PopulationBased Payments LAN Learnings Webinar November 10 2015

Population-Based Payments: LAN Learnings Webinar November 10, 2015 1: 00 – 2: 15 pm EDT

2 Welcome Anne Gauthier LAN Project Leader, CMS Alliance to Modernize Healthcare (CAMH) Elizabeth Mitchell President and CEO, Network for Regional Healthcare Improvement (NRHI) Guiding Committee Member For Public Distribution

3 Agenda For Public Distribution

4 Stakeholder Event • Over 450 participants • Positive feedback from participants • Presentations are posted online http: //www. lansummit. org • Twitter tells the story https: //storify. com/Payment_N etwork/lan-summit-2015 For Public Distribution

5 Draft APM Framework White Paper What feedback are we seeking? • the overall White Paper and proposed framework; • descriptions associated with each category; • the boundaries that differentiate one category from another; and • additional examples and case studies you can provide to illustrate and test each category in the framework. For Public Distribution Feedback by November 20 th • online via Handshake; or • by email to Payment. Network@MITRE. org
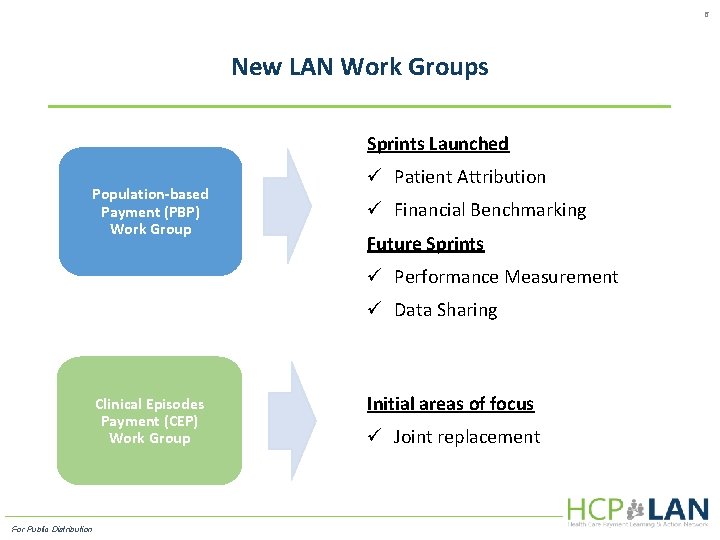
6 New LAN Work Groups Sprints Launched Population-based Payment (PBP) Work Group ü Patient Attribution ü Financial Benchmarking Future Sprints ü Performance Measurement ü Data Sharing Clinical Episodes Payment (CEP) Work Group For Public Distribution Initial areas of focus ü Joint replacement

7 LAN Communications Join work group affiliated communities to provide input on work group products Keep updated on the latest LAN info through our newsletter Visit the LAN website to learn more and find resources https: //publish. mitre. org/hcplan For Public Distribution

8 Q & A What questions do you have about the Guiding Committee report? Use the chat window in your webinar dashboard For Public Distribution

9 PANEL: Population-Based Payment Approaches Robert Mc. Conville Director of Population Health, Intermountain Healthcare Kerry Snyder Director of Health Informatics, Populytics, Inc. For Public Distribution David Muhlestein Senior Director of Research and Development, Leavitt Partners Allison Yudt Director of Value. Based Contracts, Populytics, Inc.

10 PANEL: Population-Based Payment Approaches Robert Mc. Conville Director of Population Health, Intermountain Healthcare For Public Distribution

LAN Summit: Population-Based Payment Approaches October 26, 2015 Intermountain Healthcare: Aligning Provider Financial Incentives
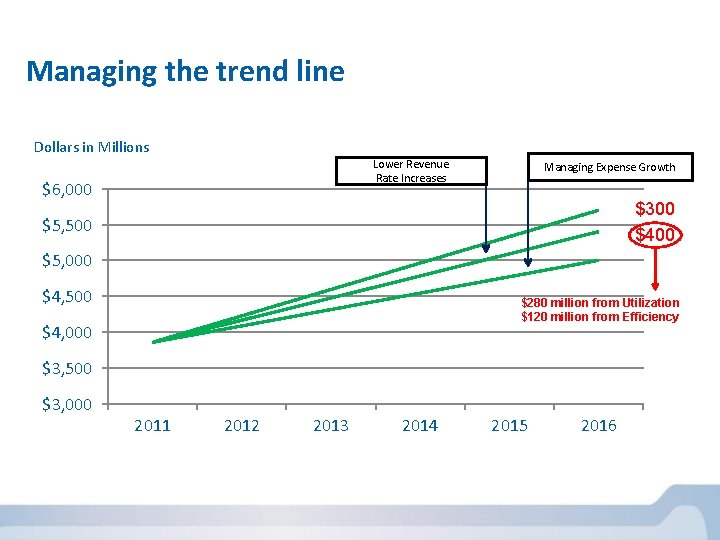
Managing the trend line Dollars in Millions Lower Revenue Rate Increases $6, 000 Managing Expense Growth $300 $400 $5, 500 $5, 000 $4, 500 $280 million from Utilization $120 million from Efficiency $4, 000 $3, 500 $3, 000 2011 2012 2013 2014 2015 2016

Aligning Financial Incentives Using Evidence-based Care Engaging Patients
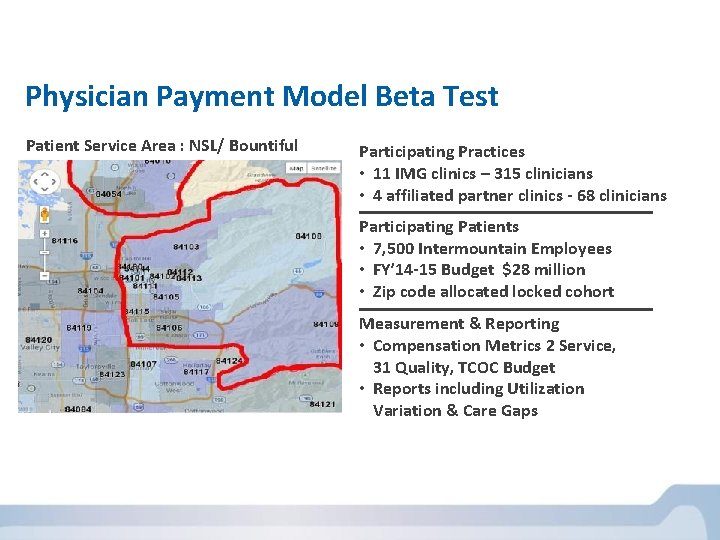
Physician Payment Model Beta Test Patient Service Area : NSL/ Bountiful Participating Practices • 11 IMG clinics – 315 clinicians • 4 affiliated partner clinics - 68 clinicians Participating Patients • 7, 500 Intermountain Employees • FY’ 14 -15 Budget $28 million • Zip code allocated locked cohort Measurement & Reporting • Compensation Metrics 2 Service, 31 Quality, TCOC Budget • Reports including Utilization Variation & Care Gaps *January 2014 projection

Guiding Principles: Quality Measure Selection 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. Simple Feasible and cost-effective Representative of clinical quality Outcomes-oriented Measures and targets will change over time Fully matured measures will be sunset Engagement from physician groups When feasible, should align with national measures Targets are thresholds, not percentiles Must be able to report measures © Intermountain Healthcare, 2013

Financial Incentives Guiding Principles 1. 2. 3. 4. 5. 6. 7. 8. Relatively simple to understand Relatively simple to manage (bias toward simplicity) Encourages decisions that add Value (Access, Quality, Cost) Discourages decisions that do not add Value Rewards are based on achieving thresholds rather than percentiles Transparency of calculation of shared savings Bias towards consistency across payers, markets, providers, etc. Incentives aligned for patients, hospitals, physicians, members, & purchasers 9. Promotes teamwork: “We’re all in this together” 10. Robust, dynamic, scalable © Intermountain Healthcare, 2013
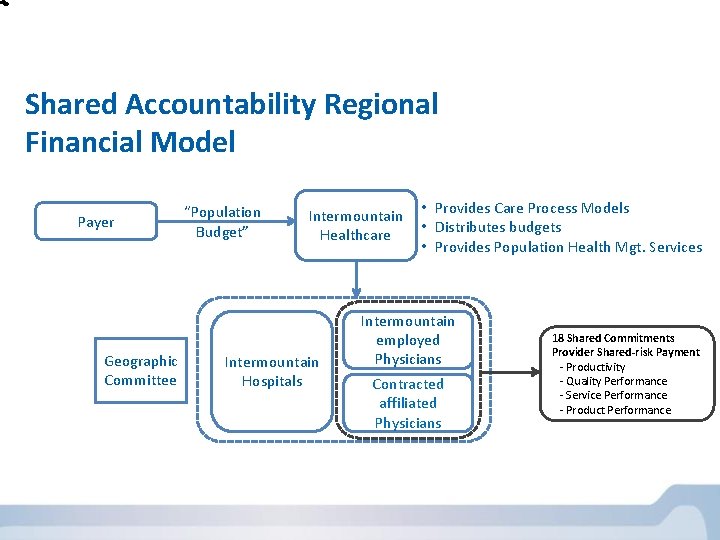
Shared Accountability Regional Financial Model Payer Geographic Committee “Population Budget” Intermountain • Provides Care Process Models • Distributes budgets Healthcare • Provides Population Health Mgt. Services Intermountain Hospitals Intermountain employed Physicians Contracted affiliated Physicians 18 Shared Commitments Provider Shared-risk Payment - Productivity - Quality Performance - Service Performance - Product Performance

2016 Physician Payment Model Available Productivity Quality Patient Experience Product Performance 2. 5% Total Payment 1/3 of Improvement * As quality and patient experience scores increase or product performance improves, total payment will increase Note: All performance payments are assessed at the group level * - capped at 12. 5%

Payer Strategy Medicare • Medicare Advantage – January 2013 • ACO – no thanks Medicaid • “ACO” model – January 2013 Commercial • – January 2016 • Followed by others

Lessons Learned… • • Invest in provider education and communication Develop guiding principles! Structure Business Intelligence to be simple & actionable Engage physicians in the development process from conception to realization Have agreement on definition and roles of data access Establish data governance Invest in provider to clinic mapping Build in enough time to get feedback from customers

Robert Mc. Conville Intermountain Healthcare Director of Population Health robert. mcconville@imail. org | 801. 442. 4561

22 PANEL: Population-Based Payment Approaches David Muhlestein Senior Director of Research and Development, Leavitt Partners

FIRST, KNOW THYSELF: HOW DIFFERENT TYPES OF PROVIDERS ARE ENGAGING – AND SUCCEEDING – IN ALTERNATIVE PAYMENT MODELS David Muhlestein, Ph. D, JD Senior Director of Research & Development Leavitt Partners @David. Muhlestein

AN ACO IS LIKE A UNICORN Or, if you’ve seen one ACO, you’ve seen one ACO Rather, ACOs are like animals… Each different, but similarities exist 24

DEVELOPMENT OF THE ACO TAXONOMY Goal to identify the structural differences of ACOs Integration Range of services directly furnished by the ACO Differentiation Total range of services either directly provided or through contracted provider Centralization Number of decision-makers that comprise the ACO 25
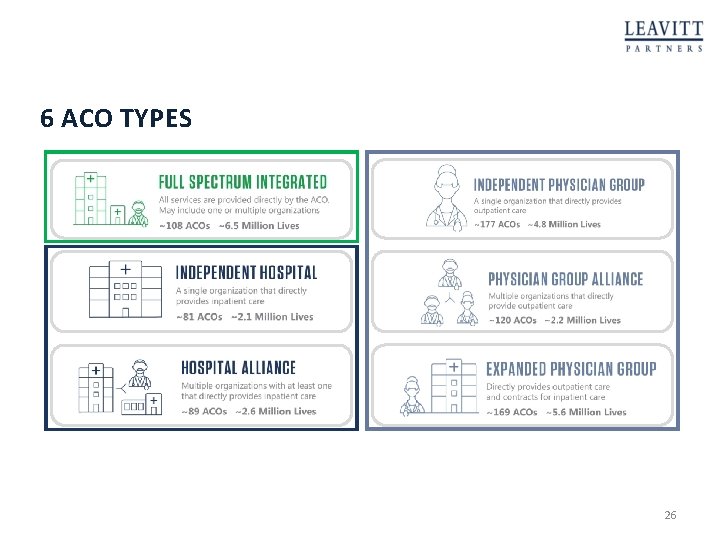
6 ACO TYPES 26

TAXONOMY LEARNINGS – CHALLENGES BY TYPE • Hospitals still viewed as revenue driver • Many moving parts, changes occur slowly • Reliance on inpatient revenue • Don’t provide as many subspecialty or post-acute care services • EMR interoperability is a hurdle given the multiple owner structure • Requires certain cultural compatibilities • Limited access to capital and heightened actuarial risk for losses given smaller patient populations • Limited ability to influence inpatient or post-acute care • Steep organizational learning curves • Increased time requirements & complexities to integrate care coordination programs • Barriers to establishing operational arrangements with hospitals • Often include multiple disparate EMR platforms 27
Polling Question WHICH OF THE SIX ACO TYPES IS BEST POSITIONED TO ACHIEVE THE TRIPLE AIM? A. D. B. E. C. F. 28
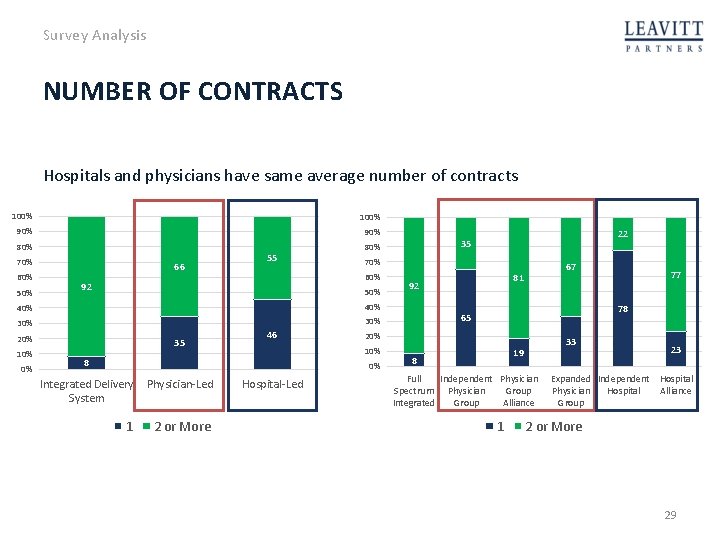
Survey Analysis NUMBER OF CONTRACTS Hospitals and physicians have same average number of contracts 100% 90% 80% 70% 60% 50% 66 55 50% 20% 0% 35 46 20% 10% 8 0% Integrated Delivery Physician-Led System 1 2 or More Hospital-Led 77 78 65 30% 67 81 92 40% 10% 70% 60% 92 22 35 33 19 8 Full Independent Physician Spectrum Physician Group Integrated Group Alliance 1 23 Expanded Independent Hospital Physician Hospital Alliance Group 2 or More 29
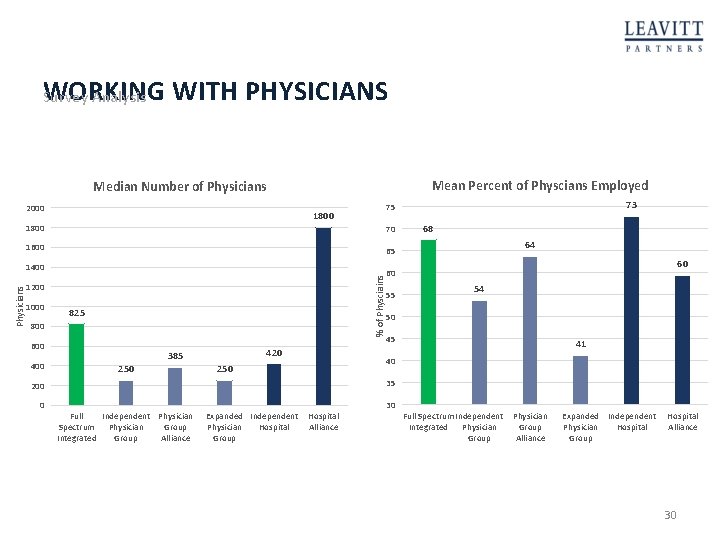
WORKING WITH PHYSICIANS Survey Analysis Mean Percent of Physcians Employed Median Number of Physicians 2000 1800 70 1600 % of Physciains Physicians 55 825 60 54 50 800 45 600 420 385 250 41 40 35 200 0 64 60 1200 400 68 65 1400 1000 73 75 30 Full Independent Physician Spectrum Physician Group Integrated Group Alliance Expanded Independent Hospital Physician Hospital Alliance Group Full Spectrum Independent Physician Integrated Physician Group Alliance Expanded Independent Physician Hospital Group Hospital Alliance 30
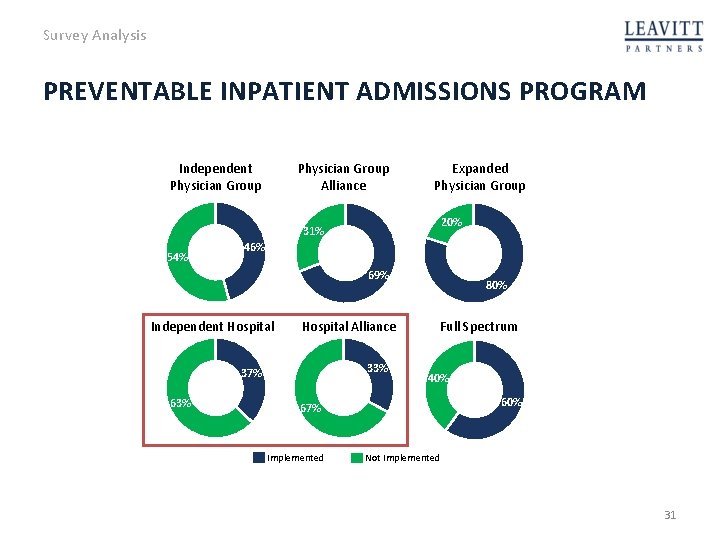
Survey Analysis PREVENTABLE INPATIENT ADMISSIONS PROGRAM Independent Physician Group Alliance 20% 31% 54% Expanded Physician Group 46% 69% Independent Hospital Alliance 33% 37% 63% 80% Full Spectrum 40% 67% 60% Implemented Not Implemented 31
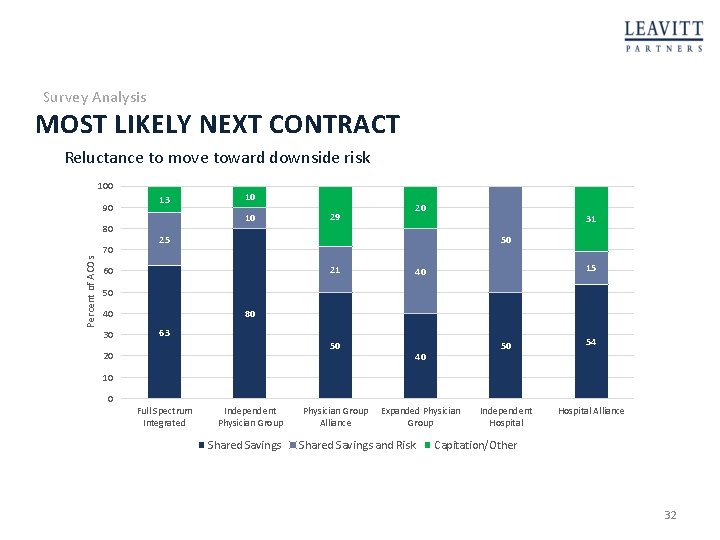
Survey Analysis MOST LIKELY NEXT CONTRACT Reluctance to move toward downside risk 100 90 80 Percent of ACOs 70 13 10 10 29 20 31 25 50 21 60 15 40 50 80 40 30 63 50 20 40 50 54 Independent Hospital Alliance 10 0 Full Spectrum Integrated Independent Physician Group Shared Savings Physician Group Alliance Expanded Physician Group Shared Savings and Risk Capitation/Other 32

KEY TAKEAWAYS Providers are meaningfully different • Recognize your needs, capabilities and opportunities • Know your population Don’t reinvent the wheel • Constant, voracious learning • Learn from others, like you, that have made progress There is no single approach to managing a population • Start where you are • Specific payment models don’t work for all providers 33

A health care intelligence business Leavitt. Partners. com

35 PANEL: Population-Based Payment Approaches Kerry Snyder Director of Health Informatics, Populytics, Inc. For Public Distribution Allison Yudt Director of Value. Based Contracts, Populytics, Inc.

Managing Multiple ACOs 2015 LAN Summit October 26, 2015 Allison Yudt Director, Value Based Contracting Kerry Snyder Director, Health Informatics

Lehigh Valley Health Network • In Allentown/Bethlehem area, north of Philadelphia • Recognized by U. S. News & World Report, Fortune, Modern Healthcare, Leapfrog, others • 5 hospital campuses, 12 Health Centers • 10 Express. CARE locations • 1161 acute care beds • 1, 340 physicians (700 network-employed) • 13, 100 employees • Ancillary Services • Physician Hospital Organization • Revenues over $2 Billion • Populytics – Population Health Management & Advanced Analytics Firm 37

Populytics® • Established December 2013 • Population health management and advanced analytics firm with a rich foundation of health plan administration experience Integrates: • Health plan management • Clinical care delivery and • Advanced information technology and analytics Supported by experts in: • Payer & Provider Informatics • Medical Management, including Wellness Services • Benefit Plan Design and Administration • Marketing, Sales & Business Development • Insurance and Risk Management 38
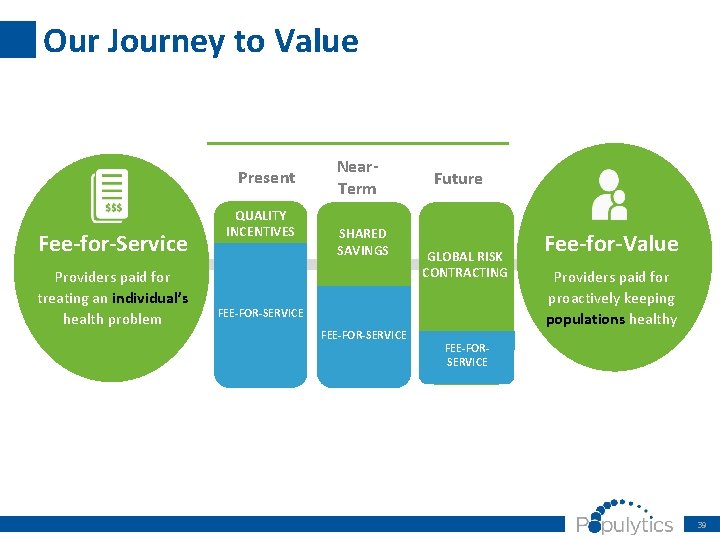
Our Journey to Value Present Fee-for-Service Providers paid for treating an individual’s health problem QUALITY INCENTIVES Near. Term SHARED SAVINGS Future GLOBAL RISK CONTRACTING FEE-FOR-SERVICE Fee-for-Value Providers paid for proactively keeping populations healthy FEE-FOR-SERVICE 39
Old Approach to Value Based Contracts 40

Overview of Value Based Contracts In Spring 2014, we reviewed 10 value-based contracts. Most Popular Measure Domains Diabetes Cancer Screening 148 Quality Measures 29 Utilization Measures BMI Cardiology Vaccines & Immunizations 177 Total Measures in 10 Contracts Admissions/ Readmissions Rx Preventive/ Wellness Care Other Asthma COPD Care Coordination/Patient Safety 0% 10% 20% 30% 40% 50% 60% 70% 80% 90% 100% 41
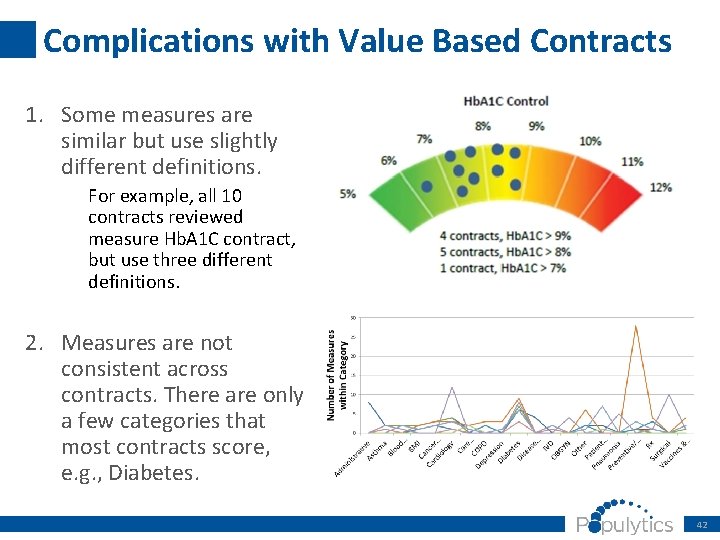
Complications with Value Based Contracts 1. Some measures are similar but use slightly different definitions. For example, all 10 contracts reviewed measure Hb. A 1 C contract, but use three different definitions. 2. Measures are not consistent across contracts. There are only a few categories that most contracts score, e. g. , Diabetes. 42

New Approach to Value Based Contracts Align Quality & Utilization Measures LVHN champions 30 priority measures using 3 primary tactics: Ø Ø Ø Physician Incentive Program – Achieving Clinical Excellence ® Analytics based on claims and clinical analytic information Consistent care management strategy Powered by 43

Lehigh Valley Physician Hospital Organization (LVPHO) • One of the largest medical groups in the U. S. • 1, 100+practioners and 3, 000 colleagues – Physicians (700+ FTEs) & APCs (400+ FTEs) 45+ specialties 145+ practice sites 2 million visits/year 400, 000 patients (>1/2 Lehigh Valley’s population) • $450 M operating budget • Growing 10 -15%/year • • 44

LVPHO Achieving Clinical Excellence® (ACE) Physician Incentive Program • • • Semi-annual practice-based group incentive plan 1037 participating providers in 217 practices 33% PCPs, 67% SCPs 71% employed, 5% aligned, 24% independent Measurement Categories – Better Care: CG CAHPs participation, Meaningful Use attestation – Better Cost: Risk Adjusted ALOS, Risk Adjusted Episode Cost, Risk Adjusted Admissions, Readmissions, ED visits, and generic Rx Utilization – Better Health: Evidence-based Quality Measures, QI Projects • Funding sources include employee health plan, shared savings from payers, and LVPHO Clinical Integration funds Utilizes medical and pharmacy claims and EMR data for employee population and shared risk arrangements Administered with internally developed software application • • 45
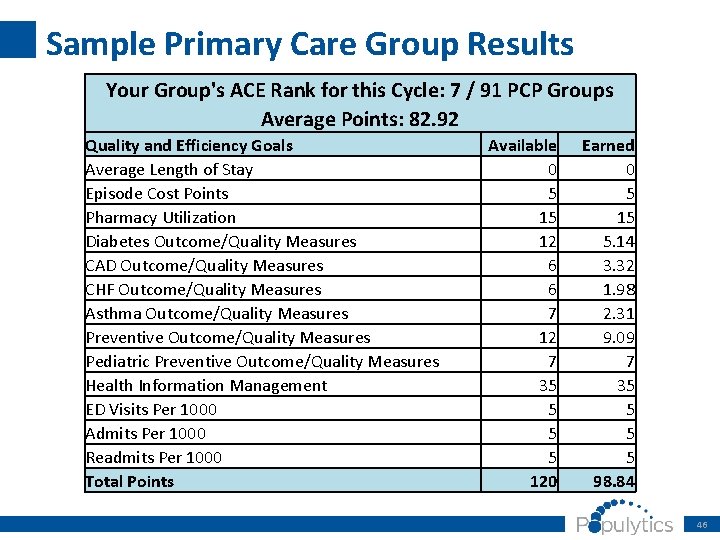
Sample Primary Care Group Results Your Group's ACE Rank for this Cycle: 7 / 91 PCP Groups Average Points: 82. 92 Quality and Efficiency Goals Average Length of Stay Episode Cost Points Pharmacy Utilization Diabetes Outcome/Quality Measures CAD Outcome/Quality Measures CHF Outcome/Quality Measures Asthma Outcome/Quality Measures Preventive Outcome/Quality Measures Pediatric Preventive Outcome/Quality Measures Health Information Management ED Visits Per 1000 Admits Per 1000 Readmits Per 1000 Total Points Available 0 5 15 12 6 6 7 12 7 35 5 120 Earned 0 5 15 5. 14 3. 32 1. 98 2. 31 9. 09 7 35 5 98. 84 46
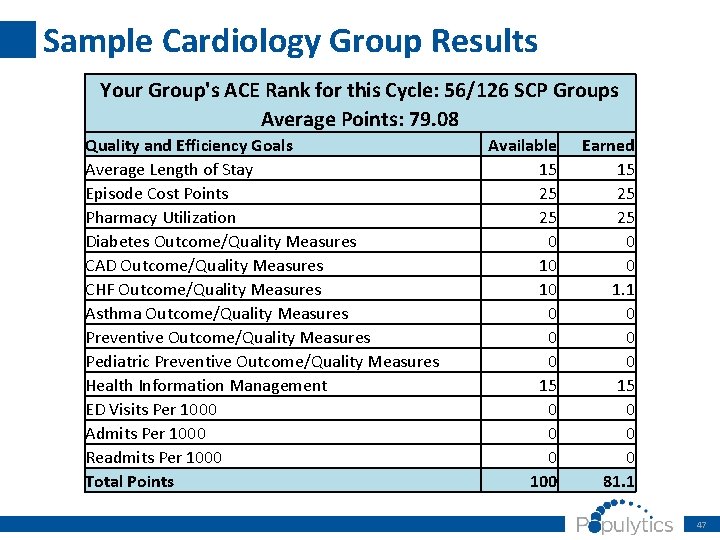
Sample Cardiology Group Results Your Group's ACE Rank for this Cycle: 56/126 SCP Groups Average Points: 79. 08 Quality and Efficiency Goals Average Length of Stay Episode Cost Points Pharmacy Utilization Diabetes Outcome/Quality Measures CAD Outcome/Quality Measures CHF Outcome/Quality Measures Asthma Outcome/Quality Measures Preventive Outcome/Quality Measures Pediatric Preventive Outcome/Quality Measures Health Information Management ED Visits Per 1000 Admits Per 1000 Readmits Per 1000 Total Points Available 15 25 25 0 10 10 0 15 0 0 0 100 Earned 15 25 25 0 0 1. 1 0 0 0 15 0 0 0 81. 1 47

Relative Episode Cost • Use Episode Grouping tool and rolling 12 months of medical & pharmacy claims • Episode costs are compared to commercial claims database of 42 M lives • Identify five most common episode base classes for each specialty • Each practice is scored on their relative costs of care for the common episodes • Episodes are risk-adjusted for severity, comorbidities, complications, and treatment 48
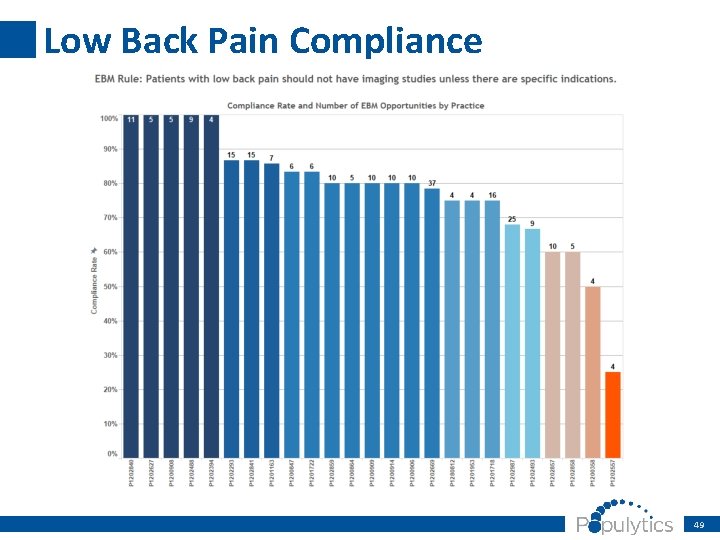
Low Back Pain Compliance 49

Changes to ACE for CY 16 • • • CG-CAHPS: participation -> results Episode cost score: more episodes included Quality measures: chart audits -> EMR Begin rewarding care gap closure projects Results: Paper reports -> Web portal Adding metrics for knowledge of and compliance with Choosing Wisely principles 50

51

52 Q & A What questions do you have about Population-Based Payments? Use the chat window in your webinar dashboard For Public Distribution

53 Key Upcoming LAN Dates Monthly “LAN Learnings” webinars December 2, 2015 2: 00 ET January 12, 2016 TBD February 9, 2016 TBD Guiding Committee Meetings November 13, 2015 December 7, 2015 January 29, 2016 For Public Distribution

54 Thank You for Participating! The webinar recording will be posted to https: //publish. mitre. org/hcplan. If you haven’t already, register for the LAN at: http: //innovationgov. force. com/hcplan Questions? Email Payment. Network@MITRE. org For Public Distribution
- Slides: 54