Pharmacy 101 Program Pharmacy 101 Unit One PBM

Pharmacy 101 Program

Pharmacy 101 - Unit One: PBM Overview This presentation provides a general overview of Pharmacy Benefit Managers (PBM). Besides covering the basics, the presentation also introduces Prime Therapeutics and describes some of its services. Objectives After completing PBM Overview you should be able to: • Describe the basic features of a PBM • Explain Prime’s and BCBSIL’s roles in decision-making and administration • Describe BCBSIL’s report utility Disclaimer: All individually identifiable health information contained within this lesson is fictitious and should be kept highly confidential. Any association to any person, living or dead, is purely coincidental. The information contained within this lesson is not for use/disclosure outside of Health Care Service Corporation and its affiliated companies. 2

Pharmacy 101 - Unit One: PBM Overview Introduction Part 1: What is a PBM? Welcome to PBM Overview! The presentation covers several key pharmacy topics including Pharmacy Programs, Benefit Design and Marketplace Trends. While each section touches upon many different topics, they are not an exhaustive description of our pharmacy programs. Instead they provide you with key information and tools to help you work with clients. Part 2: What a PBM does Unit 3: Cost Savings Unit 4: Introducing Prime Therapeutics Unit 5: Reporting 3

Pharmacy 101 - Unit One: PBM Overview Part 1: What is a PBM? 4
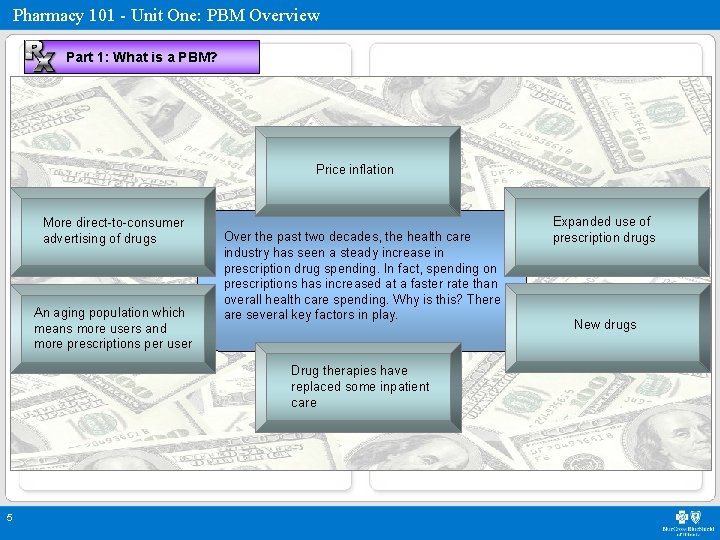
Pharmacy 101 - Unit One: PBM Overview Part 1: What is a PBM? Price inflation More direct-to-consumer advertising of drugs An aging population which means more users and more prescriptions per user Over the past two decades, the health care industry has seen a steady increase in prescription drug spending. In fact, spending on prescriptions has increased at a faster rate than overall health care spending. Why is this? There are several key factors in play. Drug therapies have replaced some inpatient care 5 Expanded use of prescription drugs New drugs

Pharmacy 101 - Unit One: PBM Overview Part 1: What is a PBM? Many employers and insurance plans have tackled these challenges by enlisting pharmacy benefit managers (PBM) to help them better manage claims administration and cut costs. PBMs come in all shapes and sizes. Their clients may be insurance companies, retail drugstores, employers, unions, Medicare and Medicaid. Some are subsidiaries of insurance plans or retail drugstores, while others are independently owned. PBMs also vary in what they do. Their role has evolved from a third party claims processor to a complex administrator, negotiator and advisor. Their primary responsibility is to process and pay prescription drug claims. In addition, they’re also responsible for managing the formulary, creating client programs, negotiating discounts with retail pharmacies and contracting with pharmaceutical manufacturers for rebates. Many also offer disease management, drug utilization review, mail-order pharmacy and network management. 6
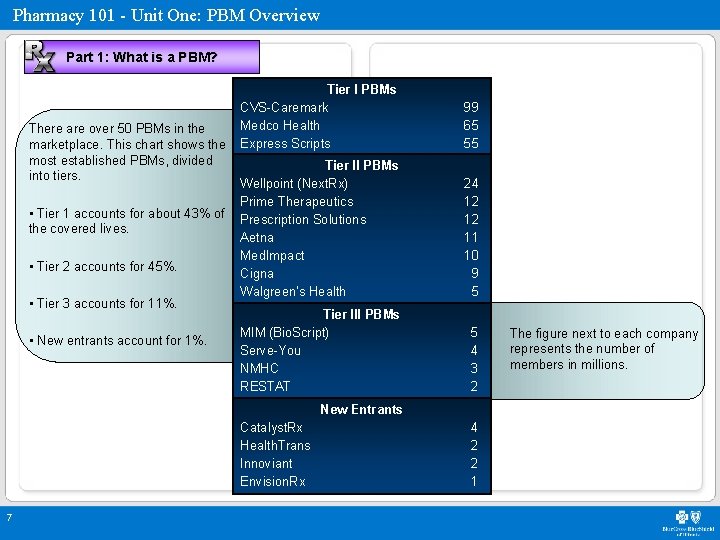
Pharmacy 101 - Unit One: PBM Overview Part 1: What is a PBM? There are over 50 PBMs in the marketplace. This chart shows the most established PBMs, divided into tiers. • Tier 1 accounts for about 43% of the covered lives. • Tier 2 accounts for 45%. • Tier 3 accounts for 11%. • New entrants account for 1%. Tier I PBMs CVS-Caremark Medco Health Express Scripts 99 65 55 Tier II PBMs Wellpoint (Next. Rx) Prime Therapeutics Prescription Solutions Aetna Med. Impact Cigna Walgreen’s Health 24 12 12 11 10 9 5 Tier III PBMs MIM (Bio. Script) Serve-You NMHC RESTAT 5 4 3 2 New Entrants Catalyst. Rx Health. Trans Innoviant Envision. Rx 7 4 2 2 1 The figure next to each company represents the number of members in millions.
Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does 8

Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does The following topics provide a general overview of the most common services PBMs offer. Claims Administration and Benefit Management Pharmacy Network Formulary Rebates and Discounts Drug Utilization Review 9

Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does Claims Administration and Benefit Management Pharmacy Network Formulary Rebates and Discounts Drug Utilization Review 10 Claims Administration and Benefit Management PBMs undertake the daunting task of managing thousands of benefit claims. Fortunately, PBMs process nearly all claims electronically, in realtime. This eliminates paper claims and reduces the need for claims adjudication. When a member fills a prescription, the pharmacist can instantly verify through the PBM, the member’s eligibility, drug coverage, the member’s copay or coinsurance and the cost to the insurer. Copays and coinsurance are examples of costsharing. The client determines how much of a drug’s cost must be shared by the member. Costsharing may take the form of copays, coinsurance, deductibles or out-of-pocket limits. One feature of cost-sharing is a tier-system of payment, which we’ll discuss later.

Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does The chart below outlines some of the strengths and limitations of a coinsurance program vs. a copay program. 11

Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does Claims Administration and Benefit Management Pharmacy Network Formulary Rebates and Discounts Drug Utilization Review 12 Pharmacy Network Management PBMs also set up and manage pharmacy networks. Most large PBMs establish nationwide networks, contracting with about 95% of US pharmacies, which means access is rarely a problem. Establishing networks involves: • Negotiating drug discounts and dispensing fees with pharmacies • Assuring pharmacy compliance with quality and customer service standards • Providing technical support to pharmacies PBMs may establish smaller preferred networks within broader non-preferred networks. Similar to a PPO plan, these preferred networks encourage members to fill prescriptions in network by offering lower copayments or coinsurance. Out of network benefits are still paid, but the member will have a higher payment. Pharmacies in these preferred (often regional) networks usually agree to lower prescription fees. This cost is counterbalanced by an increase in customers.

Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does Formulary Management You can’t have a PBM without a formulary system —a complex process which determines drug utilization policies and appropriate therapies. Claims Administration and Benefit Management Pharmacy Network Formulary Rebates and Discounts Drug Utilization Review 13 At the heart of this system is the formulary—a continually updated list of preferred drugs, typically available at lower copays. These medications have been deemed safe, effective and cost-conscious. Typically, a formulary includes all generics and select brand name drugs. At BCBSIL formulary development goes first through the National Pharmacy and Therapeutics Committee (P&T Committee). The P&T committee is made up of independent pharmacists and physicians and one rep from each of the owner Plans. They use clinical evidence to evaluate drugs on their efficacy, safety and uniqueness.

Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does What’s the difference between brand name drugs and generic drugs? Brand Name Drug: A brand name drug is patented, which means that only the original drug manufacturer may produce and sell it. Examples of brand name drugs are Lexapro, Lipitor and Singulair. Generic Drug: Once a brand name drug’s patent expires, other companies may produce generic chemical equivalents of the drug. The generic drug is then sold under its chemical name. Generic drugs are usually cheaper than brand name drugs, in part because the manufacturer doesn’t have to fund research and marketing. Today generics make up almost half of all prescriptions, and yet they represent around 20% of prescription costs (IMS Health). Examples of generic drugs are Fluoxetine (Prozac) and Ibuprofen (Motrin). 14

Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does Claims Administration and Benefit Management Pharmacy Network Formulary Rebates and Discounts Drug Utilization Review 15 Formulary Management (continued) The P&T Committee meets quarterly to keep up with new therapies, clinical research and changes in FDA guidelines. Drug costs aren’t evaluated at this point; the Committee only considers whether a drug is clinically appropriate for the formulary. BCBSIL’s Preferred Drug Committee then evaluates the P&T’s recommendations and makes the final decision on the formulary. The Committee of medical and pharmacy directors and an actuary representative uses pharmacoeconomic modeling, pipeline considerations and other factors to decide which drugs provide the most efficacy per dollar. Generic and unique brand name drugs are automatically added to the formulary. When two or more drugs in a given class are equivalent, the cheaper one is usually added. A key goal of the formulary is to establish guidelines for physicians and prescribers, so they’ll dispense drugs proven to be the most safe and effective ones on the market. Cost is a factor, but it’s secondary to clinical considerations.
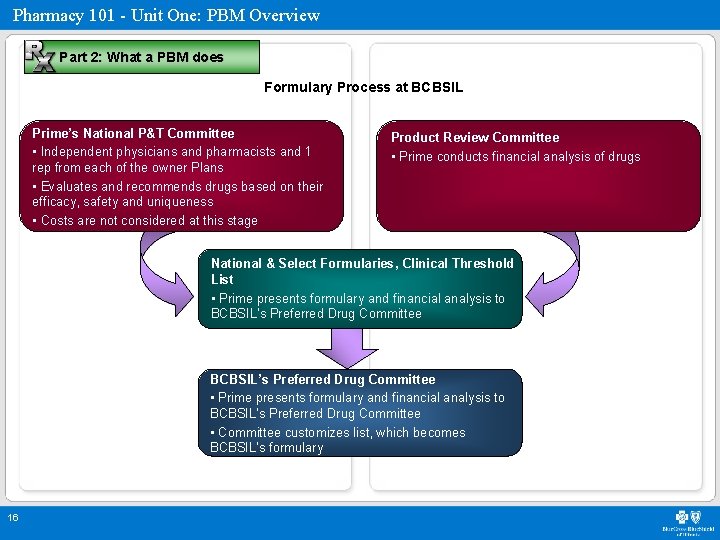
Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does Formulary Process at BCBSIL Prime’s National P&T Committee • Independent physicians and pharmacists and 1 rep from each of the owner Plans • Evaluates and recommends drugs based on their efficacy, safety and uniqueness • Costs are not considered at this stage Product Review Committee • Prime conducts financial analysis of drugs National & Select Formularies, Clinical Threshold List • Prime presents formulary and financial analysis to BCBSIL’s Preferred Drug Committee • Committee customizes list, which becomes BCBSIL’s formulary 16

Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does Formulary Management (continued) Claims Administration and Benefit Management Pharmacy Network Formulary Rebates and Discounts Drug Utilization Review 17 Tiered Copayment Benefits Once drugs have been selected, they can be classified into tiers. The tiered formulary program is designed to save both members and employers money by encouraging members to use lowerpriced generic and formulary drugs. The most common tier designs contain three tiers, though many insurance plans have created additional tiers (e. g. fourth tier for specialty or lifestyle drugs). Here’s an example of a three-tier structure: • 10$ copay - first-tier drugs (generics( • 20$ copay - second-tier drugs (formulary brand( • 35$ copay - third-tier drugs (non-formulary brand( Some benefit plans use a percentage-based tier system (e. g. 10%/20%/30%). Manufacturers ideally want their products in the lowest tier possible as these drugs are the most utilized.

Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does Rebates and Discounts As another critical cost-saving tool, the PBM uses the formulary to negotiate rebates and discounts with drug manufacturers and pharmacists. Claims Administration and Benefit Management Pharmacy Network Formulary Rebates and Discounts Drug Utilization Review 18 Rebates The PBM contracts with drug manufacturers on rebates (a sum of money to be returned to the client usually paid on a per pill basis). In return, the manufacturer’s drug is included on the formulary, which boosts both market share and utilization of the drug. Rebates are determined on a drug-by-drug basis, based on the anticipated volume of drugs that will be sold. When there are multiple drug options within a therapeutic class, there is more competition between manufacturers, which puts the PBM in a better position to negotiate rebates. On average rebates range from 5% to 25% savings, which are shared in whole or in part with the client.
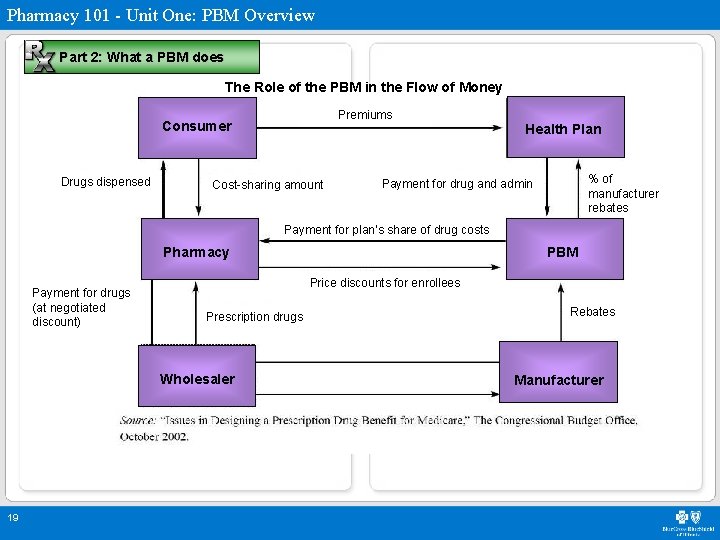
Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does The Role of the PBM in the Flow of Money Premiums Consumer Drugs dispensed Health Plan Cost-sharing amount % of manufacturer rebates Payment for drug and admin Payment for plan’s share of drug costs Pharmacy Payment for drugs (at negotiated discount) Price discounts for enrollees Prescription drugs Wholesaler 19 PBM Rebates Manufacturer

Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does Rebates and Discounts (continued) Claims Administration and Benefit Management Pharmacy Network Formulary Rebates and Discounts Drug Utilization Review 20 Discounts PBMs also negotiate dispensing fees and drug pricing with network pharmacies. To join the network, the pharmacy agrees to certain reimbursement amounts and dispensing fees (paid to the pharmacy for each drug dispensed). Pharmacies benefit from this agreement because they’re guaranteed stable reimbursement and a larger pool of customers. For brand name drugs, pharmacies usually apply the average wholesale price (AWP) or published suggested retail price set by the manufacturer. The actual price paid by a pharmacy to the manufacturer is usually lower than AWP. There are two primary sources for AWP pricing: Medi. Span (used by Prime) and First Data Bank.

Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does Claims Administration and Benefit Management Pharmacy Network Formulary Rebates and Discounts Drug Utilization Review 21 Rebates and Discounts (continued) Typically, dispensing fees for generics are higher to encourage pharmacies to promote generic substitution and make sure the pharmacy dispenses economically. In the case of generic drugs where there may be multiple manufacturers with wide price variations, PBMs set reimbursement ceilings. The maximum allowable cost (MAC) is the maximum price the PBM will reimburse a pharmacy for generic and multi -source prescription drugs. Some PBMs may have multiple MAC lists which contain varying number of drugs and levels of discounts. In the PBM industry the MAC list is considered to be highly competitive and proprietary. Here’s an example of how a discount for a generic drug could be formulated: AWP – 50 to 60% + $2. 00 (dispensing fee) = MAC

Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does Claims Administration and Benefit Management Drug Utilization Review (DUR) Often members have prescriptions from multiple physicians, or they fill them at different pharmacies. This makes it tough to track drug utilization and benefit compliance. That’s where the PBM comes in. The PBM uses its database of member information to conduct drug utilization reviews (DUR), which flag potential drug interactions, therapeutic duplication, drug misuse and quality of care. The two most common DURs are concurrent and retrospective. Pharmacy Network Formulary Rebates and Discounts Drug Utilization Review 22 Concurrent DUR This DUR is conducted at the point of sale and uses “edits” or automated checks to compares the member’s information with the prescribed drug, along with other drugs the member is taking. This review flags potential adverse drug interactions or inappropriate utilization. When a claim is flagged, the system informs the pharmacist of a potential conflict. Regardless of where the member fills the prescription, all pharmacies use the same processing systems.
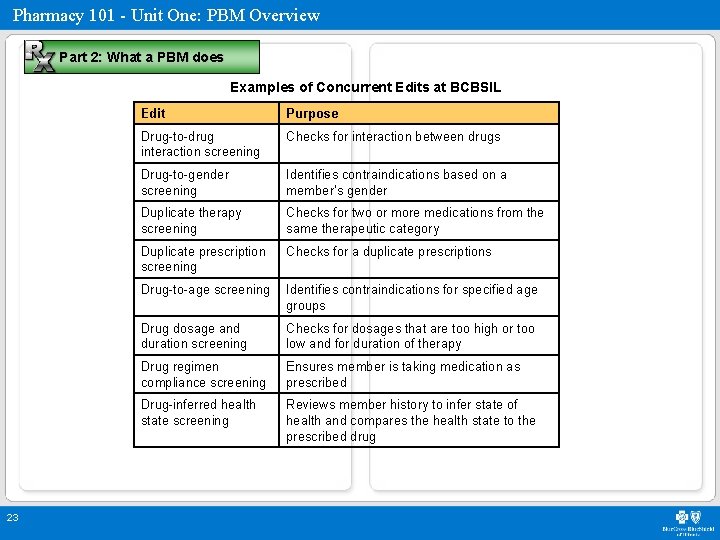
Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does Examples of Concurrent Edits at BCBSIL 23 Edit Purpose Drug-to-drug interaction screening Checks for interaction between drugs Drug-to-gender screening Identifies contraindications based on a member’s gender Duplicate therapy screening Checks for two or more medications from the same therapeutic category Duplicate prescription screening Checks for a duplicate prescriptions Drug-to-age screening Identifies contraindications for specified age groups Drug dosage and duration screening Checks for dosages that are too high or too low and for duration of therapy Drug regimen compliance screening Ensures member is taking medication as prescribed Drug-inferred health state screening Reviews member history to infer state of health and compares the health state to the prescribed drug

Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does Claims Administration and Benefit Management Pharmacy Network Formulary Rebates and Discounts Drug Utilization Review 24 Drug Utilization Review (DUR) (continued) Retrospective DUR This DUR analyzes pharmacy claims history to identify potential prescribing and dispensing issues. For example, a DUR may reveal that a physician is consistently prescribing a brand name drug instead of a generic substitute. The review also detects individual prescriptions that may have been inappropriately used. BCBSIL does several retrospective DUR programs per year on topics such as: • Appropriate use of controlled substances • Generic utilization • Diabetes • Hypertension medical management • Acetaminophen overdosage
Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does The following topics provide a general overview of the most common services PBMs offer. Mail-Service Specialty Pharmacy Prior Authorization Disease Management 25

Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does Mail-Service Specialty Pharmacy Prior Authorization Disease Management 26 Mail-Service Pharmacy Mail-service pharmacy is a rapidly growing segment of the pharmacy industry. In fact it’s estimated that by 2011 nearly 25% of prescriptions will be filled through mail order (Drug Benefit News, Nov. 2006). Almost all PBMs offer mail-service options. Mail-service pharmacies fill maintenance prescriptions that are used on a continuing basis. Besides offering convenience and cost-saving to members, mail-service pharmacies can be more cost-effective than traditional pharmacies. Industry experts have noted that mail-service prescriptions cost approximately 10% less than retail-pharmacy drugs. This translates into a nearly $85 billion savings in drug costs over the next decade (Pharmaceutical Care Management Association).
Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does Mail-Service Specialty Pharmacy Prior Authorization Disease Management 27 Specialty Pharmacy Specialty pharmacy services are geared towards a small population of members with complex and chronic conditions such as HIV/AIDS, hepatitis C, infertility, hemophilia, Crohn’s Disease, anemia, cancer and cystic fibrosis. PBMs may assist with specialty pharmacy by developing clinical and cost management techniques to lower treatment costs.

Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does Prior Authorization Prior authorization (PA) manages certain high cost drugs and those that could be inappropriately prescribed. When a drug requires prior authorization, the member usually contacts the physician who must obtain approval from the PBM before the medication may be dispensed. Mail-Service Specialty Pharmacy Prior Authorization Disease Management 28 The PBM may require the doctor to submit a preauthorization form with requested clinical information (e. g. test results, diagnoses). If approved, the member pays the normal copay or coinsurance. If denied, the member can still purchase the drug, but the drug won’t be covered. Only a few drugs require prior authorization (e. g. anabolic steroids, growth hormones). Here’s an example of how a prior authorization program can provide savings. Growth hormones are prescribed for the treatment of growth hormone deficiency. However, they can be misused by body builders to increase muscle mass and by others for anti-aging effects. A prior authorization program would deny these prescriptions and save nearly $2, 000 for a one-month supply.
Pharmacy 101 - Unit One: PBM Overview Part 2: What a PBM does Mail-Service Specialty Pharmacy Prior Authorization Disease Management 29 Disease Management Most PBMs offer disease management services to manage the cost-effectiveness and treatment of members with chronic illnesses. The PBM uses integrated medical and pharmacy data to identify disease management opportunities for conditions such as hypertension, asthma, diabetes, depression and specific cardiovascular conditions. Disease management programs don’t always lower prescription costs. In fact they can increase the drug spending. But the increase in drug therapies can cut overall costs as members may be less likely to need inpatient care.

Pharmacy 101 - Unit One: PBM Overview Key Points • PBMs process and pay prescription drug claims, manage the formulary, create client programs, and negotiate rebates and discounts with manufacturers and pharmacies. • A formulary is a continually updated list of preferred drugs, typically available at lower copays. These medications have been deemed as safe, effective, and cost-conscious. • A generic drug is a cheaper chemical equivalent of a brand name drug with an expired patent. • PBMs contract with manufacturers on rebates (an amount returned to the client for each drug used. ( • PBMs negotiate discounts with pharmacies based on AWP and MAC pricing. • PBMs use concurrent and retrospective DURs to flag potential drug interactions, therapeutic duplication, drug misuse and quality of care. 30

Pharmacy 101 - Unit One: PBM Overview Part 3: Cost Savings 31

Pharmacy 101 - Unit One: PBM Overview Part 3: Cost Savings A PBM can significantly lower drug costs. According to the Pharmaceutical Care Management Association (PCMA), PBMs on average reduce costs by 25%. Collectively, PBMs administer claims for over 210 million Americans, and over the next decade, they’re projected to save $1. 3 trillion dollars in drug costs. *Data provided by the PCMA. 32

Pharmacy 101 - Unit One: PBM Overview Part 3: Cost Savings A PBM can significantly lower drug costs. According to the Pharmaceutical Care Management Association (PCMA), PBMs on average reduce costs by 25%. Collectively, PBMs administer claims for over 210 million Americans, and over the next decade, they’re projected to save $1. 3 trillion dollars in drug costs. PBMs can negotiate discounts as much as 18% savings on brand name drugs and 47% on generic drugs. *Data provided by the PCMA. 33

Pharmacy 101 - Unit One: PBM Overview Part 3: Cost Savings A PBM can significantly lower drug costs. According to the Pharmaceutical Care Management Association (PCMA), PBMs on average reduce costs by 25%. Collectively, PBMs administer claims for over 210 million Americans, and over the next decade, they’re projected to save $1. 3 trillion dollars in drug costs. PBMs can save anywhere between 6% to 9% with DUR programs. *Data provided by the PCMA. 34

Pharmacy 101 - Unit One: PBM Overview Part 3: Cost Savings A PBM can significantly lower drug costs. According to the Pharmaceutical Care Management Association (PCMA), PBMs on average reduce costs by 25%. Collectively, PBMs administer claims for over 210 million Americans, and over the next decade, they’re projected to save $1. 3 trillion dollars in drug costs. PBM therapeutic interchange programs can save from 1% to 4. 5% on drug spending. *Data provided by the PCMA. 35

Pharmacy 101 - Unit One: PBM Overview Part 3: Cost Savings A PBM can significantly lower drug costs. According to the Pharmaceutical Care Management Association (PCMA), PBMs on average reduce costs by 25%. Collectively, PBMs administer claims for over 210 million Americans, and over the next decade, they’re projected to save $1. 3 trillion dollars in drug costs. Prior authorization can save 1% to 6% on drug spending. *Data provided by the PCMA. 36

Pharmacy 101 - Unit One: PBM Overview Part 3: Cost Savings A PBM can significantly lower drug costs. According to the Pharmaceutical Care Management Association (PCMA), PBMs on average reduce costs by 25%. Collectively, PBMs administer claims for over 210 million Americans, and over the next decade, they’re projected to save $1. 3 trillion dollars in drug costs. PBMs can negotiate rebates which reduce annual drug spending by 3% to 9%. *Data provided by the PCMA. 37

Pharmacy 101 - Unit One: PBM Overview Part 3: Cost Savings A PBM can significantly lower drug costs. According to the Pharmaceutical Care Management Association (PCMA), PBMs on average reduce costs by 25%. Collectively, PBMs administer claims for over 210 million Americans, and over the next decade, they’re projected to save $1. 3 trillion dollars in drug costs. Mail service drugs can save an average 27% on brand name drugs and 53% on generic drugs. *Data provided by the PCMA. 38

Pharmacy 101 - Unit One: PBM Overview Part 3: Cost Savings A PBM can significantly lower drug costs. According to the Pharmaceutical Care Management Association (PCMA), PBMs on average reduce costs by 25%. Collectively, PBMs administer claims for over 210 million Americans, and over the next decade, they’re projected to save $1. 3 trillion dollars in drug costs. Specialty pharmacy can lower annual costs as high as $250, 000 per member. *Data provided by the PCMA. 39

Pharmacy 101 - Unit One: PBM Overview Part 4: Introducing Prime Therapeutics 40

Pharmacy 101 - Unit One: PBM Overview Part 4: Prime Therapeutics Our PBM, Prime Therapeutics, serves over 10 million lives. Owned by ten BCBS plans, Prime has no ties to pharmacies. Its business model aligns with ours in its incentive and achievement of cost-saving goals. It also provides transparency of costs and rebates, flexibility, customization for local markets and solid customer service. We benefit from this partnership because we have more control of care and costs than we would with an outside vendor. All savings from discounts are passed through to employer groups—there is no spread pricing. Prime’s Services Prime generally provides the following services. Note that in some cases some of these services may be handled by local pharmacy programs instead of Prime. • Custom reporting through Blue Insight • Automatic concurrent and quarterly retrospective DUR to identify opportunities to improve quality and cost-savings • Support for step therapy edits and QVT • Claims processing with two-second average online adjudication • Paper claims • Benefit management • Pharmacy network development and administration 41
Pharmacy 101 - Unit One: PBM Overview Part 4: Prime Therapeutics Prime also offers Prime. Mail mail order service, which provides significant savings. Prime. Mail information can now also be easily accessed from the member website, My. Rx. Health. com on which members can: • Order prescription refills • Obtain order status updates • Review benefit information • Compare prices of both brand name and generic drugs at mail and retail • Track prescription history 42

Pharmacy 101 - Unit One: PBM Overview Part 4: Prime Therapeutics Prime also administers our Medicare Part D plans, which help beneficiaries pay for a significant share of their prescription costs. Prime assists Medicare beneficiaries with enrollment, eligibility and pharmacy-related questions. Another key service is Prime. Impact, a clinical program that targets 14 core clinical categories. Prime. Rx. Specialty provides member care, drug and disease information to members with chronic, possibly life-threatening conditions. 43

Pharmacy 101 - Unit One: PBM Overview Part 4: Prime Therapeutics The chart below shows some of the core programs offered under Prime. Impact. Note that not all of these programs are used by the Blues plans. You can learn more about these programs in Unit Two: Pharmacy Programs Overview. Physicians § Education § Safety § Adherence § Generics § Benchmark reporting Utilization Management § Step therapy § Prior authorization § Quantity limits § Retro DUR § Concurrent DUR § Medical/Rx integration 44 Member Education § Print § Web § Compliance Clinical Reporting § Generic opportunity § UM estimated savings § UM actual savings § Adherence Value-Based Prime Rx. Specialty § Benefit design § Medical/Rx § Specialty network § Product § Reporting § Member direct § Physician direct § Benefit design § Disease integration identification management § Utilization management

Pharmacy 101 - Unit One: PBM Overview Part 4: Prime Therapeutics Comparison of Functions between Local Pharmacy Departments and Prime Therapeutics The local pharmacy departments and Prime have different responsibilities. Here is a brief overview of some of their individual functions. Note that there may be some variation between the four plans, but this gives you a general overview of the breakdown of functions. Oklahoma will be converted to Prime in 2008. 45

Pharmacy 101 - Unit One: PBM Overview Part 4: Prime Therapeutics Comparison of Functions between Local Pharmacy Departments and Prime Therapeutics The local pharmacy departments and Prime have different responsibilities. Here is a brief overview of some of their individual functions. Note that there may be some variation between the four plans, but this gives you a general overview of the breakdown of functions. Oklahoma will be converted to Prime in 2008. Local Pharmacy Departments Makes decisions on all pharmacy benefits (copays, preventive drug lists, drug exclusions, etc) Makes decisions on the formulary list Makes decisions on clinical programs (step therapy, prior authorization, quantity limits, etc) Develops innovative programs (CAP, controlled substance program, “MAIL” program) 46 Prime Therapeutics Adjudicates pharmacy claims Dispenses mail order prescriptions Negotiates rebates/discounts and supports retail pharmacy contract Provides customer service Supports step therapy & prior authorization Supports account management Supports reporting

Pharmacy 101 - Unit One: PBM Overview Part 5: Reporting 47

Pharmacy 101 - Unit One: PBM Overview Part 5: Reporting Prime provides accounts with comprehensive reports on prescription drug utilization. The reports are designed to quickly identify trends and pharmacy spending, as well as potential opportunities for plan design improvement. The reporting package consists of the following components: Executive Summary: an overview of utilization, including total cost, plan and member paid, pricing and network performance, savings, drug mix and member submitted claims for both retail and mail order. Key Indicators Summary: a quarterly breakout of 9 key components and BCBSIL book of business benchmarks for comparison purposes. Summary also provides group specific graphs for total plan paid for top 10 drug classes. Additional Report Sections: include generic and formulary experience by retail and mail order, the top 25 drug classes by ingredient cost and by volume and the top 50 drugs by ingredient cost and by volume. Ad-hoc Reports: based on clients need’s The report package provides an in-depth look at the overall prescription drug utilization and cost and gives employers the opportunity to increase cost savings by adding clinical programs, such as prior authorization, step therapy or changing their benefit design. Additionally, the report package allows groups to see the effectiveness of their plan design and implemented clinical programs. 48

Pharmacy 101 - Unit One: PBM Overview Conclusion Proven in the marketplace, PBMs promote quality of care and reduce costs for their clients. Although PBMs can vary in their capabilities and responsibilities, their primary function is that of claims processing, record-keeping, formulary management, reporting and rebate negotiation with drug manufacturers. As we have seen, many PBMs such as our own Prime Therapeutics offer additional programs such as disease management, drug utilization review, mail-order pharmacy and network management. 49

Pharmacy 101 - Unit One: PBM Overview Key Points • PBMs on average reduce overall drug costs by 25%. Collectively, they administer claims for over 210 million Americans, and over the next decade, they’re projected to save $1. 3 trillion dollars in drug costs. • Some of Prime Therapeutics’ main services include claims processing, reporting, benefits management, network development, utilization management and mail service. • Members can use My. Rx. Health. com to order prescriptions, review benefits, compare drug prices and track prescription history. • Prime and the local pharmacy departments have different responsibilities. The local pharmacy department makes decisions on benefits, formulary and clinical programs. Prime supports us by adjudicating pharmacy claims, dispensing mail order prescriptions, negotiating rebates/discounts, creating reports, etc. 50

Pharmacy 101 - Unit One: PBM Overview Summary This concludes the PBM Overview. You should now be able to: • Describe the basic features of a pharmacy benefit manager (PBM) • Explain Prime’s and BCBSIL’s roles in decision-making and administration • Describe BCBSIL’s report utility 51
- Slides: 51