Physiology and Clinical Benefits of Kinetic Therapy and

Physiology and Clinical Benefits of Kinetic Therapy and Prone Positioning Frank Sebat, MS, MD SCCM 34 th Critical Care Congress 1 January 15 -19, 2005 · Phoenix, Arizona

Positional Therapy • Body movement and frequent posture changes are the norm • The supine position is uncommon and deleterious • Patients are nursed in the supine position Will frequent positional changes > 40° rotation and proning improve patient outcomes? 2

Immobility Is A Disease • Skin breakdown • Atelectasis • Pneumonia • Decreased gut motility • Vascular stasis 3

Standard of Practice for the Treatment of Immobility • Turning q 2 hours by nursing – Developed by Dr. Monroe in 1940’s to prevent skin breakdown – Little evidence regarding pulmonary complications – Compliance is difficult – Inconsistency to the degree of rotation 4

Mother Nature’s Answer to Positional Changing Minimal mobility requirement = 11. 6 minutes Minimum Physiologic Requirement, Studied and Published by Dr. Francis Keane who developed the first Roto. Rest 5

6

Kinetic Therapy Defined by the CDC to be Continuous Rotation > 40° 7
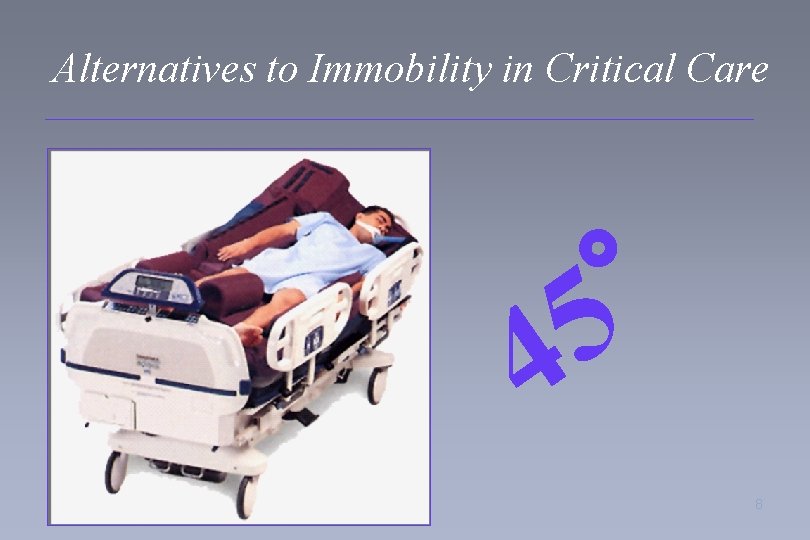
Alternatives to Immobility in Critical Care ° 5 4 8

62° Alternatives to Immobility in Critical Care 9

A Proning Bed With Kinetic Therapy ° 8 4 2 Alternatives to Immobility in Critical Care 10

A Proning Bed 11
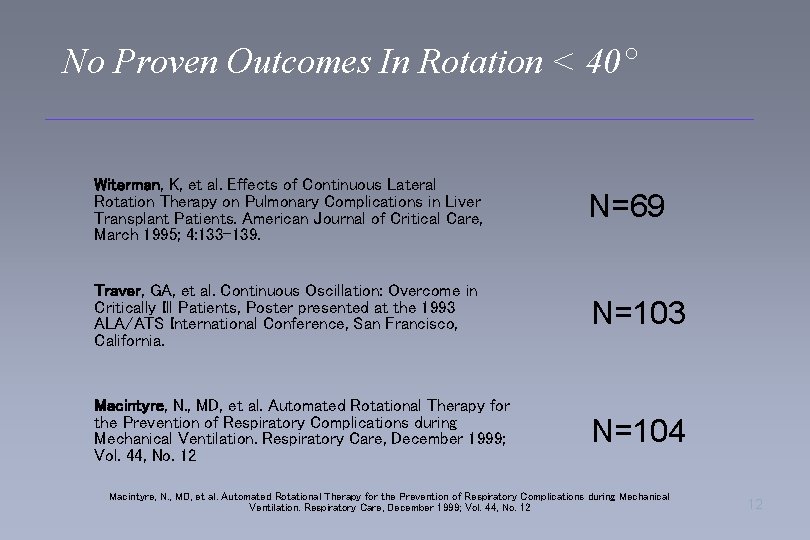

No Proven Outcomes In Rotation < 40° Witerman, K, et al. Effects of Continuous Lateral Rotation Therapy on Pulmonary Complications in Liver Transplant Patients. American Journal of Critical Care, March 1995; 4: 133 -139. N=69 Traver, GA, et al. Continuous Oscillation: Overcome in Critically Ill Patients, Poster presented at the 1993 ALA/ATS International Conference, San Francisco, California. N=103 Macintyre, N. , MD, et al. Automated Rotational Therapy for the Prevention of Respiratory Complications during Mechanical Ventilation. Respiratory Care, December 1999; Vol. 44, No. 12 N=104 Macintyre, N. , MD, et al. Automated Rotational Therapy for the Prevention of Respiratory Complications during Mechanical Ventilation. Respiratory Care, December 1999; Vol. 44, No. 12 12

Benefit of Rotation > 40° 45° Combined Kinetic Therapy and Percussion Therapy on the Resolution of Atelectasis on Critically Ill Patients. • Recruitment of Segmental lobar or whole-lung atelectasis with reduced need for bronoscopy. Raoof, Suhail, MD, FCCP; et al. . CHEST, 1999; 115; 1658 -1666. 40 -62° n=24 test-17 control-7 Kinetic Therapy in Critically Ill Patients; Combined Results Meta Analysis n= 419 • 24% reduction in ICU stay p <. 02 • 35% reduction in hours intubated p <. 04 • 50% reduction in ICU-acquired pneumonia p <. 002 Choi, SC: Nelson. LD. . Journal of Critical Care, March 1992. 13
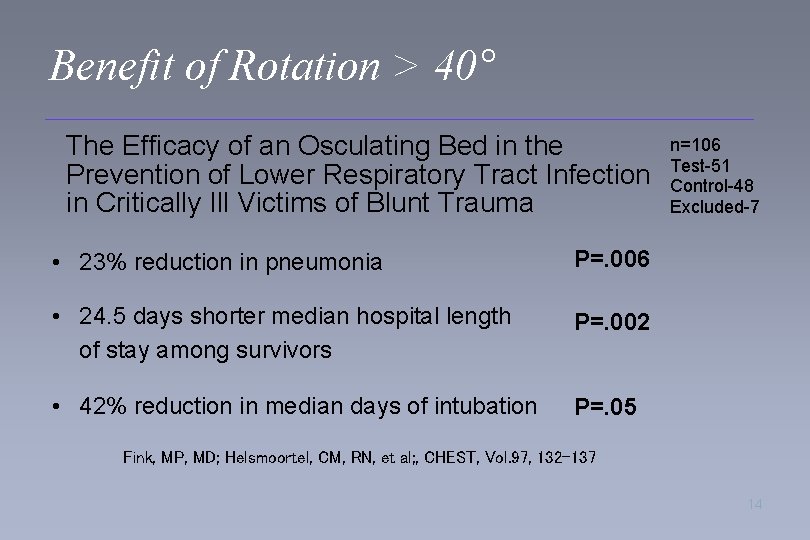
Benefit of Rotation > 40° The Efficacy of an Osculating Bed in the Prevention of Lower Respiratory Tract Infection in Critically Ill Victims of Blunt Trauma • 23% reduction in pneumonia P=. 006 • 24. 5 days shorter median hospital length of stay among survivors P=. 002 • 42% reduction in median days of intubation P=. 05 n=106 Test-51 Control-48 Excluded-7 Fink, MP, MD; Helsmoortel, CM, RN, et al; , CHEST, Vol. 97, 132 -137 14

Physiology of Positional Therapy • Pleural gradient – Triangular shape of lung with more mass posterior than anterior – Position of the diaphragm – Position of the heart 15

Physiology of Positional Therapy • Mobilization of secretions • V/Q matching • Restriction of anterior chest (proning) 16
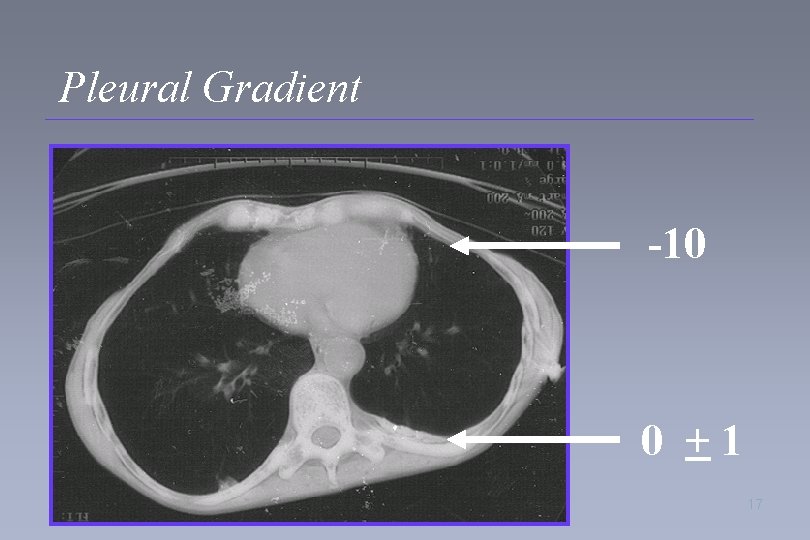
Pleural Gradient -10 0 +1 17
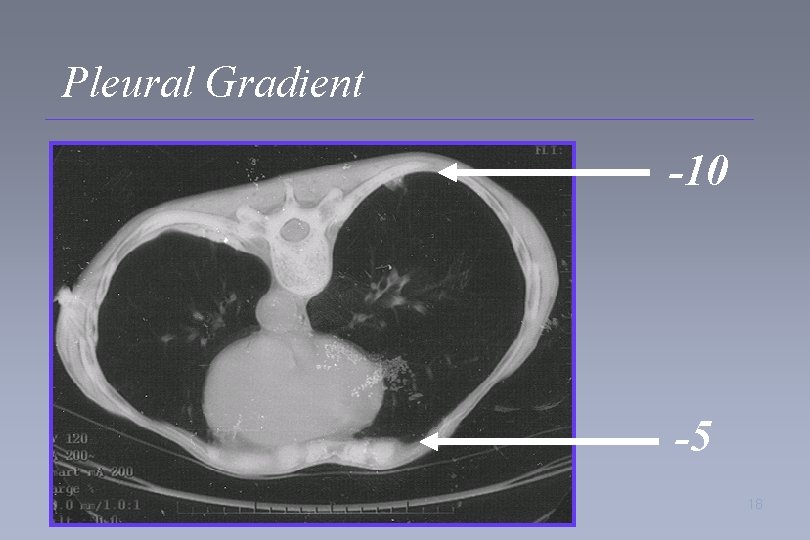
Pleural Gradient -10 -5 18
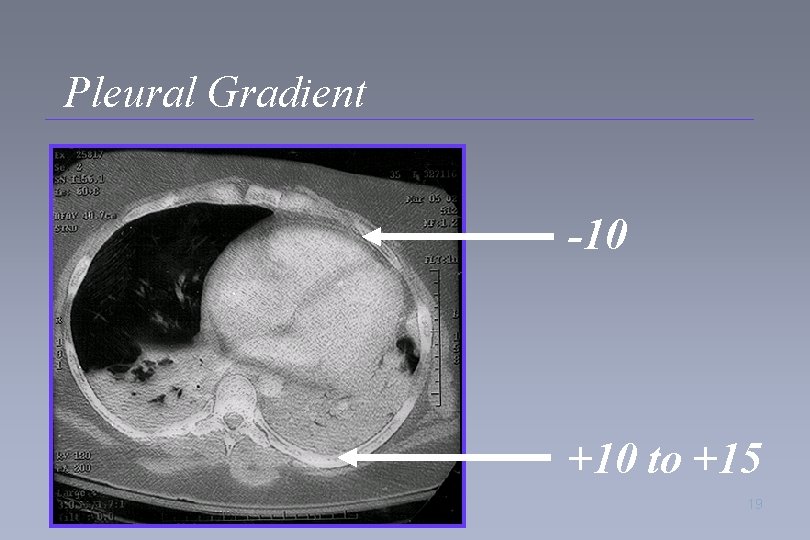
Pleural Gradient -10 +10 to +15 19
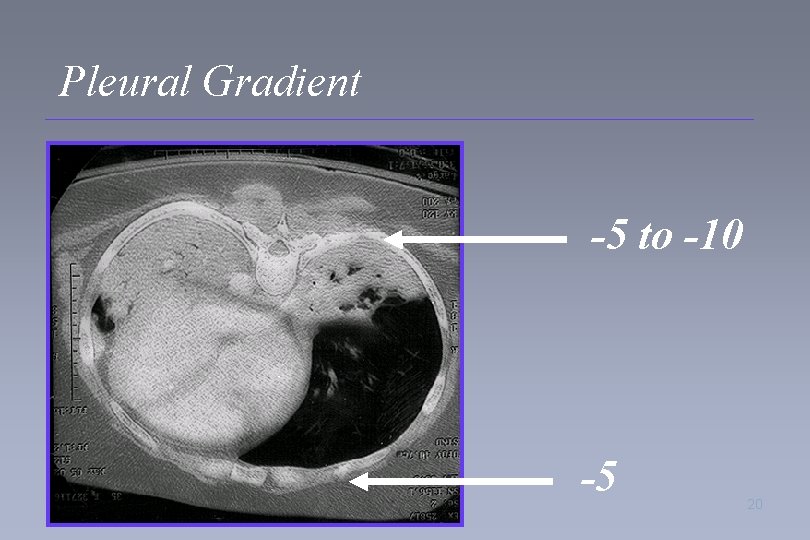
Pleural Gradient -5 to -10 -5 20

Redding California’s Introduction to Kinetic Therapy 1992 Dr. Johnson’s ARDS Patient on Roto. Rest 21

Redding California’s Experience with Kinetic Therapy 1992 -2004 • Apx. 1000 patients with ALI/ARDS treated with Roto. Rest with 62° rotation in the last 12 years – Increase need of sedation – Minimal to no hemodynamic instability – RNs request Roto. Rest prior to physicians – 14 Intensivists, 90 critical care beds in community all use Roto. Rest and now Roto. Prone for management of ALI/ARDS 22

Results of Proning Studies • A large number of small studies demonstrate: – Improved P/F ratio – Patient safety – Requires 4 -5 nurses and 1 physician – Often used as a rescue method when other methods fail – Convincing data lacking regarding morbidity and mortality 23
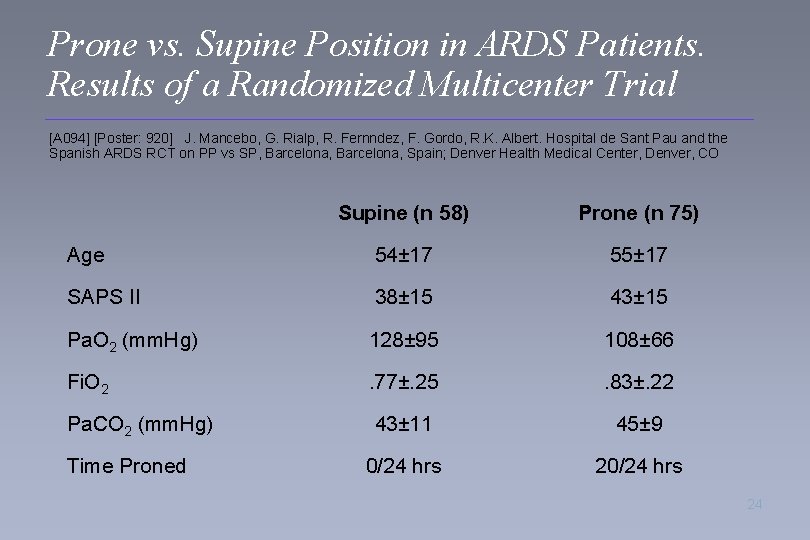
Prone vs. Supine Position in ARDS Patients. Results of a Randomized Multicenter Trial [A 094] [Poster: 920] J. Mancebo, G. Rialp, R. Fernndez, F. Gordo, R. K. Albert. Hospital de Sant Pau and the Spanish ARDS RCT on PP vs SP, Barcelona, Spain; Denver Health Medical Center, Denver, CO Supine (n 58) Prone (n 75) Age 54± 17 55± 17 SAPS II 38± 15 43± 15 Pa. O 2 (mm. Hg) 128± 95 108± 66 Fi. O 2 . 77±. 25 . 83±. 22 Pa. CO 2 (mm. Hg) 43± 11 45± 9 0/24 hrs 20/24 hrs Time Proned 24
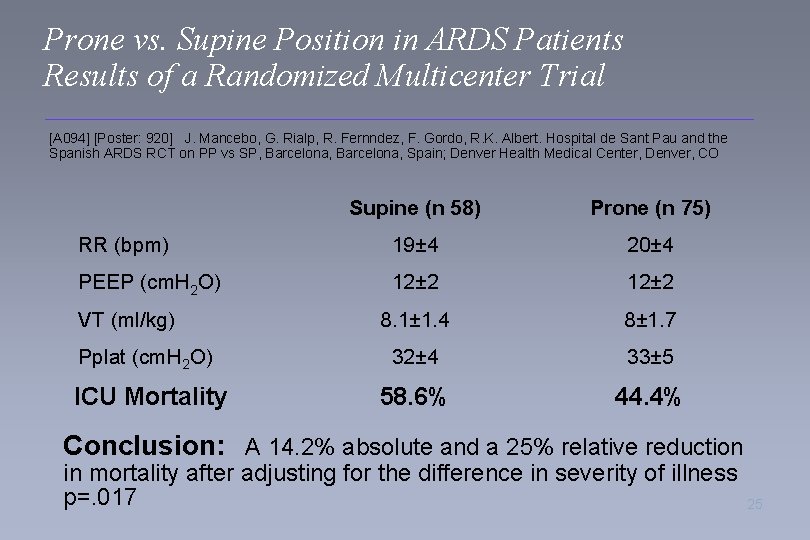
Prone vs. Supine Position in ARDS Patients Results of a Randomized Multicenter Trial [A 094] [Poster: 920] J. Mancebo, G. Rialp, R. Fernndez, F. Gordo, R. K. Albert. Hospital de Sant Pau and the Spanish ARDS RCT on PP vs SP, Barcelona, Spain; Denver Health Medical Center, Denver, CO Supine (n 58) Prone (n 75) RR (bpm) 19± 4 20± 4 PEEP (cm. H 2 O) 12± 2 8. 1± 1. 4 8± 1. 7 Pplat (cm. H 2 O) 32± 4 33± 5 ICU Mortality 58. 6% 44. 4% VT (ml/kg) Conclusion: A 14. 2% absolute and a 25% relative reduction in mortality after adjusting for the difference in severity of illness p=. 017 25

Proning Pilot Study The utility of an automated proning and kinetic therapy-unit with intermediate versus long proning time and its effect on lung recruitment and ventilator days in patients with acute lung injury (ALI) • 19 patients randomized: – 2 hr Sup/ 2 hr Pro……………. . … 12 hr prone – 45 min Sup/ 3 hr 15 min Pro………. 19. 5 hr prone • Purpose: – Feasibility – Safety – Segregation of responders 26
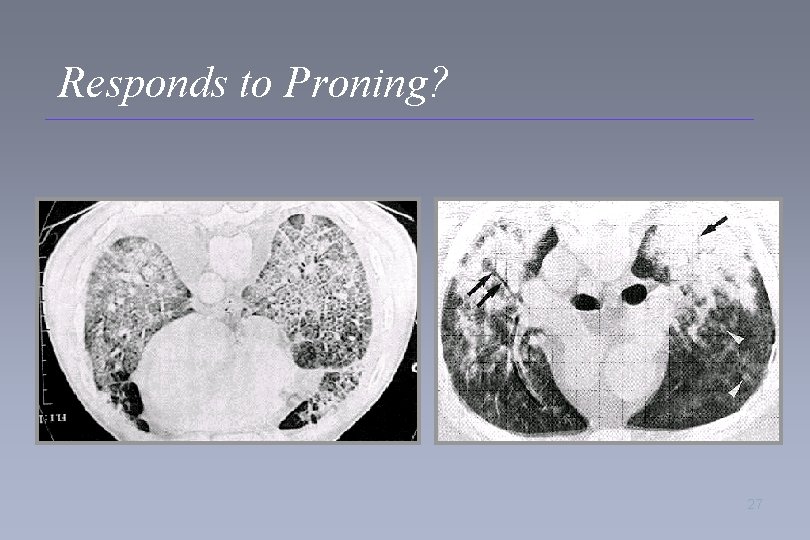
Responds to Proning? 27
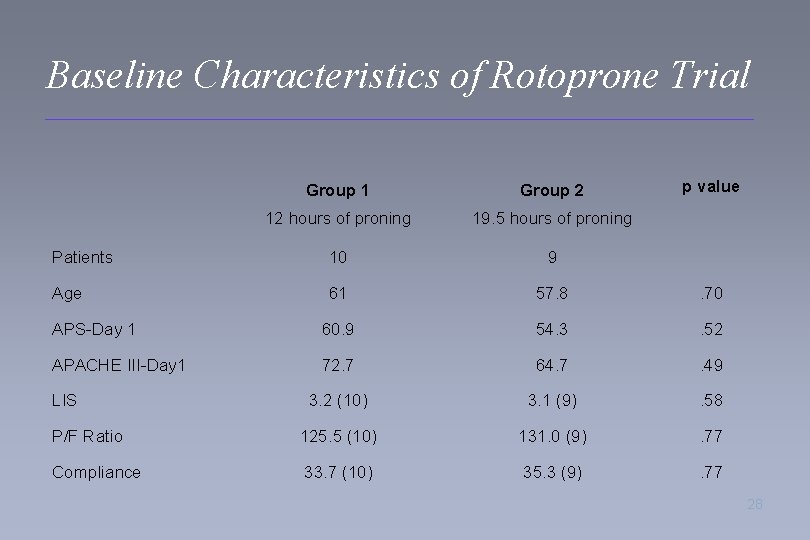
Baseline Characteristics of Rotoprone Trial p value Group 1 Group 2 12 hours of proning 19. 5 hours of proning Patients 10 9 Age 61 57. 8 . 70 APS-Day 1 60. 9 54. 3 . 52 APACHE III-Day 1 72. 7 64. 7 . 49 3. 2 (10) 3. 1 (9) . 58 P/F Ratio 125. 5 (10) 131. 0 (9) . 77 Compliance 33. 7 (10) 35. 3 (9) . 77 LIS 28
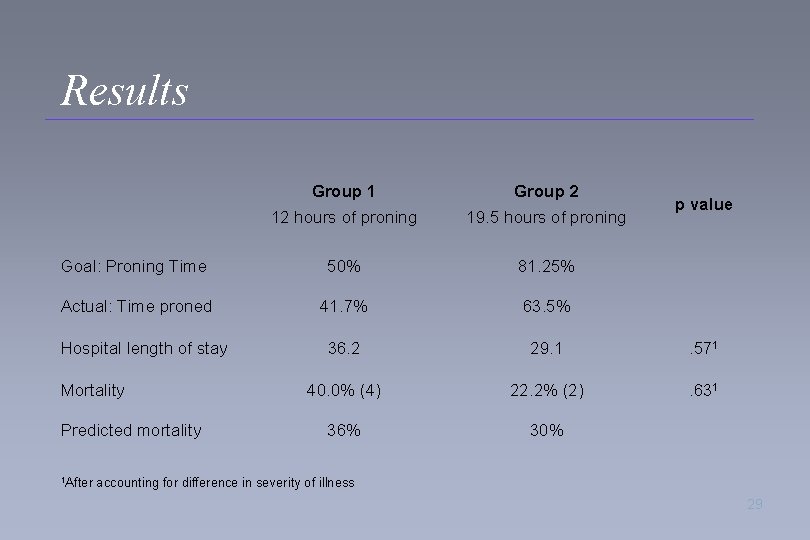
Results Group 1 Group 2 12 hours of proning 19. 5 hours of proning Goal: Proning Time 50% 81. 25% Actual: Time proned 41. 7% 63. 5% 36. 2 29. 1 . 571 40. 0% (4) 22. 2% (2) . 631 36% 30% Hospital length of stay Mortality Predicted mortality 1 After p value accounting for difference in severity of illness 29
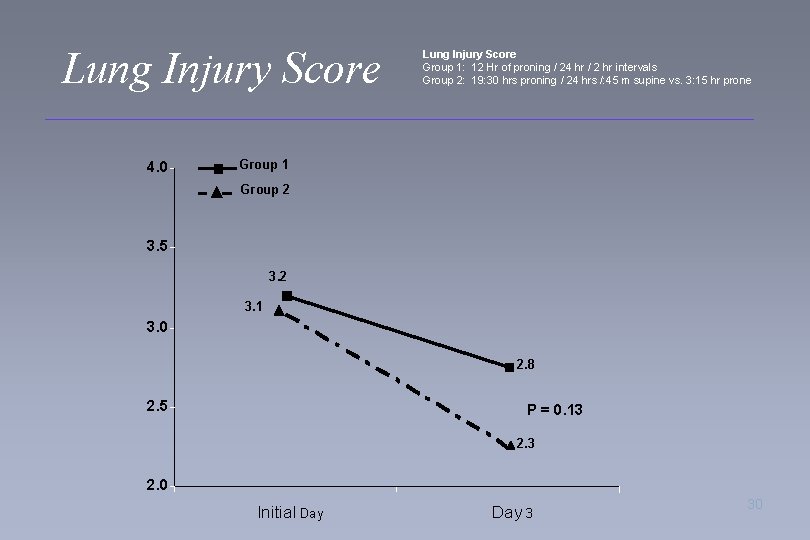
Lung Injury Score 4. 0 Lung Injury Score Group 1: 12 Hr of proning / 24 hr / 2 hr intervals Group 2: 19: 30 hrs proning / 24 hrs /: 45 m supine vs. 3: 15 hr prone Group 1 Group 2 3. 5 3. 2 3. 1 3. 0 2. 8 2. 5 P = 0. 13 2. 0 Initial Day 3 30
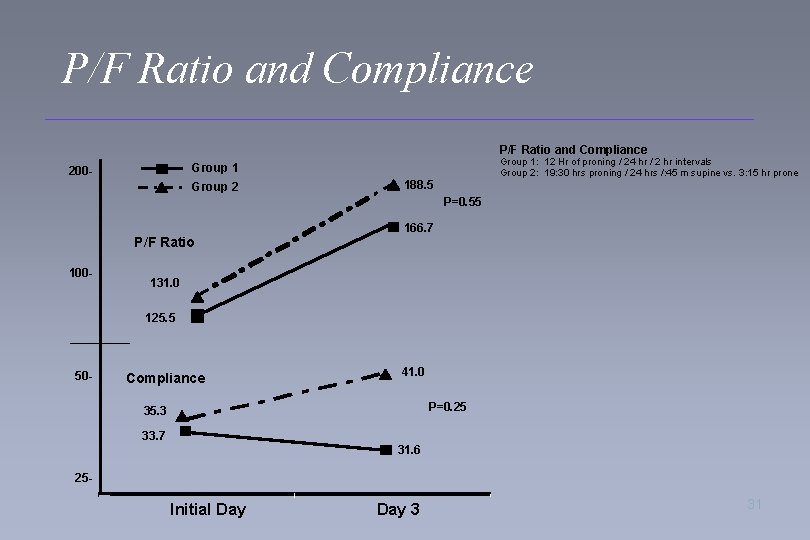
P/F Ratio and Compliance Group 1: 12 Hr of proning / 24 hr / 2 hr intervals Group 2: 19: 30 hrs proning / 24 hrs /: 45 m supine vs. 3: 15 hr prone Group 1 200 - Group 2 188. 5 P=0. 55 P/F Ratio 100 - 166. 7 131. 0 125. 5 50 - Compliance 41. 0 P=0. 25 35. 3 33. 7 31. 6 25 - Initial Day 3 31
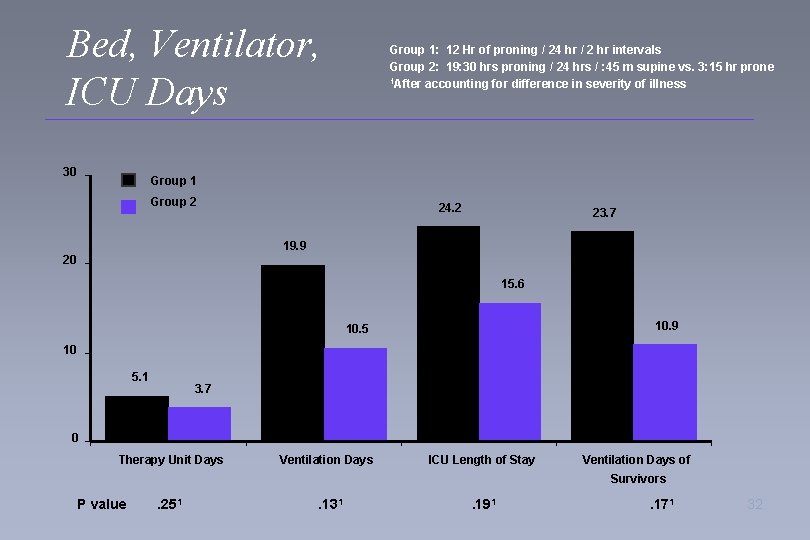
Bed, Ventilator, ICU Days 30 Group 1: 12 Hr of proning / 24 hr / 2 hr intervals Group 2: 19: 30 hrs proning / 24 hrs / : 45 m supine vs. 3: 15 hr prone 1 After accounting for difference in severity of illness Group 1 Group 2 24. 2 23. 7 19. 9 20 15. 6 10. 9 10. 5 10 5. 1 3. 7 0 Therapy Unit Days Ventilation Days ICU Length of Stay Ventilation Days of Survivors P value . 251 . 131 . 191 . 171 32
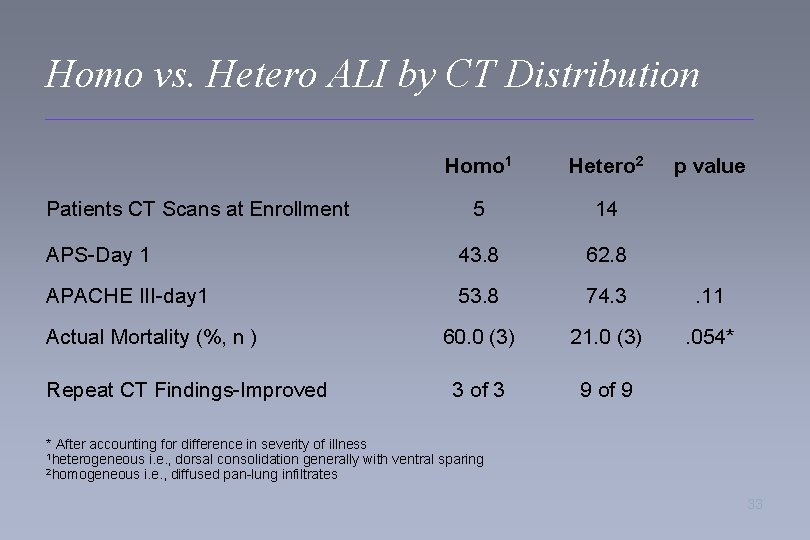
Homo vs. Hetero ALI by CT Distribution Homo 1 Hetero 2 5 14 APS-Day 1 43. 8 62. 8 APACHE III-day 1 53. 8 74. 3 . 11 60. 0 (3) 21. 0 (3) . 054* 3 of 3 9 of 9 Patients CT Scans at Enrollment Actual Mortality (%, n ) Repeat CT Findings-Improved p value * After accounting for difference in severity of illness 1 heterogeneous i. e. , dorsal consolidation generally with ventral sparing 2 homogeneous i. e. , diffused pan-lung infiltrates 33

Adverse Events • • • Facial edema 100% Right mid auxiliary line/chest skin breakdown (1 patient) Self Extubation (1 patient) Poorly functional groining CVVH catheter (1 patient) Scleral hemorrhage (2 patients) • No hemodynamic or respiratory instability requiring discontinuation of proning • Rapid mobilization of copious endotracheal secretions in patents with pneumonia 34
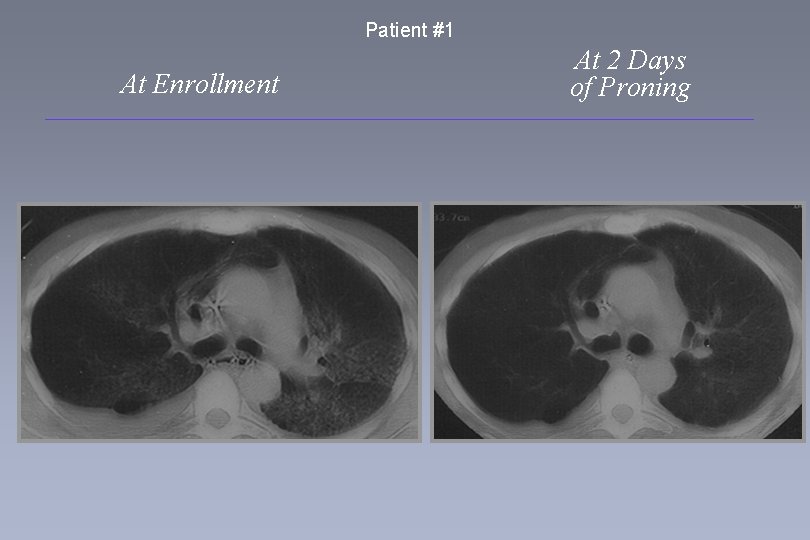
Patient #1 At Enrollment At 2 Days of Proning
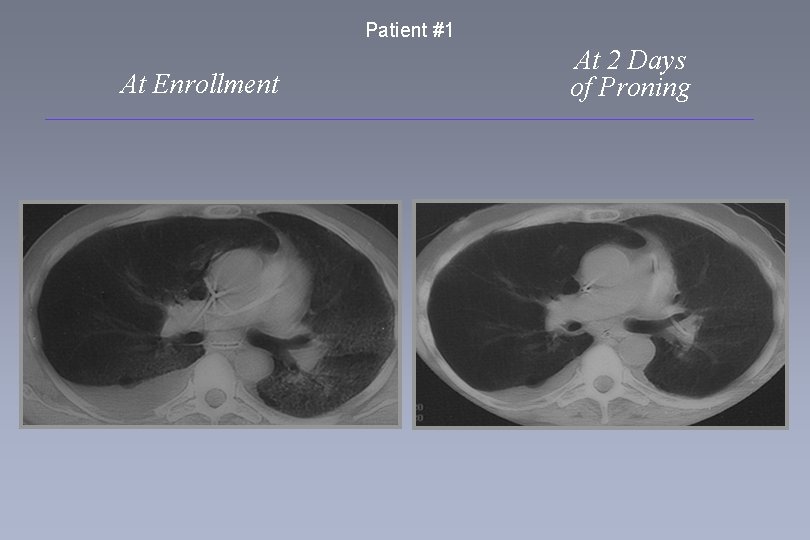
Patient #1 At Enrollment At 2 Days of Proning
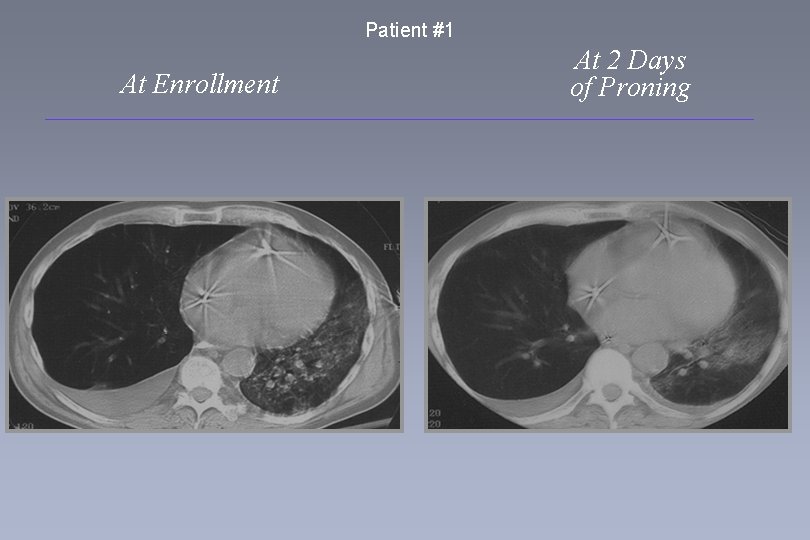
Patient #1 At Enrollment At 2 Days of Proning
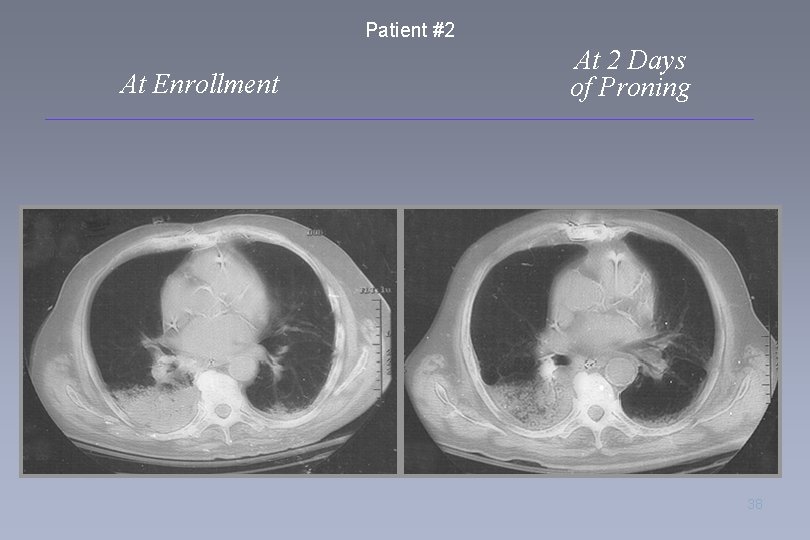
Patient #2 At Enrollment At 2 Days of Proning 38
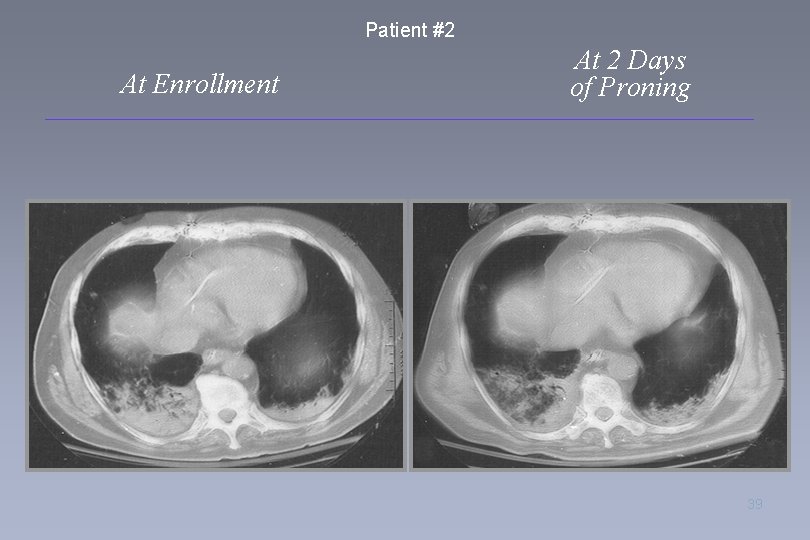
Patient #2 At Enrollment At 2 Days of Proning 39
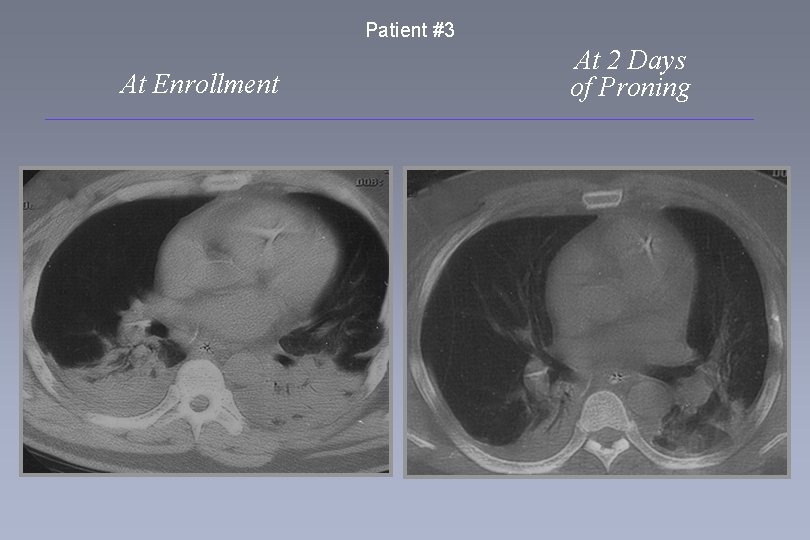
Patient #3 At Enrollment At 2 Days of Proning
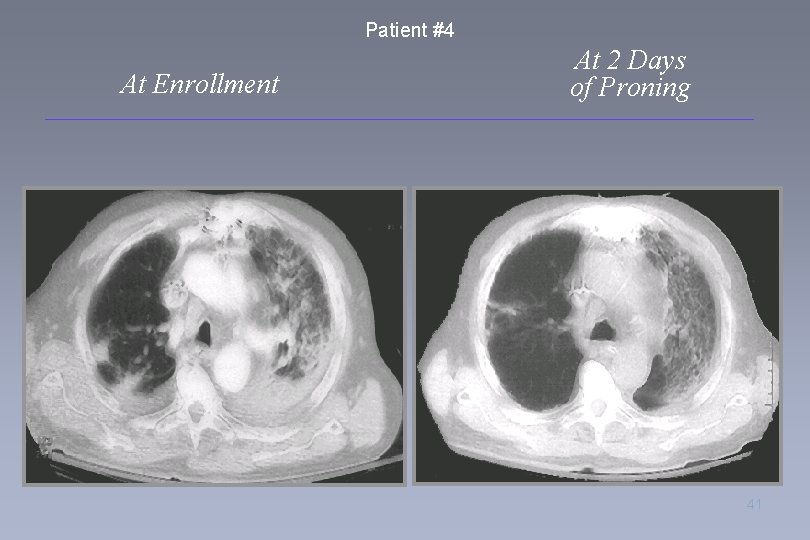
Patient #4 At Enrollment At 2 Days of Proning 41
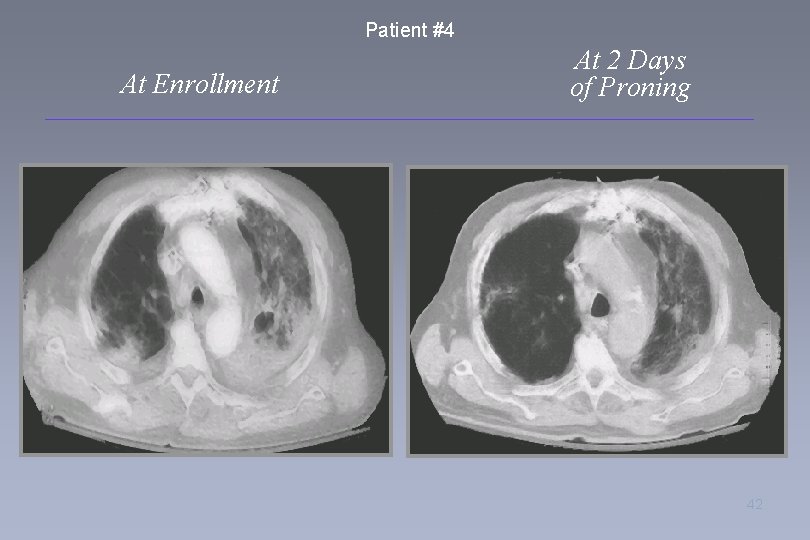
Patient #4 At Enrollment At 2 Days of Proning 42
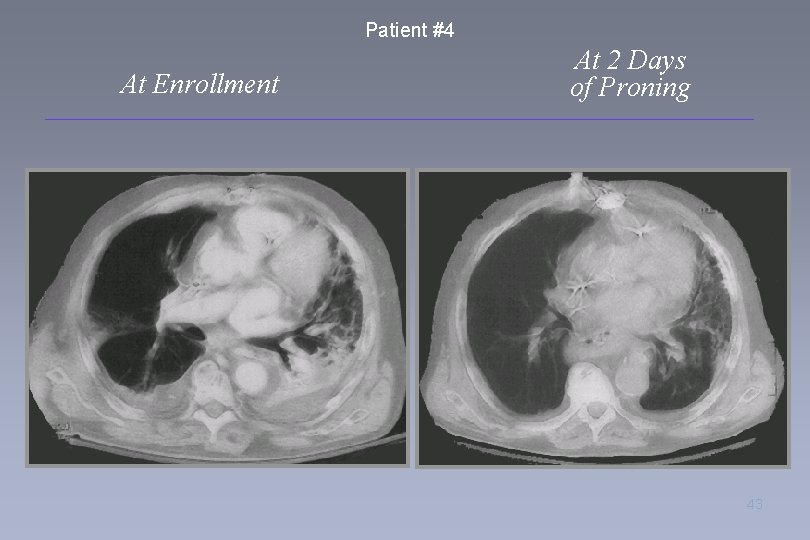
Patient #4 At Enrollment At 2 Days of Proning 43
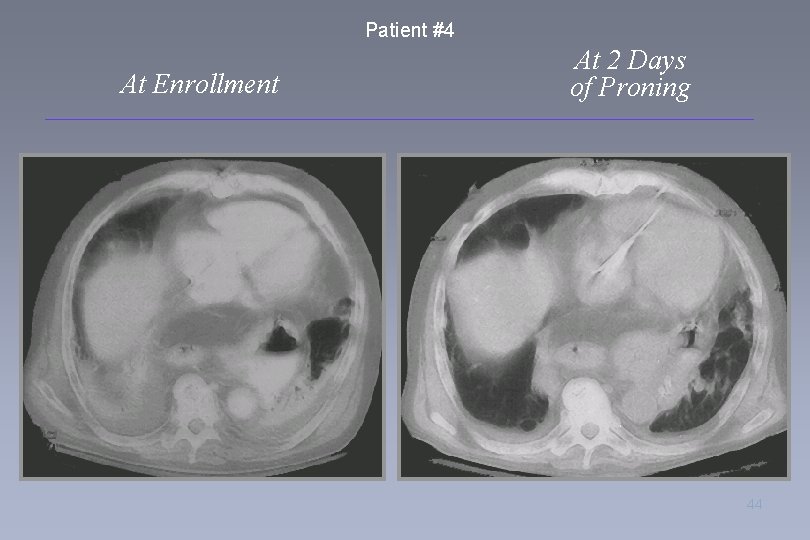
Patient #4 At Enrollment At 2 Days of Proning 44
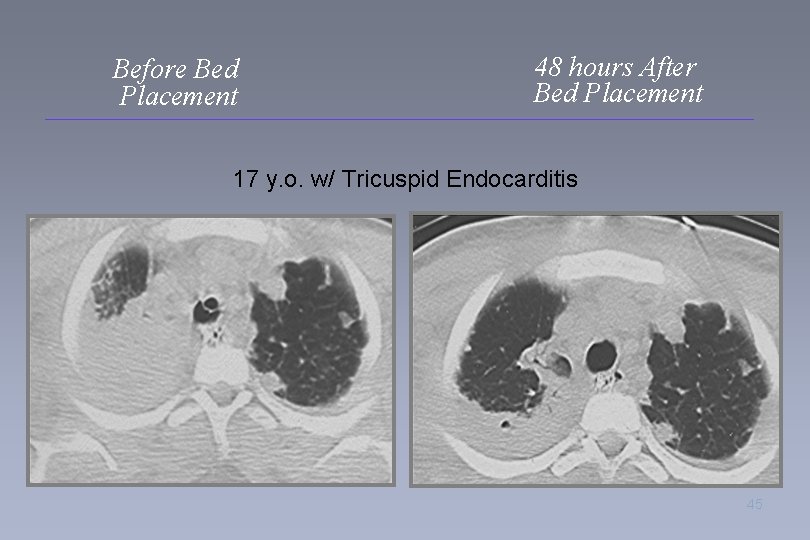
Before Bed Placement 48 hours After Bed Placement 17 y. o. w/ Tricuspid Endocarditis 45
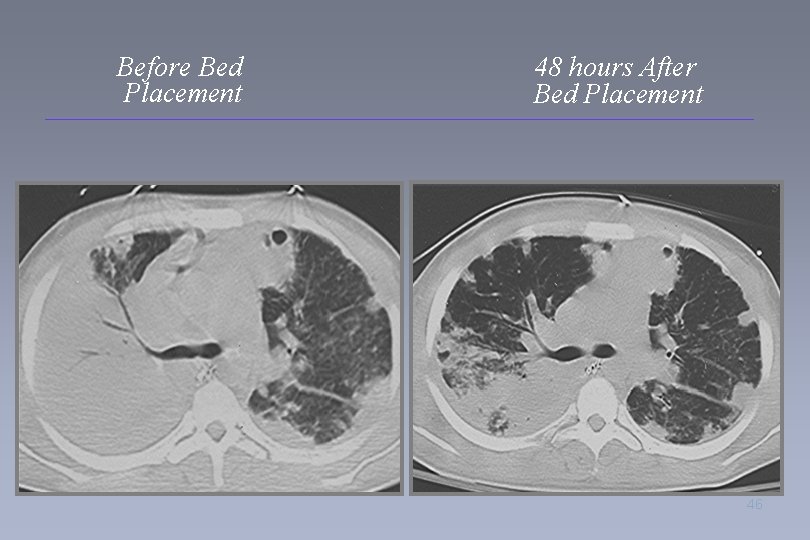
Before Bed Placement 48 hours After Bed Placement 46
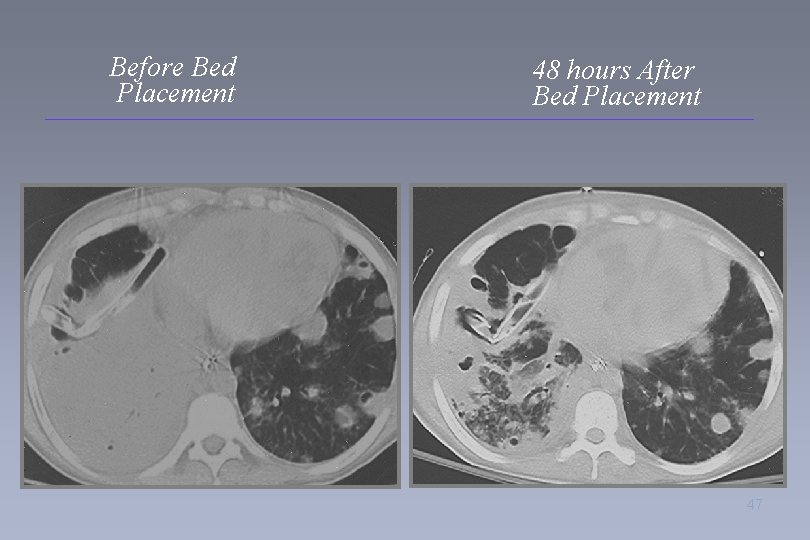
Before Bed Placement 48 hours After Bed Placement 47
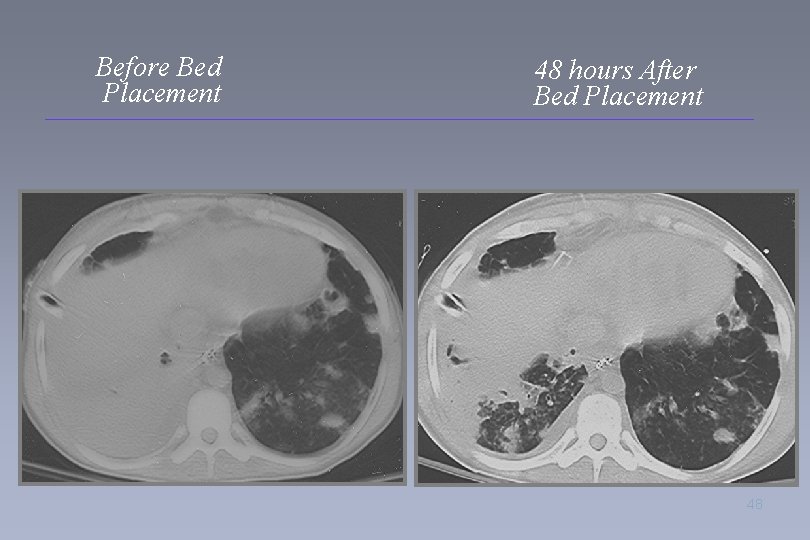
Before Bed Placement 48 hours After Bed Placement 48

Evaluation of Density Area in Dorsal Lung Region During Prone Position Using Transesophageal Echocardiography Tsubo T, Yatsu Y, Tanabe T, Okawa H, Ishihara H, Matsuki A University of Hirosaki School of Medicine, Hirosaki, Aomori-ken, Japan
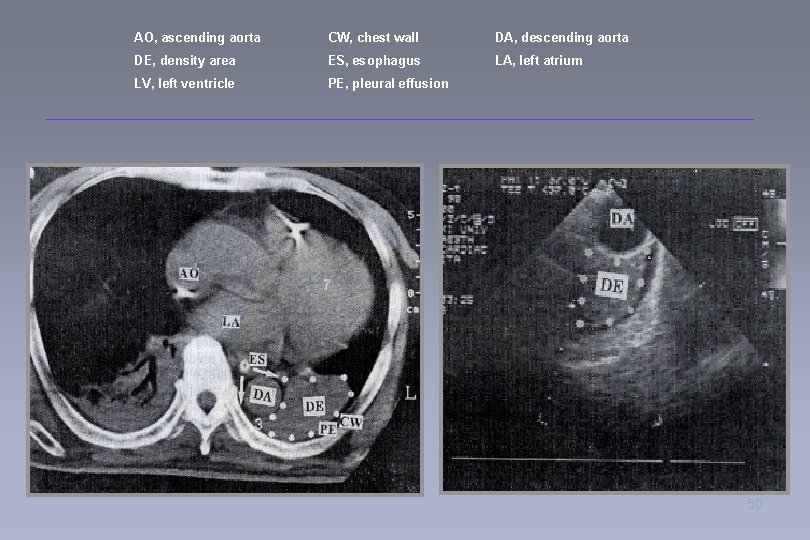
AO, ascending aorta CW, chest wall DA, descending aorta DE, density area ES, esophagus LA, left atrium LV, left ventricle PE, pleural effusion 50

Transesophageal Echocardiography Image During Prone Position 51
Conclusion: Kinetic Therapy with > 40° Rotation • Reduction in ventilator associated pneumonia and possibly hospital days • Reduction in atelectasis and need for bronchoscopy 52

Conclusion: Automated Proning • Restriction of anterior chest with possible reduction in VILI • Rapid mobilization of secretions • Improvement in oxygenation /Rapid recruitment of posterior consolidation • Accomplished with one nurse • 20 hrs proning per day well tolerated and trended toward better outcomes compared to 12 /24 hrs 53

Conclusion: Other Possible Benefits • Reduction of sinusitis • Reduced skin breakdown • Increased output from abdominal drains 54

- Slides: 55