Pharmacology Pharmacology Phase 2 a Pharmacology Ryad Chebbout

Pharmacology

Pharmacology Phase 2 a Pharmacology Ryad Chebbout 24/04/17 The Peer Teaching Society is not liable for false or misleading information…

Contents • • Pharmacokinetics Pharmacodynamics Autonomic nervous system Central nervous system Infection Cardiovascular system Endocrine system Poisoning The Peer Teaching Society is not liable for false or misleading information…

Route of Administration Enteral (oral) • Enteric-coated (intestinal absorption, e. g. aspirin) • Extended-release (slower absorption, e. g. metformin) • Sublingual/Buccal (rapid absorption + avoids 1 st pass metabolism) Parenteral (systemic circulation) • Intravenous • Intramuscular (antipsychotics) • Subcutaneous (insulin) Other • Inhalation (oral, nasal) • Topical • Rectal
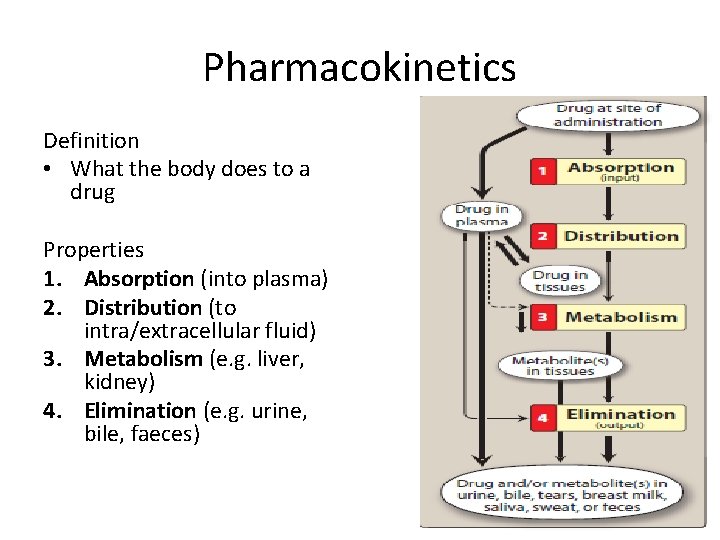
Pharmacokinetics Definition • What the body does to a drug Properties 1. Absorption (into plasma) 2. Distribution (to intra/extracellular fluid) 3. Metabolism (e. g. liver, kidney) 4. Elimination (e. g. urine, bile, faeces)

1. Absorption Mechanisms (e. g. GI mucosa) • Passive diffusion • Facilitated diffusion • Active transport • Endocytosis Variables of Absorption • p. H • Vascularity (e. g. shock reduces SC absorption) • Surface area • Contact time (e. g. with food = slower gastric emptying)
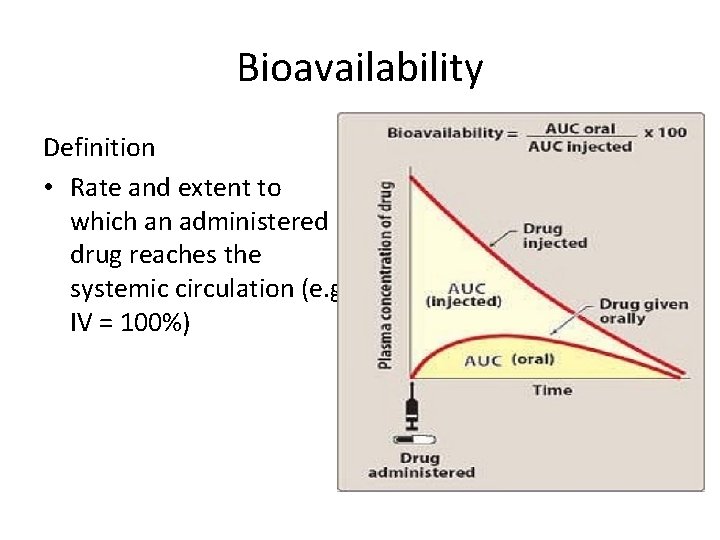
Bioavailability Definition • Rate and extent to which an administered drug reaches the systemic circulation (e. g. IV = 100%)
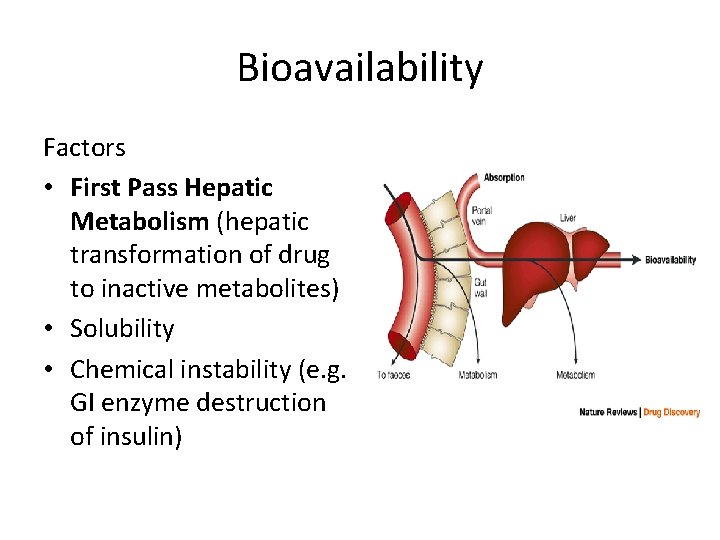
Bioavailability Factors • First Pass Hepatic Metabolism (hepatic transformation of drug to inactive metabolites) • Solubility • Chemical instability (e. g. GI enzyme destruction of insulin)
2. Distribution Definition • Drug reversibly leaves bloodstream and enters the extracellular fluid and tissues Factors • Blood flow (e. g. brain > muscles) • Capillary permeability • Plasma protein binding (e. g. albumin) • Tissue protein binding (e. g. cyclophosphamide accumulating in bladder leading to cystitis) • Lipophilicity (ability to cross cell membranes)

3. Metabolism Definition • Process of elimination, mainly through hepatic, renal and biliary routes Rates • First Order: catalysed by enzymes, rate of metabolism directly proportional to drug concentration • Zero Order: enzymes saturated by high drug doses, rate of metabolism is constant, e. g. ethanol, phenytoin Phase • 1 = polarise lipophilic drugs, reduction / oxidation / hydrolysis, catalysed by cytochrome P 450 system • 2 = conjugation, e. g. glucuronic acid, polarisation of drugs to be excreted by renal or biliary systems
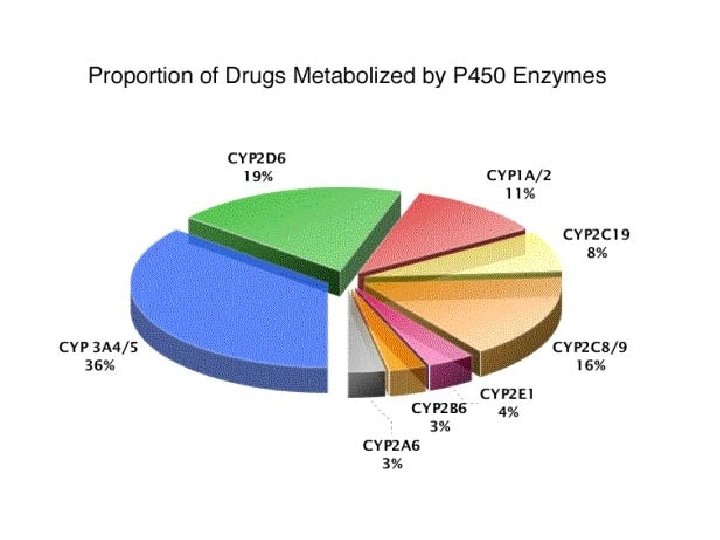
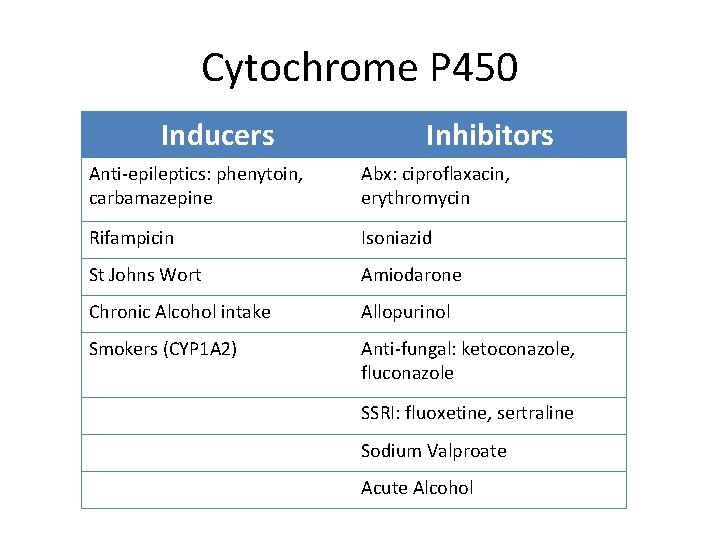
Cytochrome P 450 Inducers Inhibitors Anti-epileptics: phenytoin, carbamazepine Abx: ciproflaxacin, erythromycin Rifampicin Isoniazid St Johns Wort Amiodarone Chronic Alcohol intake Allopurinol Smokers (CYP 1 A 2) Anti-fungal: ketoconazole, fluconazole SSRI: fluoxetine, sertraline Sodium Valproate Acute Alcohol
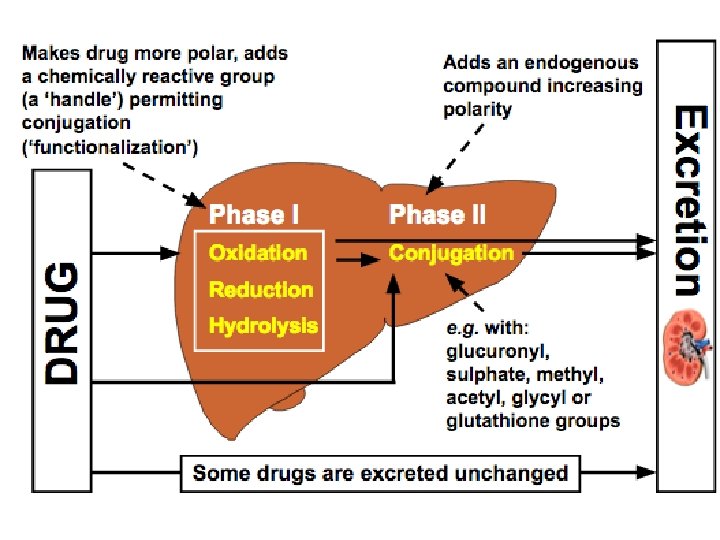

4. Elimination Renal • Excretion via urine • Must be sufficiently polar (role of phase 2) • Renal dysfunction = drug accumulation Other Routes • Intestines (faecal) • Bile • Lungs • Breast milk

Pharmacodynamics Definition • What the drug does to the body • It’s effect on cellular receptors via signal transduction Signal Transduction • Binding of drug to extracellular or intracellular receptor • Via a variety of receptors: ligand-gated ion channels, G protein-coupled receptors etc… • Leads to amplification or down -regulation of signals Intrinsic Effect • Agonist: full (equivalent to endogenous agonist), partial • Antagonist: competitive (reversibly prevents endogenous agonist binding), irreversible (covalent bond), allosteric (binds to other site, irreversible)
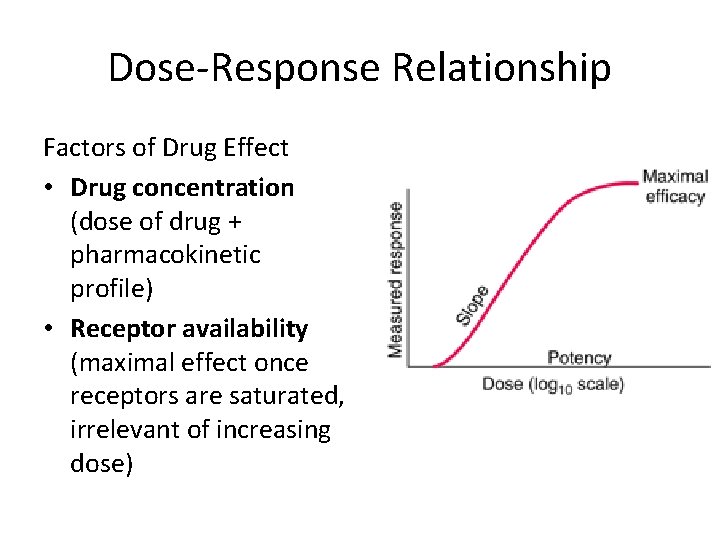
Dose-Response Relationship Factors of Drug Effect • Drug concentration (dose of drug + pharmacokinetic profile) • Receptor availability (maximal effect once receptors are saturated, irrelevant of increasing dose)
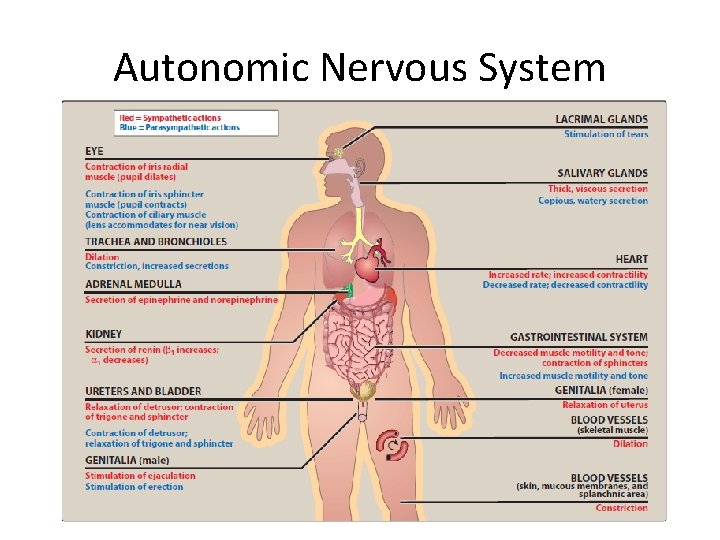
Autonomic Nervous System
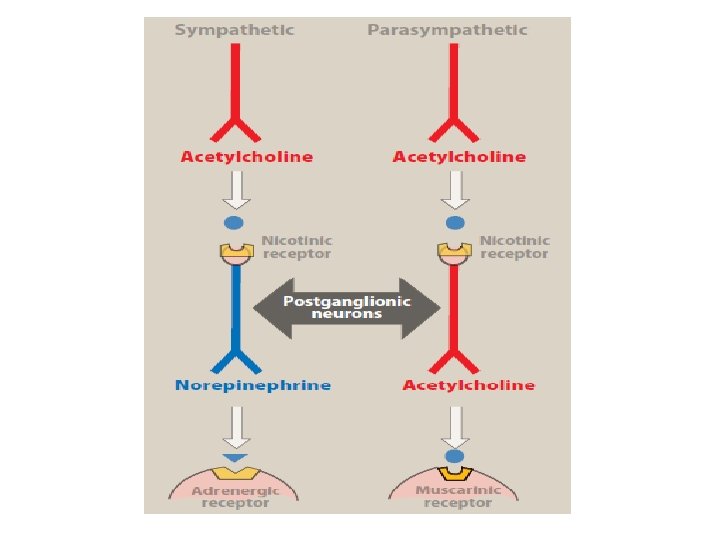
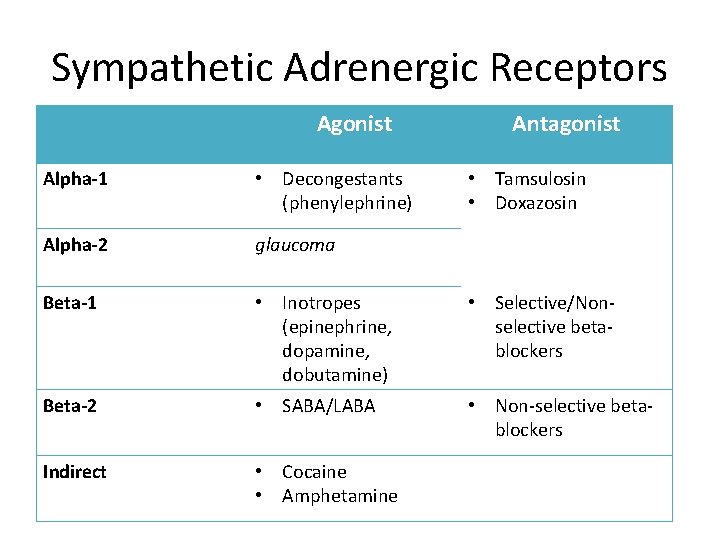
Sympathetic Adrenergic Receptors Agonist Antagonist Alpha-1 • Decongestants (phenylephrine) • Tamsulosin • Doxazosin Alpha-2 glaucoma Beta-1 • Inotropes (epinephrine, dopamine, dobutamine) • Selective/Nonselective betablockers Beta-2 • SABA/LABA • Non-selective betablockers Indirect • Cocaine • Amphetamine
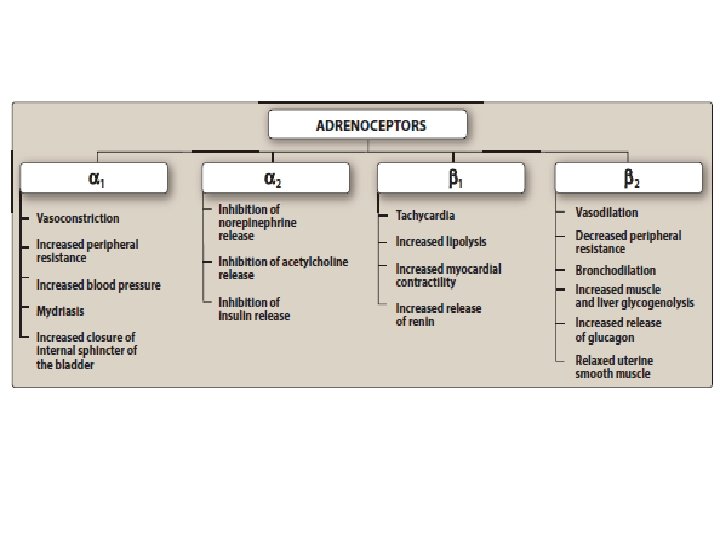

Parasympathetic Muscarinic Receptor Agonist glaucoma Antagonist • Atropine • SAMA/LAMA • Oxybutynin (indirect) • Donepezil, Galantamine • Rivastigmine, Pyridostigmine, (indirect) Neostigmine • Rocuronium, Vecuronium
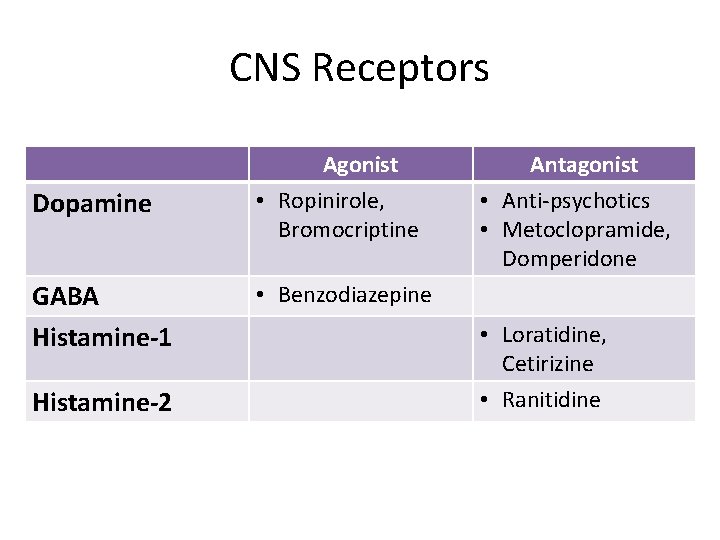
CNS Receptors Dopamine GABA Histamine-1 Histamine-2 Agonist • Ropinirole, Bromocriptine Antagonist • Anti-psychotics • Metoclopramide, Domperidone • Benzodiazepine • Loratidine, Cetirizine • Ranitidine
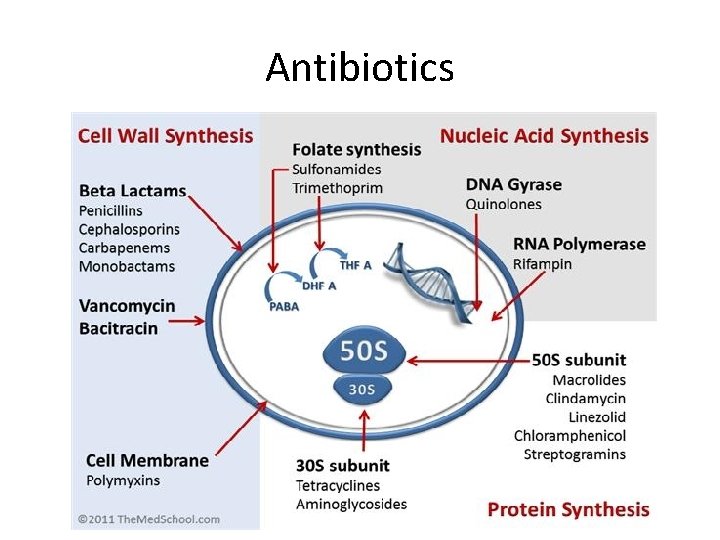
Antibiotics

Common Infections and Abx CAP • Amoxicillin +/Clarithromycin Atypical CAP • Clarithromycin IECOPD • Amoxicillin / Clarithromycin / Doxycline HAP • Co-Amoxiclav / Cefuroxime / Tazocin TB • RIPE Cellulitis • Flucloxacillin UTI • Trimethoprim / Nitrofurantoin Acute Pyelonephritis • Co-Amoxiclav / Ciprofloxacin

Common Infections and Abx Gonorrhoea • Ceftriaxone (IM) + Azithromycin (PO) Chlamydia • Doxycycline / Azithromycin (PO) Syphilis • Benzathine benzylpenicillin Gastroenteritis • (Campylobacter) Clarithromycin • (Salmonella/Shigella) Ciprofloxacin C. Difficile • 1 st: Metronidazole • 2 nd: Vancomycin Acute Abdominal Infections (e. g. appendicitis) • Cef + Met
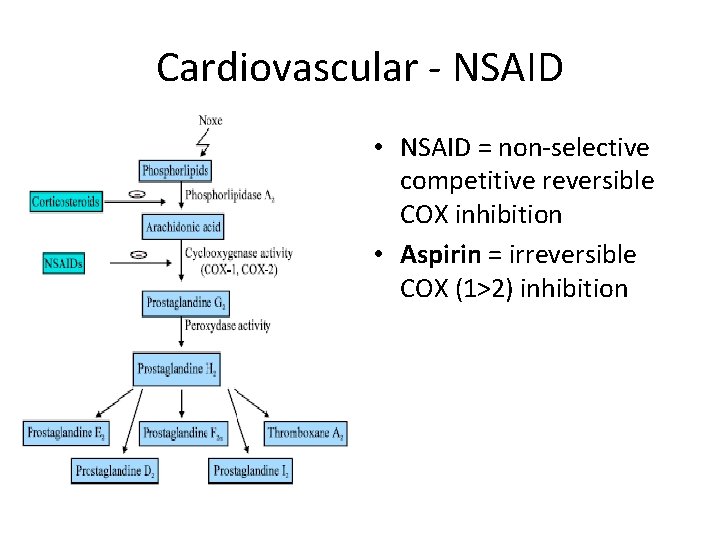
Cardiovascular - NSAID • NSAID = non-selective competitive reversible COX inhibition • Aspirin = irreversible COX (1>2) inhibition
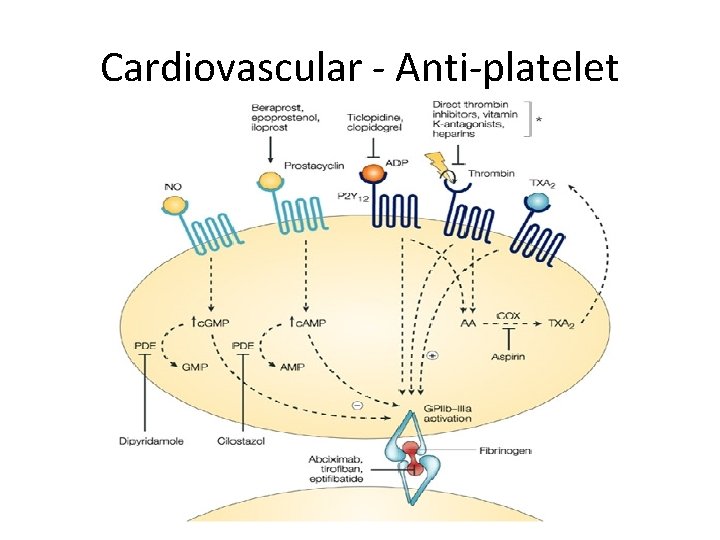
Cardiovascular - Anti-platelet
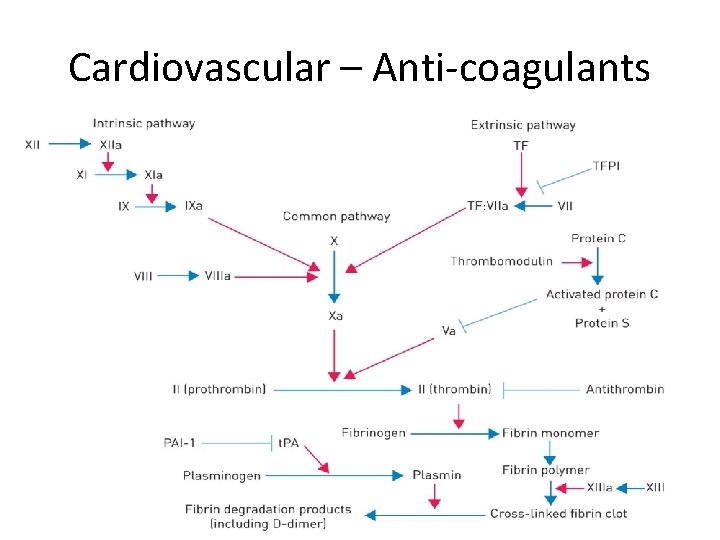
Cardiovascular – Anti-coagulants

Cardiovascular – Anti-coagulants Heparin • Activates Antithrombin (decreased thrombin and factor Xa), short half-life. • LMWH (dalteparin): activates antithrombin (decreased factor Xa) and have longer half-life • Increased APPT, Monitor using anti-factor Xa assay • SE: Bleeding, thrombocytopenia (heparininduced thrombocytopenia), osteoporosis Warfarin • Anti-Vitamin K = Decreased FII (prothrombin)/VII/IX/X and Protein C/S • Increased PT/INR • SE: Bleeding, Skin/Tissue Necrosis, Teratogenic • Reversal = Vitamin K Direct Factor Xa Inhibitors • e. g. Apixaban, Rivaroxaban • Directly inhibit FXa • SE: Bleeding (no reversal agent) Thrombolytics • e. g. Alteplase/Tenecteplase (t. PA), Streptokinase • Activate Plasminogen -> Plasmin, Increased PT/APPT • SE: Bleeding
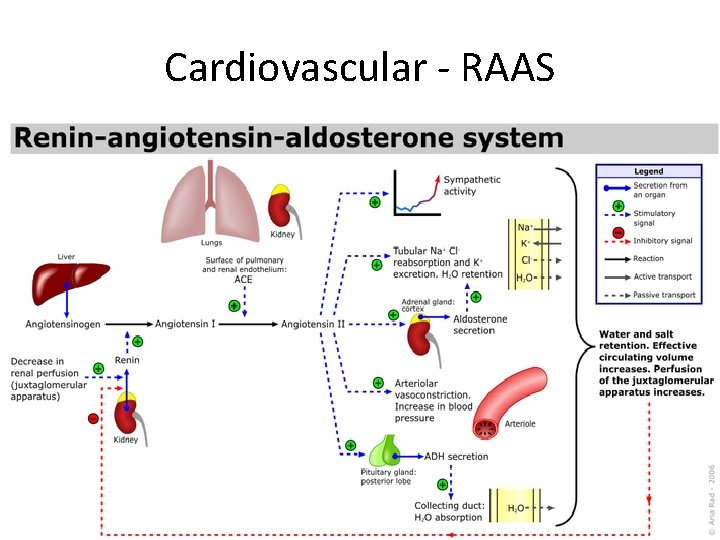
Cardiovascular - RAAS

Cardiovascular - RAAS JG cells release renin in response to: • Decrease BP detected by baroreceptors in afferent vascular walls • Decrease Na+ delivery to macula densa cells • Increase sympathetic stimulation (Beta-1) ACE functions: • Catalyses conversion of angiotensin I to angiotensin II • Degraded by bradykinin Angiotensin II effects: • Systemic arteriole vasoconstriction • Kidney efferent>afferent constriction = Increase Glomerular Pressure = Maintain GFR despite lowered overall kidney blood flow • Kidney proximal tubule/thick ascending limb Na+/H+ exchanger stimulation = Increased Na+/HCO 3/H 20 reabsorption • Adrenal cortex = Aldosterone release • Posterior Pituitary = ADH release
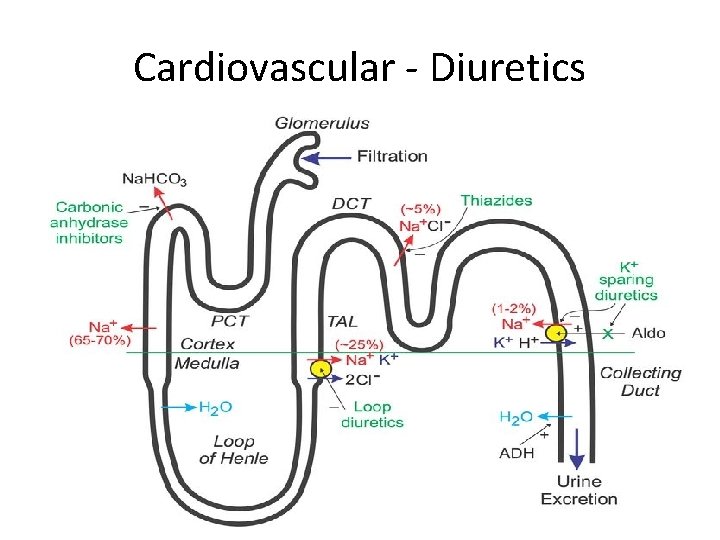
Cardiovascular - Diuretics

Cardiovascular - Diuretics Loop Diuretics (furosemide, bumetanide) • Inhibit Na/K/Cl cotransporter of thick ascending limb • IND: Oedematous States (HF, Cirrhosis, Nephrotic Syndrome, Pulmonary Oedema), HTN, Hypercalcaemia • SE: ototoxicity, hypokalaemia, dehydration, AKI, gout Thiazide Diuretics (bendroflumethiazide) • Inhibit Na/Cl cotransporter of distal tubule • IND: HTN, HF, Nephrogenic DI • SE: hypokalaemic metabolic alkalosis, hyponatraemia, hyperglycaemia, hypercalcaemia, hyperuricaemia Spironolactone • Spironolactone = competitive aldosterone receptor antagonists in collecting tubules • IND: HF, Hyperaldosteronism, Hypokalaemia • SE: hyperkalaemia, antiandrogen effects, e. g. gynaecomastia, loss of libido, erectile dysfunction
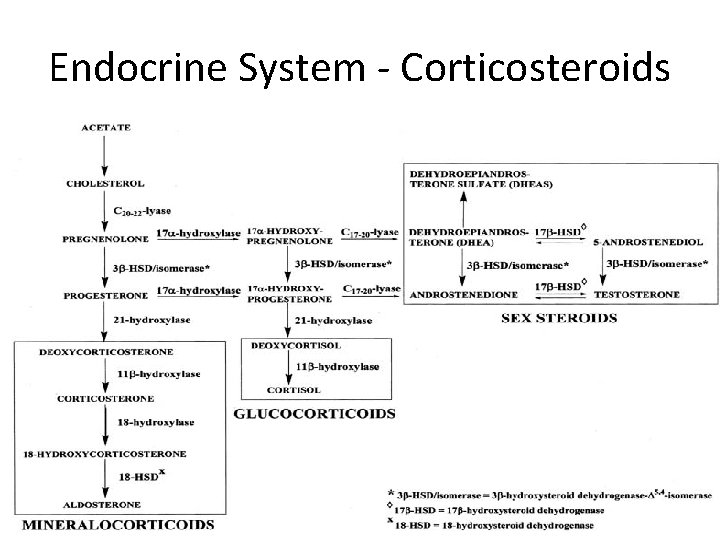
Endocrine System - Corticosteroids
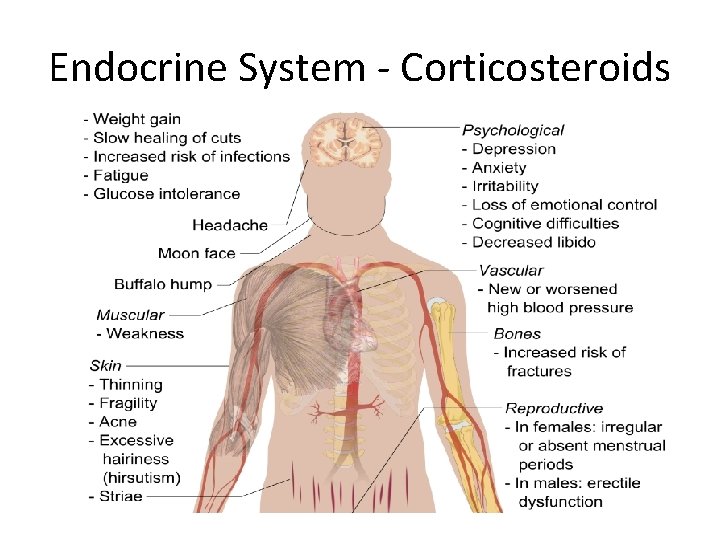
Endocrine System - Corticosteroids
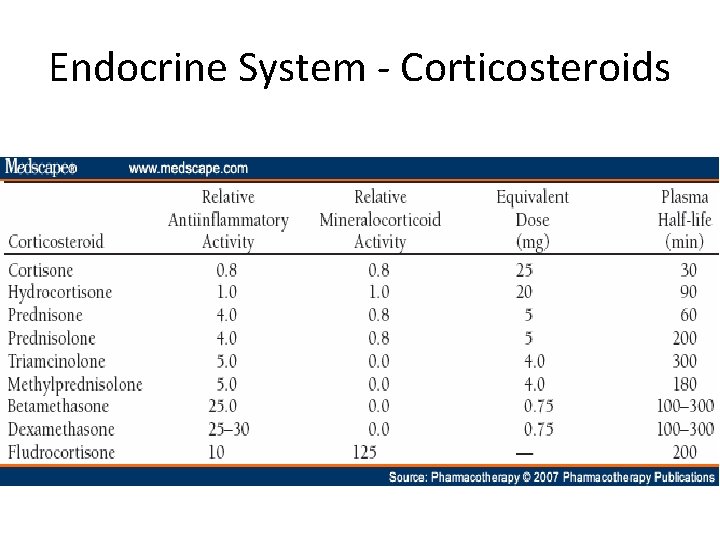
Endocrine System - Corticosteroids
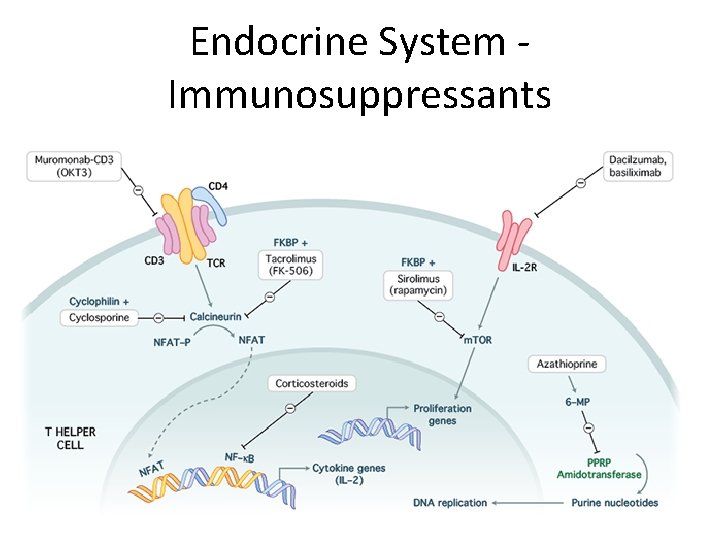
Endocrine System Immunosuppressants
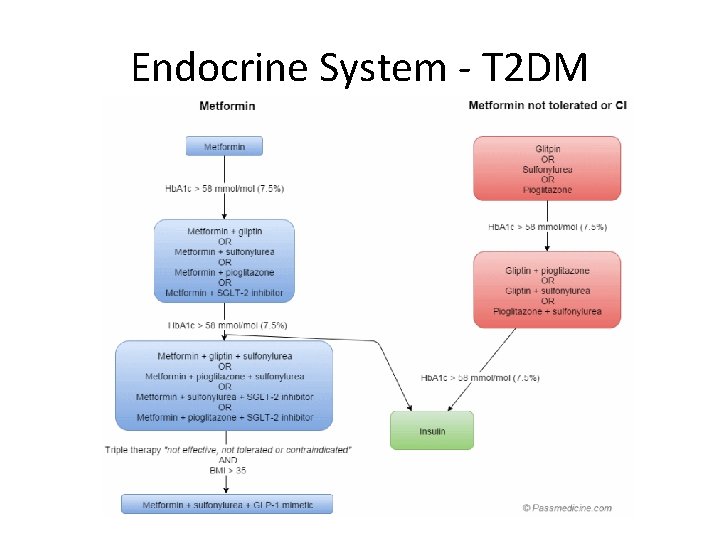
Endocrine System - T 2 DM
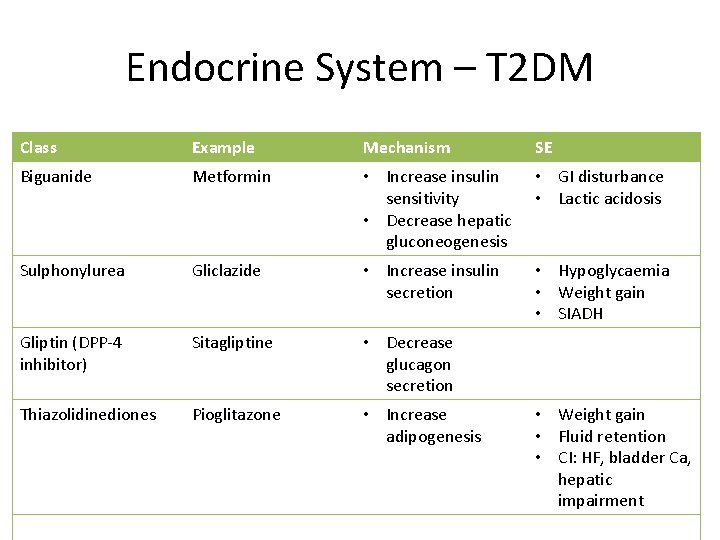
Endocrine System – T 2 DM Class Example Mechanism SE Biguanide Metformin • Increase insulin sensitivity • Decrease hepatic gluconeogenesis • GI disturbance • Lactic acidosis Sulphonylurea Gliclazide • Increase insulin secretion • Hypoglycaemia • Weight gain • SIADH Gliptin (DPP-4 inhibitor) Sitagliptine • Decrease glucagon secretion Thiazolidinediones Pioglitazone • Increase adipogenesis • Weight gain • Fluid retention • CI: HF, bladder Ca, hepatic impairment
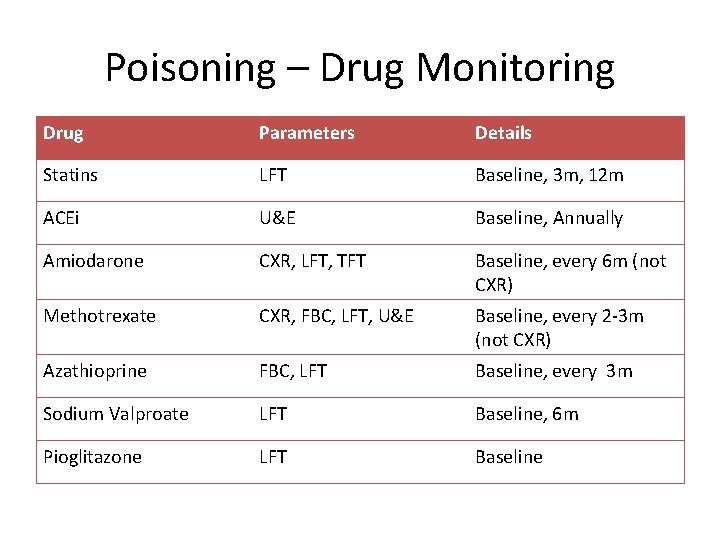
Poisoning – Drug Monitoring Drug Parameters Details Statins LFT Baseline, 3 m, 12 m ACEi U&E Baseline, Annually Amiodarone CXR, LFT, TFT Baseline, every 6 m (not CXR) Methotrexate CXR, FBC, LFT, U&E Baseline, every 2 -3 m (not CXR) Azathioprine FBC, LFT Baseline, every 3 m Sodium Valproate LFT Baseline, 6 m Pioglitazone LFT Baseline
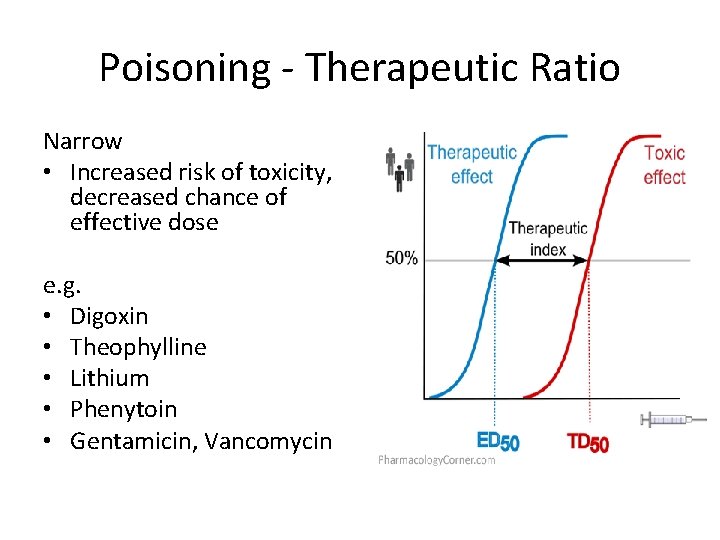
Poisoning - Therapeutic Ratio Narrow • Increased risk of toxicity, decreased chance of effective dose e. g. • Digoxin • Theophylline • Lithium • Phenytoin • Gentamicin, Vancomycin

Poisoning - Overdose Management <1 hr following ingestion • PO Activated Charcoal Digoxin • Digoxin-specific antibody fragments Salicylate (aspirin) • Haemodialysis Carbon Monoxide • 100% Oxygen Opiate/Opioid • Naloxone Organophosphate Insecticides • Atropine

Poisoning – Paracetamol Overdose Pathology • Phase 2 conjugation pathway saturated • Alternative pathway used = NAPQI = glutathione depletion • Glutathione depletion = liver/renal necrosis Risk Factors • Psychiatric Hx • Elderly, Low weight • P 450 inducers Investigation • Serum paracetamol level • U&E, LFT, Glucose, Clotting, ABG Management • IV N-acetylcysteine - On/above nomogram line - Staggered overdose - Doubt over ingestion time • Liver transplant
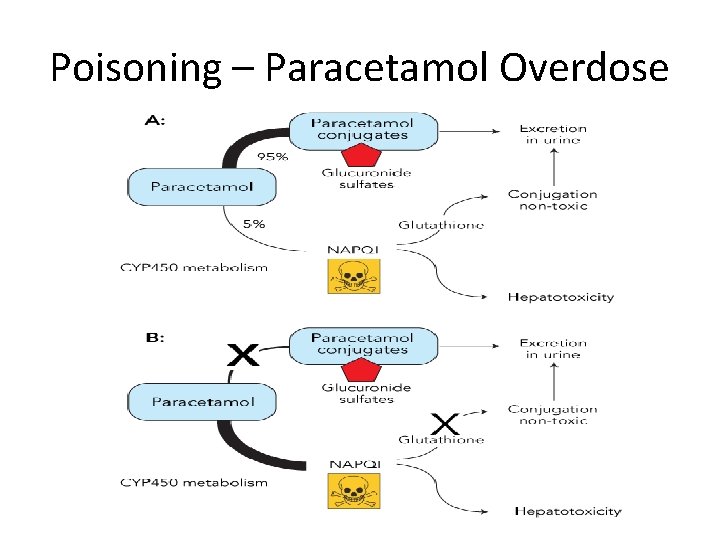
Poisoning – Paracetamol Overdose
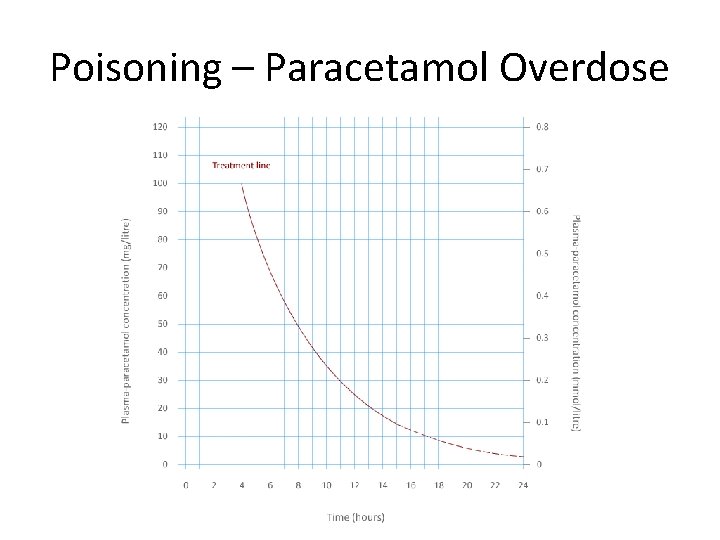
Poisoning – Paracetamol Overdose
- Slides: 46