop PTE

Evaluation • Diagnosis o Clinical • Limited as a significant proportion of PTS are subclinical o Neuroimaging • Not prognostic, but can help with risk stratification for PTS • CT – not associated with risk of EPTS, but SDH found in more kids with EPTS (Liesemer et al. , 2011) • MRI – early changes with DTI or SWI, later with structural (Gupta et al. , 2005; Messori et al. , 2005) • Can help distinguish etiology and suggest treatment – NSx, seizure drugs o Biomarkers • Inconclusive as of yet o EEG • abnormalities do not predict risk of PTE or type of seizure • Increase yield and ability to detect events especially in younger children at risk for non-convulsive seizures/status epilepticus • Identification of other abnormal EEG patterns (BS, non-reactive, abn sleep)

• • 87 pediatric (1 month -18 years), two centers, all severities Prospective study with c. EEG (minimum 24 hours) • 37/87 (42. 5%) had seizures, o 14/87[37] (16. 1%[37. 8%]) had subclinical seizures o 6/87 [37] (6. 9% [16. 2%]) had subclinical seizures only, • 16/87 [37] (18. 4% [43. 2%]) had SE, o 12/87[16] (13. 8%[75%]) had subclincal SE • Treatment - was not related to seizure incidence ( BDZ, fos. Pheny/Pheny, Phenobarb, Topamax, Keppra) • Outcomes - greater hosp-LOS (SE, subclinical-SE) and lower KOSHI score (subclinical seizures and subclinical SE)
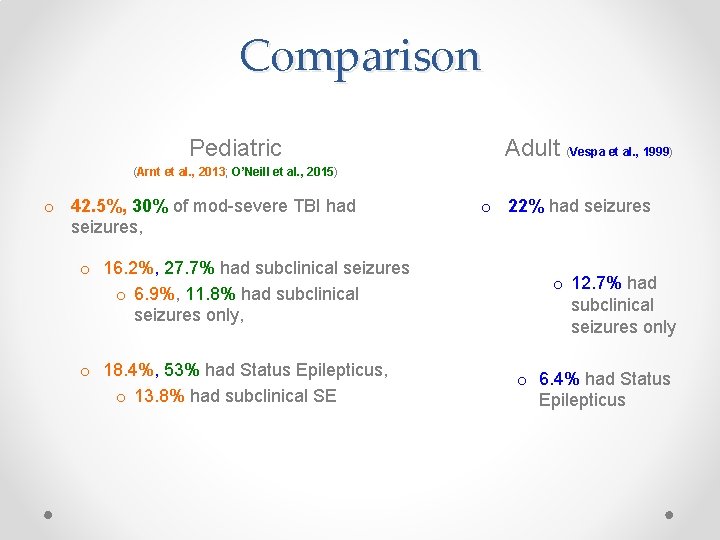
Comparison Pediatric Adult (Vespa et al. , 1999) (Arnt et al. , 2013; O’Neill et al. , 2015) o 42. 5%, 30% of mod-severe TBI had seizures, o 16. 2%, 27. 7% had subclinical seizures o 6. 9%, 11. 8% had subclinical seizures only, o 18. 4%, 53% had Status Epilepticus, o 13. 8% had subclinical SE o 22% had seizures o 12. 7% had subclinical seizures only o 6. 4% had Status Epilepticus

Post-Traumatic Epilepsy • 5% of all epilepsy and 20% of structural epilepsies are due to PTE et al. , 1999; Lamar et al. , 2014) • General prevalence of PTE in children is 0. 2 to 16. 8% o 17 -33% with PTS will develop PTE o unclear if there is a difference between early or late PTS and risk for PTE o Risk factors are similar to those for PTS • Cumulative incidence (per 100 persons)** (Annegars, 1996; Englander, 2003; Lamar et al. , 2014) o Mild 0. 7 – 4. 4 o Moderate 1. 2 – 7. 6 o Severe 4. 3 – 17 • PTE onset o 40% < 6 months; 50 -70% < 1 year; 80% < 2 years o May begin as late as 15 years after (Raymont et al. , 2010; Lamar et al. , 2014) • Treatment of PTS does NOT seem to affect rate of PTE**** (Lowenstein

Treatment in Kids • “Strength of recommendations: WEAK” • “Quality of Evidence: LOW” • “Recommendation” for prophylactic treatment when high risk of EPTS (Adelson et al. , 2003, Kochanek et al. , 2012)
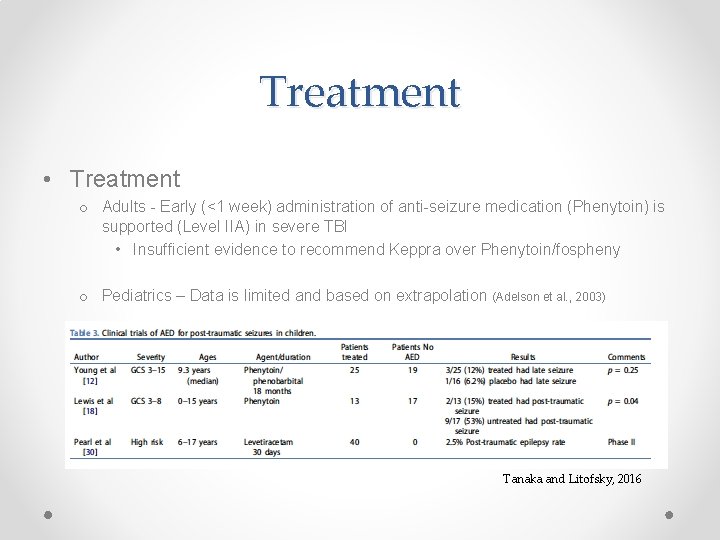
Treatment • Treatment o Adults - Early (<1 week) administration of anti-seizure medication (Phenytoin) is supported (Level IIA) in severe TBI • Insufficient evidence to recommend Keppra over Phenytoin/fospheny o Pediatrics – Data is limited and based on extrapolation (Adelson et al. , 2003) Tanaka and Litofsky, 2016

Treatment in Kids • • “Strength of recommendations: WEAK” “Quality of Evidence: LOW” • “Recommendation” for prophylactic treatment when high risk of EPTS (Adelson et al. , 2003, Kochanek et al. , 2012) • Goal is to minimise secondary injury o Paradox of PTS – product of the injury and contributor to secondary physiological, neurochemical and metabolic insult o Reduce hypoxia, hypercarbia, systemic hypotension, increased metabolic stress, raised ICP

What about kids………. Balance the developmental impact of drug neurotoxicity against harm of recurrent seizures and epilepsy

PTE and epileptogenesis Hunt et al. , 2012 • Epileptogenesis – multi-layered process from primary injury --- secondary injury -- repair mechanisms. • Effect of structural lesions – site and mode dependent – hippocampal atrophy, neocortical gliosis, shear injury at gray-white junction • Lead to hyperexcitability, hypersynchronicity, and network re-organisation • Process not well understood

Developmental Toxicity • Seizures and epilepsy o SE has high morbidity and mortality • Seizure medications o ASDs interact with ion channels, metabolic enzymes, neurotransmitter receptor systems and transporters o Prolonged SE becomes refractory (Mayer et al. , 2002) o Many hypothesis about consequences • GABA and Chloride • Dentate gyrus cell loss • Mossy fiber sprouting • [Ca]i accumulation • Adenosine receptor • Cortical dysplasia o Interfere with neuronal migration, differentiation, and myelination, as well as impair plasticity and cause cell death o Phenobarb, Phenytoin, VPA, Diazepam, Midazolam, Clonazepam – induce apoptotic neurodegeneration o ? ? Topiramate, Levetiracetam o Requires a knowledge of the role of ontogeny in the disposition and action of the drugs (Kaindl et al. , 2006)
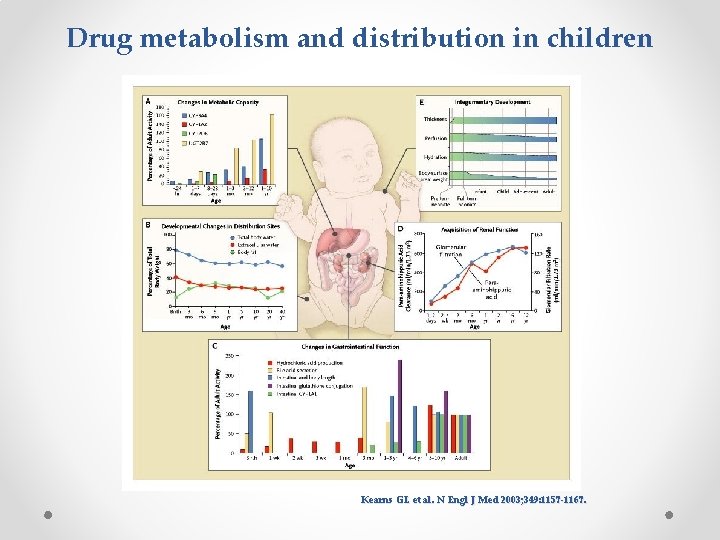
Drug metabolism and distribution in children Kearns GL et al. N Engl J Med 2003; 349: 1157 -1167.
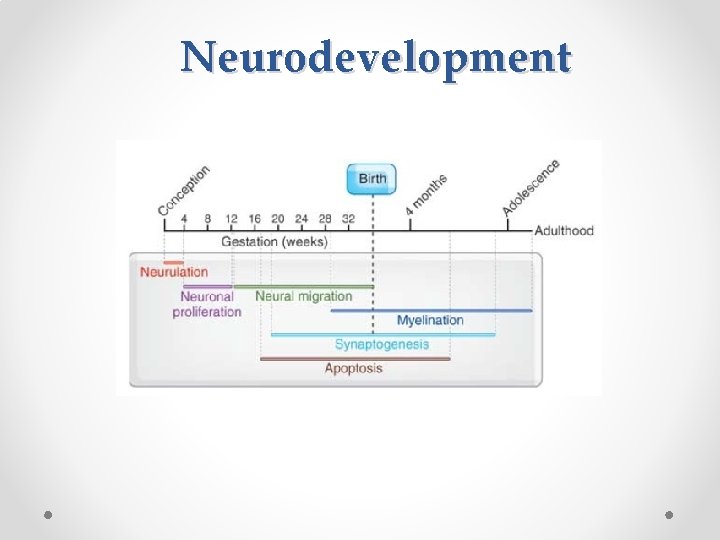
Neurodevelopment

Summary • Risk of: PTS - 30 -40%, of NCS - 15 -30%, of SE is ~ 20% • Risk of PTE - True incidence and treatment effect/need is unclear • Consistent Risk factors • NAT, severe TBI, age < 2, • SDH or parenchymal haemorrhage, contusions, length of PTA/LOC, penetrating injury, depressed skull fracture, • “ future research should be randomized and prospective, and should intervene during pre-trauma center care with initiation of continuous EEG monitoring as soon as possible” (Liesemer et al. , 2011) • Treatment - ASD are effective at preventing early seizures and should be used in those at risk o Future trials to determine if Keppra is main drug and the duration

Acknowledgements • ACH-TBI program o Dr. K. Barlow, Dr. L. Burkholder, Dr. V. Gnanakumar, Lisa Bodell • Lab o Dr. T. Shutt, Dr. Q. Pittman, Dr. R. Mychasiuk, Sydney Candy, Alyson Farran, Erik Fraunberger, Harleen Hehar, Alon Gilad • Funding o CIHR, ACHF, ACHRI, CIMVHR

END

Select References • Pagni CA, Zenga F (2005) Posttraumatic epilepsy with special emphasis on prophylaxis and prevention. Acta Neurochir Suppl. 2005; 93: 27. • Annegers JF et al. , 1998. A population-based study of seizures after traumatic brain injuries. NEJM 338(1): 20. • Arrango et al. , 2012. Post-traumatic seizures in children with sever TBII. Child Nerv Syst 28: 1925. • Englander et al. , 2003. Analyzing risk factors for late posttraumatic seizures: a prospective, multicenter investigation. Arch Phys Med Rehabil. 84(3): 365. • Christensen et al. , 2009. Long-term risk of epilepsy after traumatic brain injury in children and young adults: a population-based cohort study. Lancet. 373(9669): 1105. • Raymont et al. , 2010. Correlates of posttraumatic epilepsy 35 years following combat brain injury. Neurology. 75(3): 224. • Frey LC (2003) Epidemiology of posttraumatic epilepsy: a critical review. Epilepsia. 2003; 44 Suppl 10: 11. • Gallentine WB (2013) Utility of CEEG in children wit acute TBI. J Clin Neurophysiol 30(2): 126. • Kochanek et al. , 2012 – Chapter 17. Antiseizure prophylaxis. Pediatric Crit Care Med 13(1): S 72. • Abend et al. , (2013). Electrographic seizures and status epilepticus in critically ill children and neonates with encephalopathy. Lancet Neurology 12: 1170 -79. • Ostahowski et al. , 2016. Variation in seizure prophylaxis in severe pediatric traumatic brain injury. JNS Pediatrics, June: 1. • Adelson et al. , 2003. Guidelines for the acute medical management of severe TBI in infants, children and adolescents. Ped Crit Care Med 4(3): S 72 -S 75 • Gupta et al. , 2005 Diffusion Tensor Imaging in late post-traumatic epilepsy. Epilepsia 46: 1465. • Messori et al. , 2005. Predicting post-traumatic epilepsy with MRI: prospective longitudinal morphological study in adults. Epilepsia 46: 1472. • Mayer et al. , 2002. Refractory status epilepticus : frequency risk factors and impact on outcome. Ach Neurol 59: 205. • Kaindel et al. , 2006 Seizure meds and the developing brain, Cell Mol Life sci 63: 399. • Kearns et al. , 2003. Developmental Pharmacology – drug disposition, action, and therapy in infants and children. NEJM 349: 1157. • Lowenstein et al. , 1999. Epilepsy after head injury: an overview. Epilepsia 50 (Suppl 2): 4. • Liesemer et al. , 2011 Early psot-traumatic seizures in moderate to severe pediatric traumatic brain injury: rates, risk factors, clinical feature. J neurotrauma 28: 755. . • Oneill et al. , 2015. Incidence of seizures on continuous EEG monitoring following traumatic brain injury in children. JNS Pediatrics 16: 187. • Tanaka and Litofsky, 2016. Anti-epileptic drugs in pediatric brain injury. Expert Reviews Nuerotherapeutics Oct 16(10): 1229.
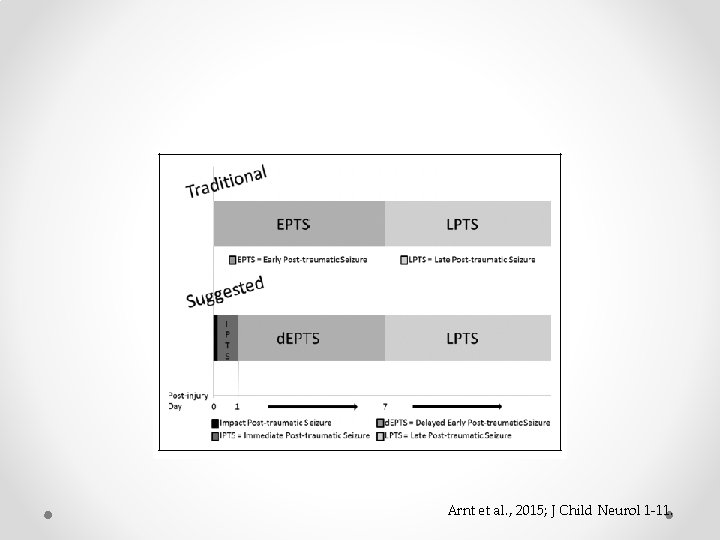
Arnt et al. , 2015; J Child Neurol 1 -11.

• Retrospective analysis – 2002 -2006 • 275 children (0 -15 years) • 34 with seizures (12%) • 23/34 (68%) had EPTS within 12 hours • Risk factors • Pre-hospital hypoxia, age, NAT, severe injury, impact seizure, subdural • Independent risk factors – age <2 (OR 3), GCS <8 (OR 8. 7), NAT (OR 3. 4)
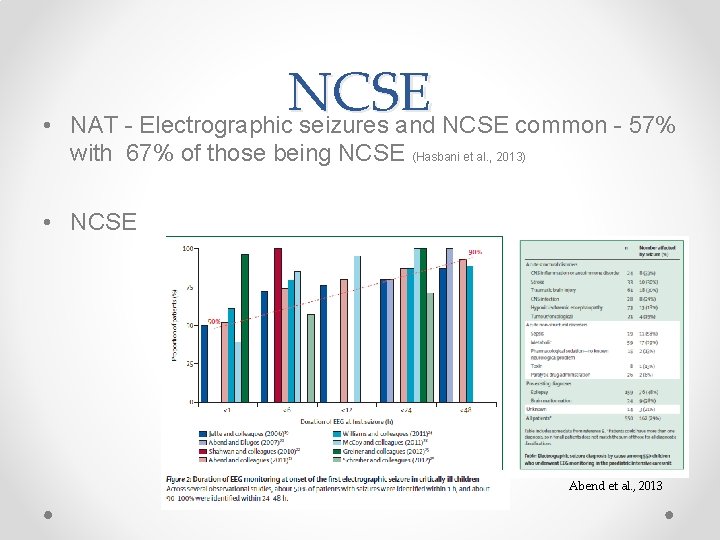
• NCSE NAT - Electrographic seizures and NCSE common - 57% with 67% of those being NCSE (Hasbani et al. , 2013) • NCSE Abend et al. , 2013


However……. • Most data is from: o retrospective studies with heterogeneous data sets o Adults o PTS/PTE - biased by suspicion of seizures o Treatment • based on o adult healthy pharmacology o “whole event” philosophy o on older drugs – phenytoin • Variation in treatment between centres may contribute to in-accurate interpretation of seizure prophylaxis outcomes (Ostahowski et al. , 2016)

• 94 patients (21 -80 years old) with moderate-severe TBI • Prospectively had c. EEG (from admission up to 14 days) • 21/94 (22%) had seizures • 12/94[21] (12. 7% [52%]) had non-convulsive seizures • 6/94 [21] (6. 4% [29%]) had status epilepticus • Seizures occurred despite prophylactic treatment (phenytoin) • Outcomes – all with SE died, no difference in LOS or in GOS between seizure and non-seizure patients

Risk Factors • Ongoing seizures and development of PTE o o o o Injury severity (esp NAT) Age < 2 (or>65) at time of the injury Seizures within the first 7 days Intracranial hemorrhage Brain contusion Penetrating injury (↑ risk by 50%), Blunt injury with contusion or hemorrhage (↑ risk by 30%)
- Slides: 32