Persistent Pulmonary Hypertension of Newborn What is PPHN

Persistent Pulmonary Hypertension of Newborn

What is PPHN Persistence of fetal pulmonary hypertension resulting in severe hypoxia
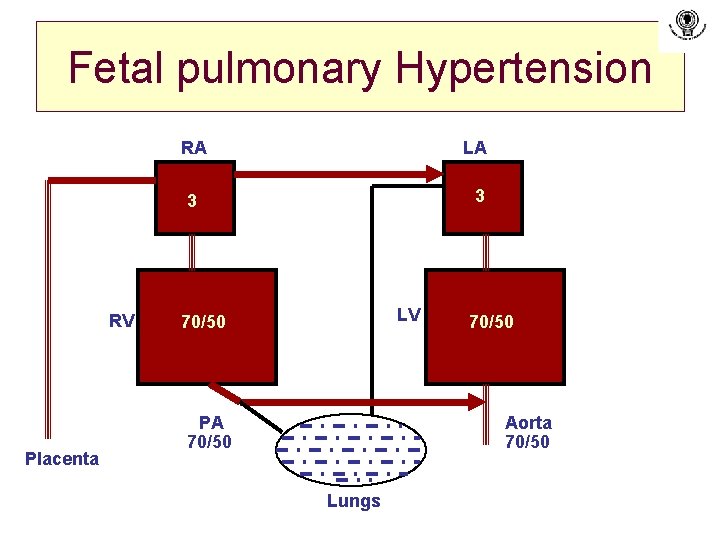
Fetal pulmonary Hypertension RV Placenta RA LA 3 3 LV 70/50 PA 70/50 Aorta 70/50 Lungs
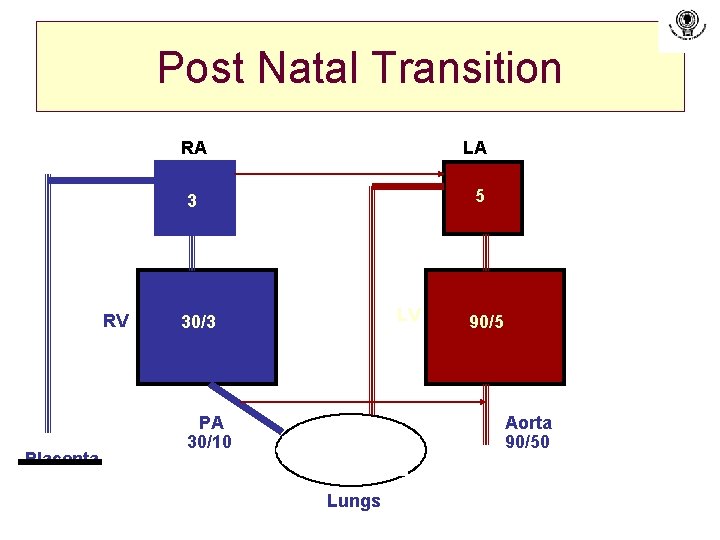
Post Natal Transition RV Placenta RA LA 3 5 LV 30/3 PA 30/10 90/5 Aorta 90/50 Lungs
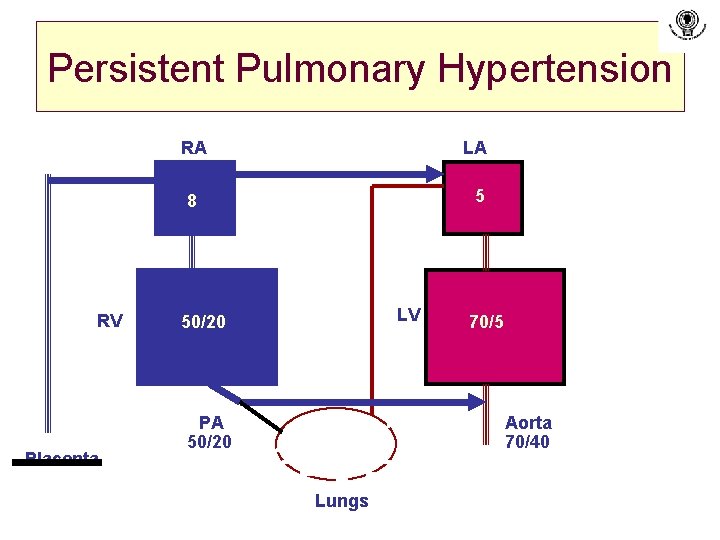
Persistent Pulmonary Hypertension RV Placenta RA LA 8 5 LV 50/20 PA 50/20 70/5 Aorta 70/40 Lungs

Persistent Pulmonary Pressures • Pulmonary vasoconstriction – Asphyxia, MAS, CDH, Pneumonia, Severe HMD – hypoxia, acidosis, hypocalcaemia, Mg – Hypothermia • Decreased pulmonary arterioles – Hypoplastic lungs, CDH, Alveo-capillary dysplasia • Muscularization of pulmonary acinar arteries – Chronic in-utero hypoxia (IUGR), Post maturity – Maternal Salicylate or Indomethacin therarpy

When to suspect PPHN • MAS, Asphyxia, Sepsis, Pneumonia, Severe HMD, CDH – Severe hypoxia, labile saturations – Sp 02 : R upper limb and L Lower limb > 10% – Pa 02 : R upper limb and L Lower limb > 20 mm of Hg – RV heave, close split/single S 2, systolic murmur (TR) • Post maturity/ IUGR – Tachypnea, cyanosis, no retractions, no creps – Others findings as before
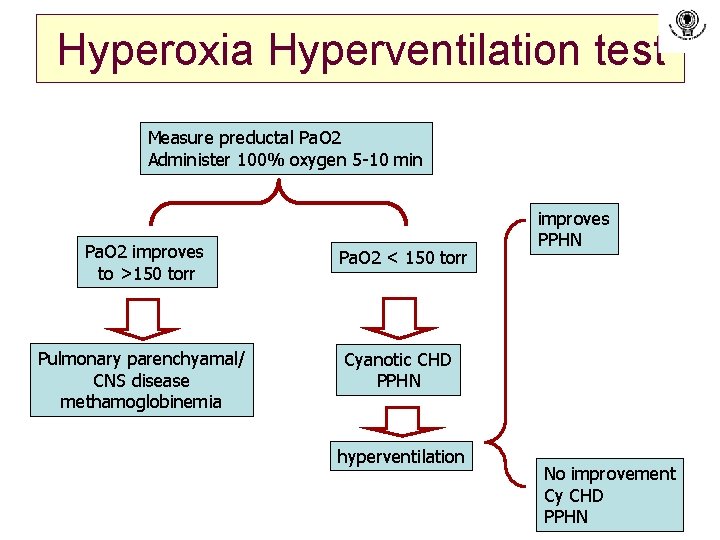
Hyperoxia Hyperventilation test Measure preductal Pa. O 2 Administer 100% oxygen 5 -10 min Pa. O 2 improves to >150 torr Pulmonary parenchyamal/ CNS disease methamoglobinemia Pa. O 2 < 150 torr improves PPHN Cyanotic CHD PPHN hyperventilation No improvement Cy CHD PPHN
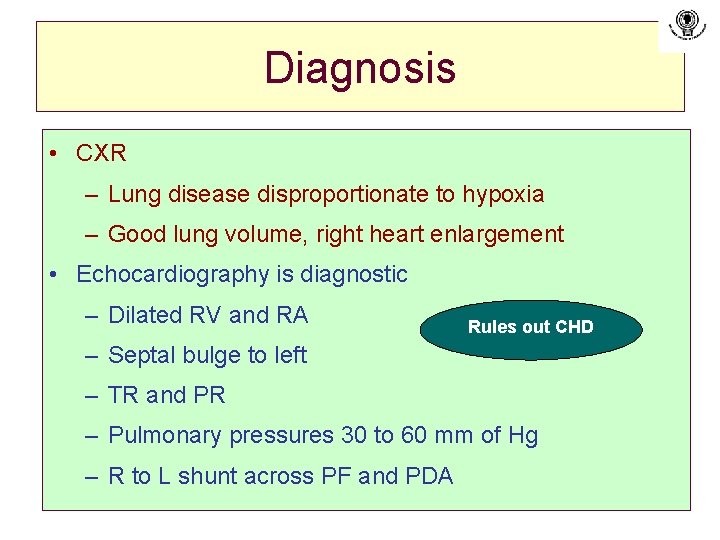
Diagnosis • CXR – Lung disease disproportionate to hypoxia – Good lung volume, right heart enlargement • Echocardiography is diagnostic – Dilated RV and RA Rules out CHD – Septal bulge to left – TR and PR – Pulmonary pressures 30 to 60 mm of Hg – R to L shunt across PF and PDA

Severity of PPHN • On Ventilation with 100% Fi. O 2 : Pa. O 2<50 mm of Hg • Aa. DO 2 > 600 for 6 to 8 hours – Alveolar Oxygen {Fi. O 2*(760 -47)- Pa. CO 2} – Arterial Oxygen • Oxygenation Index > 40 on 3 or more ABGs 30 min apart • Echocardiography: – Pulmonary pressure more than systemic pressures – Continuous Right to left shunts

Principles of Therapy • Reverse pulmonary vasoconstriction – Hypoxia, acidosis, Ca+2, Mg, Polycythemia – Hypothermia, sepsis • Improve lung disease (MAS, HMD, Pneumonia) – Surfactant, Gentle ventilation or HFV • Increase systemic pressure ECMO – Inotropes and fluids • Pulmonary vasodilators Tolazoline, Nitroprusside, • High oxygen, Alkalosis Mgsulphate, Prostacylin • Hypocarbia (HFV) • Inhaled Nitric Oxide and Sildenafil
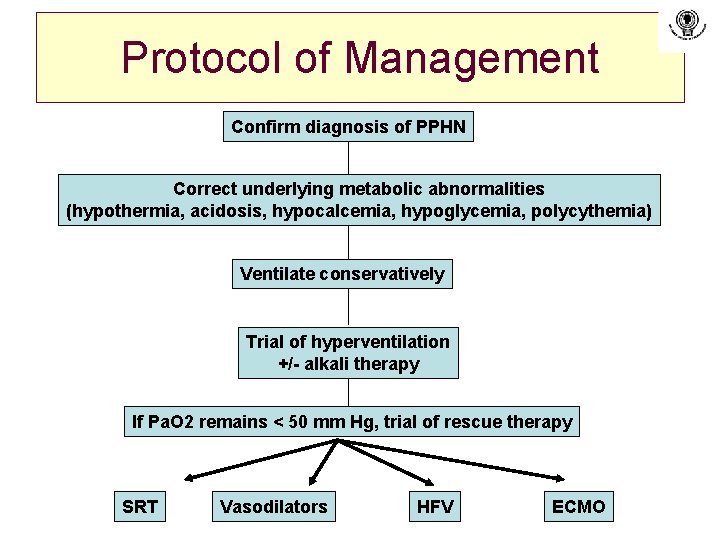
Protocol of Management Confirm diagnosis of PPHN Correct underlying metabolic abnormalities (hypothermia, acidosis, hypocalcemia, hypoglycemia, polycythemia) Ventilate conservatively Trial of hyperventilation +/- alkali therapy If Pa. O 2 remains < 50 mm Hg, trial of rescue therapy SRT Vasodilators HFV ECMO

Pulmonary Vasoconstriction • Reduce oxygen demand, maximize delivery • Nurse in thermoneutral environment • Minimize handling , Sedation, analgesia • Maintain Fluid balance, glucose & calcium homeostasis • Correct hypotension, acidosis, anemia, polycythemia & hypocalcemia. • Maintain Pa. O 2 - 80 -100 torr
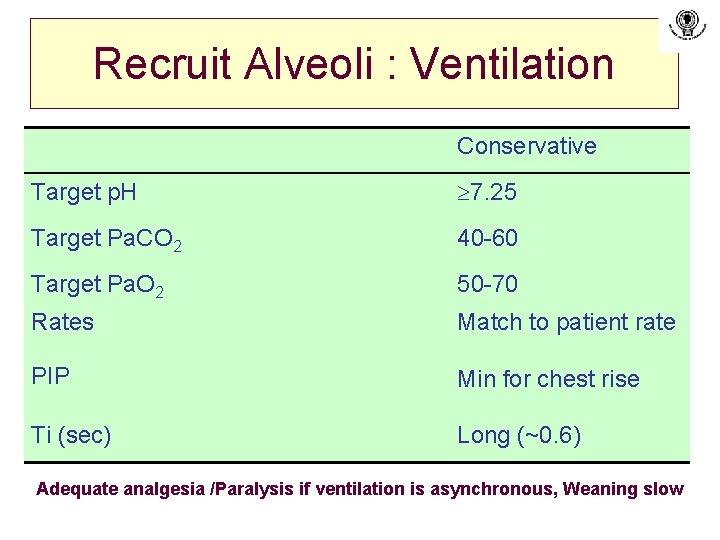
Recruit Alveoli : Ventilation Conservative Target p. H 7. 25 Target Pa. CO 2 40 -60 Target Pa. O 2 50 -70 Rates Match to patient rate PIP Min for chest rise Ti (sec) Long (~0. 6) Adequate analgesia /Paralysis if ventilation is asynchronous, Weaning slow
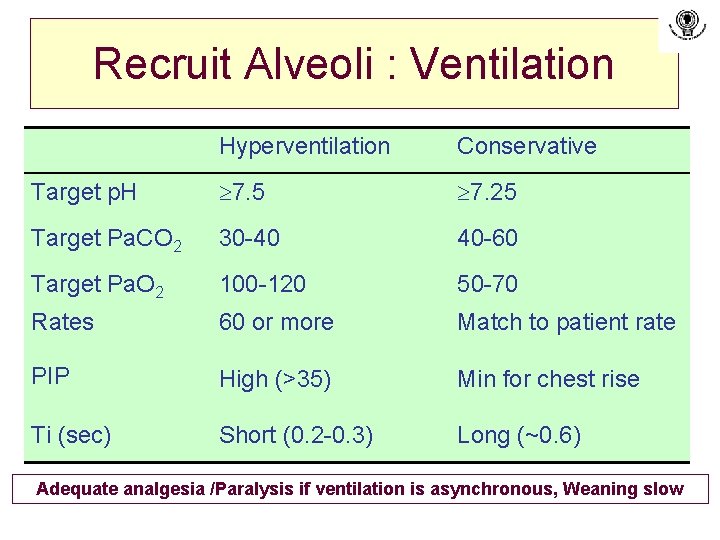
Recruit Alveoli : Ventilation Hyperventilation Conservative Target p. H 7. 5 7. 25 Target Pa. CO 2 30 -40 40 -60 Target Pa. O 2 100 -120 50 -70 Rates 60 or more Match to patient rate PIP High (>35) Min for chest rise Ti (sec) Short (0. 2 -0. 3) Long (~0. 6) Adequate analgesia /Paralysis if ventilation is asynchronous, Weaning slow

Gentle Ventilation • Accepting low p. H(7. 15 for 24 hrs), low Pa. O 2 and high Pa. CO 2 (60 to 70 mm of Hg) • Goals achieved at lower pressures & Fi. O 2 • Lesser subsequent morbidities • Comparable survival • Long-term outcome not known Wung et al

Lung Recruitment • HFV – Used as a rescue therapy (Best with inhaled NO) – Useful if lung disease is significant – High volume strategy with HFOV – MAP and Fi. O 2 for Pa. O 2, Amplitude for Pa. CO 2 – Target Pa. O 2 60 to 80 and Pa. CO 2 30 -40 mm of Hg • Surfactant – Severe HMD or MAS
Pulmonary Vasodilators • Selective – Inhaled nitric oxide – Sildenafil – Alkali therapy • Non-selective – Tolazoline – Nitroprusside – Adenosine – Prostacylin, PGD 2 and PGE 1

Inhaled Nitric Oxide • Inhaled nitric oxide ---- increased cyclic GMP---- inhibit myosin-protein in vascular smooth muscle-- relaxation • Sustained improvement in term/near term babies • Not approved for use in preterm neonates <34 weeks • A few side effects (methemoglobinemia, lung injury) • Costly (5 lakhs initial, 20, 000 1 st time and refilling 12, 000
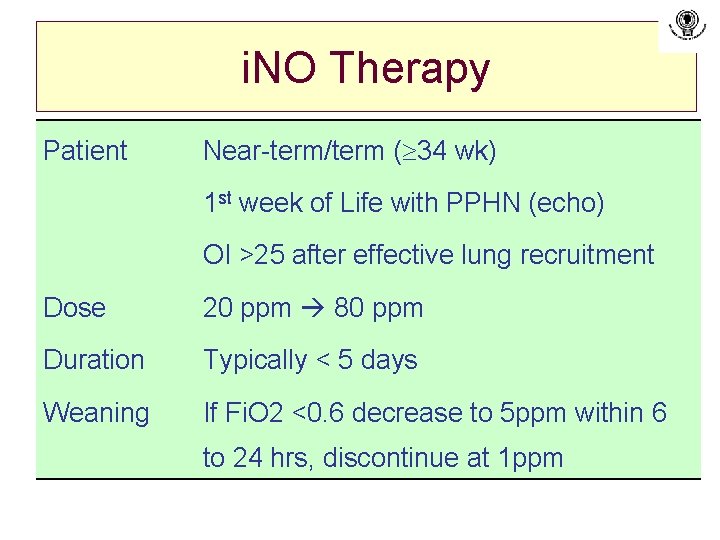

i. NO Therapy Patient Near-term/term ( 34 wk) 1 st week of Life with PPHN (echo) OI >25 after effective lung recruitment Dose 20 ppm 80 ppm Duration Typically < 5 days Weaning If Fi. O 2 <0. 6 decrease to 5 ppm within 6 to 24 hrs, discontinue at 1 ppm


Sildenafil • Potent selective pulmonary vasodilator • Augment effects of & help weaning from i. NO • Early data (alone/+i. NO)-promising. • Wait till sufficient evidence on efficacy, dosage and safety

Alkali therapy • Hypocarbia is a pulmonary vasodilator • Respiratory acidosis Metabolic acidosis • Alkali therapy(1 -2 meq/kg/hr) fraught with adverse effects – Hypernatremia. – Hypocalcemia. Long term Hearing deficit – Hyperosmolality. – Shift of oxygen dissociation curve • Variable reports of success • Evidence: use only for correction of acidosis

Prevention • Good antenatal care • Avoid NSAID during pregnancy • Prevention of asphyxia • Good supportive care- normothermia, oxygenation, perfusion, normoglycemia, normocalcemia • Avoid unnecessary interventions

Prognosis • Dependent on multiple aspects. • Mortality- 20 -40% • Neurological handicap- 12 -25%

Summary • Pulmonary vasoconstriction, pulmonary arterioles and Muscularization of acinar arteries------ PPHN • Suspect PPHN when hypoxia is severe – MAS, asphyxia, Severe HMD, Sepsis, IUGR, CDH • Confirm diagnosis by ECHO

Summary… Treatment – Relieve Pulmonary vasoconstriction – Increase systemic pressures – Ventilate appropriately – Improve lung condition : HFV, surfactant – Selective pulmonary vasodilators
- Slides: 27