Populationbased gonorrhea surveillance through the STD Surveillance Network

Population-based gonorrhea surveillance through the STD Surveillance Network (SSu. N) Lori Newman; K Ahrens; J Donnelly; S Martins; M Stenger; O Vasiliu; H Weinstock National STD Prevention Conference March 12, 2008

STD Surveillance Network (SSu. N) § Purpose: to improve national capacity to detect, monitor, and respond to emerging trends in STDs and related behaviors § Initial activities – 2006 to 2008 • Enhanced gonorrhea surveillance in STD clinics • Genital wart surveillance in STD clinics • Population-based enhanced gonorrhea surveillance

Rationale for Population-based Gonorrhea Surveillance § Gonorrhea rates still far from Healthy People 2010 objectives, but we don’t understand why § Case report data at national level limited to sex, age, race/ethnicity, and crude provider type § Need a better understanding of gonorrhea patients outside of the STD clinic setting

Objectives of SSu. N Population-based Gonorrhea Surveillance § Establish network of health departments working collaboratively with standardized methodology Collect demographic, behavioral, and clinical data on patients with gonorrhea § • § Monitor trends over time Use data to guide local, state, and national STD programs and policies
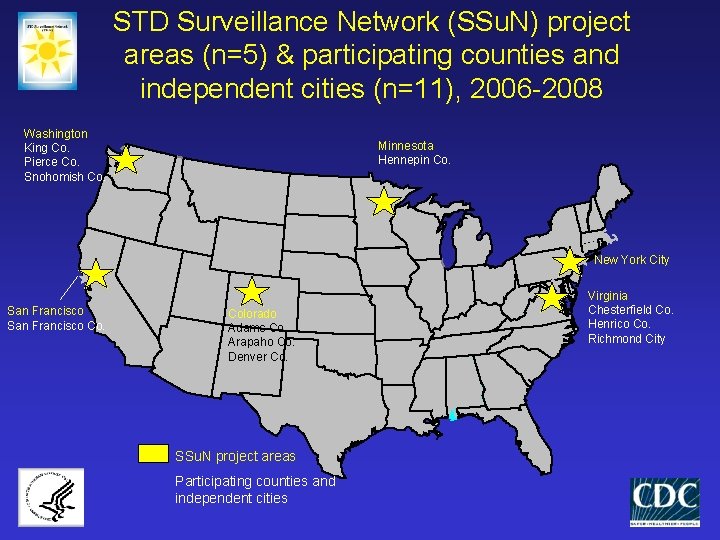
STD Surveillance Network (SSu. N) project areas (n=5) & participating counties and independent cities (n=11), 2006 -2008 Washington King Co. Pierce Co. Snohomish Co. Minnesota Hennepin Co. New York City San Francisco Co. Colorado Adams Co. Arapaho Co. Denver Co. SSu. N project areas Participating counties and independent cities Virginia Chesterfield Co. Henrico Co. Richmond City

SSu. N Methodology § Data collected on sample of patients reported with gonorrhea in selected counties • • • § Data transmitted with morbidity data • § § Phone or in-person interview of first reported patients each month until completed 10 male and 10 female SF: weekly sample adjusted for non-response for target of 100 men and 100 women per year Sample excludes patients who attend the primary STD clinic(s) Assessment of representativeness, contact rate, etc. Data collection initiated between Feb 2006 and Jan 2007 Data analyzed through Dec 31, 2007

Collaborative Data Elements § § Demographics Sexual practices Substance use Partner characteristics § § HIV history STD history Clinical history Treatment
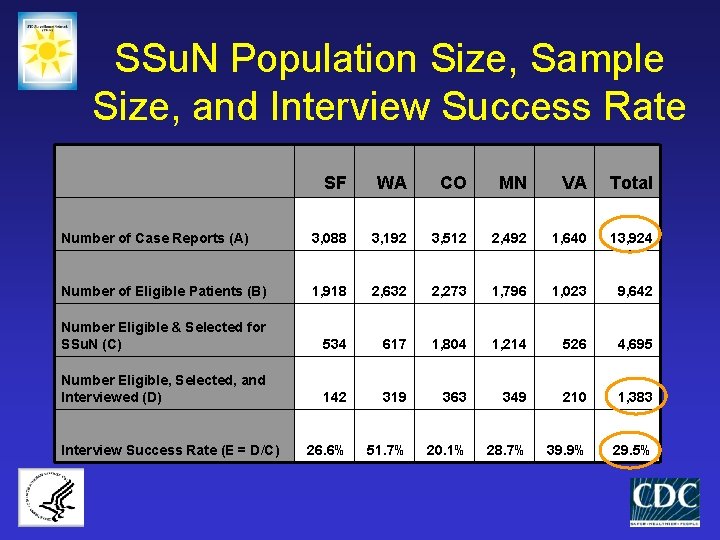
SSu. N Population Size, Sample Size, and Interview Success Rate SF WA CO MN VA Total Number of Case Reports (A) 3, 088 3, 192 3, 512 2, 492 1, 640 13, 924 Number of Eligible Patients (B) 1, 918 2, 632 2, 273 1, 796 1, 023 9, 642 Number Eligible & Selected for SSu. N (C) 534 617 1, 804 1, 214 526 4, 695 Number Eligible, Selected, and Interviewed (D) 142 319 363 349 210 1, 383 26. 6% 51. 7% 20. 1% 28. 7% 39. 9% 29. 5% Interview Success Rate (E = D/C)
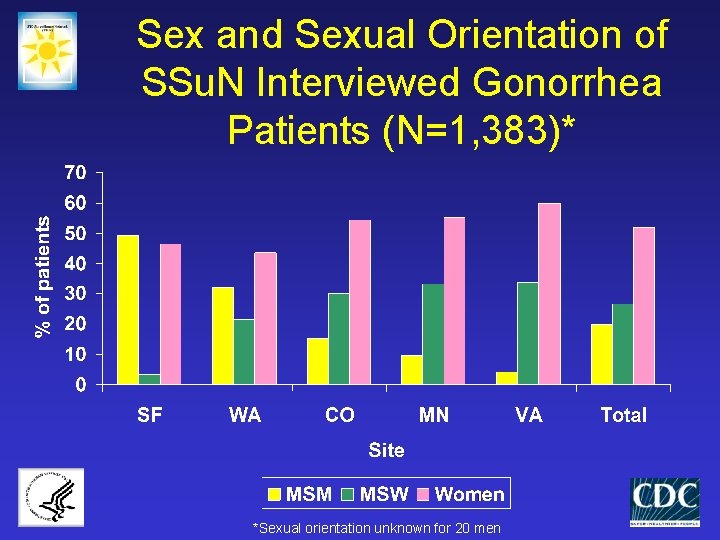
Sex and Sexual Orientation of SSu. N Interviewed Gonorrhea Patients (N=1, 383)* *Sexual orientation unknown for 20 men
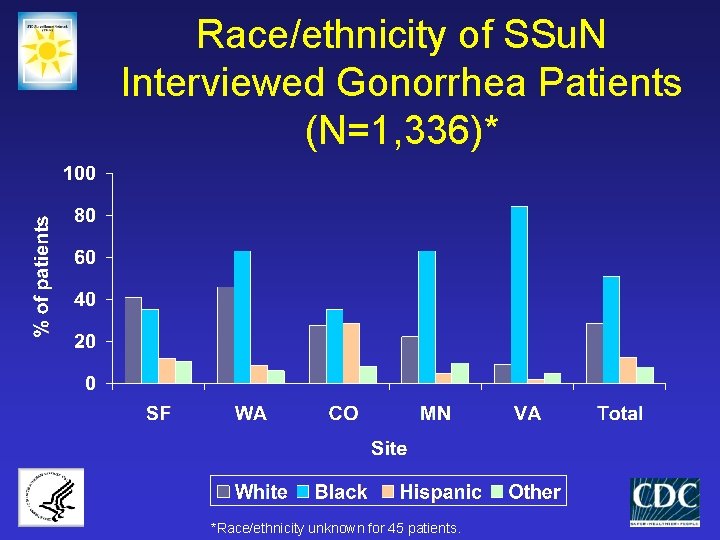
Race/ethnicity of SSu. N Interviewed Gonorrhea Patients (N=1, 336)* *Race/ethnicity unknown for 45 patients.
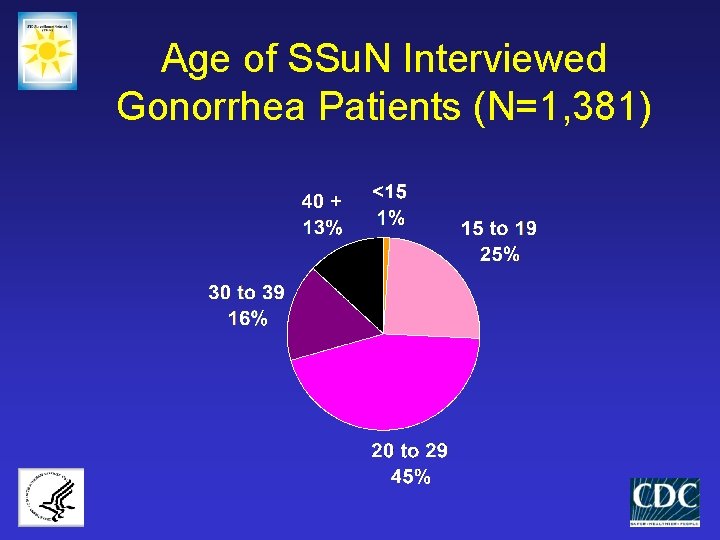
Age of SSu. N Interviewed Gonorrhea Patients (N=1, 381)
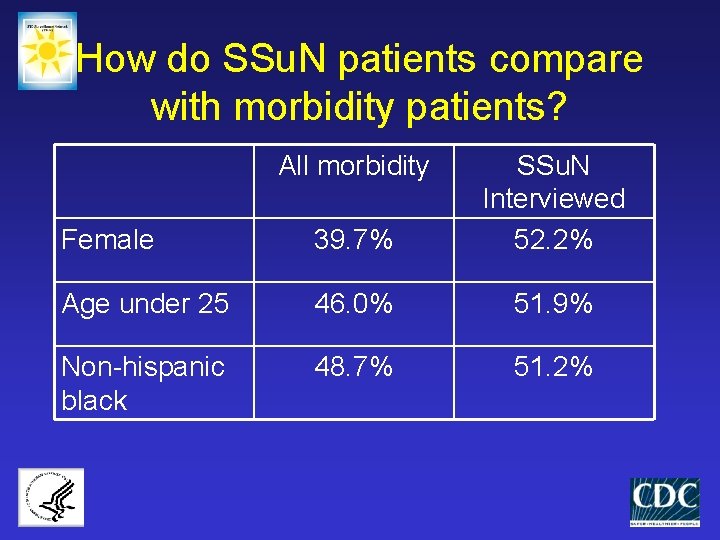
How do SSu. N patients compare with morbidity patients? All morbidity Female 39. 7% SSu. N Interviewed 52. 2% Age under 25 46. 0% 51. 9% Non-hispanic black 48. 7% 51. 2%
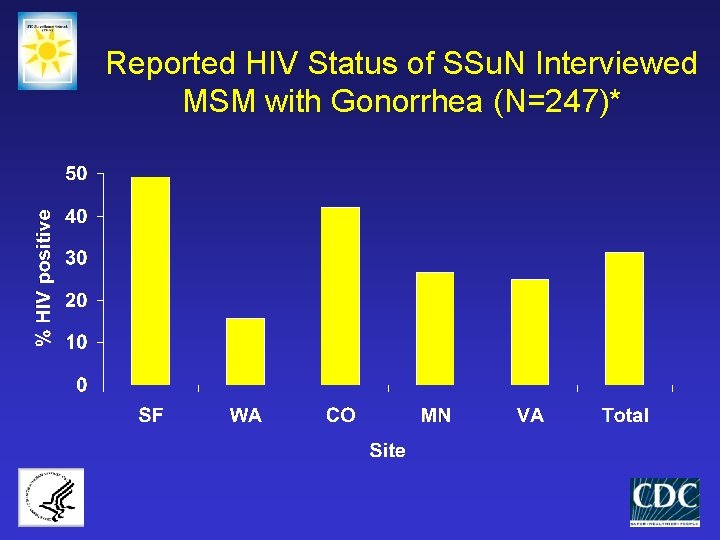
Reported HIV Status of SSu. N Interviewed MSM with Gonorrhea (N=247)*
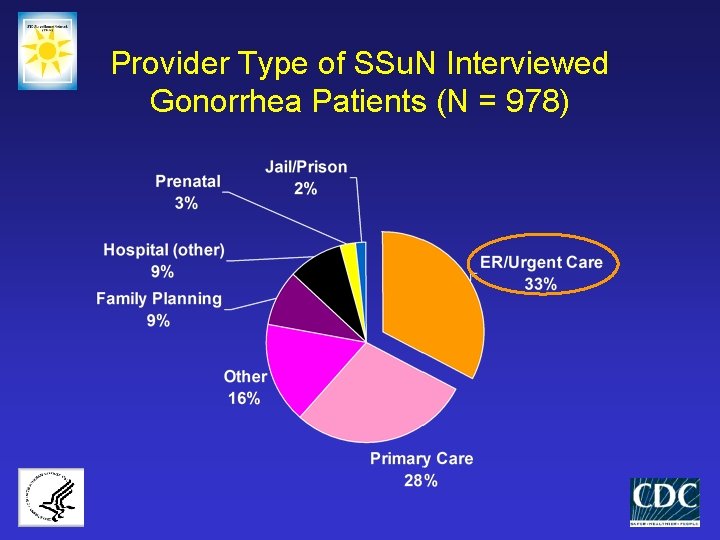
Provider Type of SSu. N Interviewed Gonorrhea Patients (N = 978)
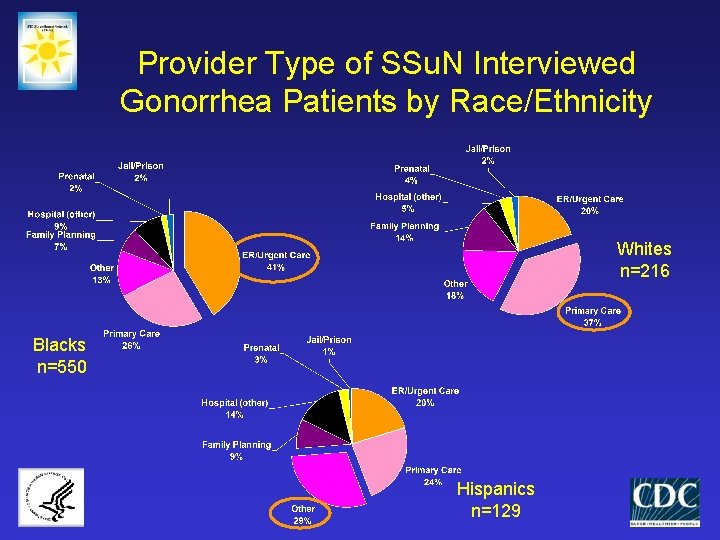
Provider Type of SSu. N Interviewed Gonorrhea Patients by Race/Ethnicity Whites n=216 Blacks n=550 Hispanics n=129
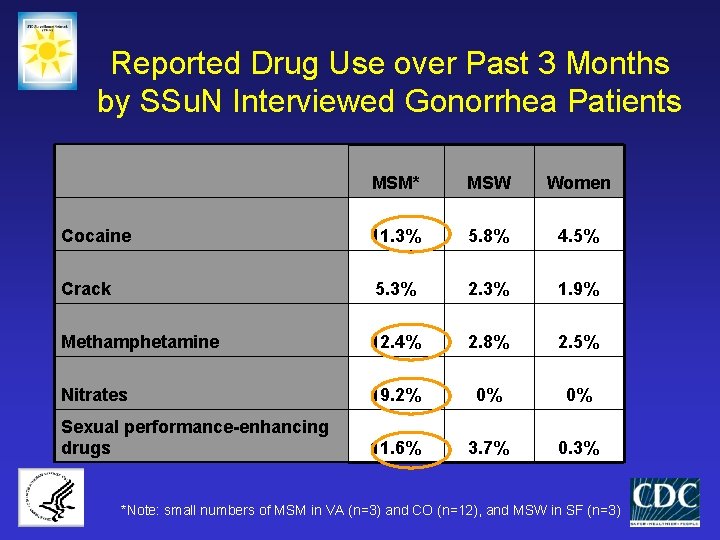
Reported Drug Use over Past 3 Months by SSu. N Interviewed Gonorrhea Patients MSM* MSW Women Cocaine 11. 3% 5. 8% 4. 5% Crack 5. 3% 2. 3% 1. 9% Methamphetamine 12. 4% 2. 8% 2. 5% Nitrates 19. 2% 0% 0% Sexual performance-enhancing drugs 11. 6% 3. 7% 0. 3% *Note: small numbers of MSM in VA (n=3) and CO (n=12), and MSW in SF (n=3)
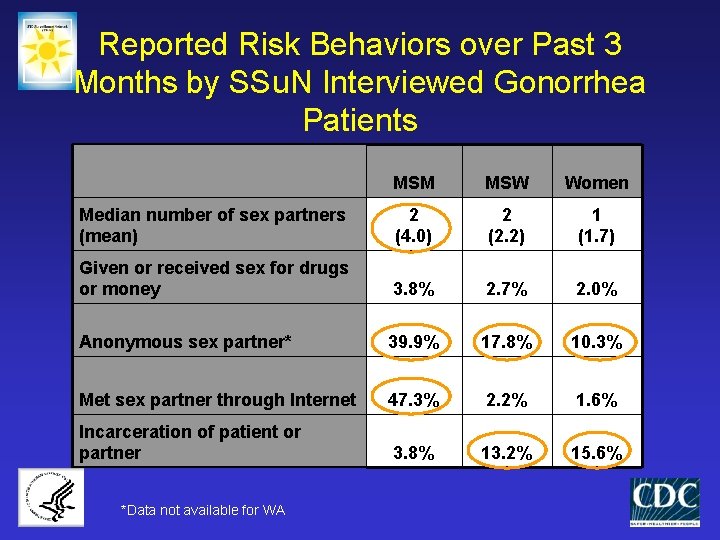
Reported Risk Behaviors over Past 3 Months by SSu. N Interviewed Gonorrhea Patients MSM MSW Women Median number of sex partners (mean) 2 (4. 0) 2 (2. 2) 1 (1. 7) Given or received sex for drugs or money 3. 8% 2. 7% 2. 0% Anonymous sex partner* 39. 9% 17. 8% 10. 3% Met sex partner through Internet 47. 3% 2. 2% 1. 6% Incarceration of patient or partner 3. 8% 13. 2% 15. 6% *Data not available for WA
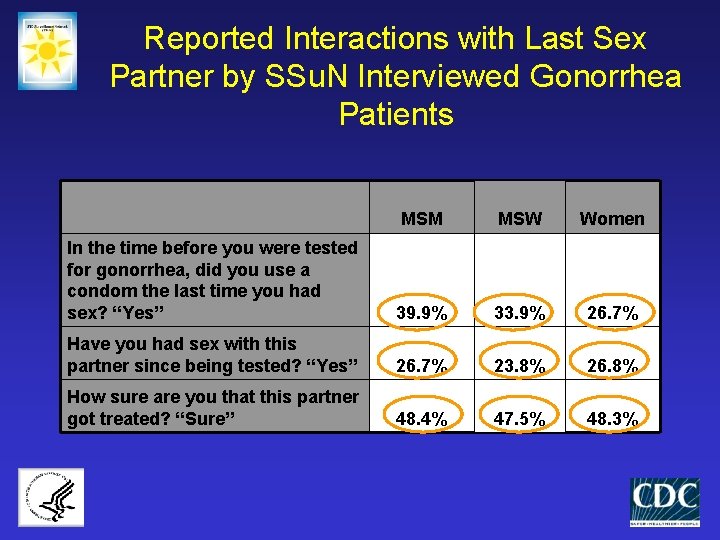
Reported Interactions with Last Sex Partner by SSu. N Interviewed Gonorrhea Patients MSM MSW Women In the time before you were tested for gonorrhea, did you use a condom the last time you had sex? “Yes” 39. 9% 33. 9% 26. 7% Have you had sex with this partner since being tested? “Yes” 26. 7% 23. 8% 26. 8% How sure are you that this partner got treated? “Sure” 48. 4% 47. 5% 48. 3%
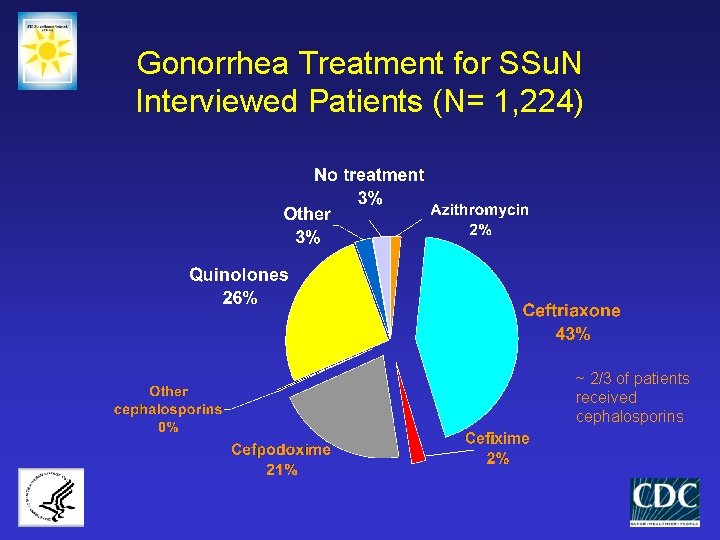
Gonorrhea Treatment for SSu. N Interviewed Patients (N= 1, 224) ~ 2/3 of patients received cephalosporins

Limitations § Only 5 geographic sites and 11 counties, so limited ability to generalize § Possible response bias since only able to contact about 1 in 3 patients with gonorrhea due to poor contact information § Slight variability in methodology between sites since integrated into routine activities § No trends over time available yet

Summary § Mixed heterosexual and MSM epidemic § MSM gonorrhea patients interviewed reported high levels of risk behavior • 30% co-infected with HIV • Greater numbers of sex partners, drug use, anonymous sex, & internet sex § Heterosexual gonorrhea risks • May involve incarceration, anonymous sex • Drug use and sex work infrequently reported § Aggressive counseling and partner management may be useful intervention strategies for both MSM and heterosexual gonorrhea populations § Important racial/ethnic differences in where gonorrhea is being diagnosed

Future Directions § Trends over time • Are changes in risk behaviors associated with changes in morbidity? § Expand number of SSu. N participating sites • Better geographic representativeness § Geocoding & linkage with census data & other data sources • Where & when is gonorrhea being diagnosed? • Gonorrhea association with SES and environmental factors • Racial/ethnic variation in access to care

Acknowledgements SSu. N Collaborating Sites • • • Colorado Department of Public Health Minnesota Department of Health San Francisco Department of Public Health Virginia Department of Health Washington State Department of Health CDC • Darlene Davis For more information on SSu. N, contact: LEN 4@CDC. GOV The findings and conclusions in this presentation are those of the authors and do not necessarily represent the views of the CDC.

- Slides: 24