Pharmacological management of STEMI post percutaneous coronary intervention




















- Slides: 24

Pharmacological management of STEMI post percutaneous coronary intervention Ann Mc. Andrew, Pharm. D Candidate 2019 University of Pittsburgh School of Pharmacy

Objectives Understand describe the acute and long-term management of ST-elevation myocardial infarction (STEMI) Identify pharmacologic treatment for patients after receiving percutaneous coronary intervention with stent placement Determine appropriateness of pharmacological treatment of patient with reference to the patient-specific data and guidelines

Patient Case CC: Chest Pain with radiation down both arms accompanied by diaphoresis HPI: DO is a 77 yo. M presenting to the ED with chest pain. Pt received electrocardiogram (EKG) which showed STEMI in leads II, III, and augmented Vector Foot (a. VL). Patient was loaded with aspirin, heparin, and Brilinta prior to cath lab. In the cath lab he received a drug-eluting stent to his distal right coronary artery (RCA).

Patient Information PMH: • Factor V Leiden with deep vein thrombosis (DVT) 20 years ago • Hypothyroidism • L hip replacement • R knee replacement • GERD s/p Nissen fundoplication Vitals (3/24) HR (bpm) 64 RR (bpm) 18 Sp. O 2 (RA) % 98 Temp (C) 36. 5 BP (mm. Hg) 173/103 Height (cm) 170 Weight (kg) 80 Home Medications Warfarin 5 mg PO daily alternating with 7. 5 mg every 3 days Celecoxib 200 mg PO daily T 4 225 mcg & T 3 15 mcg PO every morning

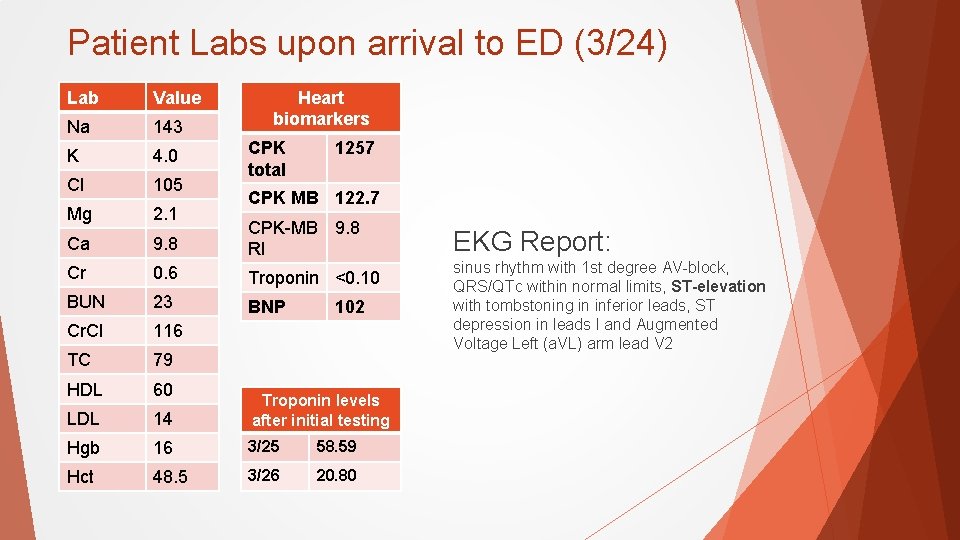
Patient Labs upon arrival to ED (3/24) Lab Value Na 143 K 4. 0 Cl 105 Mg 2. 1 Ca 9. 8 CPK-MB 9. 8 RI Cr 0. 6 Troponin <0. 10 BUN 23 BNP Cr. Cl 116 TC 79 HDL 60 LDL 14 Troponin levels after initial testing Hgb 16 3/25 58. 59 Hct 48. 5 3/26 20. 80 Heart biomarkers CPK total 1257 CPK MB 122. 7 102 EKG Report: sinus rhythm with 1 st degree AV-block, QRS/QTc within normal limits, ST-elevation with tombstoning in inferior leads, ST depression in leads I and Augmented Voltage Left (a. VL) arm lead V 2

Question to think about: Which medications should we start the patient on prior to discharge? (may be more than one answer) A. Carvedilol B. Atorvastatin C. Clopidogrel D. Ticagrelor E. Aspirin F. Lisinopril

ST-Elevation Myocardial Infarction (STEMI)

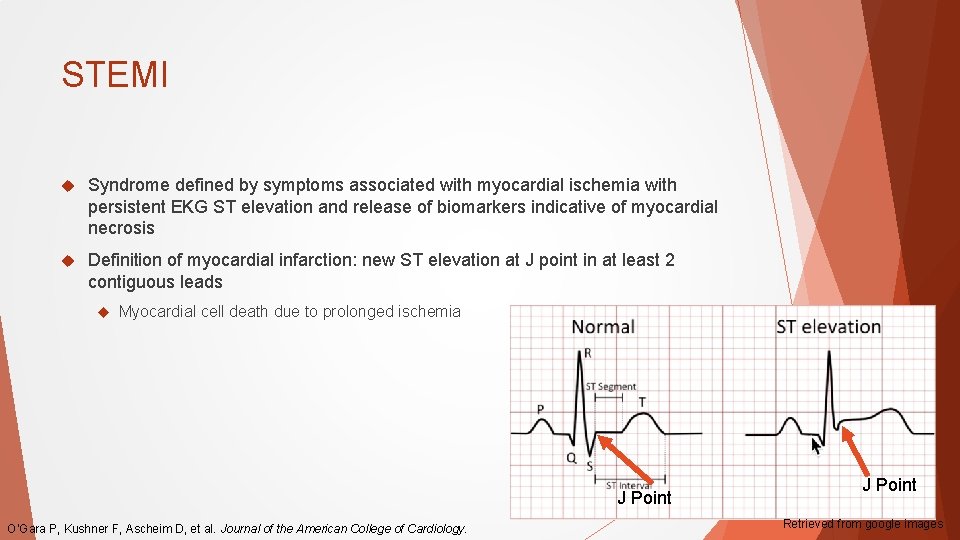
STEMI Syndrome defined by symptoms associated with myocardial ischemia with persistent EKG ST elevation and release of biomarkers indicative of myocardial necrosis Definition of myocardial infarction: new ST elevation at J point in at least 2 contiguous leads Myocardial cell death due to prolonged ischemia J Point O’Gara P, Kushner F, Ascheim D, et al. Journal of the American College of Cardiology. J Point Retrieved from google images

Clinical symptoms and diagnostic labs of MI Clinical symptoms Chest, upper extremity, mandibular, epigastric discomfort, dyspnea, and/or fatigue Persists >20 minutes Diffuse Accompanied by diaphoresis, nausea, or syncope Sometimes asymptomatic Diagnostic biomarkers Cardiac troponin or creatine kinase-myocardial band (CK-MB) Cardiac troponin I and T (expressed almost exclusively in the heart) O’Gara P, Kushner F, Ascheim D, et al. Journal of the American College of Cardiology. Thygesen K, Alpert J, Jaffe A, et al. Circulation.

STEMI vs NSTEMI vs Unstable Angina (UA) STEMI- ischemic symptoms (chest pain, dyspnea, diaphoresis) with elevated troponins AND ST-segment elevation NSTEMI- ischemic symptoms with elevated troponins with or without EKG changes (ST depression +/- T wave inversion) UA- ischemic symptoms without elevated troponins, without specific EKG changes Hedayati T, Yadav N, Khanagavi J. Cardiology Clinics.

Immediate Treatment of STEMI Reperfusion via percutaneous coronary intervention (PCI) Preferred to fibrinolytic therapy PCI has highest benefit within 12 hours of ischemic symptoms Fibrinolytic Indicated when >120 minute delay to PCI Adjunct aspirin, clopidogrel, and unfractionated heparin Stent placement in Primary PCI Bare-metal stent vs drug-eluting stent O’Gara P, Kushner F, Ascheim D, et al. Journal of the American College of Cardiology.

Medications prior to PCI in a PCI-capable hospital Aspirin load (162325 mg) P 2 Y 12 Load Clopidogrel 600 mg OR Prasugrel 60 mg OR Ticagrelor 180 mg O’Gara P, Kushner F, Ascheim D, et al. Journal of the American College of Cardiology. GP IIb/IIIa receptor antagonist: Eptifibatide 180 mcg/kg bolus Unfractionated Heparin IV bolus 50 -70 units/kg

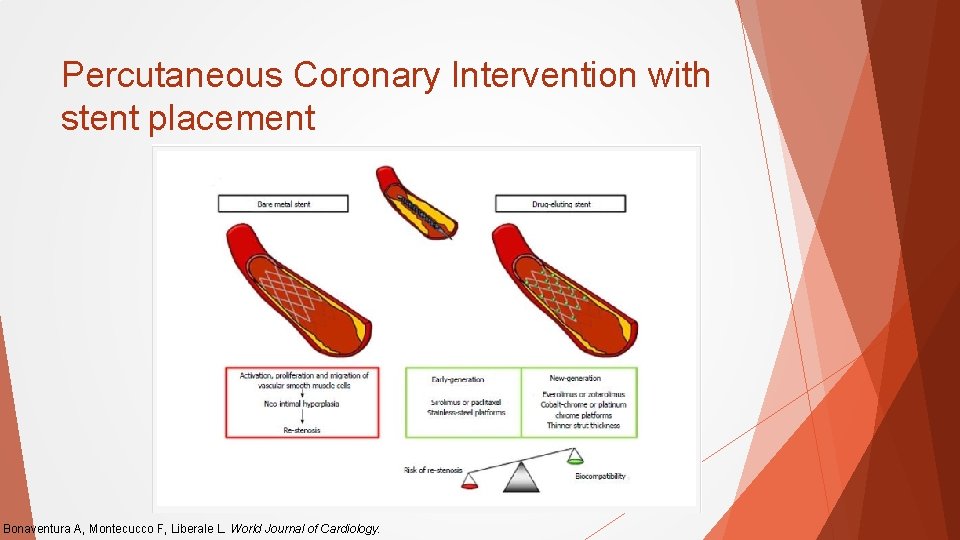
Percutaneous Coronary Intervention with stent placement Bonaventura A, Montecucco F, Liberale L. World Journal of Cardiology.

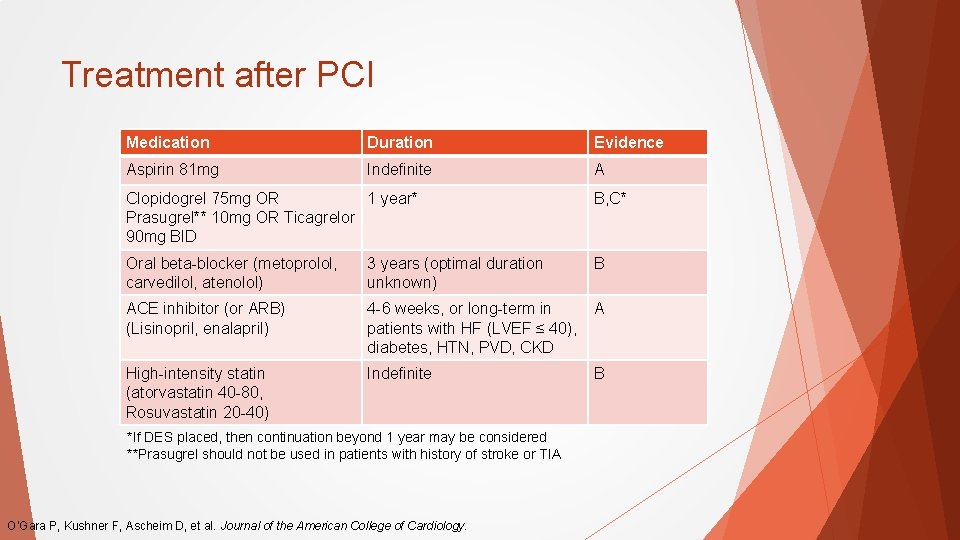
Treatment after PCI Medication Duration Evidence Aspirin 81 mg Indefinite A Clopidogrel 75 mg OR 1 year* Prasugrel** 10 mg OR Ticagrelor 90 mg BID B, C* Oral beta-blocker (metoprolol, carvedilol, atenolol) 3 years (optimal duration unknown) B ACE inhibitor (or ARB) (Lisinopril, enalapril) 4 -6 weeks, or long-term in patients with HF (LVEF ≤ 40), diabetes, HTN, PVD, CKD A High-intensity statin (atorvastatin 40 -80, Rosuvastatin 20 -40) Indefinite B *If DES placed, then continuation beyond 1 year may be considered **Prasugrel should not be used in patients with history of stroke or TIA O’Gara P, Kushner F, Ascheim D, et al. Journal of the American College of Cardiology.

Choosing a P 2 Y 12 Receptor Inhibitor TRITON-TIMI 38 PLATO Treatment arms -Prasugrel 60 mg LD, 10 mg daily -Clopidogrel 300 mg LD, 75 mg daily -Ticagrelor 180 mg LD, 90 mg twice daily -Clopidogrel 300 -600 mg LD, 75 mg daily Population 13, 608 patients with ACS scheduled for PCI 18, 624 patients with ACS, with or without ST -segment elevation Primary outcome Death from cardiovascular causes, nonfatal At 12 months- composite of death from MI, nonfatal stroke vascular causes, MI, stroke Results for primary outcome -Clopidogrel: 12. 1% -Prasugrel: 9. 9% (HR, 0. 81; 95% CI 0. 73 to 0. 90; P<0. 001) -Clopidogrel: 11. 7% -Ticagrelor: 9. 8% (HR, 0. 84; 95% CI 0. 77 to 0. 92; P<0. 001) Bleeding risk Prasugrel increases risk No significant difference Conclusion Prasugrel significantly increased risk of bleed Ticagrelor significantly reduces primary outcome without increased risk of bleed Wiviott S, Braunwald E, Mc. Cabe C, et al. The New England Journal of Medicine. Wallentin L, Becker R, Budaj A, et al. The New England Journal of Medicine

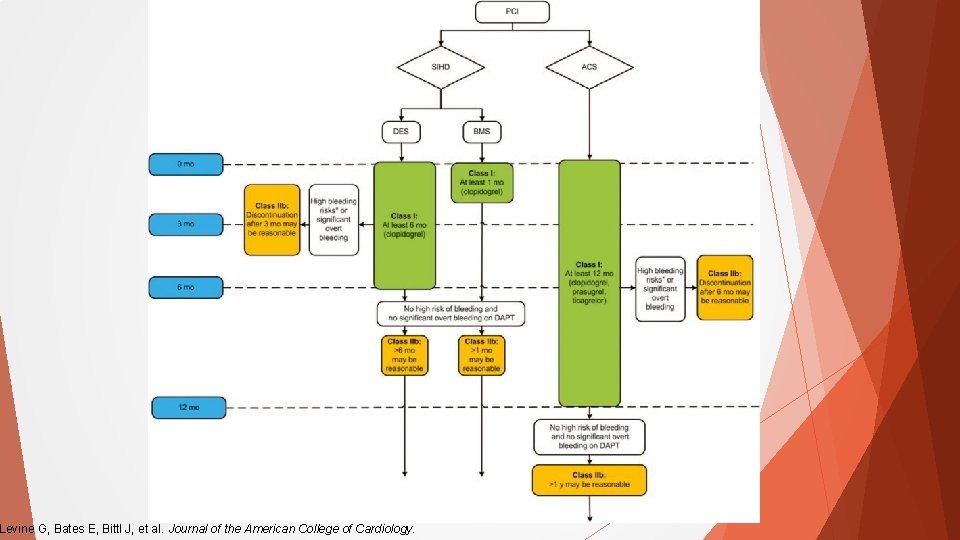
Levine G, Bates E, Bittl J, et al. Journal of the American College of Cardiology.

Back to Patient Case

Patient Case HPI: DO is a 77 yo. M presented to the ED with chest pain and diagnosed with STEMI, now s/p percutaneous coronary intervention with DES x 1 of distal RCA Prior to PCI Received aspirin 324 mg, heparin 5, 600 units, Brilinta 180 mg, and eptifibatide 12. 8 m. L/hr x 14 hrs Vitals (3/26) HR (bpm) 76 RR (bpm) 18 Sp. O 2 (RA) (%) 97 Temp (C) 36. 6 LVEF 55 -60% BP (mm. Hg) 121/72 LDL 14 mg/d. L Height (cm) 170 Hemoglobin 13. 5, hematocrit 38. 0 Weight (kg) 80

Question: Which medications would you start the patient on? (there may be more than one answer) A. Carvedilol B. Atorvastatin C. Clopidogrel D. Ticagrelor E. Aspirin F. Lisinopril

Question: Which medications would you start the patient on? (there may be more than one answer) A. Carvedilol B. Atorvastatin C. Clopidogrel D. Ticagrelor E. Aspirin F. Lisinopril

What about his statin? Patient will be on statin for one month Multiple studies have indicated that patients with LDL below 70 mg/d. L still benefit from other mechanisms of HMG-Co. A reductase inhibitors Patient counseled on anti-inflammatory benefits: - Reduce circulating C-reactive protein (CRP) - Pro-inflammatory cytokines - In vessels, statins rapidly induce favorable effects on vascular redox state and reduce vascular reactive oxygen species Antonopoulos A, Margaritis M, Lee R, et al. Current Pharmaceutical Design.

Patient’s Discharge Medications New Medications Atorvastatin 40 mg daily x 1 month Carvedilol 12. 5 mg BID Brilinta (ticagrelor) 90 mg BID Aspirin 81 mg daily Continuing Warfarin 5 mg daily alternating with 7. 5 mg every 3 days (bridging with enoxaparin 40 mg sub. Q daily) T 4 225 mcg & T 3 15 mcg PO every morning

References O’Gara P, Kushner F, Ascheim D, et al. 2013 ACCF/AHA Guideline for the management of ST-elevation myocardial infarction. Journal of the American College of Cardiology. 2013; 61(4): e 79 -118. Hedayati T, Yadav N, Khanagavi J. Non-ST-Segment acute coronary syndromes. Cardiology Clinics. 2018; 36(1): 37 -52. Thygesen K, Alpert J, Jaffe A, et al. Third university definition of myocardial infarction. Circulation. 2012; 126: 20202035. Bonaventura A, Montecucco F, Liberale L. Coronary stenting: a matter of revascularization. World Journal of Cardiology. 2017; 9(3): 207 -211. Wiviott S, Braunwald E, Mc. Cabe C, et al. Prasugrel versus clopidogrel in patients with acute coronary syndrome. The New England Journal of Medicine. 2007; 357: 2001 -2015. Wallentin L, Becker R, Budaj A, et al. Ticagrelor versus clopidogrel in patients with acute coronary syndromes. The New England Journal of Medicine. 2009; 361: 1045 -1057. Levine G, Bates E, Bittl J, et al. 2016 ACC/AHA Guideline focused update on duration of dual antiplatelet therapy in patients with coronary artery disease. Journal of the American College of Cardiology. 2016; 68(10): 1094. Antonopoulos A, Margaritis M, Lee R, et al. Statins as anti-inflammatory agents in atherogenesis: molecular mechanisms and lessons from the recent clinical trials. Current Pharmaceutical Design. 2012; 18(11): 1519 -1530.

Questions? Ann Mc. Andrew Amm 316@pitt. edu