Pick up A Homework booklet Heart Questions Whiteboard

Pick up: A Homework booklet ü Heart Questions ü Whiteboard and pen ü

Complete the questions on the heart. You can use your notes and the textbooks to help you (p 170 -177). You have 15 minutes!

We are going to look at:
Arteries: Carry blood away from the heart Arterioles: Control blood flow from arteries to capillaries Capillaries: Link arterioles to venules Venules: Link capillaries to veins Veins: Carry blood towards the heart Can you label your diagram 1 with the vessels above?
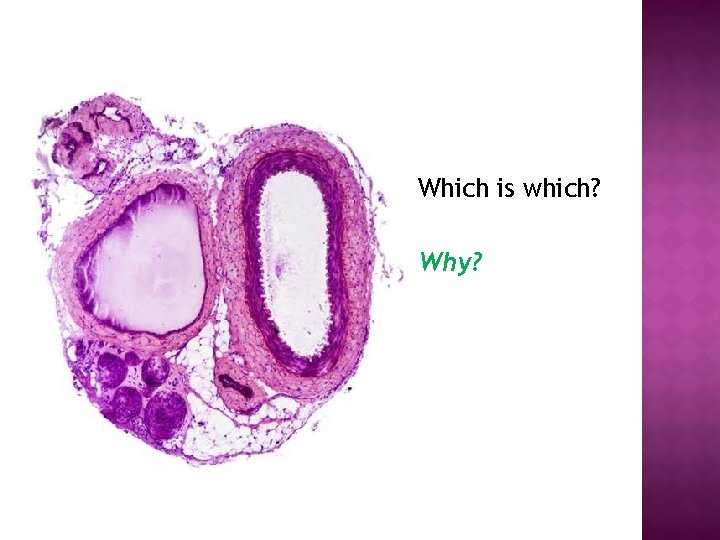
Which is which? Why?
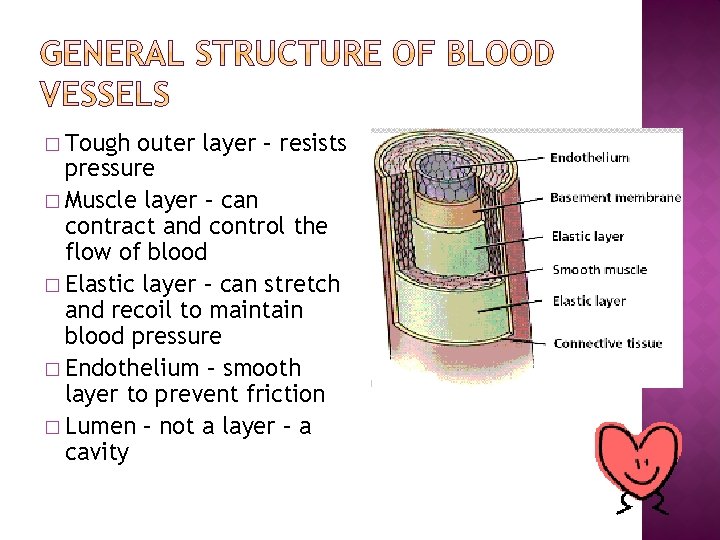
� Tough outer layer – resists pressure � Muscle layer – can contract and control the flow of blood � Elastic layer – can stretch and recoil to maintain blood pressure � Endothelium – smooth layer to prevent friction � Lumen – not a layer – a cavity
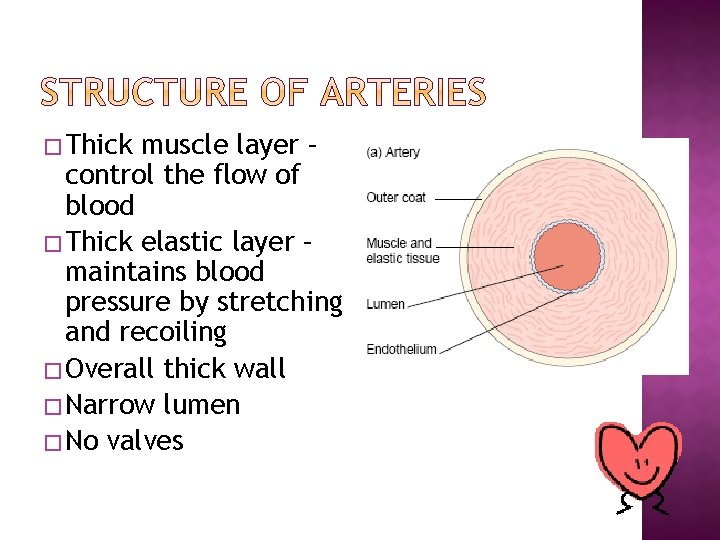
� Thick muscle layer – control the flow of blood � Thick elastic layer – maintains blood pressure by stretching and recoiling � Overall thick wall � Narrow lumen � No valves
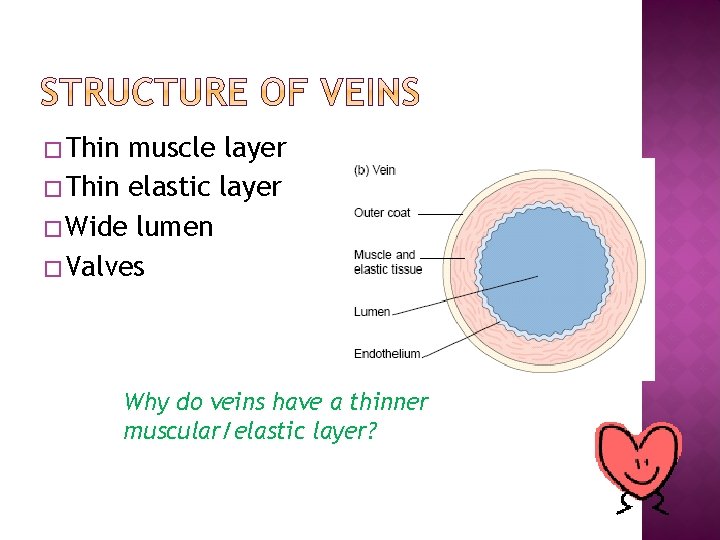
� Thin muscle layer � Thin elastic layer � Wide lumen � Valves Why do veins have a thinner muscular/elastic layer?
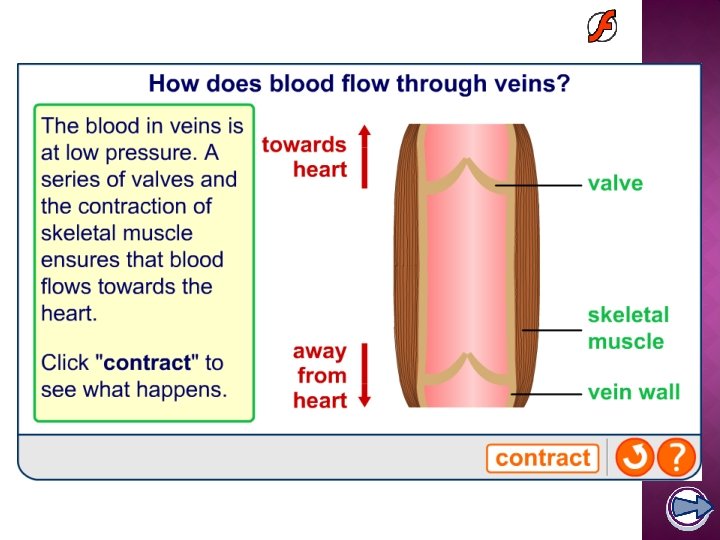
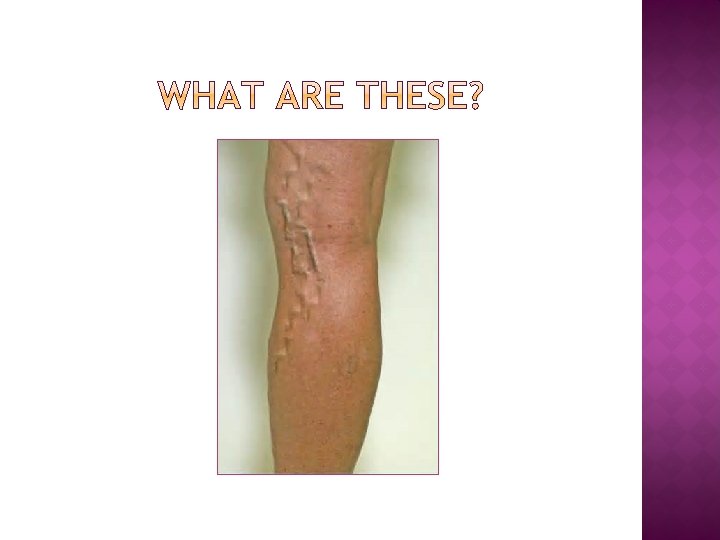
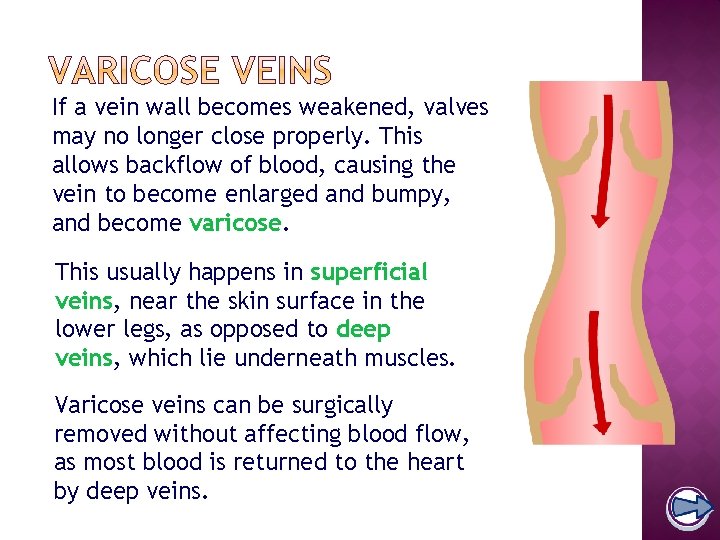
If a vein wall becomes weakened, valves may no longer close properly. This allows backflow of blood, causing the vein to become enlarged and bumpy, and become varicose. This usually happens in superficial veins, near the skin surface in the lower legs, as opposed to deep veins, which lie underneath muscles. Varicose veins can be surgically removed without affecting blood flow, as most blood is returned to the heart by deep veins.

� No muscle � No elastic � Thin only layer of cells
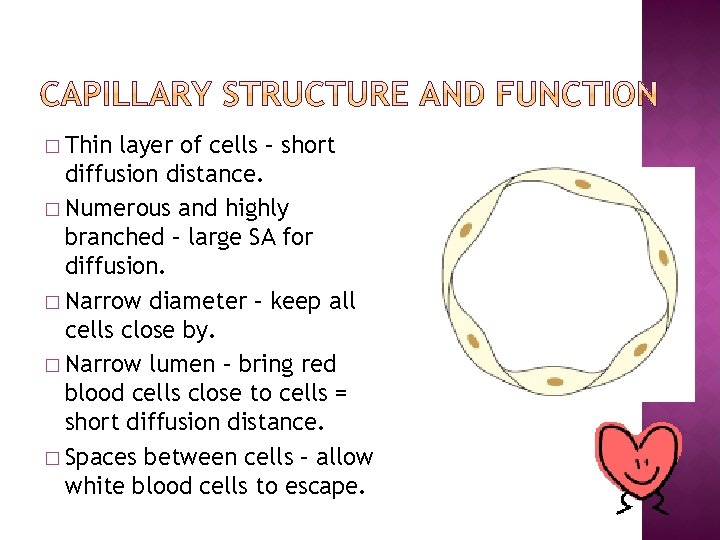
� Thin layer of cells – short diffusion distance. � Numerous and highly branched – large SA for diffusion. � Narrow diameter – keep all cells close by. � Narrow lumen – bring red blood cells close to cells = short diffusion distance. � Spaces between cells – allow white blood cells to escape.
Make a note… STRUCTURE OF VENULES � Thicker muscle layer than arteries � Thinner elastic layer than arteries � Can constrict to control blood flow through capillaries � Muscle and elastic layers � Similar to veins but lumen is smaller � Can constrict to control blood flow.

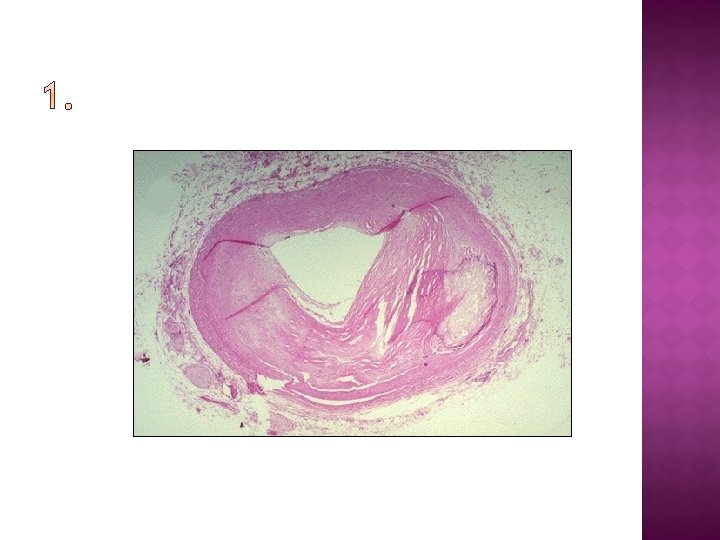
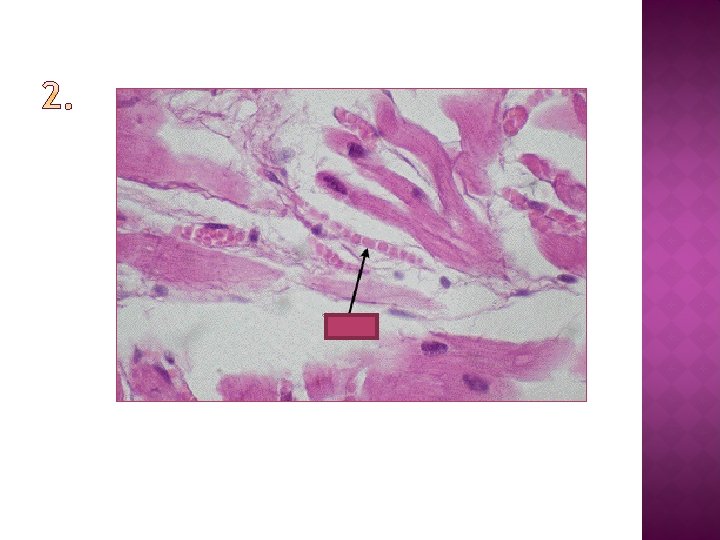
Using your knowledge of blood vessel structure (and your notes), identify the type of blood vessel in the following images and diagrams…


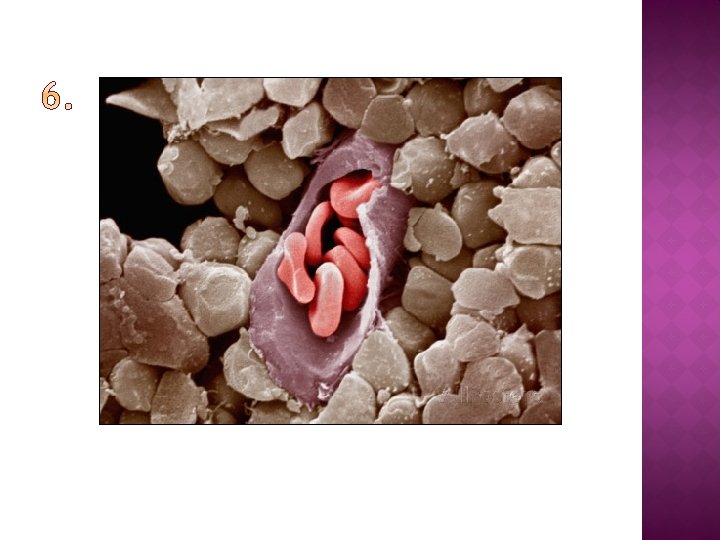
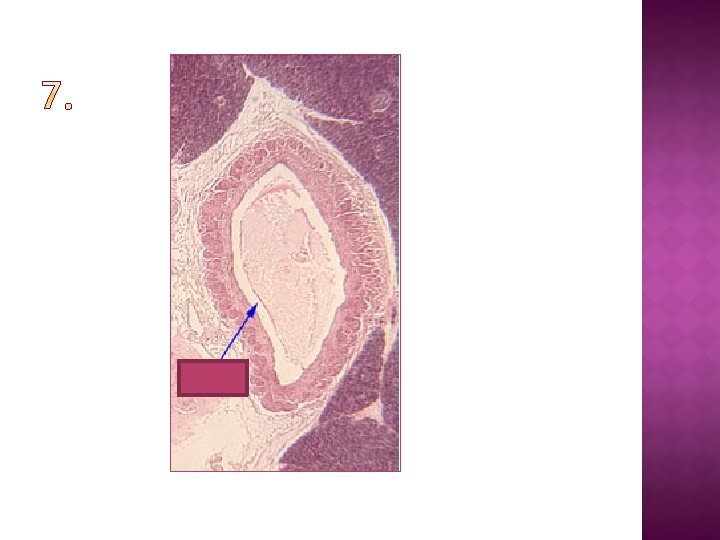
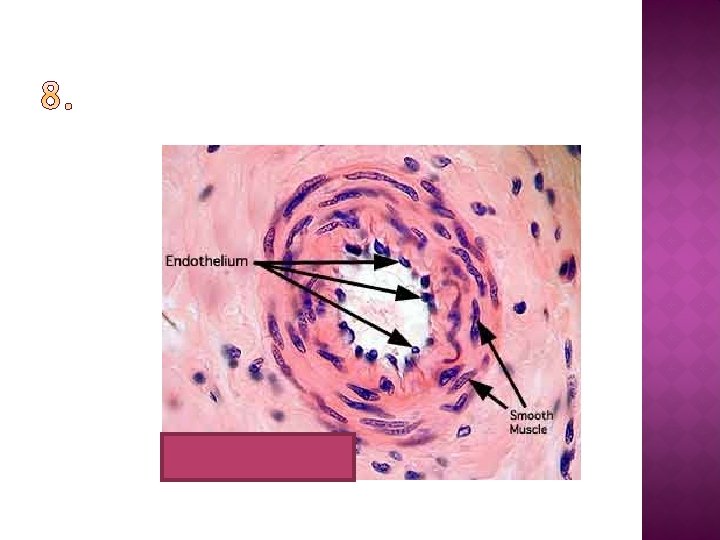

You should be able to: � explain what tissue fluid is and which substances it contains � Explain the formation of tissue fluid in terms of hydrostatic pressure � Explain the reabsorption of some tissue fluid back into the capillaries, in terms of hydrostatic pressure and water potential � Explain the role of the lymph system.

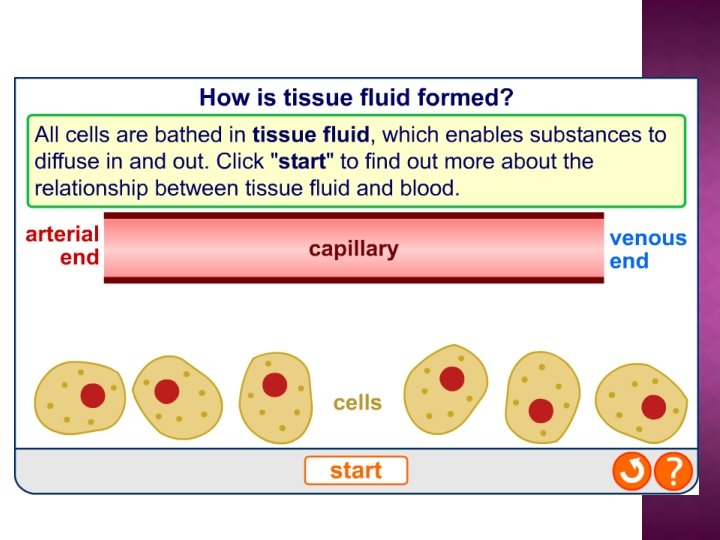
Tissue fluid is a watery solution in which the cells of the body are ‘bathed’(also known as interstitial fluid). It supplies the cells with the substances they need for their metabolic processes and also receives waste materials from the cells. Which substances can be found dissolved in the tissue fluid?
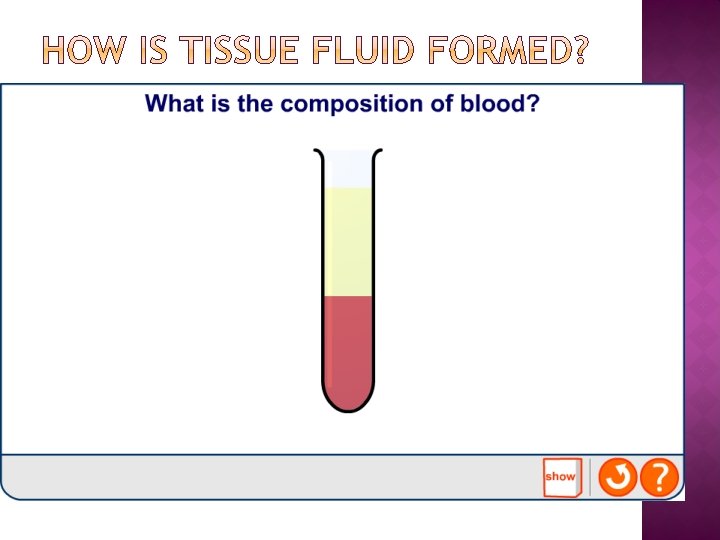

About 8% of blood plasma consists of plasma proteins, of which about half may be albumins. These are a group of small proteins involved in the transport of other substances (e. g. fatty acids, hormones) and which help regulate the osmotic pressure of blood. The balance between the hydrostatic pressure of blood (‘blood pressure’) and the osmotic pressure of blood is important in the formation of tissue fluid.
Using your diagram, explain to the person next to you how tissue fluid is formed, and how it returns to the blood. Remember to use the terms: Hydrostatic pressure Osmotic pressure (/low water potential) Ultrafiltration

Get your homework questions out ready!

ü 1. (Overall) outward pressure of 3. 2 k. Pa; ü 2. Forces small molecules out of capillary; Loss of water / loss of fluid / friction (against capillary lining);

ü 1. High blood pressure = high hydrostatic pressure; ü 2. Increases outward pressure from (arterial) end of capillary / reduces inward pressure at (venule) end of capillary; ü 3. (So) more tissue fluid formed / less tissue fluid is reabsorbed; Allow lymph system not able to drain tissues fast enough ü 1. Water has left the capillary; ü 2. Proteins (in blood) too large to leave capillary; ü 3. Increasing / giving higher concentration of blood proteins (and thus wp);

(Blood) plasma; ü More / larger proteins / less urea / carbon dioxide / more glucose / amino acids / fatty acids / oxygen / high(hydrostatic) pressure; Q Reference to blood cells / water potential = neutral Q No Protein should not be credited ü Contracts; Q Do not accept pumping of heart / heart beating

ü Loss of fluid / volume; ü Friction / resistance (of capillary wall); Q Reference to a narrow lumen is not sufficient to gain a mark unless friction or resistance is mentioned. ü Water potential (in capillary) not as low / is higher / less negative / water potential gradient is reduced; ü More tissue fluid formed (at arteriole end); ü Less / no water absorbed (into blood capillary) by osmosis; (into blood capillary); Q The last two marking points must be in context of movement into the blood capillary
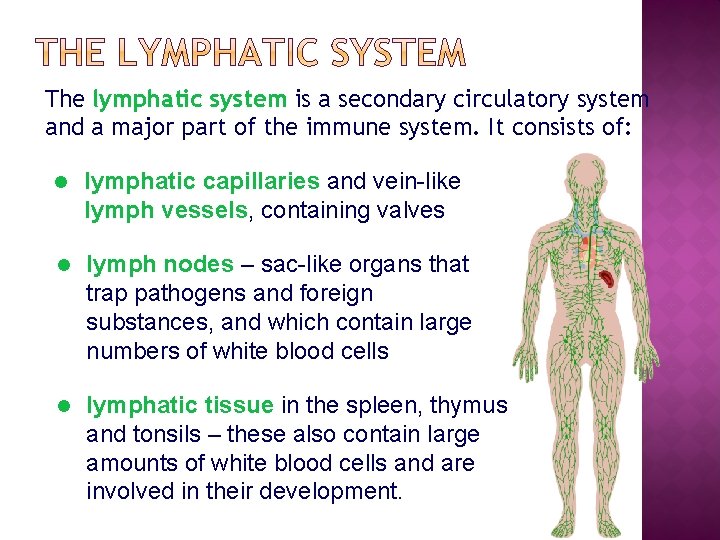
The lymphatic system is a secondary circulatory system and a major part of the immune system. It consists of: l lymphatic capillaries and vein-like lymph vessels, containing valves l lymph nodes – sac-like organs that trap pathogens and foreign substances, and which contain large numbers of white blood cells l lymphatic tissue in the spleen, thymus and tonsils – these also contain large amounts of white blood cells and are involved in their development.
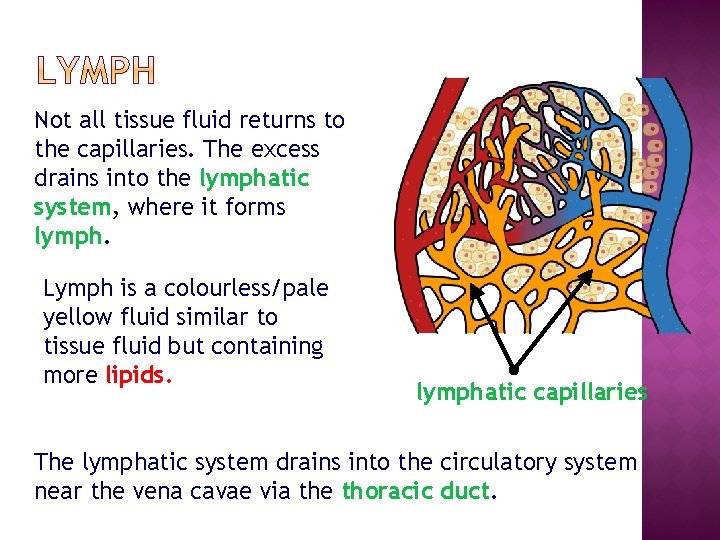
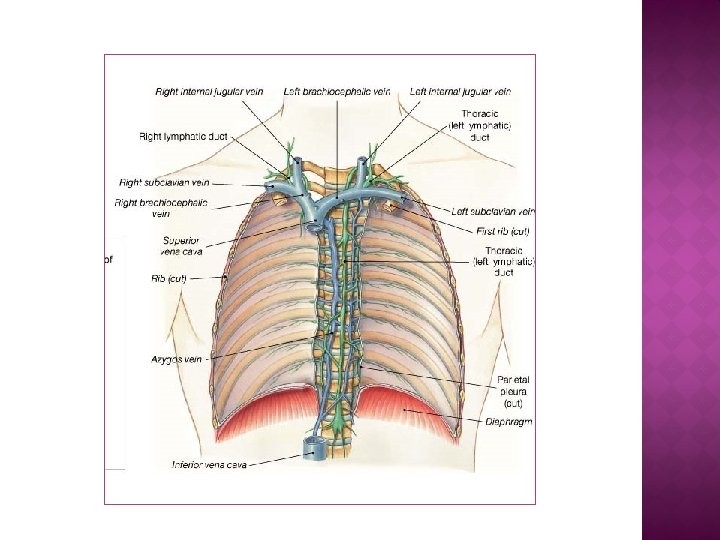
Not all tissue fluid returns to the capillaries. The excess drains into the lymphatic system, where it forms lymph. Lymph is a colourless/pale yellow fluid similar to tissue fluid but containing more lipids. lymphatic capillaries The lymphatic system drains into the circulatory system near the vena cavae via the thoracic duct.
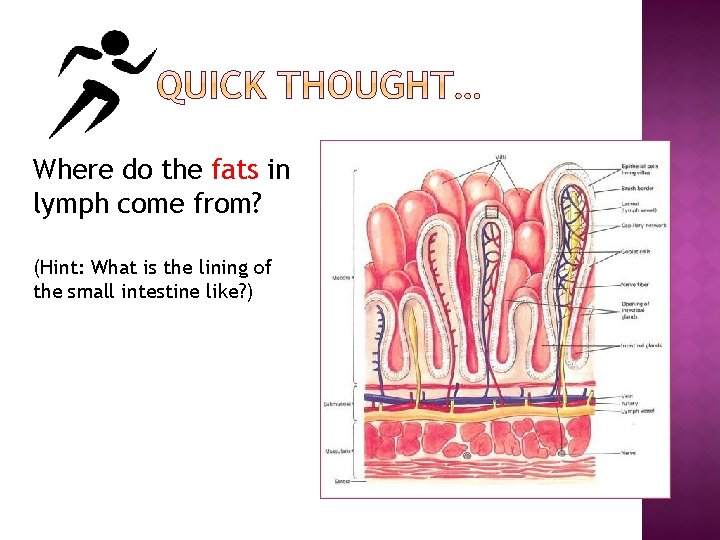
Where do the fats in lymph come from? (Hint: What is the lining of the small intestine like? )
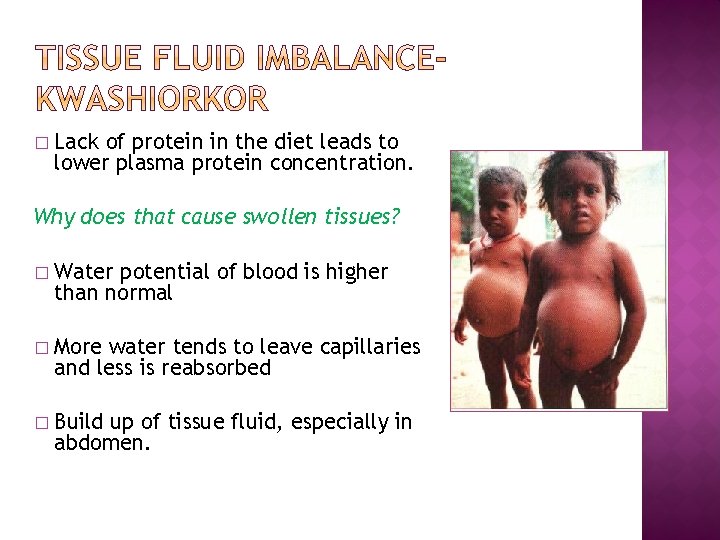
� Lack of protein in the diet leads to lower plasma protein concentration. Why does that cause swollen tissues? � Water potential of blood is higher than normal � More water tends to leave capillaries and less is reabsorbed � Build up of tissue fluid, especially in abdomen.
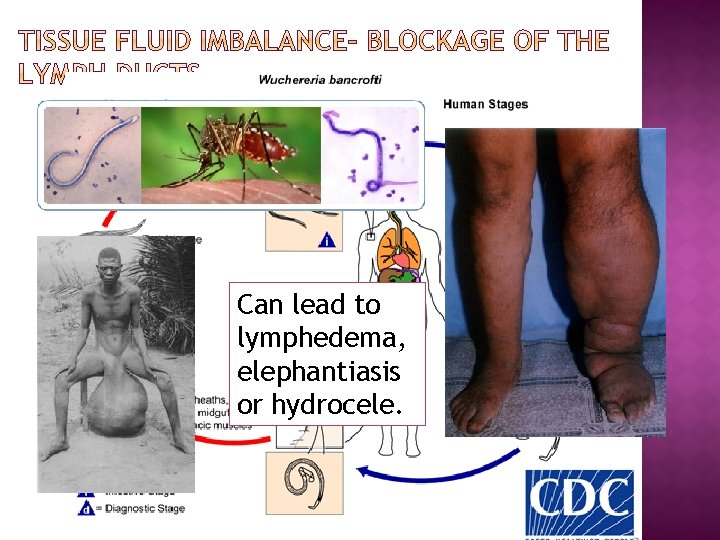
Can lead to lymphedema, elephantiasis or hydrocele.
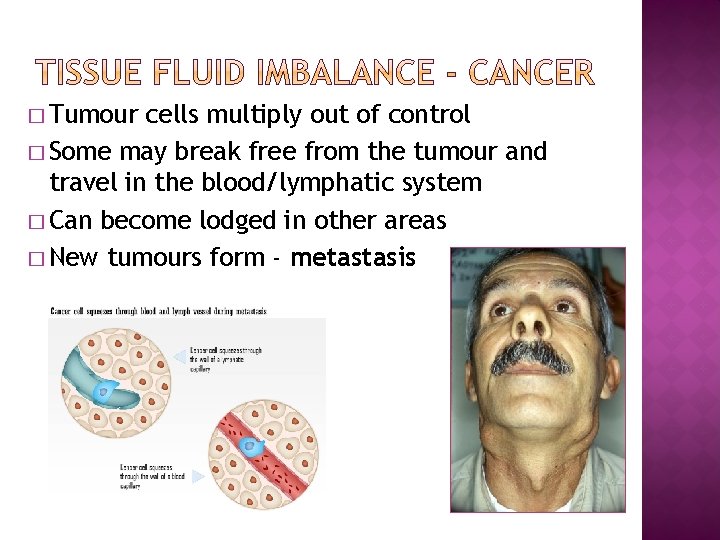
� Tumour cells multiply out of control � Some may break free from the tumour and travel in the blood/lymphatic system � Can become lodged in other areas � New tumours form - metastasis

You should be able to: � Explain the causes and consequences of cardiovascular disease � Analyse and interpret data associated with specific risk factors and the incidence of cardiovascular disease � Recognise correlations and causal relationships.

A general term that describes diseases of the heart and circulatory system. There are four main types of CVD. They are: � coronary heart disease � stroke � peripheral arterial disease � aortic disease

Key contributors to CDV development include atherosclerosis (‘hardening of the arteries’) and thrombus (blood clot) formation.
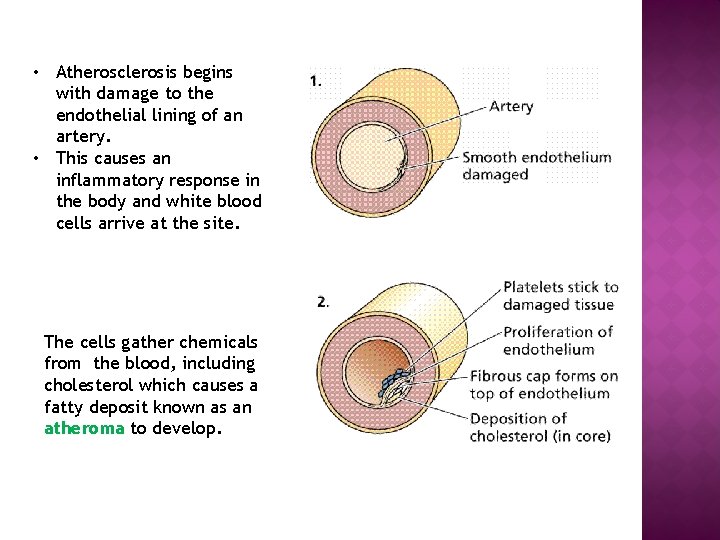
• Atherosclerosis begins with damage to the endothelial lining of an artery. • This causes an inflammatory response in the body and white blood cells arrive at the site. The cells gather chemicals from the blood, including cholesterol which causes a fatty deposit known as an atheroma to develop.
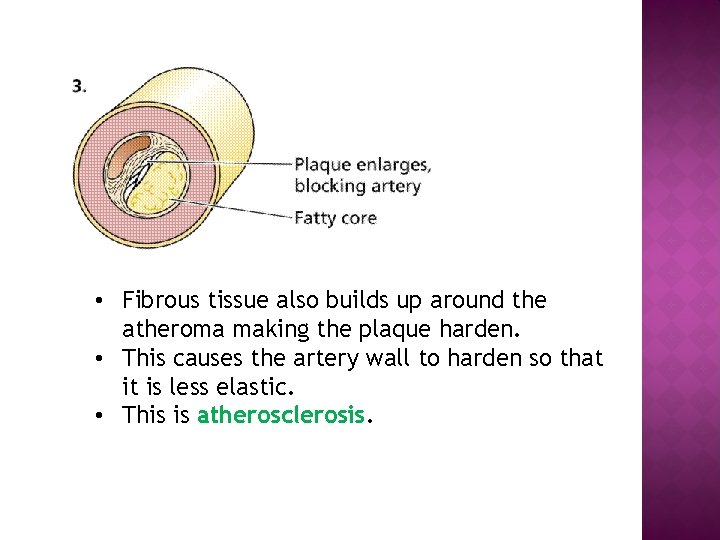
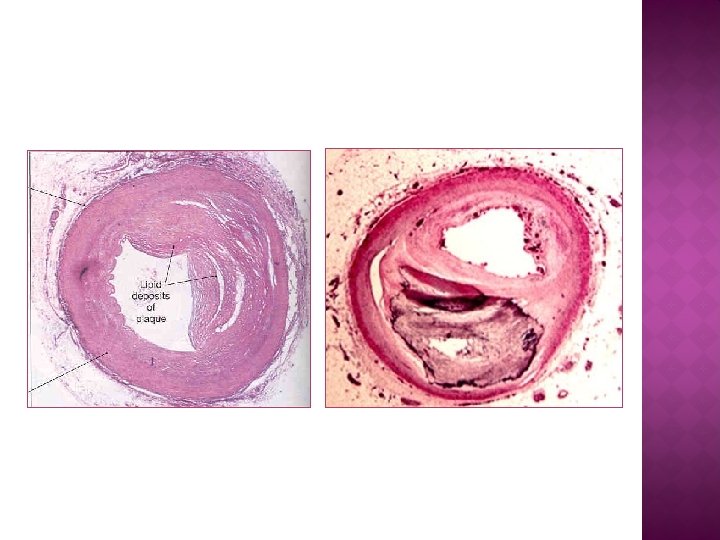
• Fibrous tissue also builds up around the atheroma making the plaque harden. • This causes the artery wall to harden so that it is less elastic. • This is atherosclerosis.

You should be able to: � Explain the causes and consequences of cardiovascular disease � Analyse and interpret data associated with specific risk factors and the incidence of cardiovascular disease � Recognise correlations and causal relationships.

Risk = the probability of some unwanted event happening Put these causes of death in order, from the most likely to the least likely: • • Accidental poisoning Heart disease Injury purposely inflicted by another person Lightning Lung cancer Railway accidents Road accidents
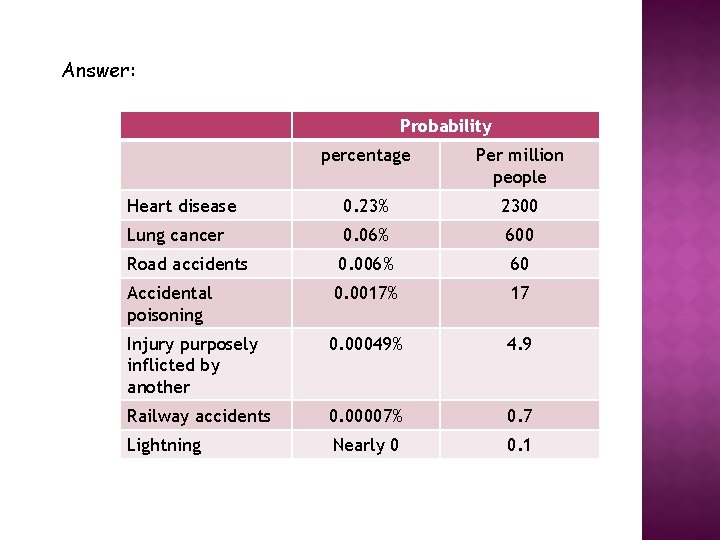
Answer: Probability percentage Per million people Heart disease 0. 23% 2300 Lung cancer 0. 06% 600 Road accidents 0. 006% 60 Accidental poisoning 0. 0017% 17 Injury purposely inflicted by another 0. 00049% 4. 9 Railway accidents 0. 00007% 0. 7 Lightning Nearly 0 0. 1

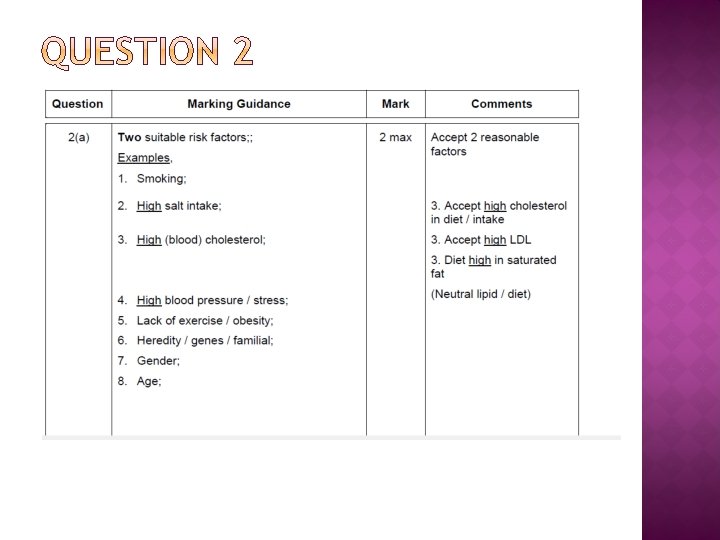
Factors that increase the risk of Cardiovascular Disease • Inheritance: Some people are genetically predisposed to some diseases. • Diet: A diet high in saturated fat, salt and alcohol increases the risk. • Age: Those most at risk are over the age of 40. • Gender: Men are more likely to suffer than women. • High Blood Pressure • Smoking: Chemicals in tobacco smoke can increase the risk. • Physical Inactivity: Exercise can help decrease the risk.

Correlation: A correlation shows a relationship between two variables Positive correlation = 1 variable increases as the other increases. Negative correlation = As 1 variable increases the other decreases. Does a correlation always mean one variable causes the other?

Where one variable directly causes a change in the other, e. g. smoking and heart disease. Only when there is a causal link between two correlated variables can we say one directly affects the other. For example: • There is a positive correlation between speaking english as a first language and life expectancy, but there is no causal link. • There is also a positive correlation between waist measurement and risk of heart attack, but here an increase in waist measurement directly increases the risk of a heart attack.

Strong correlations have been reported between the following pairs of variables. In each case, decide if there is likely to be a causal link between the variables or not. Suggest a possible reason for the correlation. • Shark attacks and ice cream sales. • Children’s foot size and their spelling ability. • Lung cancer and smoking.

Studies • Longitudinal studies follow people over many years so that they can monitor the impact of lifestyle on health over time. • Some studies gather data from smaller studies and compare them to give a bigger picture of what is happening in a population. Evaluating studies Validity: • Does the study answer the question being asked? • Have measurements been carried out with precision? Reliability: • If the study is repeated do you get the same results? • Have enough subjects been tested?

Have a go at the exam questions. You have 10 minutes!

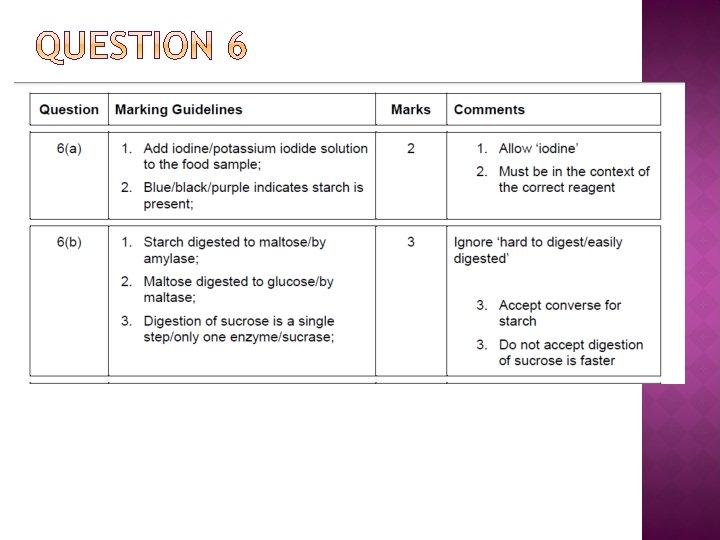
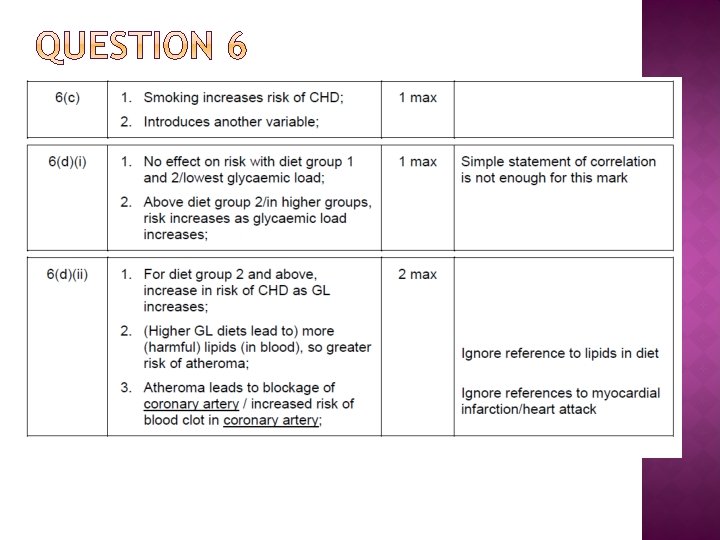
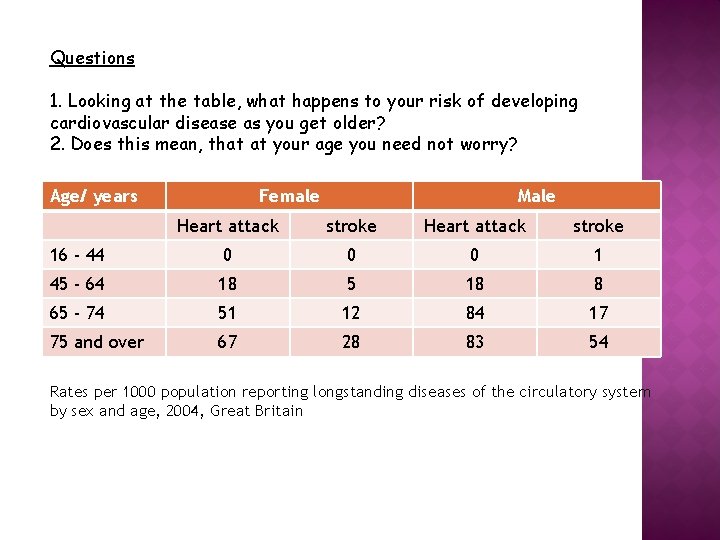
Questions 1. Looking at the table, what happens to your risk of developing cardiovascular disease as you get older? 2. Does this mean, that at your age you need not worry? Age/ years Female Male Heart attack stroke 16 - 44 0 0 0 1 45 - 64 18 5 18 8 65 - 74 51 12 84 17 75 and over 67 28 83 54 Rates per 1000 population reporting longstanding diseases of the circulatory system by sex and age, 2004, Great Britain
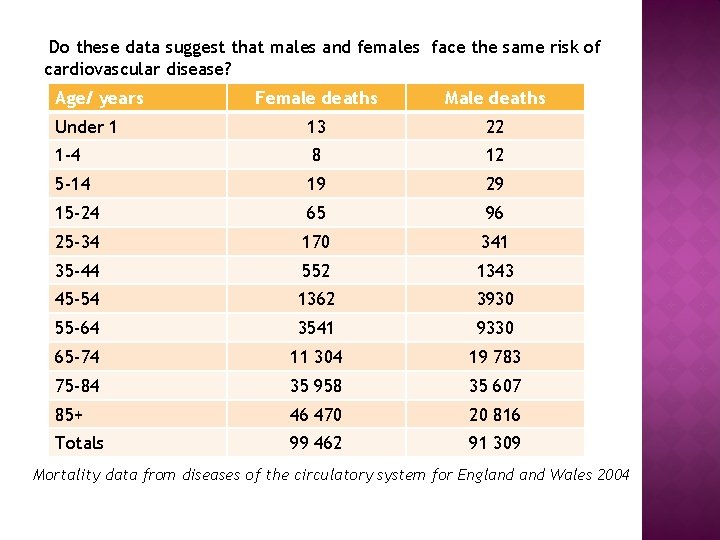
Do these data suggest that males and females face the same risk of cardiovascular disease? Age/ years Female deaths Male deaths Under 1 13 22 1 -4 8 12 5 -14 19 29 15 -24 65 96 25 -34 170 341 35 -44 552 1343 45 -54 1362 3930 55 -64 3541 9330 65 -74 11 304 19 783 75 -84 35 958 35 607 85+ 46 470 20 816 Totals 99 462 91 309 Mortality data from diseases of the circulatory system for England Wales 2004

• Comment on the reliability of the data presented in the two tables. • Many people now think that, until menopause, a woman’s reproductive hormones offer her protection from coronary heart disease. Do these data support this view? • Is it valid to draw this conclusion from these data?
- Slides: 62