Physician Wellbeing and the Physicians Health Program P

Physician Wellbeing and the Physicians Health Program P. Bradley Hall, MD Executive Medical Director, West Virginia Medical Professionals Health Program Immediate Past-President, Federation of State Physician Health Programs President, West Virginia Society of Addiction Medicine WVU School of Medicine – June 18, 2019 1

Conflict of Interest Disclosures §No relevant financial relationships with any commercial interests. §Physician Education Grant #G 180529 2

Physician Wellbeing and the PHP • Burnout, Wellness & Resilience • Potentially impairing conditions • Substance Abuse, Mental Illness & Co-morbidities • Barriers to detection and assistance • Indicators of potential impairment • Overview of Physician Health Programs • The MESSAGE objectives 3

• Airline Pilots Physicians 4

size depth of damage public trust *Fail first isn’t safe 5

Physician Wellbeing and the PHP • Burnout, Wellness & Resilience objectives 6

7

Health and Wellbeing Issues • Life / Work Balance • Satisfaction • Lack of joy / unhappiness • Stress • Distress • Burnout • Behavioral Health (interpersonal) • Mental Health • Physical Health • Substance Use / Addiction • Suicide * DIS-EASE of HUMAN-NESS 8
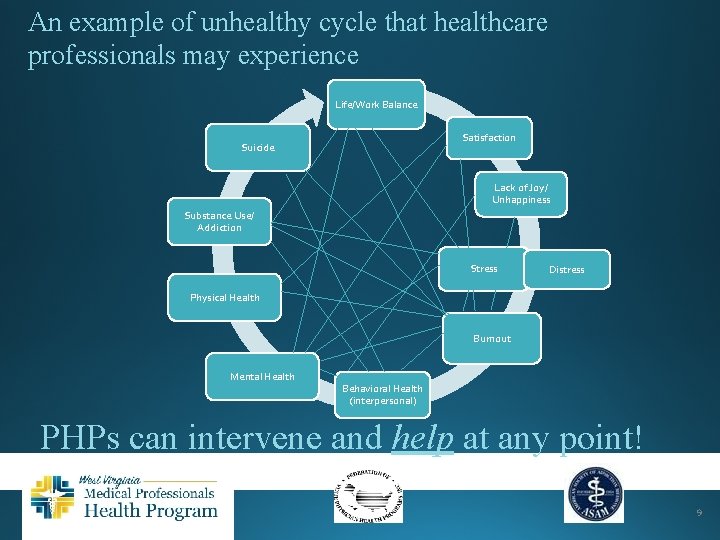
An example of unhealthy cycle that healthcare professionals may experience Life/Work Balance Satisfaction Suicide Lack of Joy/ Unhappiness Substance Use/ Addiction Stress Distress Physical Health Burnout Mental Health Behavioral Health (interpersonal) PHPs can intervene and help at any point! 9

Stigma 10

Physician Wellness “Wellness goes beyond merely the absence of distress and includes being challenged, thriving, and achieving success in various aspects of personal and professional life. ” Shanafelt TD, Sloan JA, Haberman TM. The well being of physicians. Am Med J 2003; 114: 513– 17. 11

Burnout • At least one symptom of burnout increased 2011 -2014 (45. 554. 4%) • Work / Life balance satisfaction declined 2011 -2014 (48. 540. 9%) • Burnout rates higher for all specialties in 2014 • Nearly a dozen specialties increased greater than 10% • More prevalent when compared to the general US working population even when adjusted for age, sex, hours and educational level 12

Burnout • • Burnout impacts the quality of care physicians provide and physician turnover. 13

Courtesy: Christine Sinsky, MD 14
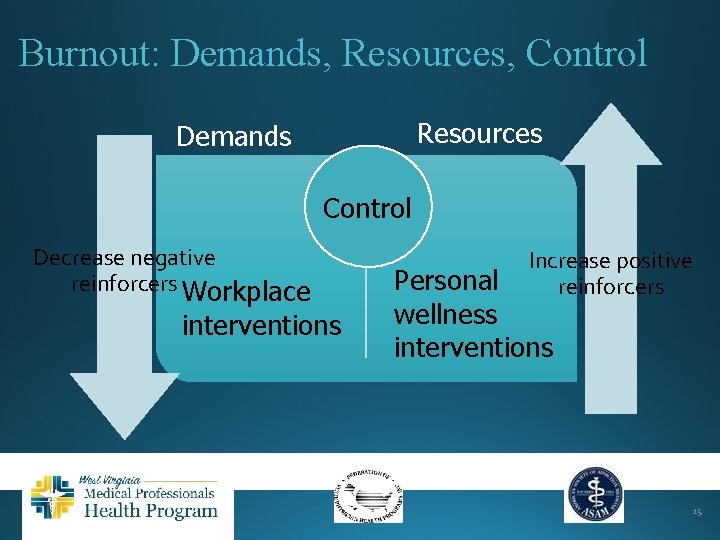
Burnout: Demands, Resources, Control Resources Demands Control Decrease negative reinforcers Workplace interventions Increase positive reinforcers Personal wellness interventions 15

Healthy Physicians Give Better Care! 16

Individual Drivers of Physician Burnout • Perfectionism • High achievement orientation • Difficulty setting boundaries • Intellectualization • Delay of gratification • Compartmentalization • Materialism 17

Environmental Drivers of Physician Burnout • Workload and time constraints • Inefficiencies/frustration (EHR) • Lack of autonomy/control • Ineffective leadership • Mission/values mismatch (loss of meaning) • Culture of incivility • Perception of fairness and respect • Diminished rewards 18

Building Wellness into the Practice Environment Professional Tension Workplace Wellness System Redesign Wellness The way out is to get “all in” 19

How Do You Prevent Burnout? • Accept shared responsibility for burnout • Elevate personal wellness to a core professional value, starting in medical school • Make wellness and satisfaction a quality outcome and incentivize it accordingly • Muster the will to address burnout generators and ask for help • Create opportunities for peer support and decrease isolation • Nurture the brain through meditation and application of mindful practice to clinical work 20

Individual Wellness: Key Targets • Awareness • Self-Care • Resilience • Engagement 21

Self-Awareness & Self-Monitoring • • 22

Self-Regulation & Resilience • Physically • Cognitively • Emotionally • Spiritually 23

Attending To Self • • 24

Resilience Bounce-Back 25

• http: //www. ama-assn. org/ama-wire/post/beat-burnout-7 -signsphysicians-should • http: //www. ama-assn. org/ama-wire/post/7 -steps-preventburnout-practice • http: //www. ama-assn. org/ama-wire/post/burnout-busters-boostsatisfaction-personal-life-practice • https: //www. stepsforward. org/modules? sort=recent&category=well being • https: //www. stepsforward. org/ • http: //www. ama-assn. org/ama/pub/physician-resources/physicianhealth/international-conference-physician-health. page 26

Physician Wellbeing and the PHP • Burnout, Wellness & Resilience • Potentially impairing conditions • Substance Abuse, Mental Illness & Co-morbidities objectives 27

West Virginia Today EPICENTER 28

Education is the Key • • 29

Children / Parents College Medical Students ALL HEALTH CARE PROVIDERS Residents Practicing Physicians Patients 30

TODAY Alcohol Use 2017 NSDUH 31

Alcohol-Impaired Driving Among Adults — United States, 2012 • Alcohol-impaired driving crashes account for approximately one third of all crash fatalities in the United States (1). • In 2013, 10, 076 persons died in crashes in which at least one driver had a blood alcohol concentration (BAC) ≥ 0. 08 grams per deciliter (g/d. L) MMWR - August 7, 2015 / 64(30); 814 -817 32

• Regrettable social behaviors were reported by 66. 1% of participants, suggesting that they may occur at a much higher rate than more serious drinking-related consequences (e. g. drinking and driving, violence, etc. ) Eugene M. Dunne; Elizabeth C. Katz Alcohol. 2015; 50(4): 393 -398. 33

2017 NSDUH 34

2017 NSDUH Report Illicit <30 days 30. 5 Million Adults (11. 2%) =1 in 9 Americans!! • Marijuana – 26 million (9. 6%) • Prescription Drugs – 6 million (2. 2%) • Prescription Pain Relievers – 3. 2 million (1. 2%) • Cocaine – 2. 2 million (0. 8%) • Hallucinogens – 1. 4 million (0. 5%) • Inhalants - 0. 6 million (0. 2%) • Methamphetamines – 0. 8 million (0. 3%) • Heroin - 0. 5 million (0. 2 %) 35

Substance Use Disorders § 19. 7 million (7. 2%) age 12 or older had an SUD § 13. 6 million (6. 4%) age 26 or older had an SUD § 5. 1 million (14. 8%) age 18 -25 had an SUD § 992 thousand (4%) age 12 -17 had an SUD In other words… 1 in 25 adolescents, 1 in 7 young adults & 1 in 16 adults age 26 or older ……. had an SUD in the past year 2017 NSDUH 36

Mental Illness • 46. 6 million (18. 9%) age 18 or older had AMI • 11. 2 million (4. 5%) age 18 or older had SMI • 3. 2 million (13. 3%) adolescents had MDE • 2. 3 million (9. 4%) 12 -17 with MDE with severe impairment 2017 NSDUH 37
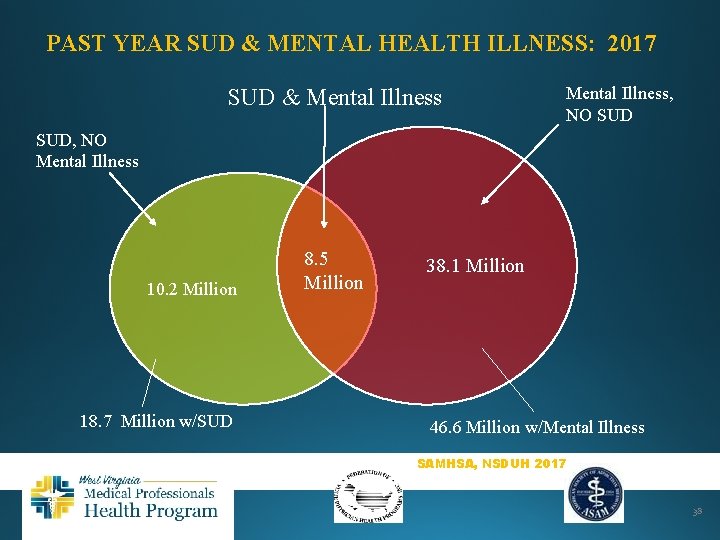
PAST YEAR SUD & MENTAL HEALTH ILLNESS: 2017 SUD & Mental Illness, NO SUD, NO Mental Illness 10. 2 Million 18. 7 Million w/SUD 8. 5 Million 38. 1 Million 46. 6 Million w/Mental Illness SAMHSA, NSDUH 2017 38

2017 NSDUH Report 39

RECOGNITION: ? ? ? 40

• Most chemically dependent physicians are untreated or unrecognized and are still practicing medicine. 41

• FSPHP Public Policy on Illness vs. Impairment Physician illness and impairment exists on a continuum with illness typically predating impairment, often by many years. • Illness is the existence of a disease • Impairment is a functional classification implying the inability of the person affected by disease to perform specific activities www. fsphp. org 42

Addiction & Mental Illness are NON-DISCRIMINATORY & POTENTIALLY IMPAIRING 43

Impairment: 44

American Medical Association definition - • • • excessive use or abuse of drugs, including alcohol 45

Historical Perspective v 1953 – FSMB calls for model physician assistance programs v 1973 – “The Sick Physician: Impairment by Psychiatric Disorders, Including Alcoholism and Drug Dependence” by AMA Council on Mental Health v 1980 – almost all state medical societies had authorized or implemented a state PHP and PHPs were communicating. v 1990 – Several state Physician Health Program’s organized the Federation of State Physician Health Programs v 1995 – FSMB published guidelines for a model Physician Health Program v 2004 – Federation of State Physician Health Programs (FSPHP) Guidelines v 2011 – American Society of Addiction Medicine 11 Policies on Physician Health v 2012 - FSMB updated the guidelines for a model Physician Health Program v 2016 – AMA Model Physician Health Program Act (1985 policy revision) v 2017 – ACGME – Symposium #3 on Physician Wellbeing v 2017 – National Academy of Medicine v 2019 – FSPHP updated Guidelines 46


The DISEASE OF ADDICTION AND IT’S PROGRESSION 48

Progressive, Incurable, and Fatal Disease: a Chronic, Relapsing Medical Condition üProgressive - Illness rarely gets better without intervention / treatment. üIncurable - Chronic condition. No such thing as a “cure”. There are no ex-addicts or ex-alcoholics. üFatal - Overdose, car accident, suicide, liver disease, heart disease, homicide èDefinition of Addiction: Continuing behavior despite suffering negative consequences as a result of that behavior. www. asam. org = definition of addiction 49

Four “C’s” of Addiction • C • C • • C C 50

Symptoms of Substance Use Disorders (SUD)

Symptoms of Substance Use Disorders (DSM-5)

Diagnosing SUD in DSM-5
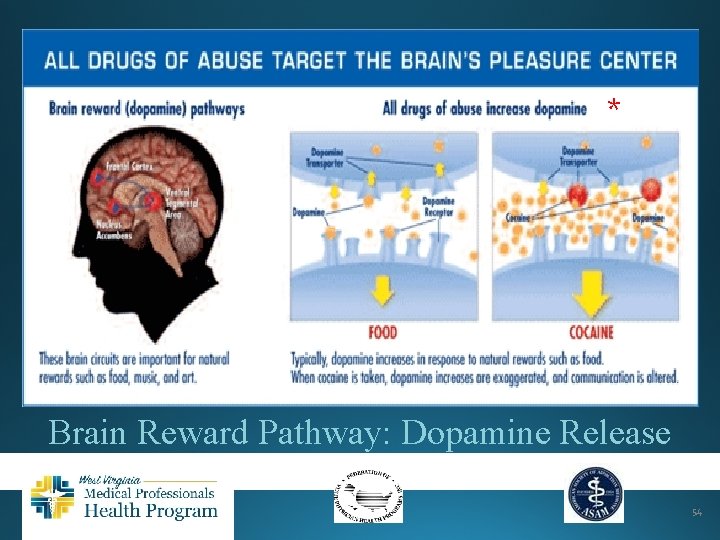
* Brain Reward Pathway: Dopamine Release 54

What Happens when Intoxicants are used? § § dopamine § 55

Addiction Progression Ø Ø Ø 56

D E N I A L 57

If you are wondering if you have a problem, that is a BIG RED FLAG. Social users don’t wonder if they have a problem, they know they do not. If you are still wondering you might want to cut down on whatever you are doing. If you are unable to cut down …… call the WVMPHP. YOU 58

AAFP This Week (vol. 4, #36, 9/9/03) n “Patients with drug or alcohol dependence or abuse problems will be hard to detect unless the physicians ask them about their use – 94% of the 22 Million people with these problems fail to recognize these problems in themselves 59

Initially, a person takes a DRUG hoping to CHANGE their MOOD, PERCEPTION, or EMOTIONAL STATE. Translation…. . HOPING TO CHANGE THEIR BRAIN 60

Report of the Council of Mental Health of the American Medical Association (1972) • take cognizance ethical responsibility to 61

Disorders of Impairment • • Alcohol Use Disorders Drug Use Disorder Psychiatric Disorders Disruptive Disorders Psychosexual Disorders Metabolic Disorders Physical Disorders 62

CAGE Cut down Anger Guilt Eye Opener +2 = 60 -90% sensitive 63

The Addicted Physician n n Typically, the hospital/ practice is the last place addiction manifests symptoms Physicians hold the workplace sacred Disruptions in family, personal health, community, social, spiritual and leisure life can all occur while the workplace remains relatively unaffected Even very small intrusions of addiction into the workplace should be taken extremely seriously in physicians 64

The *Psychology of the Physician • • • *Adapted from Myers and Gabbard: The Physician as Patient, 2008 65

Medical Specialty and Addiction • There is no specialty that "protects" a physician from a substance use disorder • • • 66

Medical Specialty and Addiction • These barriers are the products of a lack of education concerning the true nature of addiction as a primary biogenetic and psychosocial disease. • denial • Knowledge • sick • 67

Subtlety • • Even very small intrusions of addiction into the workplace should be taken extremely seriously in physicians • Tip of the Iceberg 68

Coronary Artery Disease • Hypertension • Diabetes • Hyperlipidemia • Exercise • Smoking • Diet Addiction • • • Co-Morbidities 69
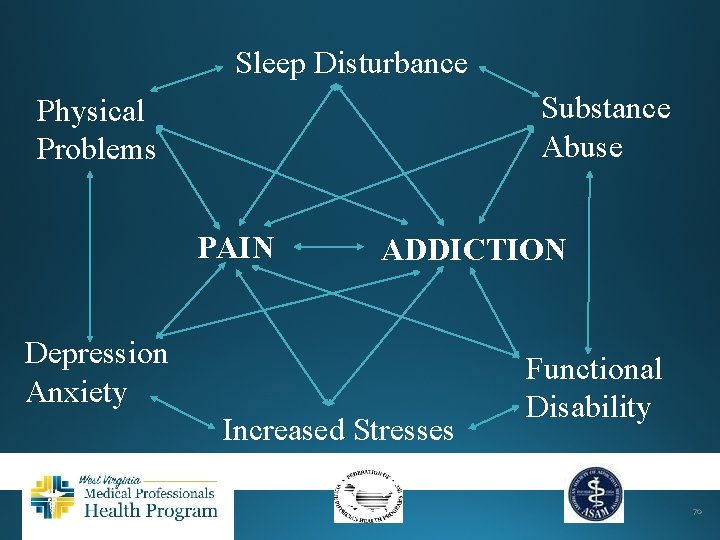
Sleep Disturbance Substance Abuse Physical Problems PAIN ADDICTION Depression Anxiety Increased Stresses Functional Disability 70

SIMILARITIES OPIOIDS NICOTINE • HIGHLY ADDICTIVE • VULERABLE POPULATIONS • PROFITABLE INTERESTS • SHIFT NECESSARY TO FIX • HIGHLY ADDICTIVE • VULNERABLE POPULATIONS • PROFITABLE INTERESTS • SHIFT NECESSARY TO FIX DIFFERENCES • NEW • ACCELERATING DIFFERENCES • OLD • DECREASING 71

Addiction is the Problem • Prescription Opioids • Heroin • Amphetamines • Inhalants • Cocaine • Benzodiazepines • Marijuana 72

Addiction • It is about any and all drug use by youth 73

Addiction is the Problem • • • Mood Altering Substances Work Television Shopping Gaming Internet *HOLE i. Phone Facebook Gambling Food Sex Our own opinion, thoughts, feelings & beliefs 74

Suicide • • • *1 in 3 adults who had serious thoughts of suicide made suicide plans and about 1 in 8 adults who had serious thoughts of suicide made a suicide attempt. (2017 NSDUH) • 75

Suicide 400 physicians 76

Suicide Risk Factors • • mental • alcohol • • • Barriers to accessing mental health and/or addiction treatment • 77

Suicide Protective Factors • Effective clinical care for mental, physical, and substance abuse disorders • Easy access to a variety of clinical interventions and support for help seeking • Family and community support • Support from ongoing medical and mental health care relationships • Skills in problem solving, conflict resolution, and nonviolent handling of disputes • Cultural and religious beliefs that discourage suicide and support self-preservation instincts PHP = Mitigatory 78

Physicians Contemplating Suicide § Findings: Multiple stressors, even absent a mental illness, creates an independent risk factor for suicide. Brooks et al, When Doctors Struggle Current Stressors and Evaluation Recommendations for Physician Contemplating Suicide, Archives of Suicide Research, DOI, Jan 2018 79

Physician Wellbeing and the PHP • Burnout, Wellness & Resilience • Potentially impairing conditions • Substance Abuse, Mental Illness & Co-morbidities • Barriers to detection and assistance objectives 80

WHOSE DOMAIN ? 81

Physician Health Programs From Thru To PREPARED POTENTIALLY IMPAIRED REPAIRED 82

CONFIDENTIAL 83

BARRIERS REPORTING THE DEADLY SILENCE 84

§ Insight § 85
DEADLY • • • 86

DENIAL • • *Most Treatment programs easily address this issue – if ABLE TO PROVIDE ADEQUATE PEER GROUP AVAILABILITY 87

MD DO M D D O 88

FEAR – ILL Physician

FEAR - OBSERVER

FEAR - OBSERVER

FEAR - OBSERVER

FEAR - OBSERVER

F E A R 94

If you are wondering if you have a problem, that is a BIG RED FLAG. Social users don’t wonder if they have a problem, they know they do not. If you are still wondering you might want to cut down on whatever you are doing. If you are unable to cut down …… call the WVMPHP. YOU 95

Physician Wellbeing and the PHP • Burnout, Wellness & Resilience • Potentially impairing conditions • Substance Abuse, Mental Illness & Co-morbidities • Barriers to detection and assistance • Indicators of potential impairment objectives 96

THE SIX “I” S 97

NON-DISCRIMINATORY & POTENTIALLY IMPAIRING 98

BEHAVIORIAL INDICATORS OF IMPAIRMENT • I • I • I Wvmphp. org 99

IRRITABILITY

IRRITABILITY Verbal Altercations with • PATIENTS • STAFF • PEERS • Other Disruptive Behaviors • “PERSONALITY CHANGE” especially after bathroom break

IRRESPONSIBILITY Shifts Work Load • Manipulates Schedule • E R • ON-CALL • “HURRY UP-CATCH UP” • Hasty Rounds • Short Cuts

INACCESSIBILITY Frequent Tardiness • Frequent Absence • “MIA”-MISSING IN ACTION • Frequent Trips to Bathroom • Frequent Trips to Parking Lot • Prolonged Lunch Breaks • UNAVAILABLE When On-Call • UNAVAILABLE For Discussions

INACCESSIBILITY

INACCESSIBILITY

INABILITY

INABILITY

INABILITY

ISOLATION

INCIDENTALS
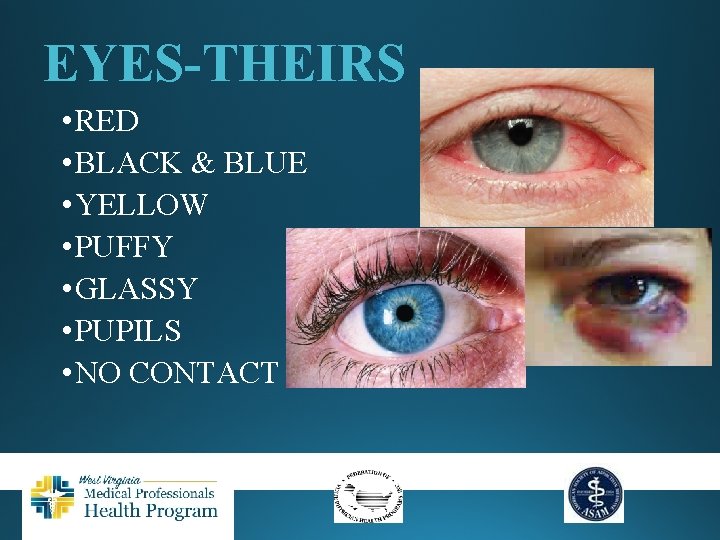
EYES-THEIRS • RED • BLACK & BLUE • YELLOW • PUFFY • GLASSY • PUPILS • NO CONTACT

EYES-YOURS

EARS • Raspy Voice • Gargling in Bathroom • Complaints from • STAFF • PATIENTS • PEERS • Phone Speech • SLURRED • INCOHERENT

EARS

NOSE-THEIRS

NOSE-YOURS

OTHER

MYTHS MUST WANT HELP • MUST HIT BOTTOM 118

Ø“ 30% of Physicians Ø higher 119

120

AMA Physicians Health Program Act (WVSMA Resolution 2017) • Legislation • Therapeutic Alternative to Discipline • Confidentiality Extended • Dual Purpose – public safety/rehabilitation • Early Detection • Mitigate Barriers • Discrimination • Adequate Funding • PHP Model Endorsement • Principles of Accountability, Communication, Collaboration & Transparency 121

Prevention Ø ** Ø Ø **Cultural shift through education 122

QUIETLY INQUIRE TO SUBSTANTIATE AUTHENTICITY 123

ARRANGE AN INTERVENTION WITH WVMPHP GUIDANCE GOAL EVALUATION 124

The initial discussion with the individual in an effort to educate them and thereby encourage participation in a formal chemical/alcohol dependency/psychiatric evaluation by qualified experts. 125

Why Doctors use Drugs • Access to pharmaceuticals (availability) • Family history of substance abuse (genetics) • Personality factors (e. g. , grandiosity, guilt) • Stress at home and/or at work • Thrill-seeking • Self-treatment of pain, sleep patterns, emotional disorders • Chronic fatigue • Social/economic status 126

Self-Medication 127

As SUD Progresses • Last effected by the illness is the practice setting. • Rapid with cocaine and slower with alcohol. 128

INTOXICATION in a Medical Professional in purely social settings should be IGNORED since it DOES NOT OCCUR DURING NORMAL WORKING HOURS ? ? ? 129

On the JOB A O B (Alcohol On Breath) is almost always an ominous sign, even when noted on a single occasion? ? ? 130

While several SIGNS of IMPAIRMENT, or a CLUSTER of them, usually suggest TROUBLE, a pattern of aberrant behavior is almost always indicative of POTENTIAL or ACTUAL IMPAIRMENT.

case afterward following his 132

Physician Wellbeing and the PHP • Burnout, Wellness & Resilience • Potentially impairing conditions • Substance Abuse, Mental Illness & Co-morbidities • Barriers to detection and assistance • Indicators of potential impairment • Overview of Physician Health Programs objectives 133

Overview Physician Health Programs (PHPs) 134

135

What is a Physicians Health Program 136

a “Provider of treatment” a place of refuge simple or easy tolerant of unwillingness, dishonesty or denial the decision maker of diagnoses or impairment 137

PHPs are a model for confidential chronic disease management through enhancing early detection, intervention, evaluation, treatment and monitoring for healthcare professionals with potential impairing conditions longitudinally over time. 138

What next? • • • 139
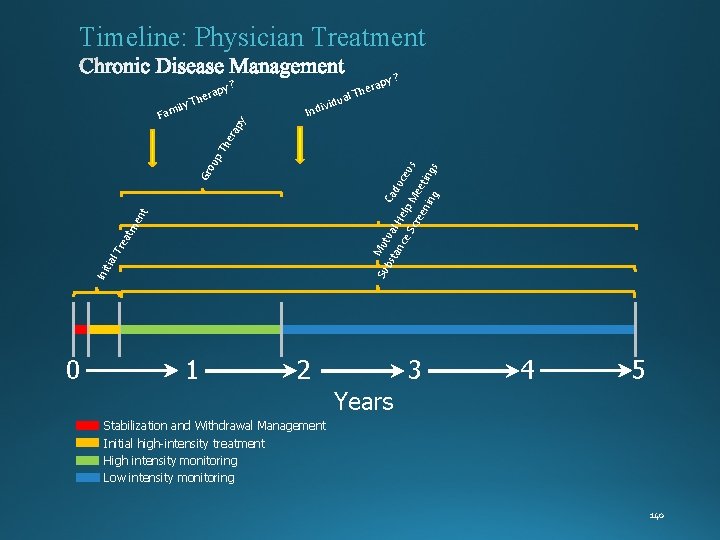
Timeline: Physician Treatment y? rap e y Th v Indi idua y? Ini tia l. T rea tm en t Su Mut bs tan ual H Cadu e c ce Sc lp M eus ree ee nin ting g s Gr ou p. T he rap y il Fam erap h T l 0 1 2 3 4 5 Years Stabilization and Withdrawal Management Initial high-intensity treatment High intensity monitoring Low intensity monitoring 140

PHP and Board Balance PHP Licensing Board Confidentiality Public protection Illness Impairment Treatment Sanctions 141
RELATIONSHIPS PHP Model Collaboration Communication Accountability Transparency Licensure Board (alternative) PARTICIPANT Participant (Patient) 142

Relationships 1 – Listen to understand, not to reply. This allows understanding of others’ perspective and open mindedness to new knowledge. 2 – The most dangerous opinion is the highest opinion we hold of our own opinion. This is particularly true to that which we are sure about. 143

same care and respect they give their own patients 144

145

PROBLEM • Chemical Dependency • Mental Illness • Dual Diagnosis • Stress Disorder • Disruptive Behavior • Psychosexual Disorder • Incompetent/Dated • Unethical PHP PHP ? HOSPITAL BOARD 146

• Independence • Employers need REVENUE • Groups need PARTNERS • Spouses need their SPOUSES • Families need INCOME • Doctors LAWYER up • State Boards Discipline AFTER the fact 147

BROTHER/SISTER’S KEEPER (Anonymity) 148

Why Do What the WVMPHP Says ? • • • 149

WVMPHP REPORTS TO BOARD • IMMINENT DANGER TO THE PUBLIC • FAILURE TO RESPOND TO TREATMENT • NON-COMPLIANCE WITH CONTRACT 150

Program Statistics Growth 1000%+ Success rate 90% 151
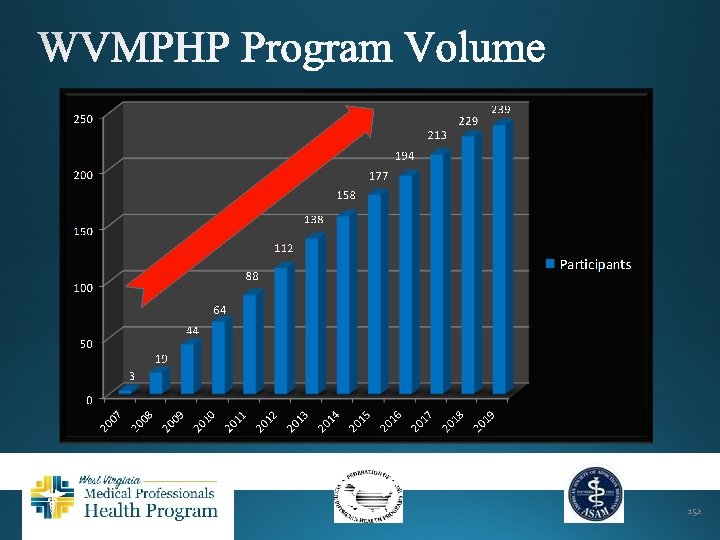
152
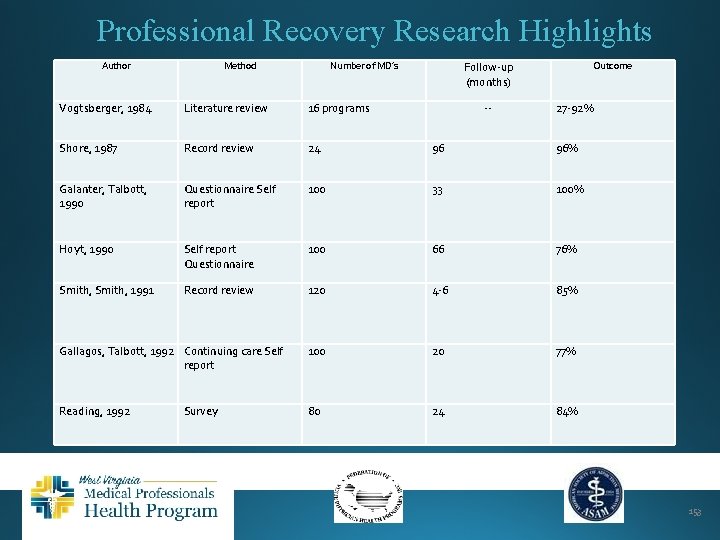
Professional Recovery Research Highlights Author Method Follow-up (months) Number of MD’s Vogtsberger, 1984 Literature review 16 programs Shore, 1987 Record review 24 96 96% Galanter, Talbott, 1990 Questionnaire Self report 100 33 100% Hoyt, 1990 Self report Questionnaire 100 66 76% Smith, 1991 Record review 120 4 -6 85% Gallagos, Talbott, 1992 Continuing care Self report 100 20 77% Reading, 1992 80 24 84% Survey -- Outcome 27 -92% 153

Blueprint PHP Study A National Survey of Physician Health Programs April 2005 §Phase I § PHPs provide early detection, assessment, evaluation and referral to intensive primary treatment § Very positive outcomes with low relapse rates and high percentage of physicians remaining licensed and employed § Conclusion: Several aspects of this continuing care model could be adapted and used for the general population §Phase II § 16 PHPs participate, 904 physicians with SUD § 78% successful completion with no relapses § Including those with relapse and further intervention, over 90% doing well at 7. 2 years § One report of patient harm (over prescribing) § “Such programs seem to provide an appropriate combination of treatment, support, and sanctions to manage addiction among physicians effectively. ” Du. Pont et al, How are addicted physicians treated? A national survey of physician health programs, Journal of Substance Abuse Treatment 37, March 2009 Mc. Clellan et al, Five year outcomes in a cohort study of physicians treated for substance use disorder in the United States, BMJ, November 2008 154

Colorado Physician Health Program Malpractice Study Results of Risk Relativity Rating: cohort. 20% better than Brooks et al, Physician health programmes and malpractice claims: reducing risk through monitoring, Occupational Medicine April 2013 155
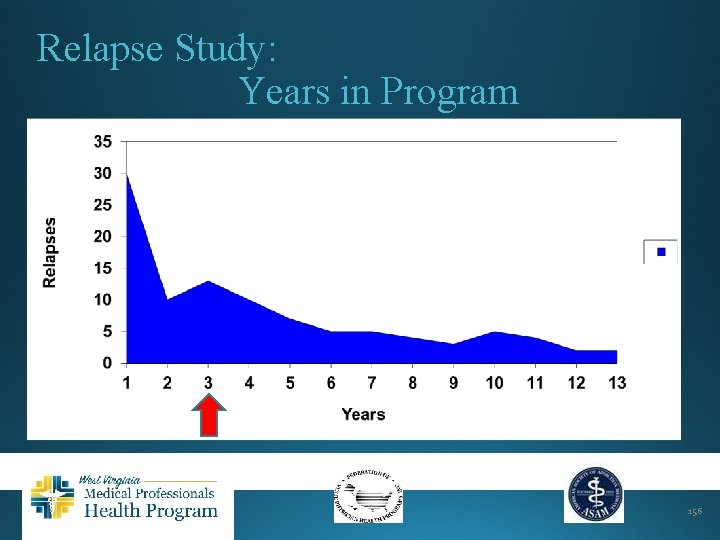
Relapse Study: Years in Program 156

Hospitals Legal Expenses Monitoring Expenses Joint Commission Continuing Medical Education Conflict of Interest Malpractice Liability Patient Care Continuity Medical Practice Act Exposure Recruiting Expenses Public Safety 157

5 8 Joint Commission MS 11. 01 üMandates…’the medical staff implement a process to identify and manage matters of individual physician health that is separate from the medical staff disciplinary process ’ üRobert Wise, MD, JCAHO, Vice President of Standards, Division of Research states, “Many states have specialized programs that deal with these matters. JCAHO accepts delegation to existing external programs as a means to meeting the standard. ” 6/7/2021

Board Consent Order v. A MAJOR ACTION – Ø Ø Data Bank Report Ø Can’t sit for Board Recertification Ø Ø Ø 159

West Virginia Medical Professionals Health Program Mission Statement: To protect healthcare consumers through seeking the early identification and rehabilitation of physicians, surgeons, and other healthcare professionals with potentially impairing health concerns including abuse of mood altering drugs including alcohol, mental illness or physical illness affecting competency so that physicians, surgeons, and other healthcare professionals so afflicted may be treated, monitored and returned to the safe practice of their profession to the benefit of the healthcare profession and the patients we serve. 160

Funding 161

Legislation Ø Ø Ø Funding 162

Structure & Function • • 163

Served Physicians Physician Assistants Podiatrists Licensees Others Non-discriminatory 164

Board Agreements * Licensure Renewal Applications –Grant confidentiality 165

Substance Abuse * Mental Illness * Behavioral Health, Leadership, & Boundaries Stress and Burnout Physical Illness Neurological Deficits Other Disorders Intervention * Education * Advocacy * 166

Treatment Outcome Comparisons § § § § 167

TREATMENT WORKS v Full Treatment Experience (Detoxification; Rehabilitation; Maintenance) v General Population relapses at 40 -60% @ 1 yr v Physicians Recover at 92% @ 1 year v Detoxification Alone at < 10% @ 1 year 168

anonymous, confidential and respectful manner. 169

Early detection Thorough assessment & evaluation Abstinence based treatment Long-term monitoring Documentation (abstinence, compliance, etc. ) 170
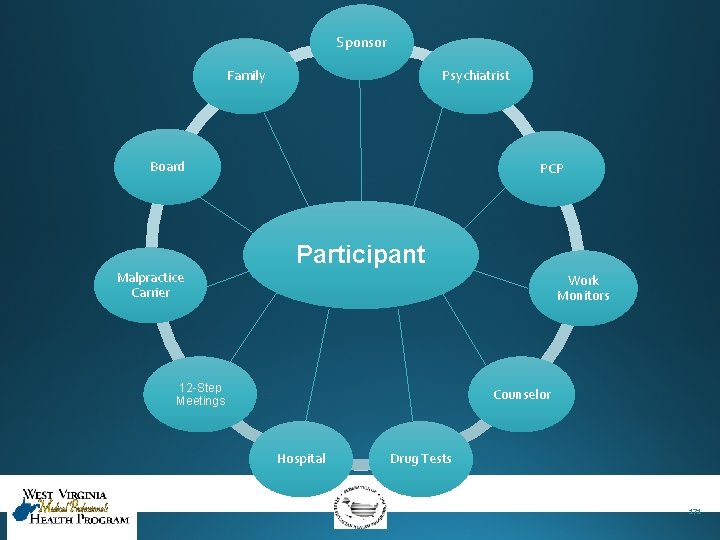
Sponsor Family Psychiatrist Board Malpractice Carrier PCP Participant Work Monitors 12 -Step Meetings Counselor Hospital Drug Tests 171
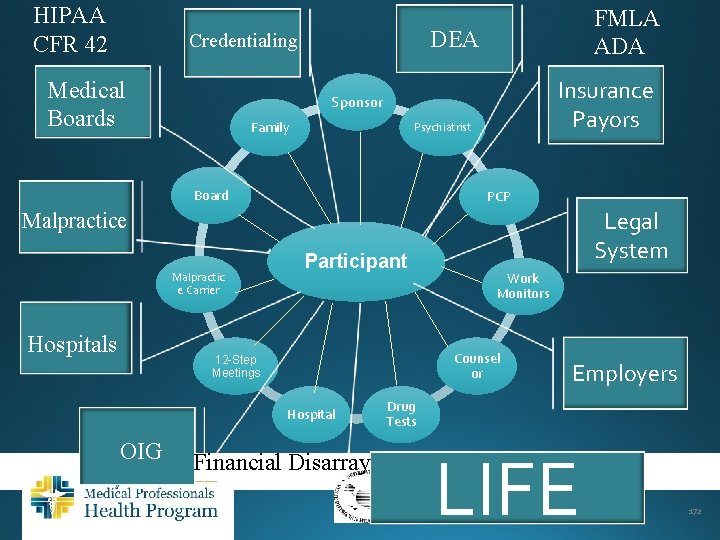
HIPAA CFR 42 DEA Credentialing Medical Boards FMLA ADA Insurance Payors Sponsor Family Psychiatrist Board PCP Legal System Malpractice Malpractic e Carrier Hospitals Participant Counsel or 12 -Step Meetings Hospital OIG Work Monitors Financial Disarray Employers Drug Tests LIFE 172

WVMPHP Statistics Students/Residents 25% Specialties – 24: ER, IM, GS, Rad Qualifying Illness: 90% SUD Psychiatric Comorbidity: 48% Referral Sources: 85% “Self” 173

Medical Illness Psych Addiction 174

Addiction Pain Psych Medical Illness 175

Complexity Addiction Pain Marital Discord Co-Dependency Financial Disarray Psychiatric *Professional Regulatory Agencies 176

Substance of Choice 177

Drugs of Abuse Active n=16 Opiates Marijuana Amphetamines Benzodiazepines Polysubstances 7 (44%) 2 (12%) 0 (0%) 7 (44%) All n=22 9 (41%) 3 (14%) 1 (4%) 0 (0%) 9 (41%) 178

If you are wondering if you have a problem, that is a BIG RED FLAG. Social users don’t wonder if they have a problem, they know they do not. If you are still wondering you might want to cut down on whatever you are doing. If you are unable to cut down …… call the WVMPHP. YOU 179

Relocations & RTW Inter-state Active 11 (16%) All 20 (30%) Continued working or Returned to work 56 (82%) 87 (78%) 180

8 1 Successful ongoing relationship years. continuous, period of 6/7/2021

SUCCESSFUL 1 PHP + 2 Boards = 4 182

REMEMBER ! Even very small intrusions of addiction into the workplace should be taken extremely seriously in physicians 183

Physician Wellbeing and the PHP • Burnout, Wellness & Resilience • Potentially impairing conditions • Substance Abuse, Mental Illness & Co-morbidities • Barriers to detection and assistance • Indicators of potential impairment • Overview of Physician Health Programs • The MESSAGE objectives 184

THE “MESSAGE” REHABILITATE 185

Lessons Learned • Long-term recovery (5 -years or more) is the expected outcome. 186

2019 Appalachian Addiction Conference October 16 – 19, 2019 Morgantown, WV www. wvmphp. org 187

Thank you…. to each and every one of you for who you are and what you do. Brad Hall, M. D. 188

• • www. wvmphp. org www. wvbom. wv. gov www. wvbdosteo. org www. wvsma. org www. wvoma. org www. fsphp. org www. asam. org 189

P. Bradley Hall, M. D. Executive Medical Director West Virginia Medical Professionals Health Program 4013 Buckhannon Pike Mount Clare, West Virginia 26408 Phone: 304 -933 -1030 Email: bhallmd@wvmphp. org Website: www. wvmphp. org 190

THE “MESSAGE” • • • 191

THE “MESSAGE” • • • 192

THE “MESSAGE” • • 193

THE “MESSAGE” • Physician health programs have 80 – 90+% success rate over 5 years • According to the AMA, 30% of physicians will have a condition which may impair their ability to practice medicine with reasonable skill & safety • Recovering addicted patients (medical professionals) CANNOT CONTROL MEDICALLY NECESSARY MEDICATION BY THEMSELVES If you are wondering if you have a problem, that is a BIG red flag. Social users don’t wonder if they have a problem, they know they do not. If you are still wondering you might want to cut down on whatever you are doing. If you are unable to cut down …… call the WVMPHP. 194

Sources • Federation of State Physician Health Programs Guidelines – www. fsphp. org • Mc. Lellan, et al. Drug Dependence, a Chronic Medical Illness. JAMA, October 2000 • Domino, et al. Risk Factors for Relapse in Health Care Professionals with Substance Use Disorders. JAMA, March 2005 • Mc. Lellan, et al. Five Year Outcomes in a Cohort Study of Physicians Treated for Substance Use Disorders in the United States. BMJ, November 2008 • Du. Pont, et al. How are Addicted Physicians Treated? Journal of Substance Abuse Treatment, March 2009 • Skipper. The Value of Physician Health Programs. Alabama Board of Medical Examiners Newsletter, December 2009 • Federation of State Medical Boards, Impaired Physician Policy – www. fsmb. org • American Society of Addiction Medicine, Physician Health Policies – www. asam. org www. wvmphp. org 195

https: //nsduhweb. rti. org/respweb/homepage. cfm http: //www. cdc. gov/nchs/ catchment-area-study. html http: //downloadily. com/docs/epidemiologic- http: //www. nimh. nih. gov/health/topics/ncsrstudy/nimh-funded-national-comorbidity-survey-replication-ncs-r-study-mental-illnessexacts-heavy-toll-beginning-in-youth. shtml http: //www. ncbi. nlm. nih. gov/pmc/articles/PMC 4005614/ http: //www. niaaa. nih. gov/research/guidelines-and-resources/epidemiologic-data http: //www. samhsa. gov/data/DAWN. aspx http: //www. drugabuse. gov/monitoring-future-survey-overview-findings-2013 http: //www. cdc. gov/nchs/deaths. htm http: //www. drugabuse. gov/ 196
- Slides: 196