PHLEBOTHROMBOSIS THROMBOSIS INTRAVITAL COAGULATION OF BLOOD IN VESSELS

PHLEBOTHROMBOSIS
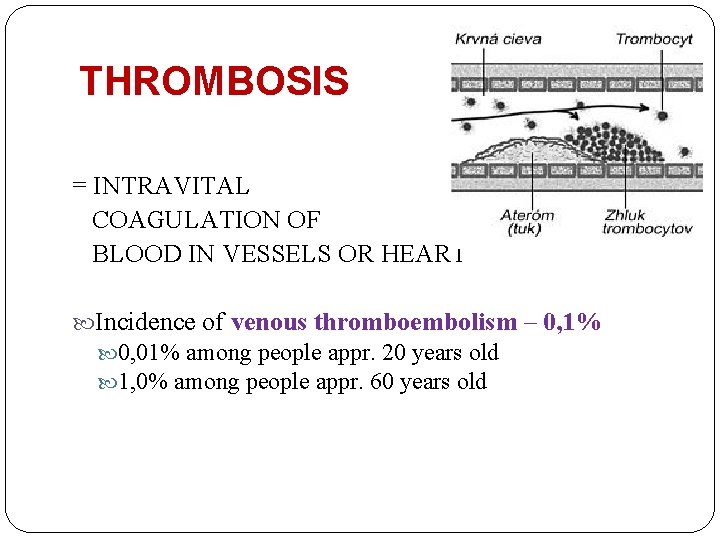
THROMBOSIS = INTRAVITAL COAGULATION OF BLOOD IN VESSELS OR HEART Incidence of venous thromboembolism – 0, 1% 0, 01% among people appr. 20 years old 1, 0% among people appr. 60 years old

Patogenesis of thrombosis = (1856) – Wirchow´s trias Most important factors activation of COAGULATION = activity of TXA 2, activity of anticoagulant sys. (AT III), levels or activation of coagulation f. . slow BLOOD FLOW = stasis, travelling by airplain, heart failure, paraplegia, immobilisation, pregnancy, varixes, operations, fractures. . . deffect of the VESSEL WALL – by damage of endothelium production of PGI 2 => proaggregatory activity

Arterial thrombi = white Thrombocytes Tight adherence => obturation = periferal ischemia Prevention = antiaggregants Venal thrombi = red Fibrinal tail Weak adherence => risk of embolisation Prevention = anticoagulants Recent thrombi Are removed by thrombolytics = fibrinolytics

Clinical conditions increasing the risk of thrombosis arterial: n atherosclerosis n smoking n hypertension n diabetes mellitus n LDL n TAG n + family history n deffect of left n high doses of synthetic oestrogens n polyglobulia … venous: n general surgery n orthopedical surgery n trauma, malignities, sepsis n immobilisation n congestive failure n nephrotic syndrome n obesity n varixes n postphlebitic syndrome n oestrogens n pregnancy
Different! thrombophlebitis phlebothrombosis

THROMBOPHLEBITIS primarily caused by mechanical, microbial or chemical irritation inflammation of vessel wall secondarily thrombosis – thrombus firmly adhering to vessel wall embolisation only occasionally clinically: local syndrome = inflammated superficial vein, can be palpated, skin above is red, warm, with significant pain and sensitivity, no big oedema, no general symptoms or only subfebrility complications: (rarely) early – spreading of inflammation to deep venous sys. , late – sec. chronic venous disease = postphlebitic syndrome
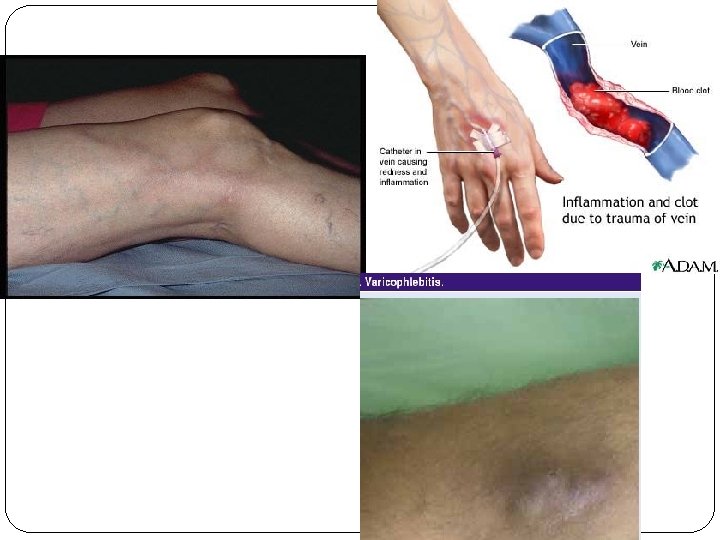

Deep Venous Thrombosis = Phlebothrombosis + it´s most dangerous complication = pulmonary embolisation (PE) – belong (after IHD and hypertension) among the most common CV diseases in hospitalised patients PE - 10% of autopsial material 85% of PE is caused by deep venous thrombosis
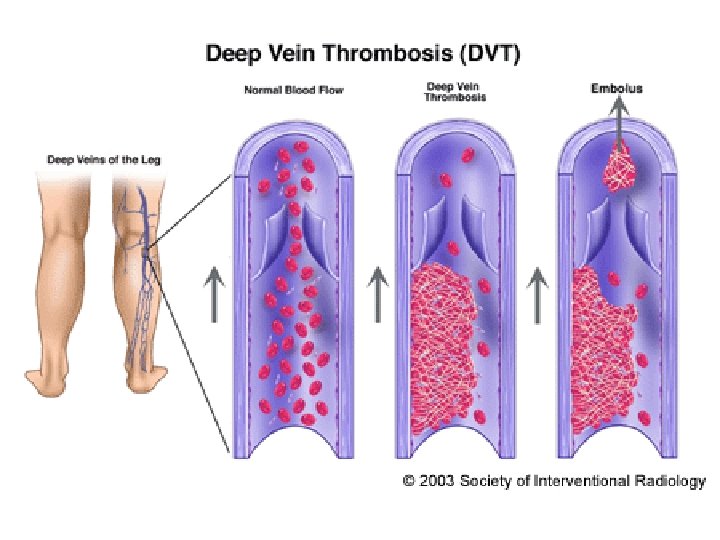

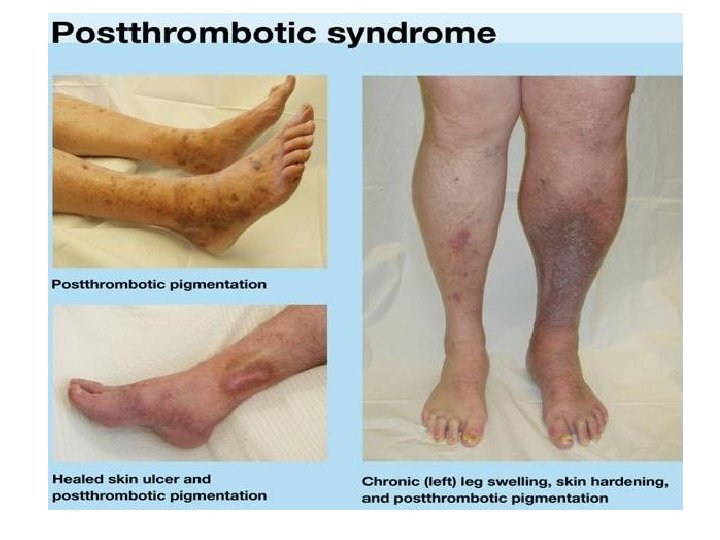
PHLEBOTHROMBOSIS (PT) deep veins of lower extremities primarily obturation of vein with thrombus and secondarily inflammatory reaction released thrombus = embolus clinically: often asymptomatic – or little symptoms = dg. only 30 -50% oedema – asymmetric pain – spontaneous, compressive – mostly while hanging down the limb, spasms, feeling of strain symptoms of blocked blood flow from the limb (erythema- pale skin- cyanosis) collaterals –forming after several days of obturation as compensatory mechanism, systemic symptoms – not specific (if there is no PE)
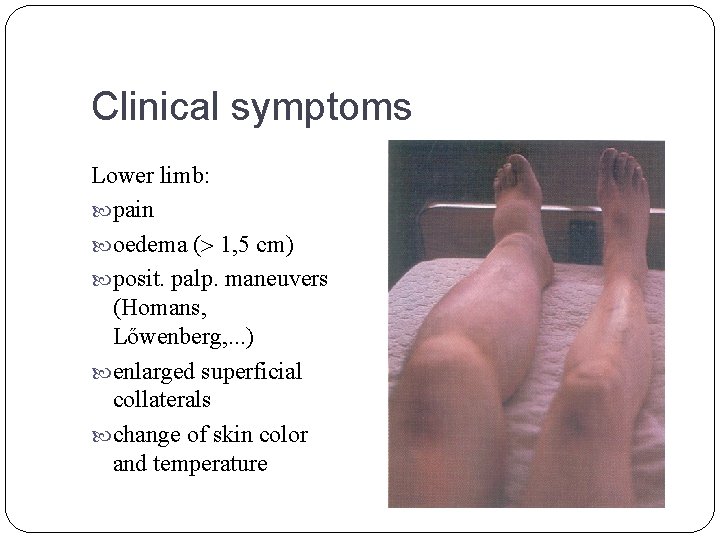
Clinical symptoms Lower limb: pain oedema ( 1, 5 cm) posit. palp. maneuvers (Homans, Lőwenberg, . . . ) enlarged superficial collaterals change of skin color and temperature
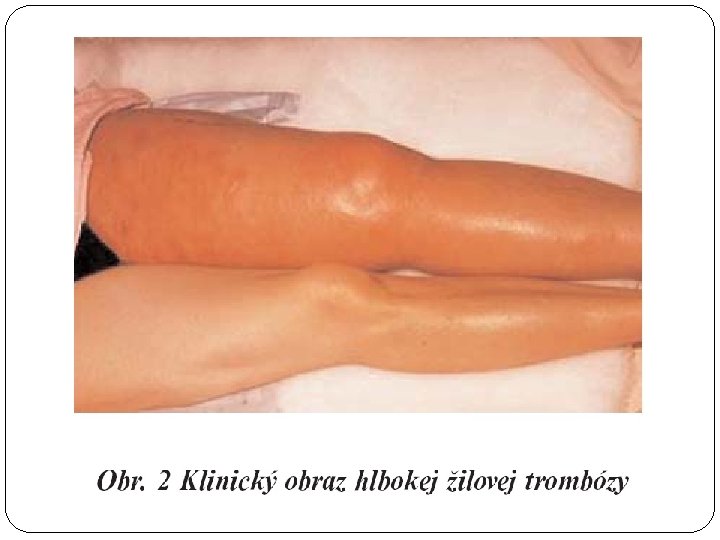

Complications of PT 1. EMBOLUS - released thrombus, carried by the blood flow– mainly to pulmonary artery pulmonary embolisation 2. Repeated small embolisation (successive) =>chronic pulmonary hypertension => cor pulmonale chronicum 3. Chronic venous insufficiency
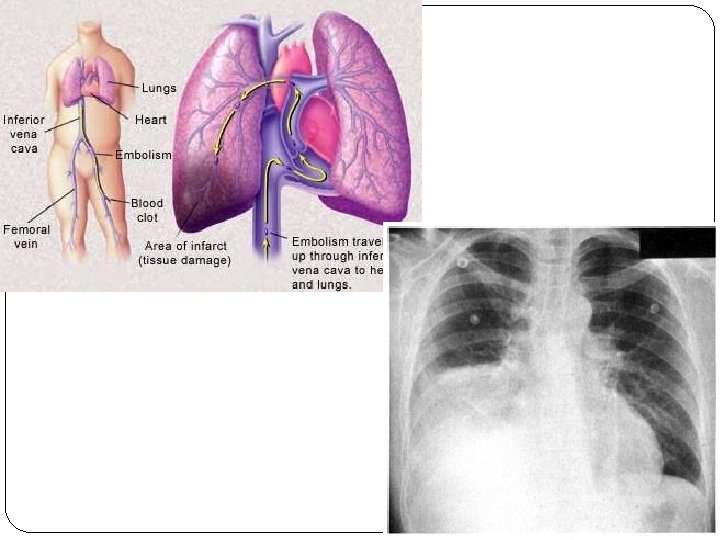
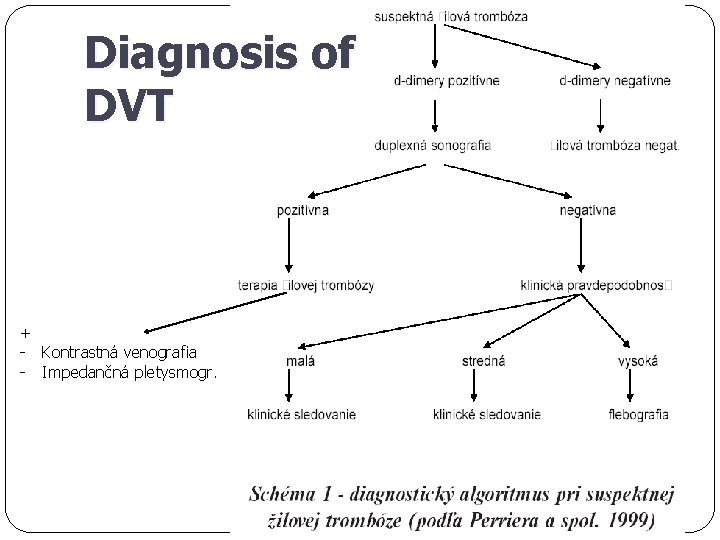
Diagnosis of DVT + - Kontrastná venografia - Impedančná pletysmogr.

Goals of the treatment of PT save the patient´s life avoid occurance of pulmonary embolism initialise / speed-up resolution of thrombus/embolus accelerate symptom regression prevention of recurrency reduce long term mortality

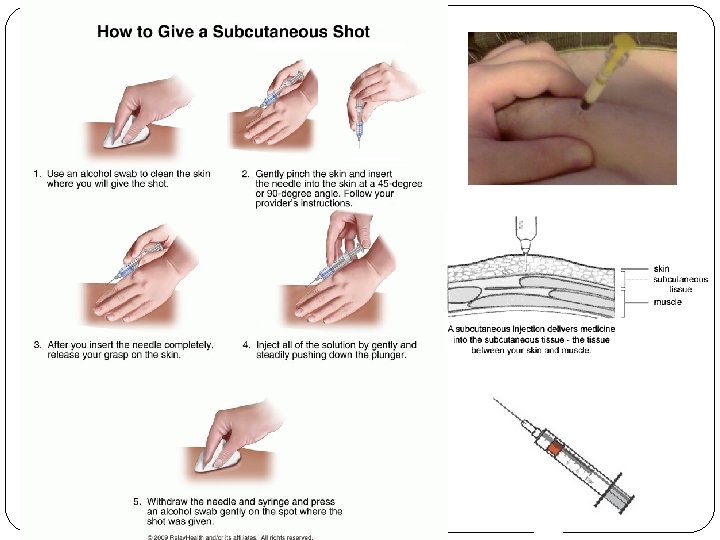
Prevention of PT nonpharmacologic limb elevation (15 -20º) early mobilisation after surgery regular exercise with legs in bed elastic, special tights walking pharmacologic low doses of heparin (5000 IU) (before operation, during postoperation period at risk patients), LMWH, fondaparinux

Antithrombotics Antiaggregatory drugs (inh. platelets) Anticoagulants (inh. coagulation factors) 1. Block activation of platelets -low-dose aspirin -indobufen -ticlopidin, clopidogrel, prasugrel, tikagrelor 2. Block final aggregation of platelets = antagonist of IIb/IIIa GP rec. monoclonal Ab (abciximab) inhibitors of synthetic peptids (eptifibatid) non-peptide inhibitor (fibans= tirobifan) Thrombolytics (dissolve thrombus) 1. p. o. -warfarin -xabans -gatrans 1. Fibrin nonspecific -Streptokinase -Urokinase 2. parenteral -UFH -LMWH -fondaparinux 2. Fibrin specific -Alteplase -Reteplase -Lanoteplase -Tenecteplase

Antithrombotics antiaggregants (antiplatelet drugs) = block FORMATION of thrombus anticoagulants = block GROWTH of thrombus thrombolytics (fibrinolytics) = DISSOLUTION of already formed thrombus

Anticoagulants DRUGS ARTIFICIALLY INDUCING “DISTURBANCES“ OF BLOOD COAGULATION GOAL: TO PREVENT THROMBOSIS OR TO PREVENT FURTHER GROWTH OF THROMBUS

ANTICOAGULANTS DIRECT n Indirect inhibitors of thrombin and factor Xa – Heparin (IIa : Xa) – LMWH (IIa : Xa) n enoxa-, fraxi-, dalte-, revi- – Fondaparinux ( Xa) n Direct inhibitors of thrombin – Hirudin, bivalirudin, desirudin – Dabigatran – p. o. = gatrans n Direct inhibitors of factor Xa – Rivaroxaban, apixaban – p. o. = xabans INDIRECT Warfarin (vit. K dependent) n
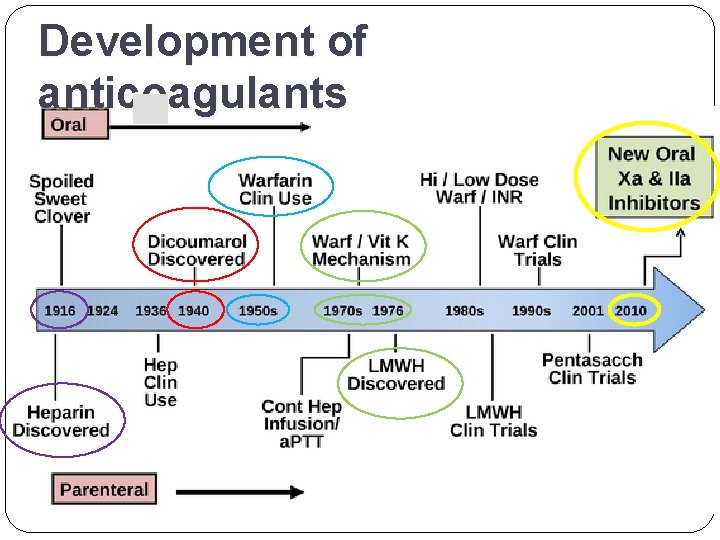
Development of anticoagulants
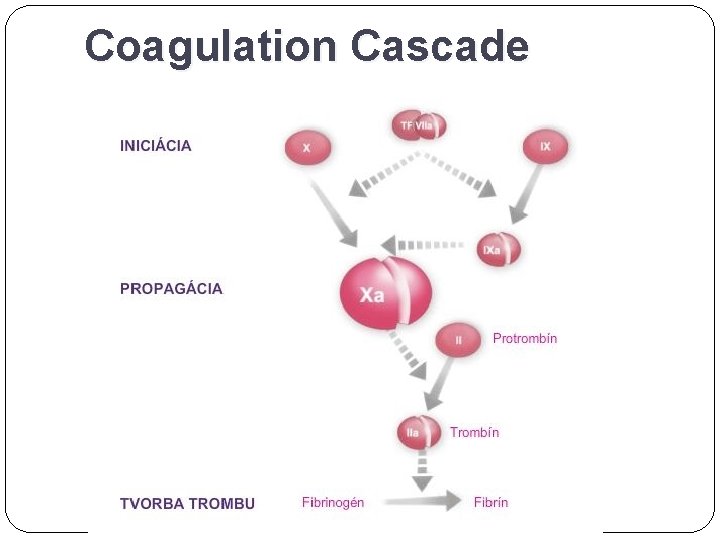
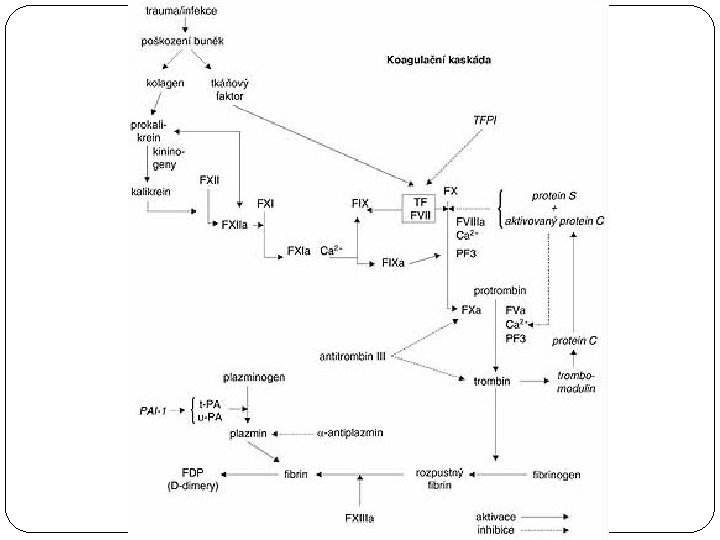
Coagulation Cascade
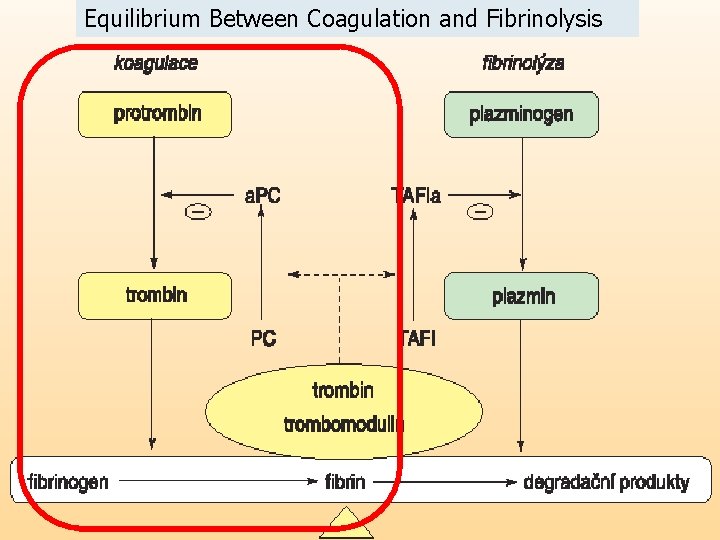
Equilibrium Between Coagulation and Fibrinolysis
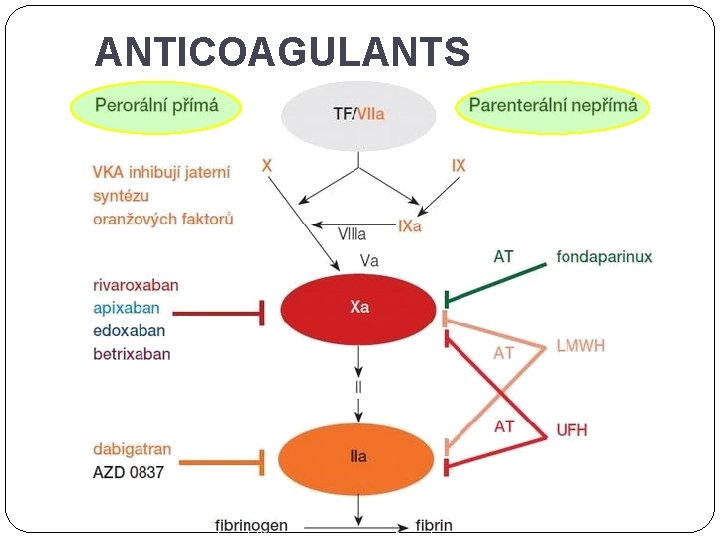
ANTICOAGULANTS

HEPARIN INDIRECT INHIBITOR OF THROMBIN SUBSTANCE PRESENT ALSO IN OUR BODY (MAST CELLS), USED FROM 1916 MW = 3 - 30 000 D (15 000 D) produced from intestinal mucosa of porcine or cattle lungs => quantified in IU heterogenous mucopolysacharid, anion (´-´ charge) ACTIVITY IS DEPENDENT FROM THE PRESENCE OF A N T I T H R O M B I N III.
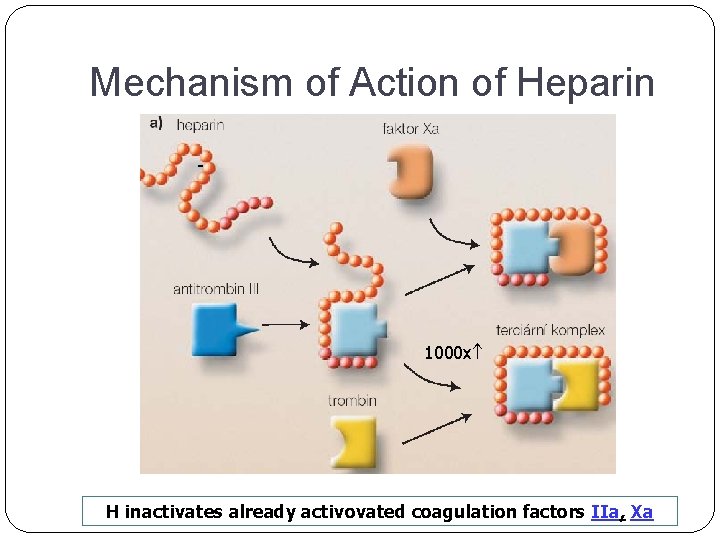
Mechanism of Action of Heparin - + 1000 x H inactivates already activovated coagulation factors IIa, Xa

Effects of heparin Anticoagulant activity Weak inhibition of platelet function - adhesivity and aggregation Weak stimulation of fibrinolysis releasing of lipoproteinic lipase clearing of lipemic plasma anti - IIa : anti –Xa = 1 : 1

Advantages of heparin acts very quickly or immediately, but shortly has massive effect it has an antidote - protamine

Disadvantages of heparin only injection (i. v. , s. c. ), i. m. – no, irregular absorption and haematoma T 1/2 is variable, prolonged with dose, unpredictable anticoagulant effect – wide variability (for different binding to proteins and unpredictable absorption after s. c. admin. ) possibility of disease reactivation after stopping administration (rebound efect) control: a. PTT (reflects effect to thrombin) – extension to 1, 5 -2, 5 x of norm
a. PTT = 1, 5 -2, 5 x normal

Indications of heparin Prophylaxis of vein thrombosis Th. of deep vein thrombosis and pulmonary embolia Acute coronary syndroms (Th) Obturation of peripheral arteries Hemodialysis, DIC

ADR of heparin Bleeding H. induced thrombocythopenia (HIT) – less serious, early f. ; more serious f. after 5 and days Allergy Reversible alopecia Possible osteoporosis in case of long-term use

LOW-MOLECULAR-WEIGHT HEPARINS (LMWH) INDIRECT INHIBITORS OF THROMBIN smaller molecules, MR 5 000 D INHIBIT MORE ANTI-Xa PRODUCED BY CHEMIC OR ENZYMATIC DEPOLARISATION OF H ACTIVITY DEPENDS ON THE PRESENCE OF A N T I T H R O M B I N III
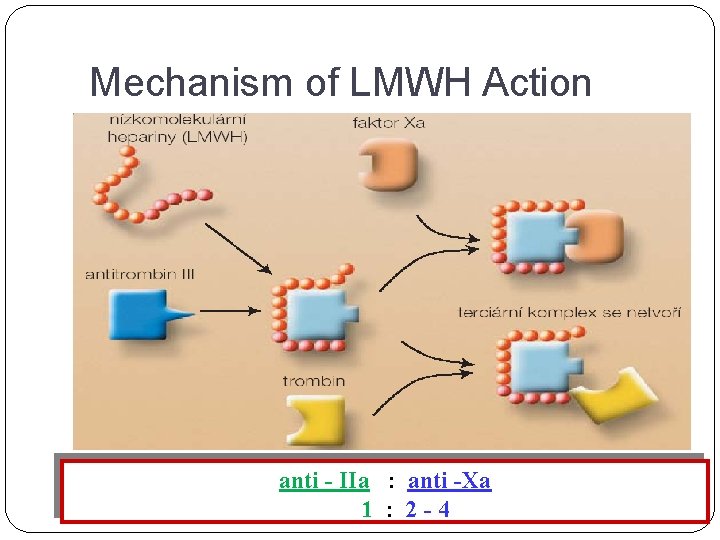
Mechanism of LMWH Action anti - IIa : anti -Xa 1 : 2 - 4

Indications of LMWH Prevention of thromboembolia (abdominal and orthopedic surgery) Prevention of ischemic complications at acute coronary syndroms (unstable angina pectoris, NSTEMI myocardial infarction) Therapy of phlebothrombosis and pulmonary embolism Hemodialysis

Advantages of LMWH Predictable response to dose according to weight Longer plasmatic half-life (1 -2 s. c. injections per day) Lower risk of thrombocytopenia, bleeding and thrombosis Heparin and LMWH can be administered during pregnancy and lactation Antidote: Protamine (60 -80% reversal of action)

FONDAPARINUX INDIRECT INHIBITOR OF THROMBIN SYNTHETIC PENTASACHARID SPECIFICALLY INHIBITING FACTOR Xa MR = 1 700 D activity depends on the presence of A N T I T H R O M B I N III doesn´t have the long chain needed for bridging to ATIII. and f. IIa 300 X ability to inactivate f. Xa
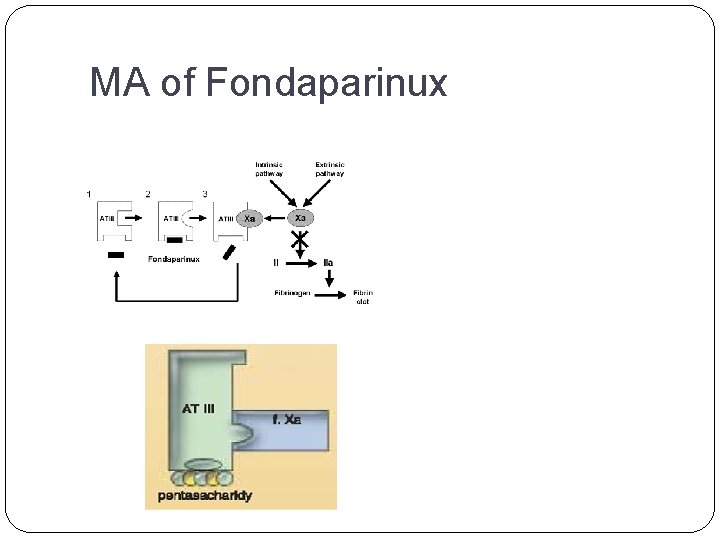
MA of Fondaparinux

Advantages of Fondaparinux of bleeding complications administered s. c. relatively long lasting effect highly predictable effect doesn´t influence aggregation of platelets doesn´t induce thrombocythopenia disadvantage = price antidote in 3 rd phase of clinical trials
HIRUDIN, BIVALIRUDIN n n PRIAMY INHIBÍTOR TROMBÍNU špecificky IREVERZIBILNE INAKTIVUJE TROMBÍN BEZ potreby prítomnosti AT III. n je prirodzený inhibítor zrážania krvi získavaný z pijavíc (hirudo medicinalis) n vyrába sa DNA REKOMBINANTNOU technikou

HIRUDIN, BIVALIRUDIN DIRECT INHIBITOR OF THROMBIN SPECIFICALLY IRREVERSIBLY INACTIVATES THROMBIN WITHOUT THE NEED FOR AT III NATURAL INHIBITOR OF BLOOD COAGULATION GAINED FROM LEECH (HIRUDO MEDICINALIS) PRODUCED BY DNA RECOMBINANT TECHNOLOGY
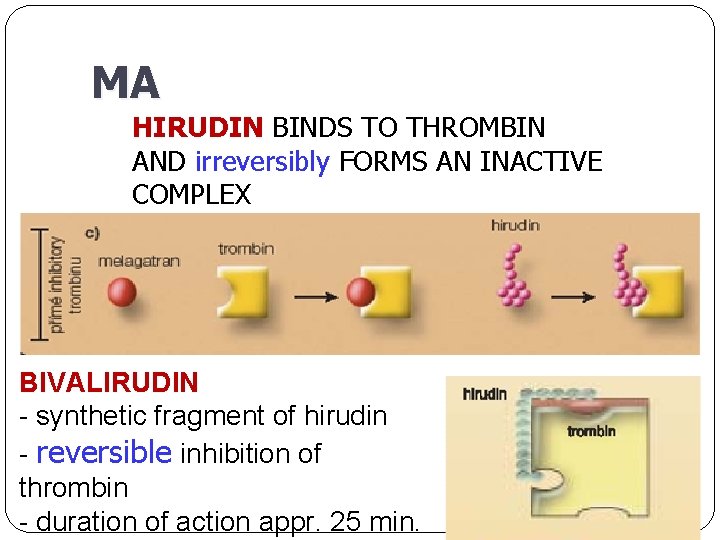
MA HIRUDIN BINDS TO THROMBIN AND irreversibly FORMS AN INACTIVE COMPLEX BIVALIRUDIN - synthetic fragment of hirudin - reversible inhibition of thrombin - duration of action appr. 25 min.

Advantages of Hirudin doesn´t bind to plasma proteins predictable anticoagulant effect indicated for patients with thrombocythopenia after heparin who need AC th. bivalirudin – indicated in AMI, as an alternative to heparin/LMWH inactivates not binded thrombin, but also thrombin binded to fibrin in thrombus anticoagulatory effectivity inhibits formation of fibrin inhibits activation of thrombocytes = mild antiaggregatory effect prevents activation of f. V, VIII, XI and XIII peg-hirudin – 1 times per day, s. c.

COUMARINS I N D I R E C T p. o. ANTICOAGULANTS = „ANTAGONISTS“ OF VITAMIN K factors II. , VII. , IX. , X. DOESN´T ACT ANTICOAGULATORY IN VITRO Warfarin – the most widely used coumarin Other use – poison for gnawers


Mech. of Action - Warfarin inhibition of epoxidreductase, decreased formation of active form of vitamin K no activation of carboxylase and no carboxylation of -glutamin residuums of factors II. , VII. , IX. , X. + inhibition of protein C and S carboxylation coumarins antagonise liver synthesis of f. II, VII, IX and X => formed molecules are incomplete, unfunctional, can´t get activated and don´t participate in coagulation
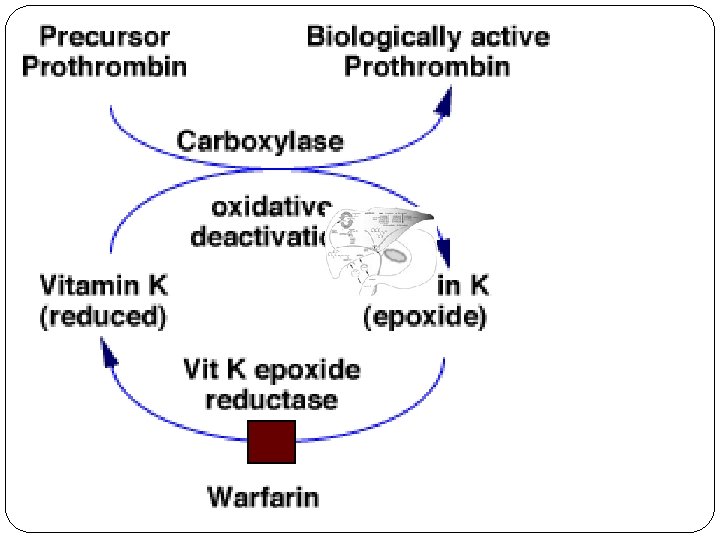

Pharmacokinetics of warfarin EFFECT STARTS WITH LATENCY OF 12 -24 HOURS, MAXIMAL EFFECT AFTER 2 -3 days AFTER discontinuation the effect REMAINS 4 -5 days 100% BA, 97% binding to plasma proteins many interactions

Interactions of Warfarin pharmacokinetic - high binding to plasma proteins - metabolised by CYP 450 pharmacodynamic - groceries with high vitamin K content can reduce effect - antibiotics that suppress bacteria in GIT that produce vitamin K can increase the effect
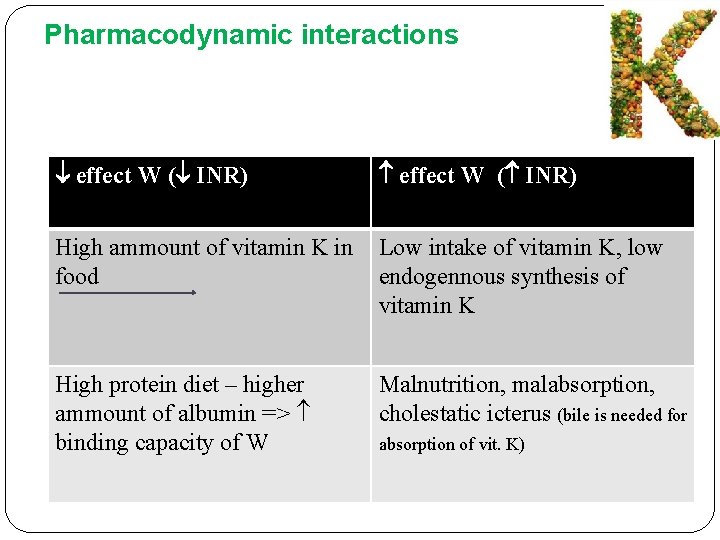
Pharmacodynamic interactions effect W ( INR) High ammount of vitamin K in Low intake of vitamin K, low food endogennous synthesis of vitamin K High protein diet – higher ammount of albumin => binding capacity of W Malnutrition, malabsorption, cholestatic icterus (bile is needed for absorption of vit. K)
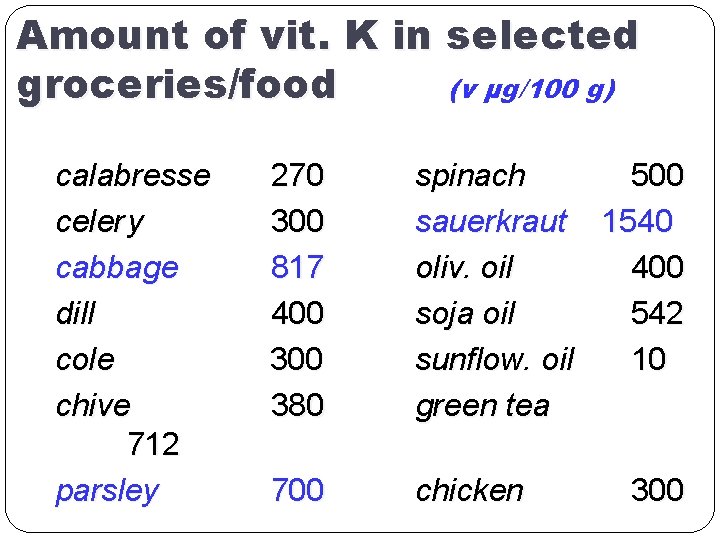
Amount of vit. K in selected groceries/food (v μg/100 g) calabresse celer y cabbage dill cole chive 712 parsley 270 300 817 400 380 spinach 500 sauerkraut 1540 oliv. oil 400 soja oil 542 sunflow. oil 10 green tea 700 chicken 300

Pharmacokinetic interactions n Metabolised in v liver: CYP 2 C 9 (S-warfarin: 70%) CYP 1 A 2 a CYP 3 A (R-warfarin: 30%) Changed to inactive metabolites easily excreted with kidneys Genetic polymorphism !

Pharmacokinetic interactions – Inhibitors of CYP 2 C ( INR, bleeding) n n Amiodarone Azole antimycotics (fluco. , mikon. , voricon. , ketoc. , itrac. ) n Metronidazole Sulphonamides, sulphometoxazol+TMP NSA (dicloph. , flurbip. , ketoproph. ) SSRI (fuoxetine, fluvoxamine) n . . n Ginger, garlic (more than 5 pcs) n n n

Pharmacokinetic interactions – Inducers of CYP 2 C ( INR, thrombosis) n Rifampicin, rifabutin, rifampin, rifapentin Carbamazepine, phenytoin Barbiturates Bosentan Griseofulvin Ethanol, cigarette smoke n St. John's wort, coenzyme Q 10, ginseng n n n

DISADVANTAGES of warfarin n latency of effect (2 -3 days) not suitable for therapy of a c u t e conditions => used for prophylaxis Need for control of therapy and correct dosage according to INR (2, 0 -4, 5 – according to indication) Testing of INR every 3 -4 weeks

INR n International normalised ratio patient´s Quick time n INR = Quick time of standard n Prophylaxis of thrombosis INR = 2, 0 – 2, 5 n Therapy of thrombosis INR = 2, 0 – 3, 0 n In pat. with antiphospholipid sy. INR = 3, 0 – 4, 5
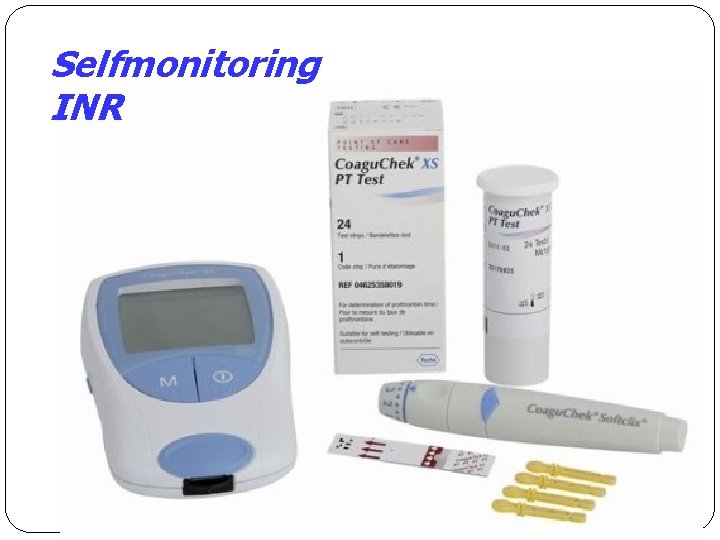
Selfmonitoring INR
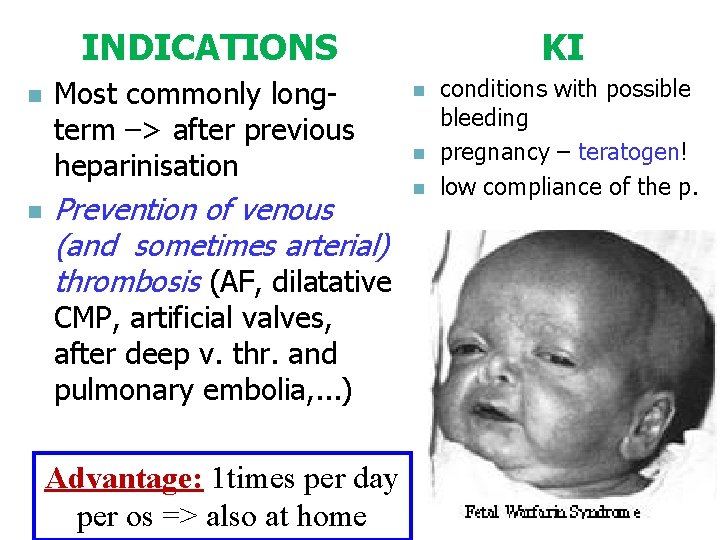
INDICATIONS n n Most commonly longterm –> after previous heparinisation Prevention of venous (and sometimes arterial) thrombosis (AF, dilatative CMP, artificial valves, after deep v. thr. and pulmonary embolia, . . . ) Advantage: 1 times per day per os => also at home KI n n n conditions with possible bleeding pregnancy – teratogen! low compliance of the p.

ADR of coumarins n n n Bleeding Teratogen Bleeding at new born whose mother takes warfarin and brest-feeds Dyspepsia Skin necrosis

Treatment of warfarin induced bleeding - at mild bleeding – lower the dose or stop administration - at more severe bleeding – vitamin K - at massive bleeding – frozen plasma, prothrombin concentrate, full blood
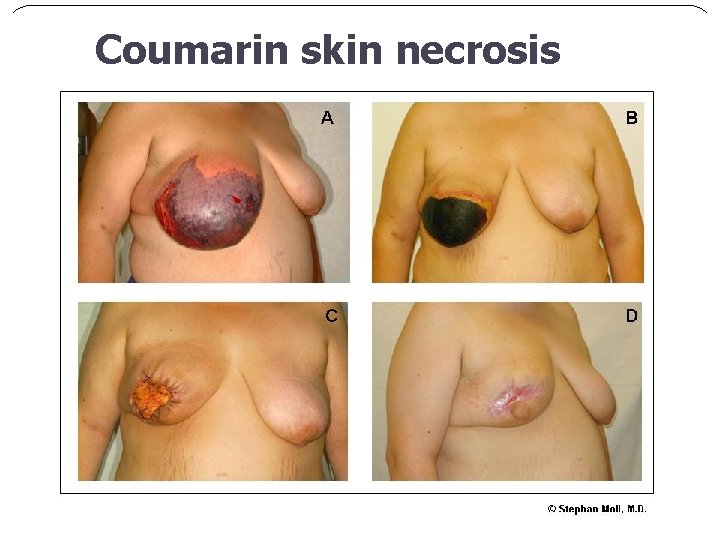
Coumarin skin necrosis
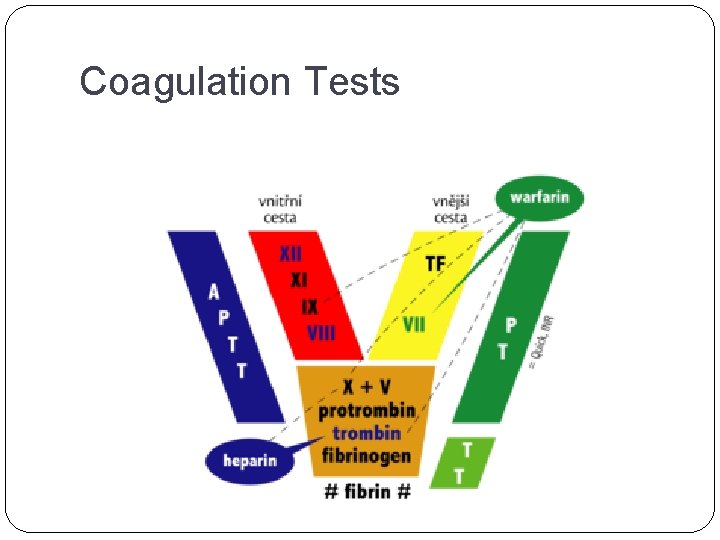
Coagulation Tests

NOAC = DOAC Advantages More targeted anticoagulant effect Lower risk of drug and food interactions When used in the approved indications and dosages according to SPC No need to check laboratory tests! Disadvantages In case of complications - the limited possibilities of laboratory monitoring (specific tests that are expensive and not yet widely available) The absence of specific antidotes => in 3 rd phase of clinical trials – still problem to handle bleeding
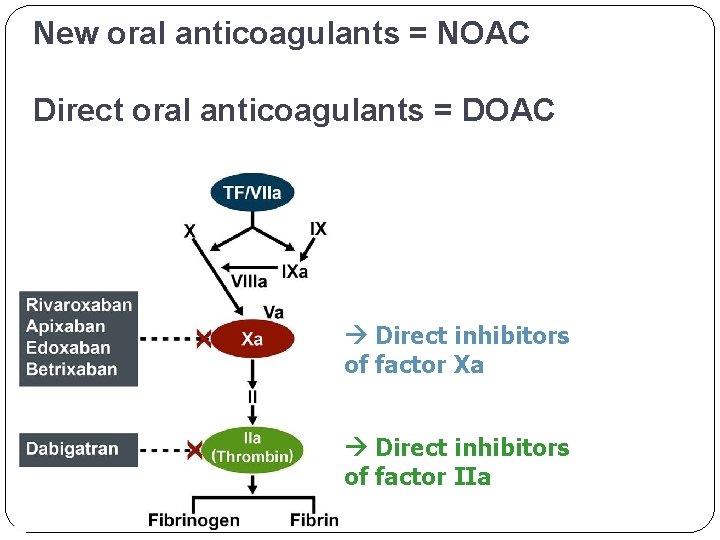
New oral anticoagulants = NOAC Direct oral anticoagulants = DOAC Direct inhibitors of factor Xa Direct inhibitors of factor IIa

Newer peroral anticoagulants Dabigatran- direct inhibitor of thrombin; approved for prevention of thrombosis after hip or knee surgery; atrial fibrillation (prevention of thr. ) Rivaroxaban- direct inhibitor of factor Xa; approved for prevention of thrombosis after hip or knee surgery; atrial fibrillation (prevention of thr. )

DABIGATRAN (g a t r a n s) n n n n Potent, competitive, direct, reversible inhibitor of thrombin Ximelagatran Inhibits: hepatotoxicity – Free thrombin – Thrombin binded to fibrin – Tr. aggregation induced by thrombin strong, predictable anticoag. effect (be carefull of bleeding) !!! p. o. , rapid onset + long duration Few interactions with drugs and food No need for regular coagulation controlls I: primary prevention of thromboembolic dis. New antidote – IDARUCIZUMAB !!! (monoclonal antibody) /Boehringer Ingelheim/

IDARUCIZUMAB = Antidote of dabigatran Praxbind® is registered in EU (also in Slovakia) from November 2015

RIVAROXABAN, APIXABAN (x a b a n s) n n n Direct inhibitors of f. Xa Selective, competitive, potent Inhibits f. Xa – free, - bound with prothrombin, - also in fibrin clot (5 x ) Anticoag. effect is directly proportional to the level in plasma and last only during this time!! !!! p. o. , fast onset of action No complicated metabolism => drug interactions

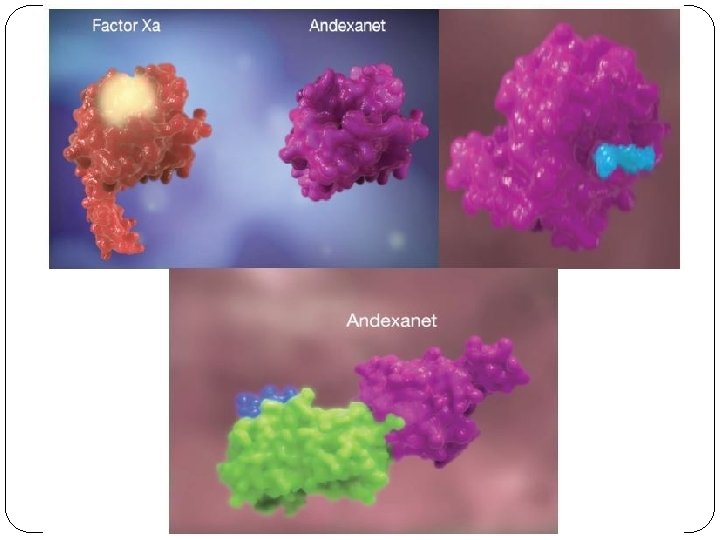
Andexanet alfa – antidote of f. Xa § Protein - modified, recombinant derivate of human factor Xa totally WITHOUT procoagulatory and anticoagulatory activity § Antidote for inhibitors of factor Xa: § direct (-xabans) § indirect (enoxaparin, fondaparinux) § Mechanism of action: andexanet is bait for inhibitors of f. Xa § Approved in USA May, 2018

Universal antidote - ? CIRAPARANTAG Synthetic small molecule: hydrogen bond (NOAC); charge – charge interactions (heparin) In 2 nd phase of clinical trials
FIBRINOLYTICS
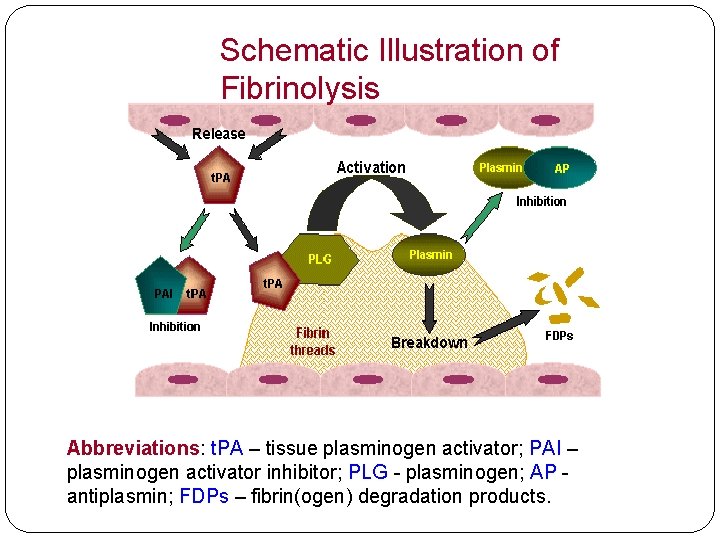
Schematic Illustration of Fibrinolysis Abbreviations: t. PA – tissue plasminogen activator; PAI – plasminogen activator inhibitor; PLG - plasminogen; AP antiplasmin; FDPs – fibrin(ogen) degradation products.
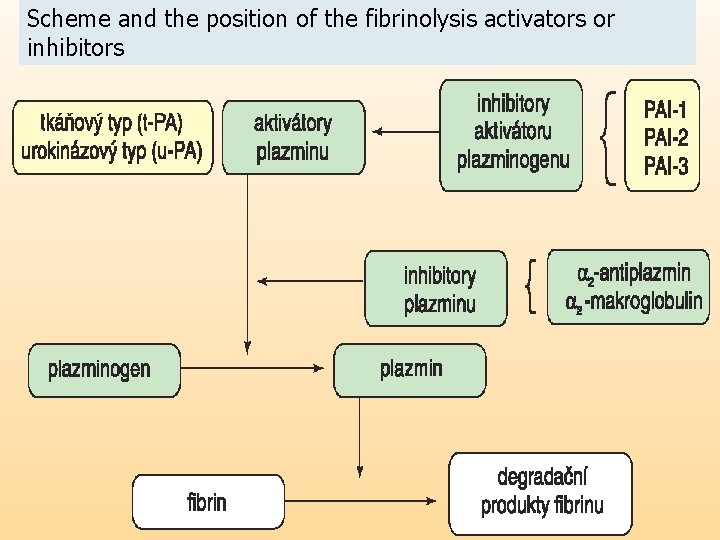
Scheme and the position of the fibrinolysis activators or inhibitors FIBRINOLYTICS = thrombolytics cause/accelerate thrombus dissolution by degradation of fibrin have strict indications and contraindications, because they risk of bleeding 4 x treatment must be combined with anticoagulant and/or antiaggregatory th. control: thrombin time – 2 -3 x extended indications: myocardial infarction, massive pulmonary embolism, DVT

1 st generation: Streptokinase Urokinase Anistreplase: plasminogen-streptokinase activator complex (APSAC) 2 nd generation: Alteplase (t-PA, tissue plasminogen activator) 3 rd generation: Reteplase (rt-PA, recombinant. plasm. activator) Lanoteplase (n. PA) Tenecteplase(TNK, recombinant. plasm. activator) Staphylokinase

Classification according to Fibrin Specificity not fibrin specific not selective fibrin specific selective Streptokinase Alteplase Antistreptase Reteplase Urokinase Lanoteplase Tenecteplase Activation of plasmin is systemic, are degraded also other proteins => ADRs Activate plasmin on the top of fibrin and less in circulation => lower risk of systemic bleeding
Indications AMI (STEMI) massive pulmonary embolia acute obturation of an artery deep vein thrombosis (not always) acute thrombotic stroke In patients with ischaemic stroke we need to apply thrombolysis till 3 hours after beginning of ischaemia. At pulmonary embolia, the time interval is much longer – even several days after beginning, but the risk of bleeding to pulmonary parenchyma is higher then.

ADRs frequently - bleeding including bleeding to CNS (appr. 3 -4 cases /1000 treated patients) febrile reactions hypotension allergic reaction after streptokinase or anistreplase, even anaphylactic shock
Absolute Contraindications stroke in last 6 months, history of bleeding to the brain serious trauma or operation in the last 3 weeks bleeding to GIT dissected aneurysm of aorta known bleeding defect

I. GENERATION: NON-FIBRINSELECTIVE AGENTS STREPTOKINASE INDIRECT activator of fibrinolytic system the oldest fibrinolytic /1933/, low price
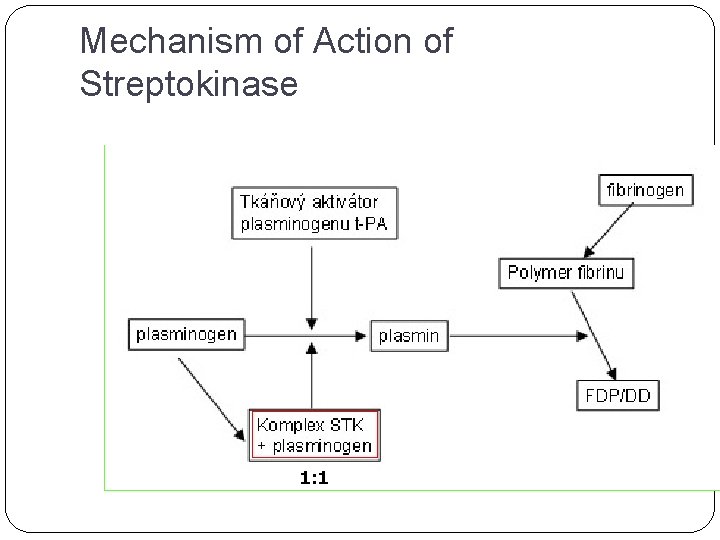
Mechanism of Action of Streptokinase 1: 1

DISADVANTAGES of STK activates also the circulating plasminogen from -haemolytic streptococcus antigenic is possible to premedicate- i. v. hydrocortisone before administration of STK can cause febrile reaction effect can be reduced by streptococcal infection or previous thrombolysis with STK it can be risky to administer repeatedly – possible occurence of allergic reaction doesn´t have to be effective, will react with already formed circulating antibodies don´t administer from 5 th day till 12 th month after previous aplication

II. GENERATION: THROMBOLYTICS FIBRINSELECTIVE ALTEPLASE DIRECT activator of fibrinolytic system high selectivity for plasminogen on the top of thrombus (on the top of thrombus activates plasminogen 100 x stronger than in circulation) natural protease from endothelium of vessels (t. PA) produced by recombinant technology short T 1/2 => in continual infusion not antigenic => Ø allergies, possibility of repeated administration

III. GENERATION: THROMBOLYTICS FIBRINSELECTIVE - better pharmacokinetics - fibrinolytic effect - smaller resistency to natural inhibitors - fibrin specificity with better safety profile

RETEPLASE Single-chain mutant of natural t. PA Produced by cultures of E. coli Not antigenic Extended T 1/2 => in 2 bolus doses à 30 min. => possibility of pre-admission treatment of AMI Preferably activates plasminogen binded to fibrin => increased fibrinolytic activity TENECTEPLASE 3 -multiple mutant of t. PA => Even longer T 1/2 than reteplase + fibrin selectivity As one i. v. bolus during 5 -10 sec. Price of 1 dose appr. 1 000 €
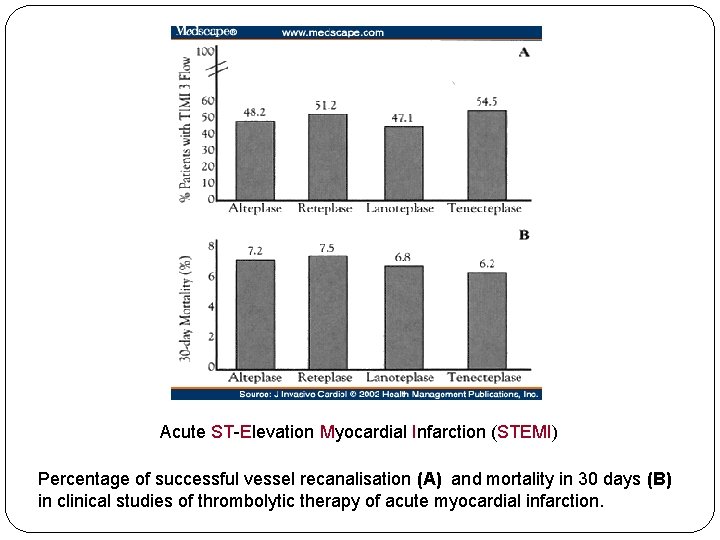
Acute ST-Elevation Myocardial Infarction (STEMI) Percentage of successful vessel recanalisation (A) and mortality in 30 days (B) in clinical studies of thrombolytic therapy of acute myocardial infarction.
- Slides: 92