PGY 101 Chapter 74 Breast Breast Cancer in

PGY 101: Chapter 74 Breast

Breast Cancer in the US • Breast Cancer is estimated to affect over 230, 000 women annually in the US • Based on SEER Database rates from 2009 -2011, the cumulative lifetime risk of an average woman in the general US population is 12. 3% • Estimated 15, 480 new cases of female breast cancer in Florida
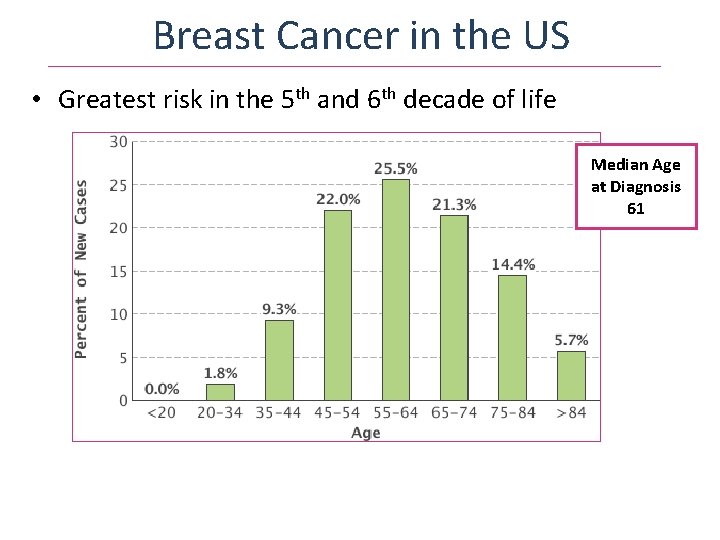
Breast Cancer in the US • Greatest risk in the 5 th and 6 th decade of life Median Age at Diagnosis 61
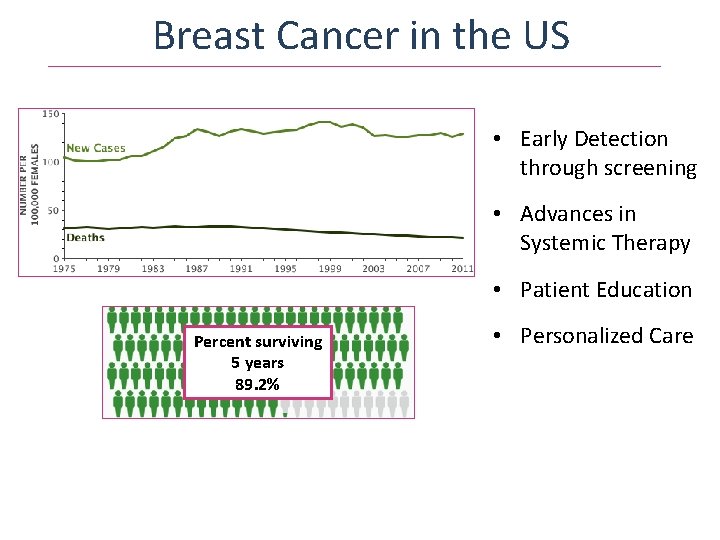
Breast Cancer in the US • Early Detection through screening • Advances in Systemic Therapy • Patient Education Percent surviving 5 years 89. 2% • Personalized Care
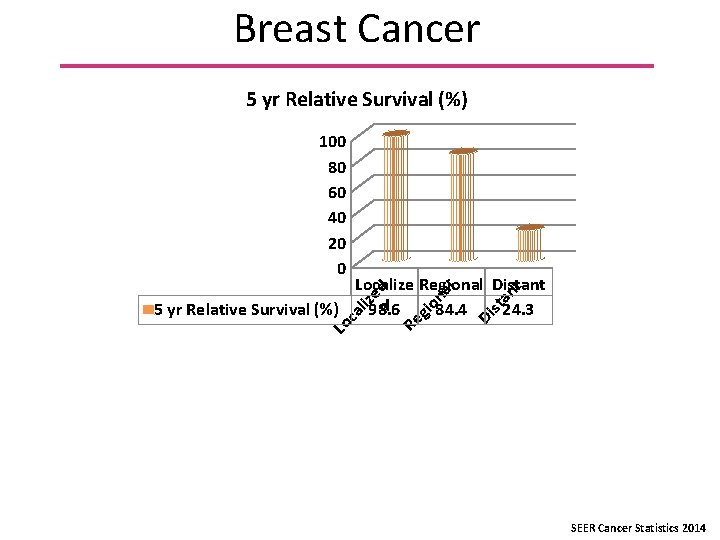
Breast Cancer 5 yr Relative Survival (%) 100 80 60 40 20 0 t st an Di gi on Re Lo ca liz e d al Localize Regional Distant d 5 yr Relative Survival (%) 98. 6 84. 4 24. 3 SEER Cancer Statistics 2014
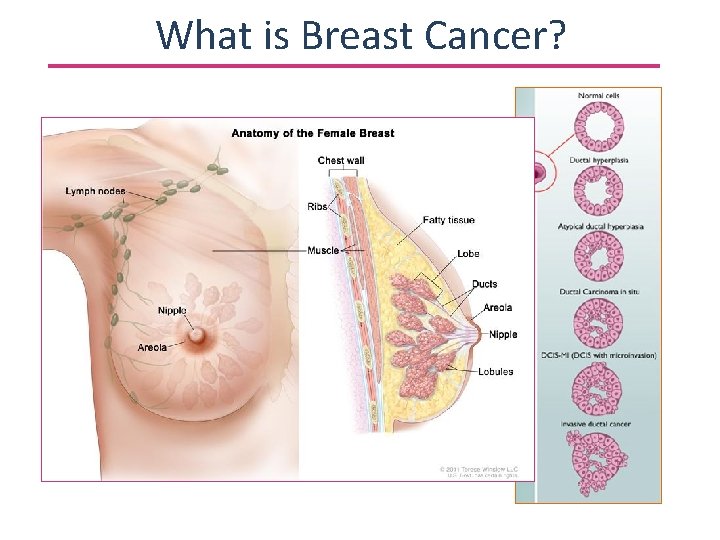
What is Breast Cancer?
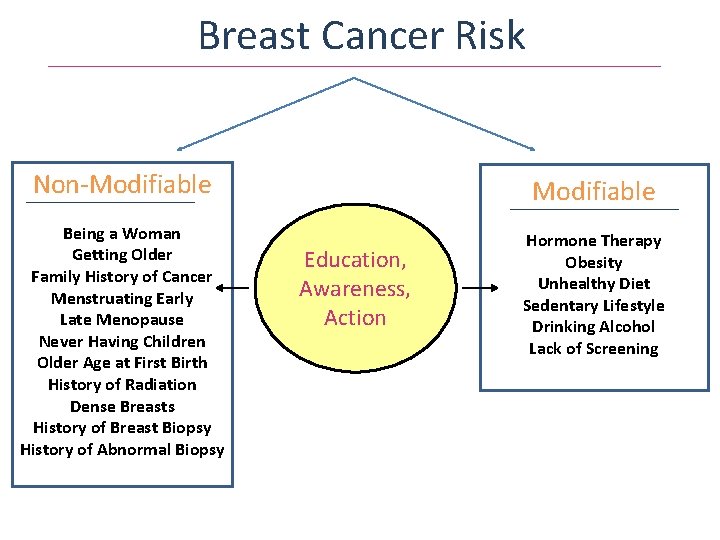
Breast Cancer Risk Non-Modifiable Being a Woman Getting Older Family History of Cancer Menstruating Early Late Menopause Never Having Children Older Age at First Birth History of Radiation Dense Breasts History of Breast Biopsy History of Abnormal Biopsy Hormone Therapy Obesity Unhealthy Diet Sedentary Lifestyle Drinking Alcohol Lack of Screening Education, Awareness, Action

Hereditary Breast Cancer Family History • History of Breast Cancer in First degree relatives increase an individuals risk of breast cancer • 2 -fold increased risk in women whose sisters or mothers have had breast cancer Stratton MR. Nat Genet. 2008; 40: 17
Genetics • Approximately 5 -10% of all breast cancer • Known inherited alterations in genes that lead to an increased risk of developing breast cancer • Lead to a 10 - to 20 – fold increased lifetime risk of developing breast cancer as well as many associated cancers • Ovarian, Pancreas, Prostate, Melanoma, Thyroid, Colon • Cancers occur at younger ages

Inherited Gene Alterations • BR (Breast) CA (Cancer) Susceptibility genes (BRCA 1 & BRCA 2) • Approximately 80% of all hereditary breast cancers • Cumulative lifetime risk of Breast Cancer: • BRCA 1 – 65 -87% • BRCA 2 – 45 -55% • Cumulative lifetime risk of Ovarian Cancer: • BRCA 1 – 39 -51% • BRCA 2 – 11 -35%
What if a Woman has a strong Family History but Negative for BRCA?

Risk Calculators
Screening • Mammography remains the only study proven to detect early breast cancer and decrease breast cancer related deaths • Breast cancer mortality reduction up to 40% • Screening detected cancers • Smaller in size • Less likely to have lymph nodes involved • Less likely to receive chemotherapy

American Cancer Society Recommendations • Yearly mammograms are recommended starting at age 40 and continuing for as long as a woman is in good health • Clinical breast exam (CBE) about every 3 years for women in their 20 s and 30 s and every year for women 40 and over • Women should know how their breasts normally look and feel and report any breast change promptly to their health care provider • Breast self-exam (BSE) is an option for women starting in their 20 s Recommendations vary based on risk

Screening • General Population – Baseline mammogram between 35 -40 and annual mammography starting at age 40. • Start 10 years younger then your youngest 1 st degree relative diagnosed with breast cancer • High Risk Population – Annual mammography and MRI starting at the age of 30 • BRCA 1 or 2 carriers • 1 st degree relative of BRCA carriers but untested • Lifetime risk of 20 -25% based on family risk assessment models • History of chest wall radiation
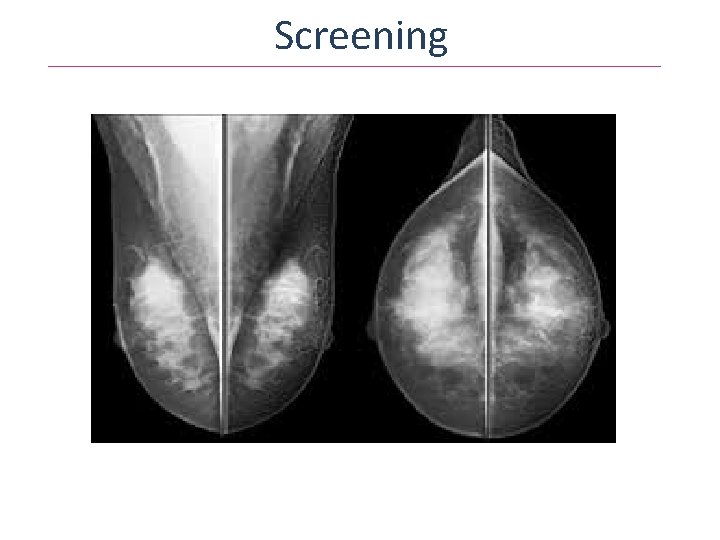
Screening
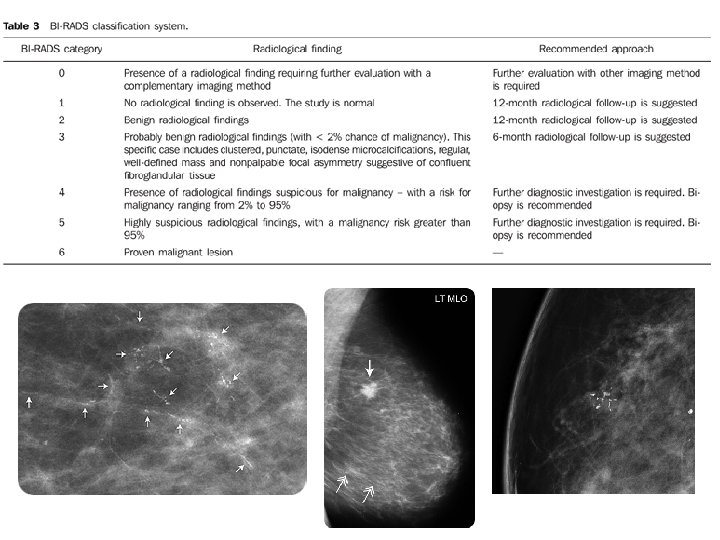
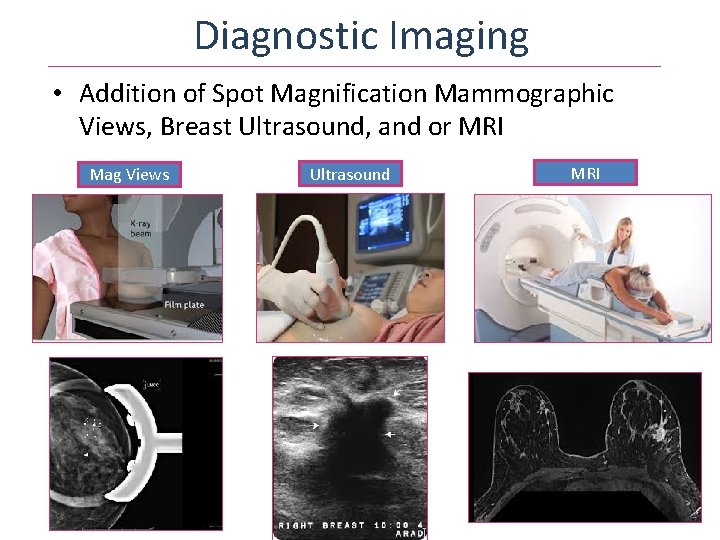
Diagnostic Imaging • Addition of Spot Magnification Mammographic Views, Breast Ultrasound, and or MRI Mag Views Ultrasound MRI
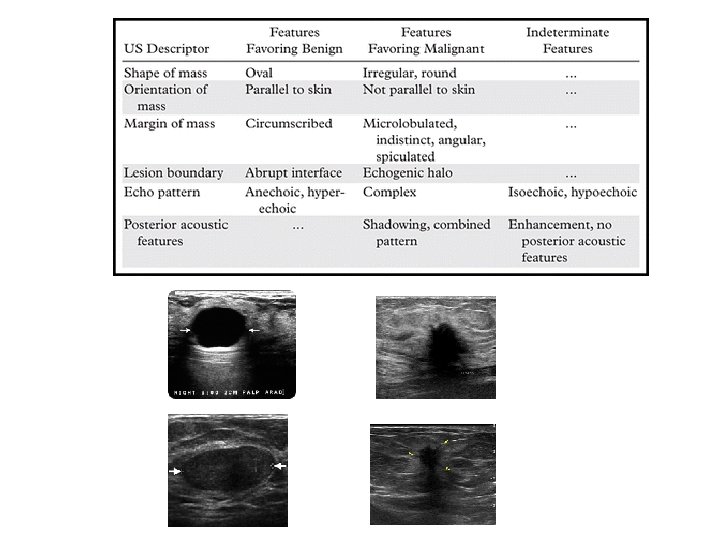
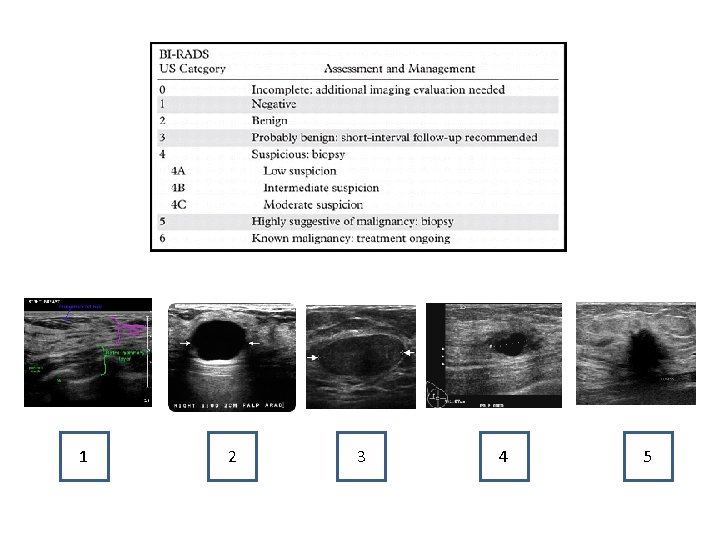
1 2 3 4 5
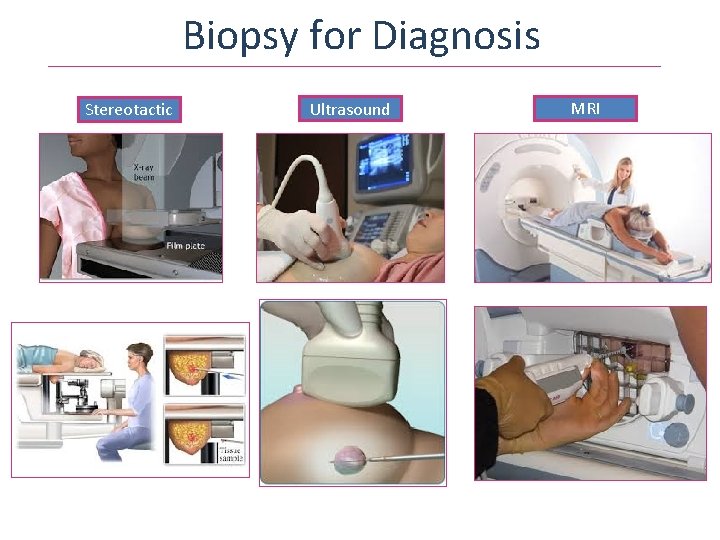
Biopsy for Diagnosis Stereotactic Ultrasound MRI
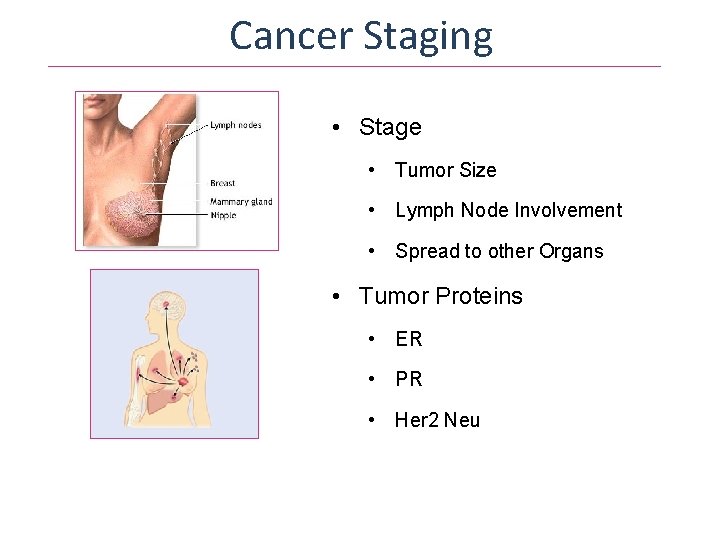
Cancer Staging • Stage • Tumor Size • Lymph Node Involvement • Spread to other Organs • Tumor Proteins • ER • PR • Her 2 Neu
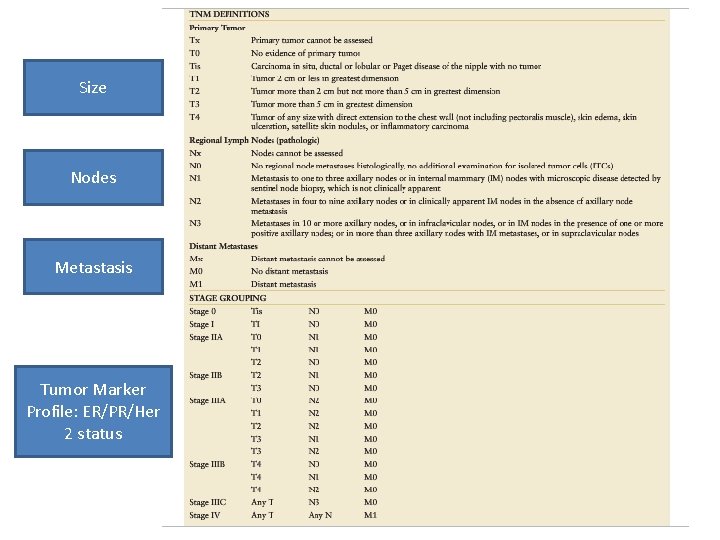
Size Nodes Metastasis Tumor Marker Profile: ER/PR/Her 2 status
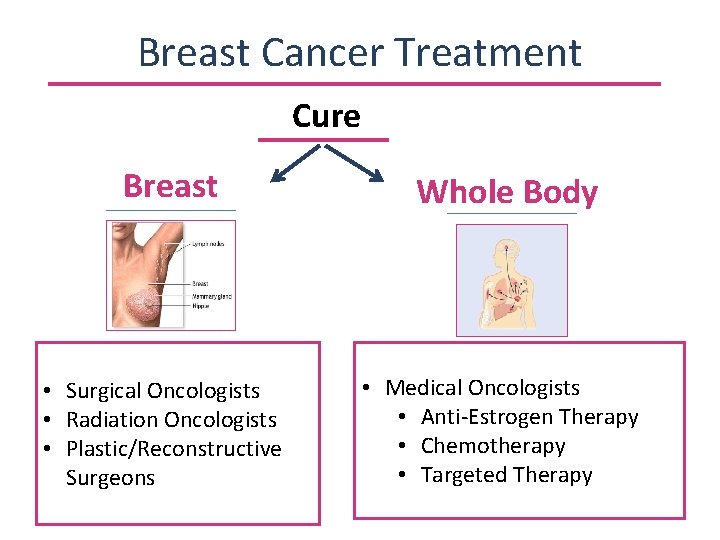
Breast Cancer Treatment Cure Breast Whole Body • Surgical Oncologists • Radiation Oncologists • Plastic/Reconstructive Surgeons • Medical Oncologists • Anti-Estrogen Therapy • Chemotherapy • Targeted Therapy
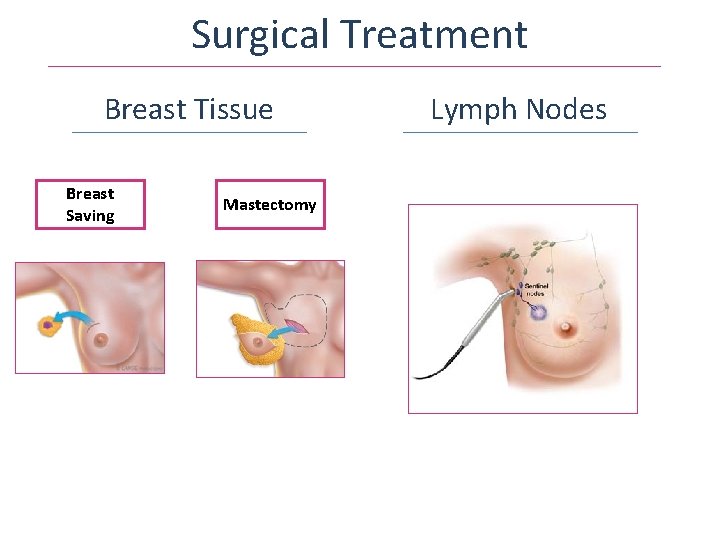
Surgical Treatment Breast Tissue Breast Saving Mastectomy Lymph Nodes

Dr. William S. Halsted (1852 -1922) Halstedian Principle: “Cancer spreads in an orderly, slow, and localized manner, contiguous with its site of origin”
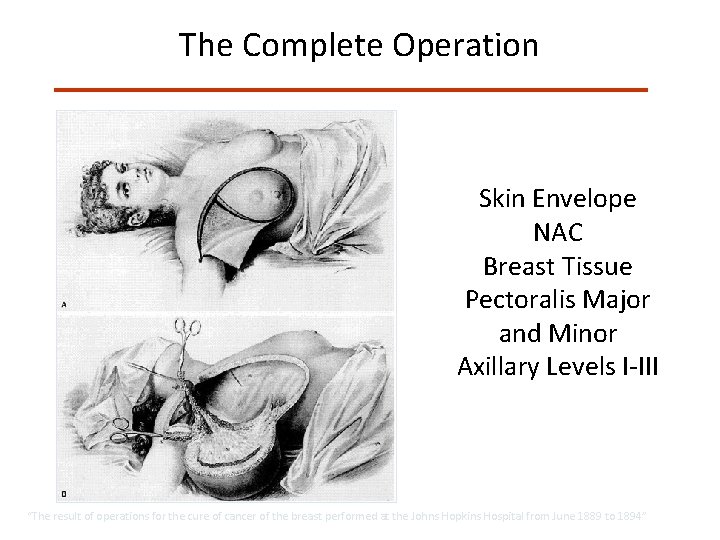
The Complete Operation Skin Envelope NAC Breast Tissue Pectoralis Major and Minor Axillary Levels I-III “The result of operations for the cure of cancer of the breast performed at the Johns Hopkins Hospital from June 1889 to 1894”
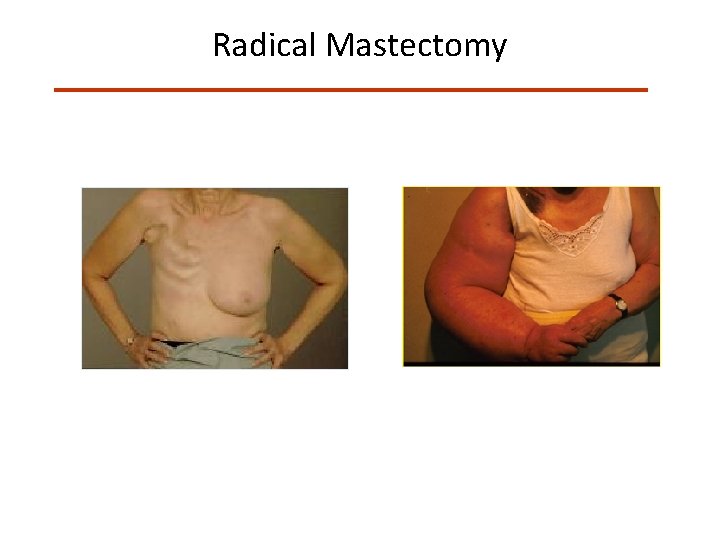
Radical Mastectomy
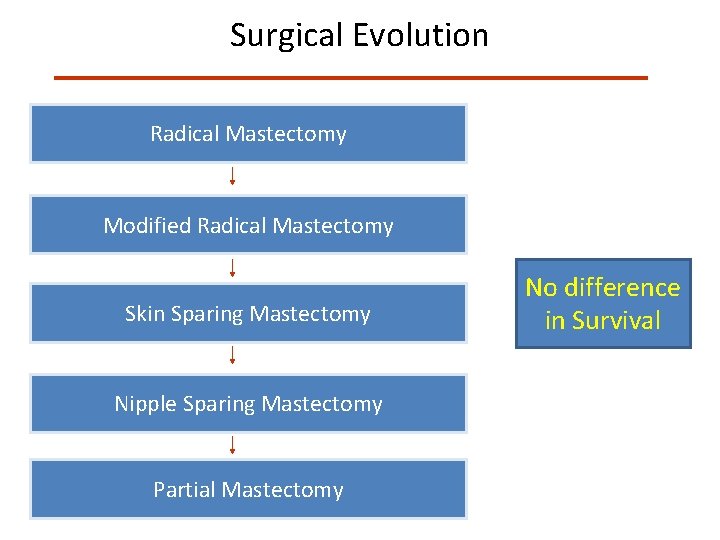
Surgical Evolution Radical Mastectomy Modified Radical Mastectomy Skin Sparing Mastectomy Nipple Sparing Mastectomy Partial Mastectomy No difference in Survival
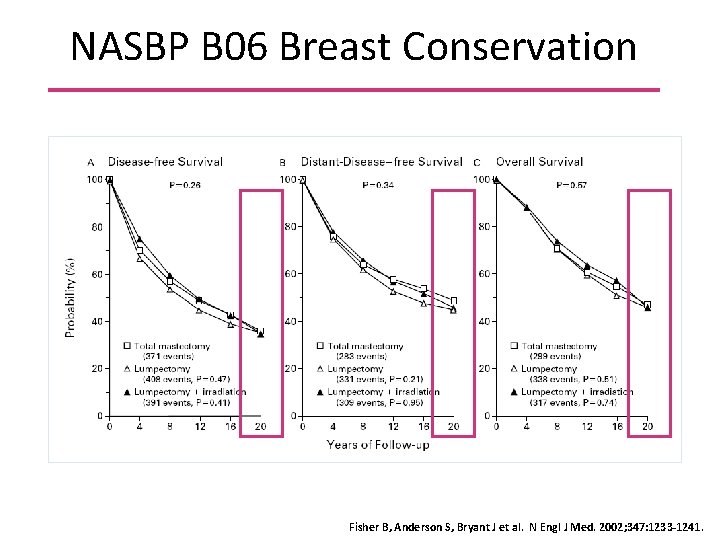
NASBP B 06 Breast Conservation Fisher B, Anderson S, Bryant J et al. N Engl J Med. 2002; 347: 1233 -1241.
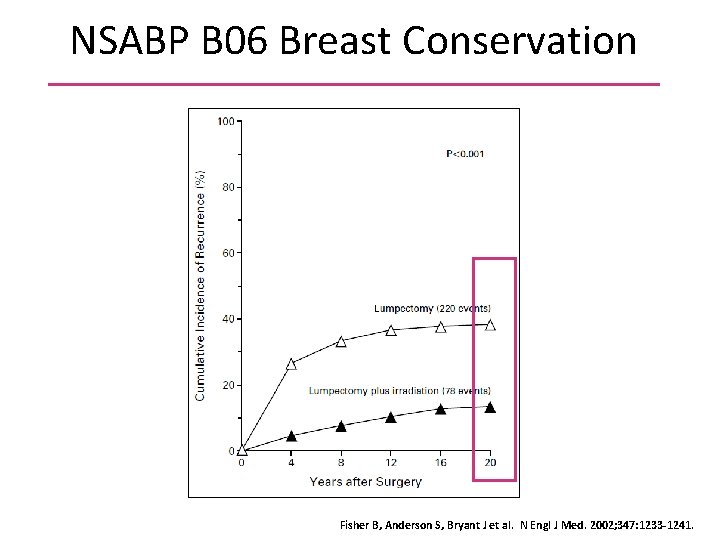
NSABP B 06 Breast Conservation Fisher B, Anderson S, Bryant J et al. N Engl J Med. 2002; 347: 1233 -1241.
Breast Conservation Candidacy • • • Focality of Disease Tumor Location PMH/Genetic Prior Radiation Cosmetic Outcome

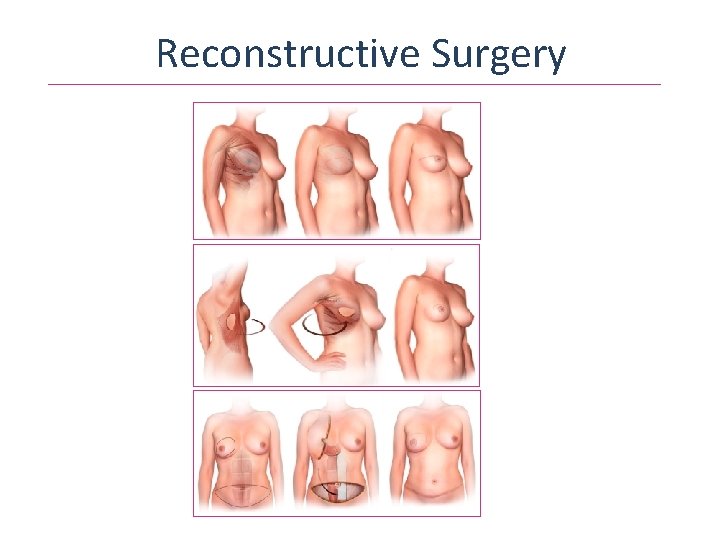
Reconstructive Surgery

Reconstructive Surgery Women’s Health and Cancer Rights Act of 1998 Mandated that all health plans include breast and nipple reconstruction as well as contralateral breast symmetry procedures to all mastectomy patients
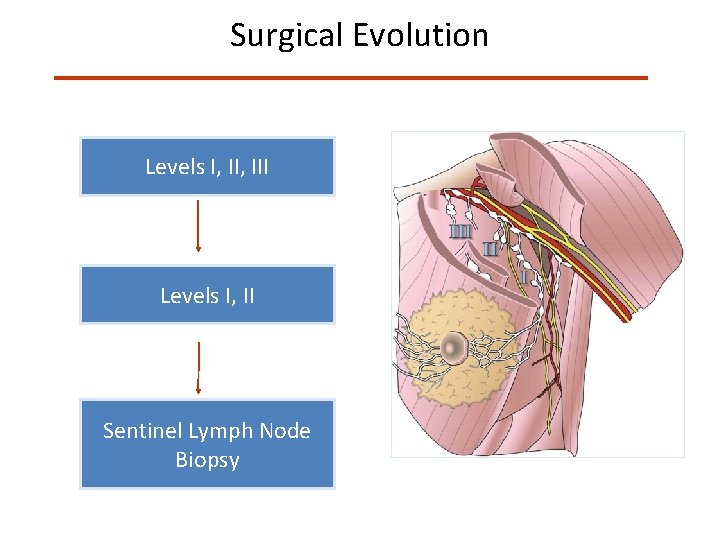
Surgical Evolution Levels I, III Levels I, II Sentinel Lymph Node Biopsy
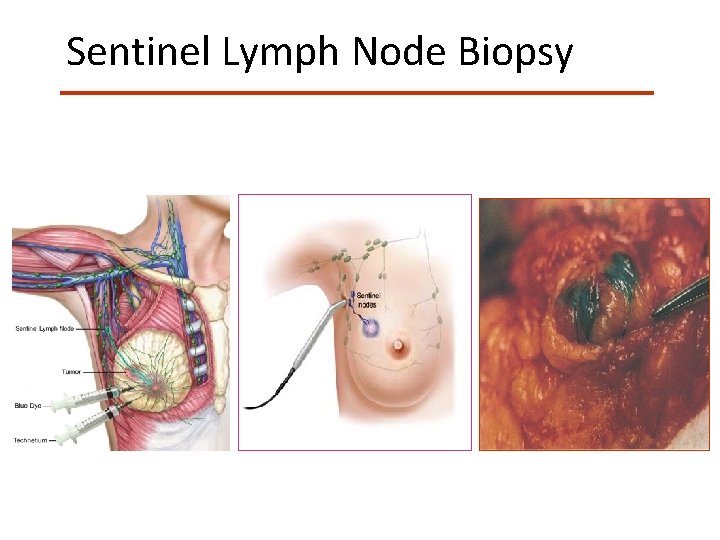
Sentinel Lymph Node Biopsy Giuliano AE. Ann Surg. 1994; 220: 391 -401
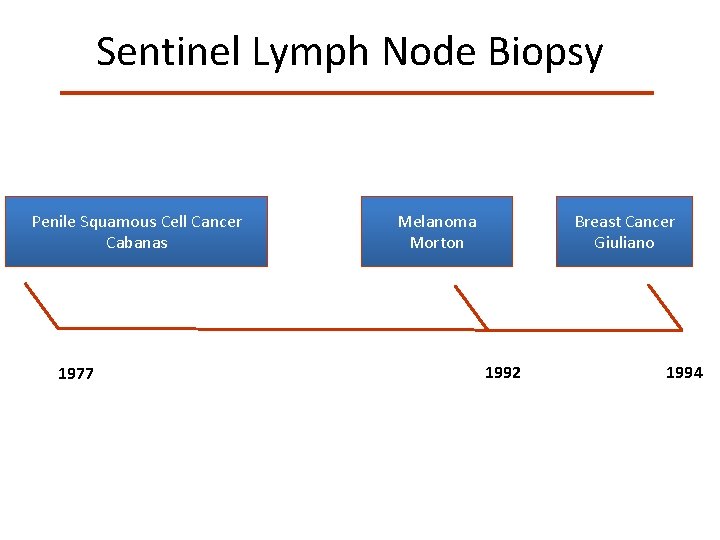
Sentinel Lymph Node Biopsy Penile Squamous Cell Cancer Cabanas 1977 Melanoma Morton Breast Cancer Giuliano 1992 1994 Cabanas RM. Cancer. 1977; 39: 456 -466. Morton DL. Surg Oncol Clin North Am. 1992; 1: 247 -259 Giuliano AE. Ann Surg. 1994; 220: 391 -401

Study Year (n) Giuliano 1994 174 Identification Accuracy 78. 0 95. 6 Negative Sensitivity Predictive Value 93. 5 93. 7 False Negative Rate 4. 3 Sentinel lymph node biopsy is an accurate method of axillary lymph node staging in women with early stage clinically node negative breast cancer Giuliano AE. Ann Surg. 1994; 220: 391 -401
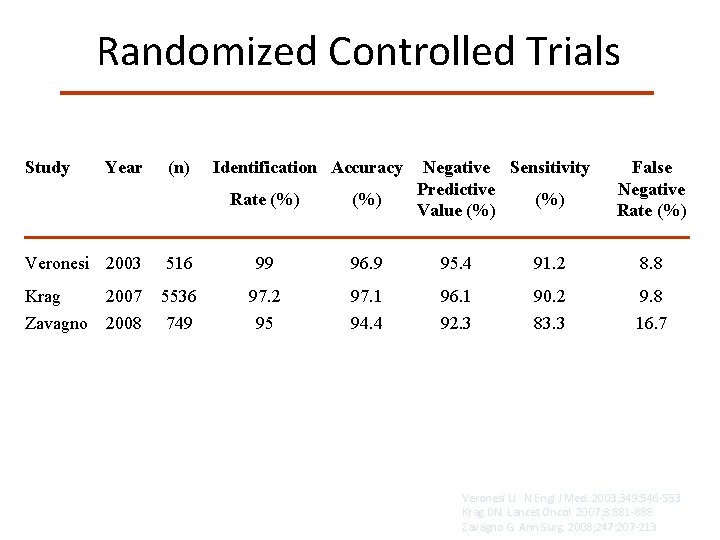
Randomized Controlled Trials Study Year (n) Identification Accuracy Rate (%) Negative Sensitivity Predictive (%) Value (%) False Negative Rate (%) Veronesi 2003 516 99 96. 9 95. 4 91. 2 8. 8 Krag Zavagno 5536 749 97. 2 95 97. 1 94. 4 96. 1 92. 3 90. 2 83. 3 9. 8 16. 7 2008 Veronesi U. N Engl J Med. 2003; 349: 546 -553 Krag DN. Lancet Oncol. 2007; 8: 881 -888 Zavagno G. Ann Surg. 2008; 247: 207 -213
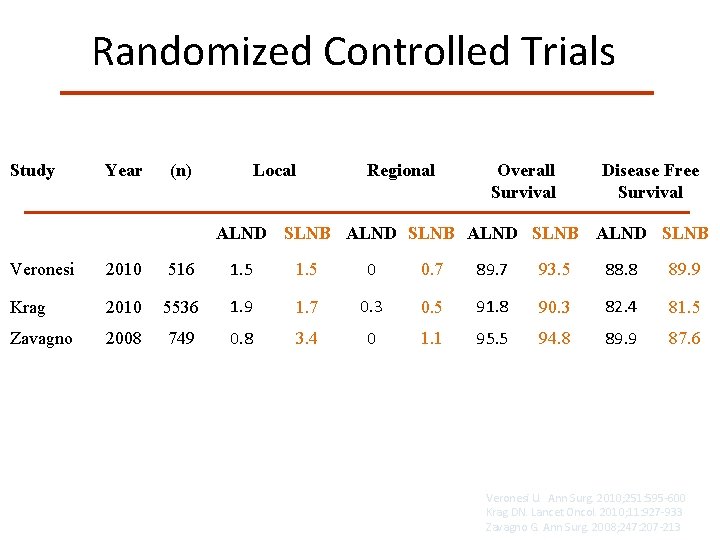
Randomized Controlled Trials Study Year (n) Local Regional Overall Survival Disease Free Survival ALND SLNB Veronesi 2010 516 1. 5 0 0. 7 89. 7 93. 5 88. 8 89. 9 Krag 2010 5536 1. 9 1. 7 0. 3 0. 5 91. 8 90. 3 82. 4 81. 5 Zavagno 2008 749 0. 8 3. 4 0 1. 1 95. 5 94. 8 89. 9 87. 6 Veronesi U. Ann Surg. 2010; 251: 595 -600 Krag DN. Lancet Oncol. 2010; 11: 927 -933 Zavagno G. Ann Surg. 2008; 247: 207 -213
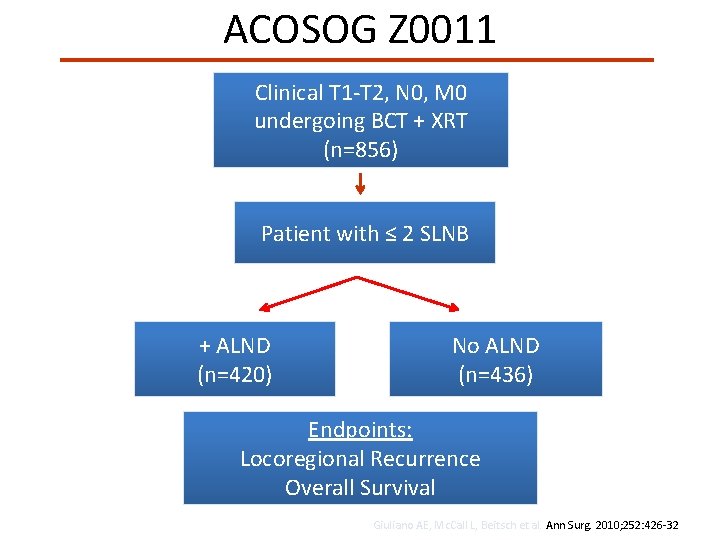
ACOSOG Z 0011 Clinical T 1 -T 2, N 0, M 0 undergoing BCT + XRT (n=856) Patient with ≤ 2 SLNB + ALND (n=420) No ALND (n=436) Endpoints: Locoregional Recurrence Overall Survival Giuliano AE, Mc. Call L, Beitsch et al. Ann Surg. 2010; 252: 426 -32
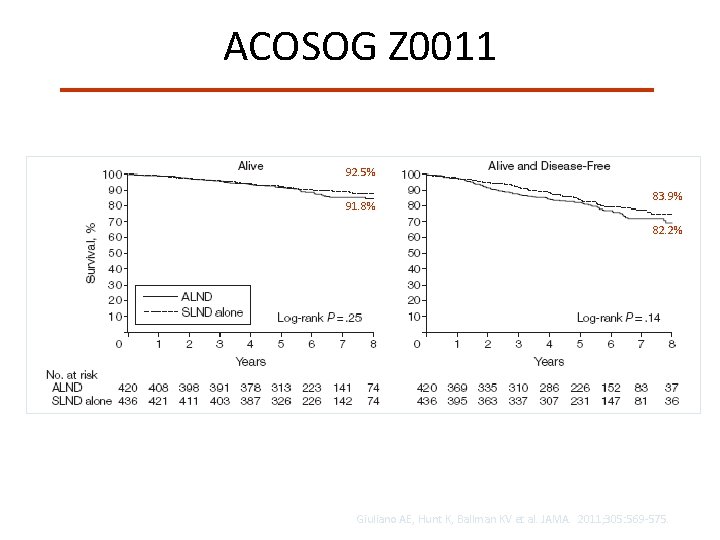
ACOSOG Z 0011 92. 5% 91. 8% 83. 9% 82. 2% Giuliano AE, Hunt K, Ballman KV et al. JAMA. 2011; 305: 569 -575.
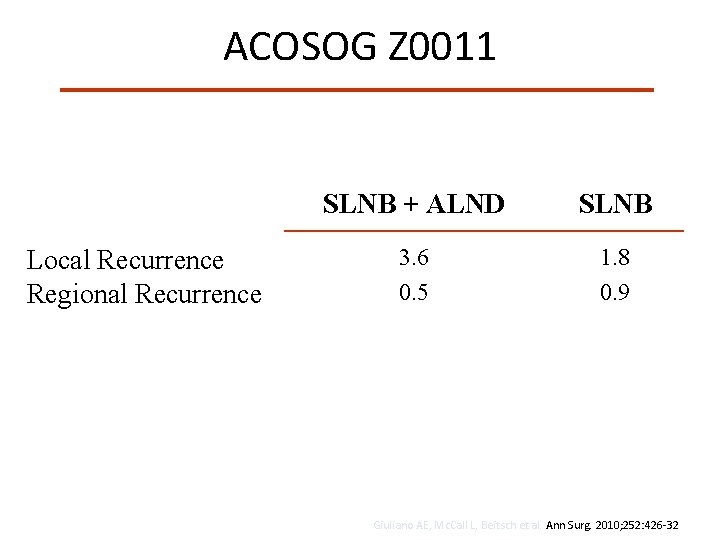
ACOSOG Z 0011 Local Recurrence Regional Recurrence SLNB + ALND SLNB 3. 6 0. 5 1. 8 0. 9 Giuliano AE, Mc. Call L, Beitsch et al. Ann Surg. 2010; 252: 426 -32

ACOSOG Z 0011 • At 6. 3 year follow-up, women with clinically node-negative early stage breast cancer with < 3 positive sentinel nodes, who underwent breast conservation surgery demonstrated: – No Benefit in Locoregional control following ALND – No Benefit in Overall or Disease-free survival following ALND
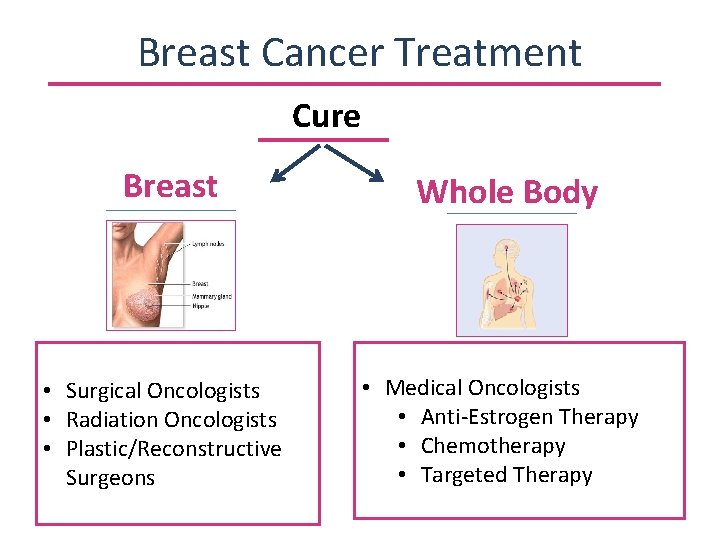
Breast Cancer Treatment Cure Breast Whole Body • Surgical Oncologists • Radiation Oncologists • Plastic/Reconstructive Surgeons • Medical Oncologists • Anti-Estrogen Therapy • Chemotherapy • Targeted Therapy

Adjuvant Therapy Radiation Therapy • Whole Breast Radiation • All Breast Conservation • Locally Advanced Mastectomy • Nodal Disease • Close Margins • Inflammatory • Partial Breast Radiation • Selected Early Stage

Additional Therapy Systemic Therapy • Chemotherapy • Endocrine Therapy • Tamoxifen • Aromatase Inhibitors • Targeted Therapy Clinical Stage Biology of the Tumor Marker Profile Oncotype


Adjuvant Therapy Systemic Therapy • Endocrine Therapy (Anti Estrogen Therapy) • Any ER or PR + patient > 1% • Premenopausal/DCIS: Tamoxifen, Postmenopausal: Aromatase Inhibitors • Chemotherapy • ER/PR/Her 2 negative • Any Her 2 + • +/- ER/PR + Her 2 negative • Node + disease • Targeted Therapy: Herceptin • Her 2 +

Genomic Profiling of Tumors
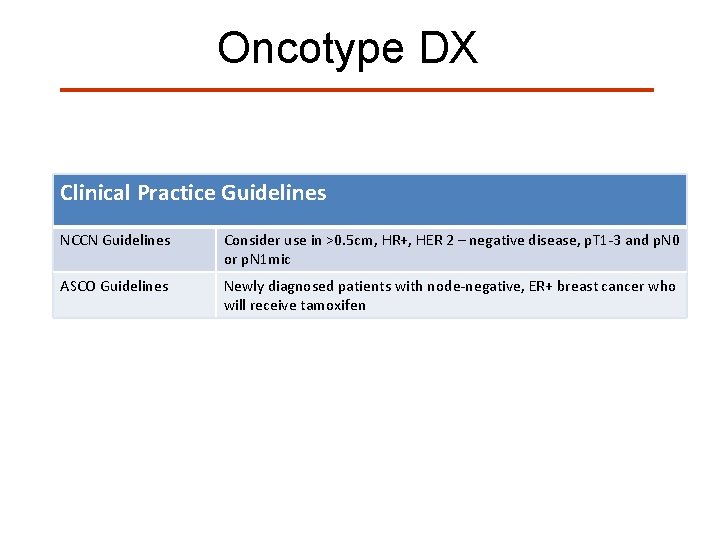
Oncotype DX Clinical Practice Guidelines NCCN Guidelines Consider use in >0. 5 cm, HR+, HER 2 – negative disease, p. T 1 -3 and p. N 0 or p. N 1 mic ASCO Guidelines Newly diagnosed patients with node-negative, ER+ breast cancer who will receive tamoxifen
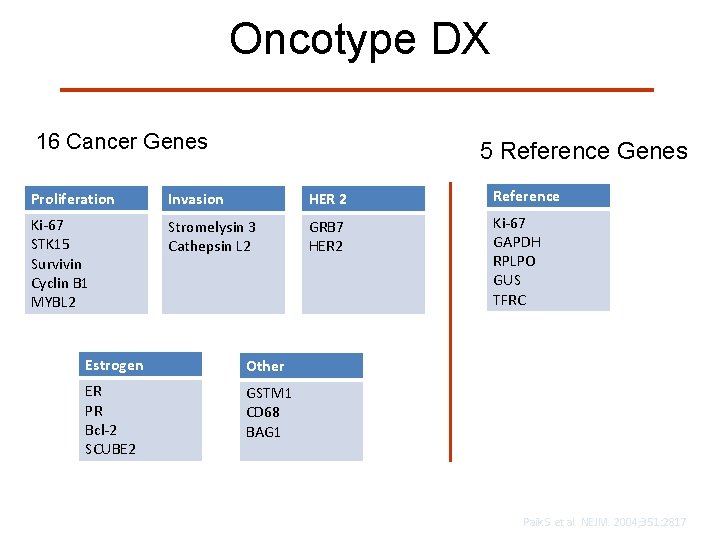
Oncotype DX 16 Cancer Genes 5 Reference Genes Proliferation Invasion HER 2 Reference Ki-67 STK 15 Survivin Cyclin B 1 MYBL 2 Stromelysin 3 Cathepsin L 2 GRB 7 HER 2 Ki-67 GAPDH RPLPO GUS TFRC Estrogen Other ER PR Bcl-2 SCUBE 2 GSTM 1 CD 68 BAG 1 Paik S et al. NEJM. 2004; 351: 2817
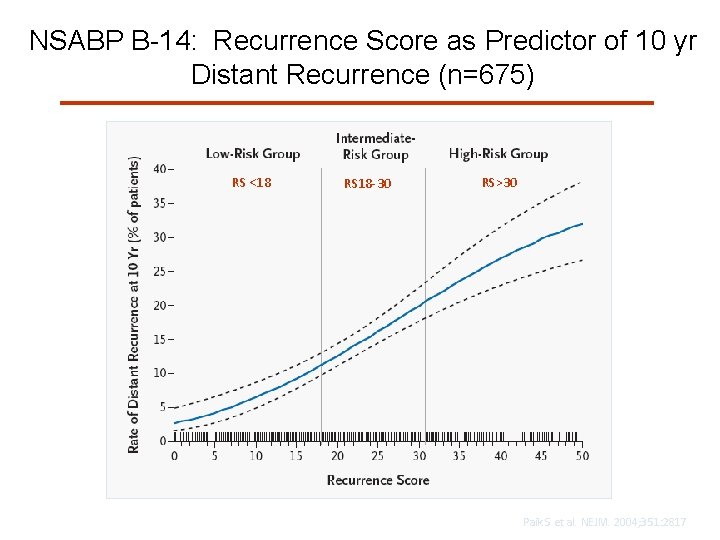
NSABP B-14: Recurrence Score as Predictor of 10 yr Distant Recurrence (n=675) RS <18 RS 18 -30 RS>30 Paik S et al. NEJM. 2004; 351: 2817
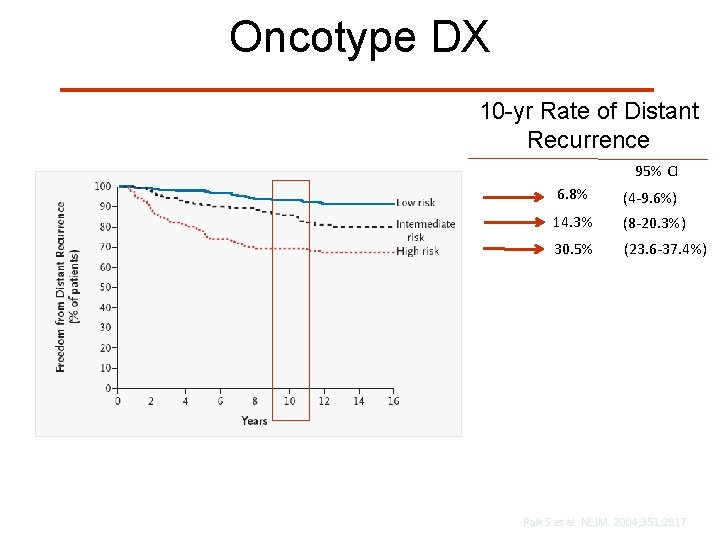
Oncotype DX 10 -yr Rate of Distant Recurrence 95% CI 6. 8% (4 -9. 6%) 14. 3% (8 -20. 3%) 30. 5% (23. 6 -37. 4%) Paik S et al. NEJM. 2004; 351: 2817
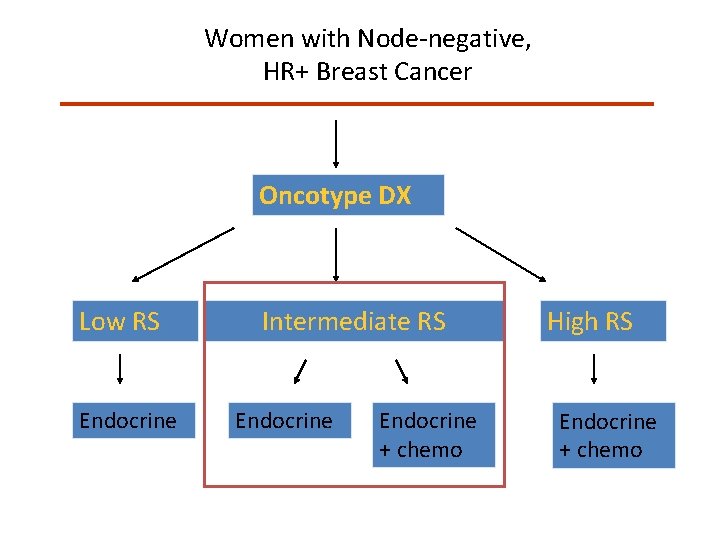
Women with Node-negative, HR+ Breast Cancer Oncotype DX Low RS Endocrine Intermediate RS Endocrine + chemo High RS Endocrine + chemo

Treatment Algorithm • Classic Treatment Design: – Surgery +/- Chemo +/- XRT +/- Endocrine • Neoadjuvant therapy: – Chemo Surgery +/- XRT +/- Endocrine • Inflammatory Breast Cancer: – Chemo +/- Surgery, XRT, Endocrine

Neoadjuvant Chemotherapy Surgical: • Treat locally advanced cancers • Convert mastectomy candidates into breast conservation candidates • Improve cosmesis in patients undergoing breast conservation Medical: • Use primary tumor and nodal response to tailor locoregional and systemic therapy • Identify better predictors of complete response
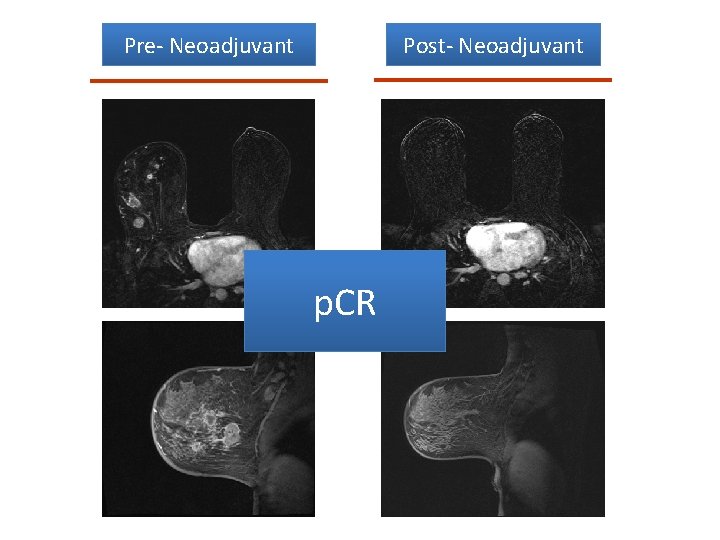
Post- Neoadjuvant Pre- Neoadjuvant p. CR
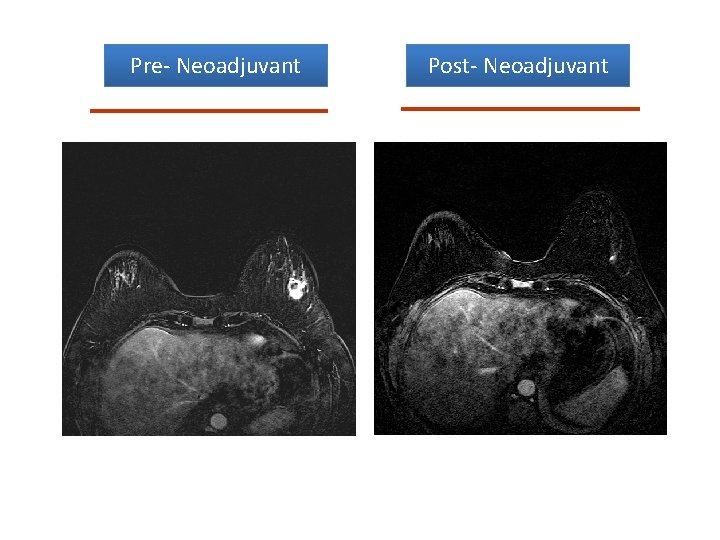
Pre- Neoadjuvant Post- Neoadjuvant

Loco-Regional Endpoints • In Breast p. CR: – 25 -30% w/ anthracyclines/taxanes – 40 -50% w/ chemo + trastuzamab in HER-2+ – 50 -60% w/ chemo + two anti-HER-2 agents • Axillary p. CR: – 30% w/ anthracyclines – Up to 40% w/ anthracyclines/taxanes – > 50% w/ chemo + anti-HER-2 therapies

True or False: 97% of the lymphatic drainage of the breast drains to the internal mammary lymph node basin.

True or False: Axillary Node Levels are based on the pectoralis major muscle

When performing a modified radical mastectomy, what levels of axillary nodes are removed? 1. Level I 2. Level II 3. Level III 4. All of the above 5. Only A & B

Which is the only screening modality that has shown to decrease mortality from breast cancer in woman over the age of 50? 1. Breast Ultrasound 2. Breast Mammography 3. Breast MRI 4. Breast Thermography
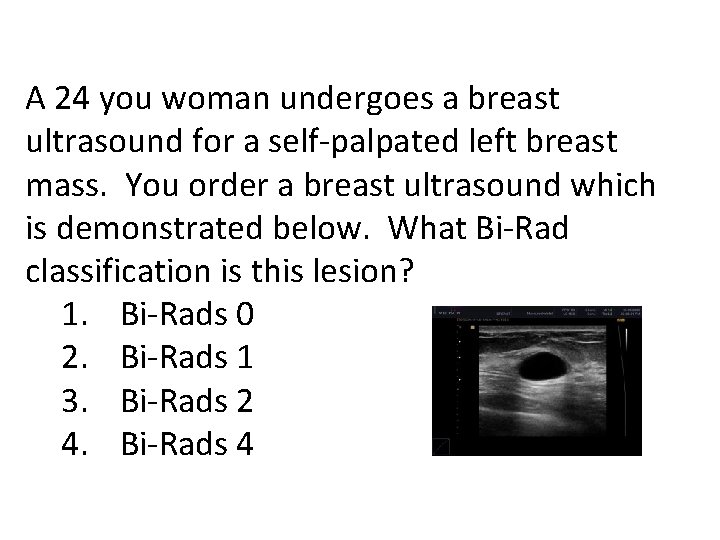
A 24 you woman undergoes a breast ultrasound for a self-palpated left breast mass. You order a breast ultrasound which is demonstrated below. What Bi-Rad classification is this lesion? 1. Bi-Rads 0 2. Bi-Rads 1 3. Bi-Rads 2 4. Bi-Rads 4
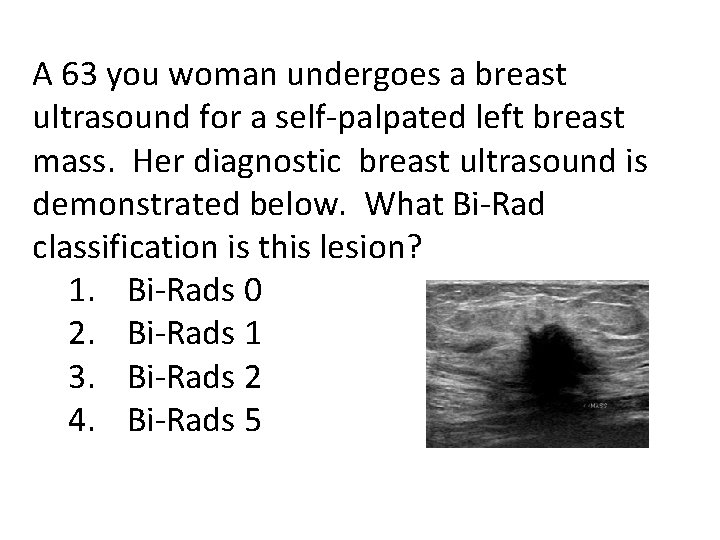
A 63 you woman undergoes a breast ultrasound for a self-palpated left breast mass. Her diagnostic breast ultrasound is demonstrated below. What Bi-Rad classification is this lesion? 1. Bi-Rads 0 2. Bi-Rads 1 3. Bi-Rads 2 4. Bi-Rads 5

Which Bi-Rads classification recommends 6 month short term follow up imaging? 1. Bi-Rads 0 2. Bi-Rads 2 3. Bi-Rads 3 4. Bi-Rads 4

True or False: Breast cancer affects 1 in 8 women in the United States.

Indications for genetic testing in a patient diagnosed with breast cancer are? 1. A woman diagnosed prior to the age of 45 2. A woman diagnosed at any age, who has two family members with breast, ovarian or pancreatic cancer 3. Any man diagnosed with breast cancer 4. All of the above

True or False: Survival is improved in patients undergoing mastectomy for a Stage II and Stage III breast cancer as compared to breast conservation surgery.

55 yo postmenopausal woman presents to you for a high risk evaluation. You perform quantitative risk assessment on her using the GAIL risk assessment model. Her 5 year risk is 4. 2% as compared to 1. 8% of the general population, and her lifetime risk is 42% as compared to 16% of the general population. Your talk to her about chemoprevention. Which medications would you use for chemoprevention? 1. Raloxifene 2. Tamoxifen 3. Exemestane 4. All of the above 5. 1 & 3

True or False: A 48 yo woman presents to your office for evaluation of newly diagnosed Triple negative inflammatory breast cancer. You explain that your treatment algorithm includes modified radical mastectomy followed by adjuvant chemotherapy and radiation therapy.
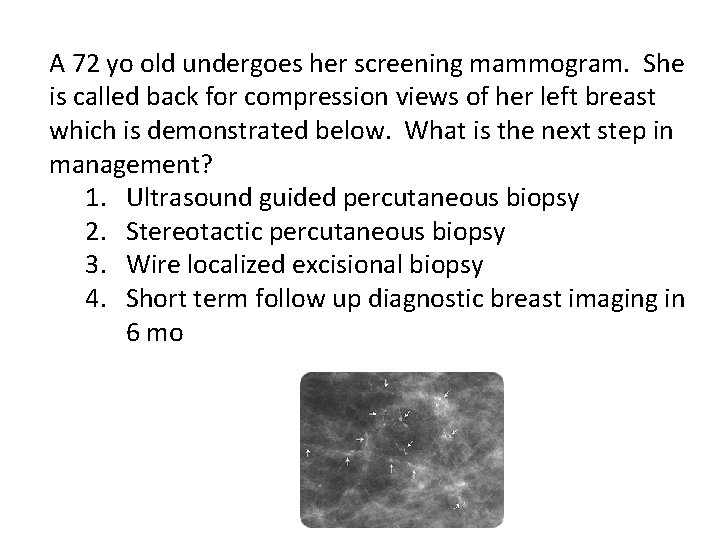
A 72 yo old undergoes her screening mammogram. She is called back for compression views of her left breast which is demonstrated below. What is the next step in management? 1. Ultrasound guided percutaneous biopsy 2. Stereotactic percutaneous biopsy 3. Wire localized excisional biopsy 4. Short term follow up diagnostic breast imaging in 6 mo

Your patient undergoes a stereotactic biopsy. Her pathology demonstrates grade 2 DCIS ER 0%, PR 24%. The area of calcifications spans 2 cm. What is not a treatment option for your patient? 1. Surgery 2. Tamoxifen 3. Radiation Therapy 4. Chemotherapy

True or False: Radiation therapy decreases risk of local recurrence by at least 50%.

True or False: Approximately 20% of all breast cancers are associated with genetic mutation.

True or False: Male breast cancer is higher in BRCA 1 gene mutation carriers.

A 62 yo woman is diagnosed with a new screen-detected left breast cancer. On clinical exam her tumor measures 3 cm in size. What is her T stage? 1. 2. 3. 4. 5. Tis T 1 T 2 T 3 T 4
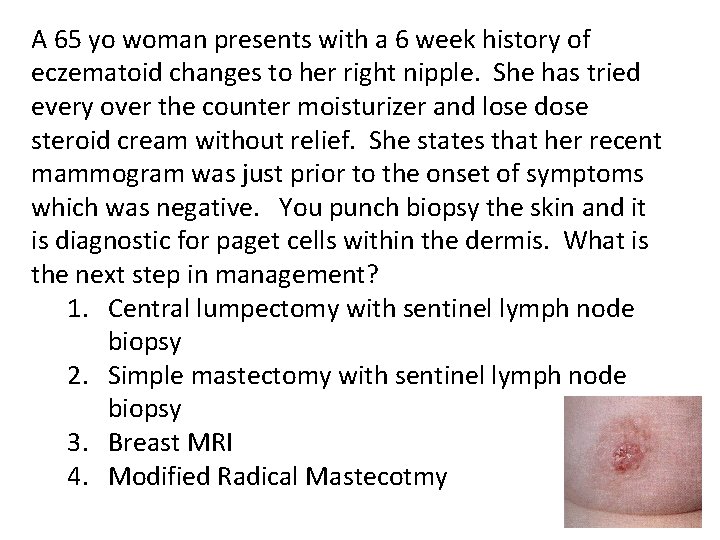
A 65 yo woman presents with a 6 week history of eczematoid changes to her right nipple. She has tried every over the counter moisturizer and lose dose steroid cream without relief. She states that her recent mammogram was just prior to the onset of symptoms which was negative. You punch biopsy the skin and it is diagnostic for paget cells within the dermis. What is the next step in management? 1. Central lumpectomy with sentinel lymph node biopsy 2. Simple mastectomy with sentinel lymph node biopsy 3. Breast MRI 4. Modified Radical Mastecotmy
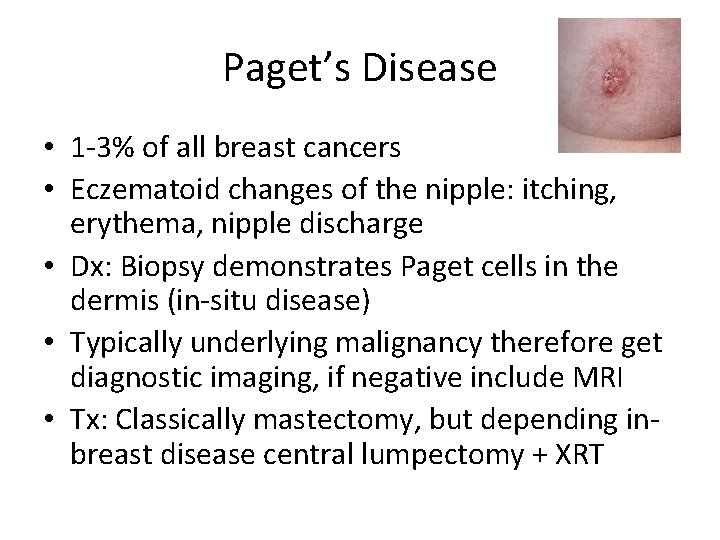
Paget’s Disease • 1 -3% of all breast cancers • Eczematoid changes of the nipple: itching, erythema, nipple discharge • Dx: Biopsy demonstrates Paget cells in the dermis (in-situ disease) • Typically underlying malignancy therefore get diagnostic imaging, if negative include MRI • Tx: Classically mastectomy, but depending inbreast disease central lumpectomy + XRT

A 57 yo woman presents to your office with complaints of a 1 month history of breast erythema, induration, and edema. She was prescribed antibiotic therapy by her PCP which did not help with her symptoms. Due to persistence in symptoms, her PCP referred her to you for evaluation. What is pathognomonic for her disease process? 1. 2. 3. 4. Dermal lymphatic invasion Pagetoid cells within the dermis Lymphovascular invasion All of the above

What is the mainstay of treatment for the above patient? 1. 2. 3. 4. Modified Radical mastectomy Chemotherapy Radiation therapy Central lumpectomy

A 62 you woman is recently diagnosed with a screen-detected right breast invasive ductal carcinoma. She undergoes wire localized segmental mastectomy with sentinel lymph node biopsy. Her final pathology demonstrates a 2 cm invasive ductal carcinoma, ER/PR positive, Her 2 neu negative with clear margins and negative lymph nodes. What adjuvant therapy does she need? 1. Chemotherapy because her tumor is > 1 cm in size plus radiation therapy and an aromatase inhibitor 2. No chemotherapy because her lymph nodes were negative, therefore only radiation therapy and an aromatase inhibitor 3. Send an Oncotype score to determine need for chemotherapy, then proceed with radiation therapy followed by an aromatase inhibitor 4. Only Tamoxifen
What if the above patient’s Oncotype returned as 12? 1. No chemotherapy, but radiation therapy followed by an aromatase inhibitor 2. Chemotherapy followed by radiation therapy and an aromastase inhibitor 3. Radiation therapy alone 4. None of the above

True or False: All woman undergoing breast conservation therapy who have a positive sentinel lymph node require completion axillary dissection.

Benign Breast Disease

Fibrocystic Changes • Generic term used to describe symptoms related to the aberration of normal development and involution of the breast • Encompasses: – Cyclical Change – Cyst formation – Fibroadenoma formation – Duct ectasia – Sclerosing Adenosis • Benign Nodular breast tissue
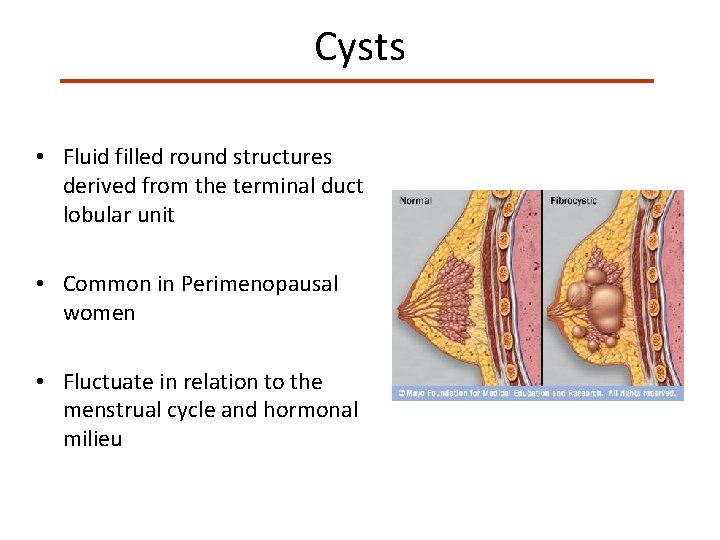
Cysts • Fluid filled round structures derived from the terminal duct lobular unit • Common in Perimenopausal women • Fluctuate in relation to the menstrual cycle and hormonal milieu
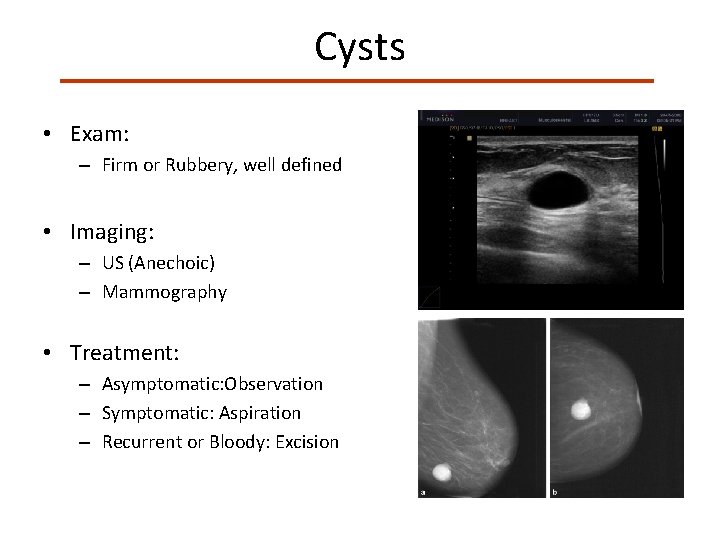
Cysts • Exam: – Firm or Rubbery, well defined • Imaging: – US (Anechoic) – Mammography • Treatment: – Asymptomatic: Observation – Symptomatic: Aspiration – Recurrent or Bloody: Excision

A 21 yo old woman presents for evaluation of a selfpalpated right breast lump. You order an ultrasound which is demonstrated below. What is the next step in management? 1. Reassure her that it is benign and tell her to follow as needed 2. Reassure her that it is benign and have her follow up in 6 months with repeat ultrasound 3. Explain that it is likely benign however recommend surgical excisional biopsy 4. Explain that you are concerned that it is malignant and move forward with an ultrasound guided biopsy

Fibroadenomas • Fibroepithelial Lesion • Solid round structures arise from the epithelium of the terminal duct lobular unit • Most common breast mass in adolescent women • Occur from teens through 70 s
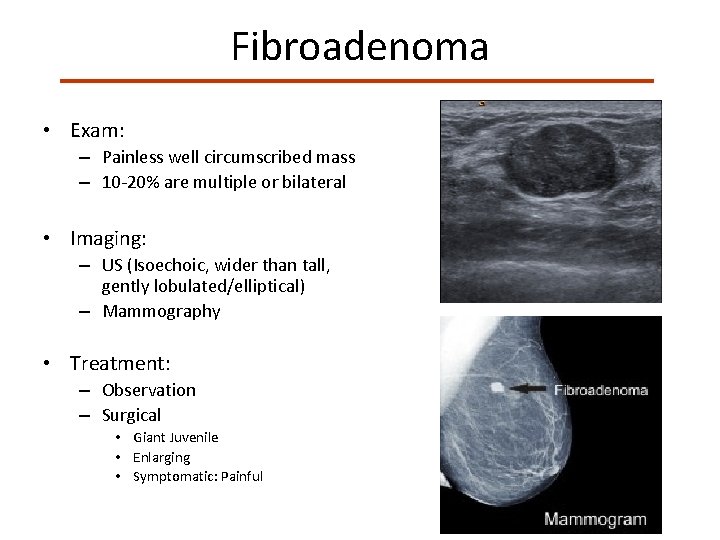
Fibroadenoma • Exam: – Painless well circumscribed mass – 10 -20% are multiple or bilateral • Imaging: – US (Isoechoic, wider than tall, gently lobulated/elliptical) – Mammography • Treatment: – Observation – Surgical • Giant Juvenile • Enlarging • Symptomatic: Painful
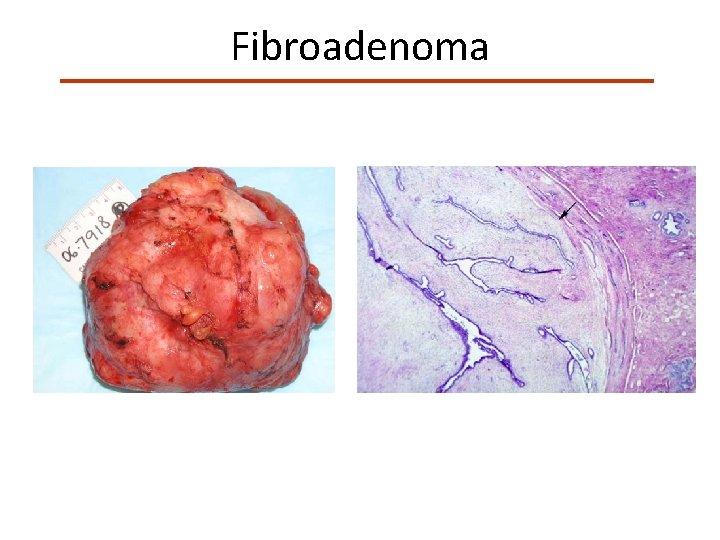
Fibroadenoma
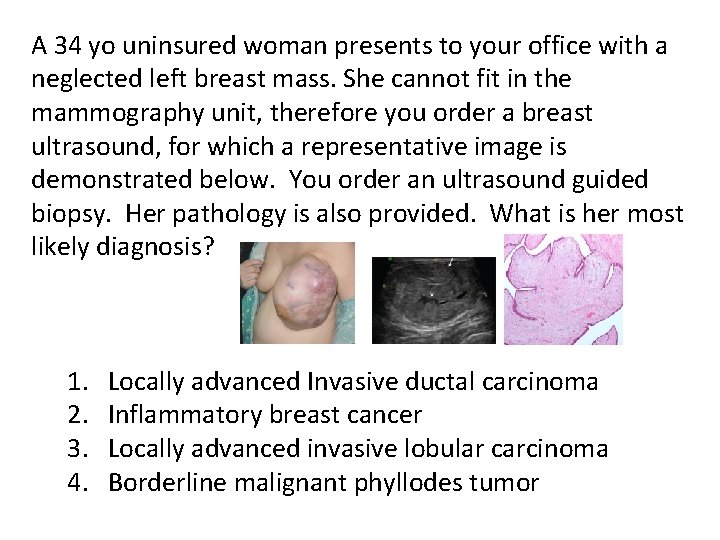
A 34 yo uninsured woman presents to your office with a neglected left breast mass. She cannot fit in the mammography unit, therefore you order a breast ultrasound, for which a representative image is demonstrated below. You order an ultrasound guided biopsy. Her pathology is also provided. What is her most likely diagnosis? 1. 2. 3. 4. Locally advanced Invasive ductal carcinoma Inflammatory breast cancer Locally advanced invasive lobular carcinoma Borderline malignant phyllodes tumor

Phyllodes Tumor • Fibroepithelial Lesion • <1% of all breast tumors • Occurs in wide range of ages: 10 -80 • Wide range of biological behavior – Benign • – <2, no atypia, no stromal overgrowth, well-circumscribed – Borderline • – 2 -10, mild atypia, no stromal overgrowth, infiltrative margins – Malignant • – >10, marked atypia, presence of stromal overgrowth, infiltrative margins
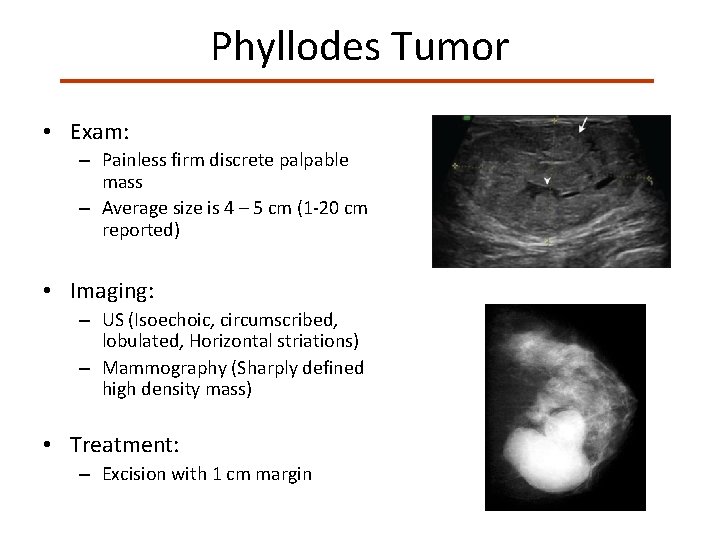
Phyllodes Tumor • Exam: – Painless firm discrete palpable mass – Average size is 4 – 5 cm (1 -20 cm reported) • Imaging: – US (Isoechoic, circumscribed, lobulated, Horizontal striations) – Mammography (Sharply defined high density mass) • Treatment: – Excision with 1 cm margin
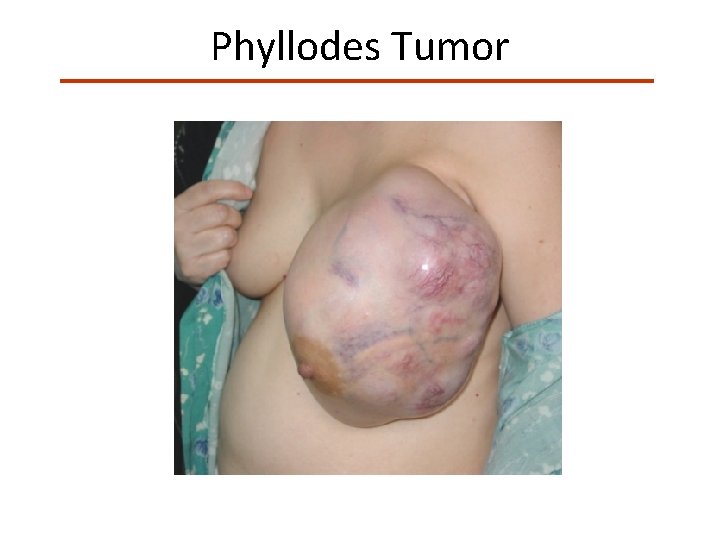
Phyllodes Tumor
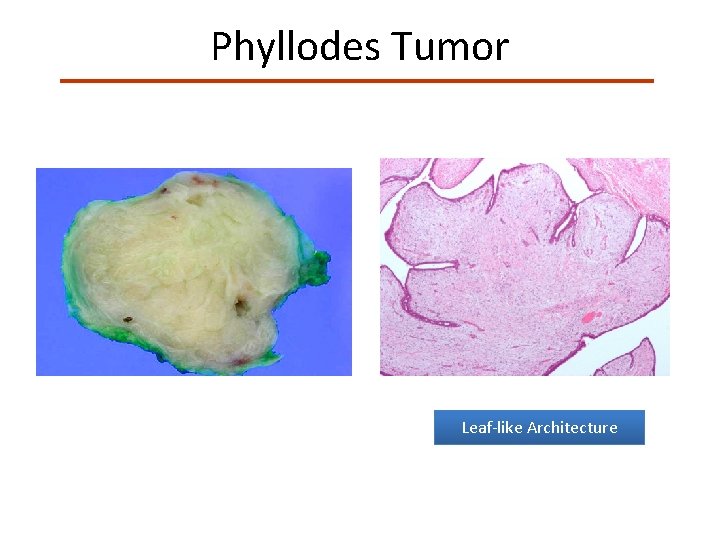
Phyllodes Tumor Leaf-like Architecture
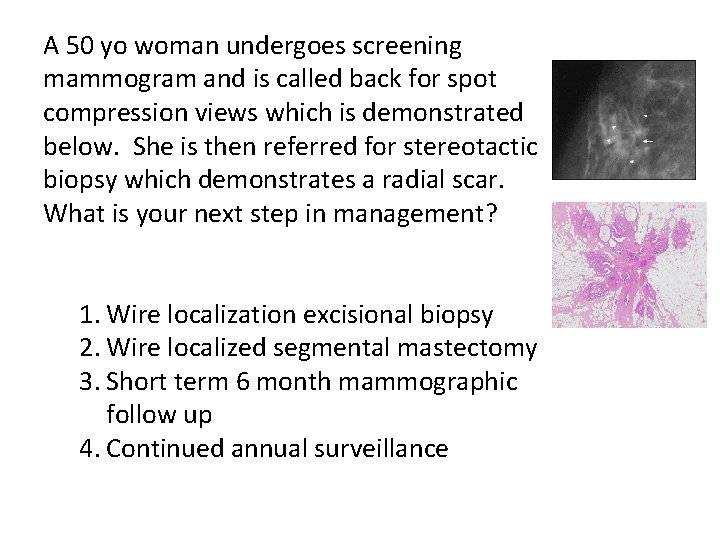
A 50 yo woman undergoes screening mammogram and is called back for spot compression views which is demonstrated below. She is then referred for stereotactic biopsy which demonstrates a radial scar. What is your next step in management? 1. Wire localization excisional biopsy 2. Wire localized segmental mastectomy 3. Short term 6 month mammographic follow up 4. Continued annual surveillance
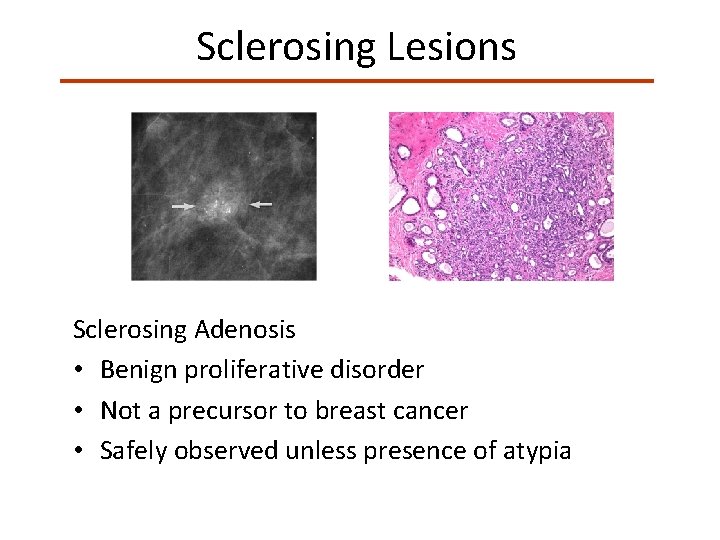
Sclerosing Lesions Sclerosing Adenosis • Benign proliferative disorder • Not a precursor to breast cancer • Safely observed unless presence of atypia
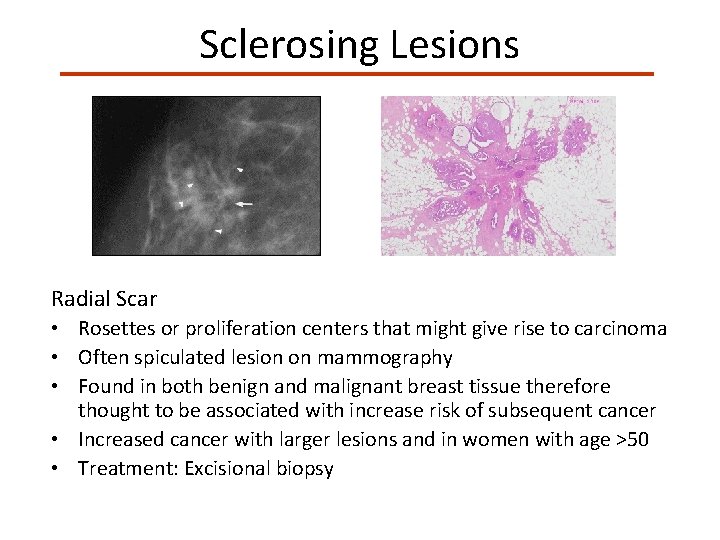
Sclerosing Lesions Radial Scar • Rosettes or proliferation centers that might give rise to carcinoma • Often spiculated lesion on mammography • Found in both benign and malignant breast tissue therefore thought to be associated with increase risk of subsequent cancer • Increased cancer with larger lesions and in women with age >50 • Treatment: Excisional biopsy

Mastalgia • Common complaint • Typically no histologic difference in women with or without mastalgia • Treatment is reassurance – rule out malignancy if age appropriate • Evening primrose oil, and vitamin E have been studied in randomized controlled trials

The most common cause of bloody nipple discharge is? 1. Duct ectasia 2. Intraductal papilloma 3. DCIS 4. Invasive ductal carcinoma
A 45 yo woman presents for evaluation of bloody nipple discharge. She states that it is unilateral, single duct, and spontaneous. She underwent diagnostic mammogram last week which was normal. What is your next step in management? 1. Repeat mammogram 2. Breast MRI 3. Retroareolar ultrasound 4. Ductogram 5. 3&4

Your previous patient undergoes an ultrasound and ductogram which is demonstrated below. What is your diagnosis? 1. 2. 3. 4. Ductal carcinoma in situ Invasive ductal carcinoma Duct ectasia Intraductal papilloma

Nipple Discharge • Accounts for 3 -8% of all breast clinic referrals • Typically associated with a benign cause – 2/3 rd of non-lactating women have a small amount of fluid on manual expression • Risk of cancer increases with age: – < 40 – 3% – 40 -60 – 1% – > 60 – 32% • Divided into Surgical and Non surgical nipple discharge – Surgical: Papillomas, DCIS, Cancer – Nonsurgical: Physiologic, endocrine, pharmacologic, idiopathic
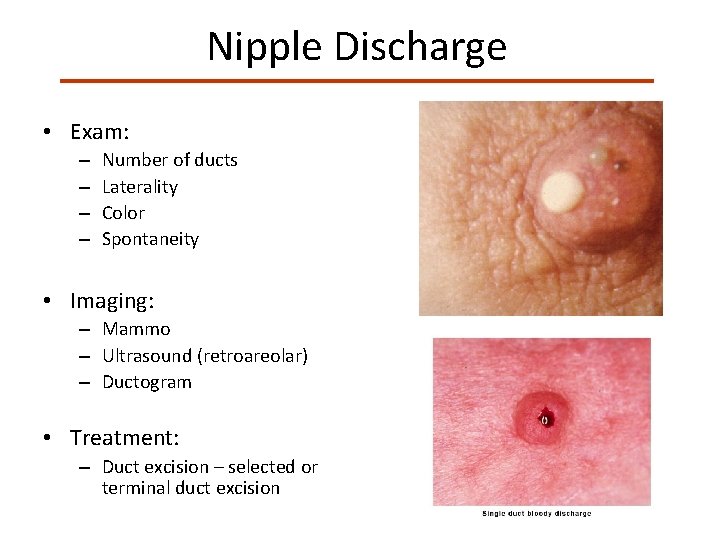
Nipple Discharge • Exam: – – Number of ducts Laterality Color Spontaneity • Imaging: – Mammo – Ultrasound (retroareolar) – Ductogram • Treatment: – Duct excision – selected or terminal duct excision
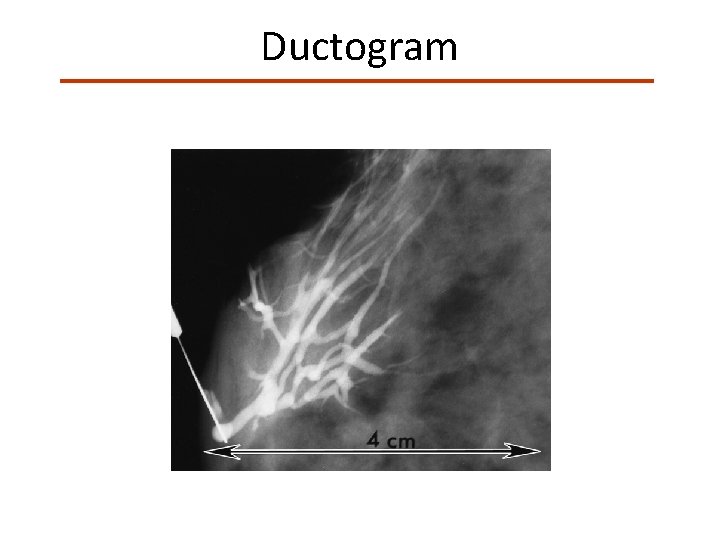
Ductogram

Duct Ectasia • Dilation of the subareolar duct in peri and post-menopausal women • Typically asymptomatic • May present with cheesy, viscous, toothpaste like discharge or have nipple retraction • Observation, unless discharge is persistent or repeated bouts of periductal mastitis/abscess
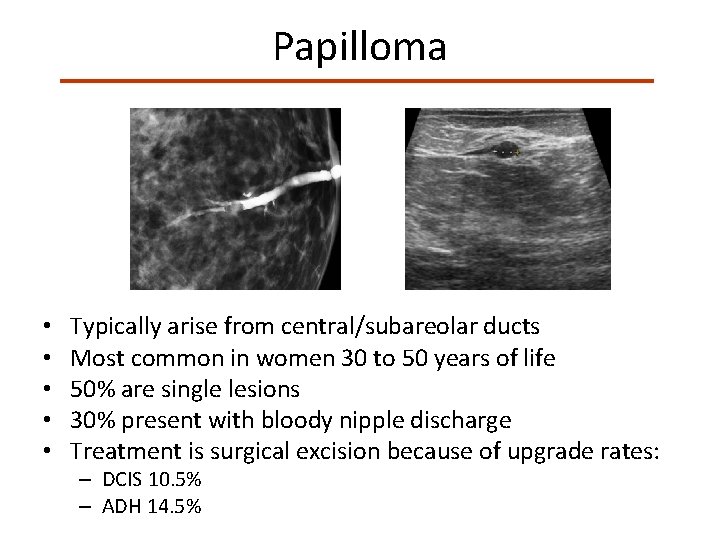
Papilloma • • • Typically arise from central/subareolar ducts Most common in women 30 to 50 years of life 50% are single lesions 30% present with bloody nipple discharge Treatment is surgical excision because of upgrade rates: – DCIS 10. 5% – ADH 14. 5%
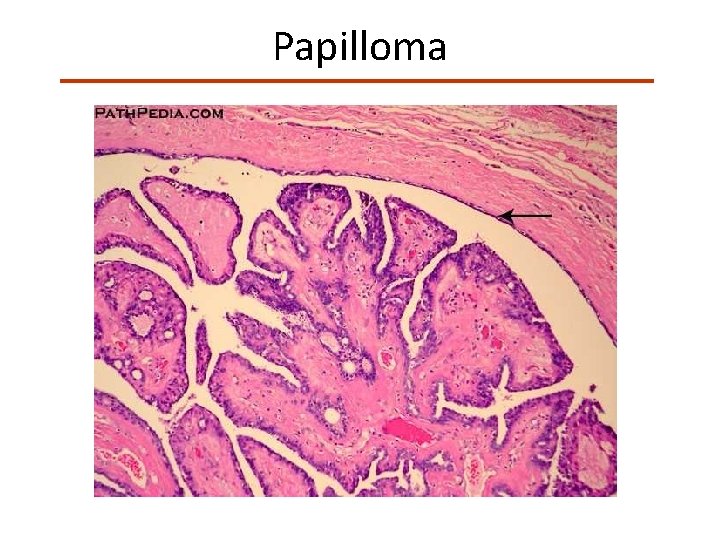
Papilloma
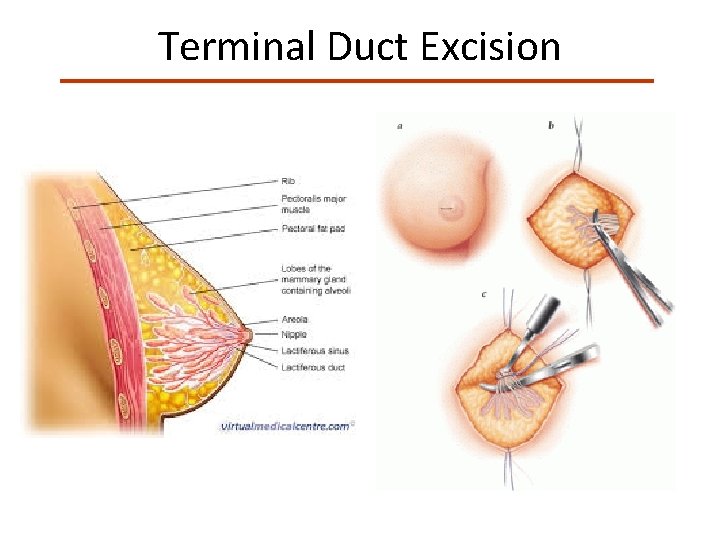
Terminal Duct Excision
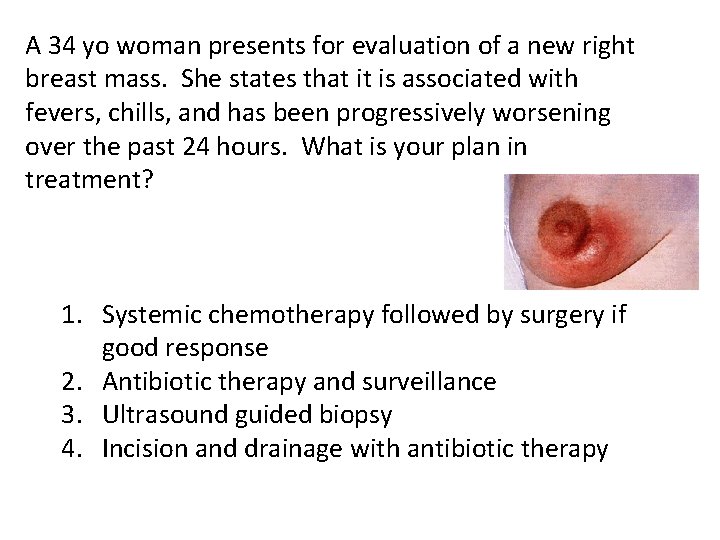
A 34 yo woman presents for evaluation of a new right breast mass. She states that it is associated with fevers, chills, and has been progressively worsening over the past 24 hours. What is your plan in treatment? 1. Systemic chemotherapy followed by surgery if good response 2. Antibiotic therapy and surveillance 3. Ultrasound guided biopsy 4. Incision and drainage with antibiotic therapy
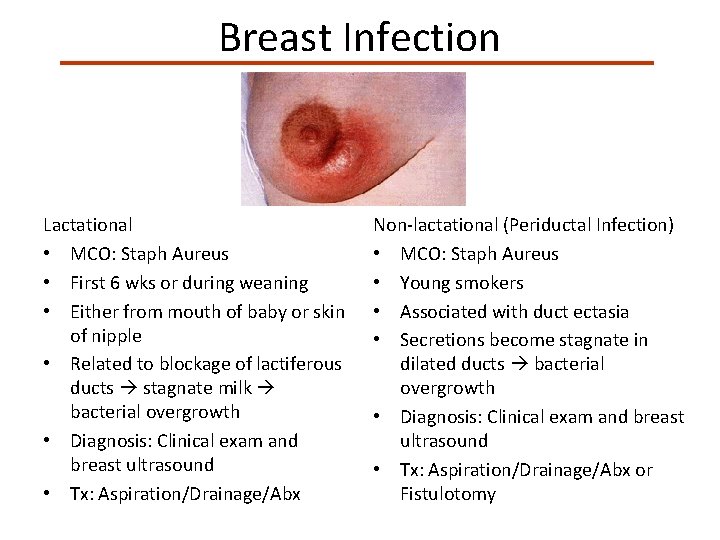
Breast Infection Lactational • MCO: Staph Aureus • First 6 wks or during weaning • Either from mouth of baby or skin of nipple • Related to blockage of lactiferous ducts stagnate milk bacterial overgrowth • Diagnosis: Clinical exam and breast ultrasound • Tx: Aspiration/Drainage/Abx Non-lactational (Periductal Infection) • MCO: Staph Aureus • Young smokers • Associated with duct ectasia • Secretions become stagnate in dilated ducts bacterial overgrowth • Diagnosis: Clinical exam and breast ultrasound • Tx: Aspiration/Drainage/Abx or Fistulotomy

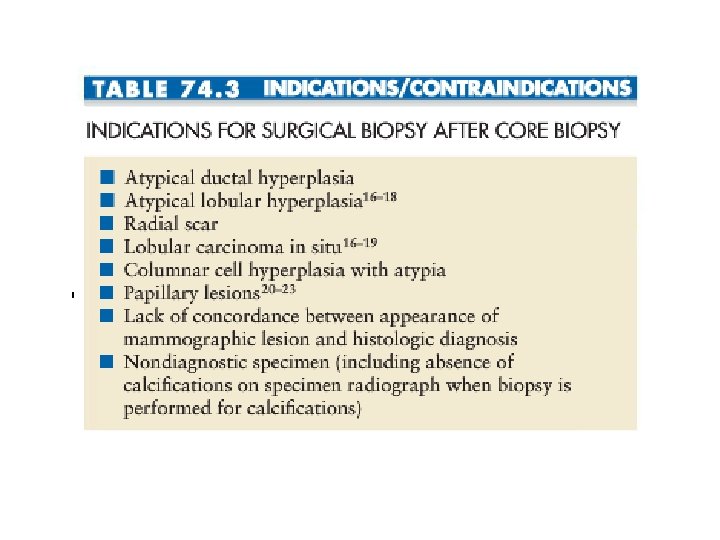
Which of the below is not an indication for surgical excision? 1. 2. 3. 4. Atypical ductal hyperplasia Radial scar Flat epithelial atypia Discordance between pathology and radiographic imaging 5. Pseudoangiomatous Stromal Hyperplasia 6. All of the above are indications for excision

Pseudoangiomatous Stromal Hyperplasia (PASH) • Myofibroblasts that proliferate in response to hormonal stimuli • Affects women from teens to 50 s • Presents as discrete painless mass • Imaging: focal asymmetry or well circumscribed mass • Treatment: Observation (some studies suggest excision) • Increase risk of recurrence up to 22%

Fibromatosis • Desmoid tumor of the breast • Affects women from teens to 80 s • Typically presents as firm unilateral painless mass • Microscopically the tumor is composed of spindle cells • Margins are infiltrative and typically invade around normal structures • Proper treatment is wide local excision • The role of adjuvant radiation and chemo is investigational
- Slides: 119