Pheochromocytoma Wendy Blount DVM Pheochromocytoma Uncommon tumor of

Pheochromocytoma Wendy Blount, DVM

Pheochromocytoma • Uncommon tumor of the chromaffin cells in the adrenal medulla • Occasionally can arise from chromaffin cells outside the adrenal gland • Right adrenal more common than left – Bilateral has been reported • • Most are malignant and functional Produce catecholamines – – – Epinephrine Norephinephrine Dopamine (rare)

Pheochromocytoma • 40%have metastasized at the time of diagnosis – – – Regional lymph nodes (sublumbar) Liver Lung Bone CNS • Many invade the caudal vena cava – Sometimes when the tumor is not found on ultrasound

Clinical Signs • 60% diagnosed on necropsy • Symptoms can be non-specific and episodic • Malignant hypertension (>95%) - HALLMARK – – – Sustained hypertension with severe episodes (50%) Normotensive between episodes (25%) Stable hypertension (25%) Normotension does not rule out pheochromocytoma Systolic BP can be >300 mm. Hg • Tachyarrhythmia – Panting, nervousness – Exercise intolerance, weakness (62%), collapse (29%)

Clinical Signs • Bleeding diathesis – Hyphema, retinal detachment – Bleeding from the gums – CNS bleed • Abdominal mass (10%) – Palpable mass – Abdominal discomfort • Abdominal effusion – Can present as an acute retroperitoneal or abdominal bleed – Or ascites (pure or modified transudate) due to portal hypertension
Clinical Signs • Tumor thrombus – Caudal vena cava – Ascites – transudate or proteinaceous effusion – Caudal peripheral edema • • PU-PD (29%) Fever Anorexia, weight loss Vomiting, diarrhea, constipation
Labwork • CBC - nonspecific – Anemic if significant bleed – Increased white count – response to tumor • Serology - nonspecific – Liver enzymes usually elevated – Can mimic hyperadrenocorticism • Urinalysis - nonspecific – Poorly concentrated urine – with proteinuria

Cardiac Work-Up • ECG – Sinus tachycardia early on – Catecholamine induced cardiomyopathy leads to life threatening arrhythmias – APCs, VPCs, idioventricular rhythms, 3 rd degree AV block • • Echocardiogram – hypertrophic cardiomyopathy Chest x-rays – Look for metastasis (3 views) – 15% • nodules 3 -5 mm+ – Vet. BLUE® ultrasound – nodules 1 -3 mm+
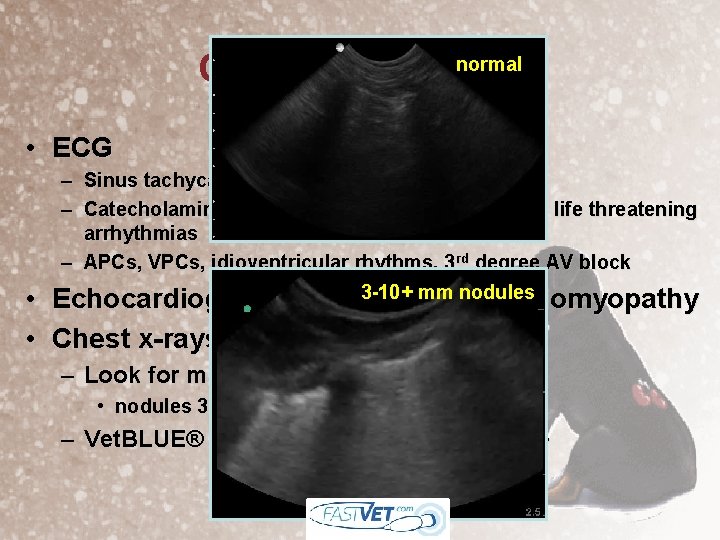
normal Cardiac Work-Up • ECG – Sinus tachycardia early on – Catecholamine induced cardiomyopathy leads to life threatening arrhythmias – APCs, VPCs, idioventricular rhythms, 3 rd degree AV block 3 -10+ mm nodules Echocardiogram – hypertrophic cardiomyopathy • • Chest x-rays – Look for metastasis (3 views) – 15% • nodules 3 -5 mm+ – Vet. BLUE® ultrasound – nodules 1 -3 mm+
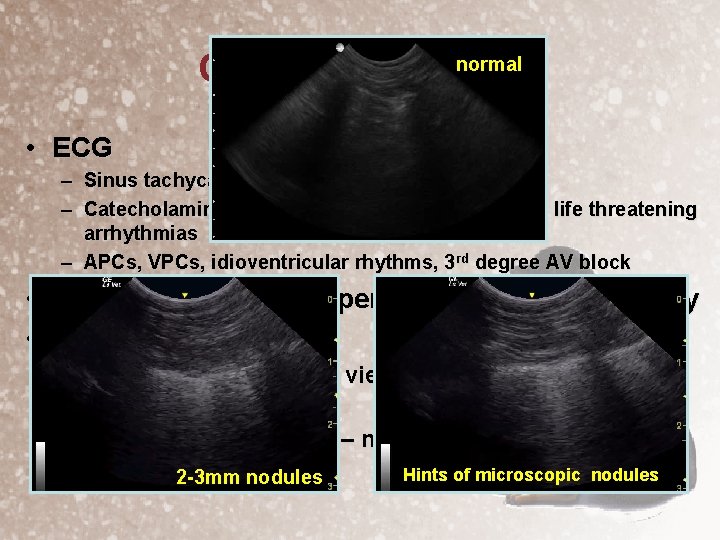
normal Cardiac Work-Up • ECG – Sinus tachycardia early on – Catecholamine induced cardiomyopathy leads to life threatening arrhythmias – APCs, VPCs, idioventricular rhythms, 3 rd degree AV block • • Echocardiogram – hypertrophic cardiomyopathy Chest x-rays – Look for metastasis (3 views) – 15% • nodules 3 -5 mm+ – Vet. BLUE® ultrasound – nodules 1 -3 mm+ 2 -3 mm nodules Hints of microscopic nodules

Abdominal Imaging • Abdominal mass may be seen on radiographs or on ultrasound – Cranial to the kidney(s) • Check caudal vena cava for invasion – 80% sensitivity, 90% specificity – CT 92% sensitivity, 90 -100% specificity • Adrenal(s) may be enlarged with mixed echogenic pattern and effacement of normal architecture (60 -80%) • Normal ultrasound does not rule out pheochromoctyoma
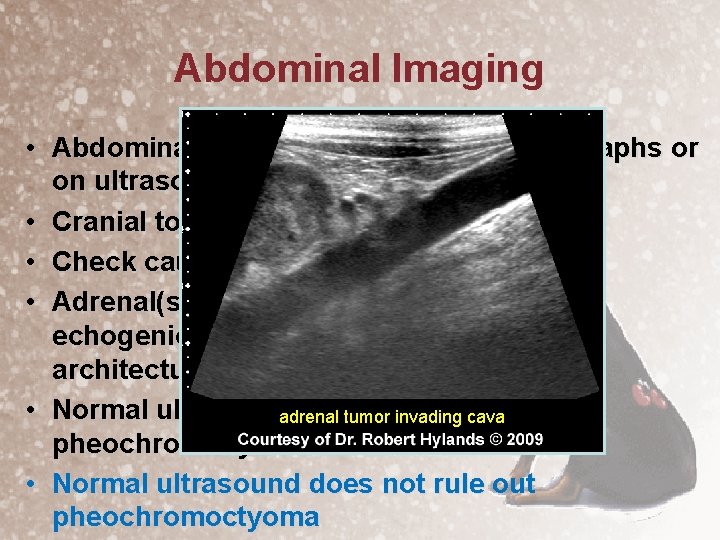
Abdominal Imaging • Abdominal mass may be seen on radiographs or on ultrasound • Cranial to the kidney(s) • Check caudal vena cava for invasion • Adrenal(s) may be enlarged with mixed echogenic pattern effacement of normal architecture (60 -80%) • Normal ultrasound does rule out adrenal tumornot invading cava pheochromocytoma • Normal ultrasound does not rule out pheochromoctyoma
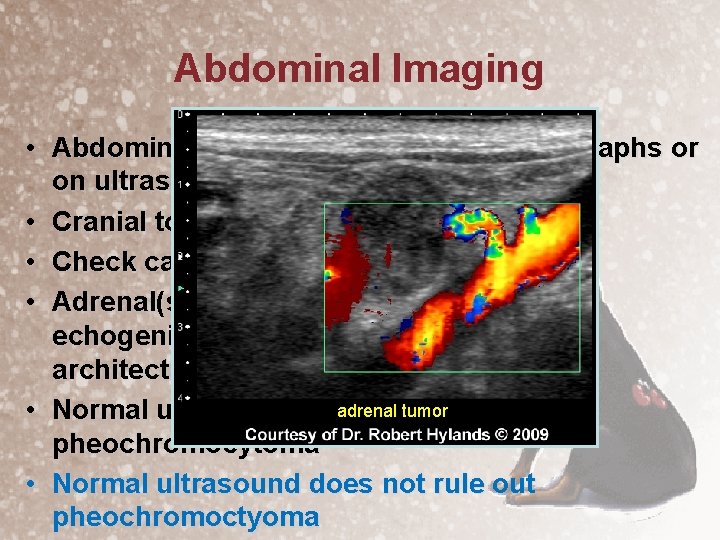
Abdominal Imaging • Abdominal mass may be seen on radiographs or on ultrasound • Cranial to the kidney(s) • Check caudal vena cava for invasion • Adrenal(s) may be enlarged with mixed echogenic pattern effacement of normal architecture (60 -80%) adrenal tumor • Normal ultrasound does not rule out pheochromocytoma • Normal ultrasound does not rule out pheochromoctyoma
Cytology • • FNA of adrenal masses is not highly productive Any adrenal tumor has propensity to bleed Catecholamine storm is possible with pheo Cytology is not highly correlated with malignancy with neuroendocrine tumors • Cytology can identify the tumor as neuroendocrine – – – Naked uniform round nuclei Cells in rosettes and rows Fine chromatin & inconsistent nucleoli
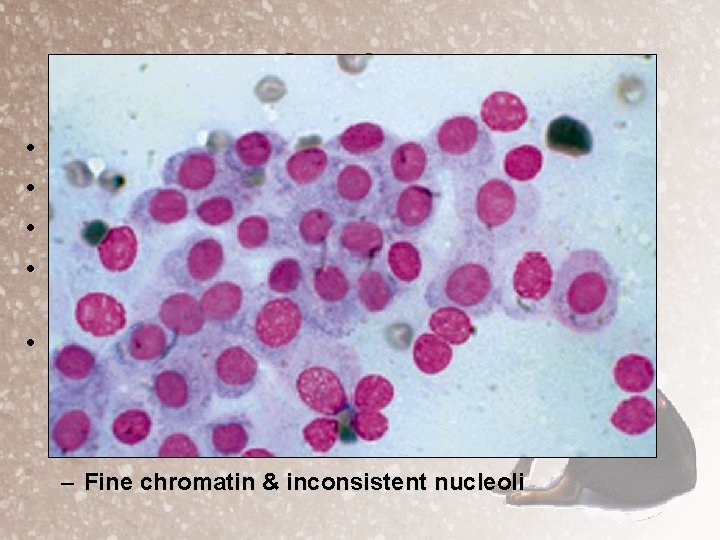
Cytology • • FNA of adrenal masses is not recommended Amy adrenal tumor has propensity to bleed Catecholamine storm is possible with pheo Cytology is not highly correlated with malignancy with neuroendocrine tumors • Cytology can identify the tumor as neuroendocrine – – – Naked uniform round nuclei Cells in rosettes and rows Fine chromatin & inconsistent nucleoli
Cytology • • FNA of adrenal masses is not recommended Amy adrenal tumor has propensity to bleed Catecholamine storm is possible with pheo Cytology is not highly correlated with malignancy with neuroendocrine tumors • Cytology can identify the tumor as neuroendocrine – – – Naked uniform round nuclei Cells in rosettes and rows Fine chromatin & inconsistent nucleoli

Plasma Free Metanephrines • Can measure plasma free metanephrines or fractionated urine metanephrines • Much higher in people and dogs with pheochromoctyomas • Requires special handling of the sample – contact the lab – Add acid, refrigerate, protect from light • Phenoxybenzamine, corticosteroids and tricyclic antidepressants can falsely increase metanephrines
Treatment • Adrenalectomy is treatment of choice • perioperative mortality 50% • Pre-treat with phenoxybenzamine for 20 days – Reduces perioperative mortality to 20% • Treat hypertension • If they survive surgery mean survival is 1 year

Acknowledgements Shelly Olin, ACVIM, Alejandro Garcia, Linda Shell, ACVIM (Neurology). Veterinary Information Network (VIN) – Canine Associate.
- Slides: 19