Plan Do Study Act QI SESSION 3 Plan










- Slides: 16

Plan, Do, Study, Act QI SESSION 3

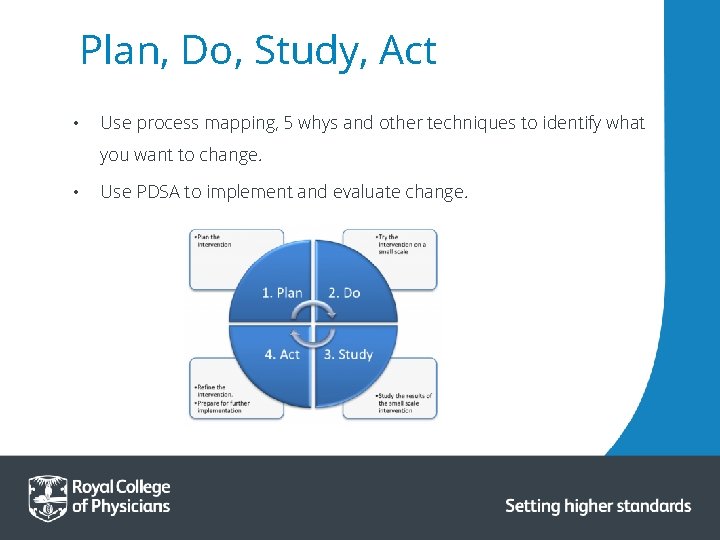
Plan, Do, Study, Act • Use process mapping, 5 whys and other techniques to identify what you want to change. • Use PDSA to implement and evaluate change.

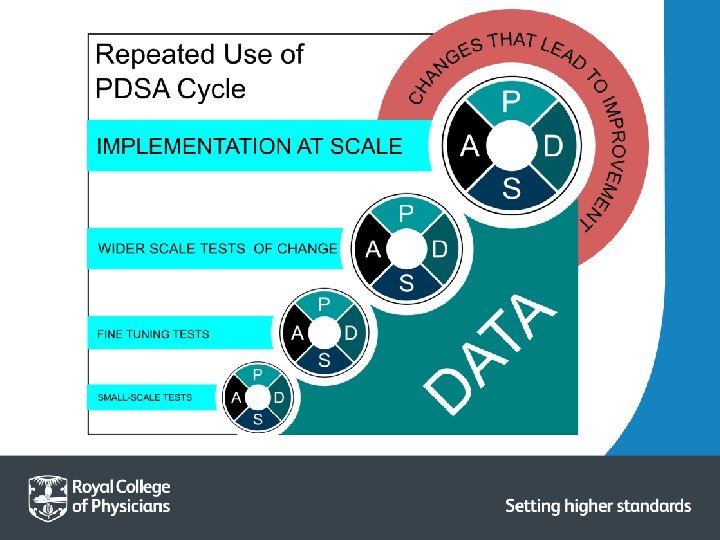
PDSA Cycle Adapt? Adopt? Abandon? Determine what modifications should be made. Prepare a plan for the next test. Set aside time to analyse the data and study the results. Compare the data to your predictions. Summarize and reflect on what was learned. State the objective of the test. Make predictions about what will happen and why. Develop a plan to test the change. (Who? What? When? Where? What data? ). Try out the test on a small scale. Document problems and unexpected observations. Begin analysis of the data.


“In God we trust…all others bring data…. ” W. E. Demming

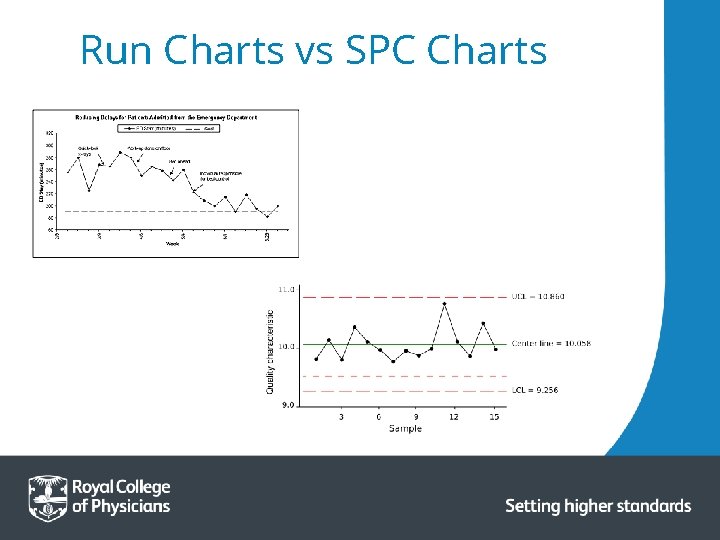
Measurement for Improvement • “All improvement requires change, but not all change is an improvement” • Make your measurement simple allowing rapid repeated cycles. • Don’t collect unnecessary data. • Consider a balancing measure…what could go wrong? • Run charts vs SPC charts…

Run Charts vs SPC Charts

PDSA Cycle Example • We have a low rate of chemotherapy treatment in our SCLC patients. • We have noticed that these patients sometimes deteriorate rapidly following referral/diagnosis. • There is often a delay between diagnosis and assessment for chemotherapy and then to the delivery of chemotherapy. • Can we speed up the patient pathway for these patients to have the best chance of being able to deliver chemotherapy? • Big Aim: to improve chemotherapy usage in SCLC patients. • Small Aim: to reduce the time between diagnosis and chemotherapy.

PDSA Cycle Example PLAN: • We will ask the oncologists to commit to a maximum 7 days between decision to treat • and start of treatment. We will assess our baseline performance by measuring the time taken by consecutive • patients in the pathway through November/December 2015. • • Time from referral to diagnosis (histology report) • Time from referral to oncology OPA • Oncology OPA to receipt of chemotherapy We will implement the new policy from 1 st Jan 2016, and continue to measure through Jan-Feb. • We predict that the new system will reduce the time to chemo by an average of 5 days. • We anticipate this will lead to more chemotherapy and better survival but it will not be a measurement of this PDSA cycle.

PDSA Cycle Example • DO: • Initials baseline measurement completed. • There was some concerns about workload but agreement was reached with the oncologists to implement the new policy. • Further measurements have been taken to demonstrate the changes.

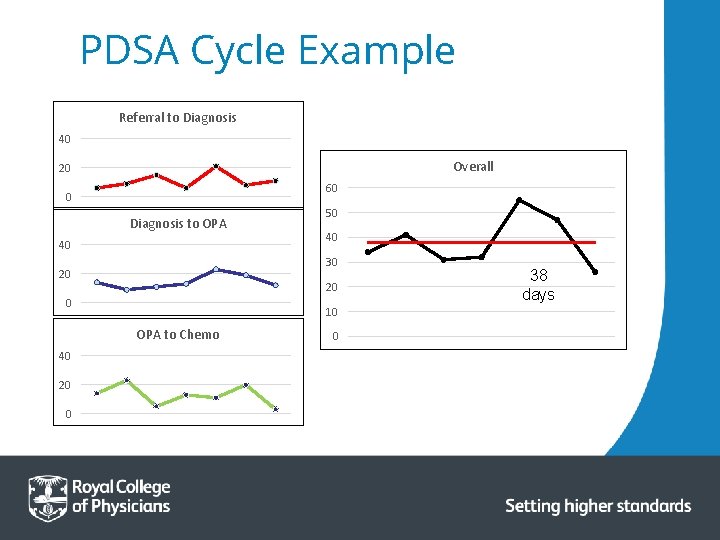
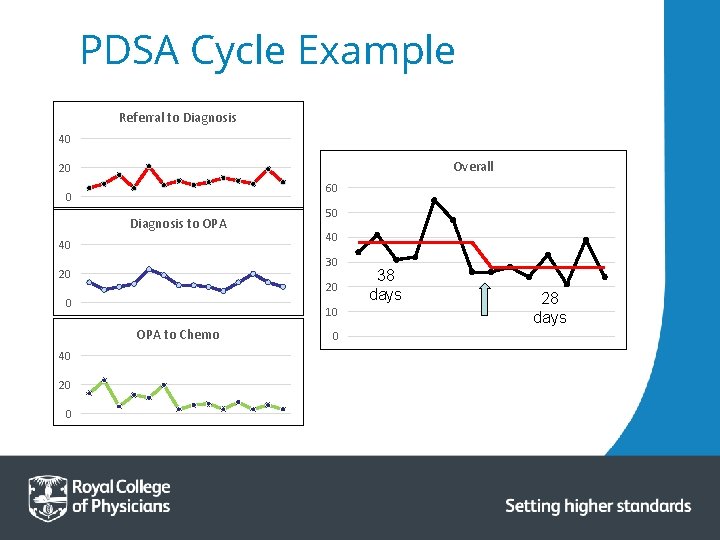
PDSA Cycle Example Referral to Diagnosis 40 Overall 20 60 0 Diagnosis to OPA 40 20 0 10 OPA to Chemo 20 0 40 30 20 40 50 0 38 days

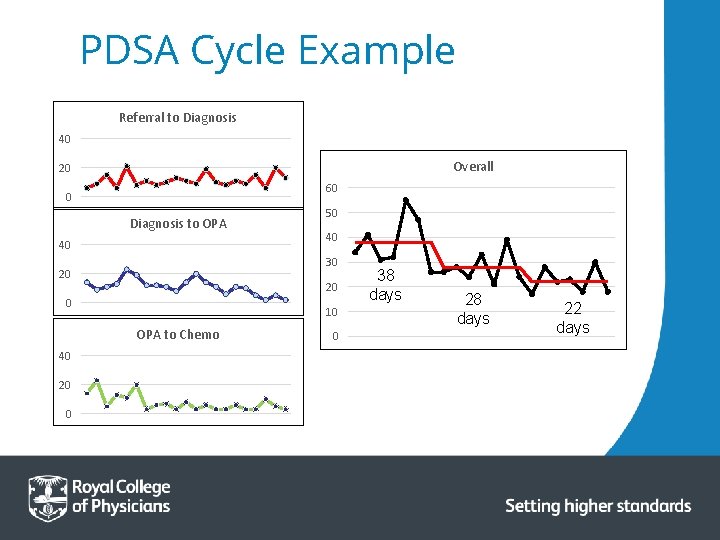
PDSA Cycle Example Referral to Diagnosis 40 Overall 20 60 0 Diagnosis to OPA 40 20 0 10 OPA to Chemo 20 0 40 30 20 40 50 0 38 days 28 days

PDSA Cycle Example • STUDY: • There has been an improvement in the length of the pathway of approx. 10 days. • The oncologists have realised that in some cases they can see the patients in the clinic on Tuesday, and start the chemo on Friday – giving a wait of only 3 days. They have been excited by this improvement and are keen to reduce the time to the OPA. • One of the patients commented that the process was very quick and she barely had time to think - we need to be careful that patients do not feel rushed into treatment.

PDSA Cycle Example • ACT: • We will try another PDSA cycle where we ask the pathologists to alert the LCNS to a probable SCLC case at the earliest opportunity. • This may bring the date of diagnosis forward, but will allow quicker booking of OPAs. • We will carry out a targeted patient experience survey to check that our patients are happy with a faster pathway. • We will audit the proportion of patients receiving chemotherapy in 6 months time to evaluate whether this has improved.

PDSA Cycle Example Referral to Diagnosis 40 Overall 20 60 0 Diagnosis to OPA 40 20 0 10 OPA to Chemo 20 0 40 30 20 40 50 0 38 days 22 days

QI Session 3: PDSA • Get into groups of 2 or 3 • Use a topic that you explored in the “ 5 Whys”, or consider: • • Streamlining a pathway • Better access to LCNS for in-patients • Increased radical treatment in older patients Use the worksheet provided to develop complete an initial PDSA cycle. • Your facilitator will help to ensure your aims are SMART. • Your facilitator will give you some dummy results that you can use to develop your STUDY and ACT sections.