PG Assembly PAEDIATRIC ANAESTHESIA Case discussion Dr Latha

PG Assembly – PAEDIATRIC ANAESTHESIA Case discussion Dr. Latha, Chennai Dr. Shanthi Paulraj, Tanjore Paediatric anaesthesia case discussion 3 month old infant with Pierre Robin Syndrome for cleft lip repair.

What are the components of Pierre Robin Syndrome (PR)?

a)Micrognathia b)Glossoptosis c) Respiratory distress in the first 24 to 48 hours

What are the other syndromes associated with cleft lip?

Syndromes associated with cleft lip are Treacher Collins syndrome Goldenhar’s syndrome Down syndrome Klippel Feil syndrome
What is the position of larynx in an infant?

At the level of C 3 to C 4

At what age does the primary lip repair done?

At the age of 3 months

How will you evaluate for difficult airway in infants?

a)H/o respiratory obstruction like noisy breathing, stridor. b) Physical examination – cranio facial deformities i) Size of mouth and tongue, ii) Size and configuration of mandible iii) Size and configuration of palate iv) Asymmetry of face v) Other cranial facial deformities

What are the challenges in anesthetizing a child with Pierre Robin Syndrome?

i. Difficult airway due to Micrognathia and Glossoptosis ii. Awake intubation technique cannot be done in paediatric age group iii. FOB guided intubation in infant needs highest experience and expertise iv. Airway obstruction during induction and post op make cause severe hypoxemia.

What are the most important monitors you will use in this case ?

1. Sp. O 2 2. Precordial stethoscope 3. ECG 4. Temperature

What are the goals in anesthetizing this child with PR syndrome?

Maintain spontaneous ventilation till airway secured Avoid airway obstruction and hypoxia

What is the position of larynx in an infant?

Position of larynx in infant is C 3 to C 4

Why is the infant more prone for airway obstruction?

Short neck and chin that meets the chest at the level of 2 nd rib

How will you assess the blood loss ? What is the fluid of choice ? When will you replace blood ?

What is Kilners rule of 10?
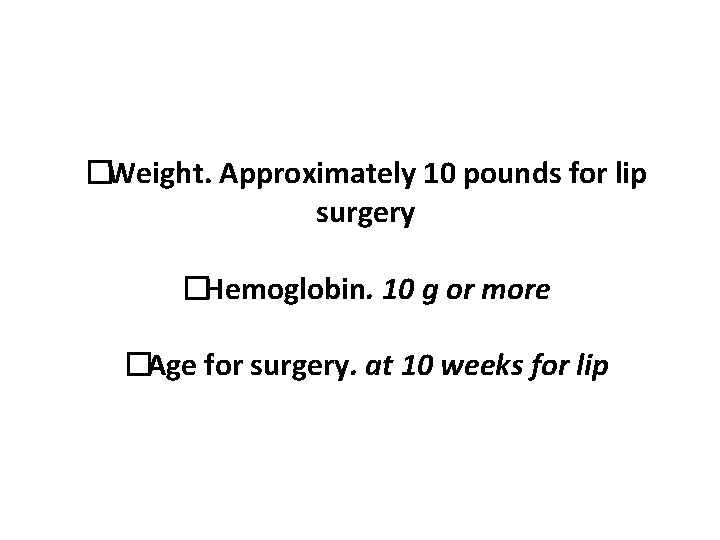
�Weight. Approximately 10 pounds for lip surgery �Hemoglobin. 10 g or more �Age for surgery. at 10 weeks for lip

Will you premedicate the infant?

No need for any sedative premedication in infants

How will you induce the child with PR syndrome?

By inhalational induction

Why are the paediatric age groups more prone for hypoxia ?

What type of ETT will you use in this case?

Ring-Adair-Elwyn (RAE) or flexo metallic tube

What difficulty will you experience in a child with Micrognathia?

Difficult Laryngoscopy in infants below 6 months due to proximity of tongue to superior larynx causing acute angle between the tongue and glottis (90°)

What is Glossoptosis and its anaesthetic significance?

Glossoptosis is a condition in which base of tongue is positioned more caudally. Anaesthetic significance is difficult visualization of glottis

Which laryngoscopic blade will you use in this case? Why?

Miller (straight) blade. i. Allows cephalad aspect of larynx to be exposed more easily, ii. Base of tongue lifted out of line of sight and iii. Protruding epiglottis lifted with tip.

What are the techniques used to visualize the glottis in this case?

Optimal External laryngeal manipulation (OLEM) and Tongue suturing to mandible in post natal period

What are the options available for difficult intubation in this case?

Options available are i. Inhalational induction followed by intubation, ii. Intubation guides – metal stylets and gum elastic boogie iii. Oxyscope iv. Paediatric FOB (ultrathin) guided intubation, v. LMA as a conduit for FOB intubation.

What are the available techniques for inhalation induction?

Three techniques with sevoflurane induction i. Incremental increase in sevoflurane (2%, 4 %, 6%, 8%) ii. High concentration of sevoflurane (8%) in O 2, and iii. High concentration of sevoflurane in the 1: 1 mixture of N 2 O and O 2

What are the possible complications during inhalation induction?

i. Due to abnormal facial anatomy improper mask fit can occur ii. Breath holding iii. Airway obstruction iv. Laryngospasm.

How will you overcome airway obstruction during induction?

i. Insertion of appropriate size oropharyngeal and nasopharyngeal airway at adequate plane of anaesthesia ii. CPAP of 5 to 10 cm. H 2 O to keep airway patent.

What are the techniques that can be used with straight blade in an infant with difficult airway?

i. Retromolar approach, ii. Paraglossal approach and iii. Lateral approach

What are the extubation criteria in this case?

The child is extubated i. Fully awake, ii. Warm iii. Able to maintain airway with intact protective reflexes.

What are the options available for postop pain relief?

i. Infra orbital nerve block, ii. External nasal block, iii. Rectal paracetomol

What is the most important post-op complication you expect in this case?

i. Airway obstruction ii. Post intubation croup.

What is the difference between adult and paediatric difficult airway management ?
- Slides: 56