Population Based Cancer Registry in Nepal Ranjeeta Subedi

Population Based Cancer Registry in Nepal Ranjeeta Subedi Nepal Health Research Council 13 June, 2019 Vancouver, Canada
Federal Democratic Republic of Nepal

An overview Established in January 2018 Led by Nepal Health Research Council PI : Prof. Dr. Anjani Kumar Jha Reached up to 9 districts (Out of 77) with three registries of the country (Kathmandu, Bhaktapur, Lalitpur in province 3, Siraha, Saptari, Dhanusha, Mohattari in province 2 East and West Rukum in province 5 and 6) Population coverage by PBCR: 20. 3%
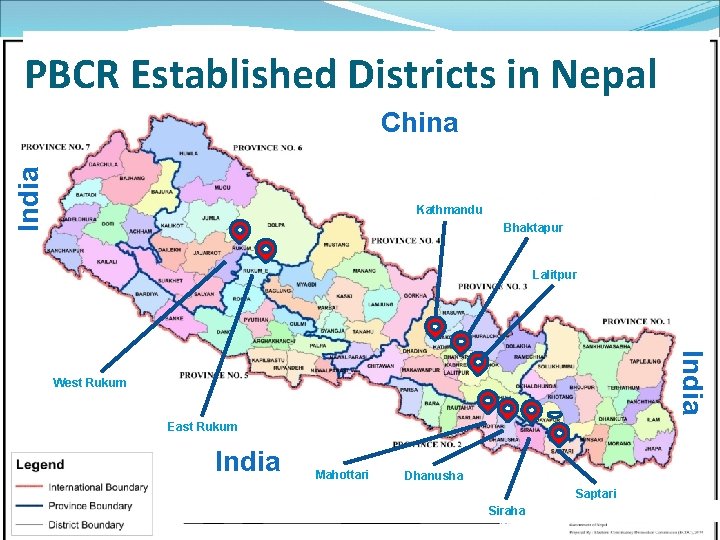
PBCR Established Districts in Nepal India China Kathmandu Bhaktapur Lalitpur India West Rukum East Rukum India Mahottari Dhanusha Saptari Siraha

Why PBCR in Nepal ? Absence of routine surveillance and national PBCR in the country Disease burden estimates so far depend upon small scale data sources and data from neighboring countries

Why PBCR in Nepal … Nepal government invest huge amount of money ( NRS. 93, 04, 09, 118 in 2016/17) for cancer treatment PBCR supports for the country to measure Global NCD Target endorsed by WHO Member States in 25% reduction of premature mortality from the four major NCDs by 2025
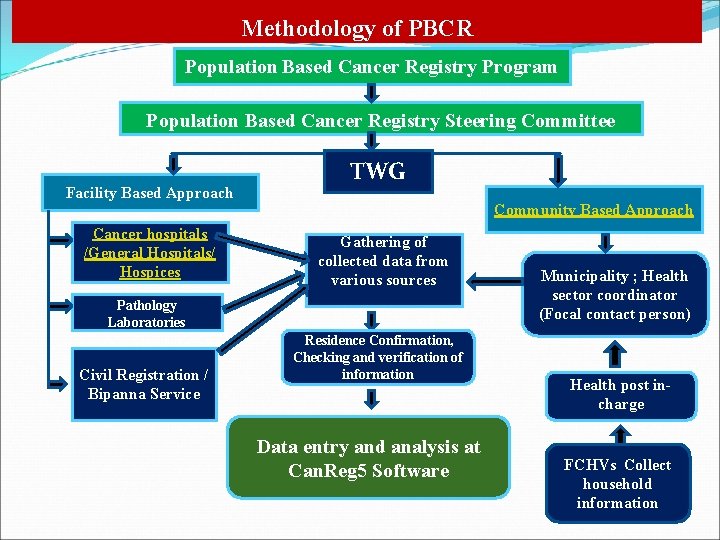
Methodology of PBCR Population Based Cancer Registry Program Population Based Cancer Registry Steering Committee Facility Based Approach Cancer hospitals /General Hospitals/ Hospices TWG Community Based Approach Gathering of collected data from various sources Pathology Laboratories Civil Registration / Bipanna Service Residence Confirmation, Checking and verification of information Data entry and analysis at Can. Reg 5 Software Municipality ; Health sector coordinator (Focal contact person) Health post incharge FCHVs Collect household information

Collaborations IARC Regional Hub Mumbai WHO Country Office, Nepal Private/Public Health Facilities Pathology Laboratories, Hospice, Civil Registration, Wards/Deprived Section of Department of Health Services within Kathmandu Valley • Local Authorities: Metropolitan city, rural/municipalities and their ward offices • •

Major Progress/Achievements Establishment of Steering Committee, Technical Working Group • Oriented around 2000 (doctors, health in charges/ coordinators and FCHVs) • Mo. U signed between B. P Koirala Memorial Cancer Hospital, Bharatpur & Nepal Health Research Council for PBCR • Published PBCR Interim Report 2018 • PBCR fully established at 9 districts

Major Progress/Achievements…. Total new cancer cases until May 31 st 2018 Kathmandu Valley: 702 Siraha, Saptari, Dhanusha and Mahottari: 256 East and West Rukum: 23
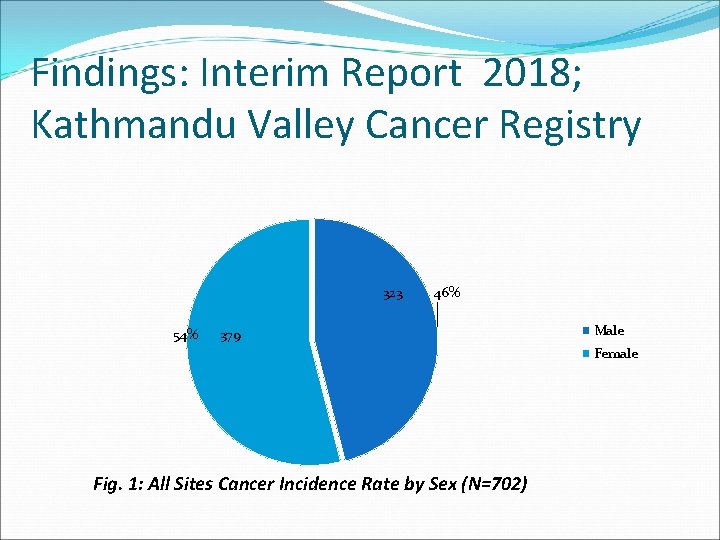
Findings: Interim Report 2018; Kathmandu Valley Cancer Registry 323 54% 46% 379 Male Female Fig. 1: All Sites Cancer Incidence Rate by Sex (N=702)
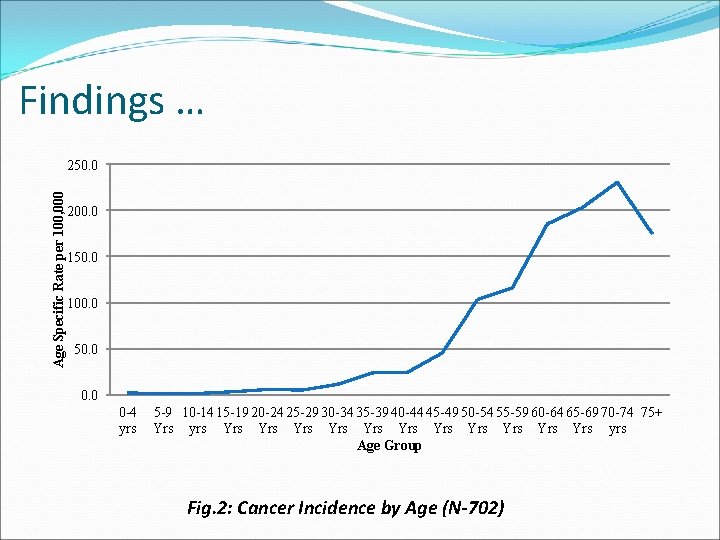
Findings … Age Specific Rate per 100, 000 250. 0 200. 0 150. 0 100. 0 50. 0 0 -4 yrs 5 -9 10 -14 15 -19 20 -24 25 -29 30 -34 35 -39 40 -44 45 -49 50 -54 55 -59 60 -64 65 -69 70 -74 75+ Yrs yrs Yrs Yrs Yrs yrs Age Group Fig. 2: Cancer Incidence by Age (N-702)

04 y 5 - rs 9 10 Yrs -1 4 15 yr -1 s 9 20 Yr -2 s 4 25 Yr -2 s 9 30 Yr -3 s 4 35 Yr -3 s 9 40 Yr -4 s 4 45 Yr -4 s 9 50 Yr -5 s 4 55 Yr -5 s 9 60 Yr -6 s 4 65 Yr -6 s 9 70 Yrs -7 4 yr s 75 + Age Specific Rate per 100, 000 Findings … 350. 0 300. 0 250. 0 200. 0 150. 0 100. 0 Male 50. 0 Female 0. 0 Age Group Fig. 3: Cancer Incidence Rates by Age and Sex Male (n=323) Female (n=379)
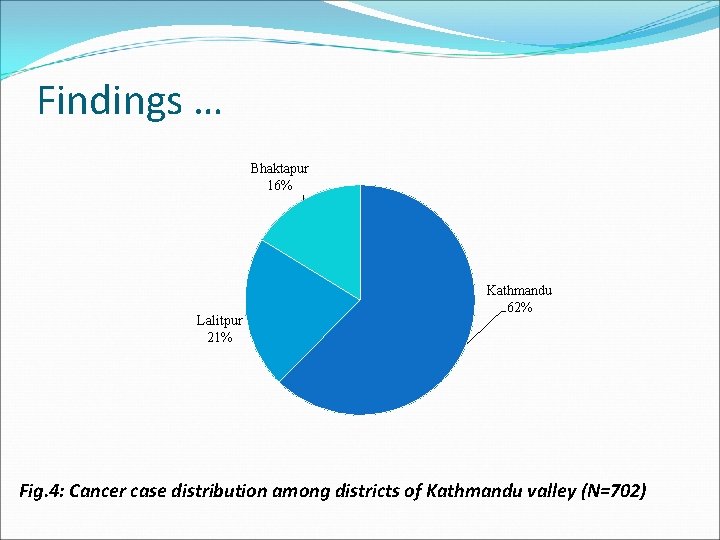
Findings … Bhaktapur 16% Lalitpur 21% Kathmandu 62% Fig. 4: Cancer case distribution among districts of Kathmandu valley (N=702)
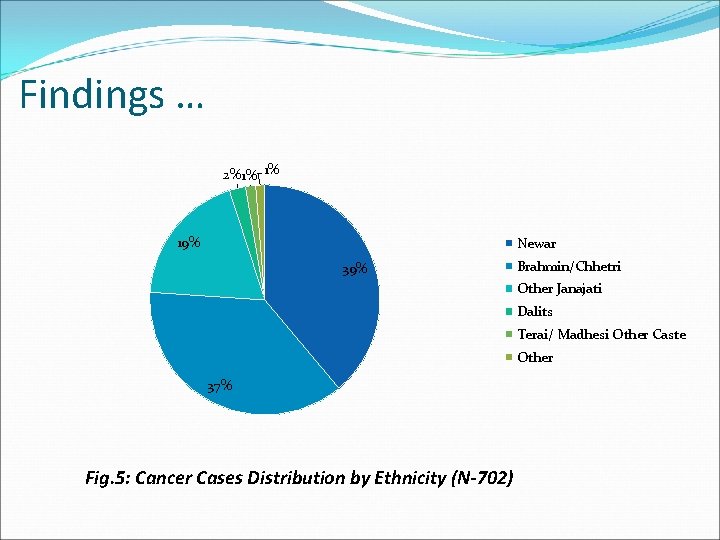
Findings … 2%1% 1% 19% Newar 39% Brahmin/Chhetri Other Janajati Dalits Terai/ Madhesi Other Caste Other 37% Fig. 5: Cancer Cases Distribution by Ethnicity (N-702)
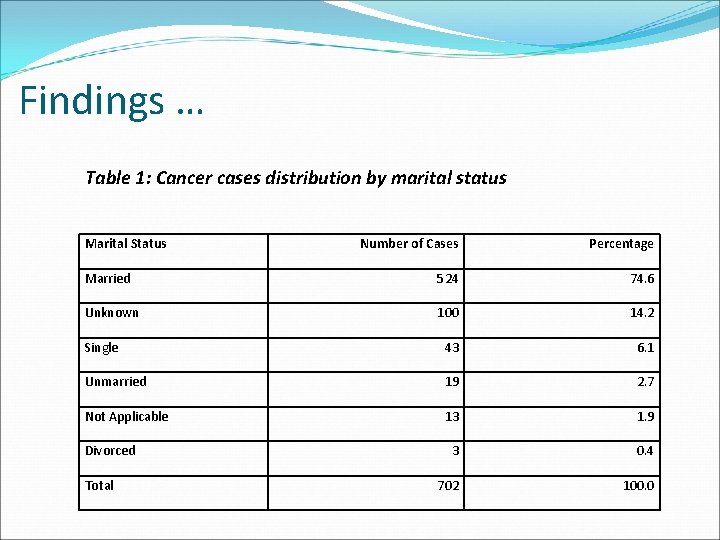
Findings … Table 1: Cancer cases distribution by marital status Marital Status Number of Cases Percentage Married 524 74. 6 Unknown 100 14. 2 Single 43 6. 1 Unmarried 19 2. 7 Not Applicable 13 1. 9 3 0. 4 702 100. 0 Divorced Total

Findings … Lungs 111(15. 8%) Breast 94 (13. 4%) Colon and Rectum 48 (6. 8%) Stomach 39 (5. 6%) 37 (5. 3%) Lip, oral cavity Cervix Uteri 34 (4. 8%) Gall Bladder 33 (4. 7%) Thyroid 27 (3. 8%) Pharynx 22 (3. 1%) Ovary 21 (3%) 0 20 40 60 Number of Cases Fig. 6: Leading cancer sites N=702 80 100 120

Findings … Lungs 71 (22%) Lip, oral cavity 28 (8. 7%) Colon and Rectum 26 (8%) Stomach 24 (7. 4%) Pharynx 19 (5. 9%) Bladder 14 (4. 3%) Larynx 11 (3. 4%) Pancreas 11 (3. 4%) Gall Bladder 11 (3. 4%) Kidney 10 (3. 1%) 0 10 20 30 40 50 Number of Cases Fig. 7: Leading Cancer Sites in Males (n=323) 60 70 80
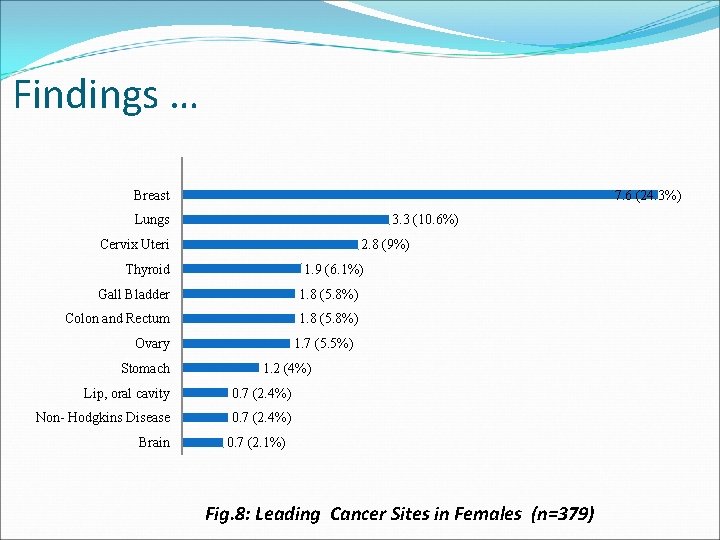
Findings … 7. 6 (24. 3%) Breast 3. 3 (10. 6%) Lungs 2. 8 (9%) Cervix Uteri 1. 9 (6. 1%) Thyroid Gall Bladder 1. 8 (5. 8%) Colon and Rectum 1. 8 (5. 8%) Ovary Stomach 1. 7 (5. 5%) 1. 2 (4%) Lip, oral cavity 0. 7 (2. 4%) Non- Hodgkins Disease 0. 7 (2. 4%) Brain 0. 7 (2. 1%) Fig. 8: Leading Cancer Sites in Females (n=379)
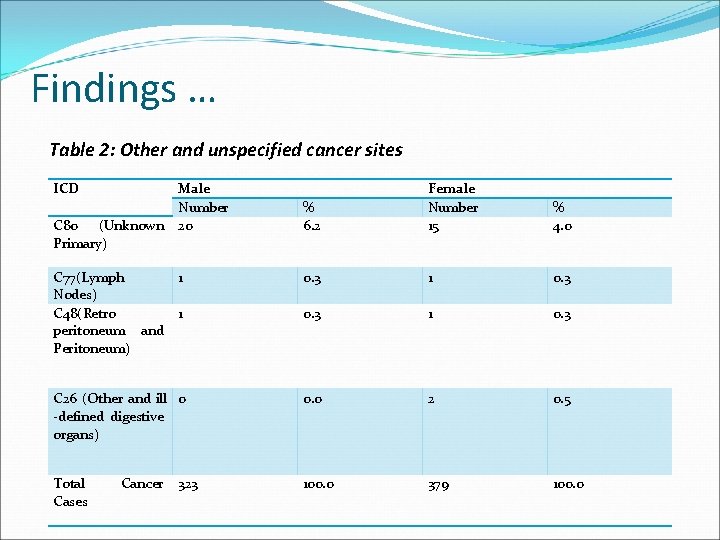
Findings … Table 2: Other and unspecified cancer sites ICD % 6. 2 Female Number 15 % 4. 0 1 0. 3 C 26 (Other and ill 0 -defined digestive organs) 0. 0 2 0. 5 Total Cases 100. 0 379 100. 0 C 80 (Unknown Primary) C 77(Lymph Nodes) C 48(Retro peritoneum and Peritoneum) Cancer Male Number 20 323
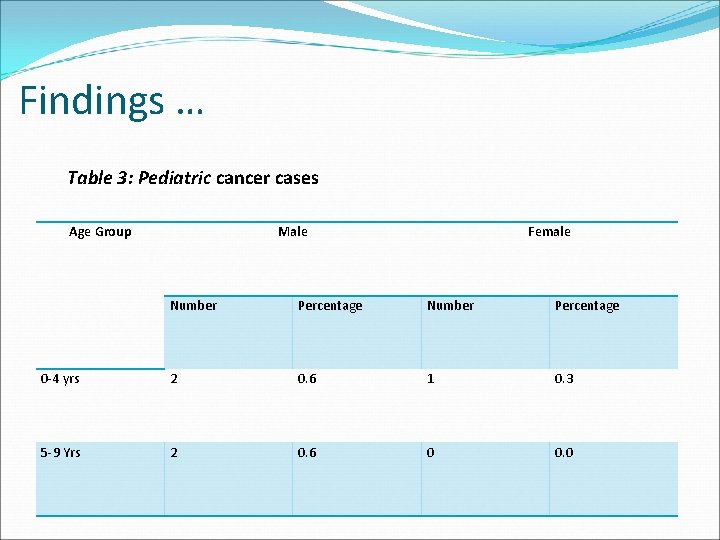
Findings … Table 3: Pediatric cancer cases Age Group Male Female Number Percentage 0 -4 yrs 2 0. 6 1 0. 3 5 -9 Yrs 2 0. 6 0 0. 0
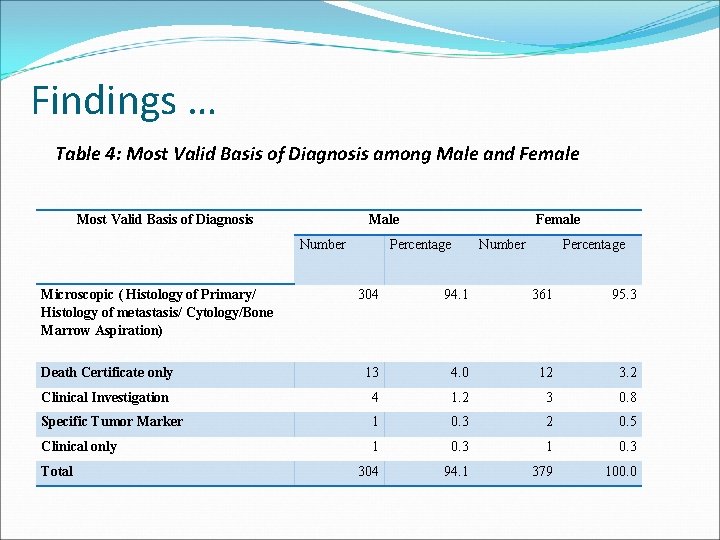
Findings … Table 4: Most Valid Basis of Diagnosis among Male and Female Most Valid Basis of Diagnosis Male Number Microscopic ( Histology of Primary/ Histology of metastasis/ Cytology/Bone Marrow Aspiration) Female Percentage Number Percentage 304 94. 1 361 95. 3 Death Certificate only 13 4. 0 12 3. 2 Clinical Investigation 4 1. 2 3 0. 8 Specific Tumor Marker 1 0. 3 2 0. 5 Clinical only 1 0. 3 304 94. 1 379 100. 0 Total

Challenges The data collection method is primarily active. No dedicated staff at data source locations; difficult to obtain data on periodic basis Hard to keep exact record of cancer cases within registry area as cancer patients visit other country (India) Limited human/financial resources No PBCR coordinating bodies at the respective provinces.

Way forward Meaningful participation of key stakeholders at planning & implementing PBCR Increment in human/financial resources Increase collaboration with hospitals outside the country and make coordination to obtain data on regular basis from there. Utilizing the information obtained in cancer control strategies.

Thank You
- Slides: 25