Pharmacologic Management of Rapid Sequence Intubation RSI James

Pharmacologic Management of Rapid Sequence Intubation (RSI) James Gibson, Pharm. D PGY 1 Pharmacy Practice Resident

Learning Objectives List the six P’s of RSI. Discuss historical rationale for “LOADing” patients undergoing RSI. Understand the rationale for use of one induction agent over another. Identify the contraindications to succinylcholine administration and how to manage patients who are not candidates.

Rapid Sequence Intubation (RSI) Induction of a patient using simultaneous Sedatives Rapid-acting paralytic agent Goal: to avoid assisted ventilation due to elevated risk of aspiration Un-fasted patient Pharyngeal/laryngeal manipulation

The Six P’s of RSI Preparation Pre-oxygenation Pretreatment and induction Paralysis Placement of the tube Post-intubation management

Preparation Assess patient—difficult airway? IV access Monitor (tele, pulse ox) Gather: Equipment for intubation Post-intubation medication(s) Pertinent patient history Supplies for surgical airway (just in case!!)

Pre-Oxygenation Goals: Establish O 2 reservoir Maximize time for intubation Prevent need for bag-mask ventilation Methods: 3 -5 minutes of 100% O 2 via face mask 4 (or 8) vital capacity breaths on 100% O 2
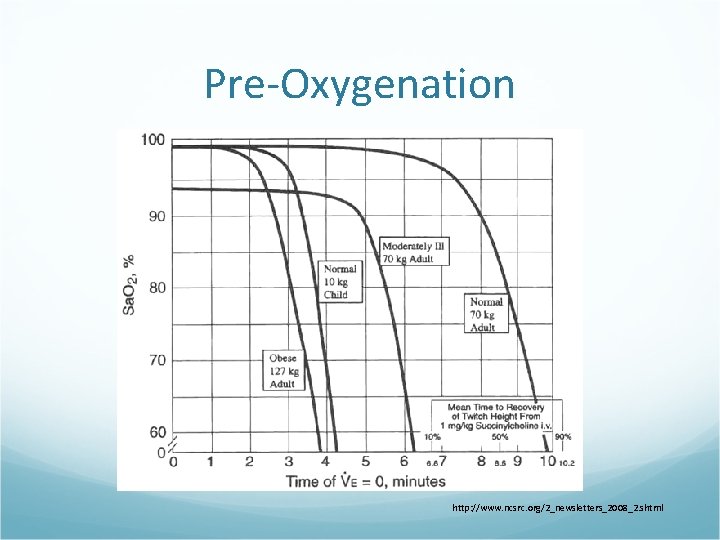
Pre-Oxygenation http: //www. ncsrc. org/2_newsletters_2008_2. shtml

Pretreatment • Goal: – Mitigate adverse physiologic reactions to intubation • Sympathetic “pressor response” • Bronchospasm • Increased intracranial pressure (ICP) • Muscle fasciculation – Begins 2 -3 minutes PRIOR to induction/paralysis • “LOAD” • Not routinely done in practice

Pretreatment Lidocaine Dose: 1. 5 mg/kg IV Opioid To prevent rise in ICP by Atropine Defasciculating agent Preventing cough Blunting pressor response May reduce reactive bronchospasm in asthma

Pretreatment Lidocaine Fentanyl 3 mcg/kg IV Opioid Provides analgesia Atropine Lessens pressor response Defasciculating agent Limits ICP increase More effective than lidocaine

Pretreatment Lidocaine Dose: 0. 02 mg/kg Opioid To prevent bradycardia caused Atropine Defasciculating agent by airway manipulation and succinylcholine Historically used in pediatrics May be more beneficial with repeated doses of succinylcholine (i. e. OR setting)

Pretreatment Lidocaine Fasciculations occur in >90% of Atropine patients given succinylcholine Muscle pain Increase intragastric pressure Defasciculating agent Increase ICP (? ) Opioid emesis Prevention Higher doses of succs (1. 5 mg/kg vs 1 mg/kg) Non-depolarizing NMB (1/10 th of paralytic dose)

Induction Agent(s) Given as rapid IV push immediately before paralyzing agent Ideally provides: Rapid loss of consciousness Analgesia Amnesia Stable hemodynamics

Induction Agents Drug Dose Thiopental 3 -5 mg/kg IV Methohexital 1 -3 mg/kg IV Fentanyl 5 -15 mcg/kg IV Midazolam 0. 1 mg/kg IV Ketamine 1 -2 mg/kg IV Etomidate 0. 3 mg/kg IV Propofol 2 mg/kg IV

Induction Agents Etomidate Ultrashort-acting non-barbiturate hypnotic Rapid onset— 30 to 60 secs Hemodynamic stability Hydrolyzed in liver and plasma ICP with minimal effects on cerebral perfusion NO analgesia ADE: Myoclonic jerks, cortisol production

Induction Agents Fentanyl Short-acting, potent Minimal histamine release Hemodynamically stable Sedation is rate- AND dose-dependent Combined with other induction agents for analgesia ADE: muscle rigidity, grand mal seizures (rare)

Induction Agents Midazolam Sedative, amnestic, muscle relaxant NOT analgesic Less cardiorespiratory depression vs. other benzos BP; HR Use lower dose in hypovolemic, elderly, or traumatic brain injury patients (0. 05 mg/kg) Does NOT contain propylene glycol

Induction Agents Ketamine NMDA-antagonist dissociative anesthesia Analgesic, amnestic, anesthetic Dissociation occurs at threshold of 1 -1. 5 mg/kg IV 4 -5 mg/kg IM (more emesis) Catecholamine reuptake inhibition ( HR, BP, CO, ICP) Maintains respiration and airway reflexes ADE: Emergence delirium (30%)—Premed: midazolam 0. 07 mg/kg Emesis (highest in adolescents ~9 yo) CI: schizophrenia (schizoaffective); <3 months (relative): Asthma exacerbation; CVD Annals of Emergency Medicine. 57. 5 (2011): 449 -461
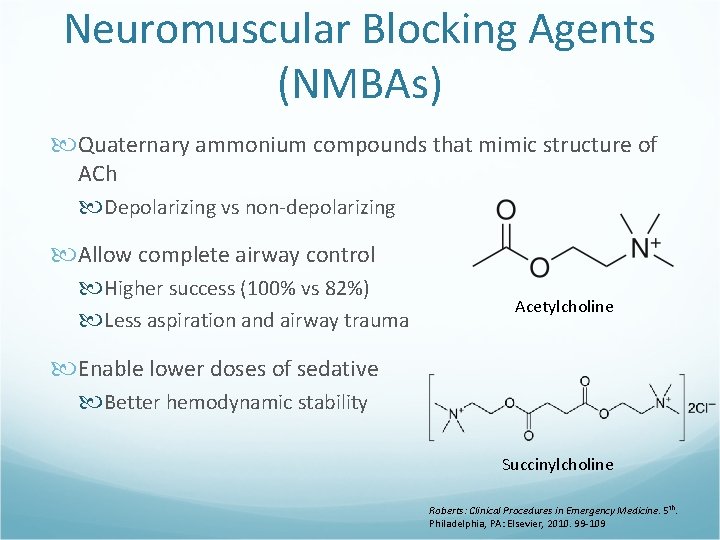
Neuromuscular Blocking Agents (NMBAs) Quaternary ammonium compounds that mimic structure of ACh Depolarizing vs non-depolarizing Allow complete airway control Higher success (100% vs 82%) Less aspiration and airway trauma Acetylcholine Enable lower doses of sedative Better hemodynamic stability Succinylcholine Roberts: Clinical Procedures in Emergency Medicine. 5 th. Philadelphia, PA: Elsevier, 2010. 99 -109

Succinylcholine Depolarizing NMBA Non-competitively binds ACh receptors initial membrane depolarization Longer degradation time than ACh Paralysis in ~60 sec. DOA: 3 -5 min Prolonged in pseudocholinesterase deficiency (genetic, hepatic/renal failure, pregnancy, cocaine) Repeat doses prolong paralysis May increase bradycardia/hypotension DOC for RSI

Succinylcholine Dose: 1. 5 mg/kg IV (infants: 2 mg/kg IV) Use ACTUAL body weight Rapid bolus; follow w/ 20 -30 m. L saline flush ADEs: Muscle fasciculation myalgias Hyperkalemia, CPK Bradycardia/hypotension Mild increase in ICP Malignant hyperthermia

Succinylcholine Hyperkalemia Typical K+ increase < 0. 5 m. Eq/L Up to a 5 m. Eq/L K+ increase in certain settings: Contraindicated in: Conditions with up-regulation of ACh-receptors (see table) Known/suspected hyperkalemia Personal/family hx of malignant hyperthermia
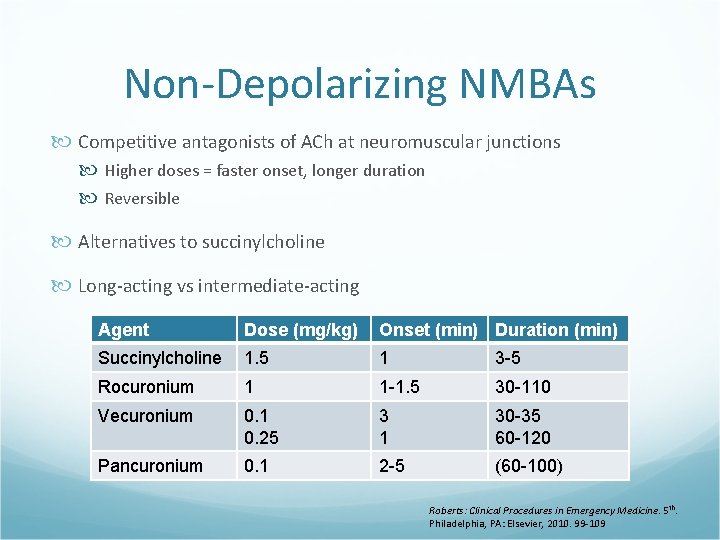
Non-Depolarizing NMBAs Competitive antagonists of ACh at neuromuscular junctions Higher doses = faster onset, longer duration Reversible Alternatives to succinylcholine Long-acting vs intermediate-acting Agent Dose (mg/kg) Onset (min) Duration (min) Succinylcholine 1. 5 1 3 -5 Rocuronium 1 1 -1. 5 30 -110 Vecuronium 0. 1 0. 25 3 1 30 -35 60 -120 Pancuronium 0. 1 2 -5 (60 -100) Roberts: Clinical Procedures in Emergency Medicine. 5 th. Philadelphia, PA: Elsevier, 2010. 99 -109

Non-Depolarizing NMBAs Pancuronium Long time to onset HR and BP (vagolytic effect) Histamine release bronchospasm/anaphylaxis Active metabolites Accumulates Renal dosing required NOT recommended for RSI

Non-Depolarizing NMBAs Vecuronium Slower onset than rocuronium Non-vagolytic; no histamine release Active metabolites Often requires “priming” dose 0. 01 mg/kg during pre-oxygenation phase, then 1. 5 mg/kg given 3 min later for paralysis

Non-Depolarizing NMBAs Rocuronium Onset similar to succinylcholine Non-vagolytic; no histamine release No active metabolites Preferred alternative to succinylcholine in RSI

Post-intubation Care After endotracheal tube is placed: Provide continued sedation/analgesia Propofol drip (No analgesia) ≤ 120 kg begin infusion at 20 mcg/kg/min 121 -150 kg begin infusion at 15 mcg/kg/min >151 kg begin infusion at 10 mcg/kg/min Bolus fentanyl and midazolam Fentanyl (analgesia): LD: 25 -100 mcg IV q 15 min PRN (max 300 mcg in first hr) MD: 25 -100 mcg IV q 30 min PRN (max 200 mcg/hr) Midazolam (sedation): LD: 1 -4 mg IV q 15 min PRN (max 16 mg in first hr) MD: 1 -4 mg IV q 1 hr PRN UWMC Form U 2914

References Claudius, C, LH Garvey, J Viby-Mogensen, et al. "The Undesirable Effects of Neuromuscular Blocking Drugs. " Anaesthesia. 64. 1 (2009): 10 -21. Print. Fleming, Bethany, Maureen Mc. Collough, et al. "Myth: Atropine should be administered before succinylcholine for neonatal and pediatric intubation. . " Can J Emerg Med. 7. 2 (2005): 114 -117. Print. Green, Steven, Mark Roback, et al. "Clinical Practice Guidelines for Emergency Department Ketamine Dissociative Sedation: 2011 Update. " Annals of Emergency Medicine. 57. 5 (2011): 449 -461. Print. Hopson, Laura, and Richard Schwartz. Roberts: Clinical Procedures in Emergency Medicine. 5 th. Philadelphia, PA: Elsevier, 2010. 99 -109. Print. Martyn, Jeevendra, and Martina Richtsfeld. "Succinylcholine-induced Hyperkalemia in Acquired Pathologic States. " Anesthesiology. 104. (2006): 158 -69. Web. 8 Mar. 2012. Walls, Ron. Marx: Rosen's Emergency Medicine. 7 th ed. Philadelphia, PA: Elsevier, 2010. 3 -22. Print.
- Slides: 28