Poster FRI 0541 Highly elevated ferritin levels are
- Slides: 1

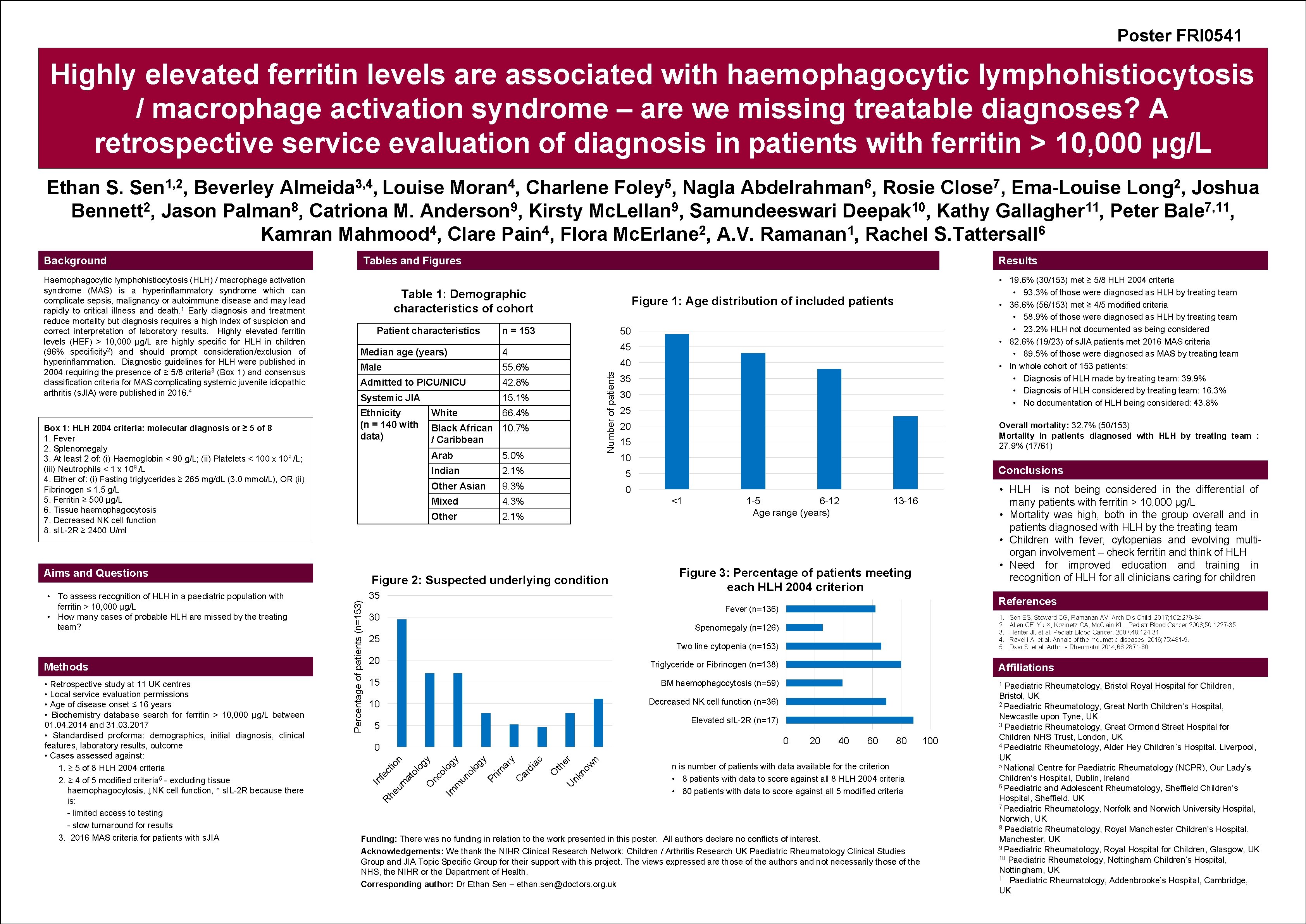
Poster FRI 0541 Highly elevated ferritin levels are associated with haemophagocytic lymphohistiocytosis / macrophage activation syndrome – are we missing treatable diagnoses? A retrospective service evaluation of diagnosis in patients with ferritin > 10, 000 μg/L 3, 4 Almeida , Louise Ethan S. Beverley Charlene Nagla Rosie Ema-Louise Joshua 2 8 9 9 10 11 7, 11 Bennett , Jason Palman , Catriona M. Anderson , Kirsty Mc. Lellan , Samundeeswari Deepak , Kathy Gallagher , Peter Bale , 4 4 2 1 6 Kamran Mahmood , Clare Pain , Flora Mc. Erlane , A. V. Ramanan , Rachel S. Tattersall 55. 6% Admitted to PICU/NICU 42. 8% Systemic JIA 15. 1% 40 66. 4% Black African 10. 7% / Caribbean 35 30 25 Overall mortality: 32. 7% (50/153) Mortality in patients diagnosed with HLH by treating team : 27. 9% (17/61) 20 15 Arab 5. 0% Indian 2. 1% 5 Conclusions Other Asian 9. 3% 0 Mixed 4. 3% Other 2. 1% • HLH is not being considered in the differential of many patients with ferritin > 10, 000 µg/L • Mortality was high, both in the group overall and in patients diagnosed with HLH by the treating team • Children with fever, cytopenias and evolving multiorgan involvement – check ferritin and think of HLH • Need for improved education and training in recognition of HLH for all clinicians caring for children 10 <1 Figure 2: Suspected underlying condition 35 1 -5 6 -12 Age range (years) 13 -16 Figure 3: Percentage of patients meeting each HLH 2004 criterion References Fever (n=136) 30 1. 2. 3. 4. 5. Spenomegaly (n=126) 25 Two line cytopenia (n=153) 20 Triglyceride or Fibrinogen (n=138) 15 BM haemophagocytosis (n=59) 10 Decreased NK cell function (n=36) 5 Im n w no nk O ia c ar d C ar y Pr im th er U m un ol og y ol 20 40 60 80 n is number of patients with data available for the criterion • 8 patients with data to score against all 8 HLH 2004 criteria • 80 patients with data to score against all 5 modified criteria R he nc io n ct fe Paediatric Rheumatology, Bristol Royal Hospital for Children, Bristol, UK 2 Paediatric Rheumatology, Great North Children’s Hospital, Newcastle upon Tyne, UK 3 Paediatric Rheumatology, Great Ormond Street Hospital for Children NHS Trust, London, UK 4 Paediatric Rheumatology, Alder Hey Children’s Hospital, Liverpool, UK 5 National Centre for Paediatric Rheumatology (NCPR), Our Lady’s Children’s Hospital, Dublin, Ireland 6 Paediatric and Adolescent Rheumatology, Sheffield Children’s Hospital, Sheffield, UK 7 Paediatric Rheumatology, Norfolk and Norwich University Hospital, Norwich, UK 8 Paediatric Rheumatology, Royal Manchester Children’s Hospital, Manchester, UK 9 Paediatric Rheumatology, Royal Hospital for Children, Glasgow, UK 10 Paediatric Rheumatology, Nottingham Children’s Hospital, Nottingham, UK 11 Paediatric Rheumatology, Addenbrooke’s Hospital, Cambridge, UK 1 0 0 Sen ES, Steward CG, Ramanan AV. Arch Dis Child. 2017; 102: 279 -84 Allen CE, Yu X, Kozinetz CA, Mc. Clain KL. . Pediatr Blood Cancer 2008; 50: 1227 -35. Henter JI, et al. Pediatr Blood Cancer. 2007; 48: 124 -31. Ravelli A, et al. Annals of the rheumatic diseases. 2016; 75: 481 -9. Davì S, et al. Arthritis Rheumatol 2014; 66: 2871 -80. Affiliations Elevated s. IL-2 R (n=17) In • Retrospective study at 11 UK centres • Local service evaluation permissions • Age of disease onset ≤ 16 years • Biochemistry database search for ferritin > 10, 000 µg/L between 01. 04. 2014 and 31. 03. 2017 • Standardised proforma: demographics, initial diagnosis, clinical features, laboratory results, outcome • Cases assessed against: 1. ≥ 5 of 8 HLH 2004 criteria 2. ≥ 4 of 5 modified criteria 5 - excluding tissue haemophagocytosis, ↓NK cell function, ↑ s. IL-2 R because there is: - limited access to testing - slow turnaround for results 3. 2016 MAS criteria for patients with s. JIA White 50 Number of patients Male Ethnicity (n = 140 with data) 2 Long , • 19. 6% (30/153) met ≥ 5/8 HLH 2004 criteria • 93. 3% of those were diagnosed as HLH by treating team • 36. 6% (56/153) met ≥ 4/5 modified criteria • 58. 9% of those were diagnosed as HLH by treating team • 23. 2% HLH not documented as being considered • 82. 6% (19/23) of s. JIA patients met 2016 MAS criteria • 89. 5% of those were diagnosed as MAS by treating team • In whole cohort of 153 patients: • Diagnosis of HLH made by treating team: 39. 9% • Diagnosis of HLH considered by treating team: 16. 3% • No documentation of HLH being considered: 43. 8% 45 4 Percentage of patients (n=153) Methods 7 Close , Figure 1: Age distribution of included patients n = 153 Median age (years) Aims and Questions • To assess recognition of HLH in a paediatric population with ferritin > 10, 000 µg/L • How many cases of probable HLH are missed by the treating team? 6 Abdelrahman , Results Patient characteristics O Box 1: HLH 2004 criteria: molecular diagnosis or ≥ 5 of 8 1. Fever 2. Splenomegaly 3. At least 2 of: (i) Haemoglobin < 90 g/L; (ii) Platelets < 100 x 109 /L; (iii) Neutrophils < 1 x 109 /L 4. Either of: (i) Fasting triglycerides ≥ 265 mg/d. L (3. 0 mmol/L), OR (ii) Fibrinogen ≤ 1. 5 g/L 5. Ferritin ≥ 500 µg/L 6. Tissue haemophagocytosis 7. Decreased NK cell function 8. s. IL-2 R ≥ 2400 U/ml 5 Foley , Table 1: Demographic characteristics of cohort gy Haemophagocytic lymphohistiocytosis (HLH) / macrophage activation syndrome (MAS) is a hyperinflammatory syndrome which can complicate sepsis, malignancy or autoimmune disease and may lead rapidly to critical illness and death. 1 Early diagnosis and treatment reduce mortality but diagnosis requires a high index of suspicion and correct interpretation of laboratory results. Highly elevated ferritin levels (HEF) > 10, 000 μg/L are highly specific for HLH in children (96% specificity 2) and should prompt consideration/exclusion of hyperinflammation. Diagnostic guidelines for HLH were published in 2004 requiring the presence of ≥ 5/8 criteria 3 (Box 1) and consensus classification criteria for MAS complicating systemic juvenile idiopathic arthritis (s. JIA) were published in 2016. 4 4 Moran , Tables and Figures at ol o Background um 1, 2 Sen , Funding: There was no funding in relation to the work presented in this poster. All authors declare no conflicts of interest. Acknowledgements: We thank the NIHR Clinical Research Network: Children / Arthritis Research UK Paediatric Rheumatology Clinical Studies Group and JIA Topic Specific Group for their support with this project. The views expressed are those of the authors and not necessarily those of the NHS, the NIHR or the Department of Health. Corresponding author: Dr Ethan Sen – ethan. sen@doctors. org. uk 100