PERTUSSIS Pathogenesis Clinical picture Lab treatment Prophylaxis By

PERTUSSIS Pathogenesis, Clinical picture, Lab ∆, treatment & Prophylaxis By Syed Nafeez

Pathogenesis: B. Pertussis is an obligate human parasite, surviving only for brief periods outside the host. Source: • Early cases, particularly in catarrhal stage • Carriers • Fomites Mode of transmission: Inhalation of infected aerosols (droplet infection) Habit: localized in cilia of resp. epitelium, doesn’t invade the bloodstream
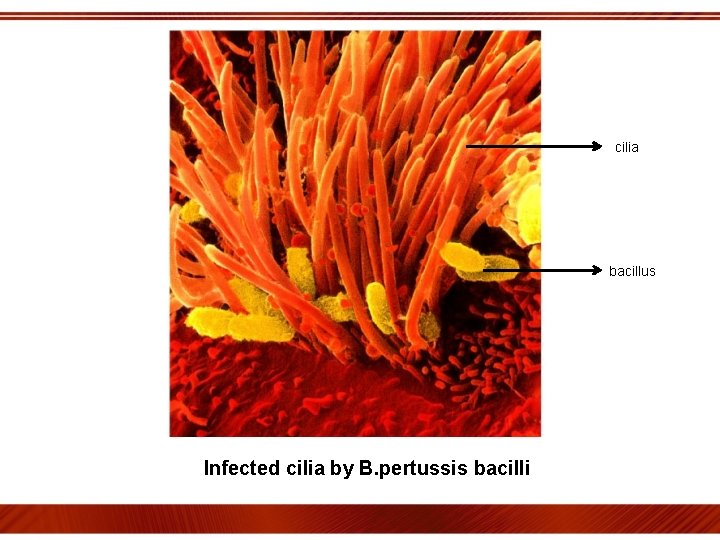
cilia bacillus Infected cilia by B. pertussis bacilli

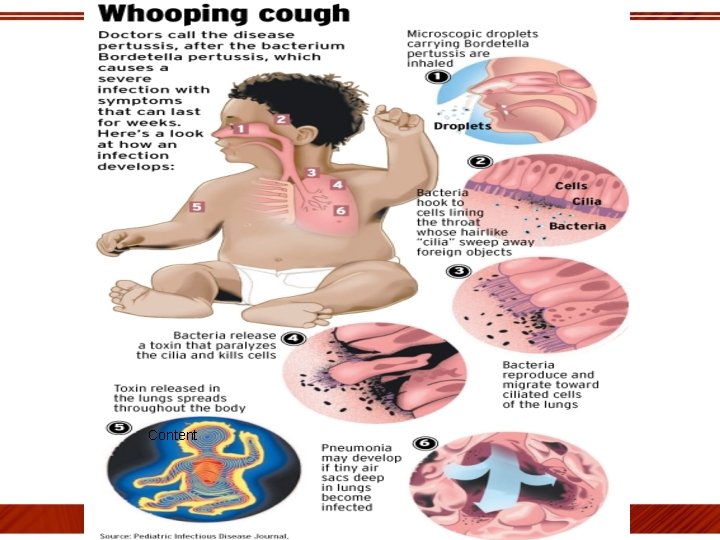
Mechanism: Droplet nuclei containing B. pertussis are inhaled Adherence & rapid multiplication on cilia of resp. epithelium of nasopharynx, trachea & bronchi Liberation of toxins(PT, TCT)& other substances…(FHA, AC) Paralyse cilia causing insitu Θ of natural defences of resp. tract secondary infections Irritate cells excessive secretions cough & catarrhal sympt Necrosis with polymorphonuclear obstruction of bronchioles ATELECTASIS infiltration diminished oxygenation Interstitial pneumonia, bronchopneumonia contributes to↑frequency of convulsions in infants
Title Content

Host response: Humoral response by the production of Ig. A & pertussis toxin antibodies is effective. These prevent attachment of the bacillus.

Clinical picture: Pertussis has an insidious onset after an IP of 1 -2 weeks & a protracted course comprising of 3 stages: • Catarrhal stage • Paroxysmal stage • Convalescent stage Each lasting for an approximate of 2 weeks
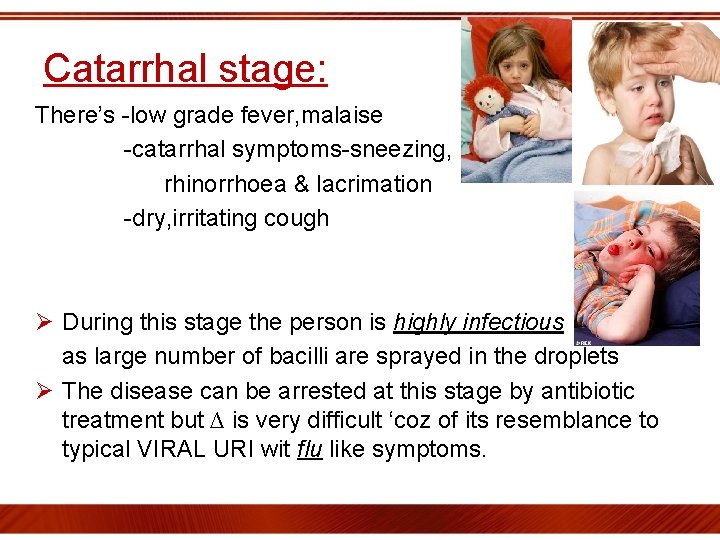
Catarrhal stage: There’s -low grade fever, malaise -catarrhal symptoms-sneezing, rhinorrhoea & lacrimation -dry, irritating cough Ø During this stage the person is highly infectious as large number of bacilli are sprayed in the droplets Ø The disease can be arrested at this stage by antibiotic treatment but ∆ is very difficult ‘coz of its resemblance to typical VIRAL URI wit flu like symptoms.

Paroxysmal stage: • Characterised by distinctive bouts of ↑frequency & intensity of cough that’s explosive in nature • During each bout, the patient experiences violent spasms of continuous coughing that almost empties the lungs following which there’s deep inspiration that produces the characteristic ‘WHOOP’ • The patient’s exhausted at the end of each bout. Post tussive vomiting, cyanosis & convulsions may occur. Young infants become apnoeic.


• About 40 -80 bouts occur throughout the day, more severe at night, yielding thick mucous plugs. • ‘WHOOP’ & major complications occur predominantly in children • The paroxysmal coughing predominates in older children & adults.

• Blood changes are distinctive & aid in ∆. There’s marked Leucocytosis with an absolute lymphocytosis. TLC-16, 000 -30, 000/μL with 60 -80% being lymphocytes Lymphocytes with lobulated nuclei lymphocytes in this blood smear from an 18 -month-old child with the infection have lobulated nuclei. The cytology of the cells could be mistaken for neoplastic lymphocytes.

Convalescent stage: There’s ↓frequency & severity of cough. The disease lasts for 6 -8 weeks, though it maybe very protracted as in premature infants, the malnourished, immunocompromised, people with genetic susceptibility.

Complications: Directly by B. pertussis Secondary infections • Pulmonary-pneumonia -sc emphysema aspirational -atelectasis • Neurological-epilepsy, paralysis • Miscellaneous-haemorrhage (sub-conjunctival, epistaxis) -otitis media -dehydration, malnutrition • In adults-rib fractures, back pain, hearing loss, urinary incontinence, hernias, rectal prolapse.

Lab ∆: Specimens: nasopharyngeal secretions blood(serum) for serological testing These are processed through: i. Culture ii. Direct Fluorescent Ab testing iii. Serological techniques-Ab titres, ELISA iv. PCR

i. Culture: Nasopharyngeal secretions required for culture are collected by following 4 methods: 1)Cough plate method: Ø A culture plate of Bordet Gengou Glycerine Potato Blood Agar is held 10 -15 cm infront of patient’s mouth during a bout of spontaneous or induced cough, such that the resp. exudate impinges directly on the medium. Ø The plate’s sealed & incubated for 48 -72 hrs. Ø Advantage is that the specimen is innoculated directly, at bedside.
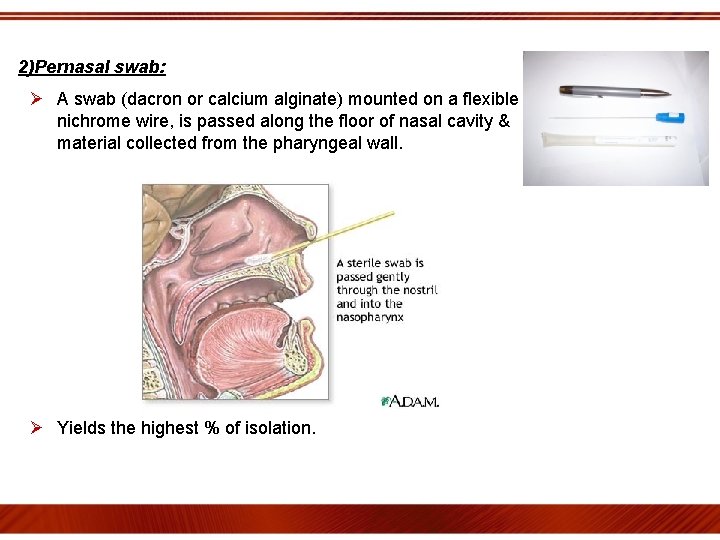
2)Pernasal swab: Ø A swab (dacron or calcium alginate) mounted on a flexible nichrome wire, is passed along the floor of nasal cavity & material collected from the pharyngeal wall. Ø Yields the highest % of isolation.

3)Nasopharyngeal aspiration: Ø Collected through a soft catheter attached to a syringe Ø Is the ‘preferred’ specimen. 4)Postnasal/peroral swab: Ø A cotton swab(West’s post nasal swab) is passed through mouth & secretions from posterior pharyngeal wall, collected. Ø There’s possibility of salivary contamination.

• Specimens should be innoculated immediately on BGGPB Agar or its modifications like Lacey’s DFP medium • In case of delay, transport media are used: Ø 0. 25 -0. 5 ml of Casamino acid solution, p. H-7. 2 Ø Modified Stuart’s medium Ø Mischulow’s charcoal agar Ø Modified Regan-Lowe medium: Is a ½ strength charcoal agar supplemented with 10% horse blood & cephalexin(40 mg/L) It Θ growth of nasopharyngeal flora. Is also the medium of choice for culture. • Culture plates are incubated for 7 days at high humidity & temperature of 35 -36 C. • Should be checked for any growth after 48 -72 hrs of innoculation & periodically thereafter.
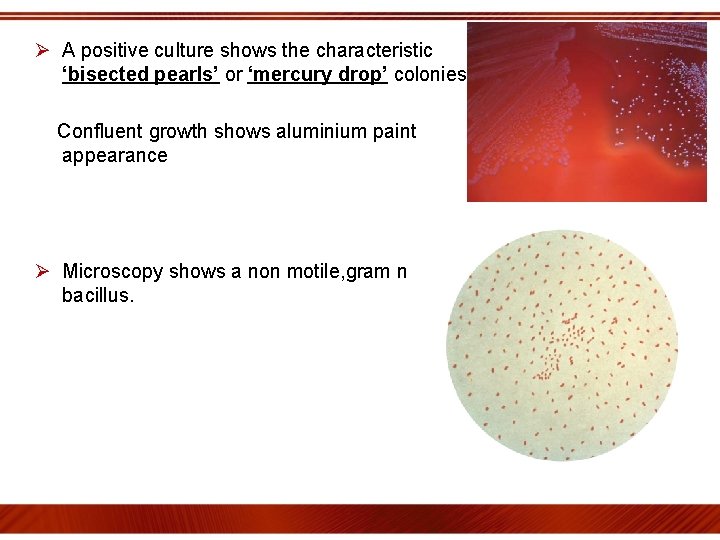
Ø A positive culture shows the characteristic ‘bisected pearls’ or ‘mercury drop’ colonies. Confluent growth shows aluminium paint appearance Ø Microscopy shows a non motile, gram negative bacillus.

ii. Direct FA testing: Used to identify the bacillus either in direct smears of clinical specimens or from culture. Ø Is inexpensive. Ø Provides rapid diagnosis & yields positive results when cultures are negative due to use of antibiotics. Ø Lacks specificity & sensitivity due to cross-reactions with nasopharyngeal flora…. . hence, unreliable & no longer recommended.

iii. Serological techniques: Focus on identifying significant variations in Ig. G & Ig. A titres(upto 4 fold ↑) against relavant B. pertussis virulence factors in both acute & convalescent phases of the disease. Ø Hence, for accurate ∆, serum samples in both phases of disease are to be collected. Ø Rise in Ab titres is demonstrated by: • • Agglutination not helpful as the rise in agglutinating & Gel precipitation precipitating Abs doesn’t occur untill 3 rd week Complement fixation tests of illness ELISA- highly specific Proposed as diagnostic method in culture sensitive cases A significant ↑ in titres(8 E -2 fold) between acute & convalescent phase is diagnostic of the disease

iv. PCR: Most sensitive method to ∆ Pertussis Ø Specimen used – nasopharyngeal aspiration Ø Primers for both B. pertussis & B. parapertussis should be included Ø Gives positive results even when the organism can’t be cultured. THE BOTTOM LINE: A major problem is the lack of access to diagnostic laboratory methods. Many routine laboratories are not equipped for the diagnosis of B. pertussis infection. This is the result of a general medical misconception that B. pertussis infection does not frequently occur in the population

Treatment: B. Pertussis isn’t susceptible to penicillins • Erythromycin is DOC adults-250 -500 mg/6 th hr 14 days children-30 -60 mg/kg/day • • Clarithromycin Azithromycin Cotrimoxazole Chloremphenicol Cough sedatives are not useful Corticosteroids reserved in severe cases, reduce duration of paroxysmal stage. Adrenergic ᵦ 2 stimulants, reduce severity of paroxysms, more useful in infants.

Prophylaxis: Preventing the spread of disease by isolation isn’t preferred as max. infectivity is in early stage when ∆ is difficult. Hence, prophylactic measures mainly include: • immunoprophylaxis Vaccines currently used: Ø DPT/DTw. P/Triple antigen vaccine Ø DTa. P Ø Tdap • Chemoprophylaxis • General prophylaxis
Immunoprophylaxis: 1)DPT/DTw. P/Triple antigen vaccine: • Composed of diphteria & tetanus toxoids, killed B. pertussis(smooth phase-1 strain)adsorbed on aluminium phosphate. thiomersol as preservative • Dosing schedule: Ø 3 Primary doses-at 6, 10 & 14 weeks of life Ø 2 Booster doses-1 st booster at 15 -18 months -2 nd at 5 years • Dose & route: 0. 5 ml, IM • Site: AL aspect of thigh in infants or deltoid

• Side-effects: Minor reactions: Ø Localized to site-soreness, swelling, redness Last for 1 -2 days Treat with analgesics Ø Systemic-fever, fussiness, drowsiness, anorexia Moderate reactions: Seen in about 1: 100/1000 shots: Ø Crying non-stop for 3 hrs or more Ø Fever of 105 F or more Less often in about 1: 1750 shots: Ø Seizures(convulsions, spasms, staring spells) Ø Collapse or fainting-child becomes blue, pale, limp & nonresponsive Severe reactions: rare Prolonged seizures, ↓consciousness, coma, permanent brain damage & death. !!!DPT vaccine is contraindicated if moderate to severe reactions occur. Also contraindicated below 6 weeks of life & above 6 yrs

2)DTa. P Vaccine: Is an acellular vaccine with pertussis component consisiting of inactivated pertussis toxin, filamentous hemagglutinin, pertactin, or fimbriae along with diphteria & tetanus toxoids in concentrations similar to DTw. P vaccine. Ø Indicated for children of 6 weeks-6 years of life. Ø Dosing schedule is the same.
3)Tdap vaccine: Is an acellular vaccine with concentrations of diphteria toxoid & pertussis component reduced to 1/10 of DTa. P vaccine. Ø for adolescents between the ages of 10 and 18 years Ø preservative free (which means that, like most new vaccines, it doesn't contain thimerosal) Ø A similar Tdap vaccine, Adacel, is being reviewed by the FDA & might be available for people between the ages of 11 and 64, which would be good news for adults who also want protection against pertussis.

Prevention and treatment prophylaxis of secondary cases The CDC has defined a close contact as: Ø someone having face-to-face exposure within 3 feet of a symptomatic patient Ø someone who has had direct contact with respiratory, oral, or nasal secretions from a symptomatic patient Ø someone who has shared the same confined space for more than 1 hour with a symptomatic person. Chemoprophylaxis is given with recommended antibiotics and dosage regimens, identical to those used for treatment of active infection. Ø should be started in the asympto-matic person within 21 days of cough onset in the index patient. Ø highly recommended for all children younger than 12 months and women in the third trimester of pregnancy who have been exposed to pertussis

Epidemiology: • • • Ø Predominantly a pediatric disease. Incidence & mortality highest in 1 st year of life. Common in females than males at all ages. Worldwide distribution with most deaths occuring in Africa, Asia, central & latin America. Ø Occurs endemically & epidemically Ø In recent years, there’s been resurgence of the disease in USA & eastern european countries Ø Also, there’s an ↑ in number of cases being reported in Asia.

The Statistics: Ø According to WHO estimates, around 2. 95 lakh persons died of whooping cough in 2002. Ø In developing countries, the case fatality rates range from 4 -15% in infants Ø About 10% of cases & 50% of deaths occur in children <1 yr Ø In India, there’s been marked decline in reported cases from 1987 -2005 year cases reported 1987 1. 63 lakh 2002 26700 2005 43955

THANK YOU

& XCUSE me if u have slept through!!
- Slides: 34