POISONING AND TOXIC EXPOSURES TYPES DIAGNOSIS AND GENERAL



















































- Slides: 59

POISONING AND TOXIC EXPOSURES – TYPES , DIAGNOSIS AND GENERAL PRINCIPLES OF MANAGEMENT Department of Pharmacy Practice Chalapathi Institute of Pharmaceutical Sciences, Guntur

What is a Poison ? “Poison is a substance ( solid/ liquid or gaseous ), which if introduced in the living body, or brought into contact with any part there of, will produce ill health or death, by its constitutional or local effects or both. ” Ref- The Essentials of Forensic Medicine and Toxicology Dr. K. Reddy

Poisoning “The development of dose related adverse effects following exposure to chemicals, drugs or other xenobiotics. ” Ref- The Essentials of Forensic Medicine and Toxicology Dr. K. Reddy

EPIDEMIOLOGY WHO (2004) - 3, 46, 000 deaths in a year d/t poisoning. In 2005 – In India 1, 13, 914 estimated cases of poisoning with insecticides Commonest cause in INDIA – Pesticides Reasons – Agriculture based economy - Easy availability pesticides - Poverty

Types of poisoning 1. Acute poisoning – excessive single dose, or several smaller doses of a poison taken over a short interval of time. 2. Chronic poisoning – smaller doses over a period of time, resulting in gradual worsening eg. Arsenic , Phosphorus , Antimony etc.

Nature of poisoning 1. Homicidal – killing of a human being by another human being by administering poisonous substance deliberately. 2. Suicidal – when a person administer poison himself to end his/ her life. 3. Accidental – Eg. Household poisons- nail polish remover , acetone. Depilatories- Barium sulphide 4. Occupational – in professional workers. Eg. insecticides, noxious fumes.

Classification of poisons According to the chief symptoms produced : Corrosives. Systemic Irritants. Miscellaneous 1. Corrosives a) Strong acids- H 2 SO 4 , HNO 3 , HCl b) Strong alkalis- Hydrates & Carbonates of Na+ , K+ & NH 3 c) Metallic salts – Zinc chloride, Ferric chloride, KCN , Silver nitrate, Copper sulphate.

Classification continued…. 2. Irritants a) Inorganic –i) Nonmetallic – Phosphorus, Iodine Chlorine. ii) Metallic – Arsenic, Antimony, Lead. iii) Mechanical – Powdered glass, hair b) Organic Vegetable – Abrus precatorius, Castor, Croton, Calotropis. Animal – Snake & insect venom, Cantharides

Classification continued……. 3. Systemic a) Cerebral CNS depressants – Alcohol, opioids, hypnotics, general anesthetics. CNS stimulants – Amphetamines, Caffeine Deliriant – Datura, Cannabis, Cocaine b) Spinal – Nux vomica c) Peripheral – Conium, Curare d) Cardiovascular - Aconite, Quinine, HCN e) Asphyxiants – CO, CO 2 , H 2 S 4) Miscellaneous – Food poisoning, Botulism.

Routes of administration Inhalational volatile gas, chemical dust, smoke, aerosol. 2. Injectable a) Intra venous – Benzodiazepines, barbiturates, 1. tricyclic antidepressants etc. Intramuscular – Benzodiazepines, opioids etc c) Subcutaneous – Botulinum toxin d) Intra- dermal – Local anaesthetics, b) organophosphates

3. Oral – Corrosives, organophosphorus 4. Through natural orifices- rectum/ vagina/ urethra Abrus precatorius, croton, calotropis 5. Through unbroken skin – organophosphorus, Mercury, Lead

Diagnosis of poisoning History – patient witness Circumstantional evidence Ø Ø suicide note containers & potential toxins at scene of discovery Physical examination Investigations -Biochemical investigations -ECG abnormalities -Radiology -Toxicologic screening

History Patient Ø If person is conscious , & immediately brought to the ED, history may be relevant Ø Mostly patient estimates of drug/ nature of substance ingested are inaccurate. Witness What substance/ substances ? What route/ routes ? What dose/ doses ? When and for how long? H /O psychiatric illness?

Circumstantial evidence Unconscious adults Empty drug containers/ wrappers /tablet neraby ↓ some sort of poisoning Tablet particles staining mouth / clothing Suicide note ↓ Assumption of poisoning

Following conditions should arouse suspicion of poisoning : Ø Sudden appearance of symptoms after food or drink in an otherwise healthy person Ø Symptoms – uniform in character, rapidity Ø Sudden onset delirium, paralysis, cyanosis, collapse etc.

Physical examination General appearance Neurological status- conscious, confused, comatose. Ø Glassgow coma scale Pupillary examination q Normal – Celphos poisoning q Miosis – Opioids, OP poisoning q Mydriasis – TCA, Theophylline, Dhatura, Methanol Convulsions - Ethylene glycol, Lithium, SSRI Muscular fasciculations – OP poisoning

Vital parameters – Cardiorespiratory system PR, BP, RR, Temp Hypotension with bradycardia : Ø Beta blockers, Cyanide, Benzodiazepines, Barbiturates, Opioids, Alchohol , OP insecticides Hypotension with tachycardia : Ø Beta -2 stimulants, Caffeine , Theophylline, Amatoxin containing mushroom

Vital parameters contd…. Hypertension with tachycardia : Ø Sympathomimetics, Ergot alkaloids, Anticholinergics, Alcohol withdrawal Respiratory depression with failure: Ø Barbiturates, Benzodiazepines, Opiates, Sedative - hypnotics, Snake venom Hyperventilation : Ø Amphetamines , Salicylates, Hallucinogens, Cyanide, CO, H 2 S

Vital parameters contd……. . Body tempearture Hypothermia : - Ø Barbiturates, Benzodiazepines, Ethanol, Opiates, Cyclic antidepressants Hyperthermia Ø Amphetamines, : - Alcohol withdrawal, MAO inhibitors, Anticholinergic agents, Salicylates

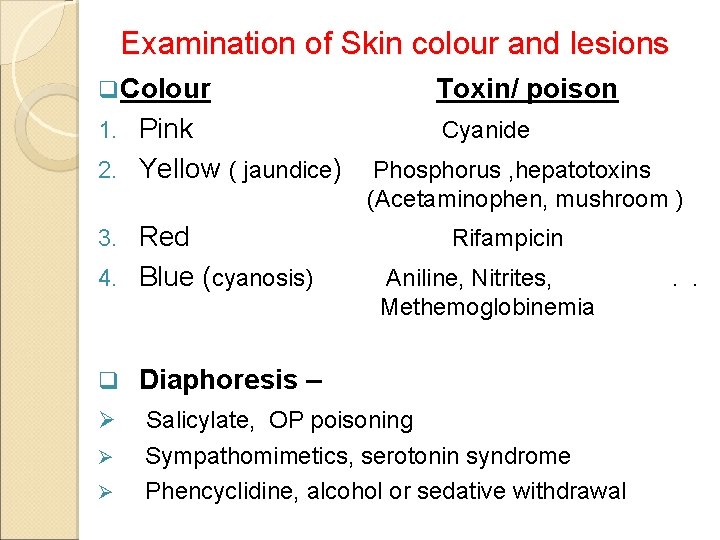
Examination of Skin colour and lesions q Colour Toxin/ poison Pink 2. Yellow ( jaundice) Cyanide 1. Red 4. Blue (cyanosis) 3. Phosphorus , hepatotoxins (Acetaminophen, mushroom ) Rifampicin Aniline, Nitrites, Methemoglobinemia q Diaphoresis – Ø Salicylate, OP poisoning Sympathomimetics, serotonin syndrome Phencyclidine, alcohol or sedative withdrawal Ø Ø . .

Examination of Skin colour and lesions contd…. c. Bruising d. Needle tracks v Diffuse v I/V ecchymosis: § Anticoagulant poisoning § Rodenticides abuse : § Opiates § Amphetamines § Cocaine Ø May be hidden in groin or interdigital spaces

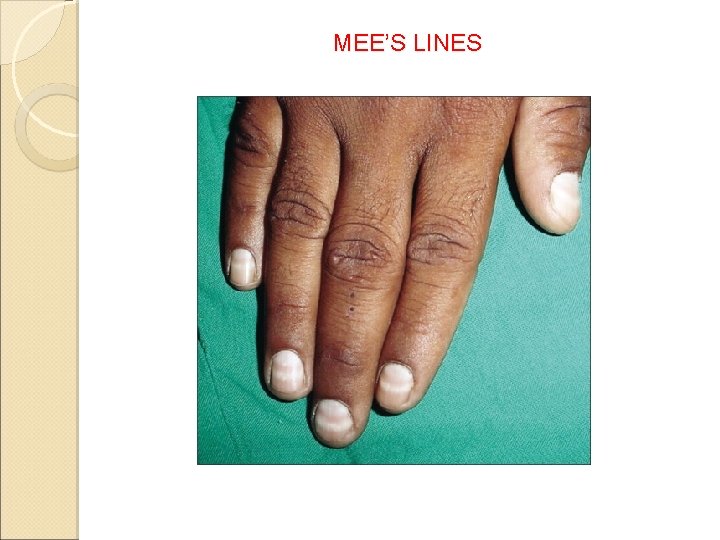
Examination of Skin colour and lesions contd…. e. Hair Ø Hair loss – Chemotheapuetic agents Thallium f. Nails Ø Mee’s lines – Arsenic poisoning Thallium

MEE’S LINES

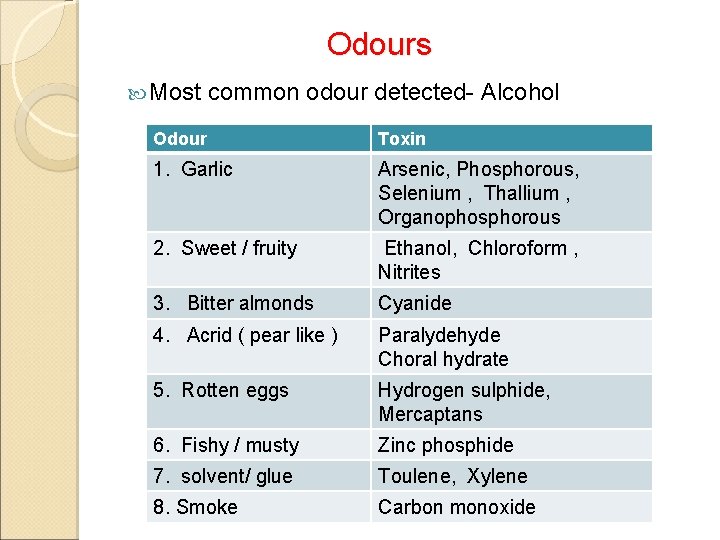
Odours Most common odour detected- Alcohol Odour Toxin 1. Garlic Arsenic, Phosphorous, Selenium , Thallium , Organophosphorous 2. Sweet / fruity Ethanol, Chloroform , Nitrites 3. Bitter almonds Cyanide 4. Acrid ( pear like ) Paralydehyde Choral hydrate 5. Rotten eggs Hydrogen sulphide, Mercaptans 6. Fishy / musty Zinc phosphide 7. solvent/ glue Toulene, Xylene 8. Smoke Carbon monoxide

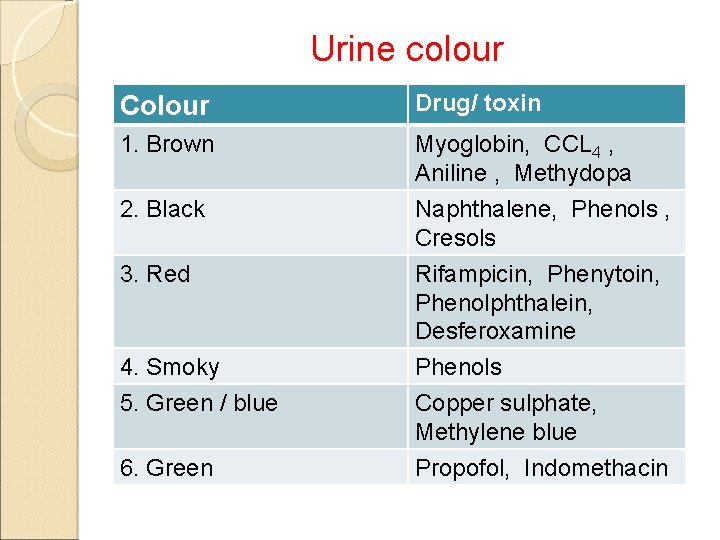
Urine colour Colour Drug/ toxin 1. Brown Myoglobin, CCL 4 , Aniline , Methydopa 2. Black Naphthalene, Phenols , Cresols 3. Red Rifampicin, Phenytoin, Phenolphthalein, Desferoxamine 4. Smoky 5. Green / blue Phenols Copper sulphate, Methylene blue Propofol, Indomethacin 6. Green

Biochemical investigations Hematologic CBC, Platelet count, Coagulation profile ◦ Hemolytic anemia- lead, NSAIDS, Quinidine ◦ Thrombocytopenia- Aspirin, Phenytoin, Procanamide ◦ Coagulopathy- snake venoms, warfarin Liver function tests S. bilirubin , enzymes – AST, ALT , ALP, coagulation profile ◦ Acetaaminophen, sulfonamides, rifampicin, TCA, INH, Renal functions tests ◦ Aspirin, lead, barbiturates, alcohol, amphetamines, copper sulphate

Other Abnormalities Hyperkalemia Ø Digoxin, Cardiac glycosides, Rhabdomyolysis, + sparing diuretics K Hypokalemia Ø Theophylline, Amphetamines, Sympathomimetics Hypernatremia Uncommon in clinical toxicology Ø Large dose of Na. HCO 3 for TCA overdose Ø Correction of life threatening metabolic acidosis Ø Hyponatremia Ø Rare

Biochemical abnormalities contd…… Metabolic acidosis Ø Acetaaminophen, Ethanol, Methyl alcohol, Toulene Metabolic alkalosis Ø Calcium carbonate, Furosemide, Laxative Anion Gap = [ Na+ ] – { [ Cl] +[ HCO 3 ] } Ø Normal – 8 - 12 mmol/ l Increased anion gap : Ø Ethylene glycol Methanol Salicylate poisoning

Biochemical abnormalities contd…. . Osmolar gap Ø Detects the presence of osmotically active susbstances in serum or plasma Ø Calculated osmolality = 2 [ Na+] + [ urea] + glucose 2. 8 18 Eg Ethanol - Osmolality = 2 [ Na+] + [ urea] + glucose + Ethanol 2. 8 18 4. 6

Biochemical abnormalities contd…. . v. Increased osmolar § Acetone § Ethanol § Ethylene glycol § Methanol gap: -

ECG abnormalities Usually non specific ECG abnormality Drugs/ toxins 1. Bradycardia & AV Block Barbiturates, ß- blockers, Antiarrhythmics 2. Ventricular tachyarrhythmias Cardiac glycosides, Fluorides, Membrane active agents, Sympathomimetics 3. QRS prolongation Amantidine , Hyperkalemia 4. QT prolongation Amantadine, Amiodarone, Thallium

Radiological studies Not particularly helpful in diagnosis. May be useful in confirming : Ø Ingestion of metallic objects. Ø Packets of heroin / cocaine ( body packing) Ø Serial chest X-ray - Aspiration pneumonitis, Bio assays of drugs Ø Ø Ø Ø Acetaminophen Acetone Ethylene glycol Methanol Salicylate Phenobarbital Theophylline Lithium ARDS

v. Toxicologic analysis v Urine , blood, gastric contents – confirm or rule out suspected poisoning. v Interpretation requires various methods: v. Thin layer chromatography – Acetaminophen v. Gas liquid chromatography – BZD, Amphetamines v. HPLC- BZD v. Mass spectrometry- Anticonvulsant v. Enzyme assays v RBC cholinestrase , serum cholinestrase – OP poisoning v Pseudocholinestrase levels – OP poisoning

Fundamentals of poisoning management 1. 2. 3. 4. 5. 6. 7. Initial resuscitation and stabilization Removal of toxin from the body Prevention of further poison absorption Enhancement of poison elimination Administration of antidote Supportive treatment Prevention of re - exposure

Management of poisoning contd…. q Initial resuscitation and stabilization – § I/V access – I/V fluids § Endo tracheal intubation - to prevent aspiration Ø Unconscious patients Ø Respiratory depression/ failure § Convulsions- give anticonvulsants q Removal of toxin from the body Copious flushing with water or saline of the body including skin folds, hair Inhalational exposure Ø Fresh air or oxygen inhalation

Prevention of poison absorption G I decontamination Performed selectively, not routinely 1. Ø Ø Ø Gastric lavage Useful IF DONE BEFORE 3 hr of ingestion of a poison Done with water ( except infants – NS), 1: 5000 potassium permangnate , 4% Tannic acid, saturated lime water or starch solution Administering & aspirating 5 ml/kg through a No. 40 F orogastric tube ( No. 28 F – children) or Ewald’s tube Position – Trendelenburge & left lateral position Performed until clear fluid is obtained or a maximum of 3 L

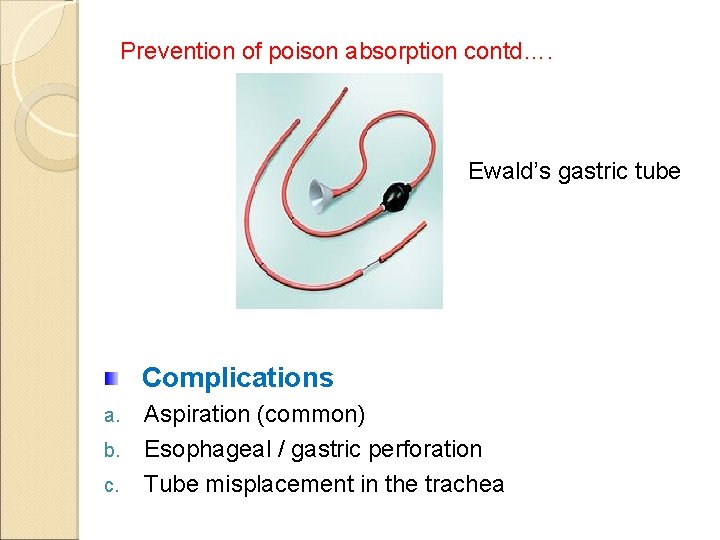
Prevention of poison absorption contd…. Ewald’s gastric tube Complications a. b. c. Aspiration (common) Esophageal / gastric perforation Tube misplacement in the trachea

Prevention of poison absorption contd…. Contraindications a. b. c. d. e. Corrosive poisoning – GE perforation Petroleum distillate ingestants- Aspiration pneumonia Compromised unprotected airway Esophageal / gastric pathology Recent esophageal / gastric surgery Lavage decreases ingestant absorption by an average of : - Ø Ø Ø 52 % - if performed within 5 mins of ingestion 26 % - if performed at 30 mins 16 % - if performed at 60 mins

Prevention of poison absorption contd…. 2. Ipecac Syrup induced emesis Used for home management of patients with : Ø Accidental ingestions Ø Reliable history Ø Mild predicted toxicity Aministered orally Dose : Ø 30 ml – adults Ø 15 ml – children Ø 10 ml – small infants

MOA Ø Ipecac irritates the stomach & stimulates CTZ centre. Ø Vomiting occurs about 20 min after administration Ø Dose may be repeated if vomiting does not occur Side effects a. Protracted vomiting Contraindications a. b. c. d. Gastric / esophageal tears or perforation Corrosives CNS depression or seizures Rapidly acting CNS poisons ( cyanide, strychnine, camphor )

Prevention of poison absorption contd……. 3. Activated charcoal Ø Greater efficacy Ø Less invasive Ø Given orally as a suspension ( in water ) or through NG tube Ø Dose – 1 g/kg body wt. Ø Charcoal adsorbs ingested poisons within gut lumen allowing charcoal- toxin complex to be evacuated with stool or removed by induced emesis / lavage

Prevention of poison absorption contd… Ø Indications- Barbiturates, Atropine , Opiates, Strychnine Ø Contraindications - Mineral acids, alkalis, cyanide, fluoride , iron Side effects a. b. Nausea , vomiting, diarrhoea or constipation May prevent absorption of orally administered therapeutic agents Complications a. b. Aspiration – vomiting Bowel obstruction

Prevention of poison absorption contd…. 4. Whole bowel irrigation Ø Administration of bowel cleansing solution containing electrolytes & polyethylene glycol Ø Orally or through gastric tube Ø Rate – 2 L/ hr ( 0. 5 L /hr in children) Ø End point- rectal fluid is clear Ø Position – sitting Indication : Ø Slow or enteric coated medications Ø Packets of illicit drugs Ø Heavy metals Ø Iron , Lithium

Contraindications Bowel obstruction b. Ileus c. Unprotected airway a. Complications: a. Bloating b. Cramping c. Rectal irritation

5. Cathartics Promote rectal evacuation of GI contents Ø Most effective – Sorbitol Ø Dose – 1 -2 g/kg Ø Salts – Disodium phosphate, Magnesium citrate & sulfate, Sodium sulfate Ø Saccharides – Mannitol, Sorbitol Ø Side effects – Abdominal cramps, nausea vomiting Complications – Excessive diarrhoea, Hypermagnesemia C/I – Corrosives Pre existing diarrhoea

Enhancement of elimination of poison 1. Alkalization of urine Ø Urine p. H ≥ 7. 5 Ø Urine output 3 -6 ml/kg Ø 5% Dextrose in 0. 45 NS containing 20 – 35 meq /L Of Na. HCO 3 to an IV solution Ø Uses – Chlorpropamide, Phenobarbital, Sulfonamides, Salicylates C/I : Congestive heart failure b. Renal failure c. Cerebral edema a.

2. Acidification of urine Enhance elimination of weak bases such as Phencyclidine & Amphetamine Ø Not used anymore Ø ØS /E- Metabolic acidosis, Renal damage 3. Extra corporeal removal Dialysis Ø Acetone, Barbiturates, Bromide, Ethanol, Ethylene glycol, Salicylates, Lithium Ø Less effective when toxin has large volume of distribution (>1 L/kg), has large molecular weight, or highly protein bound

Elimination of poison contd…. Peritoneal dialysis Ø Alcohols , long acting salicylates, Lithium Exchange transfusion Ø Indications a. b. c. d. Ø Fatal , irreversible toxicity Deteriorating despite aggressive supportive therapy Dangerous blood levels of toxins Liver or renal failure Eg. Arsine or Sodium Chlorate poisoning

Elimination of poison contd…. 4. Chelation Heavy metal poisoning Ø Complex of agent & metal is water soluble & excreted by kidneys Ø Eg. BAL, EDTA, Desferrioxamine, DMSA Ø § § BAL – Arsenic, Lead, Copper, Mercury EDTA- Cobalt, Iron, Cadmium Desferrioxamine – Iron DMSA- Lead, Mercury

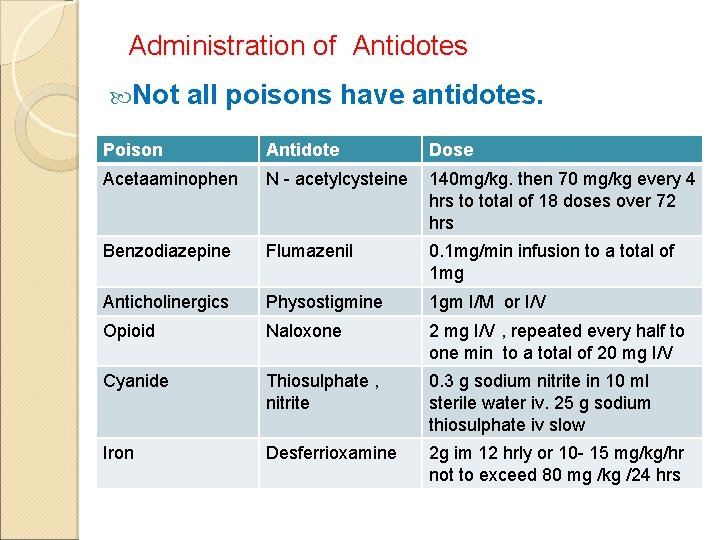
Administration of Antidotes Not all poisons have antidotes. Poison Antidote Dose Acetaaminophen N - acetylcysteine 140 mg/kg. then 70 mg/kg every 4 hrs to total of 18 doses over 72 hrs Benzodiazepine Flumazenil 0. 1 mg/min infusion to a total of 1 mg Anticholinergics Physostigmine 1 gm I/M or I/V Opioid Naloxone 2 mg I/V , repeated every half to one min to a total of 20 mg I/V Cyanide Thiosulphate , nitrite 0. 3 g sodium nitrite in 10 ml sterile water iv. 25 g sodium thiosulphate iv slow Iron Desferrioxamine 2 g im 12 hrly or 10 - 15 mg/kg/hr not to exceed 80 mg /kg /24 hrs

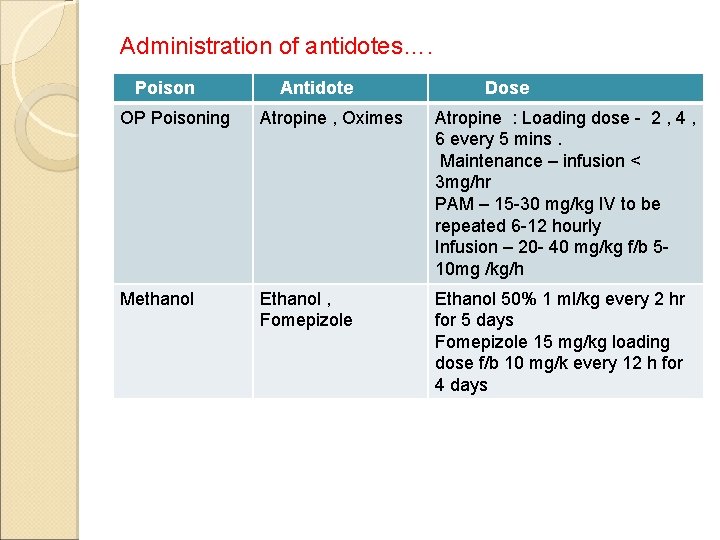
Administration of antidotes…. Poison Antidote Dose OP Poisoning Atropine , Oximes Atropine : Loading dose - 2 , 4 , 6 every 5 mins. Maintenance – infusion < 3 mg/hr PAM – 15 -30 mg/kg IV to be repeated 6 -12 hourly Infusion – 20 - 40 mg/kg f/b 510 mg /kg/h Methanol Ethanol , Fomepizole Ethanol 50% 1 ml/kg every 2 hr for 5 days Fomepizole 15 mg/kg loading dose f/b 10 mg/k every 12 h for 4 days

Supportive care Hemodynamic support- Hypotension unresponsive to volume expansion – t/t with ionotropes Correction of temperature abnormalities Hypothermia – Rewarming of the patient Ø Active / passive methods Ø External / internal methods ◦ Passive external rewarming- blankets / sleeping bags ◦ Active external warming- hot water bottles, heating blankets , forced air warming ◦ Invasive core rewarming- peritoneal dialysis, hemodialysis, gastric or rectal lavage

Supportive care contd…. Hyperthermia ◦ Externally – immersion in iced saline bath, tepid sponging ◦ Internally – gastric / peritoneal lavage Correction of metabolic derangements ◦ ◦ Hyperkalemia – Calcium gluconate 10% 10 -20 ml Insulin 10 units with 50 g of 50% dextrose Na. HCO 3 1 mmol/kg , beta-2 agonists ◦ Hypokalemia ◦ K < 2. 5 mmol/l with symptoms - I/v KCL 20 -30 mmol/h ◦ K < 3. 5 but > 2. 5 mmol/l with no symptoms – KCL 20 -40 mmol every 4 -6 hr

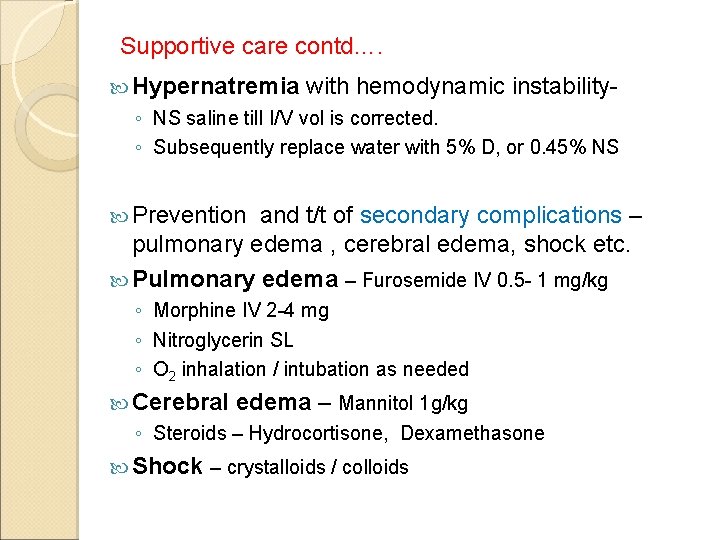
Supportive care contd…. Hypernatremia with hemodynamic instability- ◦ NS saline till I/V vol is corrected. ◦ Subsequently replace water with 5% D, or 0. 45% NS Prevention and t/t of secondary complications – pulmonary edema , cerebral edema, shock etc. Pulmonary edema – Furosemide IV 0. 5 - 1 mg/kg ◦ Morphine IV 2 -4 mg ◦ Nitroglycerin SL ◦ O 2 inhalation / intubation as needed Cerebral edema – Mannitol 1 g/kg ◦ Steroids – Hydrocortisone, Dexamethasone Shock – crystalloids / colloids

Prevention of re- exposure Adult education – instructions regarding safe use of medications & chemicals Notification of regulatory agencies - in case of environmental or workplace exposure Psychiatric referral- depressed or psychotic patients should receive psychiatric assessment, disposition & follow-up

Prevention of re- exposure Child proofing- In house hold where children live or visit, alcohols, medications, household products , non edible plants should be kept out of reach or in locked, child proof containers.

Summary Poisoning a common problem in our country A high index of suspicion required to diagnose For any poisoning the mainstay of treatment is supportive care Follow the A, B, C Don’t panic and follow a plan of action Decreasing absorption Enhancing elimination Neutralising toxins

REFERENCES 1. 2. 3. 4. 5. 6. Critical care toxicology: Diagnosis and Management of the Critically Poisoned Patient. Jeffery Brent ; 2 nd edition. Harrison’s Principles of Internal Medicine. 16 th edition, Vol 2: part 16; Poisoning, Drug overdose, and Envenomation. The Essentials of Forensic Medicine and Toxicology. Dr. K. Reddy , Section II Toxicology; 25 th edition International Programme On Chemical Safety, Guidelines On The Prevention Of Toxic Exposure ; WHO 2004 www. biomedcentral. com – Official data , D. Gunnell, 2007 Critical Care, Joseph M. Civetta ; 4 th edition

THANK YOU