Pharmacology GIT drugs Ita Armyanti FARMAKOLOGI dan BIOETIKA

Pharmacology : GIT- drugs Ita Armyanti FARMAKOLOGI dan BIOETIKA PSPD FK UNTAN 1 GIT-drugs/2013 23/11/2020

KAPITA SELEKTA GASTROINTESTINAL Drugs used in acid peptic diseases Drugs stimulating gastrointestinal motility Laxatives Antidiarrheal agents Drugs used in the treatment of Irritable Bowel Syndrome Drugs used to treat inflammatory bowel disease 2 GIT-drugs/2013 23/11/2020

Gastric acidity and Peptic Ulcer Disease Factors that Increase Acidity 6 GIT-drugs/2013 Factors that Protect Against Acidity 23/11/2020

Peptic Ulcer Disease Imbalance between defenses and aggressive factors Defensive factors: 1. Mucus: continually secreted, protective effect 2. Bicarbonate: secreted from endothelial cells 3. Blood flow: good blood flow maintains mucosal integrity 4. Prostaglandins: stimulate secretion of bicarbonate an mucus, promote blood flow, suppress secretion of gastric acid 7 GIT-drugs/2013 23/11/2020

Aggressive factors: 1. Helicobacter pylori: gram negative bacteria, live in stomach and duodenum, may breakdown mucus layer => inflammatory response to presence of the bacteria also produces urease forms CO 2 and ammonia which are toxic to mucosa 2. Gastric Acid: needs to be present for ulcer to form => activates pepsin and injures mucosa 3. Decreased blood flow: causes decrease in mucus production and bicarbonate synthesis, promote gastric acid secretion 4. NSAIDS: inhibit the production of prostaglandins 5. 8 Smoking: nicotine stimulates gastric acid 23/11/2020 GIT-drugs/2013 production

Classes of Agents 1. Proton Pump Inhibitors 2. Histamine H 2 -Receptor Antagonists 3. Prostaglandin Analogs 4. Cytoprotectants 5. Antacids 9 GIT-drugs/2013 23/11/2020
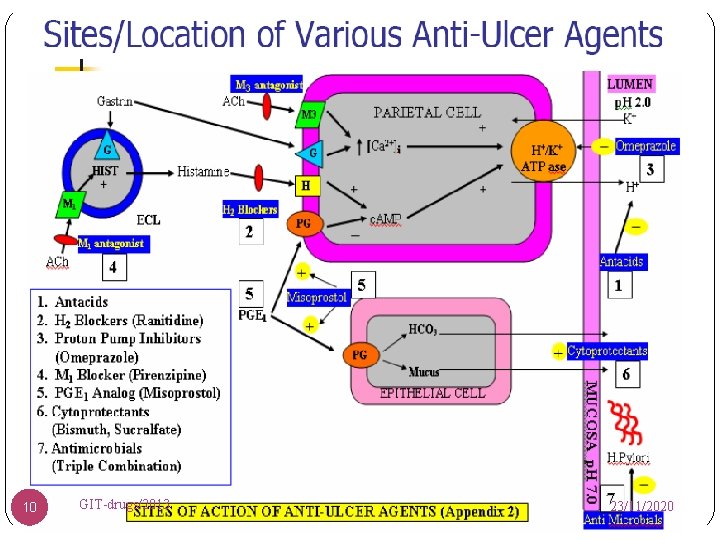
10 GIT-drugs/2013 23/11/2020

1. Proton Pump Inhibitors (PPI’s) 11 GIT-drugs/2013 23/11/2020

PPIs Most potent suppressors of acid secretion 2. Irreversible 24 -48 hr effects on acid suppression inhibitor of proton pump; blocks 98% of 1. acid secretion in all forms of ulcer and hypersecretory Zollinger-Ellison syndrome. The drug is given in gelatin coated capsule to resist breakdown in stomach acid. It reaches the intestine, well absorbed, enters blood stream, reaches the parietal cell. 12 GIT-drugs/2013 23/11/2020

PPIs Irreversibly inhibit H+/K+ATPase function to: Block gastric acid secretion Decrease pepsin concentration Increase gastric p. H Secretion of acid only resumes when new proton pumps are deployed Steady-state inhibition (affecting 70% of pumps) may take 2 -5 days 13 GIT-drugs/2013 23/11/2020

PPI Pharmacology Activated only when p. H decreases below 4 Occurs only in parietal cell Achieved only when parietal cell activation occurs (after meals) Most effective after a prolonged fast when large amounts of active proton pumps are present (i. e. breakfast) 14 GIT-drugs/2013 23/11/2020

Available PPIs Esomeprazole (Nexium) Lansoprazole (Laproton. Lapraz) Omeprazole (Protop, Pumpitor, OGB) Pantoprazole (Pantozol) (iv) Rabeprazole (Pariet) 15 GIT-drugs/2013 23/11/2020

PPI Metabolism Rapidly absorbed and Highly protein bound Extensively metabolized in the liver by the P 450 system (CYP 2 C 19 and CYP 3 A 4) Sulfated metabolites are excreted in the urine or feces Hepatic disease reduces the clearance of lansoprazole reduce dose 16 GIT-drugs/2013 23/11/2020
Common PPI Side Effects Headache (2. 9 -6. 9%) vs. Placebo (2. 5 - 6. 3%) Diarrhea (3%) vs. Placebo (3. 1%) Abdominal pain (2. 4 -5. 2%) vs. Placebo (3. 13. 3%) Constipation (1. 1 -1. 5%) vs. Placebo (0 -0. 8%) 17 GIT-drugs/2013 23/11/2020

Drug-Drug Interactions Ketoconazole and Digoxin absorption is decreased due to reduced acidity. Omeprazole may inhibit diazepam and phenytoin metabolism 18 GIT-drugs/2013 23/11/2020

2. Histamine H 2 -Receptor Antagonists (H 2 RAs) 19 GIT-drugs/2013 23/11/2020

H 2 RAs Reversibly compete with histamine for binding to H 2 receptors on the basolateral membrane of parietal cells Less potent than PPIs but still suppress acid by 70% over 24 hrs 20 GIT-drugs/2013 23/11/2020

Available H 2 RAs H 2 receptor blockers: Cimetidine (OGB, iv) First H 2 -blocker available Inhibits P 450 Drug interaction Ranitidine (OGB, iv) Does not inhibit P 450 fewer side effects Famotidine ((Famocid, Gaster: iv®) 21 GIT-drugs/2013 23/11/2020

Pharmacokinetics Rapidly absorbed after oral administration Serum concentrations peak in 1 -3 hr Therapeutic levels maintained up to 12 hrs Small percentage is protein bound 10% to 35 % metabolized by the liver Drugs and metabolites primarily excreted by kidneys (**reduce doses in renal disease) 22 GIT-drugs/2013 23/11/2020

1. inhibit 90% acid secretion in basal state as well as food-induced and nocturnal acid production. 2. they are helpful in healing gastric and duodenal ulcers and prevent their recurrence. Have benefits in preventing increased gastric acid secretion in Zollinger-Ellison syndrome. 3. Cimetidine Has several side effects, not a choice now - Under Prescription. 23 GIT-drugs/2013 23/11/2020

Common H 2 RA Side Effects All less than 3% Diarrhea Headache Drowsiness Fatigue Muscular pain Constipation Much less common Confusion, delirium in the elderly Associated with thrombocytopenia Cimetidine anti-androgen effects 24 GIT-drugs/2013 23/11/2020

Drug-Drug Interactions 1. Inhibits Cy. P 450: Inhibits the metabolism of various drugs that are concomitantly taken: phenytoin, warfarin, theophylinne, BZD. 2. These adverse effects are relatively least with ranitidine and famotidine 25 GIT-drugs/2013 23/11/2020

3. Prostaglandin Analogs: Misoprostol 26 GIT-drugs/2013 23/11/2020

Protective Effects of Prostaglandins PGE 2 and PGI 2 synthesized by gastric mucosa Acid-reducing effects Bind to EP 3 receptors on parietal cells Decrease acid production Cytoprotective effects Stimulation of mucin and bicarbonate Increase mucosal blood flow Contrast with NSAIDS which diminish prostaglandin formation by inhibition of cycloxygenase and lead to ulcer formation GIT-drugs/2013 27 23/11/2020

Misoprostol: Cytotec Synthetic analog of PGE 1 Enhanced potency Increased oral bioavailability Inhibit basal acid secretion (85 -95%) Inhibit stimulated acid secretion (75 - 85%) 28 GIT-drugs/2013 23/11/2020

Pharmacokinetics Rapidly absorbed Rapidly de-esterfied to misoprostol acid-- the active metabolite Therapeutic effect peaks at 60 -90 minutes Lasts 3 hours (qid dose required) 29 GIT-drugs/2013 23/11/2020

Side Effects Diarrhea ± abdominal cramps as high as 30% Begins within 2 weeks and often resolves spontaneously in 1 week Can exacerbate inflammatory bowel disease Contraindicated during pregnancy 30 GIT-drugs/2013 23/11/2020

4. Sucralfate: Carafate 31 GIT-drugs/2013 23/11/2020

Sucralfate Aluminium Sulfated polysaccharide, Acid activated Administered on an empty stomach 1 hr before meals Stimulates local prostaglandin synthesis, adsorbs pepsin AH 2 & antacids reduce bioavailability Not absorbed essentially free of side effects 32 GIT-drugs/2013 23/11/2020

Common Side Effects Constipation (2%) Aluminium hyphosphatemia: Avoid in renal failure May impair absorption of other drugs : tetrasiklin, warfarin, digoksin, fenitoin 2 hr interval 33 GIT-drugs/2013 23/11/2020

5. Antacids 34 GIT-drugs/2013 23/11/2020
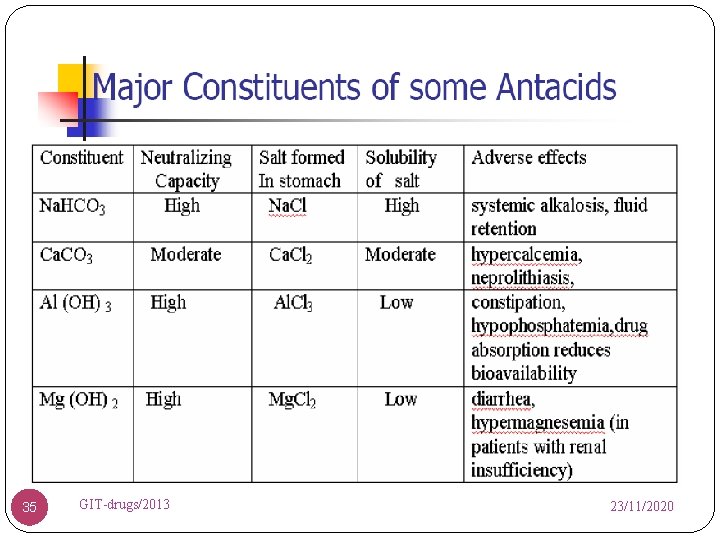
35 GIT-drugs/2013 23/11/2020

Antacids Sodium bicarbonate (Na. HCO 3) Ca. CO 3 Mg 2+ hydroxides Al 3+ hydroxide 36 GIT-drugs/2013 23/11/2020

Antacids Given orally 1 -3 hrs after meals and bedtime Mg+2 based preparations increase motility Diarrhea Al+3 based preparations relax smooth muscle Constipation Ca+2 based preparations release CO 2 Belching, nausea, distension, and flatulence. 37 GIT-drugs/2013 23/11/2020

Common Side Effects Aluminum toxicity with renal disease 38 Osteoporosis, enchephalopathy, osteomalacia Hypercalcemia Phosphate retention Calcium precipitation in the kidney Impair absorption of some drugs Take 2 hrs before or after other drugs : INH, GIT-drugs/2013 23/11/2020 tetrasiklin

Antibiotic ulcer therapy: Combinations must be used: 1. Bismuth (Scantoma, Stobiol®) – disrupts cell wall of H. pylori 2. Clarithromycin – inhibits protein synthesis 3. Amoxicillin – disrupts cell wall 4. Tetracyclin – inhibits protein synthesis 5. Metronidazole – used often due to bacterial resistance to amoxicillin and tetracyclin, or due to intolerance by the patient Standard treatment regimen for peptic ulcer: Omeprazole + amoxicillin + metronidazole 39 GIT-drugs/2013 23/11/2020

Laxatives 40 GIT-drugs/2013 23/11/2020

Constipation Abnormally infrequent and difficult passage of feces through the lower GI tract Symptom, not a disease Disorder of movement through the colon and/or rectum Can be caused by a variety of diseases (hemorrhoid, multipara) , drugs (opium, aluminium antacids) or psikis 41 GIT-drugs/2013 23/11/2020

Laxatives : Bulk forming Emollient Hyperosmotic Saline Stimulant 42 GIT-drugs/2013 23/11/2020

Laxatives: Mechanism of Action Bulk forming High fiber Absorbs water to increase bulk Distends bowel to initiate reflex bowel activity Examples: psyllium (Mulax) Methylcellulose, polycarbophil Agar-agar (>>hemiselulosa, tdk diabsorbsi & dicerna) 43 GIT-drugs/2013 23/11/2020

Laxatives: Mechanism of Action Emollient Stool softeners and lubricants Promote more water and fat in the stools Lubricate the fecal material and intestinal walls Examples: Stool softeners: docusate sodium Lubricants: mineral oil 44 GIT-drugs/2013 23/11/2020

Laxatives: Mechanism of Action Hyperosmotic Increase fecal water content Result: bowel distention, increased peristalsis, and evacuation Examples: polyethylene glycol sorbitol glycerin lactulose 45 GIT-drugs/2013 23/11/2020

Laxatives: Mechanism of Action Saline Increase osmotic pressure within the intestinal tract, causing more water to enter the intestines Result: bowel distention, increased peristalsis, and evacuation Saline laxative examples: magnesium sulfate (Epsom salts, garam Inggris) magnesium hydroxide magnesium citrate sodium phosphate 46 GIT-drugs/2013 23/11/2020

Laxatives: Mechanism of Action Stimulant Increases peristalsis via intestinal nerve stimulation Examples: castor oil senna cascara bisacodyl 47 GIT-drugs/2013 23/11/2020

Laxatives: Side Effects Bulk forming : Impaction, Fluid overload Emollient : Skin rashes, Decreased absorption of vitamins (ADEK parafin ) Hyperosmotic : Abdominal bloating, Rectal irritation Saline : Magnesium toxicity (with renal insufficiency), Cramping, Diarrhea, Increased thirst Stimulant : Nutrient malabsorption, Skin rashes, Gastric irritation, Rectal irritation 48 GIT-drugs/2013 23/11/2020

Antidiarrheals 49 GIT-drugs/2013 23/11/2020

Causes of Diarrhea Acute Diarrhea Bacterial Viral Drug induced Nutritional Protozoal 50 GIT-drugs/2013 Chronic Diarrhea Tumors Diabetes Addison’s disease Hyperthyroidism Irritable bowel syndrome 23/11/2020

Antidiarrheals Drugs that decrease peristalsis, thereby allowing fluid absorption from the intestinal contents Examples: Anticholinergics Protectants/adsorbents Opiate-related agents Probiotics Metronidazole 51 GIT-drugs/2013 23/11/2020

Anticholinergics are used to treat tenemus and vomiting Examples: Atropine Aminopentamide Isopropamide Propantheline Methscopolamine Side effects include dry mucous membranes, urine retention, tachycardia, and constipation 52 GIT-drugs/2013 23/11/2020

Protectants/adsorbents coat inflamed intestinal mucosa with a protective layer (protectants) or bind bacteria and/or digestive enzymes and/or toxins to protect intestinal mucosa from damaging effects (adsorbents) Examples: Bismuth subsalicylate (bismuth + aspirin-like product) Kaolin/pectin Activated charcoal Side effects include constipation 53 GIT-drugs/2013 23/11/2020

Opiate-related agents control diarrhea by decreasing both intestinal secretions and the flow of feces and increasing segmental contractions Examples: Diphenoxylate Loperamide Paregoric Side effects include CNS depression, ileus, urine retention, bloat, and constipation 54 GIT-drugs/2013 23/11/2020

Probiotics seed the GI tract with beneficial bacteria; use is based on theory that some forms of diarrhea are caused by disruption of the normal bacterial flora of the GI tract Must be refrigerated to maintain the viability of the bacteria Examples: Plain yogurt with active cultures Variety of trade-name products 55 GIT-drugs/2013 23/11/2020

A theory regarding the development of diarrhea is that anaerobic bacteria may increase due to disruption of normal GI flora One way to treat this is to use an antibiotic effective against anaerobic bacteria Metronidazole is an example of an antibiotic used to treat diarrhea 56 GIT-drugs/2013 23/11/2020

Cost-effectiveness studies of Zinc supplementation… zinc supplementation significantly improved the cost-effectiveness of standard management of diarrhoea for dysenteric as well as non-dysenteric illness. Sufficient evidence to recommend the inclusion of zinc into standard case management of both types of acute diarrhoea 57 GIT-drugs/2013 23/11/2020

The new WHO-UNICEF recommended policies for health professionals on the treatment of diarrhoea 1. Counsel mother to begin administering suitable home 2. 3. 4. 5. 58 6. fluids immediately upon onset of diarrhoea in a child Treat dehydration with new low osmolarity ORS solution (or with intravenous electrolyte solution in cases of severe dehydration) Emphasize continued feeding or increased breastfeeding during, and increases feeding after, the diarrhoeal episode Use antibiotics only when appropriate, i. e. , in the presence of bloody diarrhoea or shigellosis, and abstain from administering anti-diarrhoeal drugs Provide children with 20 mg per day of zinc supplementation for 10 -14 days (10 mg per day for infants under six months old) GIT-drugs/2013 23/11/2020 Advise mothers of the need to increase fluids and
Zinc and Low-osmolarity ORS: effective, safe and available 59 GIT-drugs/2013 23/11/2020

APA ITU TABURIA ? 60 GIT-drugs/2013 23/11/2020

pelengkap gizi makanan balita sehari-hari yang mengandung 12 macam vitamin dan 4 macam mineral yang dibutuhkan anak untuk tumbuh kembang secara optimal 61 GIT-drugs/2013 23/11/2020

62 GIT-drugs/2013 v. Taburia berbentuk serbuk v. Taburia mengandung: 1. Vitamin A 2. Vitamin B 1, B 2, B 6, B 12 3. Vitamin C 4. Vitamin D 3 5. Vitamin E 6. Asam Folat 7. Niasin 8. Selenium 9. Yodium 10. Besi 11. Seng 23/11/2020
KEPADA SIAPA TABURIA DIBERIKAN? Anak usia 6 bulan sampai 2 tahun 63 GIT-drugs/2013 23/11/2020

Petunjuk penggunaan taburia : 1. Sebelum memberikan taburia, sebaiknya cuci tangan terlebih dahulu dengan sabun 2. Tambahkan satu bungkus Taburia pada makanan padat anak siap santap (nasi, lauk pauk, bubur, ubi, jagung, kentang dll) 3. Pilih kapan / waktu balita makan paling banyak. Dianjurkan pada makan pagi 4. Taburia sebaiknya tidak dicampur dengan makanan yang terlalu berair, seperti minuman susu, teh, atau sayuran berkuah seperti sup, sayur bening dll karena mineral tidak larut sehingga dikhawatirkan tidak habis dikonsumsi. 5. Tidak boleh dicampur pada makanan yang panas (lapisan lemak akan pecah dan beberapa zat gizi GIT-drugs/2013 64 akan rusak) 23/11/2020

Yang perlu diketahui bila mengkonsumsi Taburia v. Selama mengonsumsi Taburia, ada kemungkinan tinja anak berwarna hitam. Hal ini bukan masalah karena warna hitam itu disebabkan oleh zat besi yang dikandung Taburia. v. Adakalanya terjadi susah buang air besar. Hal ini dapat diatasi dengan anak meminum air putih matang yang lebih banyak. v. Anak bisa mengalami diare/mencret-mencret, bila mengkonsumsi makanan yg tidak disiapkan dengan sanitasi yg baik 65 GIT-drugs/2013 23/11/2020

Terima kasih…. 66 GIT-drugs/2013 23/11/2020
- Slides: 63