Post Menopausal Bleeding Done by Awn Khawaldeh Definition

Post Menopausal Bleeding Done by: Awn Khawaldeh

Definition § Is any unscheduled vaginal bleeding that occurs after 12 months of amenorrhoea in a woman of postmenopausal age. § It is a serious symptom which may indicate the presence of malignant disease in the genital tract, So Every woman with PMB should be assumed to have a carcinoma until full investigation has proved to the contrary.

Causes of Postmenopausal Uterine Bleeding § § § Atrophic vaginitis 60 -80% Estrogen treatments 15 -25% Polyps - endometrial or cervical 2 -12% Endometrial Hyperplasia 5 -10% Endometrial Cancer 10% No cause found 10%

Vaginal Atrophy § It is the most common cause of postmenopausal uterine bleeding. § Is thinning, drying and inflammation of the vaginal walls because of having less estrogen. This is a benign condition § Clinical features: In addition to postmenopausal bleeding: Vaginal dryness , burning sensation, discharge, itching with increased frequency, urgency , incontinence and urinary tract infections § Treatment: 1. Vaginal moisturizers 2. Estrogene either in form of creams, ring or tablet.

Hormone Replacement Therapy § Any vaginal bleeding in a menopausal woman other than the expected cyclical bleeding that occurs in women taking sequential HRT should be managed § A. . Estrogen- cyclical progsetrone : Estrogene will be given everyday. Progestrone will be given for the last (12_14) days. Bleeding is considered normal if bleeding starts after the nineth day of progesterone use or soon after the progestogen phase. § B. Combined estrogen-progestrone therapy: Breakthrough bleeding is common in the first 3 -6 months , Evaluation of the endometrium is recommended during the first year, if bleeding is heavy, prolonged or if any bleeding occurs after one year of use.
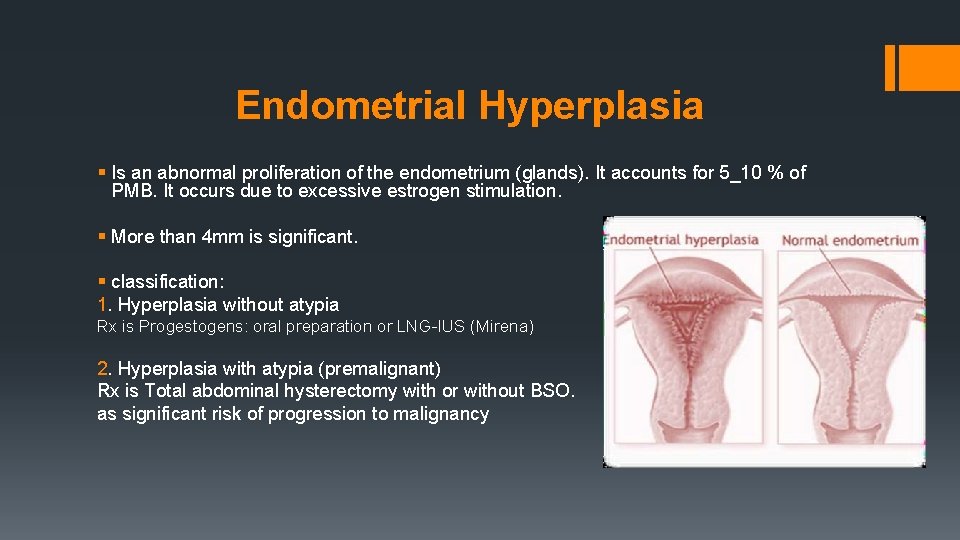
Endometrial Hyperplasia § Is an abnormal proliferation of the endometrium (glands). It accounts for 5_10 % of PMB. It occurs due to excessive estrogen stimulation. § More than 4 mm is significant. § classification: 1. Hyperplasia without atypia Rx is Progestogens: oral preparation or LNG-IUS (Mirena) 2. Hyperplasia with atypia (premalignant) Rx is Total abdominal hysterectomy with or without BSO. as significant risk of progression to malignancy

Endometrial Carcinoma § 2 nd most common gynecological cancer. § Is mainly adenocarcinoma arising from the lining of the uterus and is an estrogendependent tumor. § Accounts for 10% of postmenopausal bleeding. § 90% of patients with endometrial cancer will present with bleeding. § Has 4 stages: I. Confined to uterine body II. Involves cervix III. Outside uterus but inside the pelvis IV. Extended to blader or rectum

Risk Factors of Endometrial Carcinoma : 1. 2. 3. 4. 5. 6. 7. 8. 9. Early menarche Late menopause Nulliparity Chronic anovulation (P. C. O. S) Obesity (conversion of steroids to oestrone in their peripheral fat) Diabetes mellitus Unoppsed estrogen therapy Tamoxifen therapy (ESTROGENIC ACTIVITY ON ENDOMETRIUM) Personal or family history of: endometrial, ovarian, breast or colon cancer

Treatment of Endometrial Carcinoma § Stage 1 and 2 : total abdominal hysterectomy + bilateral salpingoopherectomy. If resectable surgery followed by chemotherapy § Stage 3 and 4 : radiotherapy If its not resectable neoadjuvant radiotherapy followed by surgery. § High dose of progestin if unfit for surgery. (paliative)

Management I. History II. Examination III. investigations

History: 1. Details of the bleeding(onset, duration, amount, color, presence of clot, whether it was related to trauma or not). 2. Associated symptoms such as pain, fever or changes in bladder or bowel function might suggest an infective process such as pyometra or the bleeding may be arising from the bowel or bladder. 3. exclude risk factors of endometrial carcinoma.

Examination 1. General examination: general condition, obesity. exclude signs of malignancy ( weight loss, pale 2. Abdominal examination: for any palpable mass. 3. pelvic examination: § Inspection of the vulva and vagina, particularly looking for atrophy( The vaginal skin looks thin, red and inflamed with areas of pinpoint bleeding). § A speculum examination (cervical polyp and cancer) § A bimanual examination to evaluate uterine size, mobility and the adnexae. 4. Per rectal examination: to exclude colorectal problems.

Investigations 1. Complete blood count 2. Coagulation studies 3. LFT, RFT 4. CHEST XRAY. specific investigations: I. Ultrasound (T. A. U , T. V. U) II. CA 125 III. Pippelle smear IV. Dilitation and curetage with biopsy V. Hysterescopy with endometrial biopsy
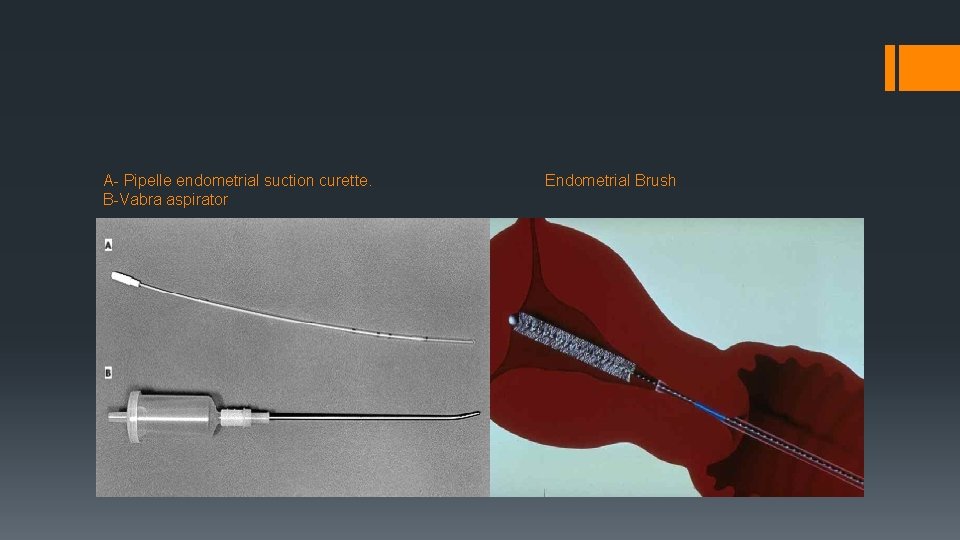
A- Pipelle endometrial suction curette. B-Vabra aspirator Endometrial Brush
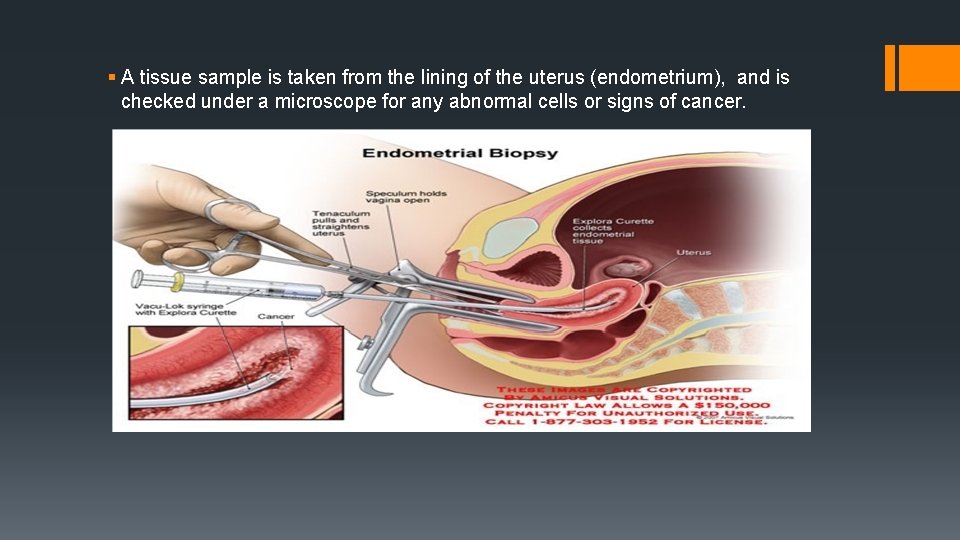
§ A tissue sample is taken from the lining of the uterus (endometrium), and is checked under a microscope for any abnormal cells or signs of cancer.
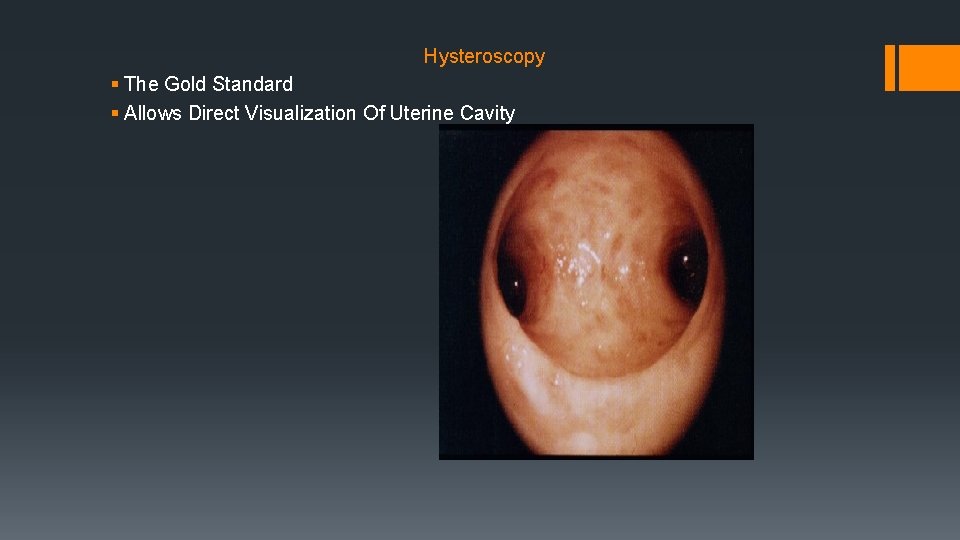
Hysteroscopy § The Gold Standard § Allows Direct Visualization Of Uterine Cavity

Management of post menopausal bleeding General measures : § Correct general condition(Anti-shock measure): § Hospitalization § • Assessment of blood loss: In some cases the blood volume loss may be excessive , rapid and possibly life threatening. § So rapid restoration of blood volume , vital parameters is followed by local examination to find out the site and source of bleeding § Definitive Treatment : The condition after diagnosis treated according to the underlying cause.

THANK YOU
- Slides: 18