Placental Abruption Liu Wei Department of Ob Gy

Placental Abruption Liu Wei Department of Ob & Gy Ren Ji hospital

General Consideration • • • Definition The separation of the placenta from its site of implantation after 20 weeks of gestation or during the course of delivery. Frequency 0. 51%-2. 33% (our country) 1% (other countries) Incidence of fetal death 200‰-350‰

Etiology • • 1. 2. 3. 4. 5. Uncertain (primary cause) Risk factors Increased age and parity Vascular diseases: preeclampsia, chronic hypertension, renal disease. Mechanical factors: trauma, intercourse, polyhydramnios, Supine hypotensive syndrome Smoking, cocaine use, uterine myoma

Pathology • • • Main change hemorrhage into the decidua basalis → decidua splits → decidural hematoma → separation, compression, destruction of the placenta adjacent to it Types revealed abruption, concealed abruption, mixed type Uteroplacental apoplexy 子宫胎盘卒中
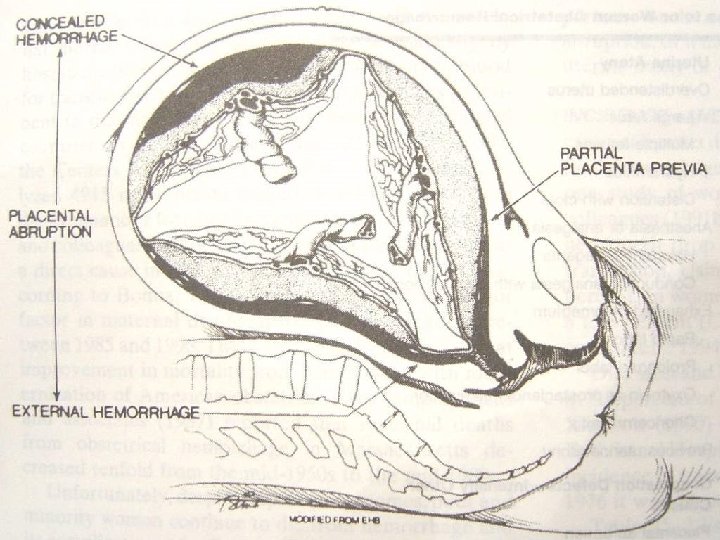
Pathology
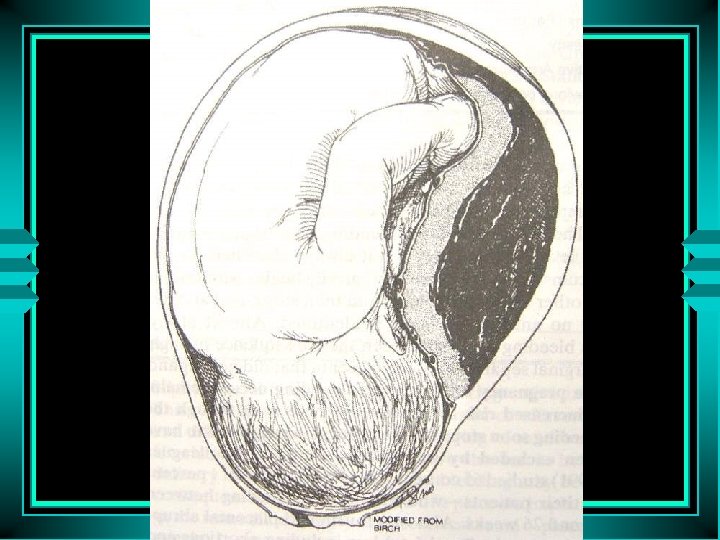
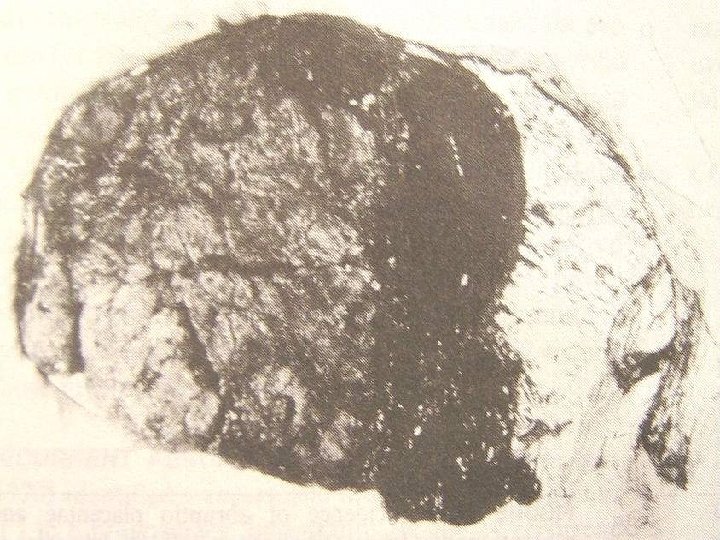

Manifestation • • • Vaginal bleeding companied with abdominal pain Mild type abruption≤ 1/3, apparent vaginal bleeding Severe type abruption > 1/3, large retroplacental hematoma, vaginal bleeding companied by persistent abdominal pain, tenderness on the uterus, change of fetal heart rate. shock and renal failure.

Adjunctive Examination • 1. 2. 3. • 1. 2. Ultrasonography Position of placenta, severity of abruption, survival of fetus Signs: retroplacental hematoma Negative findings do not exclude placental abruption Laboratory examination consumptive coagulopathy: Rt, DIC Function of liver and kidney.

Diagnosis • 1. 2. 3. 4. 5. 6. 7. sign and symptom Vaginal bleeding Uterine tenderness or back pain Fetal distress High frequency contractions Hypertonus Idiopathic preterm labor Dead fetus

Diagnosis • • 1. 2. Ultrasonography Differential diagnosis Placenta previa Painless bleeding Pre-rupture of uterus dystocia

Complication • • DIC Hypovolemic shock Amnionic fluid embolism Acute renal failure

Treatment • • Treatment will vary depending upon gestational age and the status of mother and fetus Treatment of hypovolemic shock: intensive transfusion with blood Assessment of fetus Termination of pregnancy: CS or Vaginal delivery

Treatment • 1. 2. 3. • Treatment of consumptive coagulopathy Supplement of coagulation factors: fresh blood, frozen blood plasma, fibrinogen, blood platelet. Heparin: high coagulation Anti-fibrinolysis Prevention of renal failure

END
- Slides: 15