PLEURAL EFFUSIONEMPYEMAPNEUMOTHORAX Dr Alpana K Somale Lecturer Department

























- Slides: 37

PLEURAL EFFUSIONEMPYEMAPNEUMOTHORAX Dr Alpana K Somale Lecturer Department of Pediatrics , B. Y. L. Nair Hospital Dr Alpana K Somale, lecturer 1

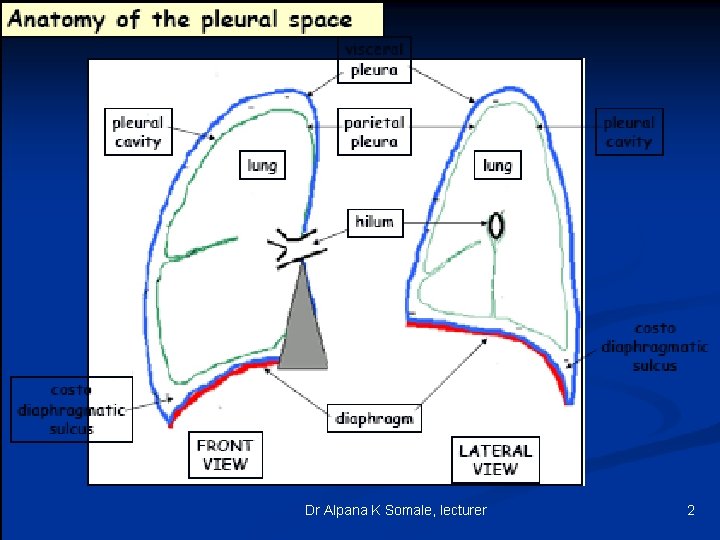
Dr Alpana K Somale, lecturer 2

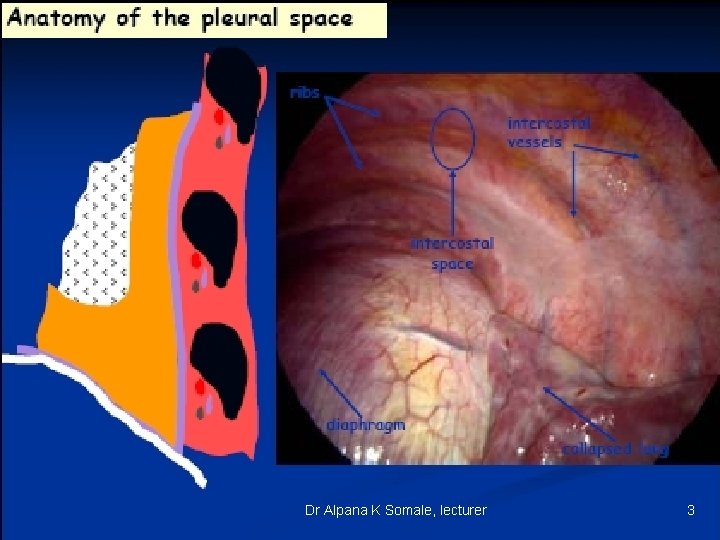
Dr Alpana K Somale, lecturer 3

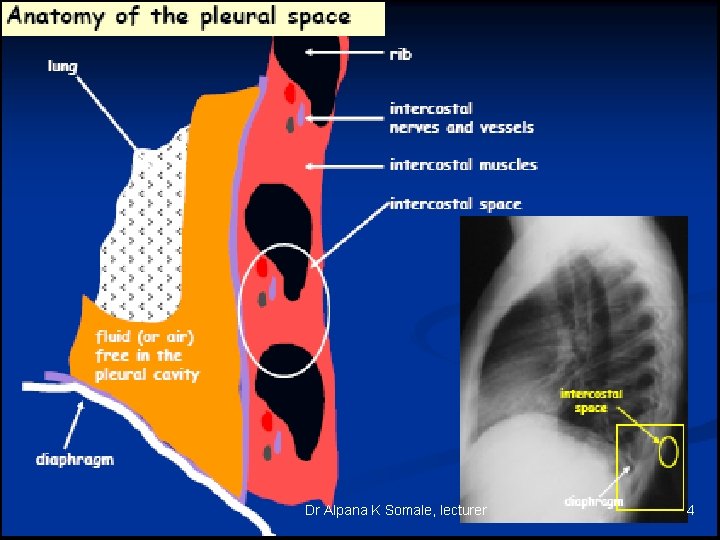
Dr Alpana K Somale, lecturer 4

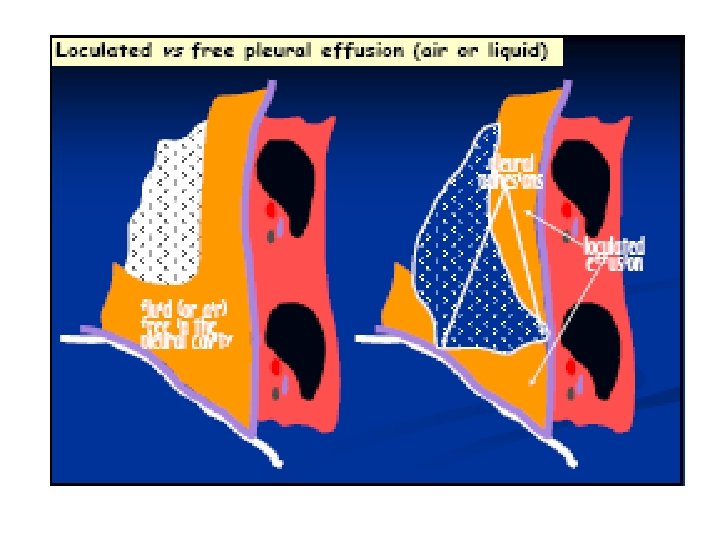
Dr Alpana K Somale, lecturer 5

History n n n Dyspnea (most common) Mild, non-productive cough Severe cough with sputum or blood u Pneumonia vs. bronchial lesion Constant chest well pain u Cancerous invasion of chest wall Pleuritic chest pain u PE vs. inflammatory pleural effusion Dr Alpana K Somale, lecturer 6

Physical Exam n n n Decreased breath sounds Dullness to percussion Decreased tactile fremitus Pleural friction rub Mediastinal shift away from the effusion Egophany (E to A) Dr Alpana K Somale, lecturer 7

Causes n n n CHF Malignancy Infection PE Others include hepatic cirrhosis, hypoalbuminemia, collagen vascular dz, TB, trauma, chylothorax, radiation, or pancreatitis Dr Alpana K Somale, lecturer 8

Pathophysiology n n n ↑ Hydrostatic Pressure (e. g. CHF) ↑ Vascular Permeability (e. g. Pneumonia) ↓ Oncotic Pressure (e. g. Nephrotic syndrome ↑ Intrapleural Negative Pressure (e. g. atelectasis) ↓ Lymphatic drainage (e. g. mediastinal carcinomatosis) Cotran, Ramzi, Vinay Kumar, Tucker Collins. Robins Pathologic Basis of Disease. Philadelphia: Elsevier, 1999. Dr Alpana K Somale, lecturer 9

Workup n n CXR/CT Thoracentesis Lab studies on fluids include protein, LDH, cytology, cell count, specific gravity, p. H, amylase, glucose, Gram’s stain, bacterial/fungal cultures u Plasma LDH and protein u AFB stain and Cx if TB suspected u If CV dz suspected, send for RF & ANA u Dr Alpana K Somale, lecturer 10

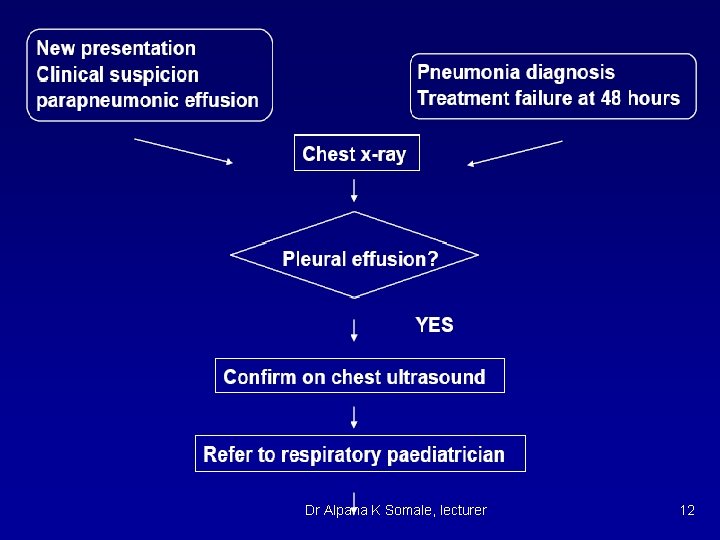
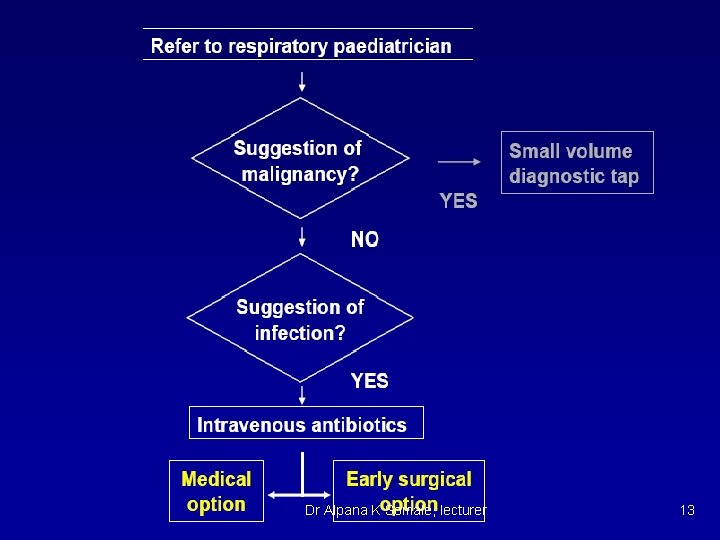
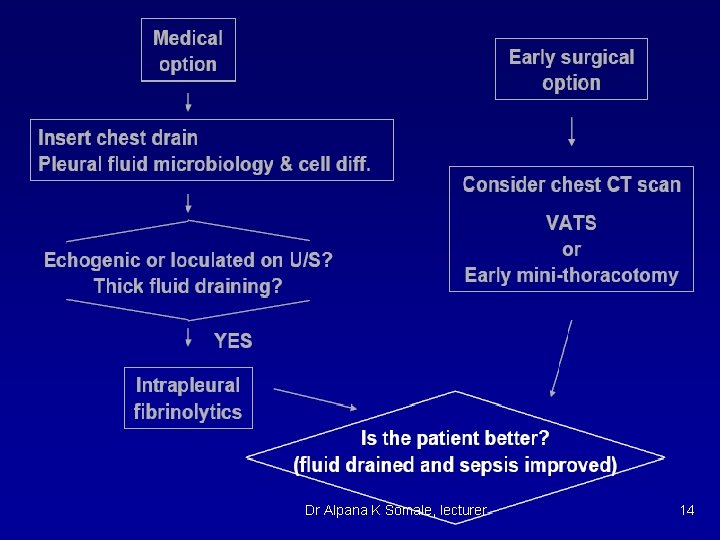
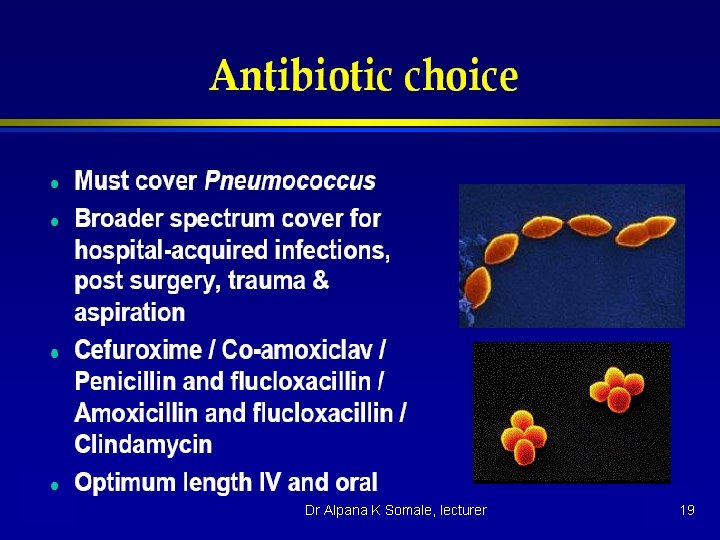
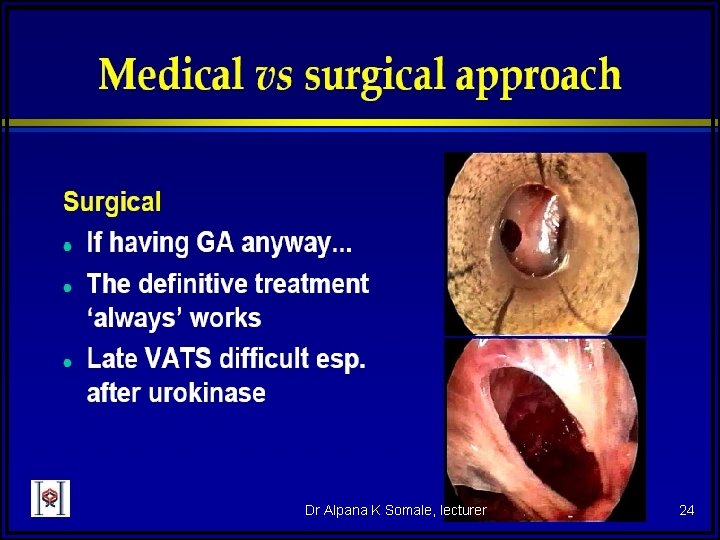
Treatment n n Treat underlying dz (such as CHF, nephrotic syndrome) if transudative fluid Exudative fluids u n n Drain and pleurodese for palliative treatment vs chemo if caused by malignancy Drain if empyema or causing severe respiratory symptoms Surgery Decortication for thick areas restricting breathing u Drainage of loculated areas u Pleuroperitoneal shunts for recurrent effusions u Dr Alpana K Somale, lecturer 11

Dr Alpana K Somale, lecturer 12

Dr Alpana K Somale, lecturer 13

Dr Alpana K Somale, lecturer 14

Dr Alpana K Somale, lecturer 15

Dr Alpana K Somale, lecturer 16

Dr Alpana K Somale, lecturer 17

Dr Alpana K Somale, lecturer 18

Dr Alpana K Somale, lecturer 19

Dr Alpana K Somale, lecturer 20

Dr Alpana K Somale, lecturer 21

Dr Alpana K Somale, lecturer 22

Dr Alpana K Somale, lecturer 23

Dr Alpana K Somale, lecturer 24

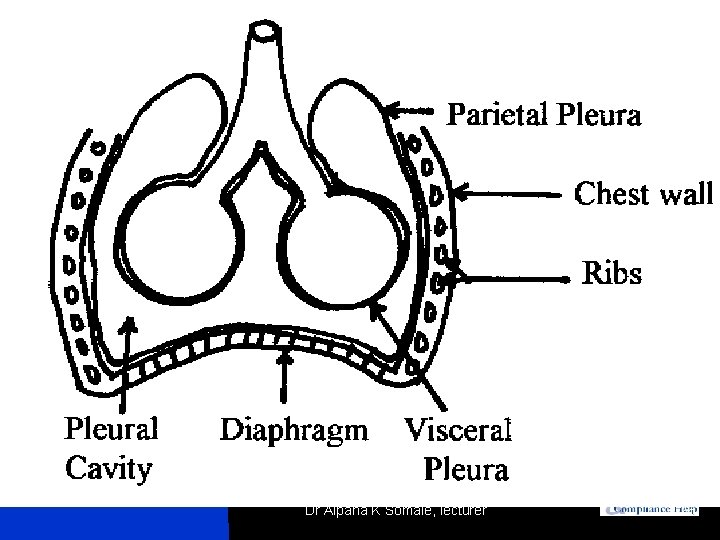
Pneumothorax Defined n Definition – “What? ” u u n “Pneumo”- gas “Thorax” – chest cavity Analagous to Pleural Effusion Pathophysiology – “How? u Pleural space « « « u Normal inspiration « « u Baseline (-) pressure space Parietal Pleura Visceral Pleura Diaphragm Transmit (-) Pressure Pathologic inspiration XS gas disrupts transmission of (-) pressure « Dr Alpana K Somale, lecturer 25

Dr Alpana K Somale, lecturer 26

Types of Pneumothorax n Spontaneous Pneumothorax u Primary bleb « u rupture of subpleural “Jimmy is a tall, wiry, 21 -year old male, who plays trombone in the marching band…. ” Secondary disease underlying lung/pleural #1 – emphysema « Chronic bronchitis, asthma, TB, … « n Traumatic Pneumothorax u Open Dr. Chest Alpana Kwall Somale, lecturer « is penetrated : outside air 27

Types of Pneumothorax 2 n n Tension Pneumothorax u “Ball-valve mechanism” u Injury to pleura creates a tissue flap that opens on inspiration and closes on expiration u One of our own patients Variations u Hemo-thorax u Chylo-thorax « Injury to thoracic duct u Empyema « Parapneumonic effusions in communityacquired pneumonia Dr Alpana K Somale, lecturer 28

Symptoms n n Dyspnea Pleuritic chest pain u n n Nerve endings at pleural capsule Sense of impending doom Sudden onset Tension pneumothorax u Spontaneous pneumothorax u Dr Alpana K Somale, lecturer 29

Physical Exam Signs n Unstable patients vs. Stable patients u n n n Vital Signs Asymmetric chest expansion Deviated trachea Diminished breath sounds unilaterally Hyper-resonance unilaterally Decreased tactile fremitus Dr Alpana K Somale, lecturer 30

Diagnosis n Unstable patient u Thoracentesis n Stable patient u CXR Rapid release of air « Vital signs stabilize rapidly « Dr Alpana K Somale, lecturer Monitor size by measuring distance from lateral lung margin to chest wall « Be sure that pneumothorax is not expanding « 31

Imaging n Plain Radiographs u Upright PA on inspiration « u u Partially collapsed lung Tension Pneumothorax « « n Detect other pathologies: pneumonia, cardiac, etc. Trachea and mediastinum deviate contralaterally Ipsilateral depressed hemidiaphragm Chest CT Not routine u Only to assess the need for Dr Alpana K Somale, lecturer surgery (thoracotomy) u 32

Treatment n n n Small pneumothorax u Resolve over days to weeks u Supplemental oxygen and observation Tension pneumothorax u Immediate decompression via chest tube or needle thoracostomy Spontaneous pneumothorax u Asymptomatic – outpatient, f/u with serial CXR u Symptomatic – inpatient, chest tube u Recurrent pneumothorax – CT to evaluate need for thoracotomy Dr Alpana K Somale, lecturer 33

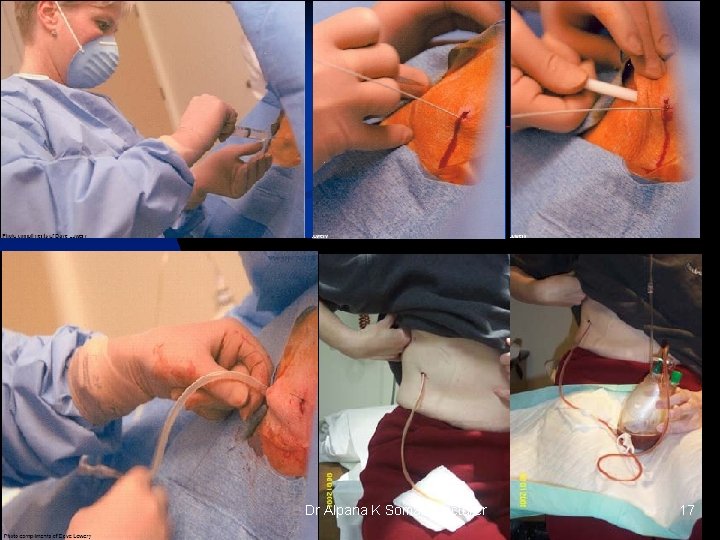
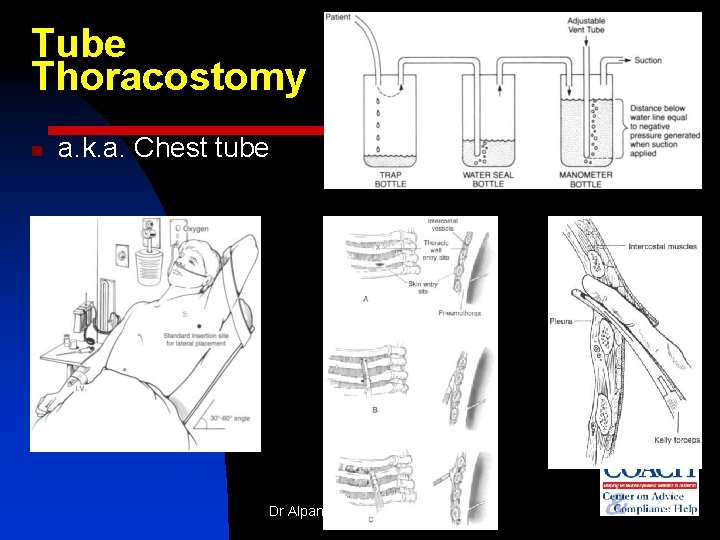
Tube Thoracostomy n a. k. a. Chest tube Dr Alpana K Somale, lecturer 34

Dr Alpana K Somale, lecturer 35

Dr Alpana K Somale, lecturer 36

Dr Alpana K Somale, lecturer 37