POSTPARTUM CARE Postpartum Psychological Adaptations Reva Rubin l

POSTPARTUM CARE


Postpartum Psychological Adaptations Reva Rubin l l Taking in: Mom wants to talk about her experience of labor & birth, preoccupied with her own needs Taking hold: More ready to resume control of her body, baby & taking on mothering role. Needs reassurance if inexperienced. Letting-go: by 5 th week, total abandon to NB Bonding: en face position, engrossement. Encourage through early interaction & breastfeeding (within 1/2 hr of birth is best).

Maternal Responses to Newborn Reva Rubin l l l Touch- progresses from fingertips → palming →cuddling → Voice- high-pitched & babies respond Odor- mom’s respond to baby’s unique smell Eye contact- en face position delay eye ointment & bright lights Nurse role- be able to answer ? About baby

Blues vs Dpression Postpartum/baby blues: transient depression in first few days: weepiness mood swings anorexia difficulty sleeping feeling of letdown Postpartum Depression *If persists past 2 weeks, or worsens Symptoms: very sad feelings hopeless worthless anxiety trouble caring for and bonding with your baby Have trouble sleeping. Not be able to concentrate. Not feel hungry and may lose weight. (But some women feel more hungry and gain weight) Postpartum Psychosis A woman who has postpartum psychosis may feel cut off from her baby. She may see and hear things that aren't there. Any woman who has postpartum depression can have fleeting thoughts of suicide or of harming her baby. But a woman with postpartum psychosis may feel like she has to act on these thoughts.

Endocrine Adaptations l Hormones: drop after delivery of placenta. – h. CG & h. PL gone by 24 hours – Estrogen & progesterone drop within 1 wk – FSH remains low for 12 days, then rises to begin new cycle – Sex is ok once lochia is alba. Menstrual period in 6 -10 wks. – Contraception necessary.

Physiological Adaptations l Uterine involution – @ umbilicus first 24 hours--should feel firm – Decreases 1 finger’s breadth per day – By 10 th day, no longer palpable l l If high (3 or 4 fingers above U) and/or deviated to right, have pt. void Risk for delayed involution: – Multiples, hydramnios, exhaustion, grand multiparity, excessive analgesia l Afterpains l www. youtube. com/watch? v=Eb. It. F_7 KYCc&feature=related


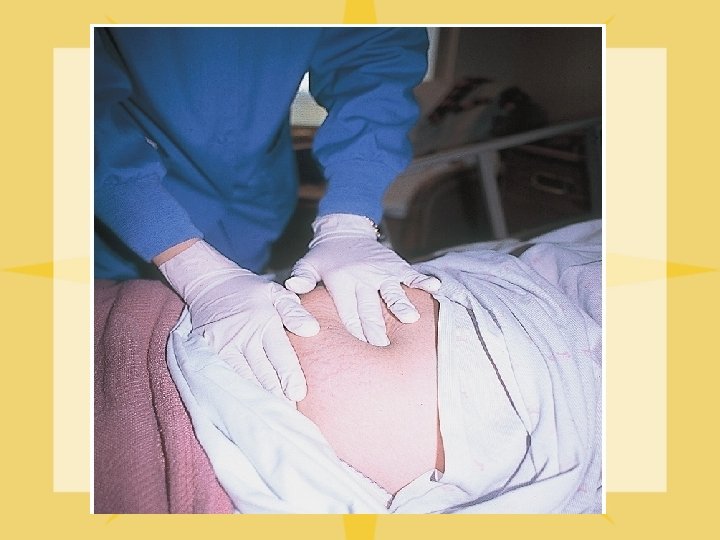
Fundal Assessment l l Every 10 -15 mins in first hour. Supine position Palpate: one hand at base of uterus & other at umbilicus. Press inward and downward and feel for firm globular mass. Assess: – Height (fingers above/below umbilicus) – Position (midline, deviated to right or left) – Consistency: firm, soft, boggy If not firm, massage & should become firm. If still boggy, notify MD/assess for clots, hemorrhage. Administer oxytocin or other oxytocic (methergine, hemabate).

Lochia l Rubra Serosa Alba l If flow increases, woman should rest more l Warning sign: if lochia returns to previous type (alba to serosa, or serosa to rubra) l l

Lochia Assessment l Check q 15 mins in 1 st hour. l Assessment: – Color (rubra, serosa, alba), amount, odor, presence of clots. – Constant trickle of vaginal flow, or soaking pad every 60 minutes is more than average. Can weigh pads--1 gm = 1 ml of blood. l Lochia should not exceed a moderate amount: 4 to 8 partially saturated pads/day

Lochia Assessment l Assessing Amounts: – Scant: peripad has stain less than 1 inch in length after 1 hour – Small: stain less than 4 inches after 1 hour--10 -25 m. L – Moderate: stain less than 6 inches after 1 hour--25 -50 m. L. l Instruct in perineal care: ∆ pad frequently, hand washing, s/s of infection & hemorrhage, no tampons

Cervix & Vagina l Cervix returns to firm, nongravid consistency by about 7 days, but external os remains slitlike or stellate l Vagina involutes in 6 wk period, with return of rugae. – Kegel exercises for pelvic floor muscles.

Perineum l Assessment: turn pt to side in Sim’s position. Lift upper buttock and assess for: – Ecchymosis, hematoma, erythema, edema, intactness, approximation, drainage or bleeding from stitches l Assess for hemorrhoids & document number, appearance & size
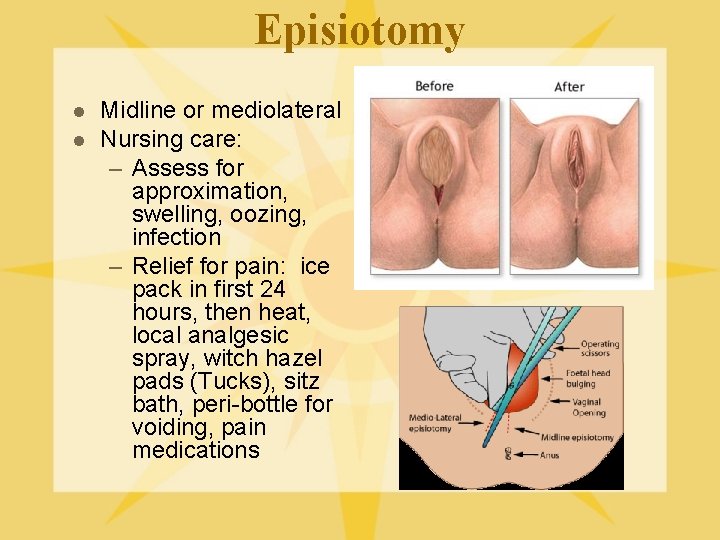
Episiotomy l l Midline or mediolateral Nursing care: – Assess for approximation, swelling, oozing, infection – Relief for pain: ice pack in first 24 hours, then heat, local analgesic spray, witch hazel pads (Tucks), sitz bath, peri-bottle for voiding, pain medications

Other Assessments l Constipation: Give stool softeners as ordered, prune juice, encourage ambulation, adequate fluid intake, fiber in diet. Homan’s sign: assess calves for redness, warmth, pain, swelling. -↑risk of DVT, thrombophlebitis. -Occur in postpartum because: l – Fibrinogin level is elevated – Dilatation of lower extremity veins – Relative inactivity during labor or prolonged time in delivery room stirrups leads to pooling, stasis & clotting of blood in lower extremities.

Thrombophlebitis l Superficial leg vein disease: – S/s: tenderness in portion of vein, local heat & redness, normal temperature or low-grade fever – Tx: local heat, elevate limb, bed rest, analgesia, elastic support hose l Deep Vein Thrombosis (DVT): – S/s: edema of ankle, leg, initial low-grade fever, then high temperature & chills, tenderness & pain, changes in limb color & difference in circumference – Tx: IV heparin, bed rest, elevation of leg, analgesics, warm moist heat, antibiotics

Urinary Retention l l Diuresis begins after birth to rid extra fluid (2000 -3000 m. L) Trauma to bladder & urethra during birth or anesthesia may cause loss of tone, difficulty sensing need to void Must assess abdomen frequently to prevent permanent damage to bladder from over distention. Check fundus to see if bladder is full. Nursing interventions? ?

Vital Signs l May have slight elevation of temp in 1 st 24 hours--dehydration. If 100. 4 or above, suspect infection. l Rapid or thready pulse--sign of hemorrhage. l BP: monitor--still at risk of PIH. Methergine (oxytocic) can ↑BP. ↓BP could be sign of hemorrhage. – Can have orthostatic hypotension due to blood loss. Assist pt. with first trip to BR. Instruct pt to dangle legs and sit first, before rising. If dizzy, do not ambulate.

Breast Assessment l Breasts – Soft: Soft on palpation, day 1 & 2 – Filling: firmer & warmth, day 3 – Engorged: appear large, reddened, taut, shiny skin, warm, hard, tense & tender/painful on palpation – Mastitis (infection): only one part of breast is warm/reddened—UNILATERAL l Nipples: look for cracking, fissures, blisters, pain

Lactation l Engorgement: day 3 or 4. – If breastfeeding: l Encourage frequent breastfeeding. l Warm compresses or warm shower. – If not breastfeeding: l Cold compresses/ice, snug bra or breast binder, oral analgesics. l Breast care: – Wash daily with water and air dry –NO SOAP – Advise pt to wear nursing bra--1 -2 sizes larger than bra during pregnancy. Avoid underwires. Use cotton nursing pads for leaking--keep nipples dry.

Discharge Instructions l l l Avoid/limit heavy lifting, stairs. Good diet, increase fluids if breastfeeding. Adequate rest, exercise/activity as tolerated. Report fever, foul smelling discharge, increased pain or bleeding to MD. Sex/contraception. Follow up in 6 weeks with MD.

Postpartum Complications l Postpartum Hemorrhage – CAUSES: Uterine atony, lacerations, retained placental fragments l Risk factors: – ↑ uterine distension: multiples, polyhydramnios, macrosomia, fibroids – Trauma: rapid or operative birth – Placental problems: previa, accreta, abruptio, retained placental fragments – Atonic uterus: prolonged pitocin, magnesium sulfate or labor; ↑ maternal age or parity; uterine scar; chorioamnionitis; anemia; prior history – Inadequate blood coagulation: fetal death or DIC
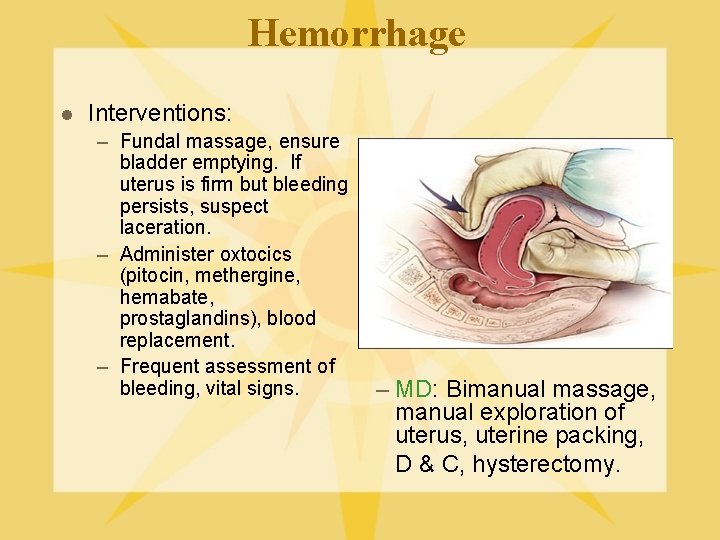
Hemorrhage l Interventions: – Fundal massage, ensure bladder emptying. If uterus is firm but bleeding persists, suspect laceration. – Administer oxtocics (pitocin, methergine, hemabate, prostaglandins), blood replacement. – Frequent assessment of bleeding, vital signs. – MD: Bimanual massage, manual exploration of uterus, uterine packing, D & C, hysterectomy.
Hemorrhage (cont. ) l Lacerations: cervical, vaginal, perineal l Retained placental fragments: – can occur well after delivery. Maternal serum test for h. CG or US. Possible D&C. – May see symptoms even after 1 week l Subinvolution: retained placenta, infection, fibroids – PO methergine, antibiotic.

Hematomas l Cause: Trauma during the birth process l Puerperal hematomas occur in 1: 300 to 1: 1500 deliveries l Most common locations for puerperal hematomas are the vulva, vaginal/paravaginal area, and retroperitoneum l Women at increased risk of developing puerperal hematomas include those who are nulliparous or who have an infant over 4000 grams, preeclampsia, prolonged second stage of labor, multifetal pregnancy, vulvar varicosities, or clotting disorders l Assessment: location, size, vital signs, pain, H&H l Treatment: evacuation and repair of bleeding source by MD

Postpartum Infection l l l Puerperal Infection: Endometritis infection of reproductive tract within 6 wks of childbirth Increased risk with: – – – – C-section Prolonged ROM, chorioamnionitis Retained placental fragments Preexisting anemia Prolonged/difficult birth, instrumental birth Internal fetal monitoring or IUPC Uterus explored after birth/manual removal of placenta – Preexisting vaginal infection (BV or chlamydia)

Postpartum Infection l Endometritis: infection of endometrium – Associated with chorioamnionitis & Csection – Signs & Symptoms – Can progress to pelvic cellulitis or peritonitis.

Endometritis l Ttreatments: l l l antibiotics oxytocics such as methergine, ↑ fluid intake pain relief diet l Nursing considerations: Fowler’s position or walking encourages drainage by gravity, gloves, strict handwashing l Usual course is 7 -10 days l May result in tubal scarring & interfere with future fertility

Post op C/Section Complications 1. Paralytic Ileus 2. Wound Dehiscence 3. Wound infection

1. A mother is experiencing shaking chills during the hour following birth. What is the nurse’s initial action? A. B. C. D. Take a rectal temperature Notify the physician or nurse-midwife Cover the woman with warmed blankets Review the order sheet for antibiotic orders

2. The nurse assesses a postpartum client and palpates the fundus at 2 cm above the midline and deviated to the right. What is the appropriate nursing action? A. Encourage the client to breastfeed B. Assist the client to empty her bladder C. Assist the client to a prone position and place a small pillow under her abdomen D. Massage the fundus

3. A nurse is caring for a client who is 2 hours postpartum who complains of severe, unremitting vaginal pain and inability to void. The fundus is firm at the umbilicus with moderate lochia rubra, and the perineum appears edematous with significant bruising. The nurse suspects the client may have A. A fourth-degree episiotomy. B. Distended bladder. C. Hematoma. D. Endometritis.

4. A 6 -day postoperative C-section client calls the clinic nurse and complains of malaise and increased pain on the right side of her incision with increased drainage. What should be the nurse’s correct initial response? A. Instruct the client to take her pain medication as prescribed B. Notify the physician or nurse-midwife C. Instruct the client to increase rest and seek assistance with household tasks D. Instruct the client to call the physician or nurse-midwife if her temperature reaches 100. 8.

5. A 6 -day postpartum client complains of fatigue and episodes of crying during the past two days. Which of the following statements is a correct response by the nurse? A. “This must be very difficult for you. ” B. “This sounds like postpartum blues. It is a normal response to birth. ” C. “You sound exhausted. Try and sleep when the baby sleeps. ” D. “This sounds like postpartum depression; you should contact your physician or nurse-midwife for a referral to a counselor. ”

6. A nurse is caring for a client with a superficial thrombophlebitis. Which of the following is the most appropriate nursing action? A. Administer anticoagulants per order B. Elevate the affected limb C. Apply ice packs to the affected limb D. Administer antibiotics per order

Breastfeeding l l www. youtube. com/watch? v=CIZ 6 r. Vzs 4 CE&feature=Pl ay. List&p=BD 065 FA 5 F 03 CD 81 A&index=38 (Breastfeeding Basics) www. youtube. com/watch? v=Ruv. JZGFOHU&feature=P lay. List&p=1330 DE 183266 B 0 BC&playnext=1&playnext _from=PL&index=3 (What’s the Big Deal? ) www. youtube. com/watch? v=Ox 8 ht. EVn. QA&feature=Play. List&p=1330 DE 183266 B 0 BC&in dex=8 (latch-on 1) www. youtube. com/watch? v=WOQz. EN_dc. Pc&feature= Play. List&p=1330 DE 183266 B 0 BC&index=9 (latch-on 2)

The Amazing Newborn

Profile of a Newborn Ø Vital statistics ØWeight: 2. 5 to 3. 4 kg. Immediately after birth. Establishes baseline. Baby may lose up to 510%. ØLength: 18 - 21 inches ØHead Circumference: 32 - 35 cm ØChest Circumference: 32 - 35 cm ØVital Signs: Heart Rate 120 -160 bpm; Respirations 30 -60 breaths/minute; Ø Temperature 97. 6 - 98. 6 axillary
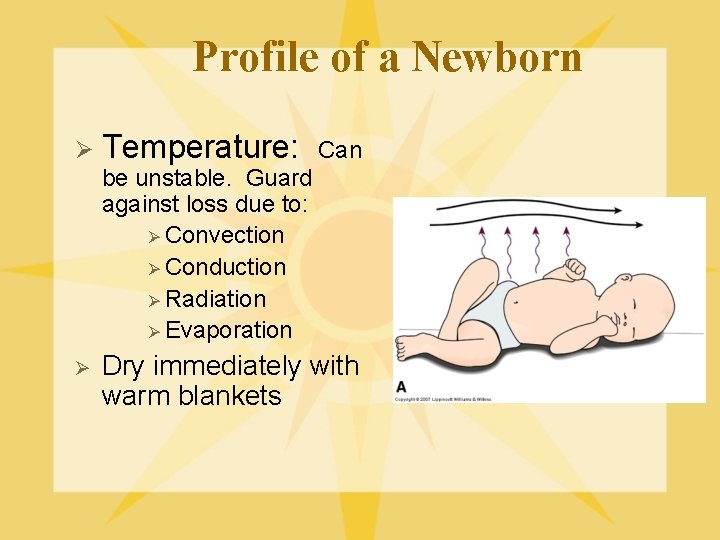
Profile of a Newborn Ø Temperature: Can be unstable. Guard against loss due to: Ø Convection Ø Conduction Ø Radiation Ø Evaporation Ø Dry immediately with warm blankets


Cardiovascular Changes after Birth l l l Closure of the ductus arteriosus/fetal shunts occurs when a neonate takes in oxygen through the lungs for the first time and when the lungs inflate, pressure in chest decreases (pulmonary artery) Common to have acrocyanosis, investigate central cyanosis (look at mucous membranes) Transition from fetal to postnatal circulation: “transitioning”

Critical Thinking l During a prenatal examination, an adolescent client asks, "How does my baby get air? " The nurse would give correct information by saying: A) "The fetus is able to obtain sufficient oxygen due to the fact that your hemoglobin concentration is 50% greater during pregnancy. " l l B) "The lungs of the fetus carry out respiratory gas exchange in utero similar to what an adult experiences. " C) "The placenta assumes the function of the fetal lungs by supplying oxygen and allowing the excretion of carbon dioxide into your bloodstream. "
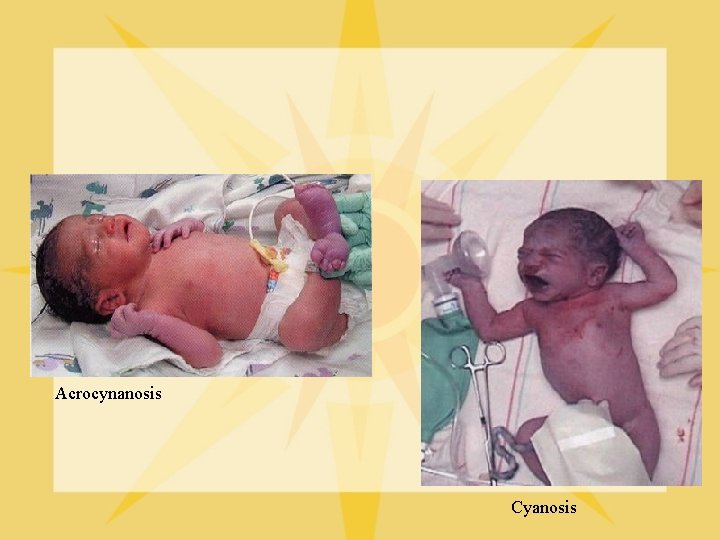
Acrocynanosis Cyanosis

Respiratory l Breathing is a result of replacement of air for fluid l Big Squeeze with vaginal birth

Factors predisposing respiration problems l l l Maternal history of diabetes Premature rupture of membranes Maternal use of barbiturates or narcotics close to birth Non-reassuring fetal monitoring strip C-section birth l l l l Cord prolapse Low APGAR Meconium staining Prematurity Postmaturity Small for gestational age Breech birth Chest, heart or respiratory tract anomalies

Newborn Assessment: Respiratory Distress l 5 symptoms of respiratory distress – Tachypnea – Cyanosis – Nasal flaring – Expiratory grunting – Retractions l Transition period (1 -2 hrs post birth) vs signs of respiratory distress that persist

Sleep Wake Cycle l Supine position decreases risk for SIDS l Sleep 16 out of 24 hours, avg. of 3 -4 hours at a time (wake q 2 -3 for feeding) l Don’t add cereal to diet till 4 -6 months of age l Infants should never sleep in parents’ bed

Gastrointestinal l l Accumulation of bacteria in GI tract necessary for digestion and synthesis of vitamin K Uncoordinated peristalsis Limited ability to digest fats & starch (deficient enzymes) Immature cardiac sphincter-regurgitates easily Stools- – 1 st meconium, sticky tarlike – 2 nd-3 rd day- transitional (diarrhea like) – BF: 3 -4 light yellow/day. Formula: 2 -3 bright yellow/day – Infants receiving phototherapy have bright green stools as a result of increased bilirubin excretion

Urinary l l Very important to observe for first void Urine light colored and odorless--kidneys do not concentrate urine well

Immune System l l l Prone to infection Inability to form antibodies until 2 months of age: most immunizations delayed until then Born with passive antibodies (protect against diseases such as polio, measles, diphtheria, pertusis, chickenpox, rubella & tetanus) l Hepatitis B vaccine: babies exposed early in life have ↑risk of chronic liver problems – Positive mom: HBIG (Hep B immune globulin) and vaccine for baby
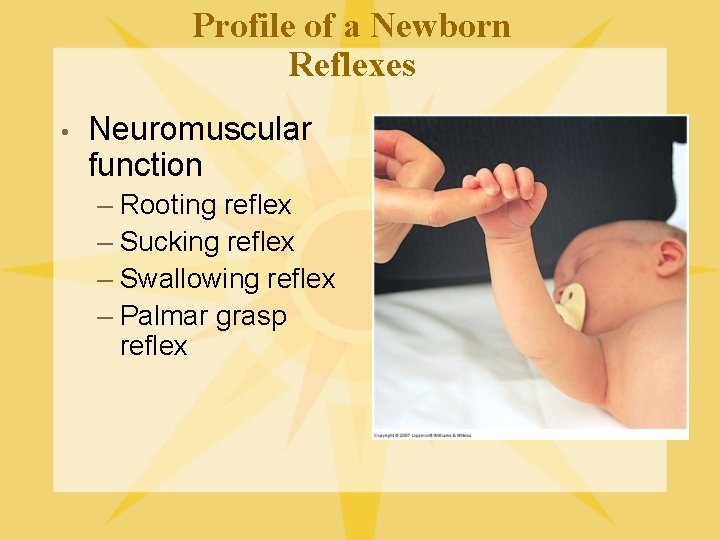
Profile of a Newborn Reflexes • Neuromuscular function – Rooting reflex – Sucking reflex – Swallowing reflex – Palmar grasp reflex
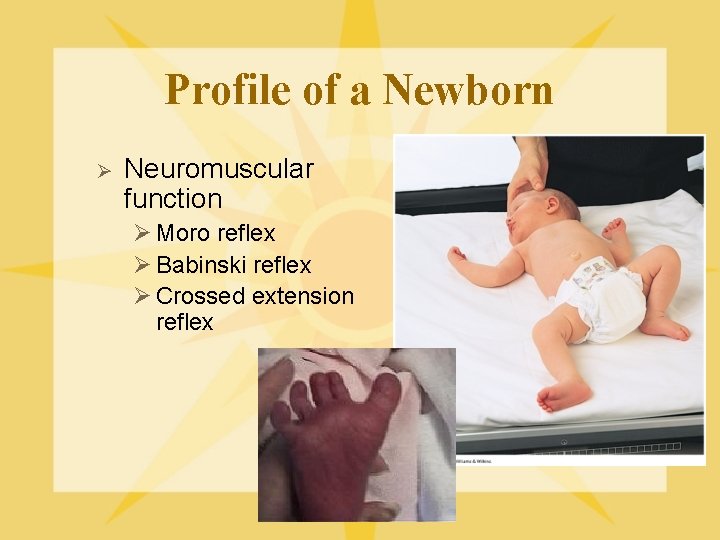
Profile of a Newborn Ø Neuromuscular function Ø Moro reflex Ø Babinski reflex Ø Crossed extension reflex
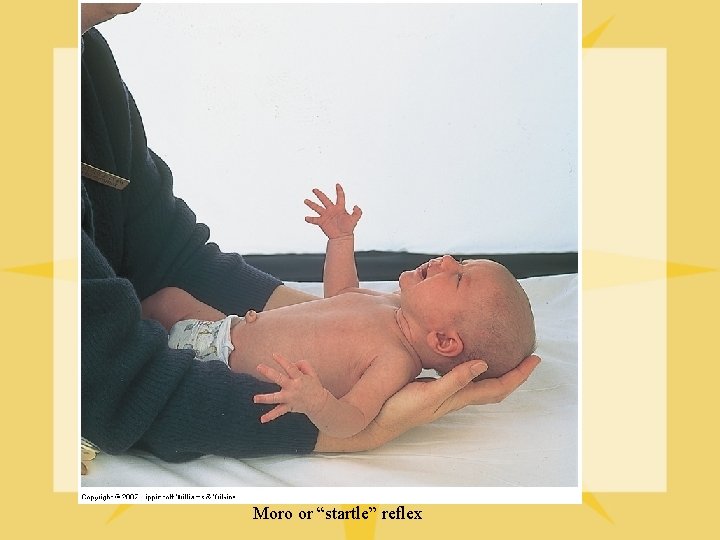
Moro or “startle” reflex

Senses l l l Hearing- yes Vision- “light” and “dark” in the first months. Approx 18” range. Touch- well-developed Taste- can discriminate Smell- well-developed

Appearance of a Newborn l Skin: Color should be pink l Cyanosis: mottling, acrocyanosis normal. Investigate central cyanosis. Look at mucus membranes l Hyperbilirubinemia: yellow tone to skin, sclera l Pallor: usually caused by anemia: blood loss? , blood incompatibility? , internal bleeding? l Harlequin sign: normal, immature circulatory system. Dependent side red, upper side pale.
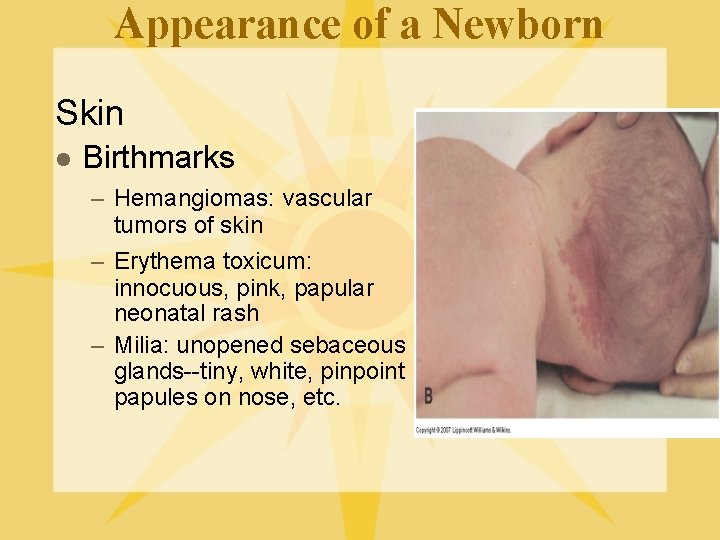
Appearance of a Newborn Skin l Birthmarks – Hemangiomas: vascular tumors of skin – Erythema toxicum: innocuous, pink, papular neonatal rash – Milia: unopened sebaceous glands--tiny, white, pinpoint papules on nose, etc.
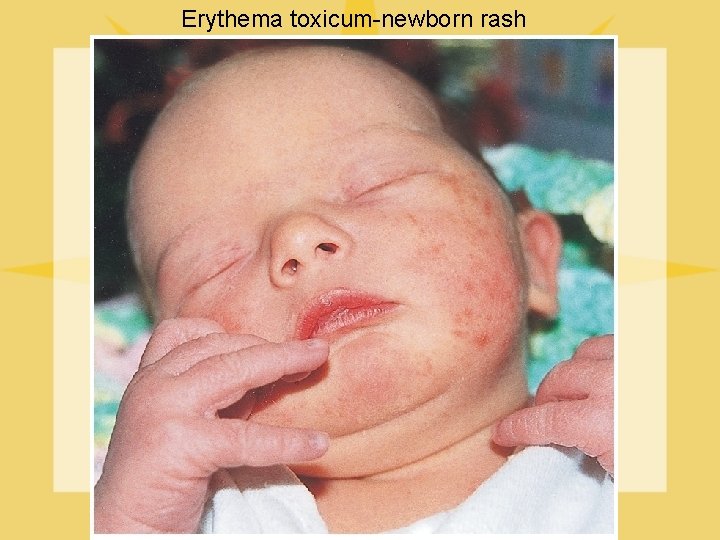
Erythema toxicum-newborn rash
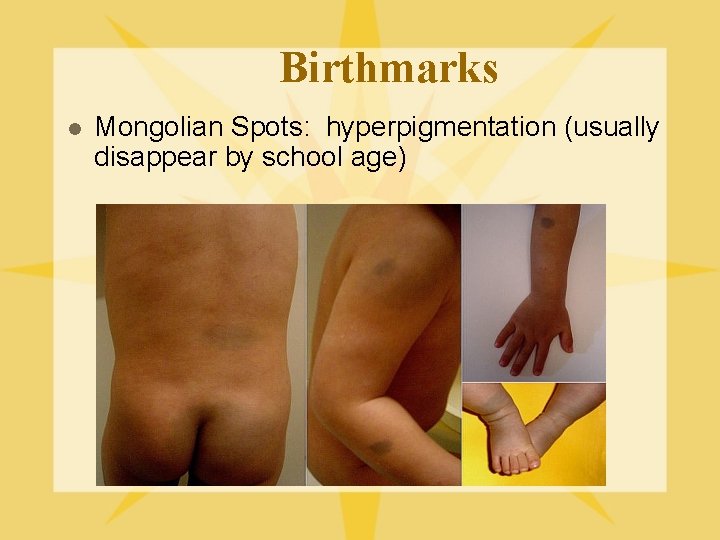
Birthmarks l Mongolian Spots: hyperpigmentation (usually disappear by school age)

Appearance of Newborn l Skin • Vernix caseosa: white, cream cheese-like substance, natural lubricant most 36 -38 weeks • Lanugo: fine downy hair on body • Desquamation: dry, peeling

Appearance of a Newborn Head: large-1/4 body length • • • Fontanelles Sutures Molding Caput succedaneum Cephalhematoma

Assessment for Well-Being l Apgar scoring--10 is perfect score Done at 1, 5 & 10 minutes • • • Heart rate Respiratory effort Muscle tone Reflex irritability Color Normal Apgars at 1 minute: 7 to 10
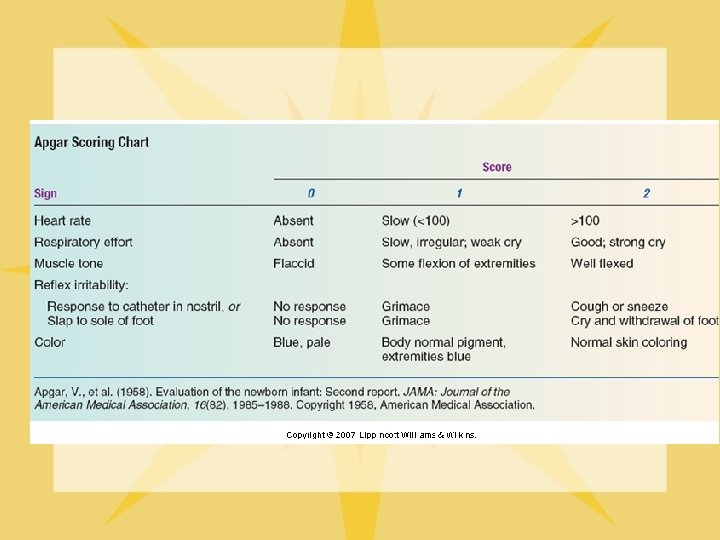

Immediate Care at Birth l l l Keep the newborn warm Promote adequate breathing pattern Inspection and care of umbilical cord Eye care Infection precautions

Critical Thinking l The nurse is planning care for a newborn. Which of the following nursing interventions would best protect the newborn from the most common form of heat loss? A) Pre-warming the examination table B) Placing the newborn away from air currents C) Drying the newborn thoroughly D) Removing wet linens from the isolette

Care of Newborn At Birth l l Identification and Registration Identification Band Birth Registration Birth Record Documentation (vitals, meds, labs)

Continuing Assessment for Well-Being l l l Respiratory evaluation Physical examination Laboratory studies: cord blood collected – – – CBC, Newborn Screen* ABO type & Rh, Direct Coombs if mom Rh - or Type O* C reactive protein if risk for infection Bilirubin level*

Assessment for Well-Being l Gestational age – neuromuscular & physical maturity – Ballard Scale • Dubowitz Maturity Scale LGA/SGA: at risk for hypoglycemia BS < 40 mg/d. L → feed immediately s/s: jitteriness, lethargy, seizures l
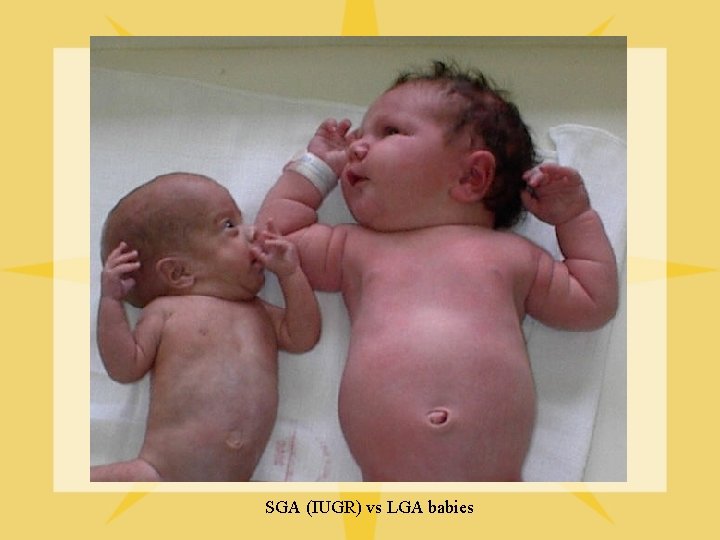
SGA (IUGR) vs LGA babies

Periods of Reactivity (P. 690, Pilleterri) l First Period 15 -30 minutes Alert, acrocyanosis, body temp falls, irregular respirations, vigorous reaction to stimuli l Resting Period 30 -120 minutes – Color, temperature stabilizing; respirations, HR slowing; sleeping (hard to wake up) l Second Period 2 -6 hours – Quick color changes with crying/movement; temperature increases; irregular respirations, HR; awake and responsive; first meconium passed

Nursing Care: Newborn and Family l l l Initial feeding Bathing Sleeping pattern Diaper area care Hearing Screen Newborn Screening Test (PKU) – Test for metabolic disorders (inborn errors of metabolism) – Done 24 hrs after first feeding

Nursing Care: Newborn and Family Medications l l Erythromycin opthalmic ointment Vitamin K administration – GI tract unable to produce Vitamin K (needed for blood coagulation) – O. 5 mg to 1 mg IM in thigh – Side effects- local irritation l l l Hepatitis B vaccination prior to discharge HBIG if needed (first 12 hours) Circumcision- per parent’s consent

Nutritional Allowances Calories: 110 calories x kg/24 hours l Protein: 2. 2 g x kg/24 hours l Fat: need linoleic acid l Carbohydrates: lactose intolerance rarely l present in newborn--switch to soy-based formula l Fluid: supplied by breast milk or formula, **do not supplement with water

Nutritional Allowances l Minerals • Calcium • Iron: supplement formula-fed babies • Fluoride: breastfeeding mom should drink fluoridated H 2 O. Make formulas with fluoridated H 2 O. Can supplement. l Vitamins: No supplementation needed until 6 mos.

Breastfeeding Promotion l l WHO promotes Breastfeeding around the world APA advocates breastfeeding for 12 months Baby Friendly initiatives in hospitals ↑breastfeeding rates and duration l

Breastfeeding l l Prolactin produced (stimulates milk production) when progesterone levels fall after placenta is delivered Colostrum- First milk produced: thick, creamy, yellow fluid composed of protein, sugar, fat, water, minerals, vitamins and maternal antibodies--digestible. Has laxative effect to aid baby to excrete meconium.
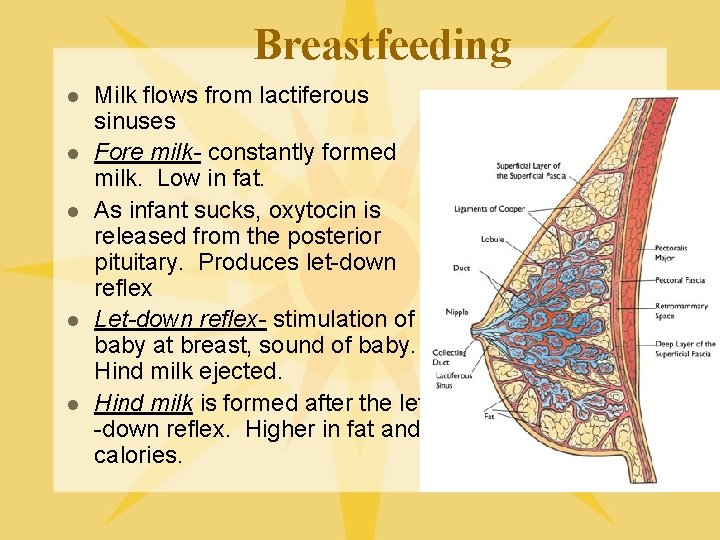
Breastfeeding l l l Milk flows from lactiferous sinuses Fore milk- constantly formed milk. Low in fat. As infant sucks, oxytocin is released from the posterior pituitary. Produces let-down reflex Let-down reflex- stimulation of baby at breast, sound of baby. Hind milk ejected. Hind milk is formed after the let -down reflex. Higher in fat and calories.

Infant Advantages in Breastfeeding l Less infection: mom’s antibodies passed, breast milk has elements that prevent absorption of viruses & bacteria from GI tract and that kill/inhibit bacteria & viruses - ↓ gastroenteritis and ↓ ear infections l Ideal composition for human baby: electrolytes, minerals, linoleic acid, trace elements, hypoallergenic--reduces allergies l l Easy to digest Reduces obesity, diabetes later in life

Maternal Advantages of Breastfeeding l l l Protective function in breast cancer prevention Release of oxytocin from the posterior pituitary gland aids in uterine involution Empowerment effect Reduces economic costs Bonding Breast milk contains lysozymes that are involved in destroying bad bacteria

Breast Feeding and Jaundice l l l Jaundice occurs in 15% of breast fed babies Pregnanediol (breakdown product of progesterone) depresses an enzyme that converts indirect bilirubin to direct bilirubin (accumulation of indirect bilirubin) Encourage frequent feedings because colostrum is a natural laxative and helps promote passage of meconium and bile
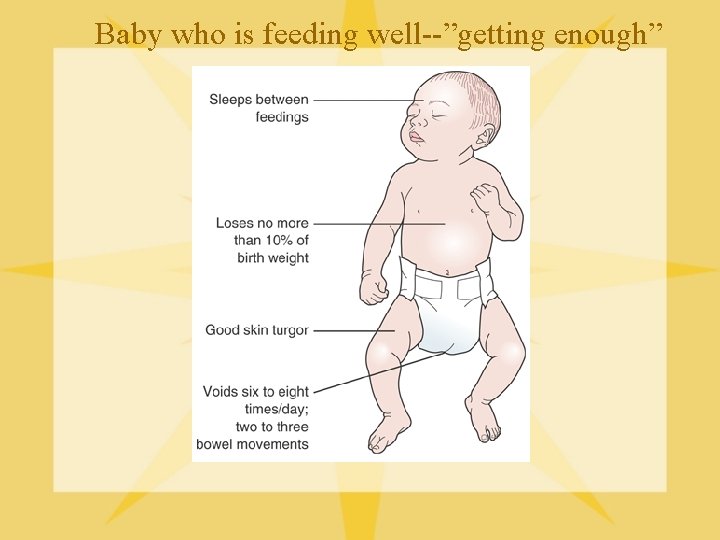
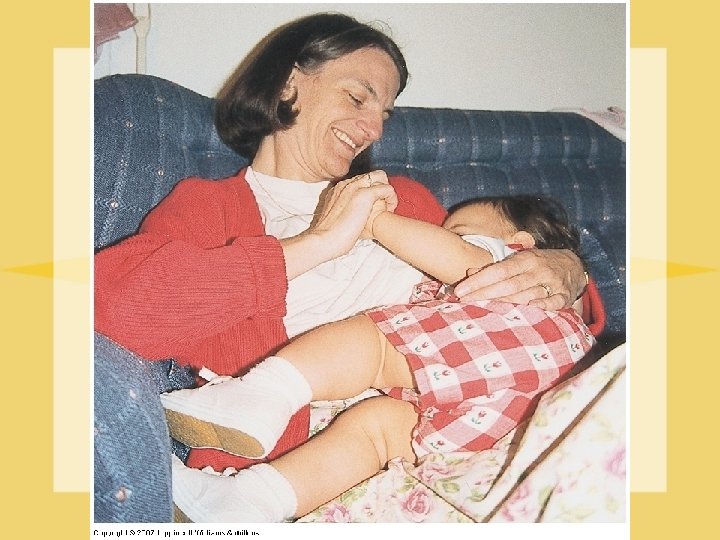
Baby who is feeding well--”getting enough”

Breastfeeding l l l Every 2 -3 hours in first weeks Promote adequate sucking Provide support Techniques for burping Multiple infants Engorgement

Problems in Breastfeeding l l l Sore nipples Supplemental feedings Working outside of the home Weaning Engorgement Mastitis

Formula Feeding Ø Preparation Ø Commercial formulas Ø Formula adequacy Ø Supplies needed Ø Formula preparation Ø Feeding techniques – 75 to 90 ml of fluid per pound of body weight per day
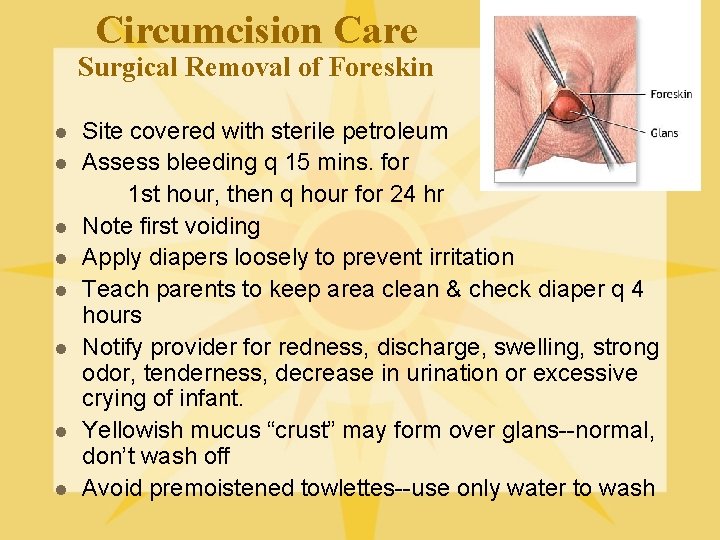
Circumcision Care Surgical Removal of Foreskin l l l l Site covered with sterile petroleum Assess bleeding q 15 mins. for 1 st hour, then q hour for 24 hr Note first voiding Apply diapers loosely to prevent irritation Teach parents to keep area clean & check diaper q 4 hours Notify provider for redness, discharge, swelling, strong odor, tenderness, decrease in urination or excessive crying of infant. Yellowish mucus “crust” may form over glans--normal, don’t wash off Avoid premoistened towlettes--use only water to wash

Circumcision Care l Heals in a couple of weeks l Monitor for complications: hemorrhage, cold stress/hypoglycemia, infection, urethral fistula, delayed healing and scarring, fibrous bands. l Discharge instructions & signs of danger

Discharge Teaching l When to call healthcare provider: – Baby’s axillary temp > 100. 4 – > 1 episode of forceful (projectile) vomiting or frequent vomiting over 6 -hr period – Refusal of 2 feedings in a row – Lethargy, difficulty awakening baby – Cyanosis with or without feeding – Absence of breathing > 20 secs – Inconsolable crying or continuous high-pitched cry – Discharge/bleeding from umbilical cord, circumcision – No wet diapers for 18 -24 hrs or < than 6 -8 wet diapers/day – Eye drainage

Hyperbilirubinemia l Hyperbilirubinemia: results from destruction of red blood cells – Physiologic jaundice l Normal physiologic process l Does not occur in first 24 hours of life l Home care – Pathologic jaundice l Abnormal destruction of RBCs l Occurs in first 24 hours of life or persists after 1 week l Causes: hemolytic disease of newborn: Rh or ABO blood incompatibility (mom Rh - or type O)
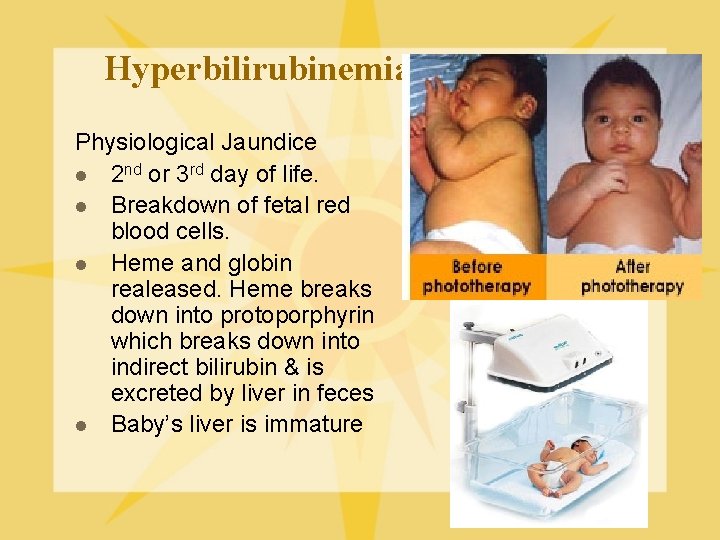
Hyperbilirubinemia Physiological Jaundice l 2 nd or 3 rd day of life. l Breakdown of fetal red blood cells. l Heme and globin realeased. Heme breaks down into protoporphyrin which breaks down into indirect bilirubin & is excreted by liver in feces l Baby’s liver is immature

Pathologic Jaundice l Before 24 hours or persistent after day 7 l Bilirubin increases more than 0. 5 mg/dl/hr, peaks at greater than 13 mg/dl or associated with anemia and hepatosplenomegaly Rh incompatibility/isoimmunization, infection, RBC disorder. ABO incompatibility: positive coombs test (test babies when mom O−/O+) Kernicterus (bilirubin encephalopathy) can result from untreated hypergbilirubinemia with bilirubin levels at or higher than 20 mg/dl → mental retardation l l

Risk Factors for Hyperbilirubinemia l l l l l ↑ RBC breakdown (cephalohematoma, extensive bruising from birth trauma) Rh or ABO incompatibility Ineffective breastfeeding & dehydration Certain medications (aspirin, tranquilizers, and sulfonamides) Maternal enzymes in breast milk- fairly uncommon Hypoglycemia Hypothermia Decreased liver function Anoxia

Lab Testing l Elevated serum bilirubin (direct and indirect) l Blood group incapability between the mother and newborn l H&H l Direct Coomb’s test--reveals presence of antibody-coated (sensitized) Rh-positive RBCs in the newborn l Electrolyte levels for dehydration from phototherapy (treatment of hyperbilirubinemia)

Nursing Assessments of Hyperbilirubinemia l Yellowish tint to skin, sclera and mucus membranes--observe by window l Note time of jaundice (integral in differentiating between physiologic and pathologic jaundice) l Treatments: early feedings, phototherapy, exchange transfusion

Neonatal Complications RDS (Respiratory Distress Syndrome) l Pathophysiology: – Low-level or absent surfactant – Inspiratory effort to inflate alveoli remains high – Pulmonary resistance prevents fetal shunts from closing – Lungs are poorly perfused and tissue hypoxia occurs with resultant acidosis l Surfactant not formed until week 34

Neonates at Risk for Respiratory Distress Syndrome (RDS) l l l Preterm infants Infants of diabetic mothers Infants born by cesarean Perinatal asphyxia Decreased O 2 tension in the lungs (one cause is meconium aspiration) Maternal factors: PROM, barbiturate/narcotic use, hypotension, bleeding

Assessment of Infants with RDS l S/S usually don’t develop immediately post birth. First S/S are subtle: – Low body temperature – Nasal flaring – Expiratory grunting – Sternal and subcostal retractions – Tachypnea (> 60 respirations per minute) – Cyanotic mucous membranes

Assessment of Infants with RDS l As distress continues: – Seesaw respirations – Heart failure – Pale, gray skin – Periods of apnea – Bradycardia – Pneumothorax

Therapeutic Management l l Administer surfactant through ET tube Oxygen administration (CPAP or assisted ventilation with PEEP) Ventilation Indomethacin or ibuprofen to close patent ductus arteriosus

Prevention of RDS l l Tocolytics (Magnesium Sulfate, Terbutaline, Procardia), corticosteroids (Betamethasone) usually given between 24 -34 weeks L: S (lecithin: sphingomyelin) ratio is 2: 1 in amniotic fluid -indicates fetal maturity, but not accurate

Transient Tachypnea of Newborn l l l l When respiratory rate continues to remain high (between 80 -120 breaths/min) after 1 hour mark Usually infant doesn’t appear distressed but instead tired from breathing too fast Usually mild retractions but no cyanosis Feeding difficulties Usually occurs from a slow absorption of lung fluid More common in C-section babies & preterm infants Peaks at 36 hours and usually resolves at 72 hours TX: close observation, O 2

Critical Thinking l The mother of a three-day-old infant calls the clinic and reports that her baby's skin is turning slightly yellow. The nurse should explain to the mother that: A) The baby is yellow because the bowels are not excreting bilirubin. B) The newborn's liver is not working as well as it should. C) The yellow color indicates that brain damage may be occurring. D) Physiologic jaundice is normal and peaks at this age.

Critical Thinking l The nurse is caring for a newborn with jaundice. The parents question why the newborn is not under the phototherapy lights. The nurse explains that the fiber optic blanket is beneficial because: (Select all that apply. ) A) The lights can be turned off intermittently. B) The eyes do not need to be covered. C) The lights will need to be removed for feedings. D) Newborns do not get overheated. E) Weight loss is not a complication of this system.
- Slides: 104