Polycystic Ovary Syndrome PCOS Prof Wafaa Mostafa Aboeleneen

Polycystic Ovary Syndrome (PCOS) Prof. Wafaa Mostafa Aboeleneen Department of Obstetrics and Gynaecology, Alexandria University, Egypt.

Objectives 1. 2. 3. 4. 5. 6. Epidemiology Diagnostic criteria Metabolic abnormalities Effect on quality of life PCOS in adolescence Management

§ PCOS is one of the most common endocrine disorders. § Heterogenous condition with significant short and long term health sequelae. § Ethnic variations (↑ in South Asians). § Genetic variations in control of insulin metabolism have a profound effect on disease expression, being infleunced by environmental factors. § Appears to run in families.

Diagnostic Criteria
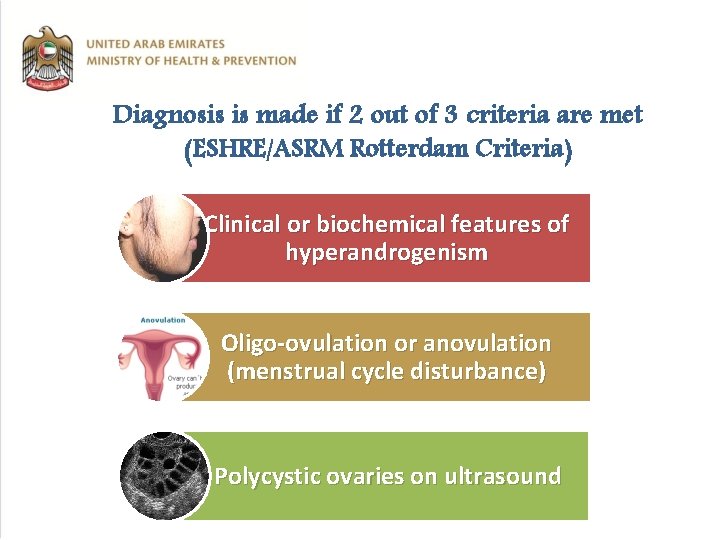
Diagnosis is made if 2 out of 3 criteria are met (ESHRE/ASRM Rotterdam Criteria) Clinical or biochemical features of hyperandrogenism Oligo-ovulation or anovulation (menstrual cycle disturbance) Polycystic ovaries on ultrasound

Diagnosis requires exclusion of: 1. Diseases of adrenal or pituitary glands Hyper-prolactinaemia, acromegaly, CAH, Cushing syndrome androgen secreting tumours. 2. Other causes of menstrual cycle irregularity Hypothalamic, pituitary or ovarian dysfunction.

Clinical Manifestations
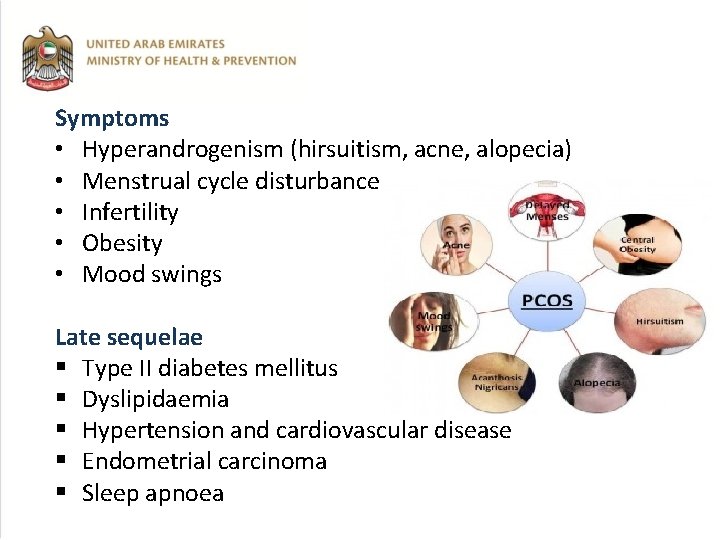
Symptoms • Hyperandrogenism (hirsuitism, acne, alopecia) • Menstrual cycle disturbance • Infertility • Obesity • Mood swings Late sequelae § Type II diabetes mellitus § Dyslipidaemia § Hypertension and cardiovascular disease § Endometrial carcinoma § Sleep apnoea

Serum Endocrinology • • ↑ or normal androgens ↑ or normal LH (↑in 40% , usually in slim women) Normal FSH ↑ or normal fasting insulin ↓ or normal SHBG (↑ free androgen index). ↑ or normal estradiol ↑ AMH Prolactin normal or slightly elevated.

Ultrasound • Polycystic ovaries are detected by pelvic US (prevalence 20 -33%). • Defined as an ovary with ≥ 12 follicles 2 -9 mm in diameter and /or an ovarian volume > 10 cm 3. • Recently, it is suggested that threshold number of follicles should be 25 and that AMH is more precise than US with a serum threshold >35 pmol/l (debatable).

Metabolic abnormalities and health consequences

• Insulin resistance, central obesity and dyslipidaemia place women at a high risk of DM and CVD. • Insulin resistance and ↑ serum insulin occur due to resistance at insulin receptor, ↓ hepatic clearance of insulin and /or ↑ pancreatic sensitivity. • Insulin ↓ synthesis of SHBG , thereby ↑ free testosterone levels and peripheral androgen action.

• Fasting insulin is not measured in routine practice, instead 75 gm OGTT is performed if: BMI >30 BMI >25 in South Asians BMI < 25 with additional risk factors e. g. age > 40 yrs. • If impaired fasting glucose (6. 1 -6. 9 mmol/l) or impaired glucose tolerance (7. 8 -11. 1 mmol/l after 2 hr OGTT), perform OGTT annually. • Hb. A 1 c may be helpful.
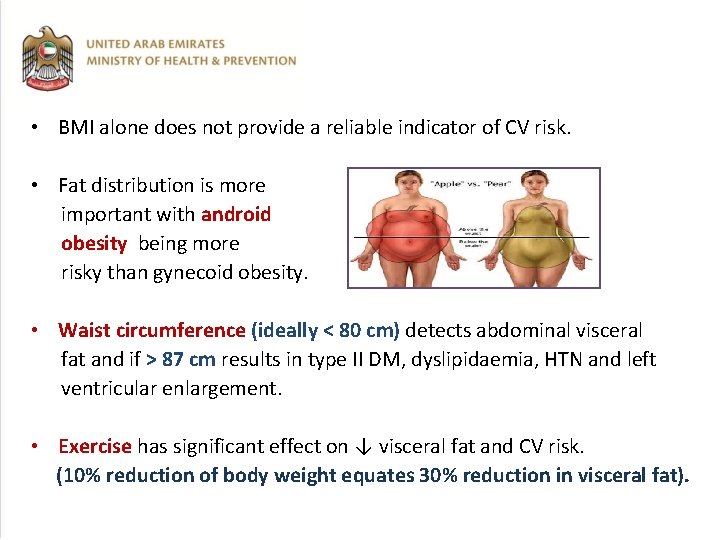
• BMI alone does not provide a reliable indicator of CV risk. • Fat distribution is more important with android obesity being more risky than gynecoid obesity. • Waist circumference (ideally < 80 cm) detects abdominal visceral fat and if > 87 cm results in type II DM, dyslipidaemia, HTN and left ventricular enlargement. • Exercise has significant effect on ↓ visceral fat and CV risk. (10% reduction of body weight equates 30% reduction in visceral fat).

In PCOS assess for CV risk factors at time of initial diagnosis: • • Obesity (BMI and waist circumference) Lack of physical activity Cigarette smoking Family history of type II DM Dyslipidaemia (in particular ↑ serum triglycerides). Hypertension (assess if oral contraceptive therapy). Impaired glucose tolerance Type II DM

Effect on quality of life

• Symptoms of PCOS lead to significant reduction in health – related quality of life. • Hirsuitism , infertility and obesity with failed attempts at weight loss are the major causes of marked psychological distress. • Depression and anxiety should be screened for and, if present, counselling and intervention should be offered.

PCOS in adolescence

• Diagnosis should not be made until 2 years after menarche. • All three elements of Rotterdam consensus are required for diagnosis. • Progressive hirsuitism is an important sign and a better marker of hyperandrogenism than acne. • Exclude late onset congenital adrenal hyperplasia.

• Menstrual irregularities are common in adolescence (65% anovulatory cycles) which tend to progress towards ovulatory cycles with increasing age. • If diagnosis of PCOS is not confirmed, follow up and diagnosis reconsidered if symptoms persist. • Start treatment during adolescent years, if troublesome problems.

Management of PCOS

• Inform patients of the long term health risks. • Strategies for reduction of metabolic risks. • Amelioration of hyperandrogenic symptoms. • Management of menstrual problems and prevention of endometrial hyperplasia /carcinoma. • Ovulation induction for those pursuing pregnancy.

Reduction of Metabolic Risks

Life-style issues • Diet, exercise and weight loss are recommended as first line treatment and should precede or accompany pharmacological treatment. • Moderate weight loss (5 -10% of total body weight) restore fertility and improve metabolic parameters (↓insulin resistance, ↓testosterone and improve CV risk markers).

• Concurrent behavioural therapy improve chances of weight loss. • Consider bariatric surgery if failure to lose weight with long term lifestyle strategies and: - BMI ≥ 40 ( morbid obesity) BMI ≥ 35 with high-risk factors e. g. HTN, type II DM. v However, surgically induced weight loss must be balanced against the risks of surgery.

Drug therapy • No medication assist with long term weight loss. • No evidence that Metformin confer any long-term benefits , however, modest reduction in body weight is reported. • Metformin can be considered in women with PCOS and impaired glucose tolerance or type II DM, combined with lifestyle modification.

• Incretin hormone –based therapies Reduce weight and improve insulin resistance, however, their use is not recommended (significant side effects). • Orlistat Induces weight reduction but without changing glucose-insulin homeostasis or lipid patterns.

Management of Hyperandrogenism

• ↑ androgens stimulate androgen receptors resulting in ↑ 5 alpha reductase activity, ↑conversion of T to dihydro-T. • T levels (2 -5 nmol/l) are associated with PCOS while levels > 5 nmol/l or rapid onset of signs of hyperandrogenism require further investigations.
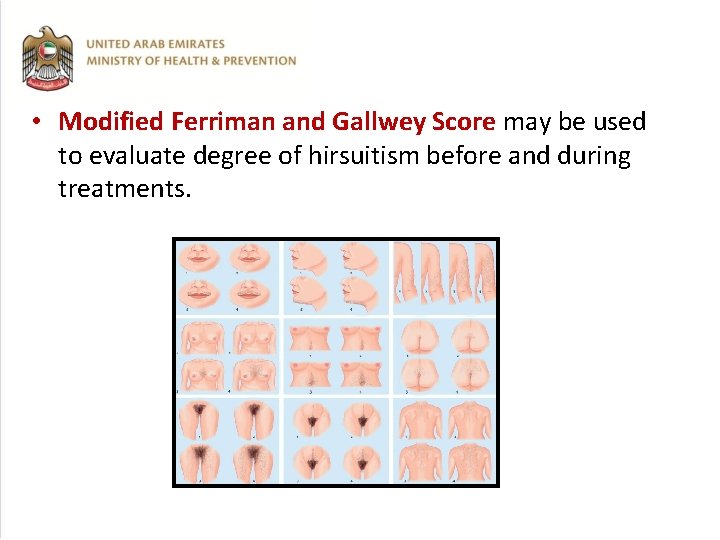
• Modified Ferriman and Gallwey Score may be used to evaluate degree of hirsuitism before and during treatments.

• Drug therapy takes at least 6 -9 months before improvement is perceived. • Physical treatments (electrolysis, waxing, bleaching) may be helpful but repeated treatments are required. • Laser and photothermolysis are more expensive but have longer duration of effect. • However, there is no permanent cosmetic treatment.

Eflornithine • Topical drug that inhibits hair growth. • Inhibits the enzyme ornithine decarboxylase in hair follicles. • Used in conjunction with hormonal therapy or for those who wish to avoid it. • May cause thinning of skin and high-factor sun block is recommended.

Hormonal therapy • Decrease the rate of hair growth and stop further progression of hirsuitism. • Adequate contraception is required in women of reproductive age as trans-placental passage of antiandrogens may disturb the genital development of a male fetus.

1. Dianette • • First line therapy. Ethinyl-oestradiol (35 ug) with cyproterone acetate (2 mg). Higher doses of cyproterone acetate do not confer additional benefit. Effect on acne and seborrhoea is evident in a couple of months.

2. Spironolactone • • Weak diuretic with anti-androgenic properties. Used if contraindications to COCP. Daily dose =25 -100 mg If used as monotherapy , may be associated with menstrual irregularities and progestin therapy is often needed.

3. Oral contraceptives (COCP) • Drosperinone, derivative of spironolactone is contained in the COCP Yasmin and is beneficial for both menstrual cycle control and suppression of hyperandrogenism. • Thromboembolism should be considered for those with PCOS who are overweight.

4. Finasteride and Flutamide • Anti-androgens. • Finasteride blocks conversion of testosterone to dihydro-testosterone. • Flutamide is a peripheral androgen antagonist. • Not widely used due to potential hepatotoxicity.

Management of Menstrual Problems

• In PCOS, intervals between menses > 3 months may be associated with endometrial hyperplasia and later endometrial carcinoma. • Cystic glandular hyperplasia progress in 0. 4% and adenomatous hyperplasia in 18% over 2 -10 years.

In oligomenorrheic women induction of a withdrawal bleed (every 3 -4 months) is advisable using: - • Cyclical gestogens (at least 12 days) • Combined oral contraceptive pills • Endometrial protection by Mirena intrauterine system
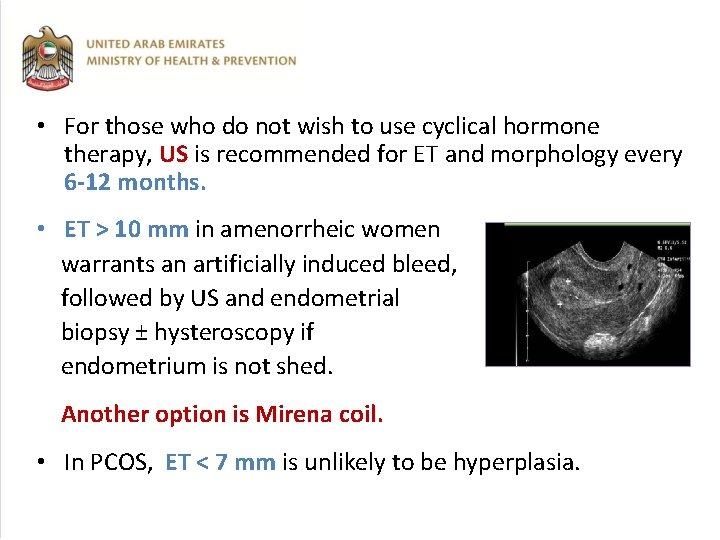
• For those who do not wish to use cyclical hormone therapy, US is recommended for ET and morphology every 6 -12 months. • ET > 10 mm in amenorrheic women warrants an artificially induced bleed, followed by US and endometrial biopsy ± hysteroscopy if endometrium is not shed. Another option is Mirena coil. • In PCOS, ET < 7 mm is unlikely to be hyperplasia.

Management of Anovulatory Infertility

• PCOS accounts for 80 -90% of women with anovulatory infertility. • Infertility in PCOS is also due to the effects of obesity, metabolic, inflammatory and endocrine abnormalities on oocyte quality and fetal development. • Treatment should be deferred till BMI < 35 but if less than 37 yrs with normal ovarian reserve, BMI < 30 is preferable.

Principles of management • Weight loss and optimize health before starting therapy. • 400 mcg folic acid daily and , if obese, 5 mg. • Perform semen analysis before ovulation induction. • Assess tubal patency before commencing therapy. • Induce regular uni-follicular ovulation.

Ovulation induction Oral anti-oestrogens Parenteral gonadotrophin therapy. Laparoscopic ovarian surgery - No randomized studies determine which therapy provides the best chance of an ongoing pregnancy. - ↑risk of OHSS and multiple pregnancy and hence careful monitoring with serial US is needed.

Clomiphene citrate (CC) • First line therapy • Commence on day 2 -5 of cycle and give for 5 days. • If oligo/amenorrhea, exclude pregnancy then induce withdrawal bleed with a progestogen (20 mg/day for 5 -10 days). • Starting dose 50 mg /day and may↑ to 100 mg if no response.

• Doses ≥ 150 mg/day do not appear to be of benefit. • If there is exuberant response to 50 mg/day, ↓ dose to 25 mg/day. • CC induces ovulation in 70 -85 % and 60 -70% should be pregnant by six ovulatory cycles of therapy. • US assessment of follicular growth (risk of multiple pregnancy = 10%).

• CC may cause ↑ LH (40%) and anti-estrogenic effects on endometrium and cervical mucus. • Measure LH on day 8 and if ↑, then alternative therapy as chance of conception ↓ and risk of miscarriage ↑ (LH adversely affects oocyte maturity). • If no pregnancy after 6 -9 normal ovulatory cycles, offer assisted conception (IVF/ICSI).

Aromatase inhibitors (Letrozole) • Inhibition of aromatase enzyme↓ aromatization of androgens to oestrogens that releases the HPA from - ve feedback of estrogen. • Effects on endometrium and cervical mucus are less than with CC. • Good pregnancy rates with ↓ incidence of multiple pregnancy, however, safety needs to be assessed.

Gonadotrophin therapy Indicated in women : • Fail to ovulate with anti-estrogens (CC resistance). • Had response to CC that ↓ chances of conception (↑LH or anti-estrogenic effect on endometrium). Low- dose Step-up Regimen should be used with a daily starting dose of 25 -50 IU of FSH or HMG.

• If no response, dose is ↑after 14 days then by only half the starting dose every 7 days. • Treatment cycles can be 28 -35 days long but the risk of multiple follicular growth and multiple pregnancy is low. • Ovulation is triggered with a single sc injection of HCG 5000 units when there is at least one follicle of at least 17 mm in largest diameter.

• HCG is withheld if ≥ 2 follicles > 14 mm in diameter. • Patients are counselled about OHSS and advised to refrain from sexual intercourse. • If conception failed after : 6 ovulatory cycles in women < 25 yrs 12 ovulatory cycles in women >25 yrs Anovulation is unlikely to be the cause of infertility and assisted conception is indicated.

Insulin sensitising agents • Metformin ↓ hepatic glucose, ↓ insulin secretion and enhance insulin sensitivity at cellular level. • RCT reported limited benefit in enhancing the chance of a live birth. • If added to CC in women with CC resistance, clinical pregnancy rate is ↑ but no improvement in live birth rate.

Surgical ovulation induction Laparoscopic ovarian diathermy (LOD) if : • Fail to respond to CC and persistently hypersecrete LH (preferably if normal BMI). • Unable to attend for intensive monitoring required for gonadotrophin therapy. • Laparoscopy is required for other indications.

• Commonly employed methods include: Monopolar diathermy Bipolar diathermy Laser surgery. • Diathermy points should be ↓ to 4 per ovary for 4 seconds at 40 watts to ↓ periovarian adhesions.

• Instillation of 500 -1000 ml of isotonic solution into the pouch of douglas prevent heat injury to adjacent tissues. • Slim patients with ↑ LH have better clinical and endocrine response. (normalization of androgens and SHBG in 60% of cases).

IVF in PCOS • Not the first line treatment. • Referral for IVF if : Tubal or male factor infertility Failure to conceive despite ovulation. • In women with asymptomatic polycystic ovaries the risk of OHSS is reduced if protocols using Gn. RH antagonist are employed.

Conclusion • PCOS is the most common reproductive endocrine disorder. • Heterogenous condition associated with mutiple ovarian follicles, menstrual irregularity, subfertility, hirsuitism, obesity and mood disturbance. • Insulin resistance, central obesity and dyslipidaemia place women at risk of DM and metabolic problems. • Weight loss is the first line therapeutic intervention.

References • Polycystic ovary syndrome. The Obstetrician and Gynaecologist. 2017; 19: 119 -29 • Polycystic ovary syndrome and the differential diagnosis of hyperandrogenism. The Obstetrician and Gynaecologist. 2013; 15: 171 -6 • Long term consequences of polycystic ovary syndrome. RCOG green-top guideline Nov 2014, no 33

Thank You
- Slides: 60