Phase 3 Final Submission Board Pack Submission due

Phase 3 Final Submission Board Pack Submission due: 21 September Northampton General Hospital NHS Trust

Executive Summary (1) This pack represents hospital group’s response to the requirements of Phase 3 Reset that was required by Sir Simon Stevens in his letter of 31 July 2020. It is confirmed the deadline of 21 September 2020 for final submission was met. Our plan is an ambitious and realistic approach to offering services to the communities we serve through the remainder of 2020 -21. We believe it represents our most likely scenario for winter period based on the best modelling scenarios available. There are risks associated with its delivery which are clearly articulated throughout the report. We have made every effort to reset to the required levels and believe the requirements can be met in many of the areas. We have maintained a clear focus on services for the most vulnerable and those in need of our urgent clinical support. For this reason we have placed a priority on cancer services and our preparations for winter. We have already restarted all services across both organisations. Cancer waits are dramatically improved with 104 -day waits virtually eliminated and plans for delivery of 62 -days in-place. Outpatient, elective and day-case services are all in operation. In some instances, diagnostic services are operating in excess of the same stage last year. Our staff are rightly proud of the progress made and are committed to deliver more. The headlines for the Board to note are: Non-Elective demand is the key risk to our reset. The impact on the bed base when seeking to maintain 85% occupancy and based on the peak demand point in our modelling (March 2021) we will be 76 beds short (29 at KGH and 47 at NGH). • We have modelled a baseline of Covid-19 at current levels for the remainder of 2020 -21 (r=1). In addition assumptions have been made for standard winter pressures and influenza. Any increase in activity over this level of modelling will affect our reset. • A key mitigation in this regard will be the support of our partners across the Health and Care Partnership to maintain services for those needing to leave hospital in a timely manner. Page 2

Executive Summary (2) • Elective and day-case services across the Group will reset to 82% of 2019 -20 activity levels by March 2021 • Endoscopy services remain at 100% of pre-covid levels for urgent and 2 -week wait patients. By March 2021, all demand will be met across both services • Workforce is a key consideration with both Trusts experiencing absence levels above expected levels and the continuing need to support all colleagues after the pressures of the first peak. This aspect cannot be overstated. This plan also continues the partnership with our colleagues at the Woodlands Hospital and BMI Three Shires. Nationally 75% of independent sector capacity remains commissioned for NHS patients. Both Trusts continue to work to ensure their allocation is fully utilised. In addition, both Trusts are exploring opportunities to access capacity in the longer term to ensure we offer services irrespective of a second peak in Covid activity. Our hospital group also offers opportunities to support each other, either through using our protected capacity for elective cases or our diagnostic service. This plan does not require services to move between sites, but we have much greater resilience though our partnership. The teams at both hospitals have worked hard to deliver this plan and submit it to regulators on-time. It will take the continued dedication of our staff to deliver it and we are dedicated to doing so. Our focus now turns to delivery of the plan across the Group by resetting our services for the benefit of the communities we serve. Our staff are central to this. They have been magnificent throughout the year and will continue to be so. They are to be congratulated for this plan and supported in its delivery. Page 3

Contents 1. 2. 3. 4. 5. 6. 7. 8. What have we been asked to do? Summary of Reset plans Summary of Performance impact Performance Impact Workforce assumptions and impact Financial assumptions and impact Responding to the demand Next Steps Page 4

1 | What have we been asked to do? Simon Stevens wrote to all NHS Trusts on 31 st July to outline arrangements for moving into ‘Phase 3’ of the Covid-19 pandemic, effective 1 st August 2020. The planning letter set out the NHS priorities for this third phase: 1. Accelerating the return to near-normal levels of non-Covid-19 health services, making full use of the capacity available in the ‘window of opportunity’ between now and winter i. Restoring full operation of all cancer services ii. Recovering the maximum elective activity possible between now and winter iii. Restoring service delivery in primary care and community services iv. Expanding and improving mental health services and services for people with learning disability and/or autism 2. Preparation for winter demand pressures, alongside continuing vigilance in the light of further probable Covid-19 spikes locally and possibly nationally i. Utilising Independent Sector provision ii. Significantly expanded flu vaccination programme 3. Doing the above in a way that takes account of lessons learned during the first Covid-19 peak; locks in beneficial changes; and explicitly tackles fundamental challenges including support for our staff Page 5
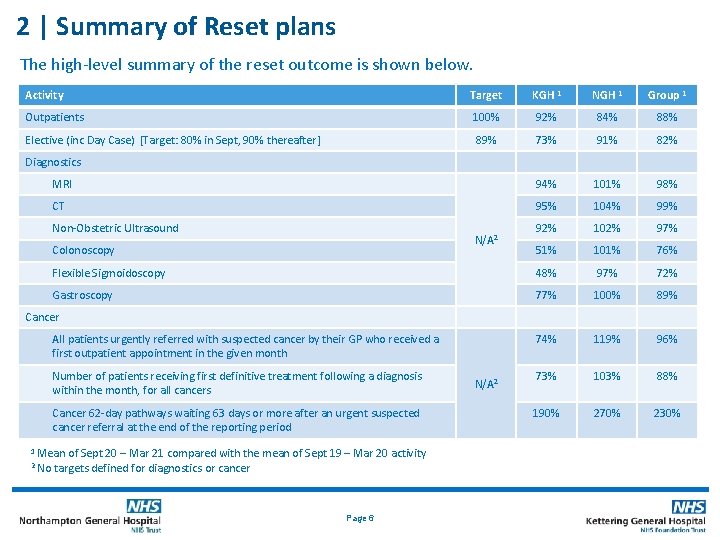
2 | Summary of Reset plans The high-level summary of the reset outcome is shown below. Activity Target KGH 1 NGH 1 Group 1 Outpatients 100% 92% 84% 88% Elective (inc Day Case) [Target: 80% in Sept, 90% thereafter] 89% 73% 91% 82% MRI 94% 101% 98% CT 95% 104% 99% 92% 102% 97% 51% 101% 76% Flexible Sigmoidoscopy 48% 97% 72% Gastroscopy 77% 100% 89% 74% 119% 96% 73% 103% 88% 190% 270% 230% Diagnostics Non-Obstetric Ultrasound N/A 2 Colonoscopy Cancer All patients urgently referred with suspected cancer by their GP who received a first outpatient appointment in the given month Number of patients receiving first definitive treatment following a diagnosis within the month, for all cancers Cancer 62 -day pathways waiting 63 days or more after an urgent suspected cancer referral at the end of the reporting period 1 2 Mean of Sept 20 – Mar 21 compared with the mean of Sept 19 – Mar 20 activity No targets defined for diagnostics or cancer Page 6 N/A 2

3 | Summary of Performance impact The forecast activity numbers will have an impact on performance, as follows: KGH • RTT performance (incomplete) – incomplete pathways will return to pre-covid levels over the period, rising from 16, 744 (Sept 20) to 19, 833 (Mar 21) • RTT performance (52 weeks) – 52 weeks will be maintained at zero • Cancer performance – returning to delivering above the 85% target from October 20 NGH • RTT performance (incomplete) – incomplete pathways are estimated to rise from 23, 889 (Sept 20) to 41, 342 (Mar 21) due to the capacity gap in the delivery of 1 st outpatient appointments post-Covid • RTT performance (52 weeks) – 52 weeks will be addressed and reduced from 454 in August to circa. 40 by December (40 is the current number of pathways where patients refuse to come in for treatment or are reliant on tertiary providers) • Cancer performance – Delivering above the 85% target from December 20 Page 7

4 | Performance impact The forecast activity planned for will have an impact on performance and this is detailed in the following slides, across the following areas: • RTT performance – incomplete pathways • RTT performance – 52 weeks • Cancer performance Page 8
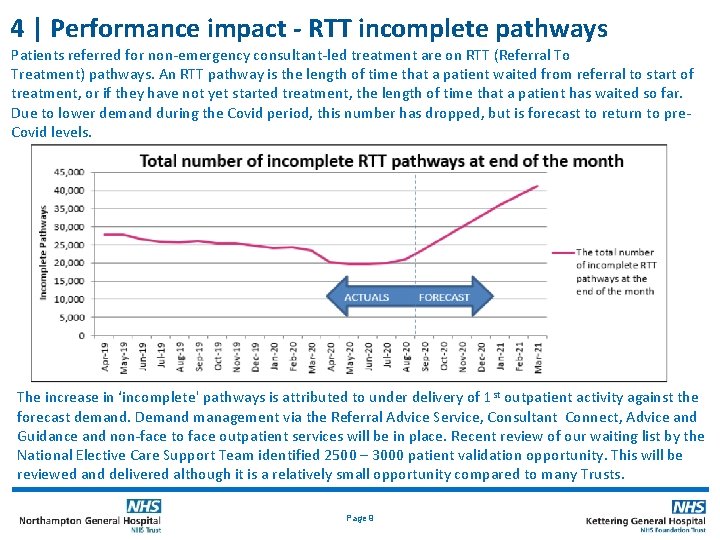
4 | Performance impact - RTT incomplete pathways Patients referred for non-emergency consultant-led treatment are on RTT (Referral To Treatment) pathways. An RTT pathway is the length of time that a patient waited from referral to start of treatment, or if they have not yet started treatment, the length of time that a patient has waited so far. Due to lower demand during the Covid period, this number has dropped, but is forecast to return to pre. Covid levels. The increase in ‘incomplete' pathways is attributed to under delivery of 1 st outpatient activity against the forecast demand. Demand management via the Referral Advice Service, Consultant Connect, Advice and Guidance and non-face to face outpatient services will be in place. Recent review of our waiting list by the National Elective Care Support Team identified 2500 – 3000 patient validation opportunity. This will be reviewed and delivered although it is a relatively small opportunity compared to many Trusts. Page 9
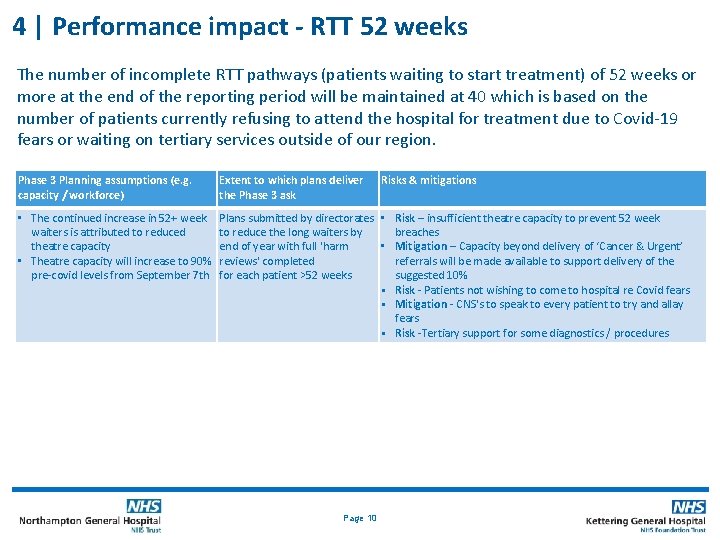
4 | Performance impact - RTT 52 weeks The number of incomplete RTT pathways (patients waiting to start treatment) of 52 weeks or more at the end of the reporting period will be maintained at 40 which is based on the number of patients currently refusing to attend the hospital for treatment due to Covid-19 fears or waiting on tertiary services outside of our region. Phase 3 Planning assumptions (e. g. capacity / workforce) Extent to which plans deliver the Phase 3 ask • The continued increase in 52+ week waiters is attributed to reduced theatre capacity • Theatre capacity will increase to 90% pre-covid levels from September 7 th Plans submitted by directorates • Risk – insufficient theatre capacity to prevent 52 week to reduce the long waiters by breaches end of year with full 'harm • Mitigation – Capacity beyond delivery of ‘Cancer & Urgent’ reviews' completed referrals will be made available to support delivery of the for each patient >52 weeks suggested 10% • Risk - Patients not wishing to come to hospital re Covid fears • Mitigation - CNS's to speak to every patient to try and allay fears • Risk -Tertiary support for some diagnostics / procedures Page 10 Risks & mitigations
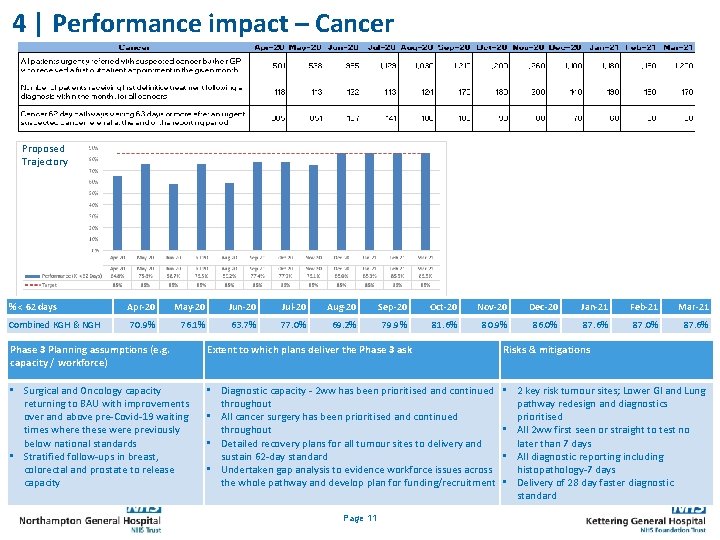
4 | Performance impact – Cancer Proposed Trajectory % < 62 days Combined KGH & NGH Apr-20 May-20 Jun-20 Jul-20 Aug-20 Sep-20 Oct-20 Nov-20 Dec-20 Jan-21 Feb-21 Mar-21 70. 9% 76. 1% 63. 7% 77. 0% 69. 2% 79. 9% 81. 6% 80. 9% 86. 0% 87. 6% 87. 0% 87. 6% Phase 3 Planning assumptions (e. g. capacity / workforce) Extent to which plans deliver the Phase 3 ask Risks & mitigations • Surgical and Oncology capacity returning to BAU with improvements over and above pre-Covid-19 waiting times where these were previously below national standards • Stratified follow-ups in breast, colorectal and prostate to release capacity • Diagnostic capacity - 2 ww has been prioritised and continued throughout • All cancer surgery has been prioritised and continued throughout • Detailed recovery plans for all tumour sites to delivery and sustain 62 -day standard • Undertaken gap analysis to evidence workforce issues across the whole pathway and develop plan for funding/recruitment • 2 key risk tumour sites; Lower GI and Lung pathway redesign and diagnostics prioritised • All 2 ww first seen or straight to test no later than 7 days • All diagnostic reporting including histopathology-7 days • Delivery of 28 day faster diagnostic standard Page 11

5| Workforce assumptions and impact (1) Workforce Requirements • Over the remainder of 2020/21 as services restart, we will need address the shortfall between current and required WTE to meet demand. This is impacted by shielding, absence and reduced efficiency due to PPE/ safety measures. The health and wellbeing of our colleagues building on what we experienced during the first phase of Covid is crucial. • A key risk to the planned activity model will be recruitment and supply of additional colleagues to expand capacity. Due to the timescales for step up, this will be mitigated by an increase in temporary staffing to meet planned demand. Additional activity achieved using additional payments will not be reflected in an increase in WTE. • The delivery of the plans are reliant on the right skill, capacity and flexibility of the workforce within the Group to deliver the whole system plan for recovery, the NCHP People Board has agreed a system People Plan to best support the whole system plan. • We are forecasting a relatively static vacancy and turnover position through to March 2021, except for international nursing colleagues arriving, which remains within our forecast, including the supernumerary time required. • The main additional wte movement across the group centres on temporary winter pressure additional bed capacity to that used currently for non-elective care and additional resources for elective care for additional outpatient lists within services such as Dermatology, Ophthalmology, Radiology and Breast Services. Given supply and time constraints this demand will be met with temporary staffing Page 12

5| Workforce assumptions and impact (2) Health and Wellbeing • At the peak of COVID 19, the Group had an absence rate of 16%. This has stabilised to 4. 7%, but remains higher than seasonal averages, and therefore our focus is to stabilise our absence rates, stemming our reliance on temporary staffing • To support people to stay healthy and well at work to reduce sickness and absence, the plan includes the annual flu vaccination programme with an ambition to vaccinate 100% of colleagues, continuing effectively use PPE and adhering to social distancing measures, accessible and timely COVID testing for staff and family members, agile working practices to support staff to remain at work, and a mechanism for staff sharing across the Group if required. • Our teams faced many additional pressures through COVID, and workforce mental health and wellbeing is a key area of focus for us, ensuring the support of the SOS and Open Office teams, along with the dedicated We Care Café and Our Space. • Our system people plan sets out ways in which our health and wellbeing workstream will continue the Targeted Team Support of psychological interventions for teams most impacted on by COVID Recruitment and Supply • It is assumed that current recruitment levels to existing vacancies and new positions (investment) will match leavers creating a stand still position, • International Recruitment: Prior to COVID we had two separate but successful International Recruitment campaigns with 322 international nurses appointed to date to mitigate this risk. These are resuming, and therefore will have a positive impact on nursing numbers in Q 4. Page 13

6 | Financial assumptions & impact (1) Financial envelope The priority for each trust is accelerating activity for non-COVID care in line with the Phase 3 goals, continuing readiness for winter and a potential increase in COVID-19 cases. • The funding envelope available for each system covers the period October 2020 to March 2021 and includes resources to meet the additional costs of COVID-19 response and recovery. • The funding available comprises • CCG allocations and, at system level, sufficient top-up funding to bring the system to a breakeven position. • Additional growth funding based on 2020/21. • Additional non-recurrent funding for the additional costs of COVID-19. The expectation is that each system will achieve financial balance within this envelope. • Whilst systems will be expected to breakeven, organisations within them will be permitted by mutual agreement across their system to deliver surplus and deficit positions. • Retrospective top-up funding will no longer be available from October and all system costs will need to be met from the envelope. • Separate funding streams or access to resources are available for PPE, testing, the hospital discharge programme, the national independent sector contract, and some national transformation and service development objectives. Only in exceptional circumstances will the principles outlined in relation to funding for COVID-19 be overruled. • The elective incentive scheme will also apply. • The expectation is that organisations will return non-NHS income to the levels seen in 2019/20 and must do so as quickly as possible. The national team will continue to discuss with the Government the treatment of income shortfalls against 2019/20 levels. Timeframes • Final system-level financial plans are required to be submitted by 5 October. • For in-year reporting purposes, individual organisations will then be required to submit organisation-level plans by 22 October, which must be consistent with the system-level plans.

6 | Financial assumptions & impact (2) Risks to financial envelope • Non-NHS income is to revert to 2019/20 levels. • Allocations will not cover loss of non-NHS income. Trusts will be asked to account for this separately and come back to NHSE/I later if there is a gap. • Covid may hit differentially in second wave and all costs may not be covered. Break glass arrangements will be available but further clarification is required. • NHSE/I have calculated 2 nd half Covid costs by reference to first half costs minus nonrecurrent items. • Incentives – it is still not clear how claw back will work if the service recovery targets are not hit and how negotiable the targets are if there are good reasons for not hitting them. Again this will need clarification. • Reliance on national PPE stock to be available and meet required demand as there is no local funding.

6 | Financial assumptions & impact (3) Regional / national requirement • System activity trajectory targets by Point of Delivery (EL/DC/OP) based on 2019/20 to be achieved for month 7 -12 • System financial position to be met within allocated financial envelope • Elective Incentive scheme in place to adjust funding support in line with actual performance against activity targets Current position • 1 st September submission • Activity forecasts did not meet trajectory targets • Financial plan exceeded draft financial envelope by £ 37. 8 m • 21 st September submission • Activity forecasts whilst improved at system level do not meet trajectory targets • System and organisation financial plans are being updated accordingly ready for submission on 5 th October & 22 nd October respectively in line with national deadlines System challenge • Activity levels to be increased, whilst there is a requirement to reduce costs to manage spend within the system financial envelopes. • The system focus is currently to maximise activity performance and to compile the financial plan that aligns to this Page 16

6 | Financial assumptions & impact (4) • The ‘baseline’ scenario for NGH is expected to meet NHSI activity targets (with the exception of Outpatients) but with additional costs expected to deliver this level of activity – opening wards, insourcing, WLIs, additional duty hours etc. • This has yet to be fully costed with the Divisions, but high-level calculations suggest revenue costs in the region of £ 5 -6 m for the remainder of 20 -21, assuming that any outsourcing to the Independent Sector will be nationally funded. • There is more to do to estimate the full additional cost (including any required capital costs) to deliver the expected activity. This will be done as part of the System financial submission on 5 th October. Indicative costs are shown below, where known: Indicative Cost £m Draft (1 st Sep) submission to New (21 st Sep) Baseline Scenario Baseline to close the gap to NHSI activity targets Total Indicative cost 5. 0 - 6. 0 3. 35 8. 35 -9. 35

7 | Responding to the demand Given the baseline scenario demand, can we deal with it? This is set out on the next few slides: 1. The baseline demand is shown in the NHS Foundry model 2. Proposals for addressing the gap in capacity to maintain 85% occupancy is provided. Page 18
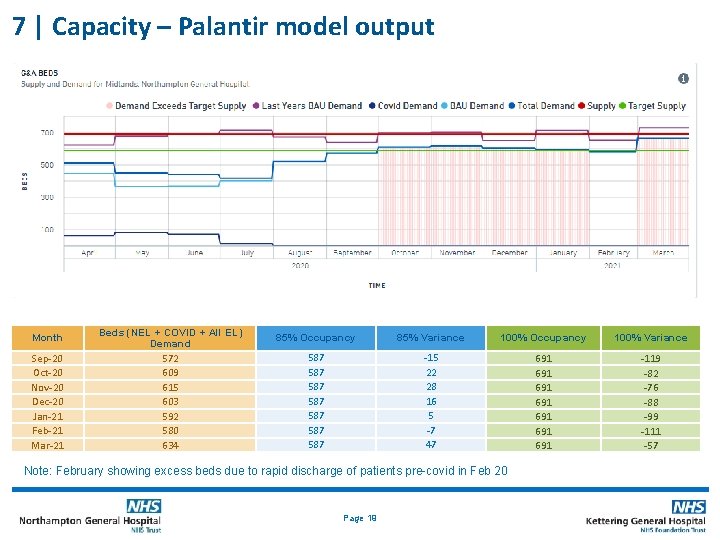
7 | Capacity – Palantir model output Month Sep-20 Oct-20 Nov-20 Dec-20 Jan-21 Feb-21 Mar-21 Beds (NEL + COVID + All EL) Demand 572 609 615 603 592 580 634 85% Occupancy 85% Variance 100% Occupancy 100% Variance 587 587 -15 22 28 16 5 -7 47 691 691 -119 -82 -76 -88 -99 -111 -57 Note: February showing excess beds due to rapid discharge of patients pre-covid in Feb 20 Page 19
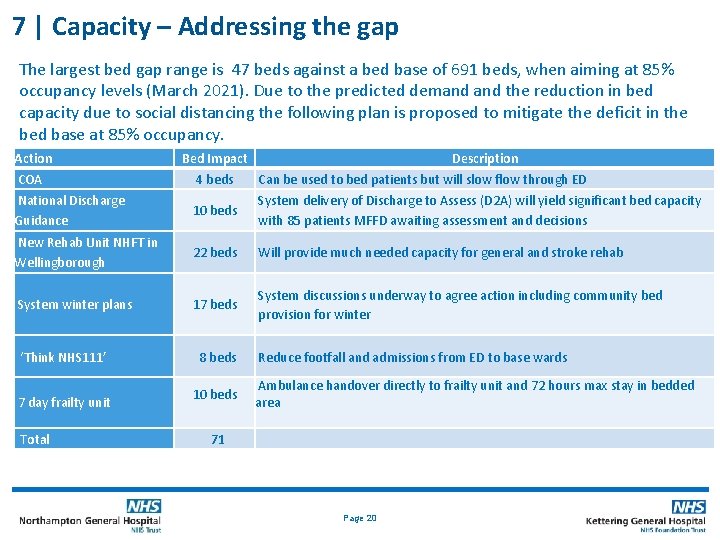
7 | Capacity – Addressing the gap The largest bed gap range is 47 beds against a bed base of 691 beds, when aiming at 85% occupancy levels (March 2021). Due to the predicted demand the reduction in bed capacity due to social distancing the following plan is proposed to mitigate the deficit in the bed base at 85% occupancy. Action COA Bed Impact Description 4 beds Can be used to bed patients but will slow flow through ED National Discharge Guidance 10 beds System delivery of Discharge to Assess (D 2 A) will yield significant bed capacity with 85 patients MFFD awaiting assessment and decisions New Rehab Unit NHFT in Wellingborough 22 beds Will provide much needed capacity for general and stroke rehab System winter plans 17 beds System discussions underway to agree action including community bed provision for winter ‘Think NHS 111’ 7 day frailty unit Total 8 beds 10 beds Reduce footfall and admissions from ED to base wards Ambulance handover directly to frailty unit and 72 hours max stay in bedded area 71 Page 20

8 | Next steps We provided our response to the Phase 3 request on 21 September. Work continues to: • Firm up our Winter plans, including agreements with our system partners • Assess the requirements of the newly issued allocations and financial guidance at system level over the coming days in order to: • submit a system financial plan by the national deadline of 5 th October. • submit organisational financial plans (aligned to the system plan above) by the national deadline of 22 nd October. • Establish reporting and monitoring mechanisms to track delivery against the plans A summary of progress against the Phase 3 submission will be provided to the Board in November 2020 Page 21
- Slides: 21