Plasma Cell Dyscrasias DR DEA THOMAS Objectives Plasma

Plasma Cell Dyscrasias DR DEA THOMAS

Objectives § Plasma cells § Immunoglobulins § Paraproteinaemia § Plasma Cell Dyscrasias § Monoclonal gammopathy of undetermined significance § Smouldering Multiple Myeloma § Others: Plasma cell leukaemia, solitary plasmacytoma, AL Amyloidosis, Waldenstrom’s Macroglobulinemia
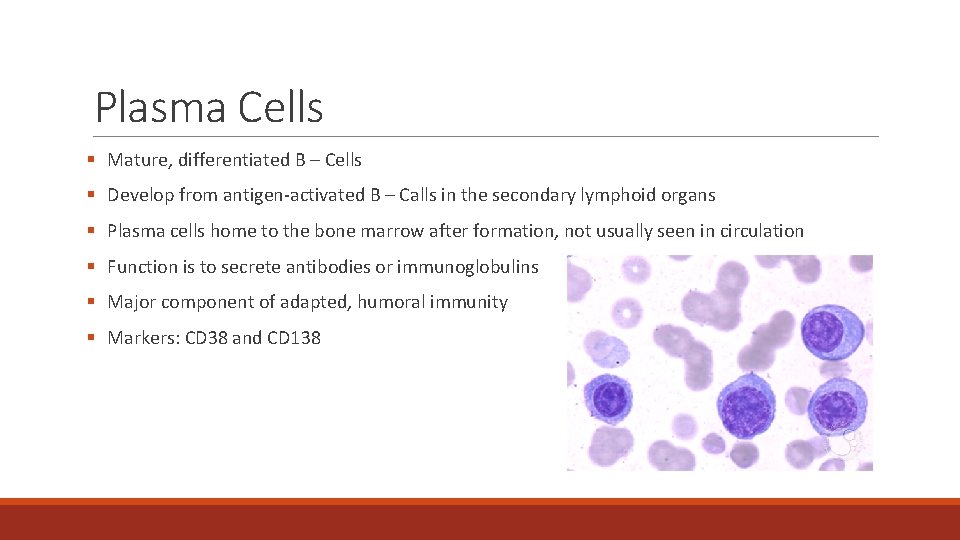
Plasma Cells § Mature, differentiated B – Cells § Develop from antigen-activated B – Calls in the secondary lymphoid organs § Plasma cells home to the bone marrow after formation, not usually seen in circulation § Function is to secrete antibodies or immunoglobulins § Major component of adapted, humoral immunity § Markers: CD 38 and CD 138
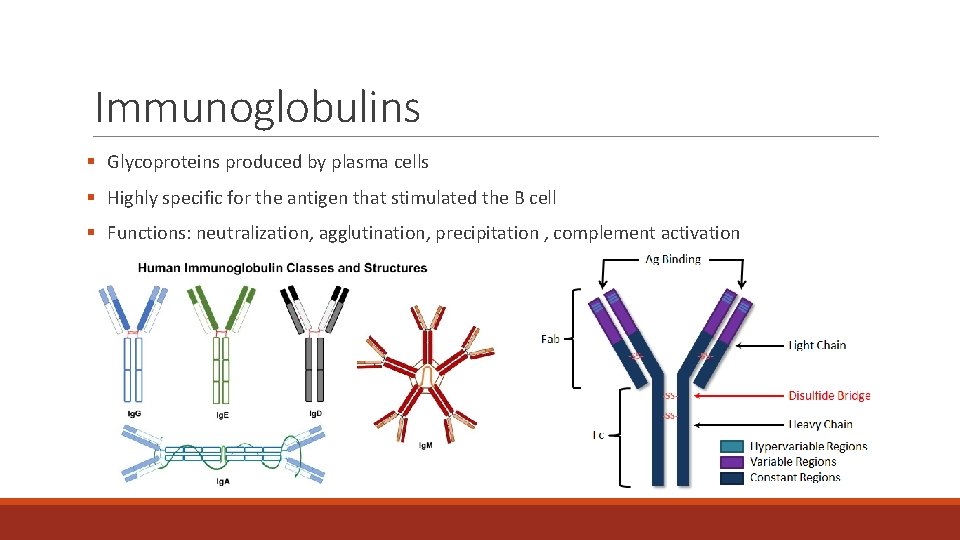
Immunoglobulins § Glycoproteins produced by plasma cells § Highly specific for the antigen that stimulated the B cell § Functions: neutralization, agglutination, precipitation , complement activation

Immunoglobulins Ig. M: Pentamer; first Ig produced against antigens, very potent and efficient Ig. G: Monomer; produced second but lasts longer in circulation Ig. E: Monomer; produced against parasites, affinity to mast cells, allergies Ig. D: Monomer; unknown function, possibly a BCR Ig. A: Dimer, primarily found in GI and bronchial secretions
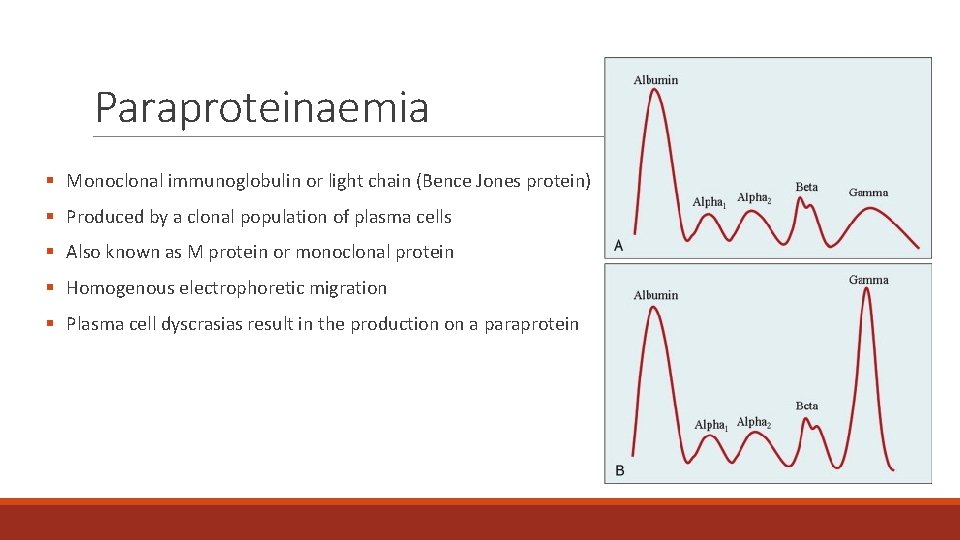
Paraproteinaemia § Monoclonal immunoglobulin or light chain (Bence Jones protein) § Produced by a clonal population of plasma cells § Also known as M protein or monoclonal protein § Homogenous electrophoretic migration § Plasma cell dyscrasias result in the production on a paraprotein
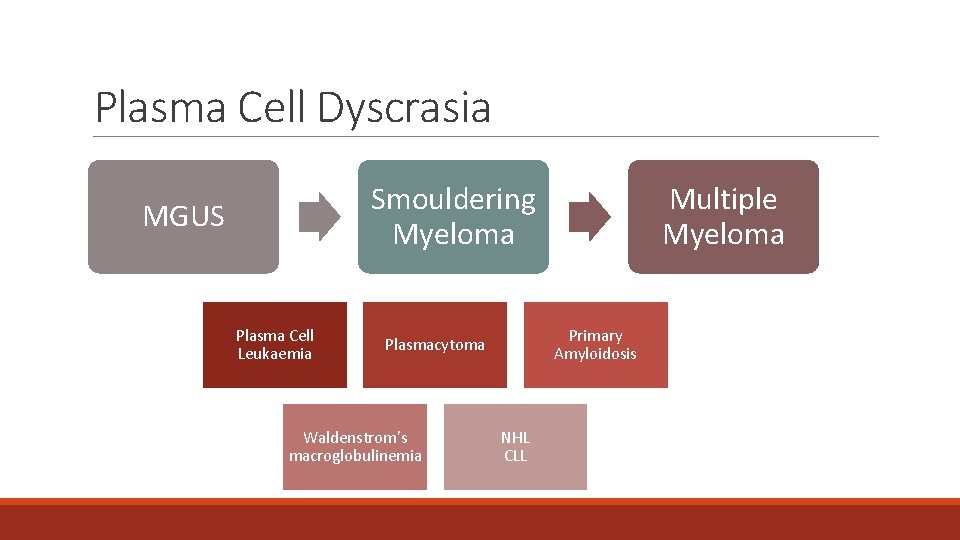
Plasma Cell Dyscrasia Smouldering Myeloma MGUS Plasma Cell Leukaemia Primary Amyloidosis Plasmacytoma Waldenstrom’s macroglobulinemia Multiple Myeloma NHL CLL

MGUS § Monoclonal gammopathy of undetermined significance § 3% in persons > 50 years DIAGNOSTIC FEATURES § Paraprotein in circulation but no organ damage Monoclonal protein spike < 3 g/ L § Risk of progression to myeloma of 1% per year Plasma cells < 10% in the bone marrow § Most myeloma cases arise from MGUS No signs and symptoms of organ damage § No screening currently for MGUS § MGUS patients are monitored for signs of MM development

Smouldering Myeloma § Asymptomatic clonal plasma cell disorder § Risk of progression to myeloma of 10% per year § Patients are further categorized into a high-risk category: § Serum proteins > 30 g/L § Ig. A SMM § Clonal BMPCs 50%-60% § Observation until development of symptomatic MM DIAGNOSTIC FEATURES Monoclonal protein spike > 3 g/ L Plasma cells: 10 – 60 % in the bone marrow No signs and symptoms of organ damage § High-Risk SMM patients can be offered clinical trials where earlier interventions for MM are being studied § If clonal BMPCs > 60%, patients are categorized and treated as MM even without organ damage
MULTIPLE MYELOMA
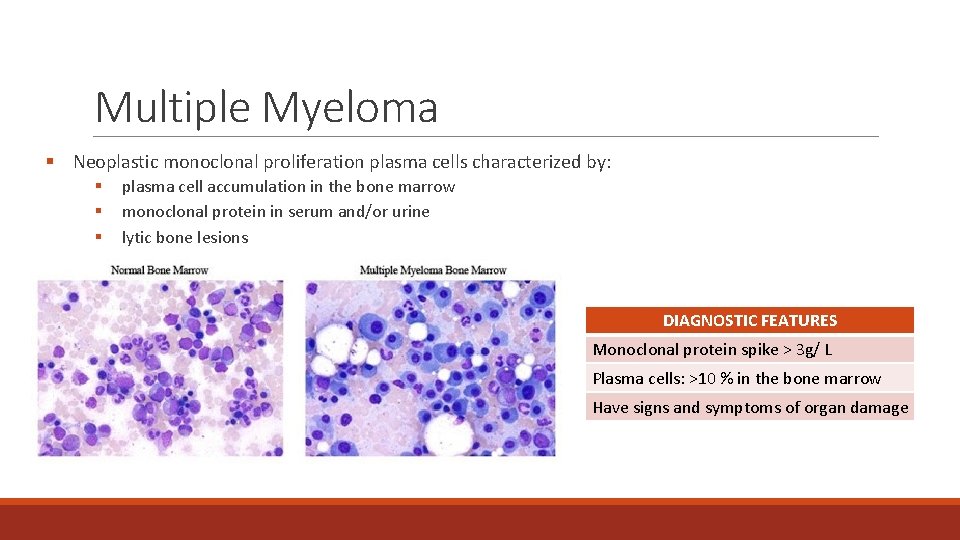
Multiple Myeloma § Neoplastic monoclonal proliferation plasma cells characterized by: § § § plasma cell accumulation in the bone marrow monoclonal protein in serum and/or urine lytic bone lesions DIAGNOSTIC FEATURES Monoclonal protein spike > 3 g/ L Plasma cells: >10 % in the bone marrow Have signs and symptoms of organ damage

Epidemiology § Approximately 230, 000 persons affected worldwide - International Myeloma Foundation § Peak incidence in the 7 th decade of life § M>F § Incidence twice as higher in people of African descents.

Aetiology § The cause of myeloma is not known § Almost all cases arise from pre-existing MGUS § Possible environmental exposure: farmers, wood workers, leather workers and those exposed to petroleum products have higher incidence § Chromosomal alterations have been found in patients with myeloma: § Hyperdiploidy § 13 q 14 deletions § translocations t( 1 l; 14)(q 13; q 32), t(4; 14) ( p 1 6; q 32), and t( l 4; 1 6) § 17 p 1 3 deletions.

CLINICAL FEATURES
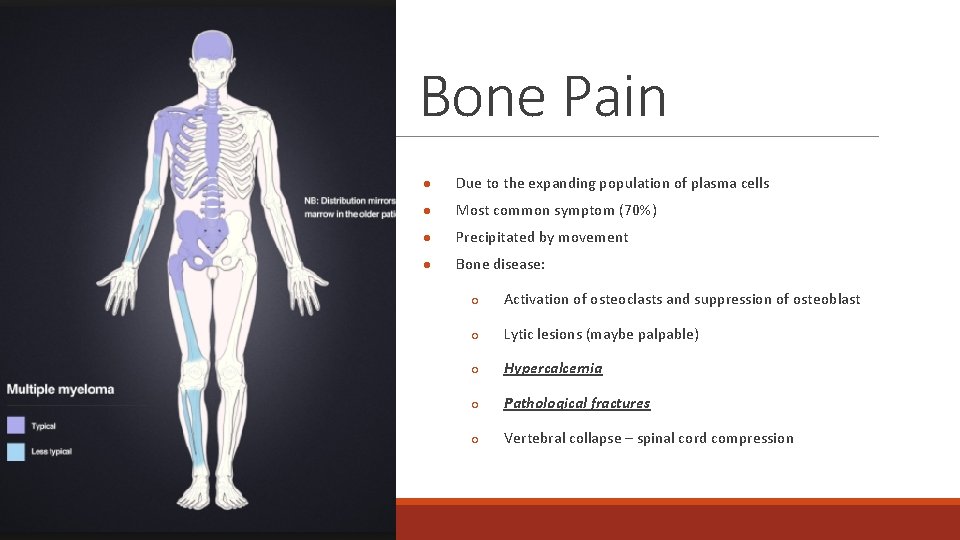
Bone Pain ● Due to the expanding population of plasma cells ● Most common symptom (70%) ● Precipitated by movement ● Bone disease: ○ Activation of osteoclasts and suppression of osteoblast ○ Lytic lesions (maybe palpable) ○ Hypercalcemia ○ Pathological fractures ○ Vertebral collapse – spinal cord compression

Immunoparesis ● Recurrent infections – pneumonias, pyelonephritis, UTI ● Deficient antibody production ● ● ○ Diffuse hypogammaglobinemia if M protein is excluded ○ Poor antibody response ○ Increased destruction of the immunoglobulins Abnormal cell-mediated immunity and neutropenia Abnormal complement function

Renal failure ● ● 25% of patients. 50% have some kind of renal damage. Causes ● ● ● ● Cast nephropathy Light chain toxic effects Hypercalcemia Glomerular deposition of amyloid Hyperuricemia Recurrent infections Proteinuria ● ● Bence - Jones proteinuria Non – selective proteinuria if glomerular damage

Hypercalcemia § § § Stones § Renal calculi Bones – bone pain Abdominal groans § Constipation § Pancreatitis § Psychiatric moans § Confusion § Mental disturbances § Depression § § Lethargy Polyuria Polydipsia Muscle Weakness

Normocytic Normochromic Anaemia ● ~80% of patients ● Lethargy, weakness, dyspnea, pallor, tachycardia ● Causes ● ● ● Replacement and extension of normal marrow by myeloma cells Inhibition of haematopoiesis by tumour factors Decreased erythropoietin production by the kidney

Other Features § Abnormal bleeding tendencies § Amyloidosis (5%) § § Features of macroglossia, carpal tunnel syndrome and diarrhoea Hyperviscosity syndrome (2%) § § Interference with platelet function and coagulation factors Thrombocytopenia occurs in advances disease Purpura, haemorrhages, visual failure, CNS symptoms, neuropathies, heart failure, DVT Folate and B 12 Deficiency

INVESTIGATIONS
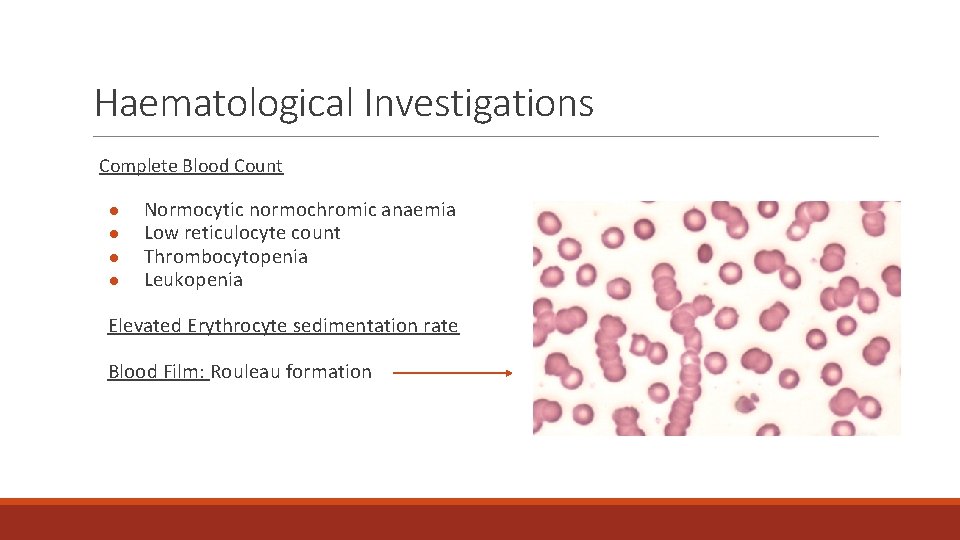
Haematological Investigations Complete Blood Count ● ● Normocytic normochromic anaemia Low reticulocyte count Thrombocytopenia Leukopenia Elevated Erythrocyte sedimentation rate Blood Film: Rouleau formation

Biochemical Investigations Urea and Electrolytes ● ● Hypercalcemia Pseudohyponatremia Elevated BUN and Creatinine Elevated uric acid Serum Proteins ● ● ● High Total proteins Low albumin High globulins Normal ALP (unless fractures) Prognostic Markers LDH ● ß 2 Microglobulin ● CRP ●

24 Hour Urine Collection ● Proteinuria ● Bence-Jones ● >1 g in 24 h is a major criteria ● Note: Dipstick is not sensitive for Bence-Jones proteins due to renal catabolism of the light chains ● Creatinine clearance ● Severity of renal impairment
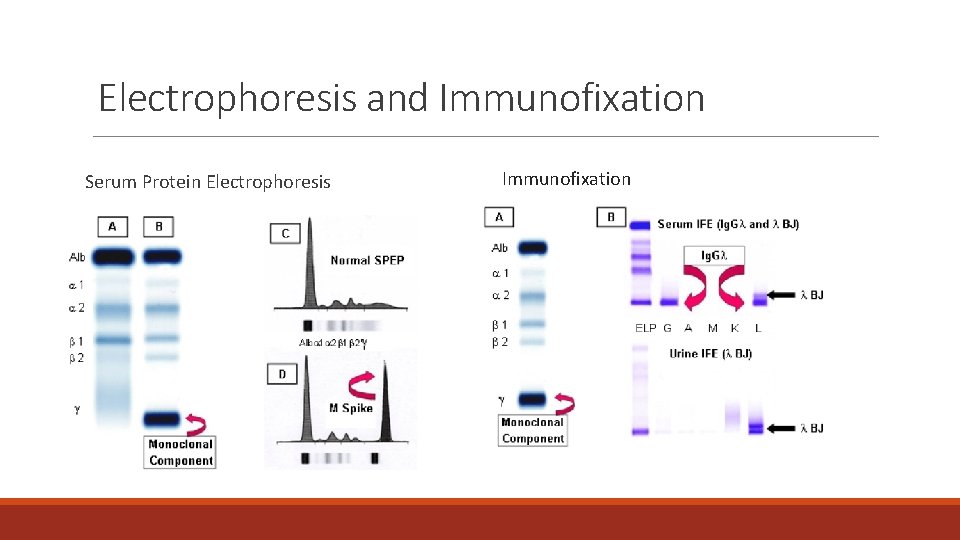
Electrophoresis and Immunofixation Serum Protein Electrophoresis Immunofixation
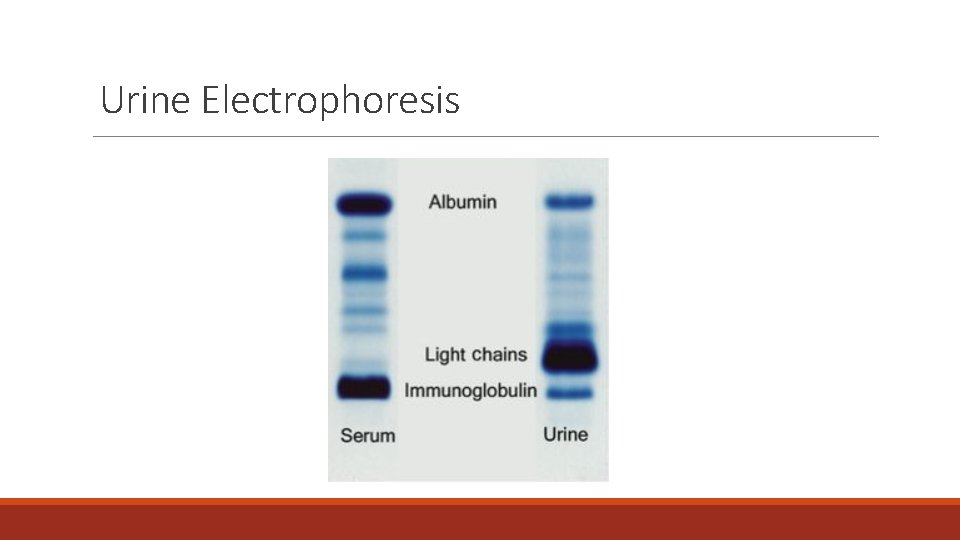
Urine Electrophoresis
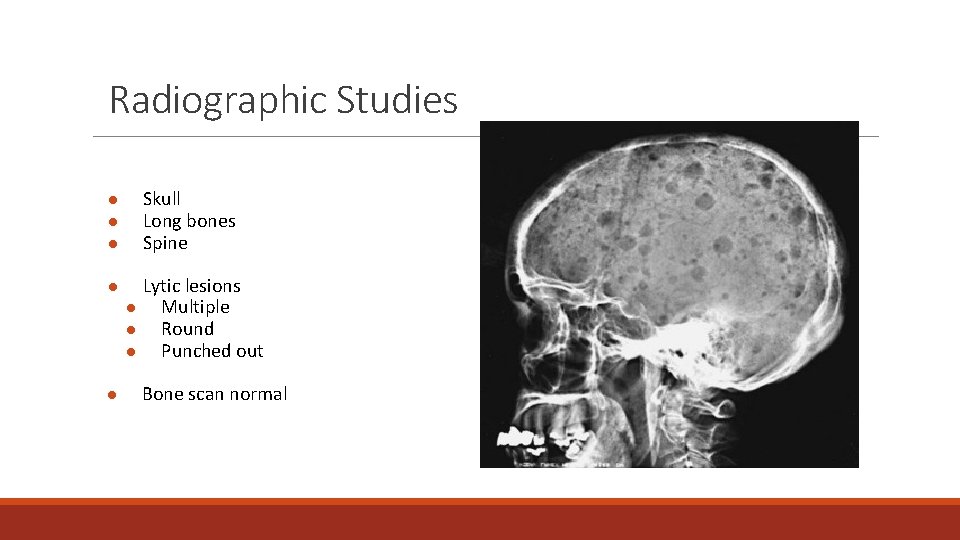
Radiographic Studies ● ● ● Skull Long bones Spine ● Lytic lesions ● Multiple ● Round ● Punched out ● Bone scan normal

Other Imaging studies ● Magnetic Resonance Imaging ● ● Thoracic and lumbar spine lesions Cord compressions Indicated when symptomatic Positron Emission Tomography
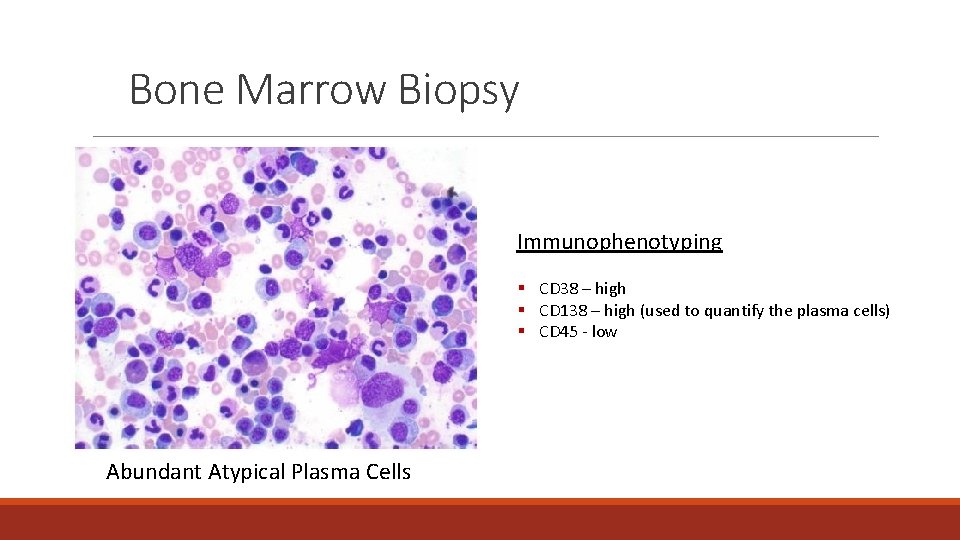
Bone Marrow Biopsy Immunophenotyping § CD 38 – high § CD 138 – high (used to quantify the plasma cells) § CD 45 - low Abundant Atypical Plasma Cells

Diagnostic Criteria International Myeloma Working Group: A or B + 1 or more myeloma defining event (C 1 or C 2) A : Clonal bone marrow plasma cells > or = 10% B: Biopsy proven bone or extramedullary plasmacytoma C 1 : Signs on end-organ damage C 2 : Biomarkers of malignancy Hypercalcaemia > 2. 75 or 0. 25 above upper limit of normal Clonal bone marrow plasma cells >/= 60% Renal Insufficiecy Cr. Cl < 40 m. L/min or Serum Creat > 177 >1 focal lesion on MRI Anaemia Hb < 10 or 2 g/d. L below lower limit Osteolytic bone lesion >/= 1 Serum Free Light Chain Ratio > 100
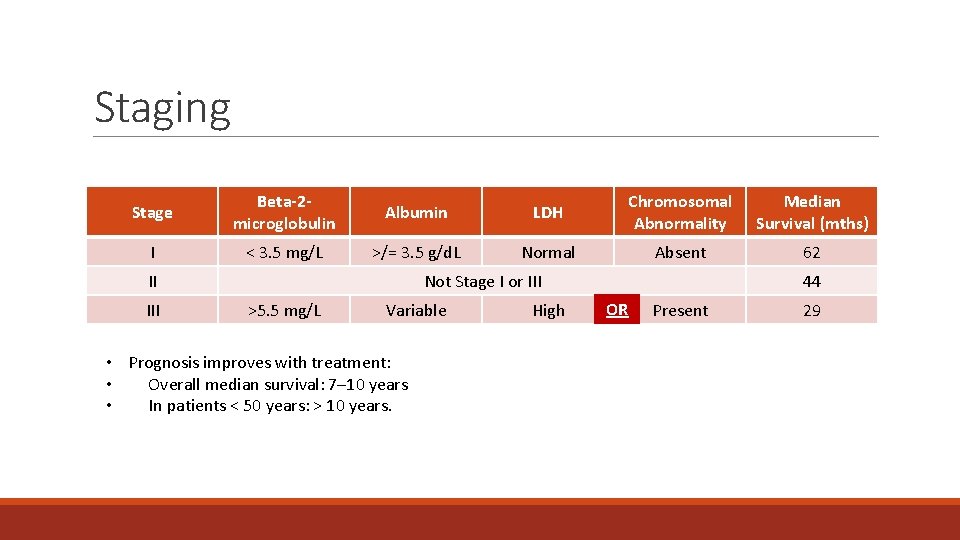
Staging Stage Beta-2 microglobulin Albumin LDH Chromosomal Abnormality Median Survival (mths) I < 3. 5 mg/L >/= 3. 5 g/d. L Normal Absent 62 II III Not Stage I or III >5. 5 mg/L Variable • Prognosis improves with treatment: • Overall median survival: 7– 10 years • In patients < 50 years: > 10 years. High 44 OR Present 29
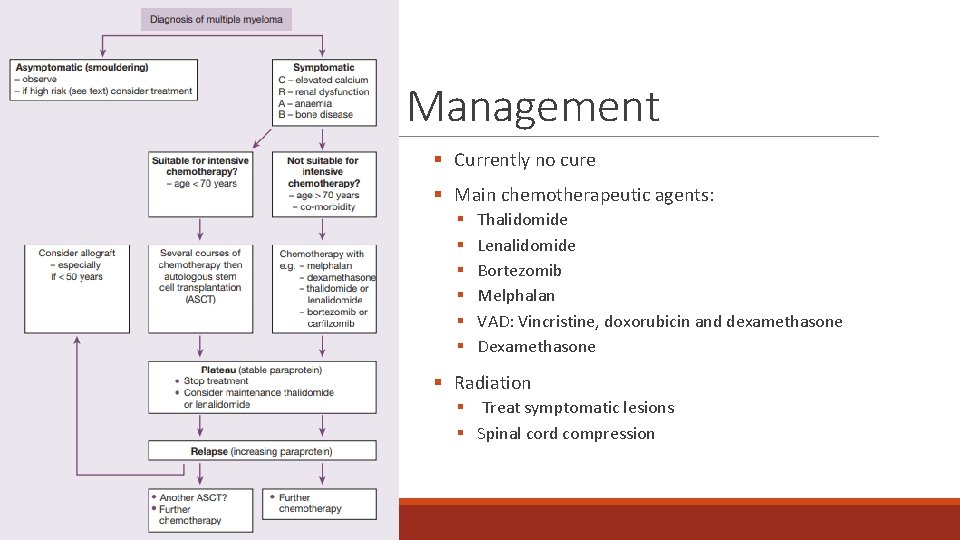
Management § Currently no cure § Main chemotherapeutic agents: § § § Thalidomide Lenalidomide Bortezomib Melphalan VAD: Vincristine, doxorubicin and dexamethasone Dexamethasone § Radiation § Treat symptomatic lesions § Spinal cord compression
![Management § Bisphonates [Ex. Zoledronate 4 mg once a month] § Decrease osteoclastic activity Management § Bisphonates [Ex. Zoledronate 4 mg once a month] § Decrease osteoclastic activity](http://slidetodoc.com/presentation_image_h2/24fdfc3960149d75dbdcc2a4adca5f64/image-33.jpg)
Management § Bisphonates [Ex. Zoledronate 4 mg once a month] § Decrease osteoclastic activity § Plasmapheresis to clear light chains in renal injury § Hydration § Monitoring for and early therapy of UTIs § Glucocorticoids in spinal cord compression § Erythropoietin and haematinics for anaemia

Plasma Cell Leukaemia § Rare aggressive form of leukaemia § Primary or Secondary § Secondary forms in patients with MM § 20% circulating plasma cells and a total count > 2 * 10^9 /L § Presents earlier than MM § Symptoms of leukaemia and MM § Worse prognosis – few months after diagnosis even with chemotherapy
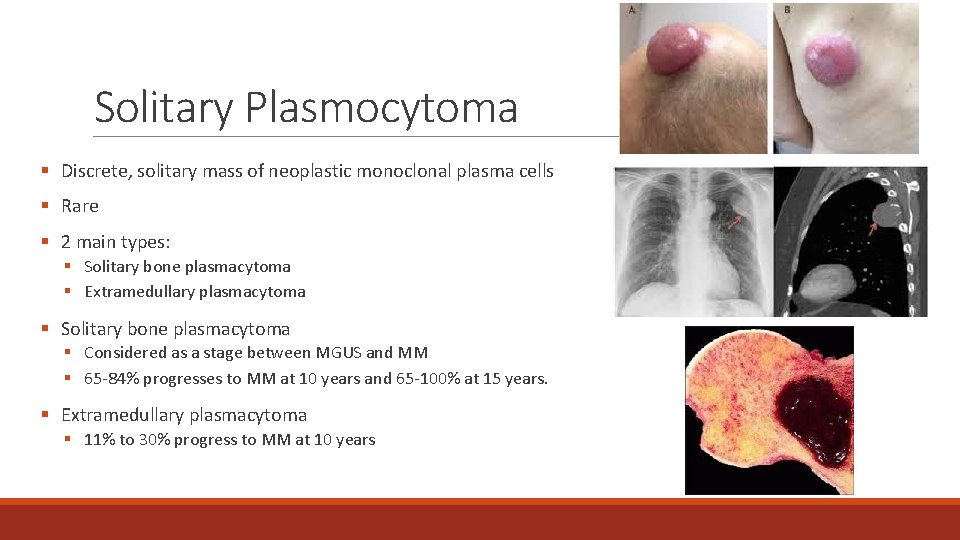
Solitary Plasmocytoma § Discrete, solitary mass of neoplastic monoclonal plasma cells § Rare § 2 main types: § Solitary bone plasmacytoma § Extramedullary plasmacytoma § Solitary bone plasmacytoma § Considered as a stage between MGUS and MM § 65 -84% progresses to MM at 10 years and 65 -100% at 15 years. § Extramedullary plasmacytoma § 11% to 30% progress to MM at 10 years
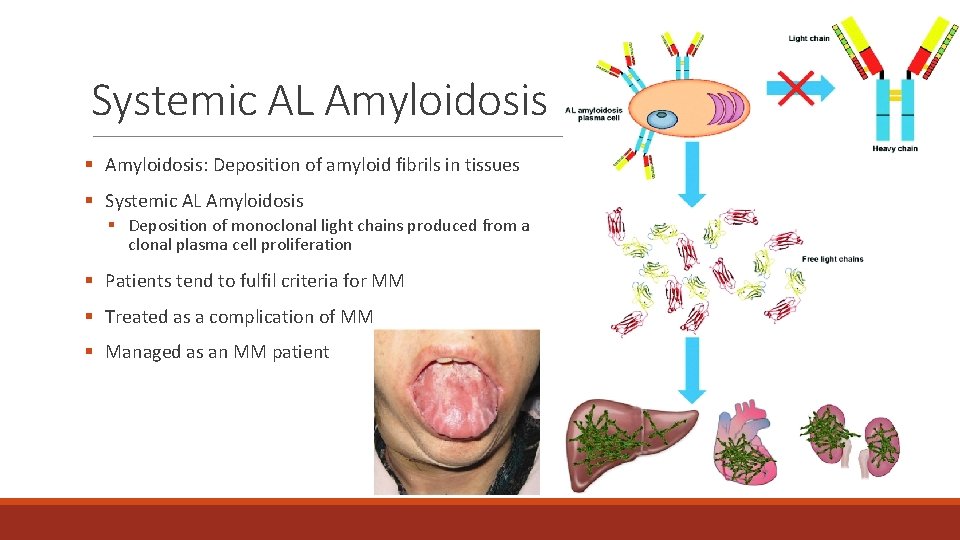
Systemic AL Amyloidosis § Amyloidosis: Deposition of amyloid fibrils in tissues § Systemic AL Amyloidosis § Deposition of monoclonal light chains produced from a clonal plasma cell proliferation § Patients tend to fulfil criteria for MM § Treated as a complication of MM § Managed as an MM patient
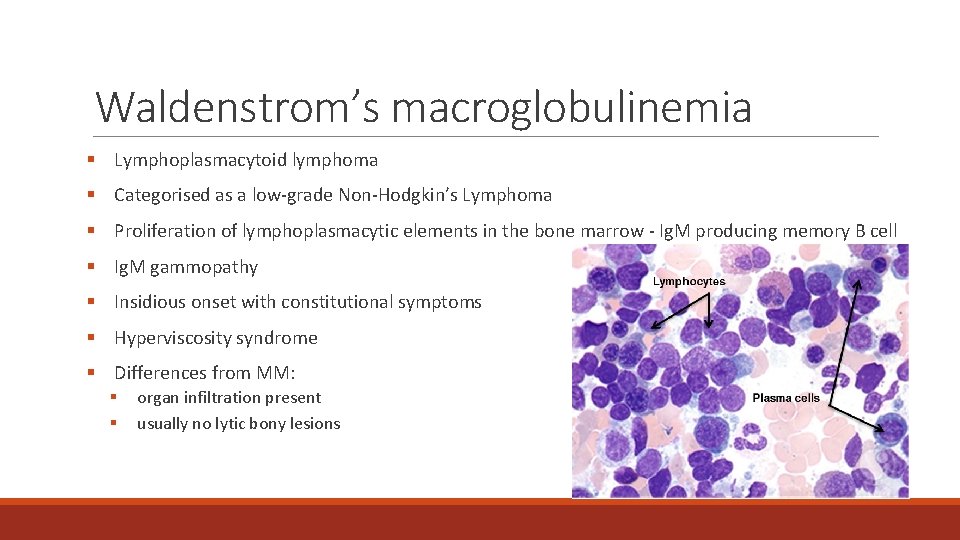
Waldenstrom’s macroglobulinemia § Lymphoplasmacytoid lymphoma § Categorised as a low-grade Non-Hodgkin’s Lymphoma § Proliferation of lymphoplasmacytic elements in the bone marrow - Ig. M producing memory B cell § Ig. M gammopathy § Insidious onset with constitutional symptoms § Hyperviscosity syndrome § Differences from MM: § § organ infiltration present usually no lytic bony lesions
![References Allen HC, Sharma P. Histology, Plasma Cells. [Updated 2020 Mar 27]. In: Stat. References Allen HC, Sharma P. Histology, Plasma Cells. [Updated 2020 Mar 27]. In: Stat.](http://slidetodoc.com/presentation_image_h2/24fdfc3960149d75dbdcc2a4adca5f64/image-38.jpg)
References Allen HC, Sharma P. Histology, Plasma Cells. [Updated 2020 Mar 27]. In: Stat. Pearls [Internet]. Treasure Island (FL): Stat. Pearls Publishing; 2020 Jan-. Available from: https: //www. ncbi. nlm. nih. gov/books/NBK 556082/ Justiz Vaillant AA, Jamal Z, Ramphul K. Immunoglobulin. [Updated 2020 Jul 25]. In: Stat. Pearls [Internet]. Treasure Island (FL): Stat. Pearls Publishing; 2020 Jan-. Available from: https: //www. ncbi. nlm. nih. gov/books/NBK 513460/ Soh, K. T. , Tario, J. D. , Jr, & Wallace, P. K. (2017). Diagnosis of Plasma Cell Dyscrasias and Monitoring of Minimal Residual Disease by Multiparametric Flow Cytometry. Clinics in laboratory medicine, 37(4), 821– 853. https: //doi. org/10. 1016/j. cll. 2017. 08. 001 Atkin, C. , Richter, A. , & Sapey, E. (2018). What is the significance of monoclonal gammopathy of undetermined significance? . Clinical medicine (London, England), 18(5), 391– 396. https: //doi. org/10. 7861/clinmedicine. 18 -5 -391 Rajkumar, S. V. , Landgren, O. , & Mateos, M. V. (2015). Smoldering multiple myeloma. Blood, 125(20), 3069– 3075. https: //doi. org/10. 1182/blood-2014 -09 -568899 Mazzucchelli, M. , Frustaci, A. M. , Deodato, M. , Cairoli, R. , & Tedeschi, A. (2018). Waldenstrom's Macroglobulinemia: An Update. Mediterranean journal of hematology and infectious diseases, 10(1), e 2018004. https: //doi. org/10. 4084/MJHID. 2018. 004
- Slides: 38