Post Dural Puncture Headache Prevention Assessment and Treatment





































- Slides: 52

Post Dural Puncture Headache Prevention, Assessment and Treatment Lee A. Ellingson MHS, CRNA Jamestown Regional Medical Center NDANA 2013 Spring Conference

PDPH Definition Potentially severe headache that develops after dural puncture, presumably secondary to the rent in the dura and resultant CSF leak, which may cause traction on the meninges and cranial nerves.

PDPH History *Spinal Anesthesia: 1885 paper by neurologist Leonard Corning: “Spinal Anaesthesia and Local Medication of the Cord with Cocaine” *Lumbar Puncture: 1891 paper by internist/surgeon Heinrich Quincke *Surgical Spinal Anesthesia: 1899 surgeon August Bier *Surgical Spinal Anesth popularized: 1900 surgeon Theodore Tuffier: 63 case studies published


Spinal and Epidural Anesthesia…. So easy… even a monkey can do it!!

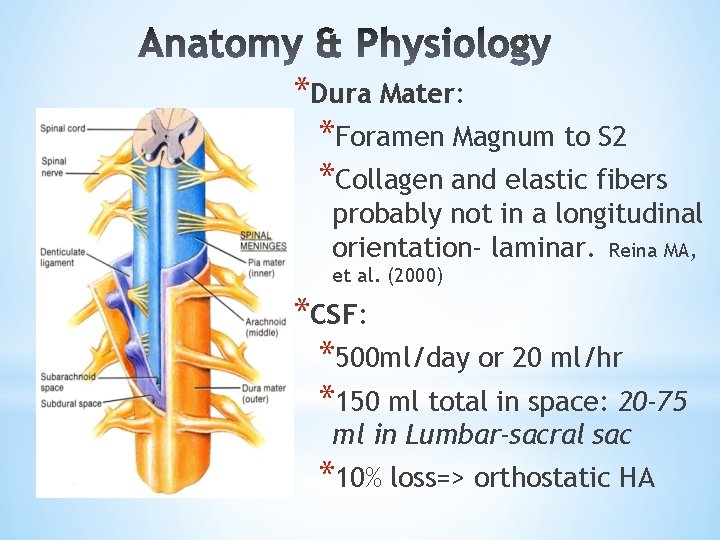
*Dura Mater: *Foramen Magnum to S 2 *Collagen and elastic fibers probably not in a longitudinal orientation- laminar. Reina MA, et al. (2000) *CSF: *500 ml/day or 20 ml/hr *150 ml total in space: 20 -75 ml in Lumbar-sacral sac *10% loss=> orthostatic HA

PDPH etiology *Two theoretical mechanisms: *Reflex vasodilitation: meningeal vessels dilate in order to increase CSF production as a response to lowered CSF pressures from dural leak. *Traction on upper level nerves: *Cervical: C 1 -3 stretch: neck & shoulder pain *Cranial: especially CN III - VII

PDPH: Predisposing Factors *Gender: Females > Males *Age: Greatest 14 – 60 years *Body Mass Index: Greater in Lower BMI *Prior history PDPH *Headache before Puncture *Motion Sickness correlation *NO correlation to Migraine history

Prevention: Needle Type Needle Size & Type rate EBP 26 ga Atracaun 5. 0% 55% 25 ga Quincke 24 ga Sprotte 8. 7% 2. 8% 66% 0% 25 ga Whitacre 3. 1% 0% Vallejo MC, et. al. (1991)

Prevention: Pencil Point *Reduction in PDPH incidence not attributed to hole size nor shape… *Pencil Point causes more traumatic dural rent than Quincke resulting in inflammatory reaction *Postulated that the tear causes an edematous plug preventing CSF leak Reina MA, et. al. (2000)

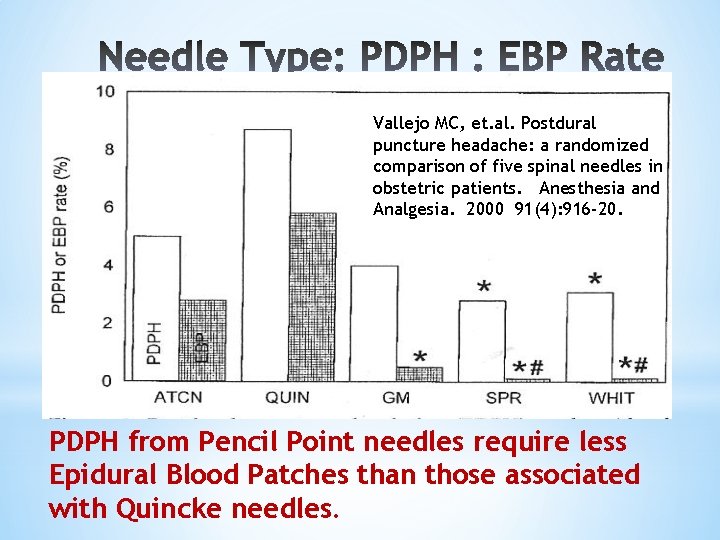
Vallejo MC, et. al. Postdural puncture headache: a randomized comparison of five spinal needles in obstetric patients. Anesthesia and Analgesia. 2000 91(4): 916 -20. PDPH from Pencil Point needles require less Epidural Blood Patches than those associated with Quincke needles.

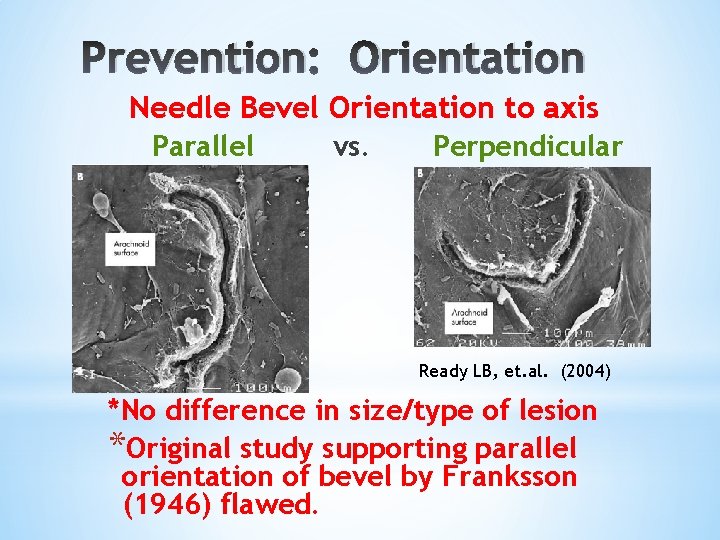
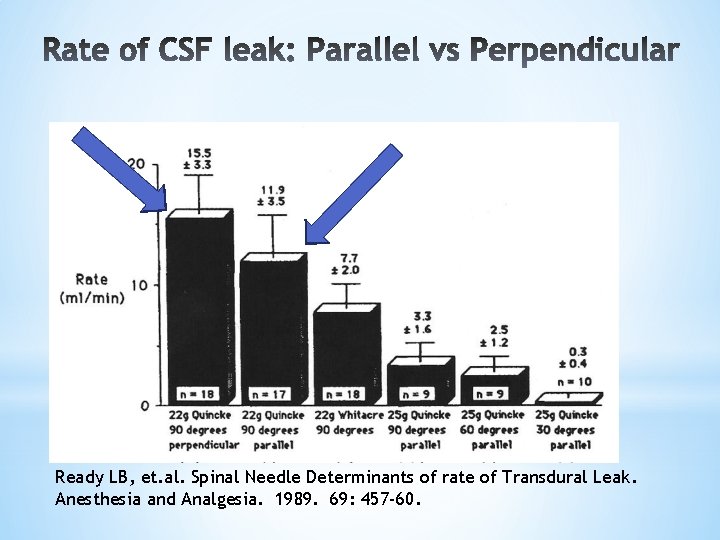
Prevention: Orientation Needle Bevel Orientation to axis Parallel vs. Perpendicular Ready LB, et. al. (2004) *No difference in size/type of lesion *Original study supporting parallel orientation of bevel by Franksson (1946) flawed.

Ready LB, et. al. Spinal Needle Determinants of rate of Transdural Leak. Anesthesia and Analgesia. 1989. 69: 457 -60.

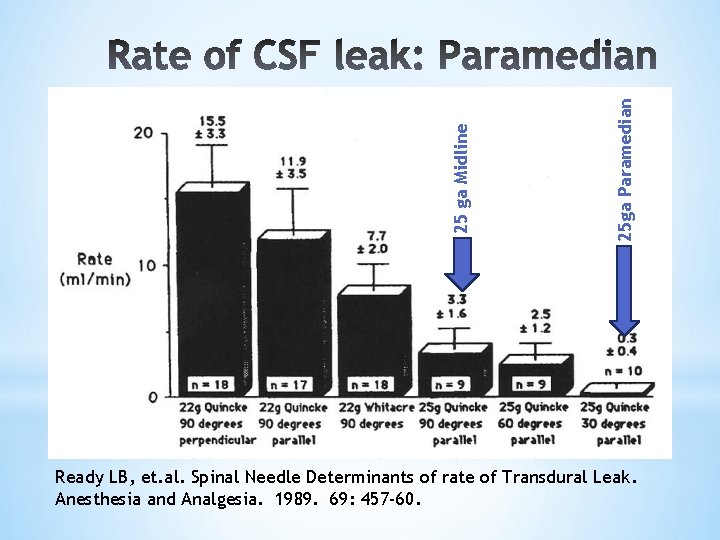
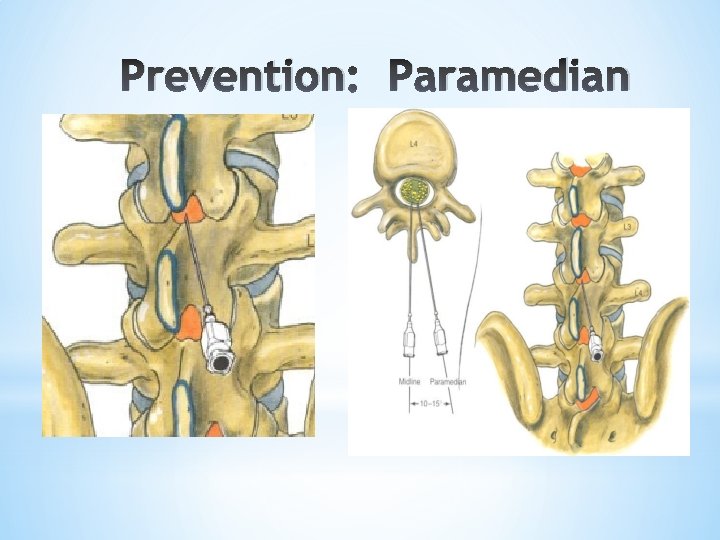
Prevention: Location *Median vs. Paramedian *30° angle insertion produces a “second flap valve mechanism” of arachnoid & dura *Paramedian approach produces a more lateral lesion with less tension on the “flap” than a posterior midline lesion upon lumbar flexion/extension Ready (1989)

25 ga Paramedian 25 ga Midline Ready LB, et. al. Spinal Needle Determinants of rate of Transdural Leak. Anesthesia and Analgesia. 1989. 69: 457 -60.

Prevention: Paramedian *Median vs. Paramedian

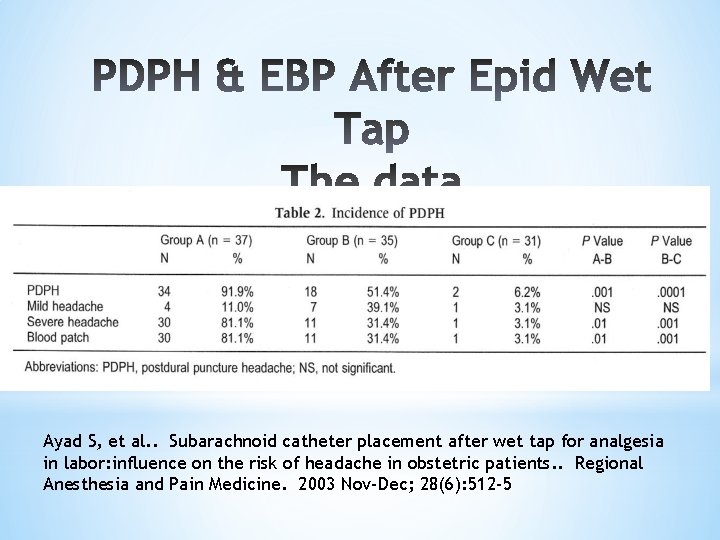
Prevention: Epidural Wet Tap *OB Epidural Wet tap PDPH incidence ~76% *115 Unintentional epidural wet tap obstetric patients at Cleveland Clinic divided into 3 groups: n=115 *A *B *C Epidural catheter reinserted different level Epidural catheter inserted subarachnoid & removed immediately after delivery Epidural catheter inserted subarachnoid & removed 24 hours after delivery Ayad S, et. al. (2003)

Prevention: Epidural Wet Tap PDPH Incid EBP Required A 92% 81% B 51% 31% C 6% 3% Lesson: If Epidural Wet Tap, use as continuous spinal catheter and don’t remove it until 24 hrs after delivery. Ayad S, et. al. (2003)

Intrathecal Catheter after Wet Tap: Why does it work? *Catheter mechanically prevents efflux of CSF during valsalva of Stage II pushing *Inflammatory fibrous reaction that closes dural rent after catheter removal *Other studies confirm same results with C -Section patients *Results NOT replicated in non-obstetric cases Ayad S, et. al. (2003)

Ayad S, et al. . Subarachnoid catheter placement after wet tap for analgesia in labor: influence on the risk of headache in obstetric patients. . Regional Anesthesia and Pain Medicine. 2003 Nov-Dec; 28(6): 512 -5

Prevention: Review What Works: *Minimize attempts / punctures *Smallest needle possible - 25 gauge *Pencil Point Please *Paramedian / Lateral Placement at 30° *If Epidural Wet Tap, place catheter Subarachnoid & leave in place 24 hours after delivery.

Prevention: Review What Does NOT Work: *Ignoring a headache after epidural wet tap *Treating an epidural wet tap headache conservatively *Bedrest after Large Bore Puncture: Only postpones onset. *Prophylactic injection of colloids. (Dextran may be the exception? ? ) *Prophylactic injection of crystalloids. (May lower incidence/severity of PDPH but NOT with lrg needles

Assessment / Diagnosis * Subjective- Symptoms: *Headache: Bi. Frontal – Occipital *Onset usually 12 – 14 hours after puncture *Postural component: necessary component *Neck & Shoulder pain *Nucchal rigidity *Nausea / Vomiting *Cranial Nerve : Visual & Auditory common

Assessment / Diagnosis * Subjective- History: *Headache Hx: *Caffeine *Nicotine *Illicit Drug *Fibromyalgia / myofascial pain syndrome *Anticoagulant med *Coag disorder *Preeclampsia/PIH *PE /DVT/CVST *Motion sickness *Prior PDPH

Assessment / Diagnosis * Objective Data: *Labs: HBG WBC ESR D-dimer *Vital Signs: especially BP & Temp *Motor Deficits *Bowel / Bladder dysfunction *Seizures *Eye Exam: Nystagmus, Photophobia, Diplopia, PERRLA

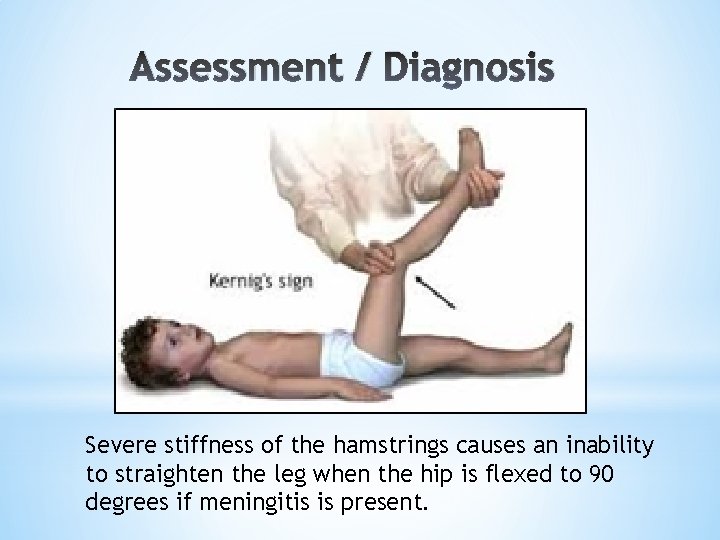
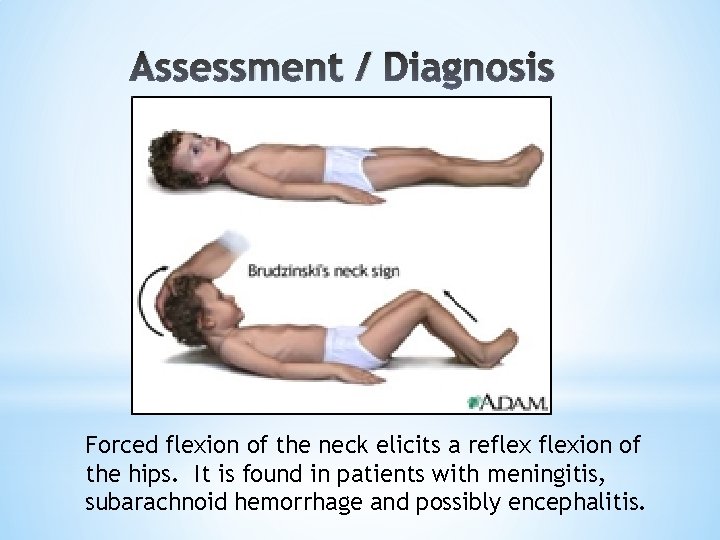
Assessment / Diagnosis * Objective Data (continued): *Auditory: Tinnitus, hyperacusis *Gutsche sign: Abd pressure relieves *Problems w/epidural catheter or aseptic technique? Sterility break? *Kernig’s sign & Brudzinski’s sign: pain with meningeal stretch associated with non-PDPH cause

Assessment / Diagnosis Severe stiffness of the hamstrings causes an inability to straighten the leg when the hip is flexed to 90 degrees if meningitis is present.

Assessment / Diagnosis Forced flexion of the neck elicits a reflexion of the hips. It is found in patients with meningitis, subarachnoid hemorrhage and possibly encephalitis.

*Tension HA: dull, entire head *Migraine HA: unilateral, throbbing *Caffeine Withdrawal: PO/IV caffeine trial *Nicotine Withdrawal: Nicotine patch trial *Lactation headache: vasopressin release at letdown. Common with history of migraine. *Brain Tumor: usually dull, not throbbing. ⇧ ICP ? *Subdural Hemmorhage: usually sudden & severe HA *Subdural Hematoma: Usually focal. ⇧ ICP? *Cortical Vein Sinus Thrombosis: usually ⇧ D-dimers

*Hypertension / Preeclampsia /Eclampsia *Meningitis *Pheumocephalus: similar to PDPH. Dx’ed with CT scan. LOR technique? *Myofascial Syndrome / fibromyalgia. Relieved with massage, spray-stretch, muscle relaxants *Inflammatory arteritis diseases. *Dehydration : *PDPH: requires postural component

Hmmm… Looks like a spinal headache and it’s after 3 PM! *%@)$(#*^@%& Now what do I do?

Caffeine: Double-blind, randomized study demonstrated that a single, oral dose of caffeine (300 mg) provided relief to 20 patients with PDPH. Beneficial effects of caffeine were rapid; relief occurred within 4 h after drug administration, and in 70% of patients, the symptoms did not recur. Side effects were infrequent and mild. Camann WR et. al. (1990) *Given to OB patients with early onset PDPH *Contradicted by some studies that find headaches recur at 48 hours *Caution: tachycardia, seizures, infant stimulation

Caffeine: Continued *Coffee-drip 142 *Coke-12 oz *Pepsi-12 oz *Mt Dew-12 oz *Tea-Black *Tea-green *No Doz *Vivarin 65 43 55 28 15 100 200 * Can administer as IV caffeine sodium benzoate in same dosing as PO * Half-life is 3 to 4 hours * Theophylline may also provide adenosine receptor block with relief

*Bedrest: postpones, but does NOT prevent/cure. No evidence for support *Hydration: No evidence to support increase in CSF. Transient relief *Abdominal Binder: Relief but uncomfortable *Analgesics: Palliative and not curative *Visual/Auditory rest: Palliative *Most resolve in 7 days with conservative therapy (except OB) Is that acceptable? ?

*Also known as Autologous Epidural Blood Patch (AEBP): *Gormley: pioneered in 1960. 2 -3 ml *Popularized in 1970 -72 by Crul and Di. Giovanni: 50 patients with 20 ml *Success rates vary 75 to 95% *OB patients: only 70% success rate due to lrg bore epid needles: Safa-Tisseront V (2001)

*Best results if start < 24 hrs after onset *Preparation: *Hydration if volume depleted *Analgesia to help tolerate procedure *Phlebotomist experienced in aseptic draw *Epidural Needle Insertion near site: Blood preferentially rises cephaled *20 ml Autologous Blood Injection – aseptically MRI after EBP of 20 ml demonstrated extradural hematoma extending 4 spinal segments (8 with 20 ml) and out through foraminal outlets with tamponade at dural puncture site. Cousins & Bridenbaugh(2009)

*Stop injection when patient expresses neck or back pain or has radiculopathy in leg(s) *Avoid early ambulation: 2 hours in decubitus increases success Martin (1994) *Avoid Heavy lifting, straining & bending 2 to 3 days

*Second Wet Tap *Back ache: 35% *Neck pain: 1% *Transient Temp spike 24 -48 hrs: 5% *Facial Nerve Paralysis: 2 cases due to CN VII pressure from ⇧ ICP by mass effect *Vasovagal syncope *Infection, arachnoiditis, bleeding rarely reported

*Failure: *30% failure rate at 24 hrs in OB pts. *May repeat AEBP in 24 hrs: hematoma clot resolves within 7 hrs *Consider alternate cause of headache: reassess PRN *Consider alternative therapies

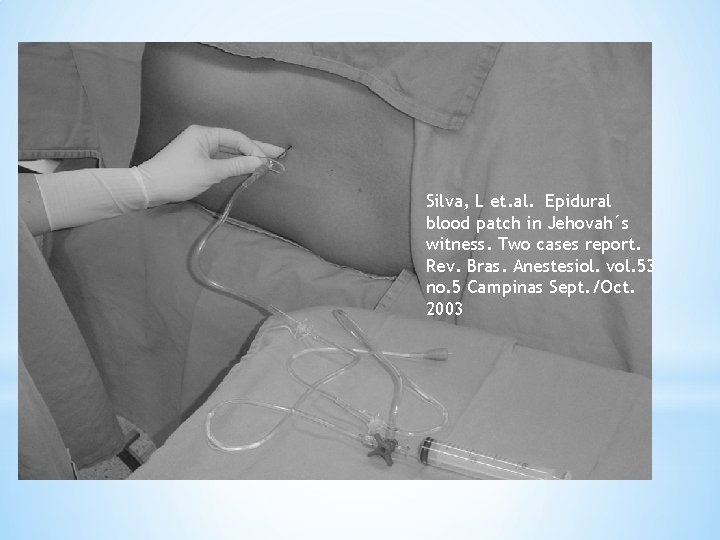
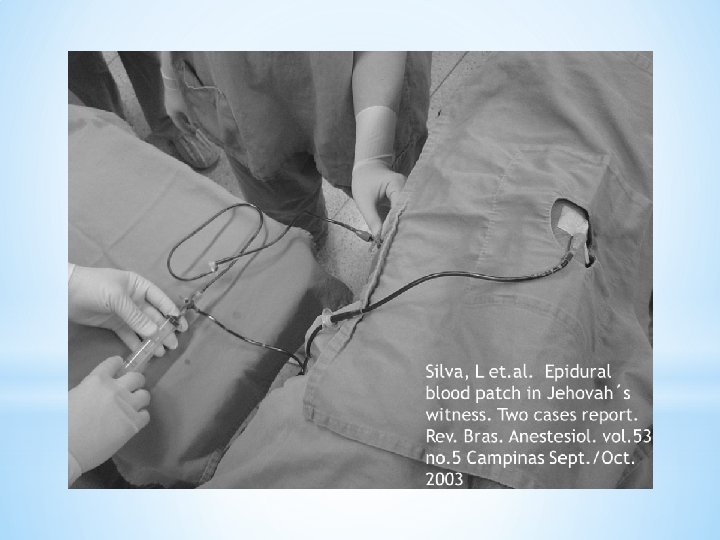
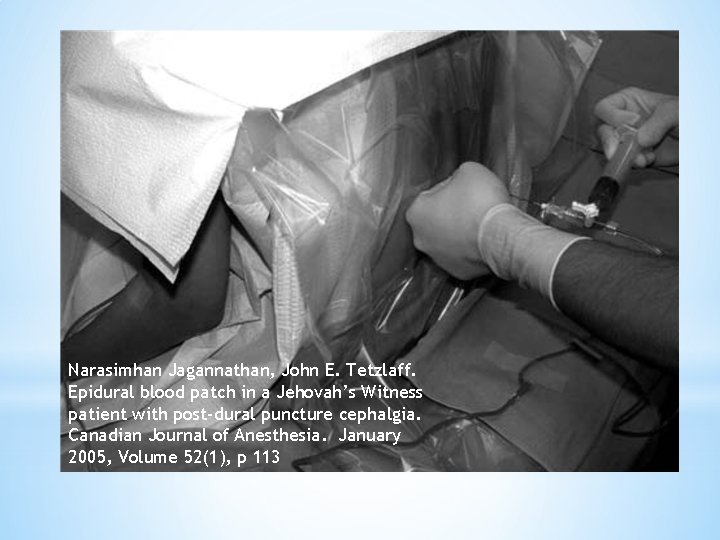
*What if cannot perform AEBP? ? *Anticoagulated patient *Patient Refusal *Sepsis *Jehovah Witness *Some JWs may allow AEBP *Consider closed loop system with stopcocks as a bypass technique. Primed with saline and continuous with patient’s circulation and epidural needle

Silva, L et. al. Epidural blood patch in Jehovah´s witness. Two cases report. Rev. Bras. Anestesiol. vol. 53 no. 5 Campinas Sept. /Oct. 2003

Silva, L et. al. Epidural blood patch in Jehovah´s witness. Two cases report. Rev. Bras. Anestesiol. vol. 53 no. 5 Campinas Sept. /Oct. 2003


Narasimhan Jagannathan, John E. Tetzlaff. Epidural blood patch in a Jehovah’s Witness patient with post-dural puncture cephalgia. Canadian Journal of Anesthesia. January 2005, Volume 52(1), p 113

*Sumatriptan: serotonin 1 -d receptor agonist *6 OB epidural wet tap patients with PDPH *30 mg subq injection in patients *Complete resolution of PDPH 4 of 6 in 30 min *2 of 6 required reinject on day 2 (1/2 life 2 hrs) *Asymptomatic yet at 5 -7 days *No reported side effects Carp H, et. al. Effects of the serotoninreceptor agonist sumatriptan on post-dural puncture headache: report of six cases. Anesth Analg. 1994; 79(1): 180– 182.

Cosintropin: synthetic form of ACTH *Useful in refractory PDPH: 1994 by Collier *Stimulates the adrenal gland to increase CSF production and β-endorphin output *0. 5 mg IV over 8 hours *Side effects similar to those of corticosteroids so caution in diabetics Carter BL, Pasupuleti R. Use of intravenous cosyntropin in the treatment of post-dural puncture headache. Anesthesiology. 2000

Cosintropin: Continued *Double Blind, randomized study: 33 pts *Compared with IV caffeine for initial treatment as alternative to AEBP *Caffeine-500 mg: 80% relief *Cosintropin-0. 75 mg: 56% relief *Lowered VAS from 8 to 3 both groups @ 2 hrs *Problems: No long term assessment, design problems, underpowered(type II error? . good pilot study Zeger W. et al. . Comparison of cosyntropin versus caffeine for postdural puncture headaches: A randomized double-blind World J Emerg Med, Vol 3, No 3, 2012

Last Ditch Alternatives: *Surgical Intervention: Dural patch. *Epidural Fibrin Glue Epidural Inj Patch : made of pooled human plasma clotting agents. *Dextran Colloid Epidural Patch: Successful case reports with 56 pts 100% relief but quite antigenic. Barrios-Alarcon (1989) *Corticosteroids: Anecdotal – increase CSF?

For those who stayed awake, I salute You

Lambert DH, et. al. Role of needle gauge and tip configuration in the production of lumbar puncture headache. Regional Anesthesia. 1997 Jan-Feb; 22(1): 66 -72. Vallejo MC, et. al. Postdural puncture headache: a randomized comparison of five spinal needles in obstetric patients. Anesthesia and Analgesia. 2000 91(4): 916 -20. Ready LB, et. al. Spinal Needle Determinants of rate of Transdural Leak. Anesthesia and Analgesia. 1989. 69: 457 -60. Reina MA , et. al. An In Vitro Study of Dural Leasions Produced by 25 Gauge Quincke and Whitacre Needles Evaluated by Scanning Electron Microscopy. Regional Anesthesia & Pain Medicine. 25(4): 393 -402, July/August 2000. Reina MA , et. al. Dura-arachnoid lesions produced by 22 gauge Quincke spinal needles during a lumbar puncture. J Neurology Neurosurg Psychiatry 2004; 75: 6 893 -897.

Barrios-Alarcon J, et. al. Relief of post-lumbar puncture headache with epidural dextran 40: a preliminary report Regional Anesthesia. 1989 Mar-Apr; 14(2): 78 -80. Camann WR, Murray RS, Mushlin PS, Lambert DH. Effects of oral caffeine on postdural puncture headache. A double-blind, placebocontrolled trial. Anesth Analg. 1990 Feb; 70(2): 181 -4. Carter BL, Pasupuleti R. Use of intravenous cosyntropin in the treatment of post-dural puncture headache. Anesthesiology. 2000; 92(1): 272– 274 Safa-Tisseront V, Thormann F, Malassine P, et al. Effectiveness of epidural blood patch in the management of post-dural puncture headache. Anesthesiology. 2001; 95(2): 334– 339. Carp H, et. al. . Effects of the serotonin receptor agonist sumatriptan on post-dural puncture headache: report of six cases. Anesth Analg. 1994; 79(1): 180– 182.

Zeger W. et al. . Comparison of cosyntropin versus caffeine for postdural puncture headaches: A randomized double-blind World J Emerg Med, Vol 3, No 3, 2012 Martin R, et. al. Duration of decubitus position after epidural blood patch. Can J Anaesth. 1994 Jan; 41(1): 23 -5. Ghaleb A et. al. Post Dural Puncture Headache. International Journal of General Medicine. 2012: 5 45– 51. Silva, L et. al. Epidural blood patch in Jehovah´s witness. Two cases report. Rev. Bras. Anestesiol. vol. 53 no. 5 Campinas Sept. /Oct. 2003 Ayad S, et al. . Subarachnoid catheter placement after wet tap for analgesia in labor: influence on the risk of headache in obstetric patients. . Regional Anesthesia and Pain Medicine. 2003 Nov-Dec; 28(6): 512 -5 Narasimhan Jagannathan, John E. Tetzlaff. Epidural blood patch in a Jehovah’s Witness patient with post-dural puncture cephalgia. Canadian Journal of Anesthesia. January 2005, Volume 52(1), p 113