Pharmacology of Autonomic System Munir Gharaibeh MD Ph

Pharmacology of Autonomic System Munir Gharaibeh. MD, Ph. D, MHPE Departmrnt of Pharmacology Faculty of Medicine mgharaib@ju. edu. jo

The Nervous System n Central Nervous System: n n Brain and Spinal cord Peripheral Nervous System: n Autonomic nervous System: n Parasympathetic System n Sympathetic System or Adrenergic System n Somatic Nervous System: October 20 Munir Gharaibeh, MD, Ph. D, MHPE
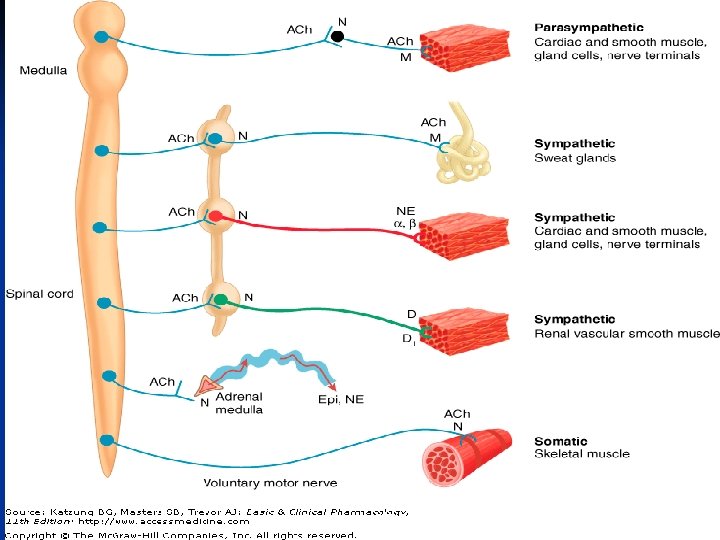
October 20 Munir Gharaibeh, MD, Ph. D, MHPE
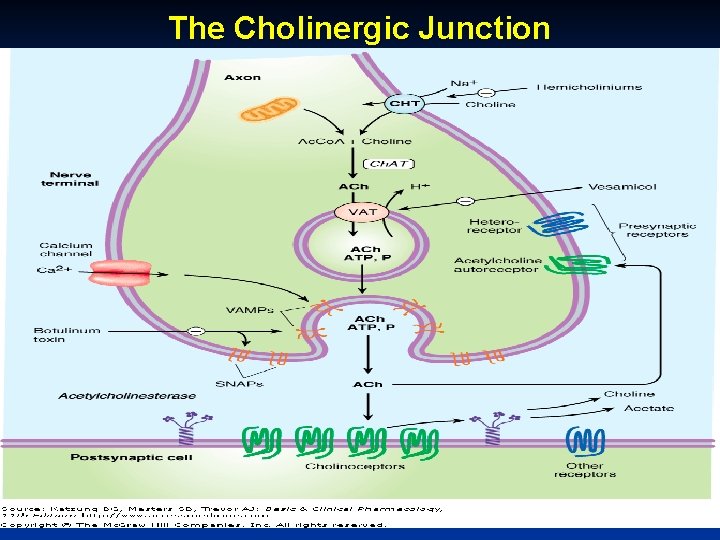
The Cholinergic Junction October 20 Munir Gharaibeh, MD, Ph. D, MHPE
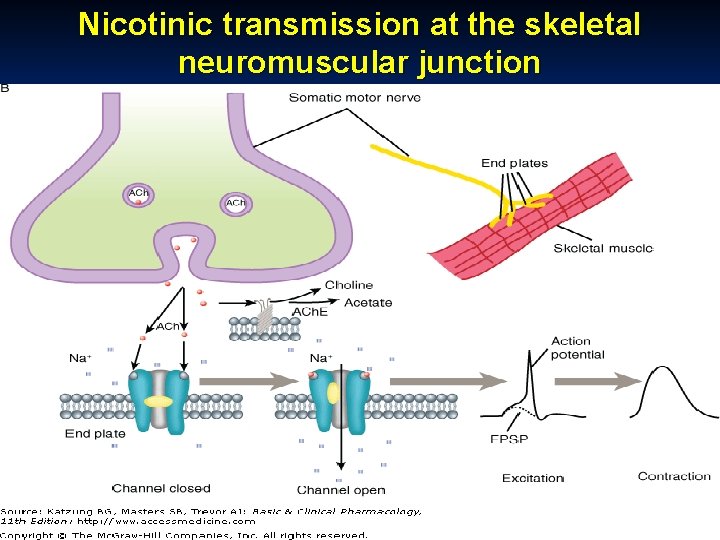
Nicotinic transmission at the skeletal neuromuscular junction October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Life Cycle of Acetylcholine Choline is transported into the presynaptic nerve terminal by a sodium-dependent choline transporter (Ch. T). This transporter can be inhibited by hemicholinium drugs. n In the cytoplasm, acetylcholine is synthesized from choline and acetyl Co-A (Ac. Co. A) by the enzyme choline acetyltransferase (Ch. AT). n Acetylcholine is then transported into the storage vesicle by a second carrier, the vesicle-associated transporter (VAT), which can be inhibited by vesamicol. n Peptides (P), adenosine triphosphate (ATP), n October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Life Cycle of Acetylcholine Release of transmitter occurs when voltagesensitive calcium channels in the terminal membrane are opened, allowing an influx of calcium. The resulting increase in intracellular calcium causes fusion of vesicles with the surface membrane and exocytotic expulsion of acetylcholine and cotransmitters into the junctional cleft. This step can be blocked by botulinum toxin. n Acetylcholine's action is terminated by metabolism by the enzyme acetylcholinesterase. n Receptors on the presynaptic nerve ending n October 20 Munir Gharaibeh, MD, Ph. D, MHPE
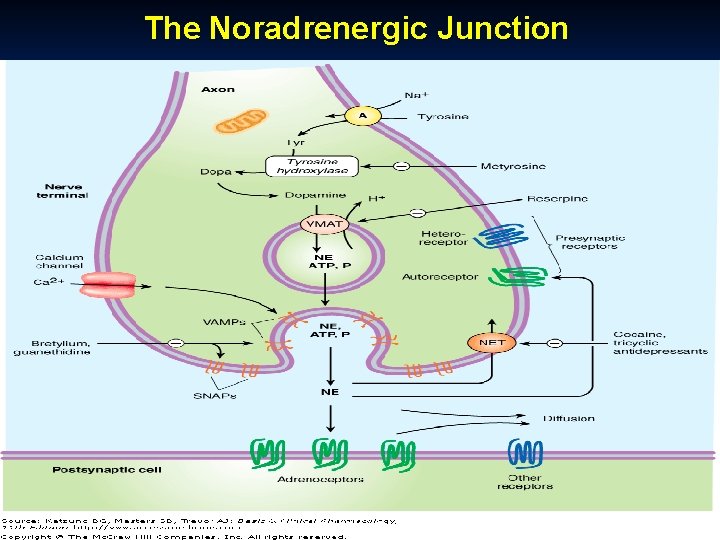
The Noradrenergic Junction October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Life Cycle of Noradrenaline Tyrosine is transported into the noradrenergic ending or varicosity by a sodium-dependent carrier (A). n Tyrosine is converted to dopa and then to dopamine which is then transported into the vesicle by the vesicular monoamine transporter (VMAT), which can be blocked by reserpine. n Dopamine is converted to NE in the vesicle by dopamine- -hydroxylase. n October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Life Cycle of Noradrenaline n n Physiologic release of transmitter occurs when an action potential opens voltage-sensitive calcium channels and increases intracellular calcium. Fusion of vesicles with the surface membrane results in expulsion of norepinephrine, cotransmitters, and dopamine- -hydroxylase. Release can be blocked by drugs such as guanethidine and bretylium. Norepinephrine diffuses out of the cleft or is transported into the cytoplasm of the terminal by the norepinephrine transporter (NET), which can be blocked by cocaine and tricyclic antidepressants, or into postjunctional or perijunctional cells. Regulatory receptors are present on the presynaptic terminal. October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Effects of Sympathetic and Parasympathetic Activity Function Sympathetic Parasympathetic Heart rate Increased Slowed Blood vessels Constricted Dilated Stomach and intestine Decreased activity and secretions Increased activity and secretions Salivary and bronchial glands Decreased secretion Increased secretion Urinary bladder Body relaxed, Body contracted, sphincter constricted sphincter relaxed Bronchial muscle Relaxed Blood sugar Raised Eye Pupils dilated October 20 Munir Gharaibeh, MD, Ph. D, MHPE Contracted Pupils constricted, accommodation for near vision
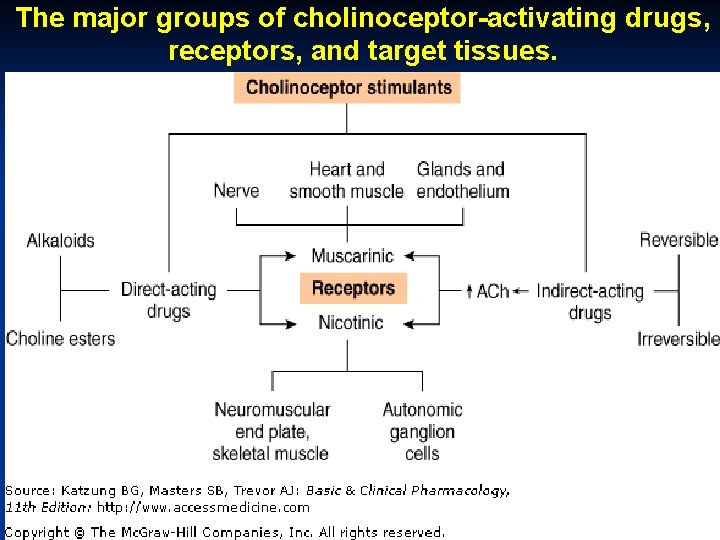
The major groups of cholinoceptor-activating drugs, receptors, and target tissues. October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Cholinergic Agonists or Parasympathomimetics Cholinergic agonists can work on all parts of the parasympathetic system, parts of the sympathetic system, and the somatic system. n Choline Esters. n Alkaloids. n Cholinesterase Inhibitors or Anticholinesterases. October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Cholinergic Agonists or Parasympathomimetcs n Choline Esters: n Acetylcholine: n Naturally released from the cholinergic nerve endings is very short acting because of rapid hydrolysis by AChase enzyme. n Used only in experimentation. Methacholine. n Bethanechol. n Carbachol: n n Synthetic, long acting. n Used in postoperative atony. n Causes flushing, sweating, colic. October 20 Munir Gharaibeh, MD, Ph. D, MHPE
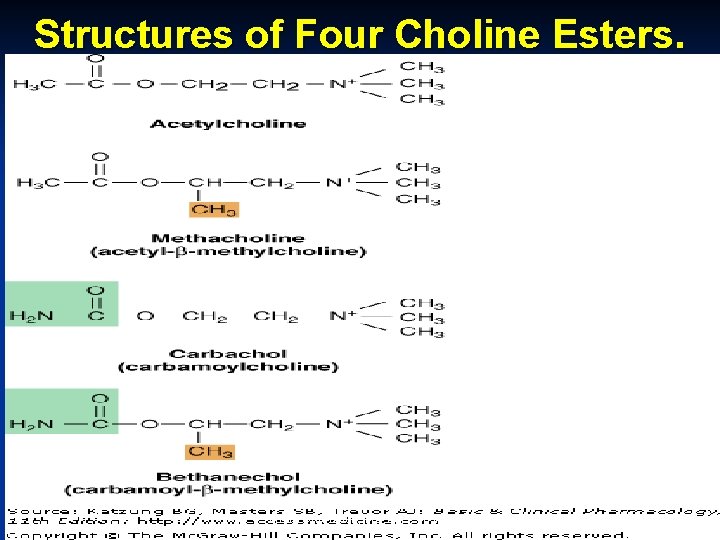
Structures of Four Choline Esters. October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Cholinergic Agonists or Parasympathomimetcs n Alkaloids: Muscarine n Nicotine. n Pilocarpine. n October 20 Munir Gharaibeh, MD, Ph. D, MHPE
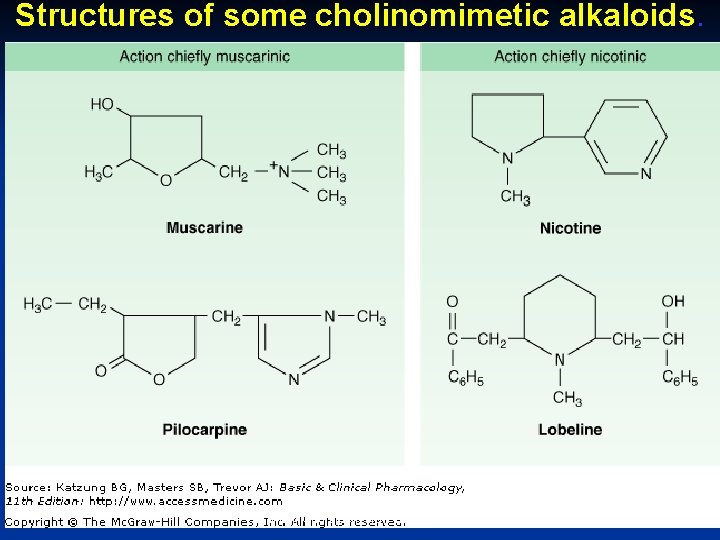
Structures of some cholinomimetic alkaloids. October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Cholinergic Agonists or Parasympathomimetcs n Cholinesterase Inhibitors or Anticholinesterases: n Prevent breakdown of ACh by cholinestearse. n Reversible: n Neostigmine: n Used in Myasthenia Gravis, Paralytic Ileus, and postoperative atony of the bladder. n Irreversible: n Parathion, Malathion: n Used as potent insecticides October 20 Munir Gharaibeh, MD, Ph. D, MHPE
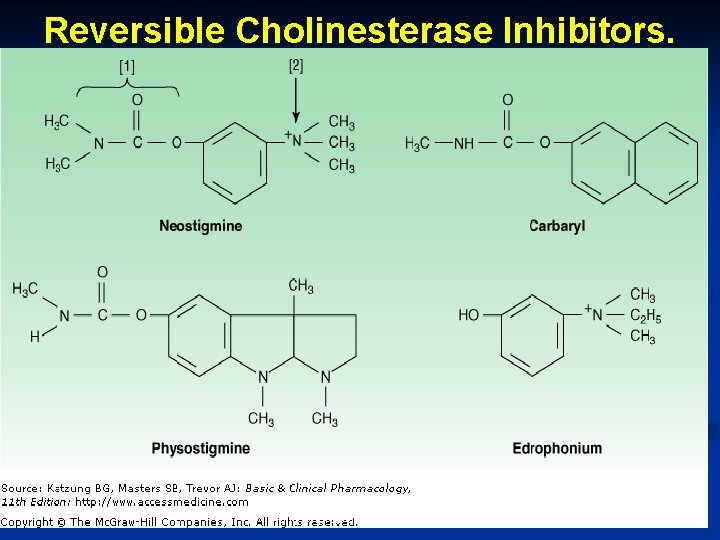
Reversible Cholinesterase Inhibitors. October 20 Munir Gharaibeh, MD, Ph. D, MHPE
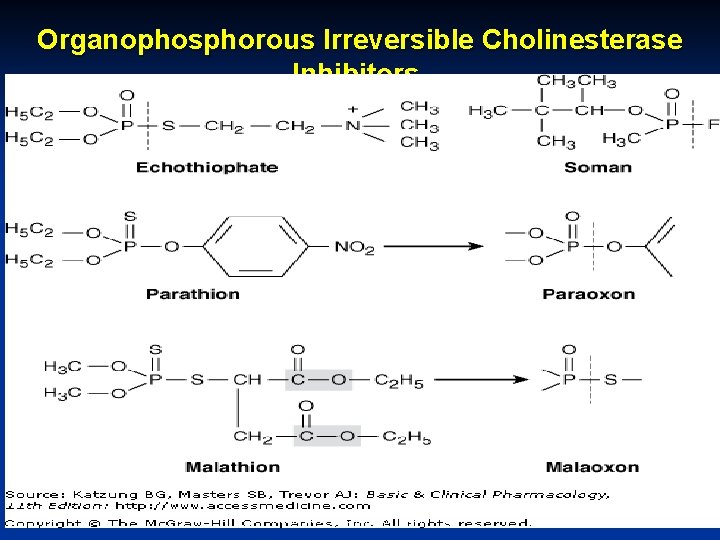
Organophosphorous Irreversible Cholinesterase Inhibitors. October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Organophosphate Poisoning Very potent agricultural insecticides and lethal war weapons. n Very easily absorbed through all parts of the skin. n Inhibit the enzyme and cause accumulation of ACh at all sites. n October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Organophosphate Poisoning Tissue or System Effects Skin Sweating Visual Lacrimation, miosis, blurring, spasm Digestive Salivation, increased secretions, tone, and motility (cramps, vomiting, diarrhea, and defecation) Urinary Frequency and incontinence Respiratory Increased secretions, bronchoconstriction, weakness of muscles Skeletal muscle Fasiculation, weakness, paralysis Cardivascular Bradycardia, decreased cardiac output, hypotension. CNS Tremor, anxiety, restlessness, confusion, convulsions, Munir Gharaibeh, MD, Ph. D, MHPE coma October 20

Treatment of Organophosphate Poisoning Stop the exposure, wash extensively, very lipid soluble. n Atropine, a parasympatholytic drug, in very large doses, until the appearance of Atropine Poisoning. n Pralidoxime, when given very early after the poisoning, can regenerate the enzyme. n October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Cholinergic Blockers or Parasympatholytics n Nicotinic Blockers: Curare-like drugs. n Muscarinic Blockers: Atropine –like drugs. October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Atropine –like Drugs n Atropine: n Natural. n Absorbed from all routes. n Actions: n GIT: Reduces motility and secretions. n Heart: inhibits vagus nerve causing tachycardia. n Lungs: relaxes bronchioles but reduces secretions. n Smooth muscles: relaxes renal and biliary Munir Gharaibeh, MD, Ph. D, MHPE October 20 tracts.

Atropine –like Drugs n Atropine: n Clinical Uses: n Smooth muscle spasm. n Eye examination. n Preoperative medication. n Adverse effects: n Dryness, redness, Hotness. n Constipation, Urinary retention. n Paralysis of accommodation. n Restlessness, hallucinations, and Delirium. n Antidote for toxicity: Physostigmine. October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Atropine –like Drugs n Hyoscine (Scopolamine): Also natural product. n Similar peripheral effects. n CNS depressant leading to drowsiness and sleep. n Used for motion sickness n Mebeverine n Propantheline n Both are synthetic. n Were used in peptic ulcer disease. n Still used for irrtiable bowel syndrome (combined with. Munir anxiolytic). Gharaibeh, MD, Ph. D, MHPE October 20 n

Sympathomimetic Drugs or Adrenergic Agonists These are the drugs which are given to mimic the actions of the sympathetic nervous system. n They are given in high concentrations relative to the endogenously released neurotransmitters after sympathetic nerve endings. n Directly Acting n Indirectly Acting n October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Sympathomimetic Drugs or Adrenergic Agonists n Directly Acting Drugs: These work directly on the adrenergic receptors. n Norepinephrine or Noradrenalin: n Epinephrine or Noradrenaline: n Isoprenaline n Dopamine n Salbutamole n Indirectly Acting: Amphetamine n Ephedrine n October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Sympathomimetic Drugs or Adrenergic Agonists n Directly Acting: n Norepinephrine or Noradrenalin: n Natural product which is purely α receptor agonist. n Given only IV. n Raises both systolic and diastolic pressure. n Was widely use in shock but caused a lot of gangrene. October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Sympathomimetic Drugs or Adrenergic Agonists n Directly Acting: n n Norepinephrine or Noradrenalin. Epinephrine or Noradrenaline: n n n n n Has mixed α and β agonistic activities. Given IM, SC, also intracardic. Increases force and rate of contraction of the heart. Raises systolic blood pressure. Brochodilator. Increases blood sugar. Used in anaphylactic shock and as a last resort in cardiac arrest. Isoprenaline Dopamine Salbutamole. October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Sympathomimetic Drugs or Adrenergic Agonists n Directly Acting: Norepinephrine or Noradrenalin: n Epinephrine or Noradrenaline: n Isoprenaline: n n Purely β 1 and β 2 agonist. n Has little effects on BP n Can cause cardiac arrhythmias. n Was used in bronchial asthma, but cardiotoxic. Dopamine. n Salbutamol. n October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Sympathomimetic Drugs or Adrenergic Agonists n Directly Acting: Norepinephrine or Noradrenalin: n Epinephrine or Noradrenaline: n Isoprenaline: n Dopamine: n n Has mixed α , β, and dopamine receptor (DA) agonistic activities. n DA receptors are present in the renal vessels and cause vasodilation. n Vasoconstriction elsewhere. n Increases BP. n Stimulates the heart. n 20 Very useful in shock. Munir Gharaibeh, MD, Ph. D, MHPE October

Positive Inotropic Agents Dopamine: Widely used in cardiogenic shock. Low doses: stimulates DA 1 receptors leading to renal vasodilation and improved renal function. Intermediate doses: works on β 1 receptors leading to positive inotropic actions. High doses: stimulates α receptors leading to vasoconstriction and elevation of blood pressure. Can cause arrhythmias and ischemic changes. Dobutamine: Selective β 1 agonist, used intermittently (IV) in CCHF. Has more inotropic than chronotropic actions. October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Sympathomimetic Drugs or Adrenergic Agonists n Directly Acting: Norepinephrine or Noradrenalin n Epinephrine or Noradrenaline n Isoprenaline n Dopamine. n Salbutamol: n n Selective β 2 agonist. n Powerful bronchodilator. n Can inhibit uterine muscle. n Given orally, IV, inhalation. n In high doses can cause tremor and tachycardia. October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Sympathomimetic Drugs or Adrenergic Agonists Directly Acting. n Indirectly Acting: n Amphetamine n Ephedrine. These are lipophilic commpounds, so can cross the BBB causing mainly CNS effects: Euphoria, abolish fatigue, increase activity, and reduce appetite. Carry the risk of dependence. Use limited to narcolepsy and hyperactive children Should not be used for appetite suppression. n October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Bronchial Asthma Is a chronic relapsing disease characterized by wheezing due to bronchospasm, infection, and excessive mucus production. n Due to antigen -antibody interaction which causes the release of inflammatory mediators. n Precipitated by cold exposure, exercise, infection, stress, dust, etc… n October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Drug Treatment of Bronchial Asthma. Bronchdilators. n Corticosteroids. n Mast cell stabilizers. n Leukotriene Modifiers. n Antimicrobials. n Hydration, expectorants and mucolytic drugs. n October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Drug Treatment of Bronchial Asthma. n Bronchdilators. n Β 2 agonists: e. g. Salbutamol, Terbutaline n Used during or just before the attack or regularly. n Can be given by inhalation, IV, or orally. n Methylxanthines; e. g. Aminophylline and Theophylline: n n n Inhibit Phosphodiesterase enzyme which breaks down c. AMP. Toxic: so blood levels should be monitored. Given slowly IV, or orally, and rectally. Can cause nausea, anxiety, tachycardia, arrhythmias, and convulsions. Interactions are very common. Ipratropium Bromide: n Atropine-like October 20 drug which is given by inhalation. Munir Gharaibeh, MD, Ph. D, MHPE

Adrenergic Blocking Drugs “Sympatholytics” n α-adrenergic n blockers: Block the sympathetic effects on α -adrenergic receptors. n Used in hypertension and bladder neck obstruction (benign prostatic hypertrophy). n Prazosin. n Terazosin. n Doxazocin (Cardura) n β-adrenergic n blockers: Block the sympathetic effects on β -adrenergic receptors. n Differ in their Selectivity and Pharmacokinetics October 20 Munir Gharaibeh, MD, Ph. D, MHPE

β-adrenergic Blockers n Nonselective β-Blockers: n n n Selective β-Blockers: n n n Block both β 1 and β 2 receptors. Propranolol: prototype. Nadolol Sotalol. Block β 1 more than β 2 receptors. Metoprolol Atenolol Bisoprolol Combined α and β-Blockers: Labetalol n Carvedilol October 20 n Munir Gharaibeh, MD, Ph. D, MHPE

β-adrenergic Blockers n Actions: n Prevent the actions of the sympathetic system, i. e. more active when the system is overactive. Reduce heart’s: rate, contractility, and excitability, and consequently reduce cardiac output. n Reduce BP. n Bronchoconstriction. n Prevent glycogenolysis (the rise in blood sugar). n Mask the symptoms of hypoglycemia. n CNS: sedation, dreams, hallucinations, depression. n October 20 Munir Gharaibeh, MD, Ph. D, MHPE

β-adrenergic Blockers n Clinical Uses: n Ischemic heart disease. n Hypertension. n Cardiac arrhythmias. n Throtoxicosis. n Anxiety: actually only block the sympathetic symptoms of anxiety. So very effective in Stage-Fright. n Essential tremor. n Migraine. October 20 Munir Gharaibeh, MD, Ph. D, MHPE

β-adrenergic Blockers n Adverse Effects: n Myocardial suppression, i. e. ? possibility of heart failure with high doses. n Bronchospasm or bronchial asthma. n CNS effects: fatigue, bad dreams, depression, sexual impairment. n Cold extremities, due to unmasking of α receptors. n Mask the symptoms of hypoglycemia which might lead to more hypoglycemia and coma. October 20 Munir Gharaibeh, MD, Ph. D, MHPE

5 -Hydroxytryptamine(5 -HT) or Serotonin Important neurotransmitter. n Actions in the brain, intestine, blood vessels. n Abnormalities are involved in several disorders: n Depression. n Vomiting caused by cytotoxic drugs. n Migraine headache. n Carcinoid Tumor of the GIT n October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Migraine Headache Migraine is characterized by recurrent attacks of headache, unilateral and pulsating, may be preceded by visual disturbances (Aura), often familial and may be precipitated by trigger factors. n Mechanism: n n Vasospasm followed by vasodilation of the cerebral vessels associated with release of mediators causing pain sensation in the area of the trigeminal nerve. October 20 Munir Gharaibeh, MD, Ph. D, MHPE

Treatment of Migraine Headache n Acute Attack: n n Analgesics: Aspirin, Paracetamole. Sumatriptan: n n n Stimulates 5 -HT receptors resulting in constriction. Given SC immediately after onset. Also given orally and as nasal spray. Can cause tightness in the chest, dizziness and nausea. Expensive. Ergotamine: From a fungus. n Stimulates α and 5 -HT receptors. n Was widely used, orally, rectally, and aerosol. n Combined with caffeine or Cyclizine (an anti emetic). n Toxic: vomiting, diarrhea, gangrene, tingling, numbness. n 20 Withdrawal causes headache. Munir Gharaibeh, MD, Ph. D, MHPE October n

Treatment of Migraine Headache Prevention: n β-Blockers: n Reduce n vasodilation. Pizotifen: n 5 -HT antagonist. n Causes drowsiness, weight gain. n Sodium valproate; n Antiepileptic n Can cause fetal malformations, liver damage, and platelet dysfunction Antidepressants n Methysergide: n n 5 -HT October 20 antagonist. Munir Gharaibeh, MD, Ph. D, MHPE
- Slides: 48