PHL 322 ANTIDEPRESSANTS AND MOOD STABILIZING DRUGS Dr

PHL 322 ANTIDEPRESSANTS AND MOOD STABILIZING DRUGS Dr. Mohamed M. Sayed-Ahmed

Introduction

Depression "Depression" is a very common psychiatric disorder that is related to the "mood" (affective disorder). n Changes in mood are associated with depression and/or mania. n Disorders of mood rather than disturbance in thought or cognition. n Clinical depression: feeling sad for more than two weeks.

Symptoms of Depression 1 - Emotional Symptoms n n n Intense feelings of sadness, hopelessness and despair Inability to experience ordinary pressure or to cope with ordinary life events Feeling of guilt and ugliness Indecisiveness and loss of motivation Loss of energy and interest

2 - Biological symptoms 1 - Retardation of thought and action 2 - Loss of libido 3 - Loss of appetite and sleep disturbance *** DEPRESSION IS THE MOST COMMON CAUSE OF SUICIDE

Symptoms of "mania" are exactly the opposite: • Happy, excited, euphoric , self-confidence, lack of judgment • Sudden odd decisions that are mostly of disastrous consequences • Excessive rapid talking , moving quickly from one to another (Flight of ideas) • Hyperactive & full of energy, unable or unwilling to sleep • Sudden irritability, rage or paranoia • Impatience, Aggression

Classification of Depression A) According to severity of symptoms: 1. Mild depression-----self-limiting 2. Moderate depression -------difficulties at home and work 3. Severe depression ----serious, associated with suicidal thoughts

B) According to type 1 - Unipolar depression (major depression): n n mood swings are always in the same direction about 75% of cases non-familial n n n accompanied by symptoms of anxiety and agitation Associated with stressful life events 25% familial n n unrelated to external stresses endogenous depression 2 - Bipolar depression (manic-depressive): n in which depression alternates with mania n enthusiasm and self-confidence, accompanied by impulsive actions

The patient swings between "mania" and "depression“ (manic-depressive illness) - It is mainly hereditary and appears in early adult life. - Alternating depression and mania

3 - Other forms of depression - Psychotic depression Postpartum depression Atypical depression What are the possible mechanisms of depression? • Depression is associated with insufficient central release of NA and 5 -HT • Led to development of the Biogenic Amine Hypothesis

The Monoamine Theory of Depression n Proposed in 1965 and states that DEPRESSION is caused by a functional deficit of Monoamine transmitter at certain sites in the brain, while MANIA results from functional excess. n Theory is based on the ability of known antidepressat drugs (TCAs and MAOIs) to facilitate monoaminergic transmission and of drugs as Reserpine to cause depression.
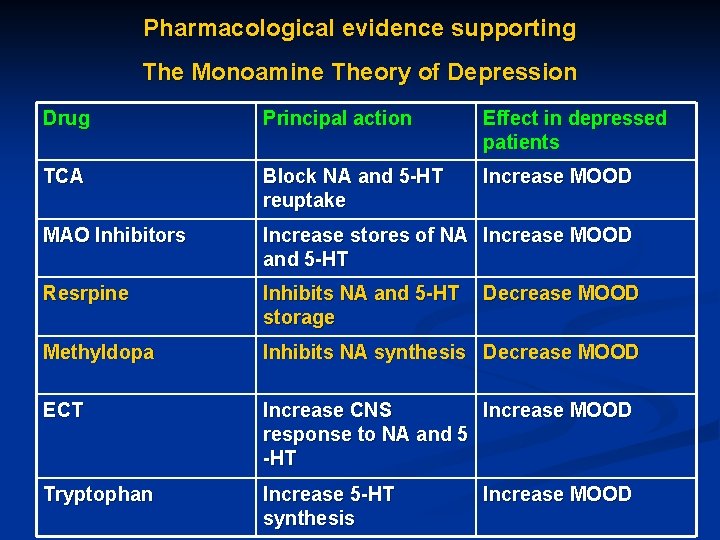
Pharmacological evidence supporting The Monoamine Theory of Depression Drug Principal action Effect in depressed patients TCA Block NA and 5 -HT reuptake Increase MOOD MAO Inhibitors Increase stores of NA Increase MOOD and 5 -HT Resrpine Inhibits NA and 5 -HT storage Methyldopa Inhibits NA synthesis Decrease MOOD ECT Increase CNS Increase MOOD response to NA and 5 -HT Tryptophan Increase 5 -HT synthesis Decrease MOOD Increase MOOD
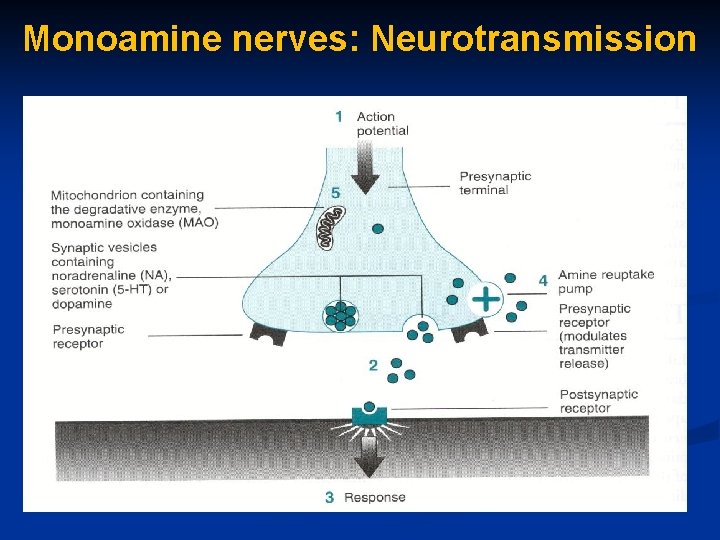
Monoamine nerves: Neurotransmission
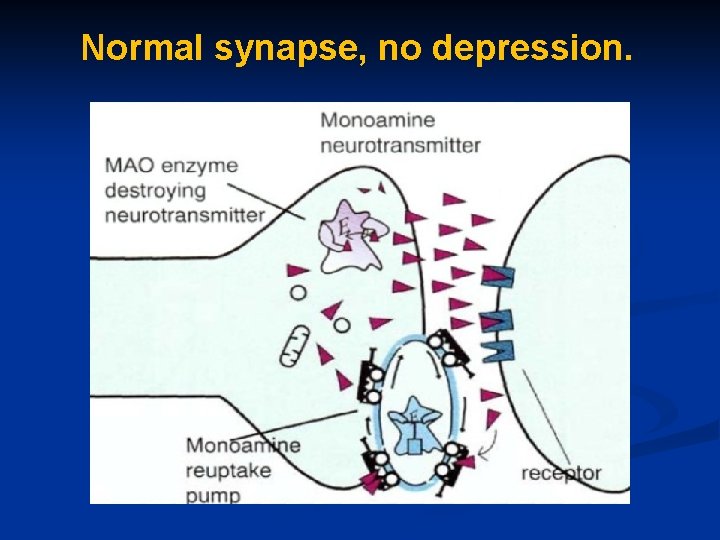
Normal synapse, no depression.
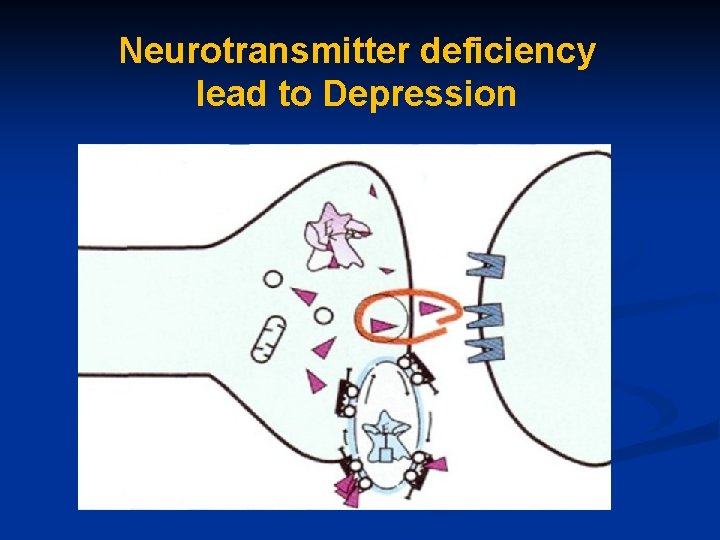
Neurotransmitter deficiency lead to Depression

5 -HT deficiency may cause the sleep problems, irritability and anxiety associated with depression n Decreased level of NE, which regulates mood, alertness, arousal, appetite, reward & drives, may contribute to the fatigue and depressed mood of the illness n However, dopamine is important for pleasure, sex & psychomotor activity n

Treatment of Depression 1. Psychological treatment 2. Pharmacological treatment 70 % of depressed patients respond to antidepressants 3. ECT ( electroconvulsive therapy) for very severe depression, which has not responded to other treatments or for patients who cannot take antidepressants

Pharmacotherapy

Sites of Action for Antidepressants 1 - Monoamine (NE or/ and 5 -HT) re-uptake pump inhibitors 2 - Blockade of pre-synaptic a 2 receptors 3 - Inhibition of MAO enzyme

Antidepressants n Antidepressants do not act immediately (show clinical effects after 2 weeks) indicating that secondary adaptive changes in the brain are important. n The most consistent adaptive change seen with antidepressant drugs is the downregulation of beta-, alpa-2 and 5 -HT 2 receptors. Alpha-1 is not affected. n Affect only people who are depressed. n Effect does not increase with increasing doses. n Antidepressants are not habit-forming. n Antidepressants differ widely in side effects.

Classification of Antidepressants 1) Tricyclics (TCAs) and Tetracyclics Imipramine Doxepin Desipramine Amoxapine Trimipramine Maprotiline Clomipramine Amitriptyline Nortriptyline Protriptyline 2) Monoamine Oxidase Inhibitors (MAOIs) Tranylcypramine Phenelzine Moclobemide 3) Selective Serotonin Reuptake Inhibitors (SSRIs) Fluoxetine Sertraline Fluvoxamine Paroxetine Citalopram Escitralopram

Classification of Antidepressants 4) Serotonin and Norepinephrine Reuptake Inhibitor (SNRI) Venlafaxine Duloxetine 5) Serotonin-2 Antogonist and Reuptake Inhibitors (SARIs) Nefazodone Trazodone 6) Norepinephrine and Dopamine Reuptake Inhibitor (NDRI) Bupropion 7) Noradrenergic and Specific Serotonergic Antidepressant (Na. SSAs) Mirtazapine 8) Noradrenaline Reuptake Inhibitor (NRI) Reboxetine 9) Serotonin Reuptake Enhancer Tianeptine

TRICYCLIC ANTIDEPRESSANTS (TCAs) • TCAs are the oldest class of antidepressant drugs • They have characteristic threering nucleus • The first TCAs discovered was Imipramine (Tofranil)

TRICYCLIC ANTIDEPRESSANTS (TCAs) Imipramine n Clomipramine n Nortriptyline n Trimipramine n Desipramine Amitriptyline Doxepin TETRACYCLIC ANTIDEPRESSANTS n Maprotiline n Amoxapine

MECHANISM OF ACTION of TCAs: • All tricyclics block reuptake pumps for both Ø Ø 5 HT and NE in nerve terminals by competing for binding site of the transport protein So ↑ conc. of NE & serotonin in the synaptic cleft & at the receptor site Facilitation of NE & serotonin transmission ---improves symptoms of depression • Some have more potency for inhibition of 5 HT uptake pump; clomipramine, imipramine, amitryptyline • Others have more potency for inhibition of NE uptake pump: nortriptyline, desipramine
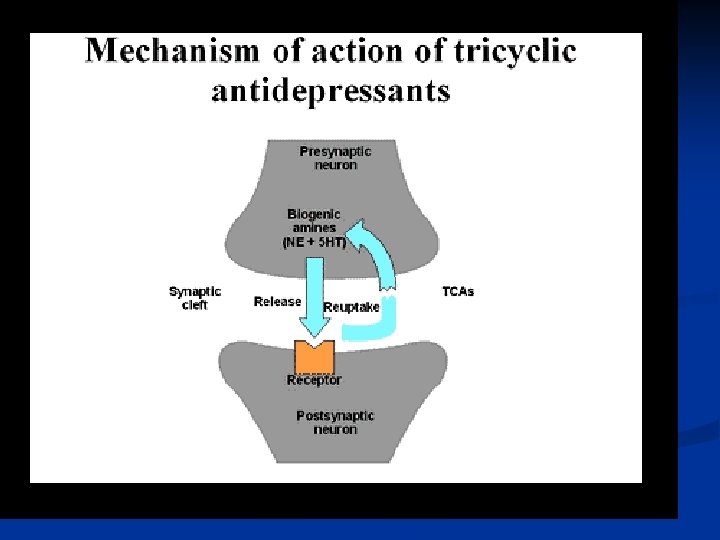

MOA of TCAs Blocking of receptors TCAs also block : n Serotonergic receptors n Alpha adrenergic receptors n Histaminic receptors n Muscarinic receptors n Their role in therapeutic benefit is not known n These actions produce the adverse effects n

PHARMACOLOGICAL ACTIONS 1 - Elevate mood 2 - Improve mental alertness 3 - Increase physical activity # The antidepressant effect may develop after several weeks of continued treatment ( 2 - 3 weeks) 4 - In non-depressed patients They cause sedation, confusion & motor incoordination

PHARMACOLOGICAL ACTIONS The reuptake block occurs quickly but antidepressant effect develops after weeks. n Amine reuptake block by tricyclics initiates a series of time-dependent changes that culminate in antidepressant effect. n Certain adaptive changes occur in receptors. n

Receptor changes n Initially presynaptic α 2 & 5 HT 1 receptors are activated n Later on desensitized / down regulated n Other adaptive changes also occur n Net effect is enhanced NE & serotonin transmission

PHARMACOKINETICS of TCAs n Peak levels: 2 -6 hours post ingestion • TCAs are "lipophilic" in nature, therefore they are well absorbed from the GIT and readily cross the blood brain barrier to penetrate the CNS. n Elimination: hepatic oxidation • TCAs are metabolized in the liver by demethylation (Imipramine to Desipramine, Amitriptyline to Nortriptyline) and by hydroxylation into metabolites that retain the biological activity of the parent compounds.

PHARMACOKINETICS of TCAs • TCAs are strongly bound to plasma proteins. n n Average t 1/2: 24 hours Up to 72 hours in overdose Large T 1/2 and large VD because TCA extensively bound to plasma protein (90 -95 %)

Therapeutic uses of TCAs n n n n Endogenous (Major) Depression -- moderate to severe. Panic attack /acute episode of anxiety. Imipramine is used for treatment of nocturnal enuresis in children and geriatric patients as it constricts internal urethral sphincter ( anti-muscarinic effect). Generalized Anxiety Disorder (GAD). Obsessive Compulsive Disorder (OCD) Attention Deficit Hyperkinetic Disorder (ADHD). Chronic neuropathic pains or Unexplained body pains.

Side Effects of TCAs block: - α 1 adrenergic receptors - H 1 histamines receptors - M 1 cholinergic receptors - 5 HT 2 receptors
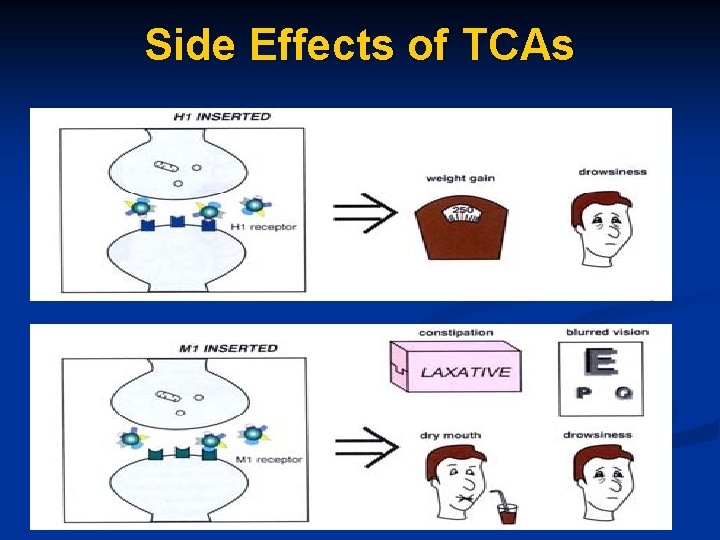
Side Effects of TCAs
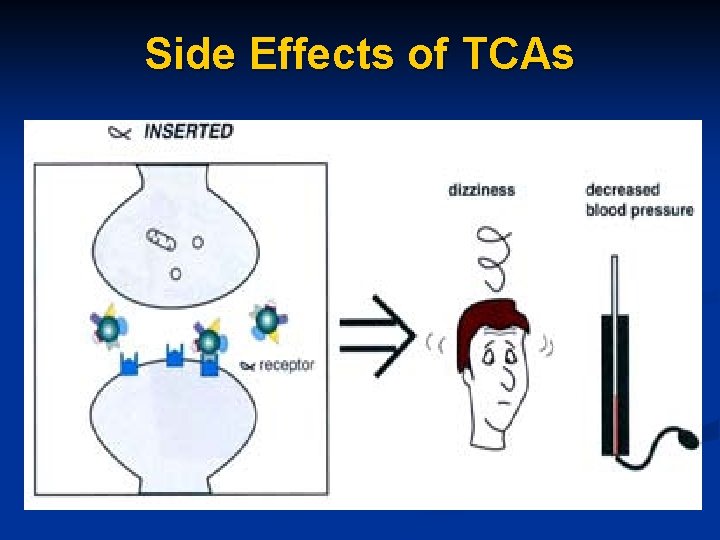
Side Effects of TCAs

Side effects of TCAs n Four major toxic effects (A, C, S, D) A = Anticholinergic C = Cardiovascular S = Seizures D = Death

ANTICHOLINERGIC EFFECTS Sedation, Delirium, coma n Tachycardia n Mydriasis n Dry mucous membranes and skin n Dry mouth n Decreased or absent bowel sounds n Constipation n Urinary retention n

CARDIOVSCULAR EFFECTS 1 - Inhibit neuronal catecholeamines reuptake leading to Cardiac arrhythmias 2 - Inhibit alpha-adrenergic receptors induces vasodilatation & Postural Hypotension 3 - Membrane Depressant (quinidine like) effects cause myocardial depression and cardiac conduction disturbance due to: * Sodium channel blockade * Potassium channel blockade

SEIZURES * Seizures occur as a result of inhibition of reuptake of Norepinepherine and serotonin in the brain. • TCAs lower the seizure threshold. • The muscular hyperactivity from seizures combined with decreased sweating can lead to severe HYPERTHERMIA.

Death Sudden Death Occurs from: 1 - Ventricular fibrillation 2 - Status Epilepticus 3 - Hyperthermia

Interaction of TCA with other drugs q TCA are strongly bound to plasma protein, therefore their effect can be potentiated by drugs that compete for their plasma protein binding site ( Aspirin and Phenylbutazone). q TCAs are metabolized by liver microsomal enzymes, therefore their effect can be reduced by inducers of liver microsomal enzymes (Barbiturates), or potentiated by inhibitors of liver microsomal enzymes (Oral contraceptives, Antipsychotics, and SSRIs). q TCA (inhibitors of monoamine reuptake) should not be given with MAOIs (inhibitors of monoamine degradation) "hypertensive crisis".

Contraindications q TCAs should not be used in patients with Glaucoma or with enlarged prostate because of their atropine-like action. q TCAs (given alone) are contraindicated in manic-depressive illness, because they tend to "switch" the depressed patient to the "manic" phase, therefore, they should be combined with "lithium salts".

Monoamine Oxidase Inhibitors Amongst the first Antidepressants n Include: - Phenelzine - Tranylcypromine - Isocarboxazid - Moclobemide - Pargyline Ø Onset of antidepressant effect is delayed for 2 -4 weeks. n

Monoamine Oxidase n MAO is found in nearly all tissues and is located intracellularly associated with mitochondria. n Present in nerve terminals that release NA, DA or 5 HT. n Located on outer surface of mitochondrial membranes. n In neurons, MAO oxidatively deaminates and inactivates any excess norepinephrine, serotonin and dopamine, that may leak out of synapstic vesicles. n MAO is not involved in the inactivation of released transmitter
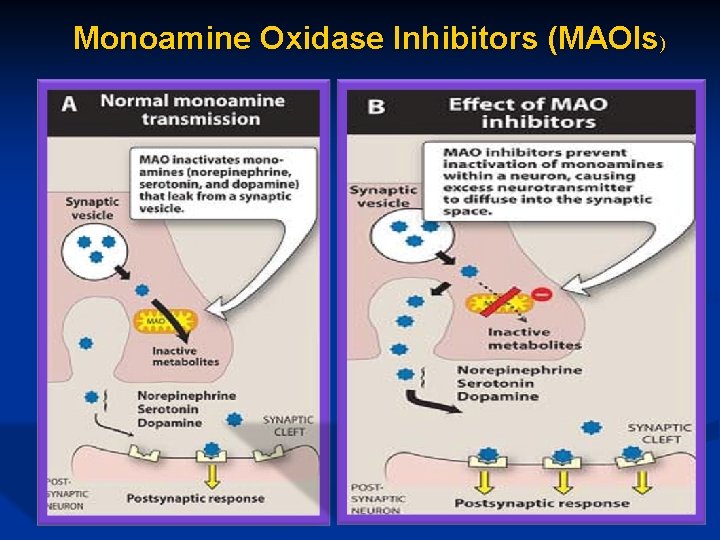
Monoamine Oxidase Inhibitors (MAOIs)

MAO Enzyme MAO exists in tow forms coded by separate genes n MAO-A: Metabolizes norepinephrine, serotonin and tyramine. Inhibition of MAO-A produces Antidepressant effect. n MAO-B: specific for dopamine. Inhibition of MAO-B produces Anti-parkinsonian effect.

Monoamine Oxidase Inhibitors (MAOIs) 1 - Irreversible and nonselective MAOIs (Classic MAOI) n Phenelzine n Tanylcypromine n Isocarboxazid n pargyline - Can not distinguish between the two isoenzymes - MAO-A and B enzyme activity can not be restored unless new enzyme is synthesized, therefore the effect of MAOIs persists for a period of 2 -3 weeks after stopping treatment, where a new (fresh) enzyme has to be synthesized

2 -Reversible and selective inhibitors of MAO-A: - Moclobemide (antidepressant action, Short acting) 3 - Selective inhibitor of MAO-B: - Deprenyl (neurodegenerative disorder) - Selegiline (used in the treatment of Parkinsonism)

Side Effects of MAOIs 1 - Hypotension: After MAO inhibition, other amines such as dopamine are able to accumulate in peripheral sympathetic nerve terminals and displace vesicular NA, thus reducing NA release and sympathetic activity (sympathetic block). 2 - Antimuscarinic effects (atropine-like sideeffects): Dry mouth blurred vision Urinary retention

Side Effects of MAOIs 3 - CNS stimulation: Insomnia Tremors Excitement Convulsions 4 - Weight gain associated with increased appetite :

Drug interactions of MAOIS 1 - Pethidine: MAOIs interact with the opioid receptor agonist (pethidine) which may cause severe hyperpyrexia, restlessness, coma, hypotension. The mechanism still unclear – but it is likely that an abnormal pethidine metabolite is produced because of inhibition of normal demethylation pathway. 2 - Levodopa: precursor of dopamine can interact with MAOIs leading to hypertensive crisis.

Drug interactions of MAOIs 3 - Amphetamine and Ephedrine: Indirectly acting sympathomimetics can interact with MAOIs causing the liberation of accumulated monoamines in neuronal terminals leading to hypertensive crisis. 4 -TCAs (inhibitors of monoamine reuptake) can interact with MAOIs (inhibitors of monoamine degradation) leading to hypertensive crisis. 5 - MAOIs & SSRIs ------- Serotonin syndrome.

MAOIs interaction with tyramine ‘cheese reaction’ This occurs when Tyramine rich foods are taken with MAOIs. q Tyramine rich foods include Old cheese , Concentrated yeast products, Pickled or smoked fish, Red beans, Red Wine, Chicken liver, Sausages. q Tyramine in food is normally degraded in the gut by MAO-A. q

Since the enzyme is inhibited by MAOIs, tyramine from ingested food is absorbed, and then taken up into adrenergic neurons where it is converted into octopamine - a false transmitter which causes massive release of NE and may result in hypertensive crisis ; severe hypertension, severe headache and fatal intracranial haemorrhage. q Treatment : Prazocin or phentolamine q N. B. At least 10 mg tyramine needs to be ingested to produce this reaction. q The special advantage claimed for Moclobemide. is that, No cheese reaction occurs with its use. q

Therapeutic uses of MAOIs Considered to be the last –line agents due to Drug / Food interactions 1. In endogenous depression, specially patients non responsive / allergic to TCAs 2. Atypical depression 3. Phobic states
Selective 5 -HT reuptake inhibitors (SSRIs) - Fluoxetine (prozac) - Paroxetine - Sertraline - Citalopram - Escitalopram Fluvoxamine

Selective Serotonin Reuptake Inhibitors n The SSRIs are currently the most widely utilized class of antidepressants in clinical practice. n They act within the brain to increase the amount of the neurotransmitter, serotonin (5 -hydroxytryptamine or 5 -HT), in the synaptic gap by inhibiting its re-uptake. n SSRIs are described as 'selective' because they affect only the reuptake pumps responsible for serotonin, as opposed to earlier antidepressants, which affect other monoamine neurotransmitters as well. Because of this, SSRIs lack some of the side effects of the more general drugs.
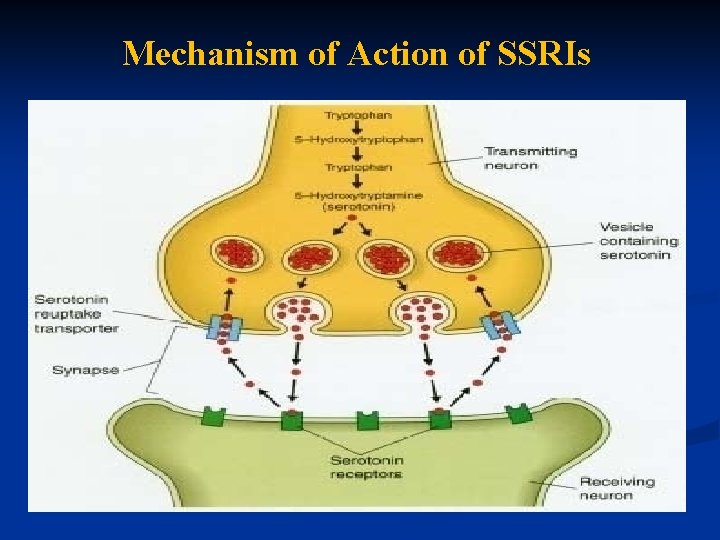
Mechanism of Action of SSRIs .
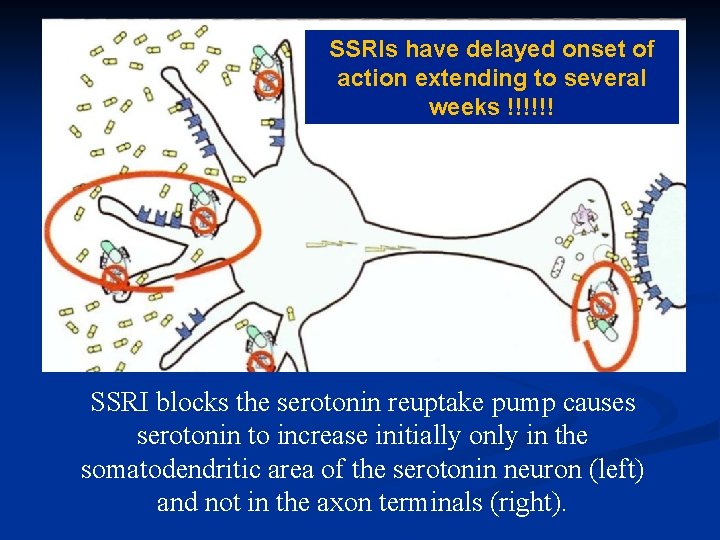
SSRIs have delayed onset of action extending to several weeks !!!!!! SSRI blocks the serotonin reuptake pump causes serotonin to increase initially only in the somatodendritic area of the serotonin neuron (left) and not in the axon terminals (right).
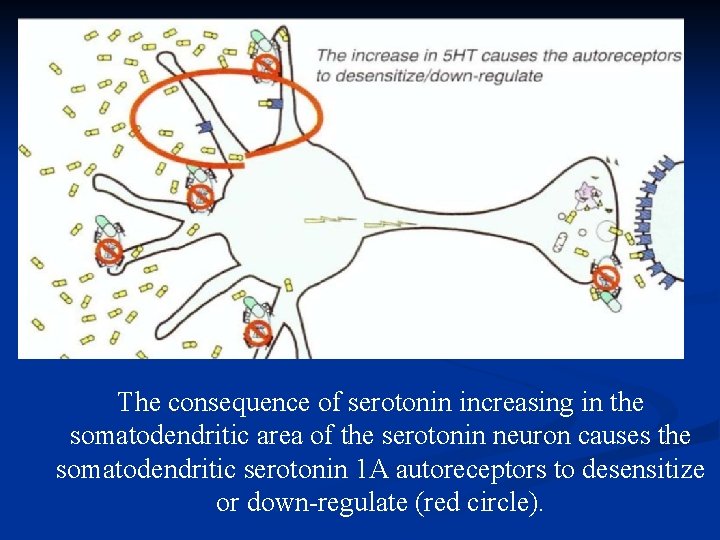
The consequence of serotonin increasing in the somatodendritic area of the serotonin neuron causes the somatodendritic serotonin 1 A autoreceptors to desensitize or down-regulate (red circle).
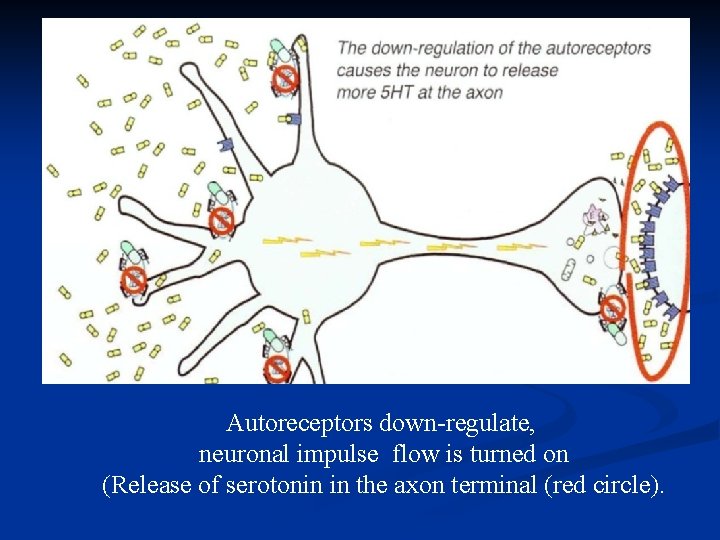
Autoreceptors down-regulate, neuronal impulse flow is turned on (Release of serotonin in the axon terminal (red circle).

• SSRIs have delayed onset of action extending to several weeks • This delay is the result of the time it takes for somatodendritic serotonin to down-regulate the serotonin 1 A autoreceptors and turn on neuronal impulse flow in the serotonin neuron. • This delay may explain why antidepressants do not relieve depression immediately.

Fluoxetine (Prozac) n The body eliminates Fluoxetine very slowly. The half-life of fluoxetine after a single dose is 2 days and after multiple dosing 4 days. n The liver then metabolizes fluoxetine into norfluoxetine, a desmethyl metabolite, which is also a serotonin reuptake inhibitor. n Norfluoxetine has an even longer half-life, i. e. 8. 6 and 9. 3 days for single and repeated dosage respectively. n Because fluoxetine's metabolism involves the P 450 IID 6 system, concomitant therapy with drugs also metabolized by this enzyme system (such as the tricyclic antidepressants) may lead to drug interactions. n Fluoxetine is approved for use in children & adolescence, is relatively safe in pregnancy.

Sertraline (Zoloft) n Sertraline HCl is a selective serotonin reuptake inhibitor (SSRI) for oral administration. It is chemically unrelated to other SSRIs, tricyclic, tetracyclic, or other available antidepressant agents. n The mechanism of action of sertraline is presumed to be linked to its inhibition of CNS neuronal uptake of serotonin (5 HT). n One property of sertraline is that it appears to be also a minor inhibitor of dopamine reuptake.

Selective Serotonin Reuptake Inhibitors n Advantages - The Most commonly prescribed antidepressants - Lacks cardiovascular and anticholinergic side effects compared to TCA - In contrast to MAOI, they do not cause ‘cheese’ reaction - Safer (low risk of overdose) - Acute toxicity is less than that of MAOI or TCA

Adverse effects of SSRIs: n n n GIT symptoms: Nausea vomiting & diarrhea. Changes in appetite ---weight loss/ gain. Sleep disturbances: Drowsiness with Fluvoxamine. Anxiety & Tremors. Sexual dysfunction: Loss of libido , delayed ejaculation. Discontinuation syndrome: n Symptoms are headache , malaise & flu like symptoms, agitation , irritability & nervousness

Therapeutic Uses of SSRIs Same as for TAC, in addition effective in the following conditions n Depression. n Anxiety Disorder. n n n Eating disorders- bulimia nervosa (fluoxetine). Post traumatic stress disorder. Premenstrual dysphoric disorder. Attention Deficit Hyperkinetic Disorder. Treatment of premature ejaculation.

Drug interactions of SSRIs • SSRIs are potent inhibitors of liver microsomal enzymes. Therefore they should not be used in combination with TCAs because they can inhibit their metabolism increasing their toxicity. • SSRIs should not be used in combination with MAOIs because of the risk of life-threatening "serotonin syndrome" (tremors, hyperthermia, cardiovascular collapse and death). Both drugs require a "washout" period of 6 weeks before the administration of the other.

NE Selective Reuptake Inhibitors (NRIs) Reboxetine Tomoxetine n Selective to NE uptake n May be more effective in noradrenaline deficiency syndrome (e. g. , depression associated with fatigue, apathy, cognitive disturbances), or non responders to SSRIs. n Also act at presynaptic α 2, postsynaptic α 1, α 2 and β adrenergic receptors (tremor, agitation, blood pressure). Advantages n n Lacks antagonistic activity at histamine H 1, muscarinic & adrenergic receptors or Na+ pump as with TCA. Fewer unwanted cardiovascular effects than TCA’s.

Serotonin and Noradrenaline Reuptake Inhibitors (SNRIs) n Serotonin norepinephrine reuptake inhibitors (SNRIs) are a class of antidepressant used in the treatment of clinical depression and other affective disorders. n They act upon two neurotransmitters in the brain that are known to play an important part in mood, namely, 5 HT and NE. This can be contrasted with the more widely-used selective serotonin reuptake inhibitors (SSRIs), which act only on serotonin.

Serotonin and Noradrenaline Reuptake Inhibitors (SNRIs) n SNRIs were developed more recently than SSRIs, and there are relatively few of them. Their efficacy as well as their tolerability appears to be somewhat better than the SSRIs, owing to their compound effect. n These new drugs, because of their specificity for the serotonin and norepinephrine reuptake proteins, lack most of the adverse side effects of TCAs and MAOIs.

Serotonin and Noradrenaline Reuptake Inhibitors (SNRIs) Venlafaxine • It is used primarily for the treatment of depression, generalized anxiety disorder, and social anxiety disorder in adults. Venlafaxine is the first and most commonly used SNRI. • Selective 5 HT and NE uptake blockers Combines the action of SSRI and NRI. • Causes dual action on serotonin and adrenergic systems, thus amplifying these two systems synergistically. • But without α 1, M 1 cholinergic or H receptor blocking properties. Venlafaxine

Venlafaxine Side Effects n Because of its relatively short half-life of 4 hours, Effexor should be administered in divided dosages throughout the day. n Side effects may include nausea, dizziness, sleepiness, abnormal ejaculation, sweating, dry mouth, gas or stomach pain, abnormal vision, nervousness, insomnia, loss of appetite, constipation, confusion/agitation, tremors, and drowsiness.

Norepinephrine and Dopamine Reuptake Inhibitor (NDRI) n n These are a class of antidepressants that are not really categorized as a special group of antidepressants. The only antidepressant in this group is Bupropion (Wellbutrin), which is an antidepressant of the aminoketone class, chemically unrelated to tricyclics or SSRIs.

Bupropion n Bupropion is a selective catecholamine (norepinephrine and dopamine) reuptake inhibitor. It has only a small effect on serotonin reuptake. It does not inhibit MAO. Bupropion is metabolised in the liver. It has at least three active metabolites; hydroxybupropion, threohydrobupropion and erythrohydrobupropion. These active metabolites are further metabolised to inactive metabolites and eliminated through excretion into the urine. Partial agonist at 5 -HT type IA receptors (decrease 5 HT activity ) but enhances dopaminergic and noradrenergic activity

Bupropion Advantages and Side Effects Advantages n Sexual side effects normally accompanying SSRI's do not accompany bupropion. Interestingly, patients commonly report increased libido, perhaps evidence of its dopaminergic properties. No weight gain, loss of appetite. n Common side effects n Dry mouth, tremors, anxiety, agitation, dizziness, headache, excessive sweating, increased risk of seizures and insomnia.

Therapeutic Uses of Bupropion n Major depression. Bupropion is useful in ADHD. Bupropion also helps in reducing craving & attenuating the withdrawal symptoms for Nicotine in tobacco users trying to quit smoking.

Serotonin-2 A Antagonist and Reuptake Inhibitors (SARI) Trazodone Nefazodone n Blocks 5 HT uptake selectively but in a less potent manner than tricyclics. This helps reduces depression. n However, they are powerful 5 HT 2 A antagonists, blockade of 5 HT 2 A receptors stimulates 5 HT 1 A receptors, which may help reduce depression. n 5 HT 2 A antagonism also reduces the risk of anxiety, sedation or sexual dysfunction which is normally associated with SSRIs.

Noradrenergic and specific Serotonergic Antidepressant (Na. SSA) Mirtazapine - α 2 receptor antagonist - Increase NE and 5 HT levels - Blocks 5 HT 2 A, 5 HT 3 and thus reduces side effects of anxiety, and sexual dysfunction n Blocking 5 HT 2 C, and H 1 receptors cause side effects: sedation, and weight gain.

Electroconvulsive Therapy n n Stimulation through electrodes placed on either side of the head with the patient anaesthetized, paralysed with a NMB drugs to avoid physical injury and artificially ventilated Response rates 60 -80 % The most effective treatment for severe suicidal depression DISADVANTAGES Confusion, Memory loss lasting for days or weeks

Antimanic agents or Mood Stabilizers

Antimanic drugs Anti-manic drugs or mood stabilizers are used in the treatment of mania both to control acute attacks and to prevent their recurrence n For bipolar disorder n In mood cycling, but are not effective in treating depression n Treatment of some cases of schizophrenia n
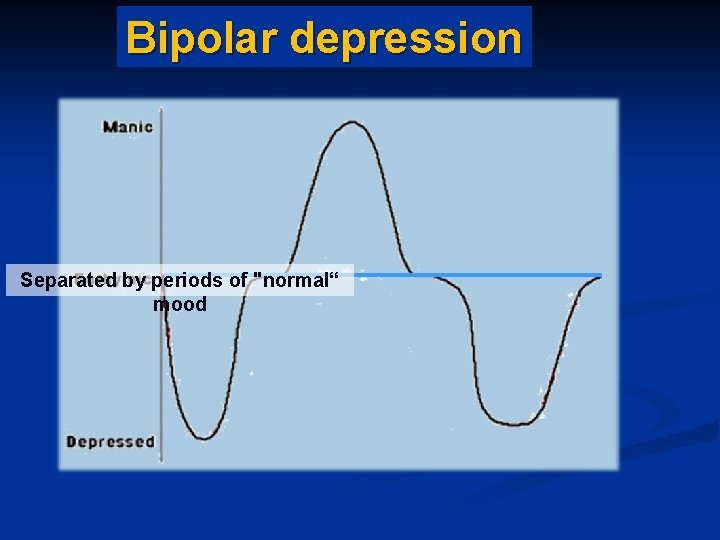
Bipolar depression Separated by periods of "normal“ mood
![Antimanic drugs 1 - Lithium salts: Lithium carbonate 2 - Anticonvulsants n Carbamazepine [Tegretol] Antimanic drugs 1 - Lithium salts: Lithium carbonate 2 - Anticonvulsants n Carbamazepine [Tegretol]](http://slidetodoc.com/presentation_image_h/f7c5239deb7723b1e3fed2a19ba90d26/image-85.jpg)
Antimanic drugs 1 - Lithium salts: Lithium carbonate 2 - Anticonvulsants n Carbamazepine [Tegretol] n Valproic acid [Depakote] n Lamotrigine [Lamictal]

Antimanic drugs 3 - Atypical antipsychotics n Olanzapine n Risperidone n Clozapine 4 - Benzodiazepines (BZs)

Lithium ion, Li+, is the oldest and best known mood stabilizing drug v Lithium salts (carbonate, citrate) are the most commonly prescribed v 60 -80% success in reducing acute manic and hypomanic states v It reduces the risk of suicide related to bipolar disorder v

Lithium: Therapeutic uses 1 - Prophylaxis and treatment of mania 2 - Prophylaxis of and maintenance treatment of bipolar disorders 3 - Lithium augmentation Prophylaxis of recurrent depression in unipolar depression and schizophrenic patients who don't respond to treatment

Proposed Mood Stabilising Mechanism of Action of Lithium Salts Neurotransmitter Lithium carbonate IP 3 formation Signalling events involving other receptors Receptor X Hormone-induced c. AMP production (but not thought to be a significant mechanism in brain)
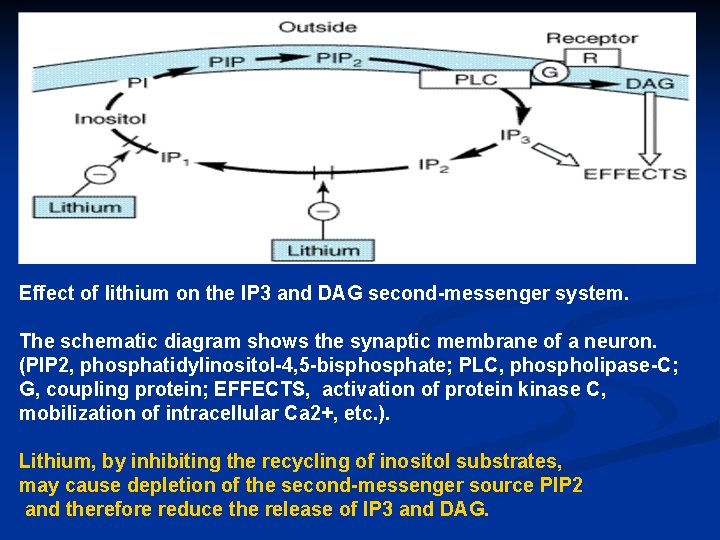
Effect of lithium on the IP 3 and DAG second-messenger system. The schematic diagram shows the synaptic membrane of a neuron. (PIP 2, phosphatidylinositol-4, 5 -bisphosphate; PLC, phospholipase-C; G, coupling protein; EFFECTS, activation of protein kinase C, mobilization of intracellular Ca 2+, etc. ). Lithium, by inhibiting the recycling of inositol substrates, may cause depletion of the second-messenger source PIP 2 and therefore reduce the release of IP 3 and DAG.

Pharmacokinetics n n n n Completely absorbed from GIT Long plasma half-life (20 hr) Not bound to plasma proteins Not metabolized in the body Distributed in all body fluids Slow entry into intracellular compartment. Its concentration can be detected in plasma, saliva, urine

Pharmacology of Lithium Salts n n no effect in normal person stabilizes mood in affective disorder low therapeutic index toxicity: correlated with plasma concentration; fine tremors, ataxia, confusion, delirium, convulsions, cardiac arrhythmias treatment should be under normal Na+ intake and normal cardiac and renal function

Lithium Carbonate n Lithium is clinically effective at plasma concentration of 0. 5 -1 m. M. n Above 1 mm, it produces a variety of toxic effects, therefore, monitoring of plasma concentration is essential

n After the drug is started, 7 -10 day must be elapsed before the antimanic effect is reached. n Lithium causes depletion of membrane phosphatidylinositol and accumulation of intracellular inositol phosphate. n Hormone-mediated c. AMP production is reduced.

Lithium Carbonate Adverse effects n Anorexia , diarrhoea , hypothyroidism , seizures (Convulsion and death if plasma concentration reaches 3 -5 Mm). n Leukocytosis , nephrotic syndrome and polyuria , impotence. n A toxic drug ; adverse reactions are dose-and concentration-dependent.

Renal Adverse Effects n Polydipsia and polyuria are frequent but reversible concomitants of lithium treatment, occurring at therapeutic serum concentrations. n The principal physiologic lesion involved is loss of the ability of the collecting tubules to conserve water under the influence of antidiuretic hormone, resulting in excessive free water clearance.

Renal Adverse Effects n Edema is a frequent adverse effect of lithium treatment and may be related to some effect of lithium on sodium retention. n Patients receiving lithium should avoid dehydration and the associated increased concentration of lithium in urine. Periodic tests of renal concentrating ability should be performed to detect changes.

Cardiac Adverse Effects q The bradycardia-tachycardia "sick sinus”syndrome is a definite contraindication to the use of lithium because the ion further depresses the sinus node. T wave flattening is often observed on the ECG but is of questionable significance q Enlargement of thyroid gland with decreased function (hypothyroidism)

Use During Pregnancy q Lithium is transferred to nursing infants through breast milk, in which it has a concentration about one-third to one-half that of serum. Lithium toxicity in newborns is manifested by lethargy, cyanosis, poor suckling and perhaps hepatomegaly. q The issue of dysmorphogenesis is not settled but the most recent data suggest that lithium carries a relatively low risk of teratogenic effects.

Drug Interactions n Renal clearance of lithium is reduced about 25% by thiazide diuretics (hydrochlorothiazide, chlorothiazide) and doses may need to be reduced by a similar amount. n A similar reduction in lithium clearance has been noted with several of the newer nonsteroidal antiinflammatory drugs that block synthesis of prostaglandins (Ibuprofen, Indomethacin). This interaction has not been reported for either aspirin or acetaminophen. n All neuroleptics tested to date, with the possible exception of clozapine and the newer antipsychotics, may produce more severe extrapyramidal syndromes when combined with lithium.

Anticonvulsant Mood Stabilizing Agents 1 - Carbamazepine 2 - Valproic acid 3 - Lamotrigine

Carbamazepine Therapeutic uses: As mood stabilizer, carbamazepine is superior to Li+ for rapid-cycling (bipolar) n Second-line treatment for mania n Drug of choice in partial seizures & Tonic-clonic seizures n

Carbamazepine: mechanism of action Ø Blockade of voltage-dependent sodium channels (↓cell excitability, suppresses neuronal firing) Attenuates glutamate (excitatory)

Carmabazepine: Side effects q GIT upset, sedation, ataxia q Induction of hepatic P 450 : efficacy of other drugs e. g. failure of oral contraceptive pills, oral anticoagulants “warfarin” q Severe bone marrow depression (agranulocytosis , aplastic anemia) • Therapeutic drug monitoring is required

Valproic acid: Mechanism of action It acts by several mechanisms Blockade of Na+ channels Potentiation of GABA (increasing synthesis and release) Blocks T-type Ca 2+ channels

Valproic acid n n Valproic acid has been effective in some patients who have failed to respond to lithium. Preferred over lithium for initial therapy but lithium is still preferred for maintenance treatment Combinations of valproic acid with other psychotropic medications likely to be used in the management of either phase of bipolar illness are generally well tolerated. Many clinicians argue for combining valproic acid and lithium in patients who do not fully respond to either agent alone.
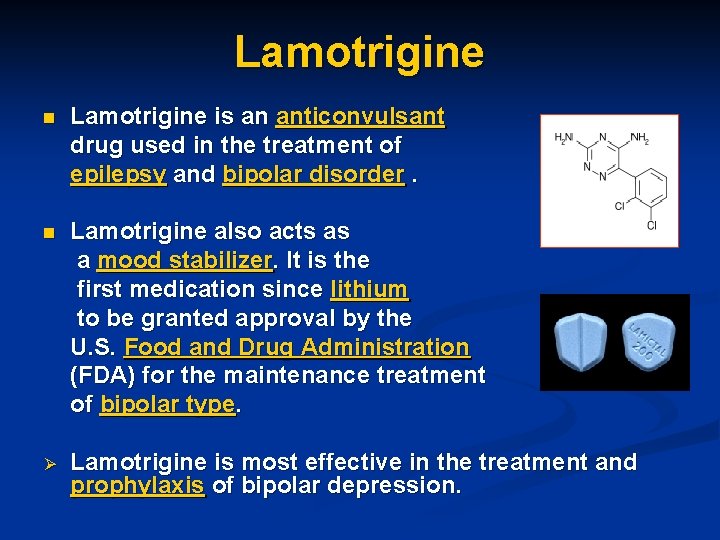
Lamotrigine n Lamotrigine is an anticonvulsant drug used in the treatment of epilepsy and bipolar disorder. n Lamotrigine also acts as a mood stabilizer. It is the first medication since lithium to be granted approval by the U. S. Food and Drug Administration (FDA) for the maintenance treatment of bipolar type. Ø Lamotrigine is most effective in the treatment and prophylaxis of bipolar depression.

Mechanism of action n n One proposed mechanism of action for lamotrigine involves an effect on sodium channels, although this remains to be established in humans. In vitro pharmacological studies suggest that lamotrigine inhibits voltage-sensitive sodium channels, thereby stabilizing neuronal membranes and consequently modulating presynaptic transmitter release of excitatory amino acids (for example glutamate and aspartate).

Pharmacokinetic data Bioavailability n Protein binding n Metabolism n Half life Excretion n 98% 55% Hepatic 24 -34 hours Renal

Side effects n Lamotrigine prescribing information has a black box warning about life threatening skin reactions, including Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis. The manufacturer states that nearly all cases appear in the first 2 to 8 weeks of therapy and if medication is suddenly stopped then resumed at the normal dosage. Patients should seek medical attention for any unexpected skin rash as its presence is an indication of a possible serious or even deadly side effect of the drug. n Lamotrigine binds to melanin-containing tissues such as the iris of the eye. The long-term consequences of this are unknown.

Atypical Antipsychotics Some atypical antipsychotics have mood stabilizing effects and are thus commonly prescribed even when psychotic symptoms are absent n Risperidone is approved for the treatment of bipolar disease n Olanzapine is approved for acute mania associated with bipolar disorder. n Clozapine is effective but have potential serious side effects ( Agranulocytosis)

Atypical Antipsychotics n Mechanism v All of action antipsychotic drugs block D 2 receptors in the brain & periphery. v Atypical antipsychotics exert part of their action through blocking of 5 HT 2 A receptors.

Benzodiazepines: in acute mania Potentiate GABAergic neurotransmission in CNS. n Diazepam : In state of extreme mood elevation. n Gives rapid sedation. n Useful until the effects of Lithium take place. n

Thank You
- Slides: 114