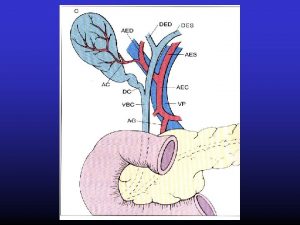
Porfyriny luov barviva Hb Porphyrins bile pigments Hb

Porfyriny, žlučová barviva, Hb Porphyrins, bile pigments, Hb Prof. Dr. V. Pelouch, CSc.

Syntéza porfyrinů a Hb Synthesis of porphyrins and Hb

Syntéza Hb • Začíná v mitochochondrii kondensací sukcinyl. Ko. A (z KC) a glycinu → NÁSLEDUJE – dekarboxylace a tvorba δaminolevulinatu • 2 δ aminolevulinate přechází do cytosolu → tvoří se porfobilinogen Synthesis of Hb • First reaction in mitochondria: condensation of succinyl. Co. A (from KC) and glycine → NEXT REACTION – decarboxylation and formation of δ- aminolevulinate • 2 δ aminolevulinate is transfered into cytosol → formed porfobilinogene




Další reakce • 4 porfobilinogen → lineární tetrapyrol → uroporfylinogen → coproporfylinogen (cytosol) → in mitochondria: protoporfylinogen → proto-porfylin → incorpo-race Fe → Hb • Postranní řetězce: A (acetyl) se dekarboxylací mění na M (metyl), P (propionyl) dekarbox. a dehydrogen. na V (vinyl) Next reactions • 4 porfobilinogen → linear tetrapyrrol → urophorfylinogen → cophroporfylinogen (cytosol) → in mitochondria: protoporfylinogen → protophofylin → incorporation of Fe → Hb • Side chains: A (acetyl) are changed by decarboxylation to M (metyl) and P (propionyl) by decarb. and dehydrogenation to V (vinyl)

Heme biosynthesis • Almost 85% of heme biosynthesis occurs in the bone marrow, • much smaller percentage in liver. • Both the mitochondria and cytoplasm are involved in this pathway

Degradace porfyrinů Degradation of porphyrins

DEGRADATION of Hb • Globin is removed, • red heme is degradated in endoplasmic reticulum (liver, spleen, bone marrow) by NADPH oxygenase • biliverdin and bilirubin are produced • Transport of bilirubin (in binding to albumin) into hepatocytes • Conjugation • Transport in bile (= gall)

DEGRADACE Hb • Globin je odstraněn • Červený hem je degradován v endoplasmatickém retikulu (játra, slezina, kostní dřeň) pomocí NADPH oxygenasy • biliverdin a bilirubin vznikají • Transport of bilirubinu (ve vazbě na albumin) do hepatocytů • Konjugace • Transport ve žluči

Degradation of Hb Icterus: pre-, intra- and posthepatal origin

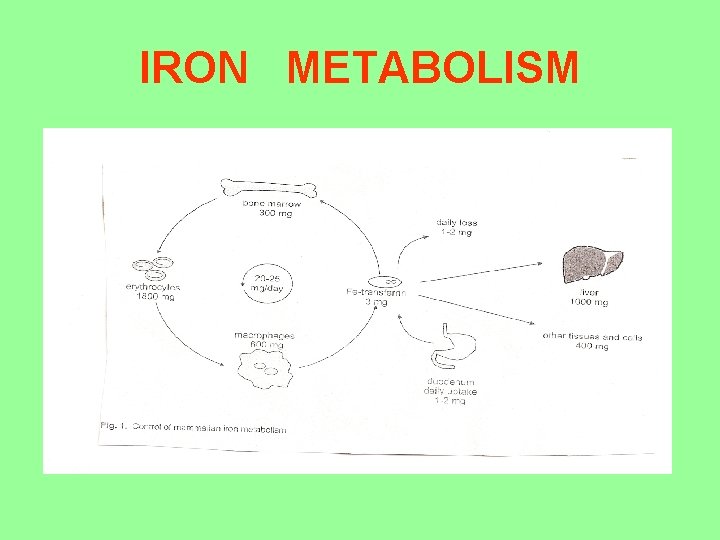
IRON METABOLISM

Text to previous slide: Control of mammalian iron metabolism • Transport molecule of iron is transferrin (glycoprotein, m. w. 80 k. Da – contains two binding sites - both sites are structural very similar, functional different; under physiological state: only about 30% are occupied). • High level of iron in body (all positions are occupied) then, non- transferrinbound iron appears.

IRON • Iron is localized in hemoproteins: Hb, Hb ferritin transport protein - quantity - see two next slides, myoglobin, cytochromes - see also previous slide, furthermore, aconitase (enzyme from Krebs cycle, here: Fe - ions are bound to S), NADPH – oxidase • Toxic effect of iron: iron (Haber –Weiss- Fenton reactions) Fe 2+ + O 2 → Fe 3+ +. O 22. O 2 - + 2 H+ → H 2 O 2 + 2 O 2 Fe 2+ + H 2 O 2 → Fe 3+ +. OH + OH • Formation of hydroxyl radical =. OH, it means the production of free radicals – see special lecture for details • Inhibition of oxidation of Fe 2+ to Fe 3+ is done by either with ceruloplasmin, ceruloplasmin or by binding of Fe 2+ to tranferrin, ferritin, lactoferrin or iron chelatation


Text to next slide • Fig. 2 (lower) - Intestinal iron uptake; iron from nutrition is absorbed to enterocytes of duodenum in both heme form (from animal sources) via heme carrier protein HCP in enterocates is degradated by hemeoxygenase 1: HO -1 and nonheme form (from plants) via DMT 1 – divalent metal transporter after their reduction by duodenum cytochrome b-like ferrireductase (Dcytb) in the presence of ascorbic acid or some AAs (cystein, histidin) • Fig 3 (upper) - Recirculation of erythocytes iron in macrophage, Ery - life span 120 days, then Ery in reticulo-endothelial system of macrophages degradated, Hb is released: globin (Gb) and heme structure persisted; releasing of Fe 2+ is done by DMT 1 (divalent metal transporter - intracellular pool of iron. In plasma is bound to haptoglobin (Hp), into cell is transfered by receptor CD 136 where iron is release by hemoxygenase HO 1

Recirculation of erythrocyte Fe in macrophage (fig. 3) Intestinal Fe uptake (fig. 2)

Haptoglobin (Hp) Glycoprotein (two α chains, two β chains): is formed in liver Haptoglobin bound Hb and complex (C) arised: Hp-Hb C is removed from blood stream by RES Physiological role: probably block again formation of hydroxyl radical (. OH) - see oxidation of iron

Bilirubin • Bilirubin (B) je vázán na albumin (1 vysoko- a 1 nizkoaffinitní místo: 25 mg B/ 100 ml plasma • 1 g Hb = 35 mg B, produkce: 250 - 350 mg B/den Dva typy B: • Přímý B = konjugovaný • Nepřímý B = nekonjugovaný • Bilirubin (B) is bound to albumin (1 high, and 1 low-affinity sites: 25 mg B /100 ml of plasma • 1 g Hb =35 mg B, production: 250 - 350 mg B/day Two types of B: B • Direct B = conjugated • Indirect B = unconjugated


Clinical Serum B total up 1 mg/d. L direct 0, 1 -0, 4 Indirect 0, 2 -0, 7 1 mg =17, 1μmol/l i c t hemolytic ↑ indirect hepatitic ↑ dir, ind obstruct ↑ dir • aspects Urine fecal B urobilinogen absent 0 -4/24 h 40 -280/24 h e r u s = žloutenka absent ↑ ↑ present ↑ ↓ present absent trace to 0 δ –bilirubin (= high direct B then arised covalent binding between direct B and albumin - longer life time than conventional direct B) Most of colorless urobilinogens formed in colon by fecal flora are oxidized to urobilinins (darkening of feces upon air is due to oxidation of residual urobilinogens)


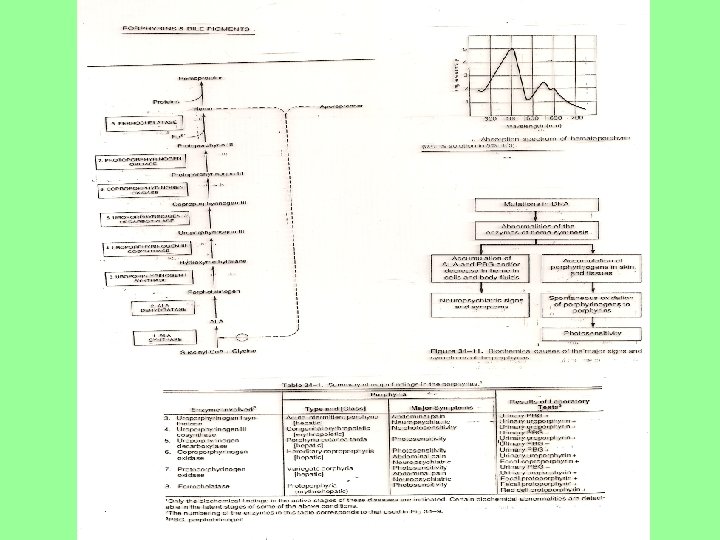
Gene determined abnormalitites • Fotosensitivita a neurologické problémy jsou projevem tohoto onemocnění • Erytrocyty a játra jsou hlavní místem metabolických vyjádření porfyrií. • Photosensitivity and neurological problems are common complaints. • Erytrocytes and liver are main places of metabolic disorders of porphyrias.

Further information • Series of hereditary and acquired diseases – porphyrias = disturbances in porphyrin metabolism • Several of these disorders – excretion of heme precursors in the stool or urine - giving them dark collor • Accumulation of porphyrins in the skin – exposure to light causes disfiguring (znetvoření, zohyzdění), poorly - healthing blisters (puchýře) • Neurological disturbances • Human vampiers – porphyria sufferers (lights shynness, bizare appearance, drinking of blood – to compensate heme deficinecy)

Bile pigments x bile acids !!! • Bile pigments: bilirubin, biliverdin (metaloproteins) • Bile acids: primary (cholic a. cholate and in weakly alkaline p. H of bile as anion – cholate), secondary acids (deoxycholic, lithocholic ) (steroid structure derived from cholesterol) Žlučová barviva Žlučové kyseliny!!! • Žlučová barviva: bilirubin, biliverdin (metaloproteiny) • Žlučové kyseliny: primarní (cholová k. • v slabě alkalickém p. H žluči jako anion – cholat), sekundární (deoxycholová, lithocholová) (steroidní struktura odvozená od cholesterolu)
- Slides: 28