Planning A Model of Whole Person Care John

























- Slides: 27

Planning A Model of Whole Person Care John Kern, MD

Plan for Today: Drilling Down into the Weeds on Planning Your Model • Team composition • Team roles and responsibilities • Work flows • Sustainability 2

Is Your Organization Ready? • Milestones Checklist Approach to Evaluate Organizational Readiness • Team Roles and Responsibilities 3

Checkpoint Whole Person Care Strategy How many of you are planning to: — Build primary care capacity for your clients independently? — Build capacity through a partnership? • Through multiple partnerships? — Undecided? 4

Exercise #1: Milestones or Readiness Checklist 15 Minutes for Team Huddle: — Review each Milestone — Assess your Progress to Date — Assign Note Taker to Record Next Steps, Challenges and Opportunities 3 -5 Minutes for Team Reports: — Team Score — Key Challenges — Opportunities 5

Team Self Assessment! Not yet started = 0 points Work in progress: — 1 points for: “we started talking about it. . ” — 3 points for: “We’re working on it. . ” Completed: — 5 points for a work plan articulated and accountabilities in place 6

Team Reports: • • 7 Team score (0 – 50 points) Top 1 -3 weak spots or challenges Top 1 -3 opportunities Anything else important to know?

One Step At a Time “My New Year’s Resolution is to lose thirty-eight thousand pounds. ” 8

Any Questions or Lessons from Exercise? 9

Thank You! Early Lunch Break! 10

Planning Sustainable Team Roles and Task Assignments 11

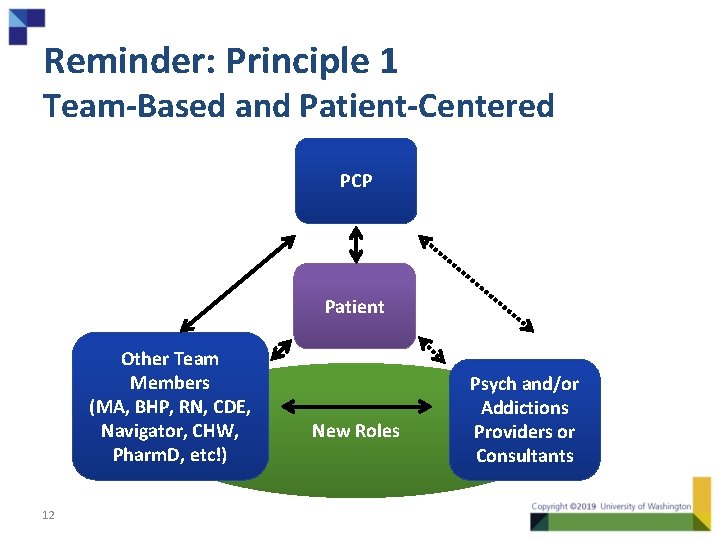
Reminder: Principle 1 Team-Based and Patient-Centered PCP Patient Other Team Members (MA, BHP, RN, CDE, Navigator, CHW, Pharm. D, etc!) 12 New Roles Psych and/or Addictions Providers or Consultants

Deep Dive into Individual Tasks and Assigning Team Roles Two Tools for Planning and Team Building: • Tasks Worksheet • Role Assignment Worksheet — Example based on existing BHT partnership — Available as spreadsheet for you to adapt if useful for planning in your organization 13

Checkpoint • Have any of you developed similar tools that have worked for you? • Would you be willing to share? 14

Exercise #2: Using One or Both of These Tools 15 Minutes for Team Huddle — Assign Tasks and Roles to Your Agency, Partner and/or your Team Members — Assign Note Taker to Capture Key Issues, Questions, Next Steps, Etc. 3 -5 Minutes for Team Reports — Describe your Anticipated Team Composition — Anticipated Challenges — Opportunities 15

Any Questions or Lessons from Exercise? 16

Building Team Workflows 17

AIMS Resources in Developing Workflows • AIMS PHQ Screening Toolkit – Available on BHT training website • Confluence Health HTN Workflow Example • Workflow Planning Tab on Roles Worksheet Initiate And Provide Treatment Collaborative Care Tasks Preform behavioral health assessment Develop & update behavioral helath treatment plan Patient edabout symptoms & treatment options Prescribe psychotropic medications Patient ed about medications & side effects Brief counseling, activity scheduling, behavioral activation 18 Who (Name and Discipline) How (Process & Communication Method) When (Patient flow & time constraints) Where (Clinic? Partner Agency? )

Very Brief Walk Through AIMS PHQ Screening Toolkit Includes: • Training Guide / FAQ for MAs, front and back office • Strategies for Training, Testing and Making Improvements to Workflows — Workflow Graphics — Training and Orientation — PDSA Cycles 19

Walk Through Confluence Health HTN Workflow • Many steps within some of the steps outlined by Confluence Health • Not just about HTN (i. e. , achieving good blood pressure control) but establishing care with a PCP and care coordination with PCP • Sub-Process to track medical outcomes and take action when outcomes are sub-optimal 20

Checkpoint • Have any of you developed similar workflows? • How did you go about that? • Any lessons learned? 21

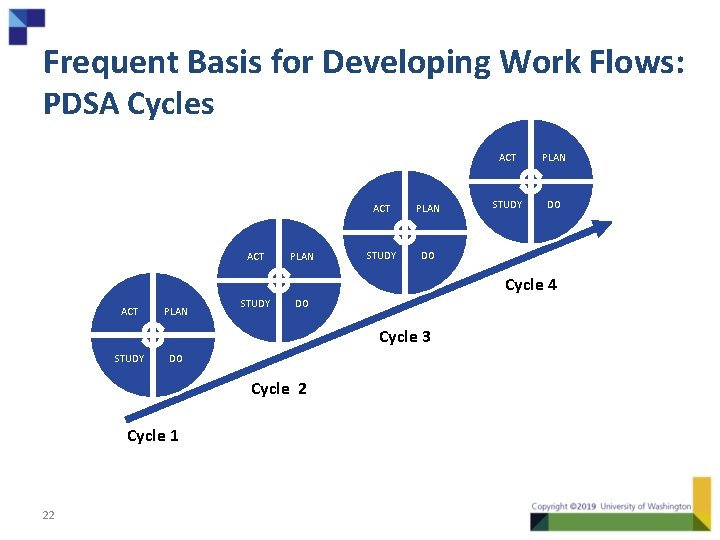
Frequent Basis for Developing Work Flows: PDSA Cycles ACT PLAN STUDY DO Cycle 4 ACT PLAN STUDY DO Cycle 3 STUDY DO Cycle 2 Cycle 1 22


Plan, Do, Study, Act Cycle • Idea(s) being tested – Can we gather info at front desk to understand our clients’ access and experience with primary care? • What are we trying to accomplish? – Get more clients well connected to PCP to improve their medical outcomes • How will we know that a change is an improvement? – Compare our baseline (X% of clients now established in primary care) to number of patients established through PDSA cycle – Was process efficient for front desk staff? • What changes can we make that may result in improvement? – Can front desk staff collect information about our clients’ PCP or most recent PCP visit in the waiting room? – If no PCP connection, can front desk staff loop in a CHW or navigator directly before appointment? 24

Fundamental Principles for Improvement Go Beyond PDSA • Why do you need to improve? – Mortality gap of our patients • Establish feedback mechanism to tell you if there is an improvement (PDSA cycles) – “Let’s follow our draft protocol / workflow for next 20 patients. . We’ll debrief and look at how efficiently that worked. ” • Test effectiveness of a change at a small scale before you implement widely – Usually multiple PDSA cycles before going system wide • Understand support what is needed to standardize a change, making it both reliable and system wide – Staff orientation, training, documentation & communication 25

Checkpoint • Final questions, ideas or resources to share around work flow strategies? • Next steps for your organization? 26

Wrap Up Thank You! Ashields@uw. edu Jkern 2@uw. edu 27