Planning and Implementing Cervical Cancer Programs Andreas Ullrich






















- Slides: 23

Planning and Implementing Cervical Cancer Programs Andreas Ullrich WHO Geneva l. WHO-IUMSP NCD PROGRAMME MANAGERS SEMINAR, 3 - 7 JUNE 2013

Overview l Principles of the WHO comprehensive approach l From new Evidence in Cervical cancer prevention to new Guidelines l From Guidelines to Implementation: country examples 2| PEPFAR meeting, Lusaka - Zambia | 26 -28 June 2010

The need for action: cancer screening mostly absent Slide 3 l. WHO NCD survey 2010

Comprehensive Approach Slide 4

Natural History of Cervical Cancer Continuum of Care PREVENTION Early detection Screening Slide 5 Diagnosis/ Treatment Palliative Care

The first-ever comprehensive guide from WHO on cervical cancer control - 2006 • Adopted and adapted in many countries, e. g. , China, Sri Lanka, Viet Nam, Cambodia, Thailand, Nigeria, Malawi, Zambia, Tanzania, Uganda, some Latin. American countries, and others Slide 6

The first-ever comprehensive guide from WHO on cervical cancer control - 2006 • Key messages: – Health education integral part of cervical cancer control – Cytology, but not <25 yrs or annually – VIA /"See and treat", in pilot settings only – HPV testing, in pilot settings only. Slide 7

Purpose of the update o Health education to be expanded o HPV vaccines to be included o New data on use of screening tests VIA /HPV o New data on "See and treat" o New data for algorithms (sequential testing) o Program planning chapter Slide 8

NEED FOR UP DATE Conventional pap smear Visual inspection with acetic acid (VIA) Hybrid Capture® 2 DNA test Care. HPV rapid DNA test

Choice of a test need to be based on: • Effectiveness of the test (sensitivity/specificity) in the target group. • Capacity to reach (coverage) a significant proportion (100%) of target group – Local infrastructure where the test will be used – Balance between performance of the test vs. coverage • Capacity of the health system to ensure treatment • Cost • Should take into consideration the new environment of HPV vaccines introduction

From interventions to policies Cervical cancer prevention = mandatory part of national health planning and monitoring UN General Assembly on NCD 2011 World Health Assembly 2013

Essentials for program planning • • • National policy Resources allocated, insurance coverage Public education Health education for target groups Screening = organized Screening linked with treatment, referral system • Heath information system (cancer registries)

Screening program options • Age: WHO recommends 30+ unless HIV+ • Frequency: depends on test and resources, achieve high coverage • Which test: depends on resources and infrastructure • Care provider: doctor, nurse, midwife, technician • Treatment: cryotherapy suitable for most lesions and easy for non-physician to learn; need LEEP for large or advanced lesions • Community outreach: interpersonal through community health workers or women’s groups; local radio; posters

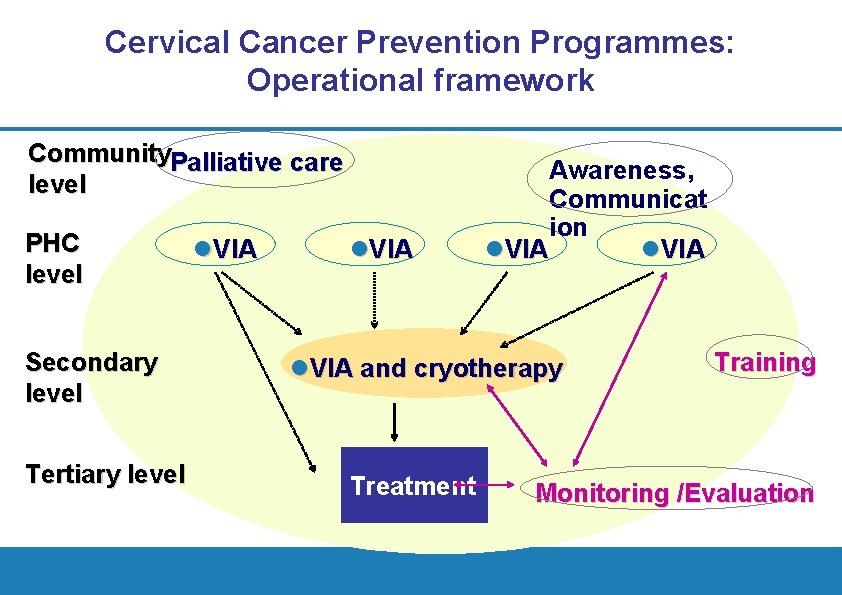
Cervical Cancer Prevention Programmes: Operational framework Community. Palliative care level PHC level Secondary level Tertiary level l. VIA Awareness, Communicat ion l. VIA and cryotherapy Treatment Training Monitoring /Evaluation

Introduction of HPV vaccines l Two vaccines available, licensed and WHOpre qualified: Cervarix (16/18) and Gardasil (16/18 + 6/11) l Up to 30% of Cervical cancer are cause by other types than 16/18 l Both vaccines require 3 doses over 6 months Slide 15

Introduction HPV vaccines (continued) l Both vaccines are preventive only , target 913 year old girls l Post vaccination follow up exists only for 9 years l HPV in HIV positives is safe Slide 16

HPV Introduction challenges l Priority setting fro HPV l Cost of vaccine/delivery l Target population/delivery system l Coordination with introduction other vaccines and inclusion in national multiyear plan (c. MYP) l HPV is part of an integrated plan fro cx prevention Slide 17

Case report Ghana l No systematic screening, opportunistic cytology (district), VIA pilot project, l HPV introduction: Demonstration project Gardasil, GAVI demonstration project l Challenges: limited human resources, low awareness, socio-cultural beliefs Slide 18

Case report Senegal l No systematic screening, 7 pilot VIA projects, one HPV pilot, l HPV introduction: GAVI demonstration project l Challenges: late presentation of cx, poor coordination between various donor activities, absence of data; Slide 19

Case report Nigeria l National NCCP, National CX policy, Capacity building VIA, 6 screening delivery centers, Advocacy awareness campaigns l HPV introduction program, l Challenges: reach out to rural communities, lack of cancer registries, scaling up screening to national coverage (PHC) Slide 20

Lessons learnt program planning l Cross Ministerial coordination l Cross program coordination > integration of services l Participation of key local stakeholders Slide 21

Resources l WHO guidelines and costing tools l WHO Regional offices / country offices focal points l Regional capacity building initiatives (e. g. EUROMED) l WHO partners UNFPA, PATH, GAVI, Pink-Red Ribbon, JHPIEGO, CDC…. Slide 22

Conclusion l Cervical cancer is part of the NCD agenda l New options for cervical cancer prevention suitable for a variety of settings l Cross over of existing programs (reproductive health, immunization, adolescent health, cancer control )is essential (from vertical to horizontal cross fertilization) Slide 23