Pharmacologic Debridement More Does Not Equal Better Jacob

Pharmacologic Debridement: More Does Not Equal Better Jacob B. Blumenthal, MD, FACP Baltimore Geriatrics Research, Education and Clinical Center/VAMC University of Maryland School of Medicine Baltimore, MD jblument@grecc. umaryland. edu Nicole J. Brandt, Pharm. D, CGP, BCPP, FASCP Peter Lamy Center on Drug Therapy and Aging University of Maryland, School of Pharmacy Baltimore, MD nbrandt@rx. umaryland. edu

…but… • Unlike Dick the Butcher – ”The first thing we do, let's kill all the lawyers” • Not: medications are bad – Rather, suggesting need for judicious use and continuous re-litigation Henry VI William Shakespeare

Outline • Demographics – Aging and Multimorbidities – Polypharmacy and ADR’s • Age-related changes – Pharmacodynamics (absorption, clearance) – Body Composition • What are we doing? Whose standard? • Bad Drugs: Beer’s List, HEDIS High Risk Meds • Semper Vigilentes – Med Review as a SOP
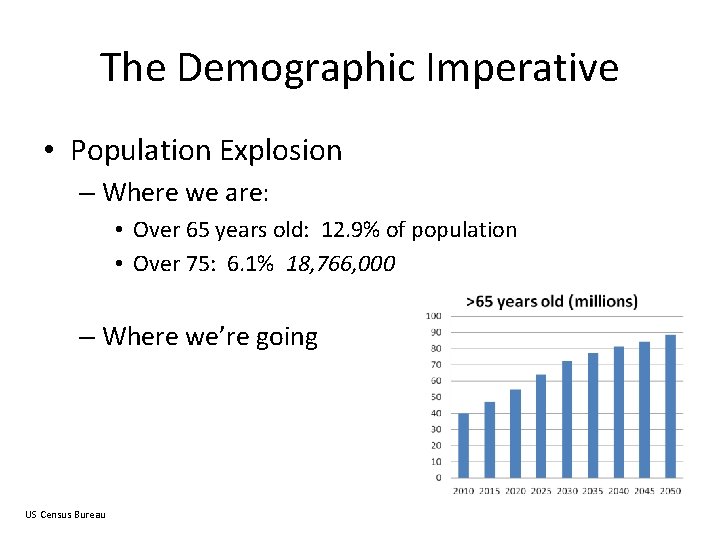
The Demographic Imperative • Population Explosion – Where we are: • Over 65 years old: 12. 9% of population • Over 75: 6. 1% 18, 766, 000 – Where we’re going US Census Bureau
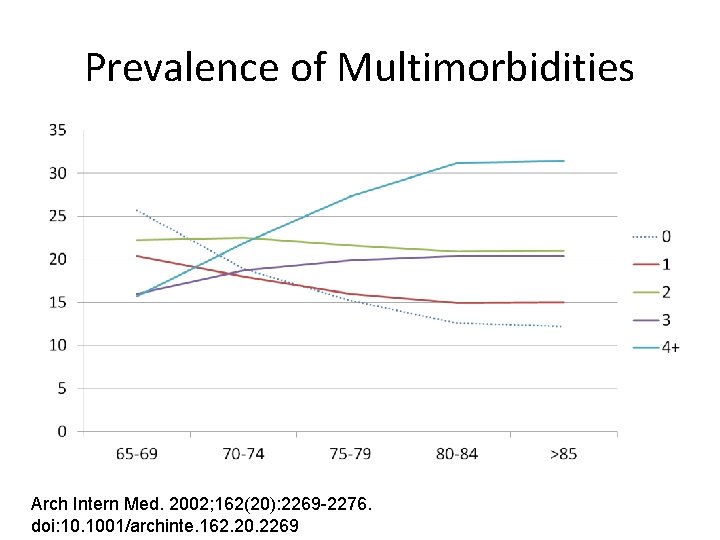
Prevalence of Multimorbidities Arch Intern Med. 2002; 162(20): 2269 -2276. doi: 10. 1001/archinte. 162. 20. 2269
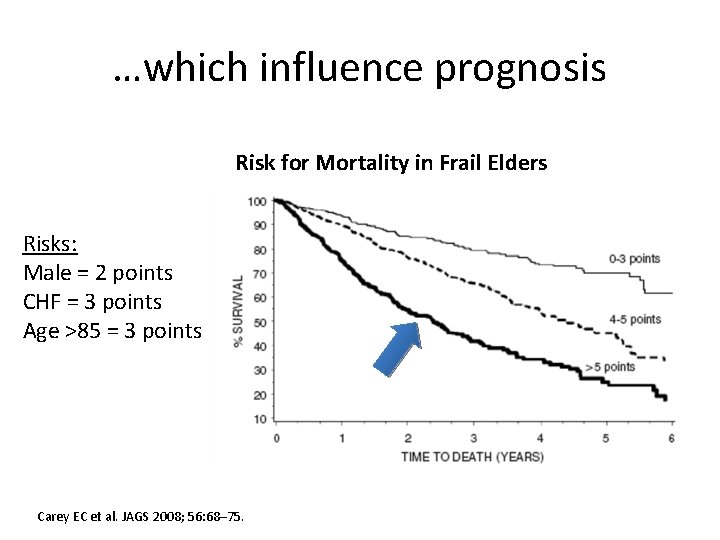
…which influence prognosis Risk for Mortality in Frail Elders Risks: Male = 2 points CHF = 3 points Age >85 = 3 points Carey EC et al. JAGS 2008; 56: 68– 75.
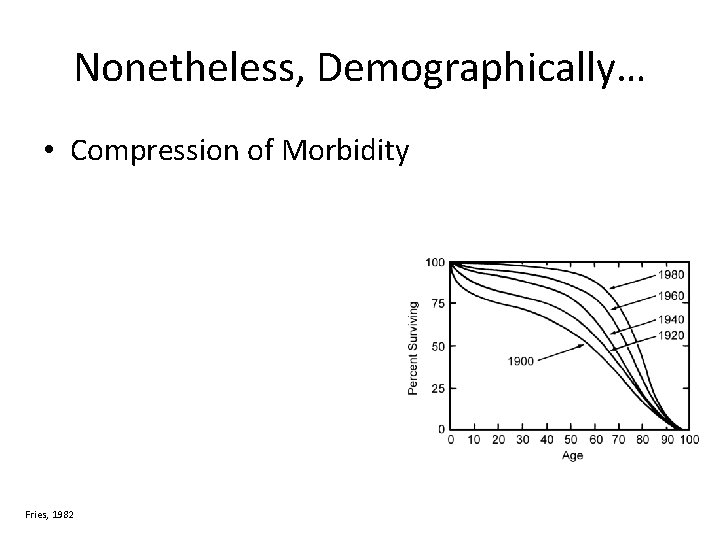
Nonetheless, Demographically… • Compression of Morbidity Fries, 1982

The Search for Clinical Decision Making Tools • Large heterogeneity difficult to find applicable studies – “No index…prospectively tested and found to be accurate in a large diverse sample…no study was completely free from potential sources of bias. Testing of transportability was limited, raising concerns about overfitting and underfitting. These factors limit a clinician's ability to assess the accuracy of these indices across patient groups that differ according to severity of illness, methodology of data collection, geographic location, and time. ” • The Controversy – How far can we extrapolate data for this population? – To what extent can we base clinical practice on biologic plausibility in the absence of clinical trail data?

Importance of Multimorbidity • Over 50% of older adults have 3+ chronic conditions • Increased risk of: – Death – Institutionalization – Increased utilization of healthcare resources – Decreased quality of life – Higher rates of adverse effects of treatment or interventions Brendan Smialowski (NY Times) • Almost all existing “guidelines” have single disease focus • Best approaches to decision-making and clinical management of older adults with multimorbidity remain unclear
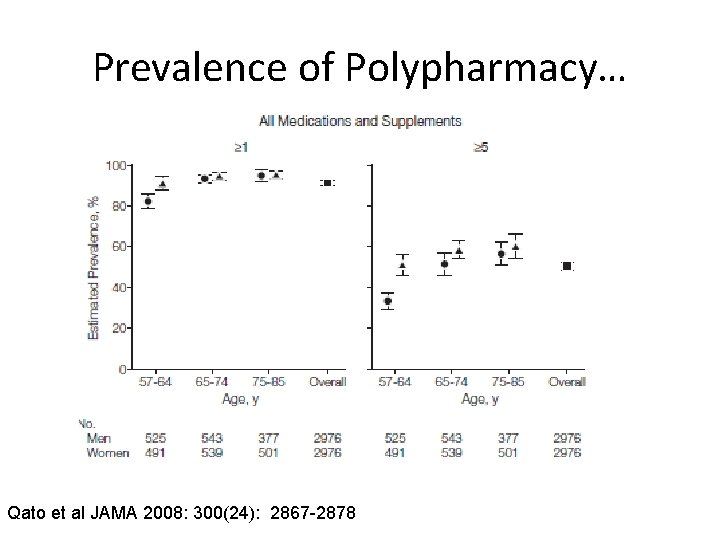
Prevalence of Polypharmacy… Qato et al JAMA 2008: 300(24): 2867 -2878

Treatment Complexity & Feasibility • Difficult to define a uniform threshold for treatment complexity and feasibility • Influenced by – Treatment regimen – Older adult’s unique characteristics • Barriers to assessing complexity and feasibility – Time-consuming – Lack of necessary training

Drugs are not benign • ~100, 000 emergency hospitalizations/year due to adverse drug events (ADEs) • 10. 7% of hospital admissions in older adults • “If medication related problems were ranked as a disease, it would be the fifth leading cause of death in the US!” Kongkaew C, et al. Annals of Pharmacotherapy 2008; 42: 1017 -1025 Budnitz et al. N Engl J Med 2011; 365: 2000 -12. Beers MH. Arch Internal Med. 2003

Pharmacokinetics Change with Age • Absorption – Other drugs, nutrition, gastric emptying • Distribution – ↑adipose/↓lean, water • Binding/Localization – ↓albumin • Biotransformation – ↓Hepatic Clearance (some drugs), great variability • Elimination – ↓GFR …and diminished homeostatic reserve
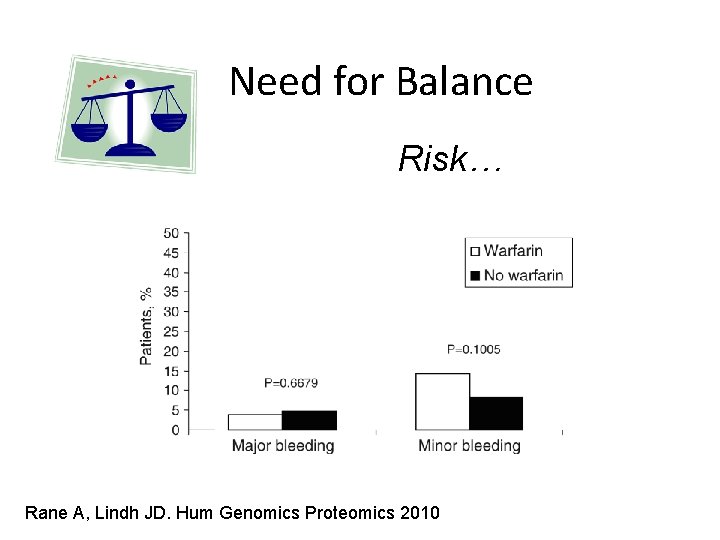
Need for Balance Risk… Rane A, Lindh JD. Hum Genomics Proteomics 2010
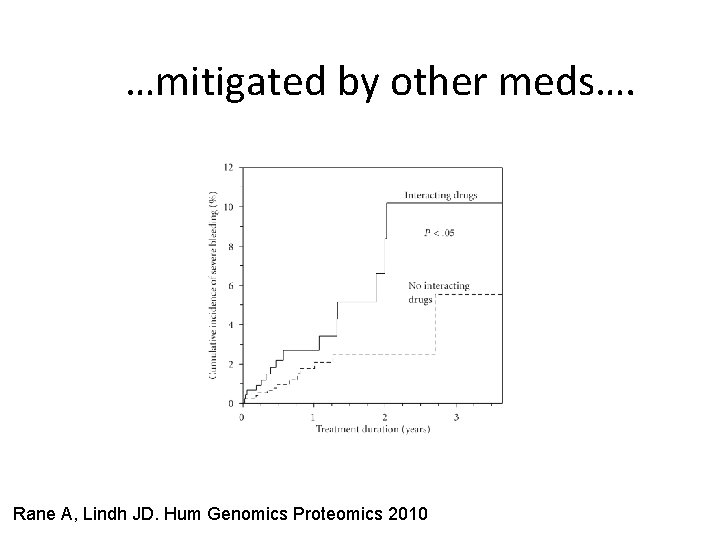
…mitigated by other meds…. Rane A, Lindh JD. Hum Genomics Proteomics 2010
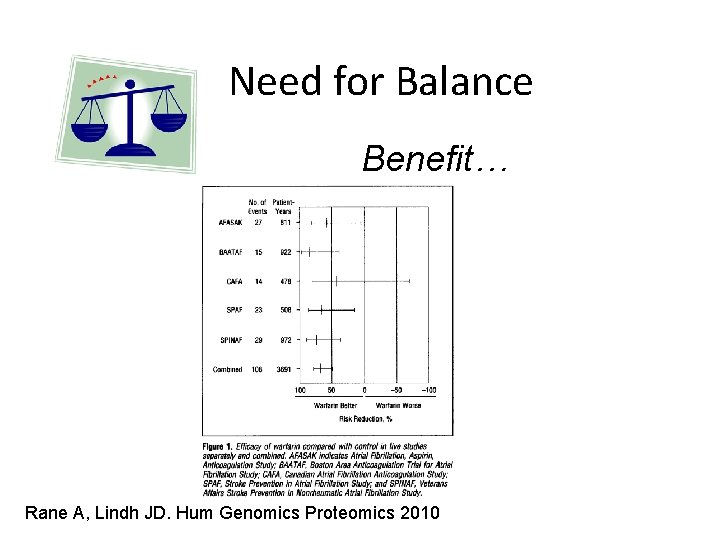
Need for Balance Benefit… Rane A, Lindh JD. Hum Genomics Proteomics 2010
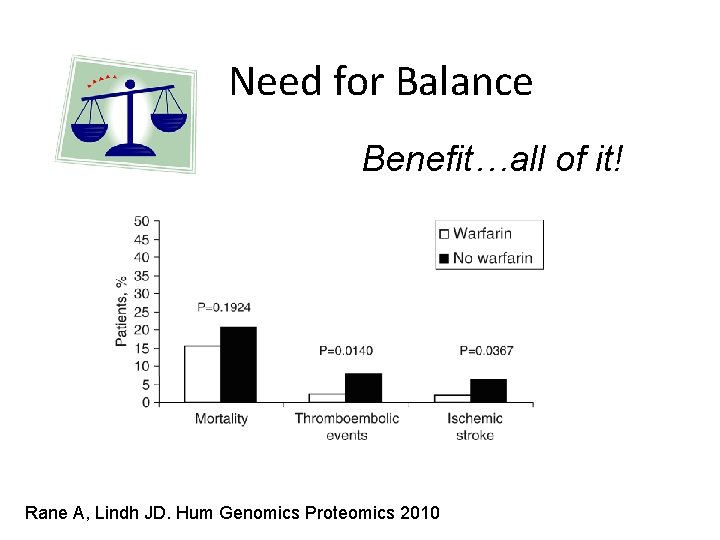
Need for Balance Benefit…all of it! Rane A, Lindh JD. Hum Genomics Proteomics 2010
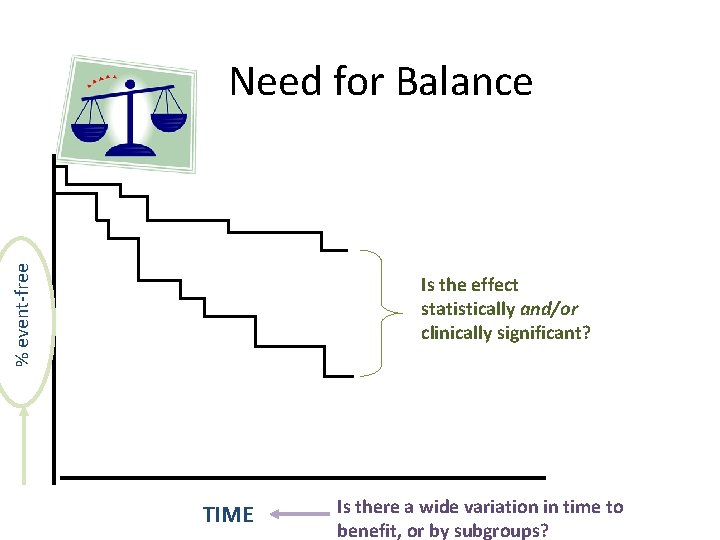
% event-free Need for Balance Is the effect statistically and/or clinically significant? TIME Is there a wide variation in time to benefit, or by subgroups?

Diabetes Mellitus • Less stringent control reasonable in those with a long history of diabetes, limited life expectancy, or comorbid conditions ADA Standards of Medical Care in Diabetes 2012. Sjoblom P. Diabetes Res Clin Prac 2008; 82: 197 -202. Drug withdrawal study in 17 nursing homes in patients with Hb. A 1 c <6: safe to discontinue all oral meds, and stop or reduce insulin

Top Five Problematic Medication Classes leading to ED 1. 2. 3. 4. 5. 15. 0% Hematologic 67% Endocrine agents 18. 7% Cardiovascular agents 19. 0% Central Nervous System Agents Anti-infective Oral Hypoglycemic Oral Antiplatelet 46. 8% Warfarin Insulin Budnitz et al. N Engl J Med 2011; 365: 2000 -12. 2
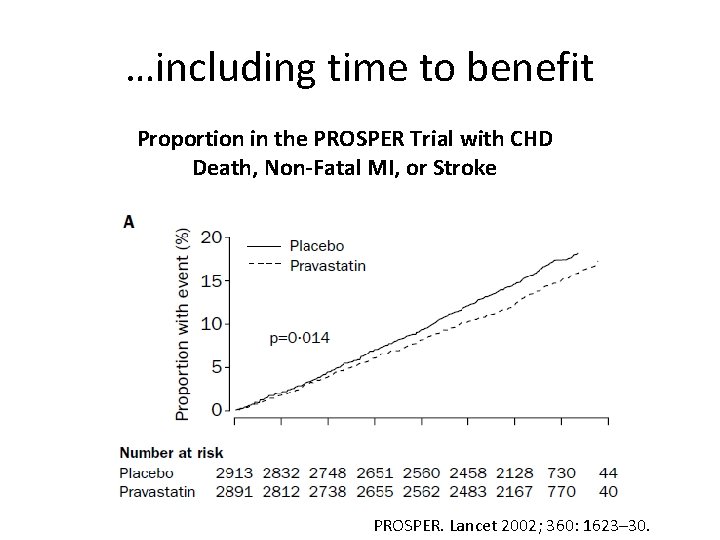
…including time to benefit Proportion in the PROSPER Trial with CHD Death, Non-Fatal MI, or Stroke PROSPER. Lancet 2002; 360: 1623– 30.
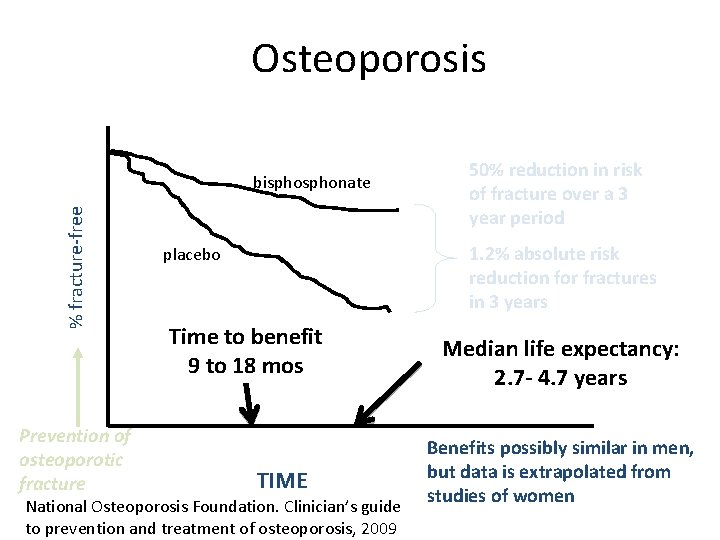
Osteoporosis % fracture-free bisphonate Prevention of osteoporotic fracture 50% reduction in risk of fracture over a 3 year period 1. 2% absolute risk reduction for fractures in 3 years placebo Time to benefit 9 to 18 mos TIME National Osteoporosis Foundation. Clinician’s guide to prevention and treatment of osteoporosis, 2009 Median life expectancy: 2. 7 - 4. 7 years Benefits possibly similar in men, but data is extrapolated from studies of women

No “best” approach to either communicate prognosis nor effect “optimal” clinical decision making Guidelines lack adequate ways to assess prognosis Published prognosis measures have limited generalizability Overwhelming to evaluate prognosis Uncertainty in how to use prognostic measures in clinical practice

Consider patient preferences… • Influenced by the way risk information is presented to the patient • Multimorbidity patients face more preference-based and complex decisions • Eliciting preferences may make clinical management more timeconsuming

…and patient capabilities Medication Management Capacity Drug Regimen Unassisted Grading Scale (DRUGS) Edelberg HK, Shallenberger E, Wei JY. Medication management capacity in highly functioning community-living older adults: detection of early deficits. J Am Geriatr Soc. 1999 May; 47(5): 592 -6. Hopkins Medication Schedule (HMS) Carlson MC, Fried, LP, Xue QL, et al. Validation of the Hopkins Medication Schedule to Identify Difficulties in Taking Medications Journal of Gerontology: Feb 2005; 60 A, 2: Health Module 217 -223 Medication Management Instrument for Deficiencies in the Elderly (Med. Ma. IDE) Orwig D, Brandt N, Gruber-Baldini, A. Medication Management Assessment for Older Adults in the Community. The Gerontologist 2006; 46: 661 -668

PUTTING IT ALL TOGETHER…

Inappropriate Prescribing Methods to Look at Inappropriate Prescribing e. g. : – American Geriatrics Society 2012 Beer’s Criteria – STOPP (Screening Tool of Older Persons’ potentially inappropriate Prescriptions) – START (Screening Tool to Alert doctors to the Right Treatment) – Clinical Judgment Hamilton HJ. Inappropriate Prescribing and adverse drug events in older people. BMJ Geriatrics (2009). Accessed at www. biomedcentral. com/1471 -2318/9/5 Bergert FW, Conrad D, Ehrenthal EJ et al. Pharmacotherapy Guidelines for the aged by family doctors for the use of family doctors. Inter J Clin Pharm Ther (2008) 46: 600 -616.

HISTORY AND DEVELOPMENT OF THE AGS 2012 BEERS CRITERIA

Mark H Beers, MD 1954 -2009 “ A ballet-dancing opera critic who hiked the Alps and took up rowing after diabetes cost him his legs” • MD, University of Vermont • First medical student to do a geriatrics elective at Harvard‘s new Division on Aging • Geriatric Fellowship, Harvard • Faculty, UCLA/RAND • Co-editor, Merck Manual of Geriatrics • Editor in Chief, Merck Manuals

Beers Criteria: History and Utilization • Original 1991 – Nursing home pts • Updates – 1997: All elderly; adopted by CMS in 1999 for nursing home regulation – 2003: Era of generalization to Med D, then NCQA, HEDIS – 2012: Further adoption into quality measures

Specific Aims AGS 2012 Beers Criteria Specific aim – update 2003 Beers Criteria using a comprehensive, systematic review and grading of evidence Strategy: 1. Incorporate new evidence 2. Grade the evidence 3. Use an interdisciplinary panel 4. Incorporate exceptions

Method Framework • Expert panel – 11 members • IOM 2011 report on guideline development – Includes a period for public comment • Literature search

Panel Members • Co-chairs – Donna Fick, Ph. D – Todd Semla, MS, Pharm. D • Panelists (voting) – – – – – Judith Beizer, Pharm. D Nicole Brandt, Pharm. D Catherine Du. Beau, MD Nina Flanagan, CRNP, CS-BC Joseph Hanlon, Pharm. D, MS Peter Hollmann, MD Sunny Linnebur, Pharm. D Stinderpal Sandhu, MD Michael Steinman, MD • Nonvoting Panelists – Robert Dombrowski, Pharm. D (CMS) – David Nau, Ph. D (PQA) – Bob Rehm (NCQA) • AGS Staff – Christine Campenelli – Elvy Ickowicz, MPH • Others – Sue Radcliff (research) – Susan Aiello, DVM (editing)

Method • Literature search: ADE, inappropriate drug use, med errors, polypharmacy x age/human/English 25, 549 citations 12/1/2001 – 3/30/2011 19, 044 excluded 6, 505 prelim review 4238 excluded 2, 267 reviewed by co-chairs Additional searches, additions 844 excluded 2169 reviewed Additional searches, additions 258 included in evidence tables

Method • Survey to panel to rate (strong agree strong disagree) – 2003 Beers meds – New additions • Ratings tallied, shared with panel, 2 rounds of consensus • In-person: review survey draft and lit search • 4 groups reviewed lit, selected citations • Evidence tables prepared, rated quality of evidence and strength of recommendation • Final group consensus

Designations of Quality and Strength of Evidence: ACP Guideline Grading System, GRADE Quality • High Evidence – Consistent results from well-designed, well-conducted studies that directly assess effects on health outcomes (2 consistent, higher-quality RCTs or multiple, consistent observational studies with no significant methodological flaws showing large effects) • Moderate Evidence – Sufficient to determine effects on health outcomes, but the number, quality, size, or consistency of included studies, generalizability, indirect nature of the evidence on health outcomes (1 higher-quality trial with > 100 participants; 2 higher-quality trials with some inconsistency, or 2 consistent, lower-quality trials; or multiple, consistent observational studies with no significant methodological flaws showing at least moderate effects) limits the strength of the evidence • Low Evidence Insufficient to assess effects on health outcomes because of limited number or power of studies, large and unexplained inconsistency between higher-quality studies; important flaws in design or conduct, gaps in the chain of evidence – Or lack of information on important health outcomes –

Designations of Quality and Strength of Evidence: ACP Guideline Grading System, GRADE Strength of recommendation • Strong: – Benefits clearly > risks and burden OR risks and burden clearly > benefits • Weak: – Benefits finely balanced with risks and burden • Insufficient: – Insufficient evidence to determine net benefits or risks

AGS 2012 BEERS CRITERIA CLINICAL HIGHLIGHTS & EVIDENCE

Need for Updates or New Criteria • Continuous arrivals of new drugs on the market 1 • Older formulations unavailable in European formularies 2 • Only 12 -21% of the medications identified are being used by older adults 3 • Tangible benefit to patients in terms of clinical outcomes 2 Fick D, Cooper J, Wade W, et al. Arch Intern Med 2003; 163: 2716 -2724 1 Hamilton H, Gallagher P, Ryan C, Arch Intern Med 2011; 171(11): 1013 -1019 2 Rudolph J, Salow M, Angelini M et al. Arch Inern Med 2008; 168 (5): 508 -513 3

Beers Criteria- 3 Main Tables 1) Table 2: Medications or medication classes that should be avoided in persons 65 years or older 1) Table 3: Medications that should not be used in older person known to have specific medical diseases or conditions. 1) Table 4: Medications that should be used with caution

Beers Criteria: Overall Results • A total of 53 medications or medication classes, which are divided into three tables. • Constructed and organized by: – major therapeutic classes and – organ systems

Beers Criteria: Table 2 Results – 34 potentially inappropriate medications/classes to avoid in older adults independent of diagnoses or conditions. – Notable mentions: – Sliding Scale Insulin – Antipsychotics for Behavioral Health issues associated with dementia – Non benzodiazepine Hypnotics – Megestrol

Sliding Scale Organ Rationale System/ Therapeutic Category/D rug(s) Insulin, Higher risk of sliding scale hypoglycemia without improvement in hyperglycemia management regardless of care setting. Recom Quality of mendati Evidence on Strength of References Recommen dation Avoid Strong Moderate Queale 1997 Important to look at during transitions in care due to the fact that PO Diabetes meds are stopped when they are admitted and typically have insulin protocols in place.
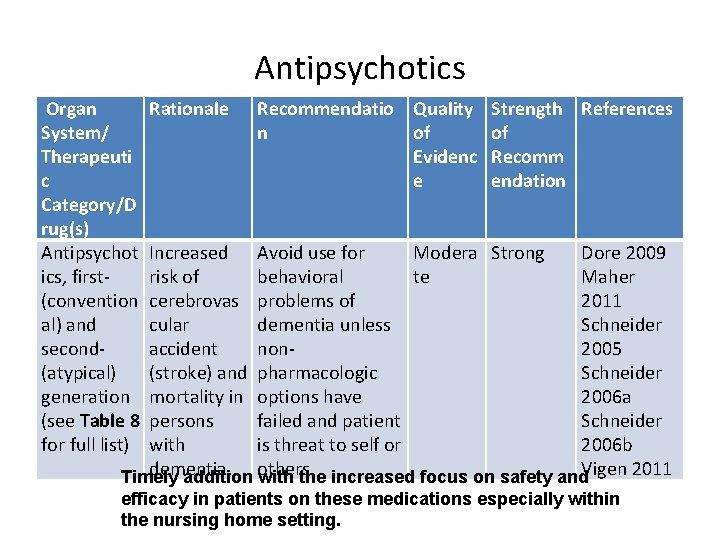
Antipsychotics Organ System/ Therapeuti c Category/D rug(s) Antipsychot ics, first(convention al) and second(atypical) generation (see Table 8 for full list) Rationale Recommendatio Quality Strength References n of of Evidenc Recomm e endation Increased Avoid use for Modera Strong Dore 2009 risk of behavioral te Maher cerebrovas problems of 2011 cular dementia unless Schneider accident non 2005 (stroke) and pharmacologic Schneider mortality in options have 2006 a persons failed and patient Schneider with is threat to self or 2006 b dementia. Timely addition others. with the increased focus on safety and. Vigen 2011 efficacy in patients on these medications especially within the nursing home setting.
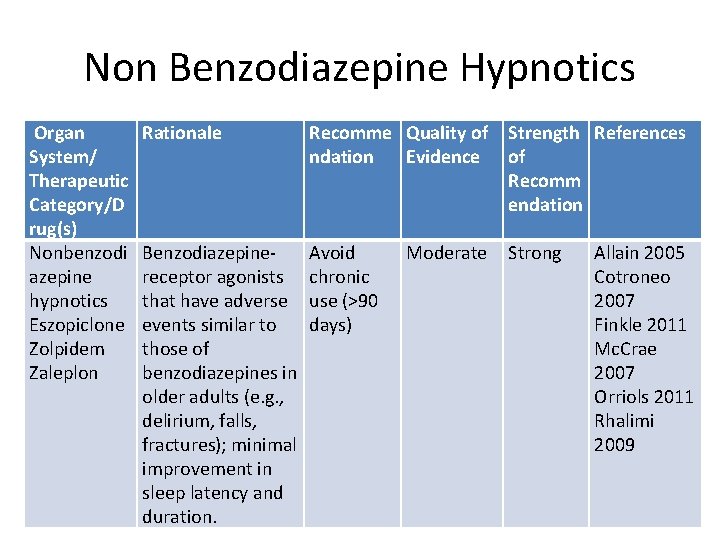
Non Benzodiazepine Hypnotics Organ System/ Therapeutic Category/D rug(s) Nonbenzodi azepine hypnotics Eszopiclone Zolpidem Zaleplon Rationale Recomme Quality of ndation Evidence Strength References of Recomm endation Benzodiazepinereceptor agonists that have adverse events similar to those of benzodiazepines in older adults (e. g. , delirium, falls, fractures); minimal improvement in sleep latency and duration. Avoid chronic use (>90 days) Strong Moderate Allain 2005 Cotroneo 2007 Finkle 2011 Mc. Crae 2007 Orriols 2011 Rhalimi 2009

Megestrol Organ Rationale Recomm Quality System/ endation of Therapeutic Evidence Category/D rug(s) Megestrol Minimal effect on Avoid Moderat weight; increases e risk of thrombotic events and possibly death in older adults. Strength of References Recomme ndation Strong Bodenner 2007 Reuben 2005 Simmons 2005 Yeh 2000
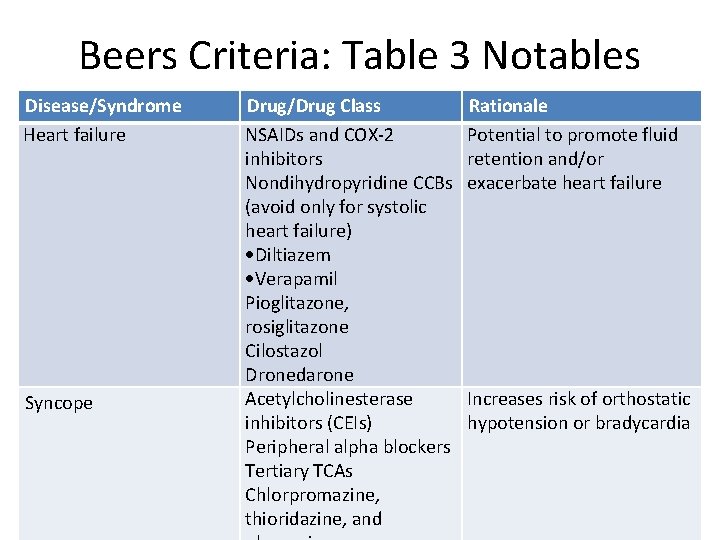
Beers Criteria: Table 3 Notables Disease/Syndrome Heart failure Syncope Drug/Drug Class NSAIDs and COX-2 inhibitors Nondihydropyridine CCBs (avoid only for systolic heart failure) Diltiazem Verapamil Pioglitazone, rosiglitazone Cilostazol Dronedarone Acetylcholinesterase inhibitors (CEIs) Peripheral alpha blockers Tertiary TCAs Chlorpromazine, thioridazine, and Rationale Potential to promote fluid retention and/or exacerbate heart failure Increases risk of orthostatic hypotension or bradycardia
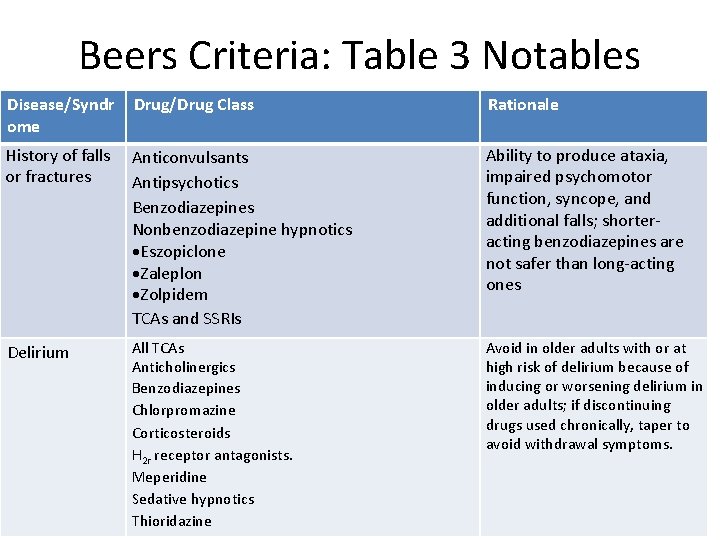
Beers Criteria: Table 3 Notables Disease/Syndr ome Drug/Drug Class Rationale History of falls or fractures Anticonvulsants Antipsychotics Benzodiazepines Nonbenzodiazepine hypnotics Eszopiclone Zaleplon Zolpidem TCAs and SSRIs Ability to produce ataxia, impaired psychomotor function, syncope, and additional falls; shorteracting benzodiazepines are not safer than long-acting ones Delirium All TCAs Anticholinergics Benzodiazepines Chlorpromazine Corticosteroids H 2 r receptor antagonists. Meperidine Sedative hypnotics Thioridazine Avoid in older adults with or at high risk of delirium because of inducing or worsening delirium in older adults; if discontinuing drugs used chronically, taper to avoid withdrawal symptoms.
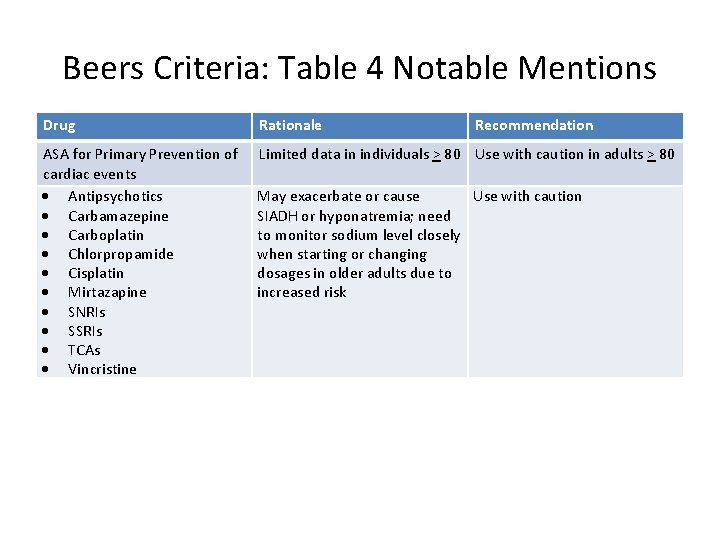
Beers Criteria: Table 4 Notable Mentions Drug Rationale Recommendation ASA for Primary Prevention of cardiac events Antipsychotics Carbamazepine Carboplatin Chlorpropamide Cisplatin Mirtazapine SNRIs SSRIs TCAs Vincristine Limited data in individuals > 80 Use with caution in adults > 80 May exacerbate or cause Use with caution SIADH or hyponatremia; need to monitor sodium level closely when starting or changing dosages in older adults due to increased risk

Limitations • Older adults often under-represented in drug trials potentially underestimating medication related problems/evidence grading. • Does not comprehensively address the needs of palliative and hospice care patients • Does not address other types of potentially inappropriate medications – e. g. : • dosing of primarily renally eliminated medications, • drug- interactions

Take Home Points • This is just one tool that can be utilized to optimize medication management in older adults. • Need to make sure the Beers list is used in a patient centered manner

Resources Available Online www. americangeriatrics. org For the Health Professional • Downloadable pocket card • Evidence tables with links to supporting references • Beers app – AGS i. Geriatrics For the Layperson • Summary in lay language • Q & A on what to do if one of your drugs is on the Beers list • Medication diary & tips for safe use of meds
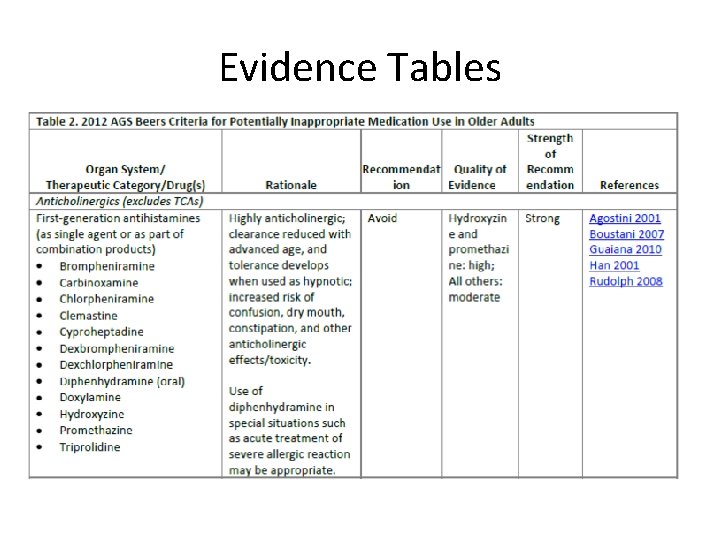
Evidence Tables

Patient Education

Beers Criteria only Part of Quality Prescribing Quality prescribing includes: • Correct drug for correct diagnosis • Appropriate dose (label; dose adjustments for co-morbidity, drug-drug interactions) • Avoiding underuse of potentially important medications (e. g. , bisphonates for osteoporosis) • Avoiding overuse (e. g. , antibiotics) • Avoiding potentially inappropriate drugs • Avoiding withdrawal effects with discontinuation • Consideration of cost
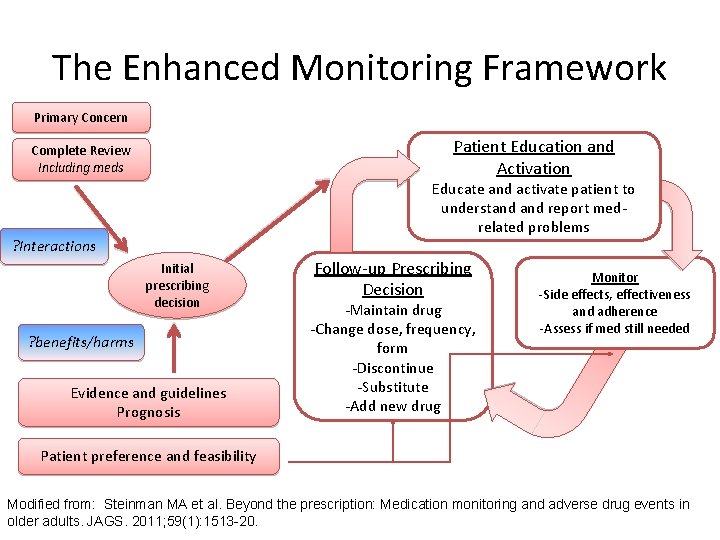
The Enhanced Monitoring Framework Primary Concern Patient Education and Activation Complete Review Including meds Educate and activate patient to understand report medrelated problems ? Interactions Initial prescribing decision ? benefits/harms Evidence and guidelines Prognosis Follow-up Prescribing Decision -Maintain drug -Change dose, frequency, form -Discontinue -Substitute -Add new drug Monitor -Side effects, effectiveness and adherence -Assess if med still needed Patient preference and feasibility Modified from: Steinman MA et al. Beyond the prescription: Medication monitoring and adverse drug events in older adults. JAGS. 2011; 59(1): 1513 -20.

Why is this important? • Quality Metrics – HEDIS: http: //www. ncqa. org/HEDISQuality. Measurement /HEDISMeasures/HEDIS 2013 Final. NDC Lists. aspx • Improved patient care • Decrease liability

Take Home Points • Medication Management & Monitoring takes a team! • It needs to be patient centered. • Most importantly, monitoring needs to be evaluated on an ongoing basis.
- Slides: 59