Posterior Urethral Valve Syndrome Dr Tricia A Jacobsen

Posterior Urethral Valve Syndrome Dr. Tricia A. Jacobsen 6/30/03

Initial Presentation • 31 y/o G 5 P 2022 • EDC 9/10/03, LMP 12/7/02 – conceived on OCP’s • Preg dated by LMP, conf by 7 W 1 D u/s • Prenatal course uncomplicated prior to admission

Past OB Hx • 2 Spontaneous Abortions • 2 Spontaneous Vaginal Deliveries uncomplicated

Past GYN Hx • No h/o of ovarian disease • No abnormal Pap Smears • No h/o STD’s • Menses regular, began at age 12

Past Surgical Hx • No surgical history
Past Medical Hx • H/O Migraines • Meds – Lo-estrin 1/20 with Fe • NKDA • Social – ¼ PPD cig. Occ ETOH

Prenatal labs • O+, Antibody screen neg • RI, VDRL NR • Hep B Sag – neg • HIV neg • CBC – 6. 8/13/36. 7/304 • Pap – WNL • One hour Glucola – 52 • Quad Screen – DS risk neg; 1: 622

16 week u/s – 4/2/03 • Anatomy Scan – wnl • Amniotic fluid – Volume wnl • Normal IUP est. at 16 w 5 d consistent with LMP • EFW of 159 grams • Placenta – fundal, no evidence of previa

6/17/03 • Called Attending MD c/o contractions • c/o mild contractions or “Cramping” • No LOF, No Vaginal bleeding • Positive Fetal Movement • Prenatal course uncomplicated until that day • No other illnesses or symptoms

6/17/03 cont. • Pt sent for an ultrasound in Rocky Hill • Found to have oligohydramnios with a 3 cm pocket • Distended fetal bladder 4. 9 cm by 2. 9 cm • Bilateral hydronephosis • Pt sent to Labor and Delivery for complete evaluation

Evalulation on L&D – 6/17/03 PE - no acute distress, no h/a, scotomata - VS: 122/72, 84, 98. 7 – – – Lungs –CTA, no wheezing CV – RRR, S 1 S 2 Abd – Soft, NT, +BS, no RUQ pain, + FM Ex – NT, no edema Spec – os appeared closed, Cultures sent, Nitrazine neg, fern neg, no pooling – Pelvic – Cx long, thick, closed – FHR – 130’s, reactive, Ave LTV, no variable, no decels – Toco – negative – occasional cramp

Evaluation on L&D - 6/17/03 cont. • Labs – O+, Antibody screen neg CBC – 8. 8/12. 2/34. 0/252 Chem 7 – WNL U/A – WNL GC/CHL – neg/neg GBS - neg

6/17/03 eval cont. • U/S revealed 27 wk fetus in cephalic • • • presentation, AFI < 3 cm, + FM, FB, Placenta anterior, Grade 1 Distended bladder noted, + hydronephrosis Pt admitted, Celestone started, MFM consulted and formal u/s ordered for the am Pt remained on L&D for continuous monitoring due to oligohydramnios

MFM Evaluation began • 6/18/03 – formal ultrasound revealed – Distended, thick walled bladder with a keyhole appearance in the area of the posterior urethra – Ureters and renal calyces were distended – Hydronephrosis – Left renal pelvis = 7 mm Right renal pelvis = 10 mm -- Amnioinfusion with 300 cc of warm normal saline was performed with asp. of 20 cc for chromosomal analysis
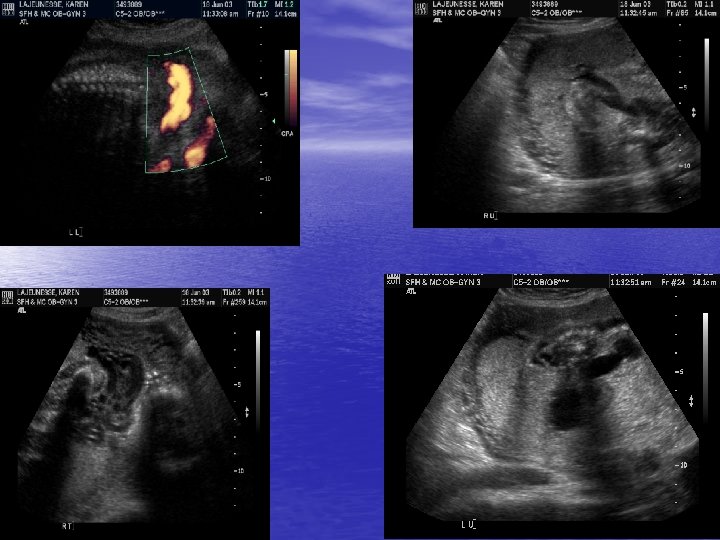

MFM Eval. Cont. • Chromosomal (FISH) Analysis: – Chrom #13 = 2 – Chrom #18 = 2 – Chrom #21 = 2 – Chrom X = 1 – Chrom Y = 1 – Normal Male Fetus

Posterior Urethral Valve Syndrome • Bladder outlet obstruction that is produced by a membrane within the posterior urethra • Within the scope of obstructive uropathies – Urethral atresia – Persistent cloaca – Chromosomal abnormalities – Hypospadius, epispadius or stenosis

PUVS Cont. • Incidence = 1 in 5, 000 to 8, 000 males • Affects only males • Most common cause of severe obstructive uropathies • Etiology – may be failure of complete disintegration of the urogenital membrane

PUVS - Diagnosis • Distended, thick walled bladder with a dilated • • posterior urethra – “Keyhole” app. Dilated ureters with b/l hydronephrosis Fluid volume/urine volume varies Presence of increased cortical echogenicity w/ or w/o cortical cysts may be consistent with renal dysplasia and a poor prognosis Cortical cysts are associated with irreverisble, advanced renal damage – fetus not amenable to intervention
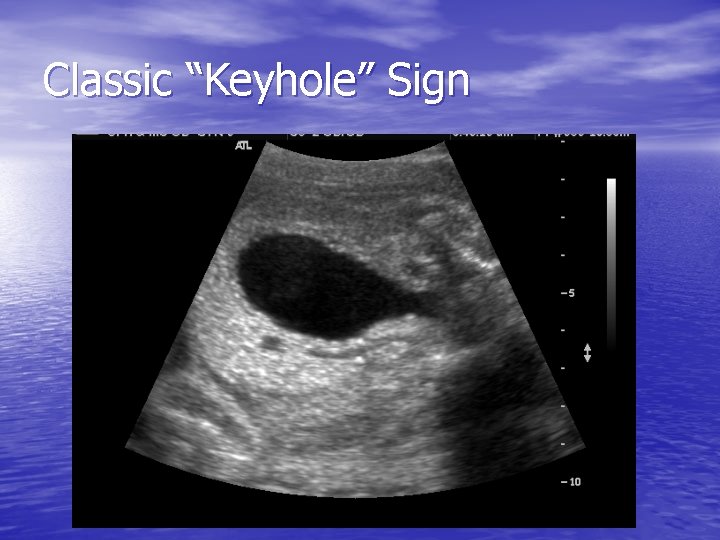
Classic “Keyhole” Sign
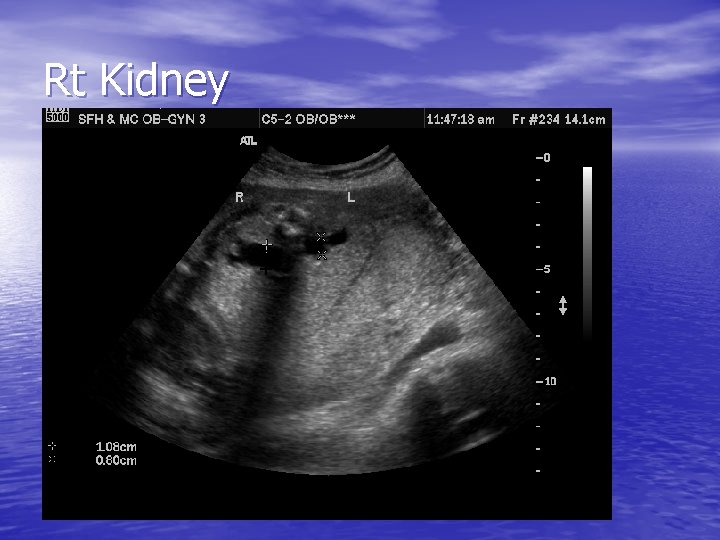
Rt Kidney
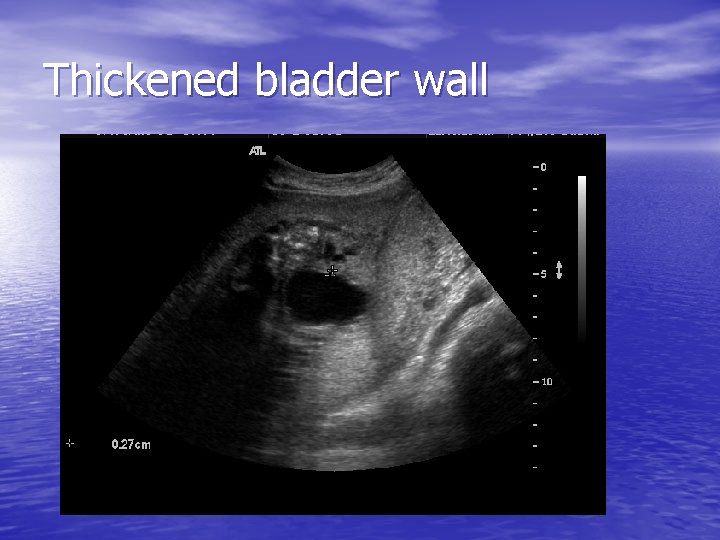
Thickened bladder wall
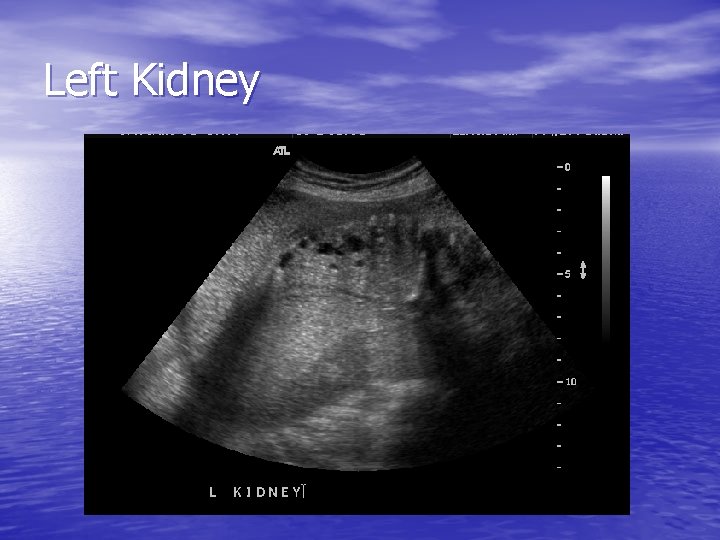
Left Kidney
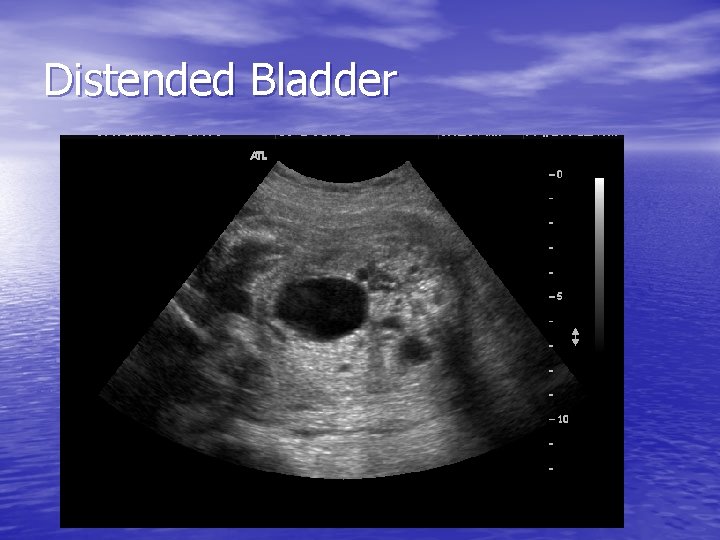
Distended Bladder
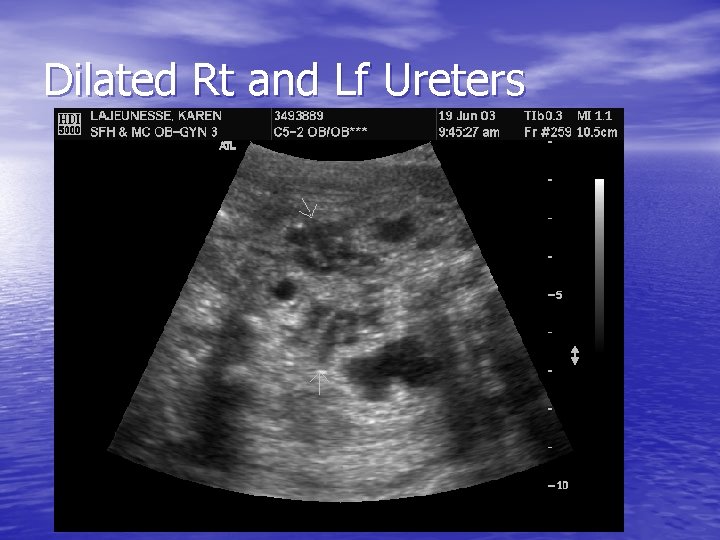
Dilated Rt and Lf Ureters
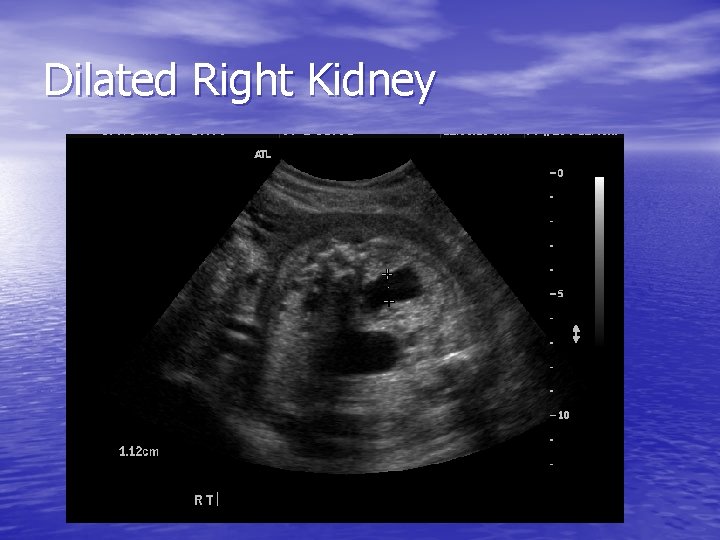
Dilated Right Kidney
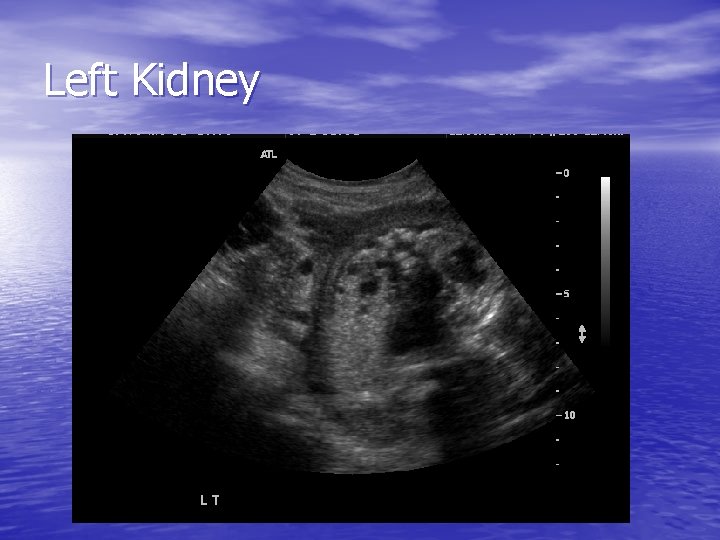
Left Kidney
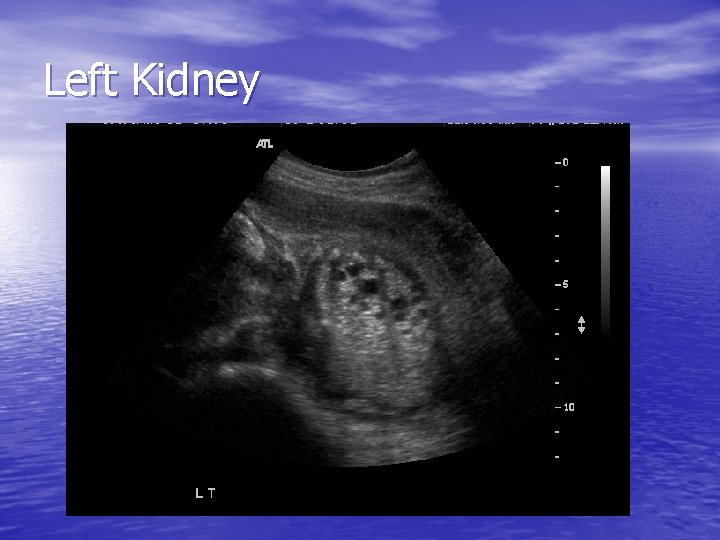
Left Kidney
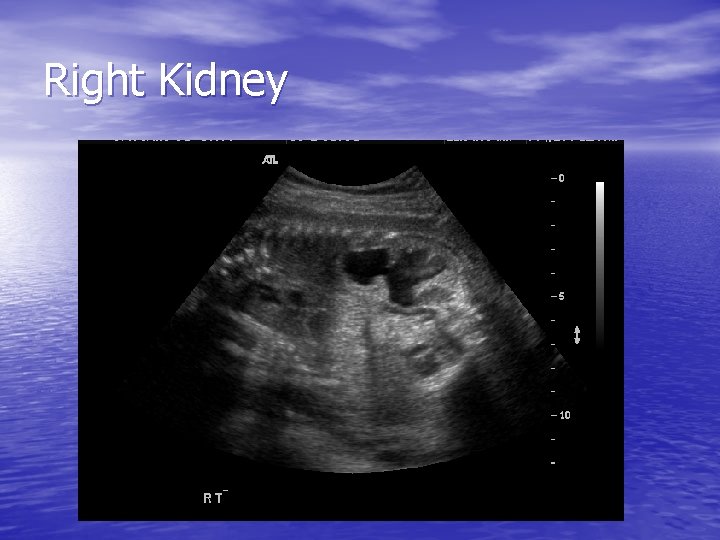
Right Kidney

PUVS - Pathology • Obstruction appear to be a diaphragmatic membrane with small opening in posterior urethra • Simple mucosal membrane with fibrous stroma • Dilatation of the prostatic urethra occurs b/w the obstructing membrane and the bladder neck

PUVS - Findings • Elevated intravesicular pressures leading to reflux to ureters and renal pelvises • Hydronephrosis develops from continued urine production with obstruction • Renal pelvis and calyceal systems become distended, compress renal parenchyma

PUVS - Findings • Histologically – Smooth muscle hypertrophy and • • hyperplasia within the bladder wall – increased bundle of smooth muscle Dilation of distal and proximal tubules associated with peritubular and interstitial fibrosis Fibrosis = echogenic appearance of the renal parenchyma on ultrasound

PUVS • After 14 wks, amniotic fluid is dependent on fetal urine production • Fetal swallowing, breathing, and AFI falls dramatically • During 18 – 24 week from canalicular to alveolar phase results in underdeveloped lungs if no fluid

Work up – First step – ultrasound • Bladder evaluated prior to and following • • drainage by fine needle vesicocentesis Overall size of bladder and degree of proximal urethral dilation (keyhole sign) Urethral and kidney evaluation for dilation or abnormalities, echogenicity, or cysts After vesicocentesis – the degree of bladder thickness is assessed Rule out other anomalies ie NTD, cardiac defects

WU – ultrasound cont • Long axis of the kidney is measured when evaluating underlying hydronephrosis • Kidneys which are large for gestational age and are less hyperechogenic – better prognosis • Kidneys which are hyperechogenic and are small have poorer prognosis due to advanced renal fibrosis

Work up – Second step • Prenatal evaluation for fetal karyotype • Amniocentesis if fluid available – fluid may be infused the aspirated to obtain cells • CVS if early – prelim results in 2 -3 days • Final results in 7 -10 days • May cultures cells from fetal urine – although more difficult to culture

Final Eval – Third step • Evaluation of fetal kidney function with sequential vesicocenteses • Completely drain fetal bladder at 48 -72 hr intervals at a minimum of three occasions • Fetuses w/ progressive hypotonicity and values that fall below threshold benefit from in utero intervention i. e. shunt placement
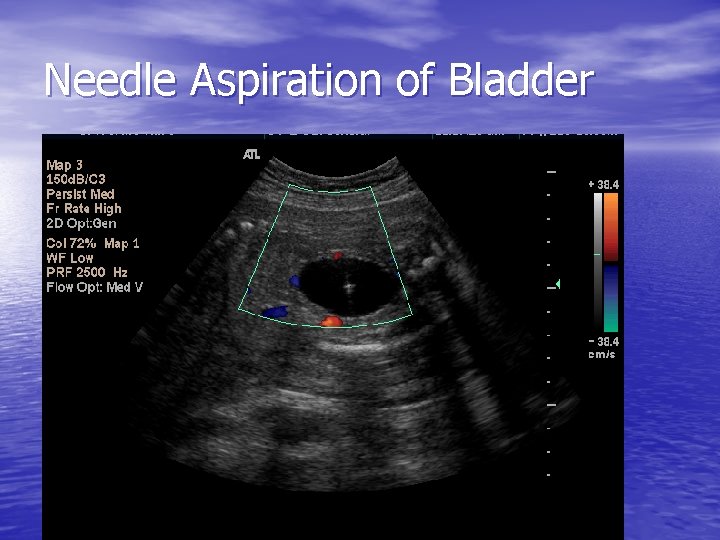
Needle Aspiration of Bladder

Eval cont • Fetuses with isolated megacystis, bilateral hydronephrosis, decreased amniotic fluid volume, absent anomalies, a 46 XY karyotype and serially improving hypotonicity with values below the recommended thresholds would be candidates for vesicoamniotic shunt placement

Prognosis • Outcome depends upon severity • Classified as good or poor • Poor prognostic factors include diagnosis before 24 wks, oligohydramnios, increased cortical echogenicity with cysts indicating renal dysplasia and marked hydronephrosis

Prognosis cont • Fetuses that present with these findings have a very poor prognosis • These die in the neonatal period from severe pulmonary hypoplasia • Normal fluid volume with stable hydronephrosis have better outcomes • Normal renal cortical echogenicity does not exclude renal dysplasia

Sonographic factors • Good prog factors – – – Normal fluid Diagnosis after 24 wk Asymmetric hydronephrosis – Urinary ascites – Isolated • Poor prog factors – Oligohydramnios – Diagnosis before 24 wks – Echogenic kidneys – Perinephric urinoma – Associated abnormalities
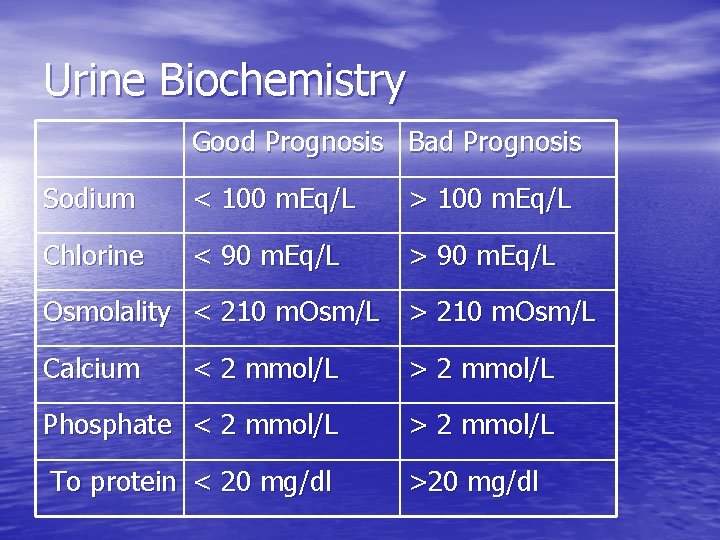

Urine Biochemistry Good Prognosis Bad Prognosis Sodium < 100 m. Eq/L > 100 m. Eq/L Chlorine < 90 m. Eq/L > 90 m. Eq/L Osmolality < 210 m. Osm/L > 210 m. Osm/L Calcium < 2 mmol/L > 2 mmol/L Phosphate < 2 mmol/L > 2 mmol/L To protein < 20 mg/dl >20 mg/dl

6/19/03 – Bladder tap #1 • Sodium • Chloride • U osm • Protein • Calcium - 116 mmol/L 92 mmol/L 265 112 mg/dl 8. 5 mg/dl

6/20/03 Bladder tap #2 • Sodium • Chloride • U osm • Protein • Calcium - 114 mmol/L 90 mmol/L 249 95 mg/dl 9. 2 mg/dl

6/23/03 Bladder tap #3 • Sodium • Chloride • U osm • Protein • Calcium - 118 mmol/L 93 mmol/L 255 113 mg/dl 8. 1 mg/dl

Management • Poor prognosis group – may offer termination because infants ultimately die of pulmonary hypoplasia – or offer conservative management • Fetuses with normal fluid and stable hydronephrosis – serial u/s until delivery • Poor or good prognosis – depends upon serial renal urine biochemistries

Management cont • Fetuses with good prognosis – placement of vesicoamniotic shunt with Rodeck catheter (double pigtail) – Counsel re: rupture of membranes, infection, injury to fetus, intraplacental bleeding, PTL – High density plastic with open metal tipped proximal and distal ends placed at fundal region – best fetal position vertex, back down – Memory of the plastic allow return to shape – Follow with serial u/s to confirm placement

Management Cont • Consultation with pediatric urologist • Route of delivery – routine obstetric indications • Average of delivery due to spontaneous • rupture of membranes = 33 -35 wks Following delivery – sterile ostomy bag to abdomen until renal function and anatomical evaluation by pediatric urologist

Summary • PUVS – bladder outlet obstruction • Affects 1 in 5, 000 – 8, 000 boys • Etiology unknown • Obstruction of posterior urethra • Diagnosed by u/s • Prognosis – dependent upon severity of hydronephrosis and urine chemistries

References • Ultrasound and Fetal Therapy, “fetal shunt procedures” Johnson M. P. , Feldman and M. I. Evans; chapter 1 • Bettelheim et al, Prenatal diagnosis of fetal urinary ascits, Ultrasound Obstetrics and Gynecology 2000; 16: 473 -475 • Sonographic Diagnosis of Fetal Medicine, 634 – 637.
- Slides: 51