Placenta Previa Placenta previa is used to describe

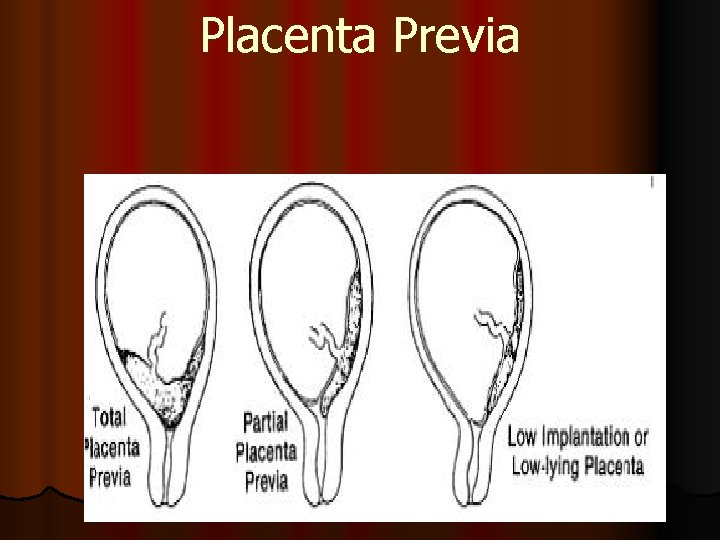
Placenta Previa Placenta previa is used to describe a placenta that is implanted over or very near the internal cervical os. Previa – latin word =denotes position of placenta in relation to the presenting part. There are several possibilities: Total placenta previa—the internal os is covered completely by placenta. Partial placenta previa—the internal os is partially covered by placenta. Marginal placenta previa—the edge of the placenta is at the margin of the internal os Low-lying placenta—the placenta is implanted in the lower uterine segment such that the placental edge does not reach the internal os, but is in close proximity to it. Vasa previa—the fetal vessels course through membranes and present at the cervical os.
Placenta Previa
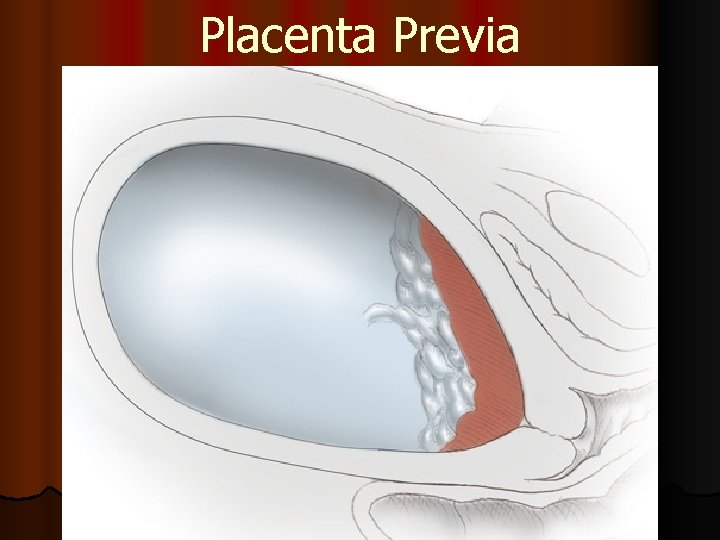
Placenta Previa

Placenta Previa The relationships and definitions used for classification in some cases of placenta previa depend on cervical dilatation at the time of assessment. A low-lying placenta at 2 -cm dilatation may become a partial placenta previa at 8 -cm dilatation because the dilating cervix has uncovered placenta. Conversely, a placenta previa that appears to be total before cervical dilatation may become partial at 4 -cm dilatation because the cervix dilates beyond the edge of the placenta. Digital palpation in an attempt to ascertain these changing relations between the placental edge and internal os as the cervix dilates usually causes severe hemorrhage, so please do not try.

Placenta Previa With both total and partial placenta previa, a certain degree of spontaneous placental separation is an inevitable consequence of lower uterine segment formation and cervical dilatation. Such separation is usually associated with hemorrhage. And although technically this constitutes a placental abruption, it usually is not termed such.

Degrees Degree I Lateral placenta previa – only the lower margin of placenta covers the upper part of the lower uterine segment but does not reach internal os. l Degree II Marginal placenta previa – the edge of the placenta reaches the margin of the internal os , but placenta does not cover it. l Degree III Incomplete or partial placenta previa – the placenta covers the internal os when it is closed , but partially covers it when fully dilated. l Degree IV Central or total placenta previa - the placenta completely covers the internal os even after it is fully dilated. l

l l l l For practical purpose these degrees can be graded as Incomplete - MINOR--- mild degree - degree I and degree II anterior Complaete – MAJOR --- severe degree – degree II posterior, degree III, degree IV. Posterior placenta previa is more commmon. Foetal loss rises with higher degrees of placenta previa. Posterior placenta previa degree II is more dangerous. (It interferes with the engagement of the fetal presenting part more than that of anterior one. Control of hemorrhage by the pressure of the presenting part is less likely in these csaes. Birth asphyxia is more common. Cord prolapse and cord compression is more. )

Incidence Placenta Previa placenta previa complicated almost 1 in 300 deliveries Associated predisposing Factors 1. Advancing maternal age increases the risk of placenta previa 1 in 1500 for women 19 years or younger and is 1 in 100 for women older than 35 years had a 1. 1 -percent risk for previa compared with that of 0. 5 percent for women less than 35 2. Multifetal pregnancy 40 percent higher in multifetal gestations compared with singletons 3. prior cesarean delivery increases the risk for placenta previa 1. 3 percent for those with one prior cesarean delivery and 3. 4 percent in women who had six or more (a threefold increased risk for previa )

Incidence 4. a prior uterine incision with a previa increases the likelihood that cesarean hysterectomy will be necessary to control bleeding from a placenta accreta, increta, or percreta l 5. Twofold in women who smoked cigarettes ( l theorized that carbon monoxide hypoxemia caused compensatory placental hypertrophy. Perhaps related, defective decidual vascularization, the possible result of inflammatory or atrophic changes, is implicated in the development of previa. ) 6. Women with otherwise unexplained elevated screening levels of maternal serum alphafetoprotein (MSAFP) are at greater risk for previa (increased MSAFP levels of 2. 0 Mo. M at 16 -week screening) l Increased family planning acceptance with limitations and spacing of births , lowers the incidences of pl. pr. l

Aetiology l Not are definitely known. Responsible factors Persistance of chorionic activity in the decidua capsularis and its sudsequent development into capsular placenta coming in contact with decidua vera of lower segment can explain the formation of lesser degrees of pl pr. . l Dropping down theory : Low implantation of the ovum in the smooth and spaceous uterine cavity of the multipara. poor decidual reaction in the upper segment may be the cause. l Defective decidua , results in spreading of the chorionic villi over a wide area in the uterine wall to get nourishment l Large placenta as in twins can encroach lower segment. l

Pathological anatomy l l l Placenta – seen after delivery May be large and thin Often a large tongue shaped extension from the main placental mass is seen Extensive areas of degeneration with infarction and calcification is seen Placenta at times morbidly adherent to the lower segment due to poor decidual formation.
Pathological anatomy l l l Umbilical cord – It may be attached to the margin – batteledore or into the membranes –villamentous Insertion of the cord may be closed to the internal os or the fetal vessels may run across the internal os giving rise to vasa previa which can rupture along with rupture of the membranes. Lower uterine segment and cervix – Soft and friable due to increased vascularity.

Causes of haemorrhage l l l l The non elastic placenta gets detached from the progressively dilating lower uterine segment during last trimester of pregnancy and there by bleeding occurs from the opened maternal sinuses. The bleeding is inevitable , as it is a physiological phenomenon. In some cases coitus may excite bleeding. Separation of the placenta may be provoked by trauma, including vaginal exam. , external version , or during high rupture of membranes. It is the maternal blood that is always lost. Rarely from torn placenta fetal blood can be lost. In vasa previa, fetal blood from torn blood vessel in fetal membrane crossing internal os is found –rare one.

l l The mechanisms of spontaneous control of bleeding are 1 Thrombosis of the open sinuses, 2 Mechanical pressure by the presenting part, 3. Placental infarcts

Placenta Previa Clinical Findings The most characteristic event in placenta previa is painless haemorrhage, which usually does not appear until near the end of the second trimester or after. (However, bleeding may begin earlier, and some abortions may result from such an abnormal location of the developing placenta. ) With many previas, bleeding begins without warning and without pain in a woman who has had an uneventful prenatal course. Fortunately, the initial bleeding is rarely so profuse as to prove fatal. –WARNING haemorrhage Usually it ceases, only to recur. In some women, particularly those with a placenta implanted near but not over the cervical os, bleeding does not appear until the onset of labor. Then, it may vary from slight to profuse and clinically may mimic placental abruption.

Placenta Previa When the placenta is located over the internal os, the formation of the lower uterine segment and the dilatation of the internal os result inevitably in tearing of placental attachments. The bleeding is augmented by the inherent inability of myometrial fibers of the lower uterine segment to contract and thereby constrict the avulsed vessels. Hemorrhage from the implantation site in the lower uterine segment may continue after placental delivery because the lower uterine segment contracts poorly. Bleeding may also result from lacerations in the friable cervix and lower uterine segment, especially following manual removal of a somewhat adhered placenta.

Placenta Previa Placenta Accreta, Increta, and Percreta Placenta previa may be associated with placenta accreta or one of its more advanced forms, placenta increta or placenta percreta. Such abnormally firm attachment of the placenta might be anticipated because of poorly developed decidua in the lower uterine segment. Almost 7 percent had an associated abnormal placental attachment. Approximately half of specimens from previas showed myometrial spiral arterioles with trophoblastic giant-cell infiltration, only 20 percent from normally implanted placentas had these changes.

Placenta Previa Coagulation Defects Coagulopathy is rare with placenta previa, even when there is extensive separation from the implantation site. Presumably thromboplastin, which incites intravascular coagulation that commonly characterizes placental abruption, readily escapes through the cervical canal rather than being forced into the maternal circulation.
Symptoms l Bleeding l l – per vagina is painless , apparently causeless, and recurrent. Often during sleep – pt finds herself in pool of blood on waking up. Starts any time after 28 weeks Highest incidence at 36 -38 weeks. May cease spontaneously within few hours to recur Warning haemorrhage is usual. l Pain in abdomen is absent unless spontaneous labour starts. l l

Signs l l l l l Evidences of late pregnancy present Evidences of blood loss – shock and anemia may be present depending on the degree of haemorrhage. P/A Obstetric findings Abdomen is soft Uterus is in normal consistancy -relaxed, soft and elastic without any localised area of tenderness. Size of the uterus =gestation age. Fetus is felt normally The presenting part usually non engaged Malpresentaion or unstable lie is more common FHS audible usually , absent in marked placental separation
Signs l l l Vulval inspection. Presence of active bleeding –bright red in colour If bleeding has ceased , cloth staining should be looked for to assess blood loss. Presence of blood in webs of toes of feet should be looked for. From this suspected diagnosis of placenta previa is to be made. 2 days following cessation of bleeding , gentle P/S examination should be done to exclude cervical polyp, , cervical carcinoma.

Confirmation of placenta previa by vaginal examination is done in DOUBLE SET UP – IN operation theater with all preparation ready for LSCS , as it is risky and dangerous , procedure can excite severe bleeding which may kill the patient l In cases with dilated cervix, confirmed diagnosis is made by palpating the placenta in the lower uterine segment, which is tough and elastic and friable. ( blood clot is soft and friable. ) l l In closed os , placenta can be felt in the fornices as indefinite boggy mass on the indistinctly felt presenting part.
Differential diagnosis l l l Abruptio placentae Cervical polyp Cervical carcinoma Fetal haemorrhage in ruptured vasa previa is identified by Singer’s test ( fetal hb is resistant to alkali to form alkali hematin) Cicumvallate placenta causes slight bleeding , diagnosis is made after delivery, after examination of placenta.

d/d of placenta previa and abruptio placenta Vaginal bleeding is revealed, bright red , painless and recurrent Vaginal bleeding is either concealed or revealed but dark red , painful and continuous Pain in abdomen is absent Pain in abdomen is present, acute in severe cases Patient is ordinarily not shocked, unless bleeding is severe Incidence of preeclampsia is not high shock, moderate to severe present depending on amount of revealed or concealed bldg. Incidence of preeclampsia is high.

d/d of placenta previa and abruptio placenta Uterus is felt elastic and soft with floating fetal presentation or abnormal presentation FHS is usually normal P/V exam –pl acenta in lower segment Uterus is felt firm or hard and tender in severe cases enlargement of fundus , fetus is felt with difficulty, absent FHS P/V exam – can not detect placenta , soft friable blood clot can be felt Placental sonography is diagnostic Retroplacental sonolucency of blood clot is suggestive

Placenta Previa Diagnosis Placenta previa or abruption should always be suspected in women with uterine bleeding during the latter half of pregnancy. The possibility of placenta previa should not be dismissed until sonographic evaluation has clearly proved its absence. The diagnosis can seldom be established firmly by clinical examination unless a finger is passed through the cervix and the placenta is palpated. Such digital cervical examination is never permissible unless the woman is in an operating room with all the preparations for immediate cesarean delivery—even the gentlest digital examination cause torrential hemorrhage.

Double set-up" examination l This type of examination should not be performed unless delivery is planned, for it may cause bleeding that necessitates immediate delivery. l This "double set-up" examination is rarely necessary today because placental location can almost always be ascertained by sonography.

Placenta Previa Sonographic Localization The simplest, safest, and most accurate method of placental localization is provided by transabdominal sonography. The average accuracy is 96 percent to 98 %. False-positive results are often a result of bladder distension. ( Therefore, scans in apparently positive cases should be repeated after emptying the bladder. ) Additionally provides information regarding fetal maturity , well being of fetus , rules out congenital anomalies. The use of transvaginal sonography has substantively improved diagnostic accuracy of placenta previa. Although it may appear dangerous to introduce an ultrasound probe into the vagina in suspected cases without touching the cervix, the technique has been shown to be safe. TVS 100% accuracy as compared to 70 %TAS

Sonographic Localization l Transperineal sonography was reported accurate to localize placenta previa by Hertzberg and colleagues. l well accepted by pts. l Internal os is visualised in 97 -100% of cases. l Colour doppler flow study l Prominent venous flow in the hypoechoic areas near the cervix is consistent with the diagnosis of placenta previa.
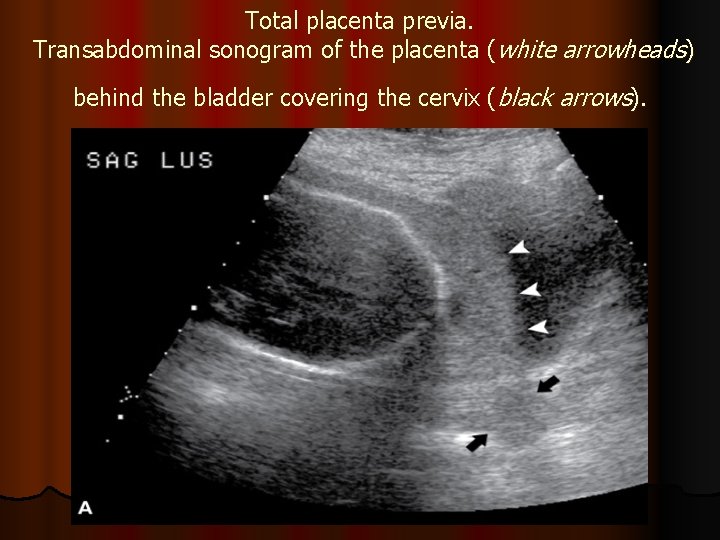
Total placenta previa. Transabdominal sonogram of the placenta (white arrowheads) behind the bladder covering the cervix (black arrows).
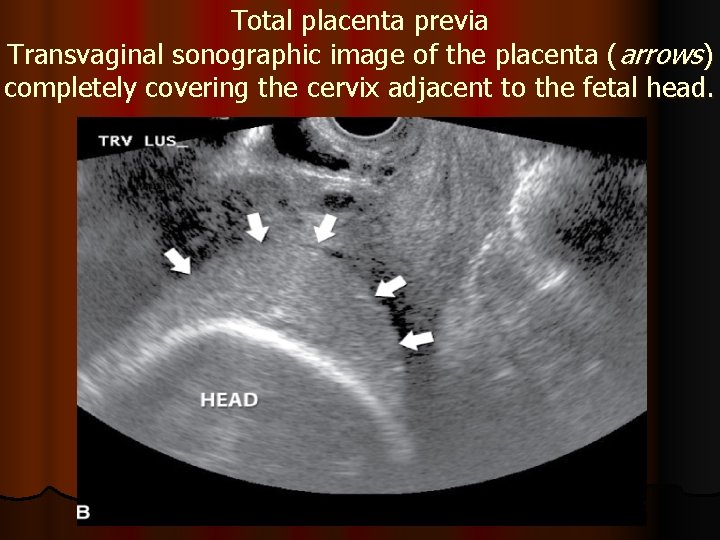
Total placenta previa Transvaginal sonographic image of the placenta (arrows) completely covering the cervix adjacent to the fetal head.

Placenta Previa Magnetic Resonance (MR) Imaging A MR imaging to visualize placental abnormalities, including previa. It is unlikely that MR imaging will replace sonographic scanning for routine evaluation in the near future. MR imaging may prove useful for diagnosis of placenta accreta. Limitations of MRI More time consuming , lack of portability, costilest

l l Placental migration USG at 17 weeks of gestation, reveals placenta covering the internal os in about 10% cases. l Repeat USG at 37 weeks showed no placenta in the lower uterine segment in more than 90% cases. l During third trimester there is potential ten fold growth of lower uterine segment compared to the placenta. l Due to this disproportionate growth there is an apparant migration of placenta towards the fundus.

Placenta Previa Placental "Migration. " l. The apparent peripatetic nature of the placenta has been well established at midpregnancy. l 12 percent of placentas were "low lying in midpregnancy. “ l Of those not covering the internal os, previa did not persist and hemorrhage was not encountered. l Of those covering the os at midpregnancy, approximately 40 percent persisted as a previa. l. Thus, placentas that lie close to the internal os— but not over it — during the second trimester or early third trimester are unlikely to persist as a previa by term.

Placenta Previa The mechanism of apparent placental movement is not completely understood. l migration is clearly a misnomer because decidual invasion by chorionic villi on either side of the cervical os persists. l The apparent movement of the low-lying placenta relative to the internal os probably results from inability to precisely define this relationship in a three dimensional manner using two-dimensional sonography in early pregnancy. l This difficulty is coupled with differential growth of lower and upper myometrial segments as pregnancy progresses. l Thus, those placentas that "migrate" most likely never had actual circumferential villus invasion that reached the internal cervical os in the first place.

Management -Prevention l l l This is an inherent obstetric hazard, in majority cause is unknown. To minimise risks, following guidelines may be helpful. Adequate antenatal care to improve anemia and health status of woman Antenatal screening at 20 weeks to know exact location of placenta and to repeat it whenever necessary to confirm. Significance of warning haemorrhage should not be ignored. Family planning and limitations of births to reduce incidences of pl. pr.

Management -Prevention l l l l At home – rest, immediately transfer to hospital in 108 , or other vehicle. Admission to hospital No p/v exam. Of APH PT. Immediate assessment of patient vitals and attention to Amount of blood lost, Blood samples taken for bl. grp and x match Iv line taken , infusion of saline or ringer lactate started

Placenta Previa Management of Placenta Previa l. Women with a previa may be considered in one of the following categories: l. A. The fetus is preterm and there are no other indications for delivery l. B. The fetus is reasonably mature l. C. Labor has ensued l. D. Hemorrhage is so severe as to mandate delivery despite gestational age.

A. The fetus is preterm and there are no other indications for delivery l. Management with a preterm fetus, but without persistent active uterine bleeding, consists of close observation. Expectant treatment–Macafee – 1945 l. Objects: 1. to advance fetal maturity 2. to treat maternal anemia 20 % cases avail expectant treatment. -Total bed rest in hopital till 38 weeks. -pt goes to toilet with relative or under supervision -To have adequate food , iron folic acid vit b 12 capsule a day -Tab diazepam or alprazolam at night

Expectant treatment–Macafee – 1945 l l l For some women, prolonged hospitalization may be ideal. However, a woman is usually discharged after bleeding has ceased and her fetus judged to be healthy. The woman and her family must fully appreciate the possibility of complications and be prepared to transport her to the hospital immediately. In properly selected patients, there appears to be no benefit to inpatient versus outpatient management of placenta previa. Importantly, there are no differences in maternal or fetal morbidity rates with outpatient versus inpatient observation

l l Premature termination may be needed in 1. recurrence of brisk haemorrhage and which is continuous, 2. the fetus is dead 3. the fetus is found to be congenital abnormal

B. The fetus is reasonably mature l l l l Placental sonography grading of pl pr 38 weeks of pregnancy Active treatment Placenta previa I , II anterior induction of labour ARM constant fetal monitoring ang maternal monitoring delivery Placenta previa II posterior, III, IV , withbaby alive or even dead baby. Caesarian section is done under blood transfusion. Cesarian section is also done in high risk pregnancy, malpresentation and elderly primigravida in all cases of placenta previa

C. Labor has ensued l l l l Low rupture of membranes for mild degree plaenta previa close observation , fetal and maternal monitoring as in normal cases. Precautions during vaginal delivery 1. all possible steps to be taken to restore the blood volume 2. methergin. 2 mg to be given iv with antr shoulder delivery 3. exam of cervix after delivery to rule out carvical tear Baby’s Hb to be cheked BT given if nacessary. Caesarean section in severe degree placenta previa.

Placenta Previa l. Delivery l. Cesarean delivery is necessary in practically all women with placenta previa. l Most often, a transverse uterine incision is possible. l. However, because fetal bleeding may result from a transverse incision into an anterior placenta, a vertical incision is sometimes employed. l But, even when the incision extends through the placenta, maternal or fetal outcomes are rarely compromised. l. Ward (2003) described an alternative surgical technique in which a cleavage plane is developed following the uterine incision. l The operator undermines the placenta toward the closest edge until the membranes are palpable and they are then ruptured with the fetus delivered around the intact placenta.

Placenta Previa l. Because of the poorly contractile nature of the lower uterine segment, there may be uncontrollable hemorrhage following placental removal. l. When bleeding from the placental bed cannot be controlled by conservative means, other methods can be attempted. l. Oversewing the implantation site with 0 -chromic sutures may provide hemostasis. l. In some women, bilateral uterine or internal iliac artery ligation may provide hemostasis. l. Cho and colleagues (1991) described placing interrupted 0 -chromic sutures one centimeter apart and forming a sutured circle around the bleeding portion of the lower segment. .

Placenta Previa Pelvic artery embolization also has gained acceptance. l. If such conservative methods fail, and bleeding is brisk, then hysterectomy is necessary. l For women whose placenta previa is implanted anteriorly in the site of a prior hysterotomy incision, there is an increased likelihood of associated placenta accreta and need for hysterectomy. l

Placenta Previa Maternal and Perinatal Outcomes A marked reduction in maternal mortality rates from placenta previa was achieved during the last half of the 20 th century. placenta previa is an important cause of maternal morbidity and mortality. an approximately threefold increased maternal mortality ratio of 30 per 100, 000.

Placenta Previa Complications Maternal During pregnancy Antepartum haeamorrhage with varying degrees of shock Malpresentation Premature labour During labour Early rupture of membrane Cord prolapse Slow dilatation of the cervix Intrapartum haeamorrhage Increased incidences of operative interferance

Placenta Previa PPH – Imperfect retraction of the lower uterine segment , Large surface area of placenta – anemia, twins Ocassionally associated morbidly adherent placenta – pl accreta, increta, percreta on the lower uterine segment Retained placenta Puerperium Sepsis is increased Due to increased operative interferance Placental site near the vagina Anemia Devitalised state of pt Subinvolution and embolism

Perinatal Outcomes l l l Preterm delivery as a result of placenta previa is a major cause of perinatal death. the neonatal mortality rate to be threefold increased in pregnancies complicated by placenta previa. This was primarily because of increased preterm birth rates. this risk appears related to fetal-growth restriction and limited prenatal care. an association of increased congenital malformations and previa was not confirmed fetal anomalies were increased 2. 5 -fold in pregnancies complicated by placenta previa. The association of fetal-growth restriction with placenta previa is less certain.
l Fetal complications l Low birth weight Asphyxia Intrautrine death Birth injuries Congenital malformations l l
- Slides: 51