PFAPA SYNDROME Cormac J OConnor MD LT MC





















- Slides: 22

PFAPA SYNDROME Cormac J. O’Connor MD, LT, MC, USN Naval Hospital Camp Pendleton, CA

Introduction • Fever is the presenting complaint in 30 -50% of pediatric acute visits • Most “recurrent fevers” are actually superimposed viral infections

Introduction • In periodic fever cases in the U. S. , PFAPA is the most common cause

PFAPA • • • Periodic Fever Aphthous ulcers Pharyngitis Adenopathy

Key Points • PFAPA – Fevers are brief (<5 d), unheralded periodic fevers with “APA” symptoms and no other focus of disease – Wellness between fevers with normal growth, development and activity

Key Points • Patients with PFAPA are completely well • Have fewer viral URI’s than their siblings

Case Presentation • 2 ½-year-old boy in ER for 2 days of fever to 101 F and neck tenderness, without URI symptoms • Exam, CBC and UA were normal, d/c home with “febrile illness” • Symptoms resolved fully in 3 -4 days

Case Presentation • Symptoms recurred every 4 weeks for the next 18 months • Review of medical, family, social, travel, and exposure histories was unremarkable • Multiple ER visits resulted in febrile illness or URI diagnoses

Case Presentation • Most impressive was the speed of clinical change • Oral ulcers noted with fever • Referred to NMCSD pediatric infectious disease department

Case Presentation • Febrile episodes recurred every four weeks from 2 ½ - 4 years old • He is nearly 6 years old and in full health without sequelae

Discussion • Medline and Google searches using the keywords Recurrent, Pediatric and Fever identified in the literature similarities between this case and the PFAPA syndrome

Discussion • Identified in 1987 by Marshall, et al – aka Marshall’s syndrome, then later PFAPA syndrome • Etiology – Infectious vs. Autoimmune unclear • Incidence – Far greater than other recurrent fevers (Cyclic neutropenia, FMF, HIDS, etc. )

Discussion • Onset typically 2 -5 yo • Usually resolves by 8 yo • Male > female • No known ethnic predilection

Discussion Periodic Fever – usually 3 -5 days – repeats every 3 -4 weeks • Aphthous ulcers – small, shallow, and resolve rapidly • Pharyngitis – with or without exudate • Adenopathy – cervical – usually bilateral and short-lived • No skin, respiratory, gastrointestinal, or joint involvement

Diagnostic Criteria • Periodic fevers onset < 5 yo • Absence of URI sx including >1 of: – apthous stomatitis – cervical lymphadenitis – pharyngitis • Exclude cyclic neutropenia • Normal, asymptomatic intervals

Why isn’t it Cyclic Neutropenia? • PFAPA – Onset ~ 2 -5 yo – Fever 3 -5 d q 4 weeks, no neutropenia – Well intervals • Cyclic neutropenia – Onset usually during infancy – Fever 5 -7 d, q 21 d, with ANC <200/mm 3 – Associated infections

Treatment • Prednisone – 2 mg/kg/d x 1 -2 doses • Tonsillectomy • Cimetidine – 150 mg/d

When to Suspect and What to Do? • In typical presentations – No concern for other dx • After 3 -4 febrile episodes • One expert recommends only CBC, throat Cx, ESR, & ASO titer

Differential Diagnoses • Periodic Fever Syndromes – PFAPA – Cyclic Neutropenia • Recurrent, non-periodic, fever syndromes – recurrent tonsillitis, EBV, HBV, FMF, HIDS, TRAPS, JRA

Conclusion • PFAPA is the #1 cause of periodic fever in the U. S. A. • Punctual periodic fevers, with aphthous ulcers, pharyngitis, and cervical adenopathy • Completely well intervals

Questions?

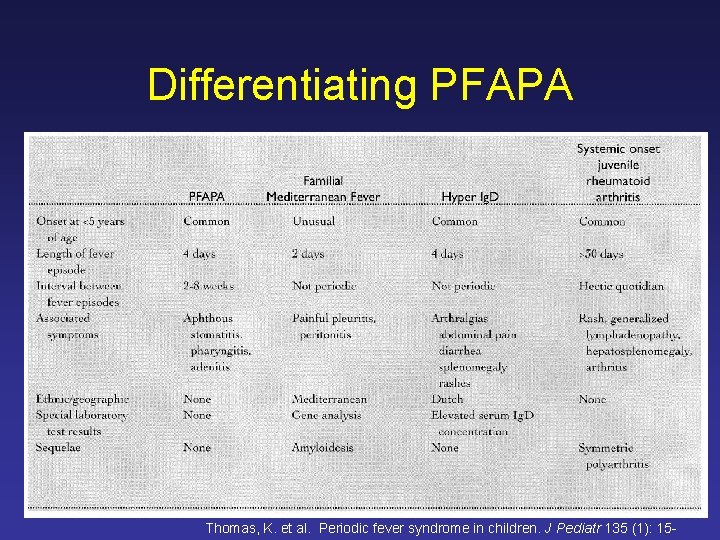
Differentiating PFAPA Thomas, K. et al. Periodic fever syndrome in children. J Pediatr 135 (1): 15 -