Post cesarean Infection Mahin Jamshidi MD Professor Of




















































- Slides: 58

Post cesarean Infection Mahin Jamshidi MD Professor Of Infectious Disease IRAN UNIVERSITY OF MEDICAL SCIENCES 2019

Background Surgical site infection (SSI) is the most common complication post cesarean delivery The rate of SSI ranges from 3% to 15% worldwide. infection occurring within 30 days from the operative procedure in the part of the body where the surgery took place.

Background The risk for developing SSI has significantly decreased in the last three decades, Improvements in hygiene conditions, Antibiotic prophylaxis Sterile procedures Despite this decrease, the occurrence of SSI is expected to increase given the continuous rise in the incidence of cesarean deliveries.

Genitourinary tract microbiology Gram positive aerobic Gram negative aerobic Anaerobic Mycoplasma Other GBS E. coli Peptostreptococ cus Mycoplasma Chlamydia S. auerus Klebsiella Peptococcus Ureaplasma Enterococcu s Proteus Bacteroides Pseudomonas Gardnerella Enterobacter Colestridium Gibbs, Am J Obstet Gynecol 1987

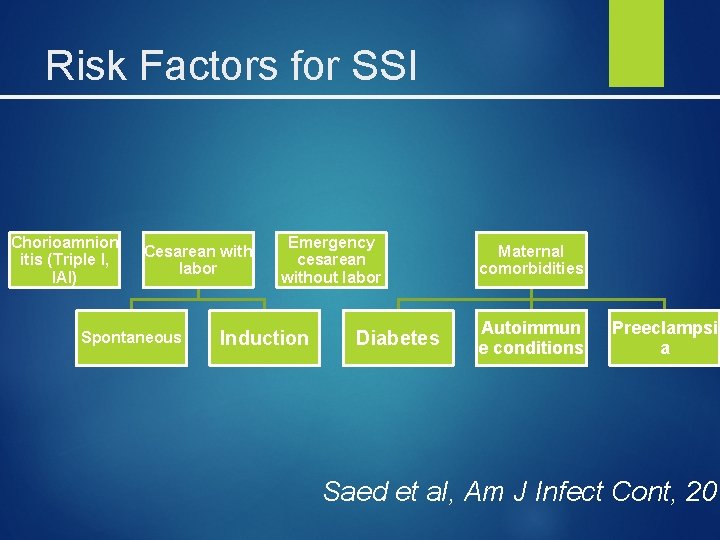
Risk Factors for SSI Chorioamnion itis (Triple I, IAI) Cesarean with labor Spontaneous Emergency cesarean without labor Induction Diabetes Maternal comorbidities Autoimmun e conditions Preeclampsi a Saed et al, Am J Infect Cont, 201

Risk Factors for SSI ●Prolonged labor ●Prolonged rupture of membranes ●Multiple cervical examinations ●Internal fetal or uterine monitoring ●Large amount of meconium in amniotic fluid ●Manual removal of the placenta ●Low socioeconomic status ●Operative vaginal delivery ●HIV infection ●Colonization with group B Streptococcus ● Bacterial vaginosis

Definition Of SSI It divides SSIs into: incisional SSI organ/space SSI. Incisional SSI : superficial, involving the skin and subcutaneous tissue deep SSI, involving fascial and muscle layers.

organ/space SSI. Endometritis Septic thrombophlebitis Abdominal abscess

Post cesarean infectious SSI includes Wound infection Endometritis Necrotizing fasciitis Septic thrombophlebitis

outside uterine Infection UTI Aspiration Pneumonia…

wound infection Clinical manifestations Symptoms include localized erythema, induration, warmth, and pain at the incision site. Purulent wound drainage and separation of the wound. systemic fever and leukocytosis. diagnosis of wound infection is clinical.

Endometritis Postpartum endometritis refers to infection of the decidua It is a common cause of postpartum fever and uterine tenderness

Endometritis The potential for infection is enhanced at least 10 -fold in cesarean deliveries compared with vaginal births because of the presence of foreign bodies (eg, suture material), myometrial necrosis at the suture line, and formation of hematomas and seromas.

Epidemilogy the frequency of postpartum endometritis is 11 percent for cesareans performed after the onset of labor and 1. 7 percent for those performed electively Cesarean

Late onset postpartum endometritis Most cases of endometritis develop within the first week after delivery 15 percent present between one and six weeks postpartum Delayed presentation is more common after vaginal than cesarean delivery, and may present as late postpartum hemorrhage

Endometritis Mild and cured with antibiotic therapy, extension of infection to the peritoneal cavity can result in peritonitis, intraabdominal abscess, or sepsis. Necrotizing myometritis, necrotizing fasciitis of the abdominal wall, septic pelvic thrombophlebitis, and toxic shock syndrome are rare complications.

CLINICAL FINDINGS Endometritis Postpartum fever, tachycardia that rise in temperature, midline lower abdominal pain, and uterine tenderness. Purulent lochia, chills, headache, malaise, and/or anorexia are additional findings observed in some women excessive uterine bleeding

Endometritis with toxic shock syndrome Although rare, clostridia, streptococci, and staphylococci can lead to endometritis with toxic shock syndrome and other serious complications (eg, necrotizing myometritis, necrotizing fasciitis). This diagnosis is made in the following settings:

Group. A Streptococcus (GAS) patients with early-onset infection (within the first 48 hours postpartum) High fever (>38. 5°C). Hypotension Involvement of at least two other organ systems (eg, renal, liver, or pulmonary insufficiency; coagulopathy; soft tissue necrosis; erythematous macular rash with desquamation) suggests toxic shock syndrome.

Staphylococcal toxic shock syndrome High fever >38. 9°C, hypotension, diffuse erythroderma, desquamation involvement of at least three organ systems. Onset may be early (within 24 hours of delivery) and difficult to distinguish from GAS toxic shock.

C. sordellii lethal toxic shock-like syndrome. less than one week postpartum when they had sudden onset of clinical shock: Progressive, Refractory hypotension Massive and generalized tissue edema, hemoconcentration, Marked leukemoid reaction (total neutrophil count 66, 000 to 93, 600/mm 3), Absence of rash or fever, limited or no myonecrosis, and a rapidly lethal course.

C. perfringens has been found in necrotizing endomyometritis and fatal toxic shock after medical abortion Should be considered in patients who rapidly become gravely ill with evidence of intravascular hemolysis that can be extreme. It can cause Clostridial myonecrosis (gas gangrene), a life-threatening muscle infection that can be identified by radiographic imaging.

Diagnostic criteria for postpartum endometritis clinical postpartum fever that cannot be attributed to another etiology after a thorough history and physical examination. oral temperature of ≥ 38. 0°C (≥ 100. 4°F) on any two of the first 10 days postpartum, Exclusive of the first 24 hours low grade fever during this period is common and often resolves spontaneously, especially after vaginal birth.

The presence of one or more of the clinical findings described above (eg, tachycardia, midline lower abdominal pain, uterine tenderness, leukocytosis) supports the diagnosis, but these findings are nonspecific. In particular, variable degrees of midline abdominal pain, uterine tenderness, and leukocytosis are common after cesarean delivery, and to a lesser extent after vaginal delivery, in the absence of infection. Some degree of malodorous yellow-red lochia is also normal after any delivery

Diagnostic criteria for postpartum endometritis The presence of "Maternal Early Warning Criteria" (table 1) suggests that the patient is at risk for serious maternal morbidity and mortality and should be evaluated promptly Sepsis should be considered in these critically ill women, even if afebrile

Maternal Early Warning Criteria BP <90 HR>120 RR>30 Urin out put < 350 cc 2 hrs O 2 Saturation <95%

ROLE OF CULTURES Blood(immunocompromised, septic, or fail to respond to empiric therapy) Cervix – Cervical specimens for gonorrhea and chlamydia testing is not indicated Endometrium – Endometrial cultures are not performed routinely because of the difficulty in obtaining an uncontaminated specimen through the cervix Urin -Absess

Necrotizing fasciitis is a rare but serious infection causing significant morbidity after CD Necrotizing fasciitis is suspected with: severe pain, crepitus, wooden-hard induration of the subcutaneous tissues, bullous lesions, skin necrosis or ecchymosis, and elevated serum creatine kinase level; a hallmark of necrotizing

Necrotizing fasciitis Diagnosis fasciitis is rapid progression of clinical manifestations Imaging studies such as computed tomography or magnetic resonance imaging may show edema extending along the fascial plane The diagnosis is confirmed at the time of repeat surgery

Septic pelvic thrombophlebitis (SPT) is a rare condition that occurs in the setting of pelvic vein, endothelial damage venous stasis, hypercoagulability

SPT can present with two somewhat distinctive syndromes. Ovarian vein thrombophlebitis usually ill, fever and abdominal pain within one week after delivery or surgery; thrombosis of the ovarian vein (usually on the right side) can sometimes be visualized radiographically.

Patients with deep SPT present more subtly Isolated fever in the early postpartum or postoperative period Do not have abdominal or pelvic tenderness Radiographic imaging typically does not identify thrombosis of a specific vein

Septic pelvic thrombophlebitis SPT should be suspected in patients who have persistent fever despite antibiotic therapy (usually for presumptive endometritis or other pelvic infection) in the few weeks following vaginal delivery, cesarean delivery, or pelvic surgery

TREATMENT Intravenous regimens Clindamycin 900 mg every eight hours PLUS Gentamicin 5 mg/kg every 24 hours (preferred) OR 1. 5 mg/kg every 8 hours cefotetan, cefoxitin, ceftizoxime, piperacillin with or without tazobactam, and ampicillin-sulbactam ] the initial antibiotic choice in some hospitals.

TREATMENT Metronidazole provides good activity against most anaerobes and can be useful with ampicillin and gentamicin, but is not the preferred choice for breastfeeding women if a drug with a better safety profile is available.

GBS positive patients Resistance to clindamycin in invasive GBS isolates ranges from 13 to 43 percent For those patients who are known to be colonized with GBS as a result of universal screening, Addition of ampicillin to a clindamycin- plus-gentamicin regimen or use of ampicillin-sulbactam (3 g IV every six hours) is recommended.

Bacteroides fragilis clindamycin resistance — In geographic regions or institutions where B. fragilis has significant clindamycin resistance, ampicillin-sulbactam (3 g IV every six hours) is a reasonable alternative

Duration IV Therapy Intravenous treatment until the patient is clinically improved (no fundal tenderness) and afebrile for 24 to 48 hours. Oral antibiotic therapy after successful parenteral treatment is not required

Oral and intramuscular regimens Clindamycin 600 mg orally every 6 hours plus gentamicin 4. 5 mg/kg intramuscularly every 24 hours OR ●Amoxicillin-clavulanic acid 875 mg orally every 12 hours OR ●Cefotetan 2 g intramuscularly every 8 hours OR ●Meropenem or imipenem-cilastatin 500 mg intramuscularly every 8 hours OR ●Amoxicillin 500 mg plus metronidazole 500 mg orally every 8 hours

Duration Oral Therapy 14 day. If an intramuscular antibiotic regimen is used, we suggest 48 to 72 hours of intramuscular therapy then switch to an oral antibiotic to complete a seven day course.

Persistent postpartum fever resistant organisms Vancomycin Other etiologies of fever physical examination to look for non-uterine sources of infection and worsening pelvic findings (eg, new mass, worsening pain). Imaging. Sonography is useful for visualizing pelvic abscesses and fluid collections, but insensitive for diagnosis of septic pelvic thrombophlebitis or ovarian vein thrombosis where computed tomography (CT) or magnetic resonance imaging (MRI) are more helpful.

Relapse of endometritis — For patients who present with recurrent signs/symptoms of endometritis after having been treated for endometritis on initial hospitalization, we suggest change of antibiotics from the initial regimen and further evaluation, as outlined above.

SPT Treatment We suggest systemic anticoagulation for patients with suspected, presumptive, or documented SPT). The duration of anticoagulation depends on the clinical presentation. For patients who do not have documented thromboses or underlying hypercoagulable state, we discontinue anticoagulation 48 hours after the resolution of fever For patients who have radiographic evidence of pelvic branch vein thromboses, we continue anticoagulation for at least two weeks. For patients who have radiographic evidence of extensive pelvic thromboses (eg, thrombosis involving the ovarian vein, iliac veins, or vena cava) or septic emboli, we continue anticoagulation for at least six weeks

Prophylaxis Preoperative vaginal prep Pre-incision antibiotics Gentle cord traction vs. manual removal Subcutaneous closure > 2 cm Suture skin closure Antibiotics in special circumstances CS after labor, ROM Obesity Chorioamnionitis (Triple I, etc. ) Sood, Curr Opin Infect Dis 2018,

Pre-incision Antibiotics • Therapeutic tissue levels at time of microbial contamination • Agent of choice − Long acting − Narrow focus on likely bacteria − Inexpensive − Few adverse effects

Antibiotics for Cesarean 1 st generation cephalosporin is first line for all patients undergoing CS < 60 mins prior to incision 1 g for patients < 80 kg 2 g for patients > 80 kg 3 g considered for patients > 120 kg Azithromycin for non-elective CS MRSA – add vancomycin to preop abx IAI Give one dose after CS Add clindamycin or metronidazole

Standard Antibiotic Prophylaxis for CS Cefazolin 1 g IV for patients < 80 kg Timing < 60 min before incision Re-dose Surgery more than 4 hours Blood loss greater than 1500 ml Allergy Clindamycin 900 mg Gentamycin 5 mg/kg Multi dose No ACOG, PB 132, 2018

Adjunctive Azithromycin for non-elective cesarean

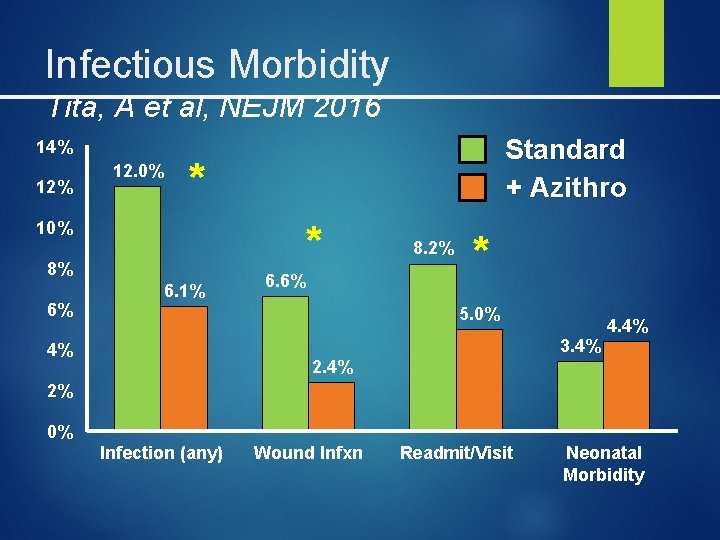
Infectious Morbidity Tita, A et al, NEJM 2016 14% 12. 0% Standard + Azithro * 10% * 8% 6% 6. 1% 6. 6% 8. 2% * 5. 0% 4. 4% 3. 4% 4% 2% 0% Infection (any) Wound Infxn Readmit/Visit Neonatal Morbidity

Post-cesarean Oral Antibiotics RCT of PO cephalexin & metronidazole vs placebo for prevention of SSI in women with BMI > 30 Cefazolin 500 mg + metronidazole 500 mg or placebo Q 8 hours for 48 hours Standard preoperative IV antibiotics Primary outcome superficial incisional, deep incisional, or organ space infections Stratified by membrane status Mean BMI 40

Post-Cesarean Cephalexin and Metronidazole Ruptured Membranes C/M (n = 63) Placebo (n = 63) RR (95% CI) P SSI 6 (9. 5) 19 (30. 2) 0. 31(0. 13 -0. 71) . 008 C/M Placebo (n = 139) RR (95% CI) P 12 (8. 7) 0. 58 (0. 24 -1. 44) . 47 Intact Membranes SSI (n = 138) 7 (5. 0) Valent et al. JAMA 2017

Vaginal Cleansing Meta-analysis and Systematic Review, 2017 Vaginal Cleansing Controls RR (95% CI) Endometritis 4. 5% 8. 8% 0. 52 (0. 37– 0. 72) Postoperative fever 9. 4% 14. 9% 0. 65 (0. 50– 0. 86) Outcomes Vaginal cleansing resulted in less endometritis among subgroups Laboring patients Patients with ROM Povidone-iodine solution (not CHX) Preoperative antibiotics

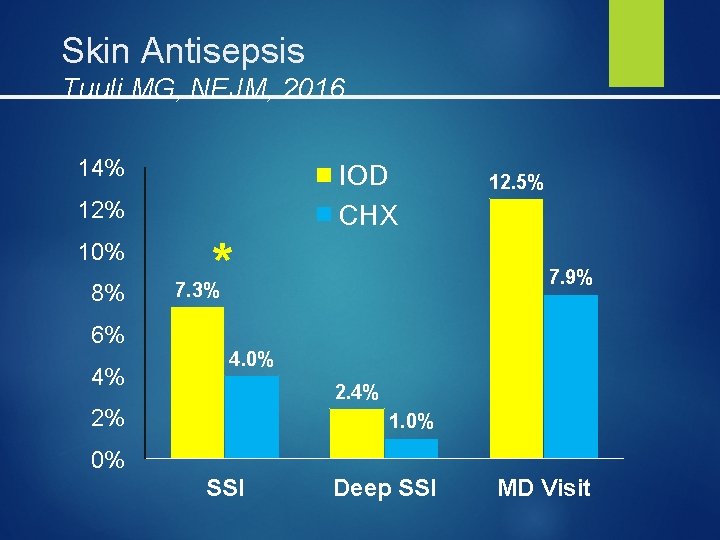
Skin Antisepsis Tuuli MG, NEJM, 2016 RCT of chlorhexidine alcohol vs iodine-alcohol 572 women in CXH group 575 in IOD group Primary outcome Superficial or deep wound infection within 30 days

Skin Antisepsis Tuuli MG, NEJM, 2016 14% IOD CHX 12% 10% 8% 6% 4% * 12. 5% 7. 9% 7. 3% 4. 0% 2. 4% 2% 1. 0% 0% SSI Deep SSI MD Visit

Peri-operative antibiotics for Cesarean in the setting of Triple I, IAI, Chorioamnionitis

Cesarean Prophylaxis and IAI If the patient is already receiving broad spectrum antibiotics for another indication (IAI, pyelo, etc), additional cefazolin is not necessary One additional dose of chosen regimen should be given after cesarean PLUS Clindamycin 900 mg IV or metronidazole 500 mg IV for at least one dose ACOG CO 712, 2017 ACOG PB 199, 2018

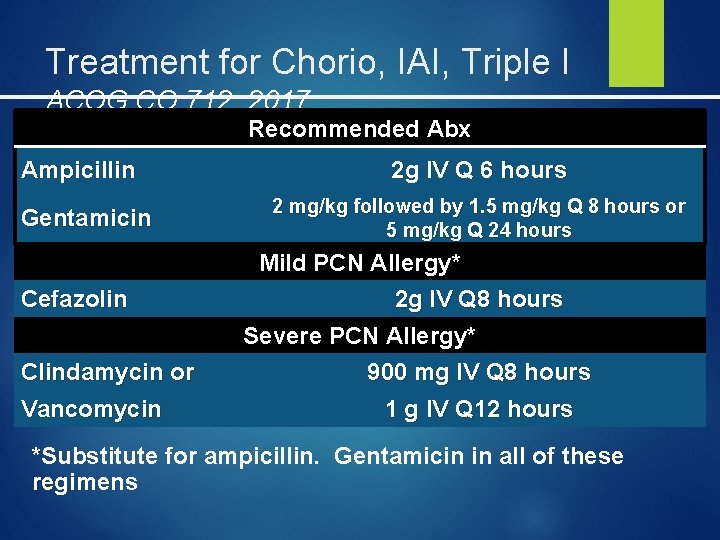
Treatment for Chorio, IAI, Triple I ACOG CO 712, 2017 Recommended Abx Ampicillin Gentamicin 2 g IV Q 6 hours 2 mg/kg followed by 1. 5 mg/kg Q 8 hours or 5 mg/kg Q 24 hours Mild PCN Allergy* Cefazolin Clindamycin or Vancomycin 2 g IV Q 8 hours Severe PCN Allergy* 900 mg IV Q 8 hours 1 g IV Q 12 hours *Substitute for ampicillin. Gentamicin in all of these regimens

Treatment for Chorio, IAI, Triple I ACOG CO 712, 2017 Alternative Regimens Ampicillin/Sulbactam Piperacillintazobactam 3 g IV Q 6 hours 3. 375 Q 6 hours or 4. 5 g Q 8 hours Cefotetan 2 g IV Q 12 hours Cefoxitin 2 g IV Q 8 hours Ertapenum 1 g IV Q 24 hours