Physiology of Blood Platelets Small granulated nonnucleated bodies

Physiology of Blood

Platelets • • Small granulated non-nucleated bodies 2 -4 micron in diameter Life span…. . 8 days Count… 300, 000/mm 3

Hemostasis It is a prevention of blood loss after injury Mechanism 1. Constriction of the blood vessel. local myogenic contraction, nervous reflex & local factors ( serotonin, ADP , thromboxane A 2) 2. Formation of platelet plug 3. Conversion of platelet plug to a definitive clot by fibrin threads ( blood clot) 4. Dissolution of the clot by plasmin after tissue repair

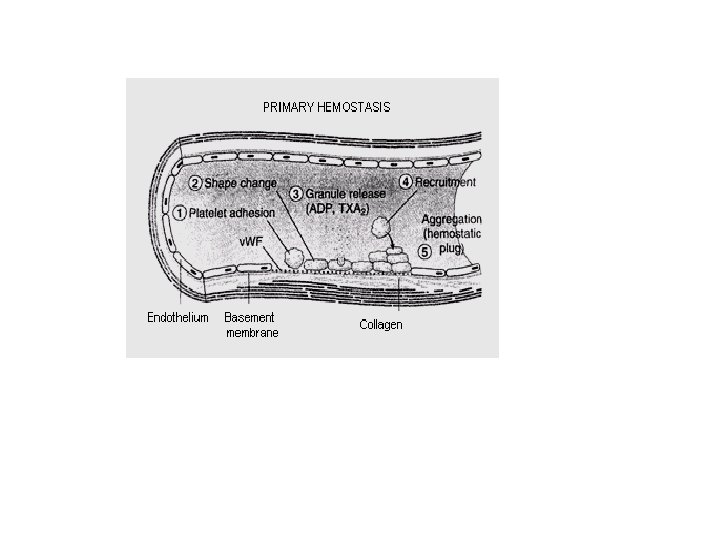
2 - Platelet plug formation Platelet reactions 1 - Platelet adhesion ( to subendothelial collagen- needs von-Willebrand factor) 2 - Platelet activation ( swell& change the shape) 3 - Platelet release reaction ( Ca 2+ , coagualtion factors, serotonin, thromboxane A 2. . . . 4 - Platelet aggregation ( platelet plug) 5 - Platelet procoagulant activity ( activation of coagulation factors) 6 - Platelet fusion ( fusion of aggregated platelets)

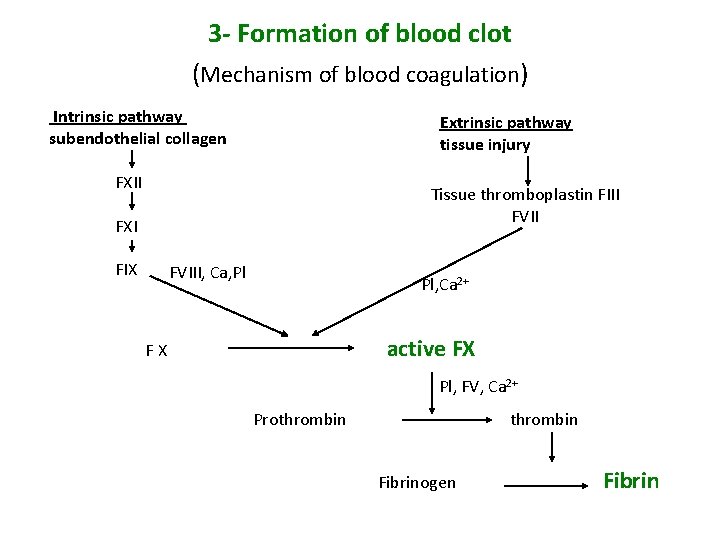
3 - Formation of blood clot (Mechanism of blood coagulation) Intrinsic pathway subendothelial collagen Extrinsic pathway tissue injury FXII Tissue thromboplastin FIII FVII FXI FIX FVIII, Ca, Pl Pl, Ca 2+ active FX FX Pl, FV, Ca 2+ Prothrombin Fibrinogen Fibrin

Coagulation factors • Plasma proteins synthesized by the liver • Most are known by capital Roman numerals • Inactive serine protease enzymes which when activated lead to activation of other factors in a cascade effect

4 - Dissolution of the clot by plasmin after tissue repair Plasmin ( fibrinolysin) • Plasmin is formed from inactive plasminogen by the action of tissue plasminogen activator TPA & thrombin • Plasmin lyses fibrin & fibrinogen into fibrinogen degradation products

Anticlotting mechanisms General limiting reactions…smooth endothelium, rapid blood flow, heparin, liver Specific limiting reaction • Prostacyclin # thromboxane A 2 • Antithrombin III …… inhibits F IX, X, XII • Protein C & protein S …. inhibit F V & VIII • Fibrinolytic system ( plasmin)……lyses of fibrin Anticoagulants ( heparin , dicumarol ) In vitro anticoagulants……precipitation of Ca 2+ , silicon coated tubes & heparin In vivo anticoagulants ……. . Heparin & dicumarol
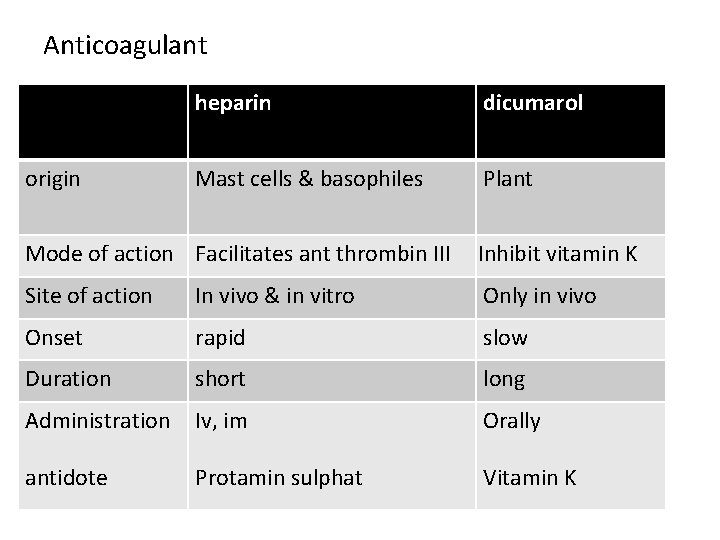
Anticoagulant origin heparin dicumarol Mast cells & basophiles Plant Mode of action Facilitates ant thrombin III Inhibit vitamin K Site of action In vivo & in vitro Only in vivo Onset rapid slow Duration short long Administration Iv, im Orally antidote Protamin sulphat Vitamin K

Abnormalities of hemostasis Thrombocytopenic purpura Decreased platelet count Subcutaneous hemorrhage Plonged bleeding time Vitamin k deficiency vit K is important formation of factors II, VII, , IX, X in the liver It is a fat soluble vitamin & is formed by intestinal flora Its absorption is decreased in obstruction of bile duct Hemophilia Congenital sex-linked disease transmitted by females to males Characterized by sever bleeding after trauma It is due to absence of factor VIII or IX or XI

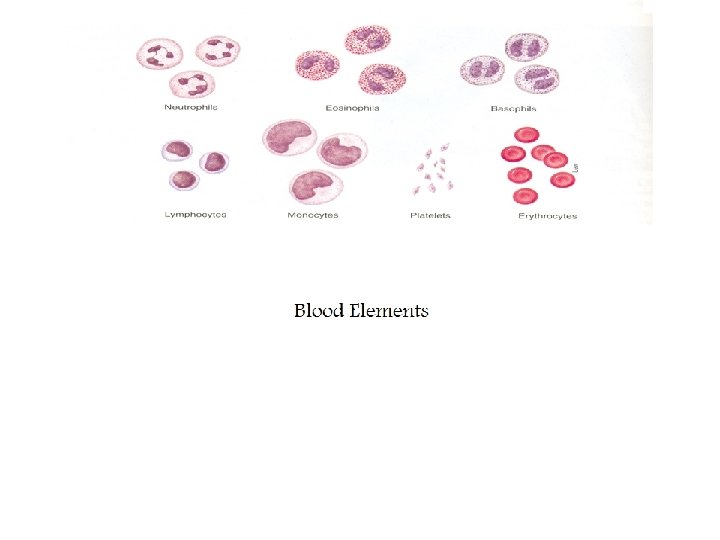
White blood cells 4000 -11000 Granulocytes Neutrophils----50 -70% ingest & kill bacteria Agranulocytes Lymphocytes 20 -40% immunity Esinophils 1 -4 % parasites & allergy Monocytes 2 -8% tissue macrophage Basophils 0. 5% histamine & heparin
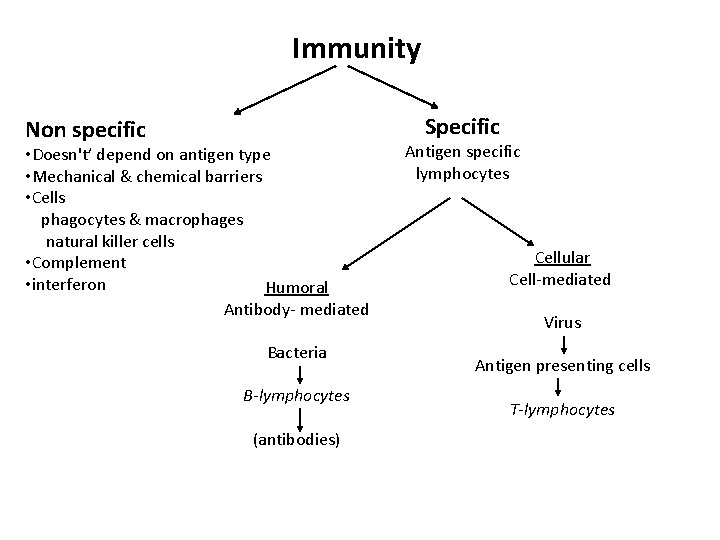
Immunity Specific Non specific • Doesn't’ depend on antigen type • Mechanical & chemical barriers • Cells phagocytes & macrophages natural killer cells • Complement • interferon Humoral Antibody- mediated Bacteria B-lymphocytes (antibodies) Antigen specific lymphocytes Cellular Cell-mediated Virus Antigen presenting cells T-lymphocytes
- Slides: 15