PNEUMOTHORAX MANAGEMENT IN A NEONATE By Nicole Stevens

PNEUMOTHORAX MANAGEMENT IN A NEONATE By: Nicole Stevens (RN, RM, NICU cert. )
Pnuemothorax • Definition • Pathophysiology • Risk Factors • Signs & symptoms • Diagnosis • Nursing management • Medical management • Prognosis • Case Study • References

Definition • A pnuemothorax is a type of pulmonary air leak. When air dissects from an alveolus, it follows the tracheobronchial tree and may accumulate in different areas: • Pneumothorax: air in the pleural space • Pneumomediastinum: air in the mediastinum (centre of chest, bordered by lung walls on each side, spine at the back, chest wall at the front and diaphragm below) • Pneumopericardium: air in the space surrounding the heart • Subcutaneous emphysema: air in the subcutaneous tissue • Pneumoperitoneum: air in the peritoneal space (3)
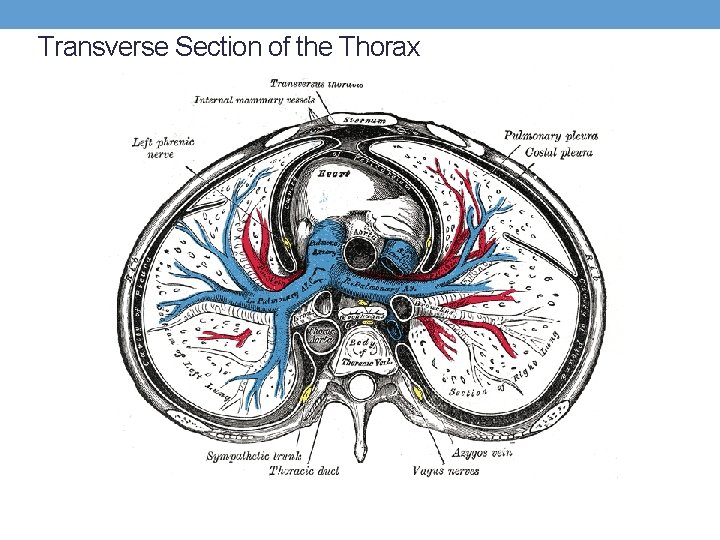
Transverse Section of the Thorax

Pneumothorax • Refers to the presence of air or gas in the pleural cavity between the visceral and parietal pleura, which results in violation of the pleural space. (1) • Can be life threatening • Can vary in severity from being able to be conservatively managed, to requiring insertion of an intercostal catheter (ICC).

Risk Factors Those at risk fall into 3 categories: • Healthy term neonates • Neonates with pulmonary disease • Neonates receiving positive-pressure support (CPAP, ventilation) Why are healthy term neonates at risk? : • Generate pressures of 40 – 80 cm of water for first breath • Therefore a spontaneous air leak can be occur in 2 – 10% of newborns

Risk Factors Pulmonary disease: • Such as RDS, result in stiff, non-compliant lungs, that require higher pressures for alveolar ventilation • Aspiration syndromes cause a ball-valve obstruction of debris with distal air trapping (meconium, milk, amniotic fluid, blood and mucous) • Hypoplastic lungs create a risk for air leaks because lung growth and development are abnormal and the lungs are stiff and non-compliant (diaphragmatic hernia, oligohydramnios) • Alveolar rupture (eg. with PIE), is associated with positive pressure ventilation

Risk Factors Neonates receiving positive pressure ventilation are at risk: • Can result in overdistention with alveolar rupture and air dissection • ETT displacement can increase risk • The administration of surfactant has lowered the incidence of pnuemothorax in ventilated neonates. Prevention: • Use the lowest pressures possible to achieve physiological results • Use synchronised ventilation and volume guarantee if available • Consider high frequency ventilation options, if conventional ventilation not effective, or if high pressures are needed.
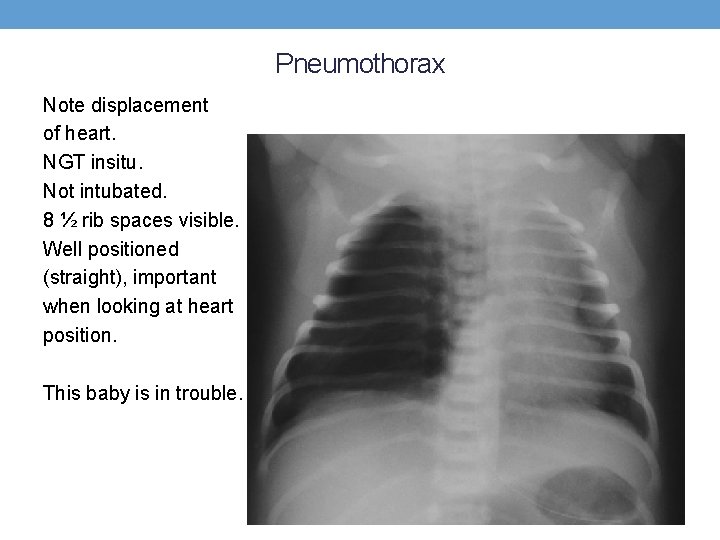
Pneumothorax Note displacement of heart. NGT insitu. Not intubated. 8 ½ rib spaces visible. Well positioned (straight), important when looking at heart position. This baby is in trouble.
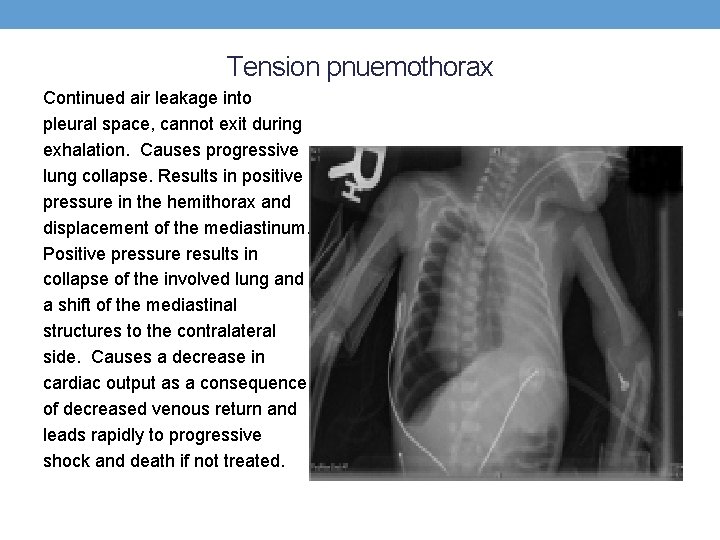
Tension pnuemothorax Continued air leakage into pleural space, cannot exit during exhalation. Causes progressive lung collapse. Results in positive pressure in the hemithorax and displacement of the mediastinum. Positive pressure results in collapse of the involved lung and a shift of the mediastinal structures to the contralateral side. Causes a decrease in cardiac output as a consequence of decreased venous return and leads rapidly to progressive shock and death if not treated.

Signs & Symptoms • Asymptomatic air leaks can occur in term neonates; these frequently require no treatment and resolve spontaneously in 24 – 48 hours. In more significant cases, typical symptoms seen: • Irritability • Sudden deterioration with desaturation • Increase in respiratory distress • Diminished chest movements • Drop in blood pressure • Colour change • Blood gases may reflect hypoxia, respiratory and/or metabolic acidosis

Signs & Symptoms & diagnosis • Unequal or decreased air entry • Displaced apex beat • Transillumination (not always reliable especially in term/oedematous infants) • CXR will confirm diagnosis (but not always a quick turn around time to have performed)

Medical Management Prepare for needle aspiration or ICC insertion Pain relief: • Oral sucrose • Infiltration of insertion site with 1% lignocaine before preparing and draping the field • IV morphine bolus and/or infusion In an emergency can do a needle aspiration: • 21 g butterfly needle, 3 way tap, 10 m. L syringe, alcohol swab, sterile gloves • Infant supine, insert over the top of the rib in the 2 nd or 3 rd intercostal space (mid clavicular). Aspirate air into syringe, expel using 3 way tap, repeat as required until air all removed.

Medical Management • Following needle aspiration an ICC will need to be inserted for ongoing management • See neonatal handbook, or own hospitals clinical practice guidelines for procedure instructions. • Under controlled circumstances effort is generally made to perform the insertion in line with the auxilla (for cosmetic reasons). • The ICC will need to be connected to a Heimlich valve or an underwater seal drainage set. • Familiarise yourself with what equipment your units have because in a high anxiety situation you don’t want to be playing guessing games on what goes where!!

Nursing roles • Have equipment ready to attach to ICC • Keep end sterile and hand to doctor when they are ready to attach • Set suction as required if using underwater seal drainage (until water bubbling gently in chamber). Appropriate volume of water needs to be added to chamber as indicated in instructions. • Continue with observations • Ensure pain relief is adequate • Counsel parents • Handover to NETS nurse • Copy appropriate paperwork for transfer

Prognosis • If it is an isolated event and treatment, if required, is initiated early, the prognosis is excellent • The rate of recurrence can be as high as 30% • Patients with cystic fibrosis have an especially high rate of recurrence • If other trauma was sustained at the same time or tension pnuemothorax occurred with subsequent shock and hypoperfusion, the prognosis worsens. • If the patient was hypoxic for a long period there may be brain injury. (1)

1. Case Study: Baby BJ • Antenatal hx: 26 yr old, G 2 P 1, previous LUSCS (breech); bld grp O +ve, serology neg. GDM on insulin; gestational ITP (maternal platelets on day of delivery 82) • Delivery hx : APH, breech until 2/52 ago, decision to perform LUSCS, no labour. Pink liquor. • Baby: cried at 20 secs, then apnoeic, IPPV for 1 min, then good respiratory effort • Apgars 9 & 9. Birth weight: 2670 g

2. Baby BJ • For admission to SCN from theatre, Issues: • Prematurity • Risk of hypoglycaemia • ? RDS • Maternal ITP • Breech until late in pregnancy Plan: • Observe resp. status, aim Sa. O 2 above 91%; BSL at 1 hr, feed if able then (dependent on resp effort); otherwise IV insertion, 10% dextrose and antibiotics

3. Baby BJ • Admitted to SCN at 1840 hrs. Hep B, Vit K given • Initial Gas: p. H: 7. 136, PCO 2: 78. 9, HCO 3: 26. 6, BE: -2, Lactate: 1. 6; TBG: 1. 7. CRP: <3, FBE: NAD (plt: 200) Plan: • IV bung inserted, 10% dextrose commenced and 2 m. L/kg bolus given (recheck TBG in 30 mins) • Hypoglycaemia resolved and not an ongoing issue • IV antibiotics commenced (Benpen 12/24, 60 mg/kg & Gent 36/24, 5 mg/kg) • Commenced CPAP of 6 cm/H 2 O; Fi. O 2: 25% at 2000 hrs • NETS notified of baby on CPAP – keep for now • CPAP increased to 7 at 2245 hrs, grunting

4. Baby BJ • Remained stable in a CPAP of 7 overnight, intermittent grunt and mild work of breathing. Fi. O 2 at 21 -23%. • CXR and bloods done 1630 hrs (CRP 4. 7, FBE NAD, plt: 167) • Reduced to CPAP of 6, in air • Parents and sibling visiting • Urine output at 1 m. L/kg/hr • Next night: increased WOB, ? Apnoeic episode, febrile, tachypnoeic, no increase in O 2 requirement • Xray taken


6. XRAY interpretation (@ 1643 hrs) • Bilateral but diffuse reticular granular densities • Lungs do not appear hyperinflated • No pleural effusions • Heart is not enlarged • NG tube is noted, tip below L) hemidiaphragm Impression: findings would favour hilar membrane disease (RDS), with infection also in the differential

7. Baby BJ (1/7) • CPAP increased to 7 in the AM (Cap. G p. H: 7. 16, CO 2: 77) • Excessive handling around time gas collected, GNC, bloods etc. • CPAP reduced to 5 later in the afternoon, in air mild WOB (p. H 7. 34, p. CO 2 47) • Generalised oedema noted; Urine output increasing (3. 5) • Phototherapy commenced (SBR 158 at 40 hrs of age) • OPos group, coombs neg • Hungry, irritable at times, having small amounts of EBM as available for comfort, taking well. • Had been febrile overnight (? Environmental), CRP 3. 0

8. Baby BJ (1/7 cont…) • Genta level taken prior to the 2 nd dose because of concerns regarding renal function (urine output still low in the morning when dose due, significant oedema still present and Na level 135) • Genta trough level: 1. 4 so dose withheld. Nursing issues: • Weigh nappies of babies on CPAP especially in first couple of days, once diuresis evident and baby stable consider discontinuing • Be mindful of renal function when giving genta as it is metabolised in the kidneys and levels may stay high.

9. Baby BJ (1/7 cont. . ) • Very unsettled 1700 hrs, crying++, not able to settle. • Increased WOB noted and slight O 2 requirement (25%) • Asked paed to r/v • Significant deterioration (colour change, desaturation, O 2 up to 100%) at approx. 1900 hrs, following an unsettled period. Registrar in attendance, transilluminated appeared to be a pnuemothorax, CXR attended to – confirmed pnuemothorax, consultant called. • Preparation for insertion of intercostal catheter • Morphine bolus given & sucrose given • Pigtail catheter inserted by registrar at 1945 hrs


11. Xray interpretation (1/7 @ 1914 hrs) • Large right sided pneumothorax • Displacement of the mediastinal contents towards the left • Air space opacity in the left lung is increased likely to be due to a degree of compression from the pnuemothorax Baby had an initial deterioration then stabilised slightly. Investigations done, requiring 50 – 100% oxygen. Decision made to go straight to ICC insertion rather than needle first. 2 paediatricians present during this time. Paediatricians prepared to needle if further deterioration. Preparations also made for intubation if required.


13. Xray interpretation (1/7 @ 2006 hrs) • R) pneumocath noted (pigtail catheter used) • No residual pneumothorax • Heart not enlarged, and cardiothymic contour normal • NG tube seen with tip below the level of the diaphragm • Bilateral air space opacities in both lungs are unchanged from previous SIGNIFICANT IMPROVEMENT INSTANTLY AS CHEST DRAIN INSERTED – AUDIBLE HISS HEARD!

14. Baby BJ • NETS called to retrieve, on their way • Gas (p. H 7. 17, CO 2 78) • 2205 hrs NETS arrived • Morphine infusion commenced • Still on CPAP, apnoeic episode when being examined by NETS doctor • Decision to intubate for safety for transport • Intubated/ventilated


16. Xray interpretation (2/7 @ 0028 hrs) • R) sided pleural catheter insitu • Air space opacity in both lungs unchanged • ET tube is seen with tip at the level of T 4 • NG tube is seen with tip below diaphragm • Heart size normal • No residual pneumothorax

17. Baby BJ • Gas (after intubation/ventilated): p. H: 7. 32, p. CO 2: 48, HCO 3: 25, BE: -1. 7, Lact: 2. 5 • Prepared for transport • Left at 0100 hrs Outcome: • Returned to BHS the next day, self ventilating in air, ICC out, NGT for feeds, IVT weaning. • Established feeds over the next 2 weeks and went home doing very well.

References • (1) Gluckman, W. DO, MBA, FACEP. (2013). Paediatric Pneumothorax. http: //emedicine. medscape. com/article/1003552 • (2) NETS handbook (Pneumothorax Drainage) www. netsvic. org. au/nets/handbook • (3) Fernandes, C. J. (2014) Pulmonary air leak in the newborn http: //www. uptodate. com/contents/pulmonary-air-leak-in-the-newborn • Merenstein, G. B. & Gardner, S. L. (2006). Handbook of Neonatal Intensive Care. 6 th Edition. Mosby, Elsevier.
- Slides: 34