Pessaries the basics Lieschen H Quiroz MD Female

Pessaries: the basics Lieschen H. Quiroz, MD Female Pelvic Medicine & Reconstructive Surgery Department of OB/GYN University of Oklahoma Health Sciences Center 1

Objective • • • To learn of surgical and nonsurgical options for management of prolapse To learn the basics of pessary fitting To learn about risks and benefits of pessaries 2

Introduction 24% of U. S. women are affected with one or more pelvic floor disorders. l 40% of women from 60 -79 years of age, and about 50 % of women 80 and older. l Study: 11% of women had surgery for prolapse or urinary incontinence during their lifetime and 30% of those who had surgery had at least 2 procedures to correct them. l Nygaard, I; JAMA 2008 ; Luber KM et al Am J Obstet Gynecol 2001; Olsen AL et al Obstet Gynecol 1997 3
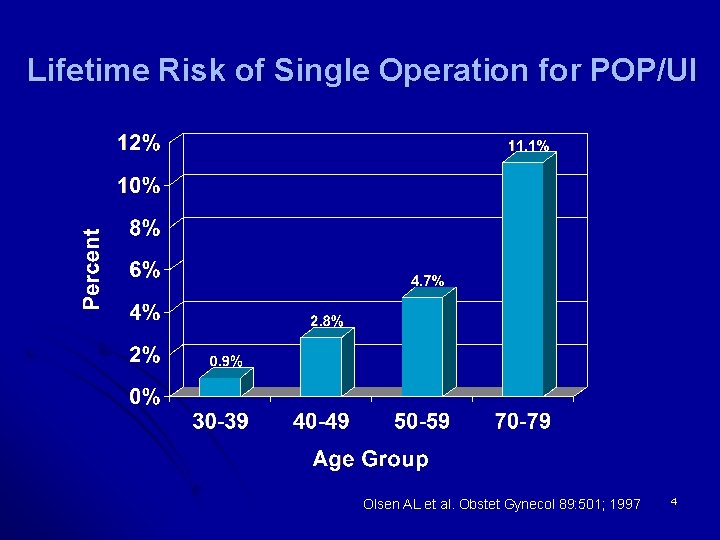
Lifetime Risk of Single Operation for POP/UI Olsen AL et al. Obstet Gynecol 89: 501; 1997 4

Pelvic Floor Disorders Urinary incontinence l Pelvic organ prolapse l Fecal incontinence l Other sensory and emptying abnormalities of the lower urinary tract and lower gastrointestinal tract l 5

Pelvic organ prolapse 6

Definition: Pelvic organ prolapse l l Pelvic organ prolapse- herniation of pelvic organs toward or through the vaginal opening Described in 3 compartments: l l Anterior wall (bladder or cystocele) Posterior wall (rectum or rectocele) Apex (enterocele) Standardized measurement is the POP-Q scale 7

Epidemiology ICS defines prolapse at stage >0. l Prolapse above or to the hymen typically is not symptomatic and does not require treatment if not bothersome l Approx. 200, 000 surgeries a year, costing >1 billion dollars annually l Bradley C. S. , et al. Vaginal wall descensus and pelvic floor symptoms in older women. Obstet Gynecol 106. (4): 759 -766. 2005 Boyles S. H. , et al. Procedures for pelvic organ prolapse and urinary incontinence. Obstet Gynecol 1979– 1997. Am J Obstet Gynecol 188. 108 -115. 2003 8

Risk factors l Most established: l vaginal childbirth l OFP-Vaginal parity of 2, RR 8. 4 of developing pop l WHI- Every additional VD conferred increased risk of prolapse by 10 -20% l advanding age-population study l Among 1000, every additional 10 years of age conferred an increase risk of pop of 40% l Obesity 9

Diagnosis l Symptoms l Women typically present with complaints of “feeling a bulge” or “something falling out” of the vagina. l May be associated with bladder or bowel complaints l Obstructed voiding l Splinting l Urinary or defecatory urgency, frequency, constipation, urinary/anal incontinence 10

Treatment and Prevention l Prevention not clearly defined l l C-S Obesity Pelvic Floor PT Observation l l l Viable option in asymptomatic patients Patients with Stage 3 or 4 disease may need evaluation on a regular basis Obstructed defecation or voiding with hydronephrosis from chronic ureteral kinking is an indication for treatment regardless of symptoms 11
Pessary l l Pelvic Organ Prolapse described 1550 BC Egypt Hippocrates described treatment for prolapse; succussion and pomegranate treatment l various other objects described l Egg therapy l Current pessaries- silicone 12

Nonsurgical treatment: Pessary l l l Silicone device that support the pelvic organs when inserted in the vagina Up to 1/3 of women who have had surgical repair for POP will have a subsequent procedure, pessaries offer a viable treatment option Approximately 80% of women who desire a trial of pessary are effectively treated. Of those fitted, approx. 50% continue using it at 1 year. Cundiff G. W. et al: The PESSRI study: symptom relief outcomes of a randomized crossover trial of the ring and Gellhorn pessaries. Am J Obstet Gynecol 196. (4): 7884. 2007; e 1– 8 13

The Use and Care of Pessaries 14
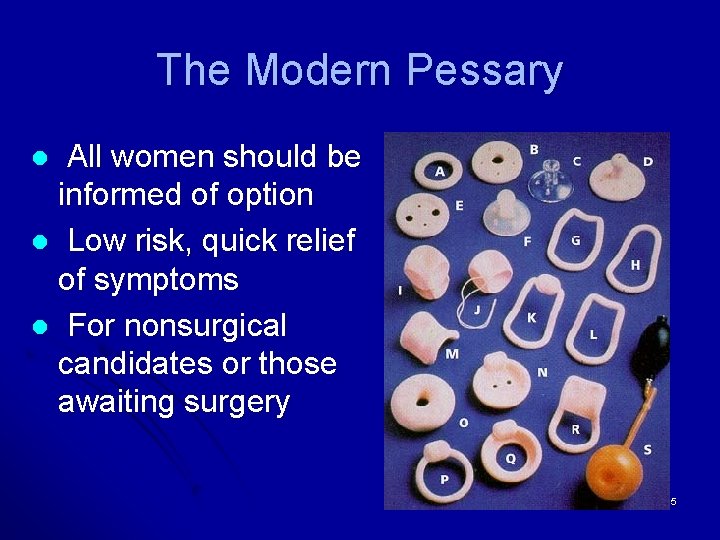
The Modern Pessary All women should be informed of option l Low risk, quick relief of symptoms l For nonsurgical candidates or those awaiting surgery l 15

Modern Pessaries 16
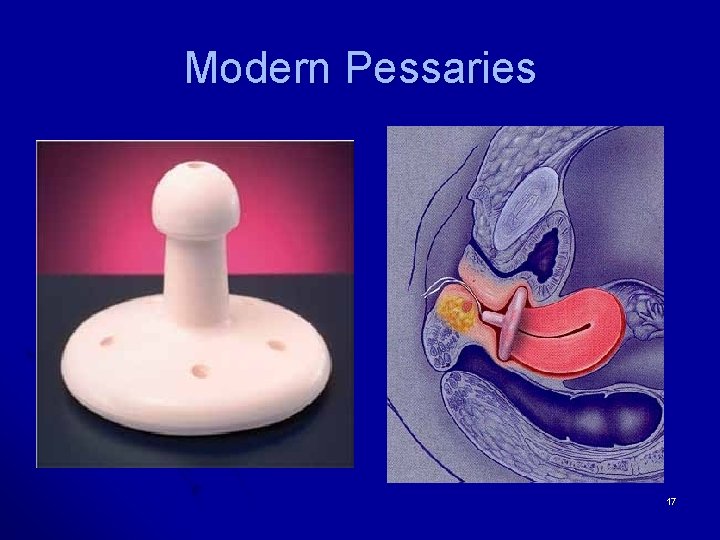
Modern Pessaries 17
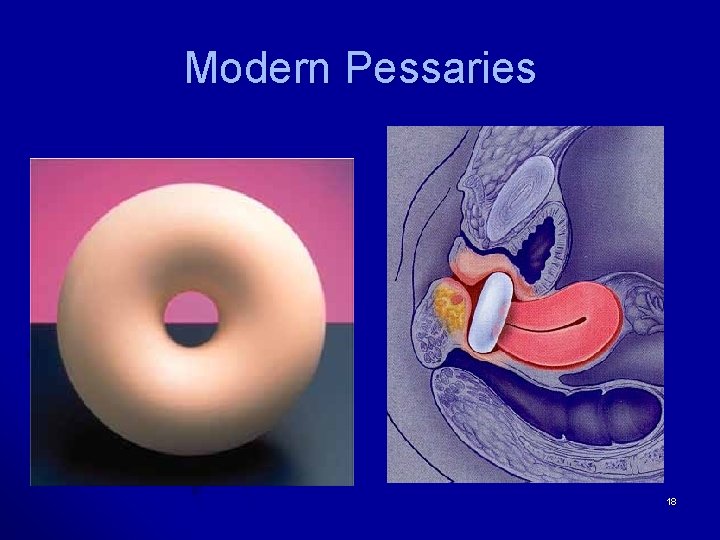
Modern Pessaries 18

What is the right type of pessary? l Survey of AUGS members : l 77% used pessary as first-line therapy for POP 12% reserved pessary for non-surgical candidates l l l 22% used ring for all defects 78% tailored pessary type to specific site of defect l l Anterior – ring Apical – ring Posterior - donut Complete procidentia - Gellhorn Cundiff G et al. A survey of pessary use by members of the American Urogynecologic Society. Obstet Gynecol 19 2000; 96: 18 -22.

Pessary: Evaluation and Outcome l Successful fitting 56 -73% (Clemons et al, 2004) l l Short vaginal length and wide introitus risk factors for unsuccessful fitting Handa, 2002 l FU 1 year l Improvement in stage in 4/19 (21%) l None had worsening of prolapse Clemons et al, 2004. Risk factors associated with an unsuccessful pessary fitting trial in women with pelvic organ prolapse. American Journal of Obs and Gynec. 190; 345 -50. Handa V et al, 2002 Do pessaries prevent the progression of pelvic organ prolapse? Int Urogynecol J Pelvic Floor Dysfunct. 13(6): 349 -51; discussion 352 20

Disadvantages of Pessary l l l Odor Discharge Vaginal ulcerations Must remove for coitus Case reports of: l l Erosion into bladder Fistula formation Ureteral obstruction with urosepsis or uremia Small bowel prolapse and incarceration 21

Summary PFD are common and costly in terms of health care dollars and patient quality of life l Effective nonsurgical interventions exist for urinary incontinence and POP l Primary care providers are ideal for screening for these disorders l Better understanding of PFD in women of all ages l 22

Thank You 23
- Slides: 23