POST OPERATIVE CARE Presented by Dr Ryan Fernandes

POST OPERATIVE CARE Presented by Dr Ryan Fernandes Moderator : Dr Ananth Prabhu

The aim of post operative care is to provide the patient with as quick, painless & safe a recovery from surgery as possible.

GENERAL MANAGEMENT ü ü IMMEDIATE POST OPERATIVE PERIOD Ensure airway, breathing & circulation are satisfactory Monitor pain Watch for complications Monitor blood pressure, pulse & oxygen saturation

PATIENT RECOVERY ü ü Once the patient is fully conscious & comfortable & their functions are stable, the patients are transferred to the ward High risk patients are kept in the ICU During rounds, a simple system for ensuring that everything is checked & recorded is represented by the acronym SOAPSubjective Objective Assessement Plan

1) SUBJECTIVE Ask patients how they are Pain, nausea & mobility Anxiety, disorientation, change in behaviour – signs of complications 2)OBJECTIVE TPR Fluid balance Wound care Nutritional status Review of drug chart

3) ASSESSMENT Review all the information obtained under S & O & list the problems that the patient is now facing which needs addressing 4)PLAN ü Formulate & agree a plan with patient & staff ü Record the plan in the notes ü Anticipate when discharge from hospital ü Notes should be dated signed & legible

Pain Management ü ü ü TECHNIQUES FOR POST OPERATIVE PAIN RELIEF Regular intramuscular injections (may get pain break through) Local anesthetic block- ideal if it works Indwelling epidural- good pain control Continuous infusions- reduce oscillations in pain relief but risk of over dose Patient controlled analgesia- pain relief titrated to patients needs

Complications Associated With Monitoring Systems Air Embolism Phlebitis Finger Necrosis

AIR EMBOLISM > 15 ml air accidentally introduced. Enters right atrium causing inadequate heart filling. Results in drop in BP, rise in pulse rate & distension of JVP Avoided by running fluids through sets. Head down when catheters are introduced.

PHLEBITIS Catheter introduced into a vein results in inflammation around the area. Most important cause of post operative fever Degree of phelbitis depends on : 1) Time of application 2) Nature of fluid infused 3) Amount of bacterial contamination ü ü ü Check regularly for edema, induration & tenderness Mark the date of insertion Change after 72 hours

FINGER NECROSIS Arterial lines are usually inserted into the radial or femoral arteries In some patients – blood supply predominantly arises from radial artery This may cause ischemic necrosis of the fingers Check patency of both arteries using Allens test

RESPIRATORY COMPLICATIONS ü ü Causes of acute post-operative shortness of breath Myocardial infarction & heart failure Pulmonary embolism Chest infection Exacerbation of asthma or chronic obstructive airway disease

MEASURES TO BE TAKEN Oxygen to be started immediately IV access if needed Blood for full blood count, electrolytes & cardiac enzymes ABG if necessary In case of chest infection-sputum for microbiology
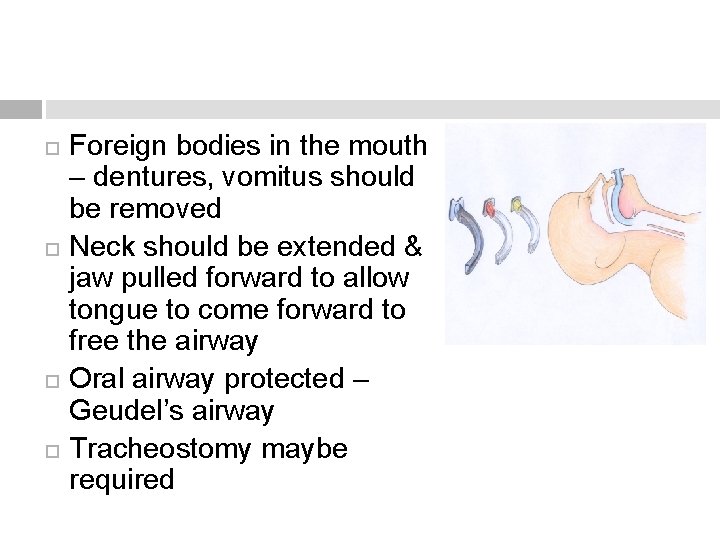
Foreign bodies in the mouth – dentures, vomitus should be removed Neck should be extended & jaw pulled forward to allow tongue to come forward to free the airway Oral airway protected – Geudel’s airway Tracheostomy maybe required

Cardiovascular Complications HYPOTENSION Commonest cause : hypovolaemia either due to bleeding or insufficient fluid replacement Myocardial infarction Septic shock, epidural anesthesia ü ü ü Treatment involves – Increase fluid input Administer high flow oxygen Patient tilted head down to maintain cerebral perfusion

HYPERTENSION q Maybe dangerous in patients with ischaemic heart disease or CVA as it precipitates stroke q Commonly related to inadequate pain relief q Anxiety q Settles with appropriate analgesia

Deep Vein Thrombosis RISK FACTORS Age > 60 yrs Recent surgery Immobilisation Trauma Oral contraceptive pill Obesity Heart failure Cancer

PREVENTION OF DVT Early mobilisation Hydration Compression stockings Low molecular weight heparin as prophylaxis Calf pumps Minimize use of tourniquets

Gastro-intestinal Complications PREDISPOSING FACTORS Poorly controlled pain Use of opioids Surgery on GIT Female sex Young adult History of pre-operative vomiting Acute gastric dilatation

TREATMENT GENERAL MEASURES ü Adequate pain control ü Avoid opiates ü Keep stomach empty ü Start oral feeds slowly ü Maintain hydration & blood pressure ü Epidural anesthesia DRUGS ü Dopamine receptor agonists eg. Prochlorperazine ü Metoclopramide ü H 1 receptor antagonists eg. Cyclizine ü 5 HT receptor antagonists eg. Ondansetron

URINARY COMPLICATIONS Oliguria is defined as urine output less than 0. 5 ml/kg/h Commonest cause- reduced renal perfusion due to peri-operative hypotension or inadequate fluid replacement May lead to acute renal failure

Prevention of Post Operative Renal Failure Monitor Renal Function Serum urea, creatinine, electrolytes Input/output monitoring q Assess Volume Status Pulse & Blood pressure Serial Body weight Central venous pressure q Prevent Sepsis Catheter care Drain abscess Give antibiotics

Contd… Optimise cardiac function Monitor cardiac output q Relieve Urinary Obstruction Prompt diagnosis Catheter drainage q Avoid nephrotoxins Limit toxins Avoid aminoglycosides Adjust drug doses q Consider diuretics Mannitol & frusemide

Urinary Retention Commonly seen in post-operative patients Most perineal & pelvic operations Procedures under spinal anesthesia Occurs due to interference of neural mechanisms responsible for normal bladder emptying & over distended bladder Pain & fluid deficiency Cathetrisation should be performed prophylactically when an operation is expected to last 3 hours or longer

Urinary Infection One of the causes for post-operative pyrexia Risk factors – Immunocompromised Diabetic Pre-existing Urinary infection H/O catheterisation TREATMENT ü Urine for C/S ü Adequate hydration ü Proper bladder drainage ü Relevant antibiotics

Complications Related To Specific Surgical Specialities Abdominal Surgery Anastamotic leakage Bleeding or abscess Slow recovery of intestinal motor functions The return of function occurs as – small bowel, large bowel, stomach

NECK SURGERY Must be observed for accumulation of blood in the wound May lead to rapid asphyxia A record of pre & post operative status of recurrent laryngeal nerve must be done NEUROSURGERY ICP should be monitored post operatively A rise may be signalled by a deterioration in the state of consciousness

VASCULAR SURGERY Patency of grafts & anastamoses in patients with femoropopliteal bypass & abdominal aneurysmal repairs Regular clinical assessment & doppler u. SG PLASTIC SURGERY Viabilty of flaps Perfusion Blood supply maybe compromised by position, dressing or collection of fluid

GENERAL COMPLICATIONS FEVER 40% patients develop pyrexia after major surgery 80% of cases no particular cause is found Pyrexia does not necessarily imply sepsis The inflammatory response to surgery manifest as temperature

The causes include: Days 2 - 5 : atelectasis of lung Days 3 -5 : superficial & deep wound infection Day 5 : chest infection including viral respiratory tract infection, UTI & thrombophlebitis >Days 5 : wound infection, anastomotic leakage, intracavitary collections & abscesses. Infected intravenous cannula sites, DVTs, transfusion reaction, wound haematomas,

PROPHYLAXIS AGAINST INFECTIONS In pateints with foreign material inserted – 3 doses of prophylatic antibiotics, one dose pre operatively & 2 doses post operatively Prophylactic antibiotics appear to reduce the risk of any contamination developing into infection by destroying bacteria before they are incorporated into the biofilm

PRESSURE SORES Due to friction or persisting pressure on soft tissues Affect pressure points in recumbent position ü ü ü RISK FACTORS: Poor nutritional status Dehydration Lack of mobility

MANAGEMENT Unconscious patients : position in bed to be changed every 30 minutes. High risk patients – air filter mattress which automatically alters pressure areas Early mobilisation prevents pressure sores & reduces respiratory complications

CONFUSIONAL STATES : Seen in 10% of patients Elderly patients Increased morbidity, mortality & hospital stay Usually presents with: ü Anxiety ü Incoherent speech ü Clouding of consciousness ü Destructive behaviour

Causes of Confusion ü ü ü ü Epilepsy Head injury Dehydration Septic shock Alcohol withdrawal Hypoglycemia Opioids

DRAINS Uses: 1) To drain purulent collections 2) Prevent accumulation of blood 3) Indicate the possibility of leaking surgical anastomosis

COMPLICATIONS 1) Trauma during insertion 2) Failure to drain 3) Sepsis at drain site 4) Drain site metastasis 5) Erosion by drain of the adjacent tissue 6) Perforation of abdominal viscera

DRAIN MANAGEMENT ü Quantity & character of drain fluid ü Excess loss of body fluid should be replaced by additional IV fluids ü Blood loss through drain should be investigated ü Coagulation profile & platelet count ü Low BP & urine output inspite of absence of blood in the drain needs to be investigated Drains should be removed once the drainage has stopped or become less than 25 ml/day – potential tract for contamination & infection

ü ü ü BLOOD TRANSFUSION During 1 st 24 hours post surgery, plasma or ECF loss may result in artificially high measurement of Hb. In a stable patient, tranfusion is indicated if the Hb falls below 8 g/dl. Monitor pulse, Bp & temperature during transfusion

Complications of Blood Transfusion Tachycardia Pyrexia Rash Pruritis Flushing Urticaria Bronchospasm Hypotension

MOBILISATION Immobilisation increases the risk of DVT, urinary retention, atelectasis, pressure sores, fecal impaction After laparotomy patients are encourged to sit out on a chair even as early as 1 st post operative day This improves ventilation & reduces pulmonary complications by reducing the pressure on the diaphragm

WOUND CARE Within hours of wound being closed the dead space fills with an inflammatory exudate Within 48 hours of closure a layer of epidermal cells from the wound edge covers the bridge Hence sterile dressings applied in theatre should not be removed before this time

Wounds should be inspected only if soakedbacterial contamination of wound. In case of infected wounds – daily dressings, pus for C/S, antibiotics. Skin sutures should be removed between 6 -10 days

WOUND DEHISCENCE It is the partial or complete disruption of any or all of the layers in a wound. Most commonly occurs from the 5 th to 8 th post operative day when the strength of the wound is at the weakest Usually presents with serosanguinous discharge

Risk Factors In Wound Dehiscence GENERAL Malnourishment Diabetes Obesity Persistent cough Sepsis Cancer Patients on steroids LOCAL q Inadequate or poor wound closure q Poor local wound healing q Increased intra-abdominal pressure

T U O Y K N A H
- Slides: 46