POISONING DORCAS BIO PHYSICIAN ASSISTANT OUTLINE OF PRESENTATION

POISONING DORCAS BIO ( PHYSICIAN ASSISTANT)

OUTLINE OF PRESENTATION §DEFINITION OF POISONING §EPIDEMIOLOGY §ROUTES OF POISON EXPOSURE §GENERAL APPROACH TO A POISONED PATIENT §SPECIFIC MANAGEMENT OF A POISONED PATIENT §SPECIFIC DRUGS AND THEIR MANAGEMENT §ENVENOMATION §SUMMARY

DEFINITION A poison is any substance that causes harm to the body when it gets into it.

EPIDEMIOLOGY §Over 4 million poisonings America occur annually. § 10% of ED visits and EMS responses involve toxic exposures. § 70% of accidental poisonings occur in children under 6 years old. § 80% of attempted suicides involve a drug overdose. § In Ghana 1000 deaths occur annually, (Ghana Death rate - Demographics, Index Mundi).
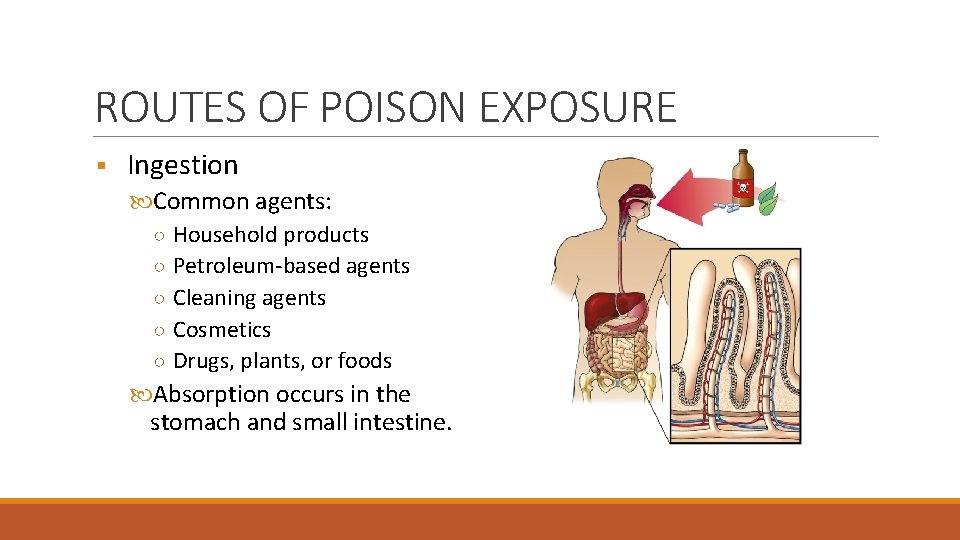
ROUTES OF POISON EXPOSURE § Ingestion Common agents: ○ Household products ○ Petroleum-based agents ○ Cleaning agents ○ Cosmetics ○ Drugs, plants, or foods Absorption occurs in the stomach and small intestine.

CONTD § Inhalation �Common agents § Toxic gases, vapors, fumes, aerosols § Carbon monoxide, ammonia, chlorine § Tear gas § Carbon tetrachloride �Absorption occurs via the capillary— alveolar membrane in the lungs.
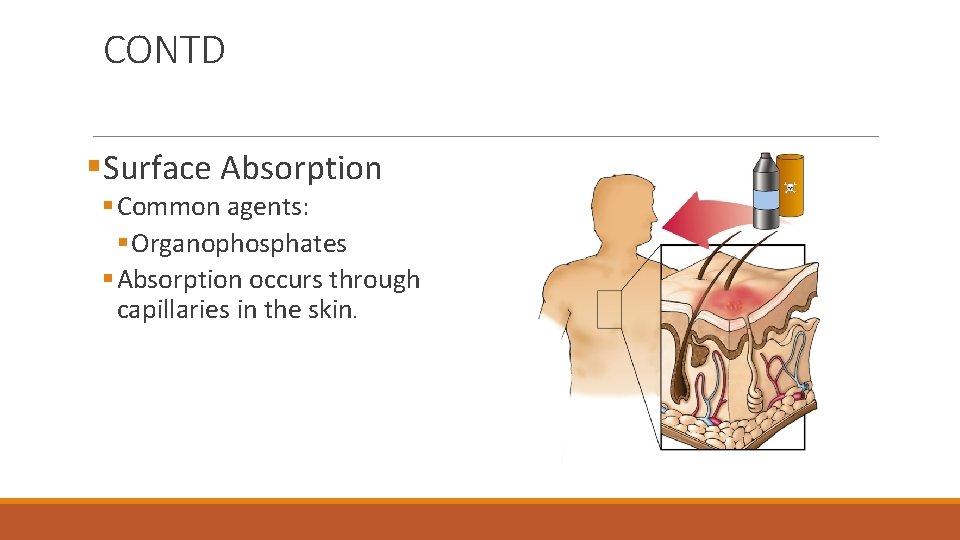
CONTD §Surface Absorption § Common agents: § Organophosphates § Absorption occurs through capillaries in the skin.

PRIMARY ASSESSMENT §A- (Airway) §B-( Breathing) §C- (Circulation) §D-(disability- Is The Patient Conscious Or Comatose) §E-(exposure- Remove Clothing, Irrigate Eyes And Wash Skin With Copious Of Amounts Of Soap And Water)

GENERAL APPROACH TO POISONED PATIENT §History Taking §Physical Examination §Management

HISTORY TAKING §What §When §How much §Any alcohol intake §Any treatment attempt § Why, ( under psychiatric care and what medications) §What is your weight?

PHYSICAL EXAMINATION • A (Airway) • B (Breathing) • Respiratory effects include cough, hoarseness, stridor, dyspnea, retractions, wheezing, chest pain or tightness, rales, decreased RR • C (Circulation) • Cardiac effects include dysrhythmias.

CONTD §D (Disability-AVPU/ Glasgow Coma Scale) §Central nervous system effects include dizziness, headache, confusion, seizure, hallucinations, coma §Glucose level

SPECIFIC MANAGEMENT §Decreasing drug absorption §Increasing drug elimination §Antagonizing the effects ( Antidotes)

DECREASING DRUG ABSORPTION §Ingested poisons: §Gastric lavage: used when a potential amount of toxin is ingested and effective within an hour of poisoning. Contraindicated in acids, alcohol and petroleum products §Activated charcoal: given within an hour of poison ingestion at a dose of 50 g in adults. §Inhaled poisons: give high flow oxygen 12 l/min and bronchodilators if the patient is wheezing

INCREASING DRUG ELIMINATION §Alkaline diuresis : §for serious poisoning with salicylates and theophylline IV 1. 26% sodium bicarbonate infusion is given over 3 hours forced diuresis. §Heamodialysis
ANTAGONIZING THE EFFECTS (ANTIDOTES) §IRON………………. . Desferrioxamine § OPIATES……………. . Naloxone § PARACETAMOL……………. N Acetyl cysteine § HEPARIN………………. . Protamine §CARBON MONOXIDE. . . . Oxygen §ORGANOPHOSPHATES……Atropine/ Pralidoxime §BENZODIAZEPINES…………. Flumazenil
SPECIFIC DRUGS AND THEIR MANAGEMENT. §ANALGESIACS §PARACETAMOL STAGE 1 12 -24 HOURS Nausea, vomiting weakness, fatiguability STAGE 2 24 – 48 HOURS STAGE 3 72 – 96 HOURS Abdominal pain, decreased urine, increased liver enzymes Liver dysfunction STAGE 4 4 – 14 DAYS Liver failure

CONTD §Give acetyl cysteine within 16 hours of ingestion. Loading dose of 140 mg/kg then 70 mg/kg 4 hourly for 16 doses

SALICYLATES §Common Overdose Drug § aspirin § toxicity occurs due to disturbance in acid base balance §Respiratory alkalosis §Metabolic acidosis

SIGNS AND SYMPTOMS • Common Features: – Vomiting, Dehydration, Tinnitus, Vertigo – Sweating, Bounding pulses, Hyperventilation • Uncommon Features: – Confusion, Disorientation, Coma, Convulsions – Hematemesis, Hyperpyrexia, clotting abnormalities, renal failure

MANAGEMENT §Activated Charcoal § Given in those who have taken more than 250 mg/Kg body weight less than 1 hour ago §Gastric Lavage § May be considered in those who have taken more than 500 mg/kg body less than 1 hour ago. Steps must be taken to protect the airway §Urinary Alkalization § increase urinary p. H from 5 to 8 there is a 10 -20 fold increase in the renal salicylate clearance by giving an infusion of Sodium Bicarbonate.

TRICYCLIC ANTIDEPRESSANTS §Amitriptyline §Signs and symptoms §Anticholinergic effects §Dry Mouth, Dry Eyes, Dilated Pupils, Urinary Retention, Blurred Vision, Dizziness, Palpitations, §Cardiac effects( Quinidine effects) §Heart block, tachycardia, bradycardia

MANAGEMENT • Activated Charcoal if more than 4 mg/Kg within 1 hour. – N. B WATCH OUT FOR THE AIRWAY • Correct Hypoxia with Oxygen • Correct Acidosis with sodium bicarbonate when acid base imbalance is suspected

ANTI – DIABETICS §Sulphonylureas: Glibenclamide, Gliclazide §Biguanides : Metformin, Phenformin §Signs and symptoms §Sweating §Confusion §hypoglycaemia

MANAGEMENT §Activated charcoal within 1 hour of ingestion §Gastric lavage §Correct hypoglycaemia using 10% and 20% dextrose

BENZODIAZEPINES §Diazepam, lorazepam §Signs and symptoms §Drowsiness §Dilated pupils §Respiratory depression

MANAGEMENT §Activated charcoal §Gastric lavage §Monitor oxygen saturation and administer oxygen §flumazenil

OPIOIDS §Heroin, morphine , codeine, pethidine §Signs and symptoms §Respiratory depression §Pinpoint pupils §Hypotension §unconciuosness

MANAGEMENT §Monitor oxygen saturation and give oxygen §Give naloxone 0. 8 -2 mg IV every 2 minutes as level of consciousness and respiration increases

ORGANOPHOSPHATES §Insecticides and weedicides §Organic phosphate insecticides cause irreversible inhibition of the enzyme cholinesterase. As result acetylcholine causing excessive parasympathetic. These agents are absorbed by all routes including skin and mucosa. §Signs and symptoms: headache, blurred vision, bradycardia, vomiting, lacrimation, salivation, excessive urination and diarrhea.

MANAGEMENT if substance came into contact with skin and eyes wash thoroughly with water. Atropine Sulphate at a dose of 0. 4 – 0. 4 mg/kg (maximum dose is 1 mg/kg in 24 hours) and repeat half the dose till signs of toxicity disappear

CONTD §Pralidoxime is given at a dose of 25 -50 mg/kg IM or IV in infusion. The dose is given 1 -2 hours then repeated every 6 -12 hours.

ALKALINES ( CAUSTIC SODA) § Typically occurs by ingestion or surface absorption § Slower onset of symptoms allows for longer contact and more extensive tissue damage. §Signs and symptoms § Facial burns § Pain in the lips, tongue, throat, or gums § Drooling, trouble swallowing § Hoarseness, stridor, or shortness of breath § vomiting

MANAGEMENT §Resuscitation : §Airway §Breathing § Circulation §IV Antibiotics: § Aspiration Pneumonia And Oesophageal Rupture

CARBON MONOXIDE §inhalation of gas from an enclosed place. E. g : Gas Stoves, Fire Smoke, Auto Mobile Exhaust §Signs and symptoms §Headache §Cyanosis §Convulsion §Coma

MANAGEMENT §Give oxygen intra nasally 12 l/min. §Administer 100% oxygen if carboxy haemoglobin levels are above 40%. §Hyperbaric oxygen therapy.

ENVENOMATION : SNAKE BITES §Life threatening condition that mostly occurs in farmers, hunters and rice pickers §Venom of snakes contain complex mixture of proteins with enzymatic activity Classification: §Neurotoxin: respiratory arrest §Cytotoxin: soft tissue destruction leading to necrosis and compartment syndrome §Cardio toxins : cardiac arrest as a result of coronary vasoconstriction and AV block §Haemotoxin : alteration in coagulation leading to profuse bleeding

MANAGEMENT §Systemic support: §Iv fluids §Oxygen therapy §Haemo transfusion §Anti-venom: Give polyvalent anti-venom if in doubt but if the snake species is known give a monovalent anti-venom intravenously over 30 minutes.

CONTD §Antibiotics §Tetanus prophylaxis §Necrotic tissue debridement

PREVENTION §Medicines and drugs should be placed in secured locations, e. g. locked cupboard. §Drugs shouldn’t be stored in attractive bottles , e. g. Coke and Fanta bottles. §Hospital must stock anti-venom. §Drugs when not in used must be clearly labelled. §Adding the antidote to the toxin, e. g. combination of Methionine and Paracetamol. §Hazard warning labels on chemicals. §All cases of poisoning, adverse effects of drugs and overdose cases must be documented.

SUMMARY §Get as much history as you can to identify the toxin. §Mainstay of any poisoning is supportive. §Don’t forget ABC. §For specifics substances there may be antidotes. §For specific circumstances consider decreasing the absorption or the elimination of the drug.

THANK YOU
- Slides: 42