Peripheral Neuropathy Clinical Management Course February 12 2007

Peripheral Neuropathy Clinical Management Course February 12, 2007 Peter D. Donofrio, M. D. Professor of Neurology
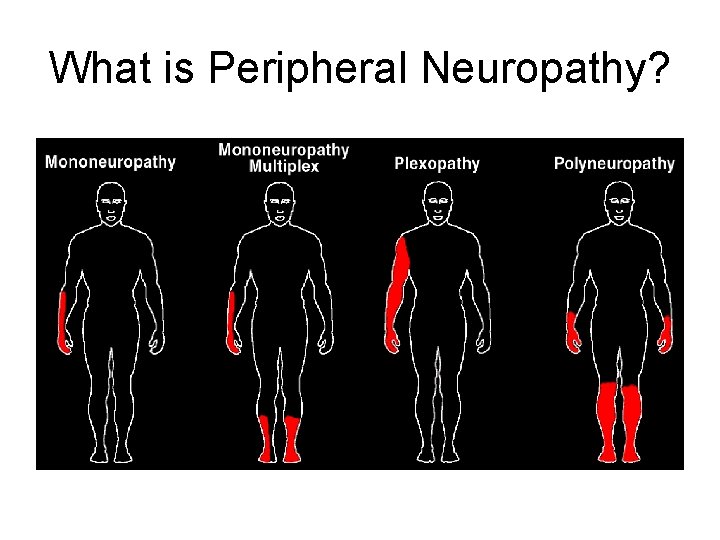
What is Peripheral Neuropathy?

Common Mononeuropathies • Median at the Wrist (CTS) • Ulnar at the Elbow (Tardy Ulnar Palsy) • Peroneal Palsy at the Fibular Head
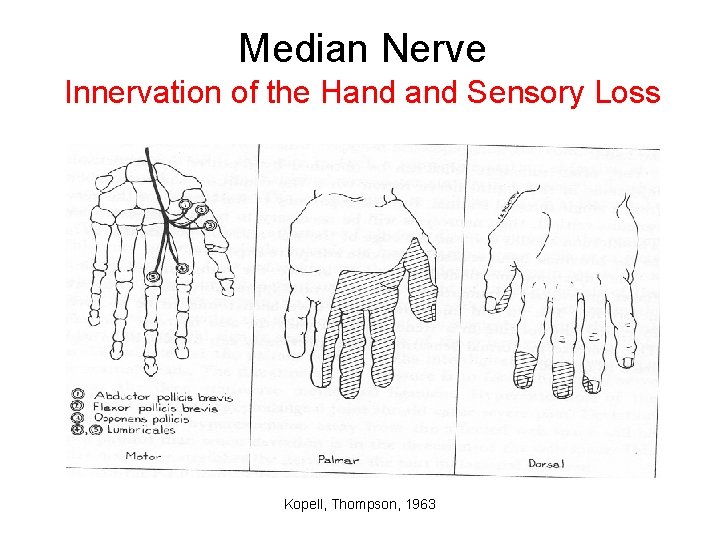
Median Nerve Innervation of the Hand Sensory Loss Kopell, Thompson, 1963
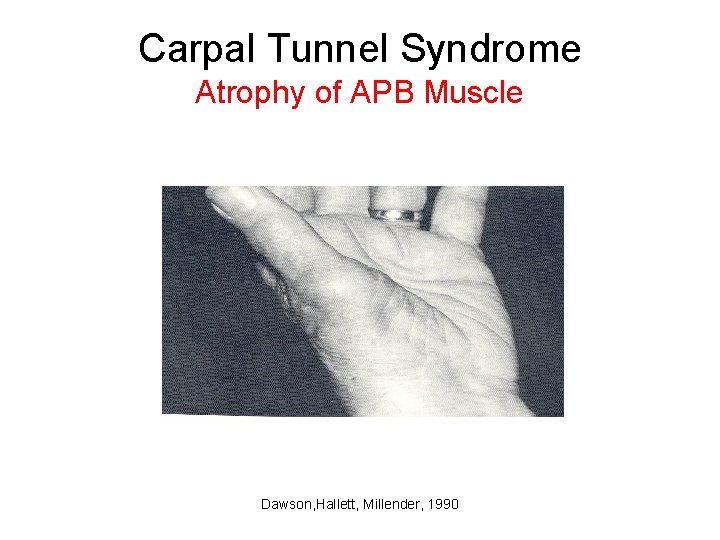
Carpal Tunnel Syndrome Atrophy of APB Muscle Dawson, Hallett, Millender, 1990
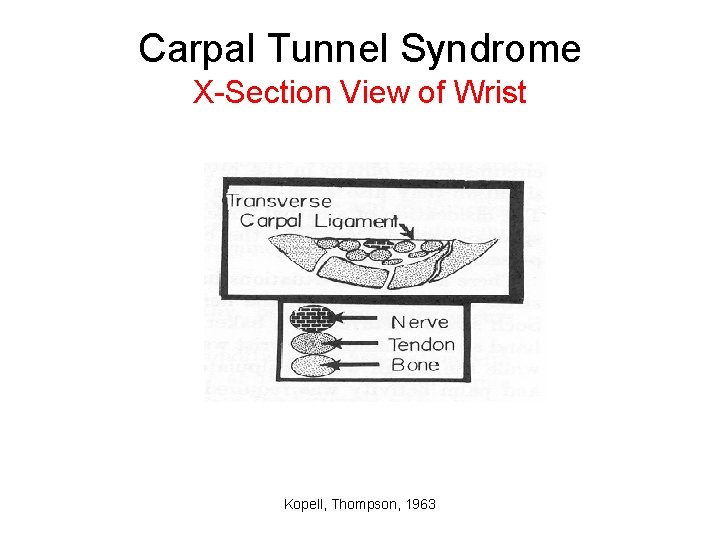
Carpal Tunnel Syndrome X-Section View of Wrist Kopell, Thompson, 1963
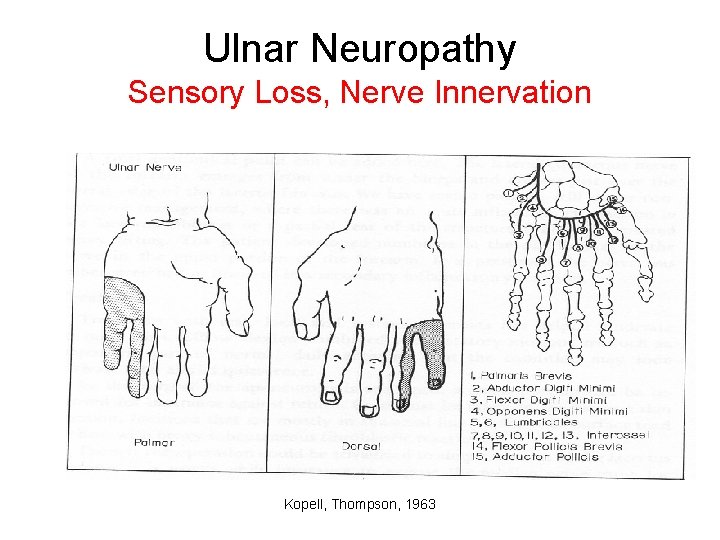
Ulnar Neuropathy Sensory Loss, Nerve Innervation Kopell, Thompson, 1963
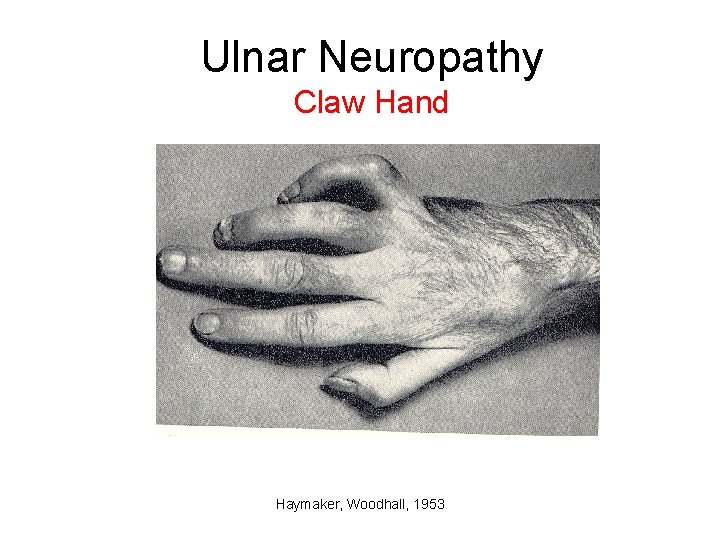
Ulnar Neuropathy Claw Hand Haymaker, Woodhall, 1953
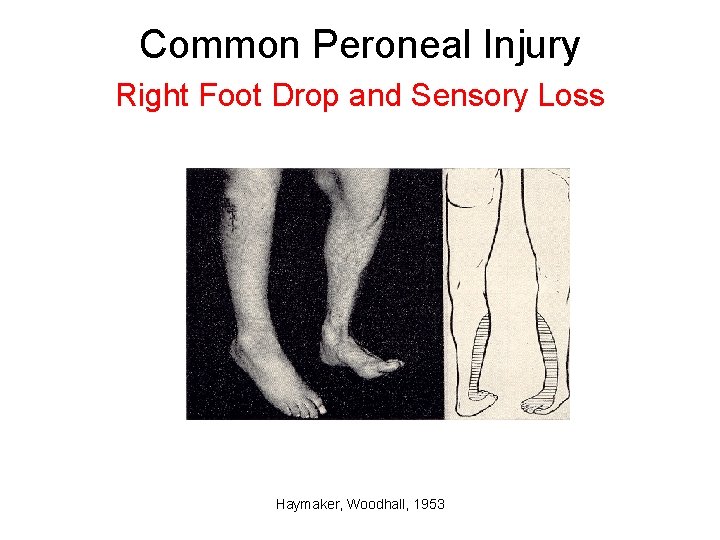
Common Peroneal Injury Right Foot Drop and Sensory Loss Haymaker, Woodhall, 1953
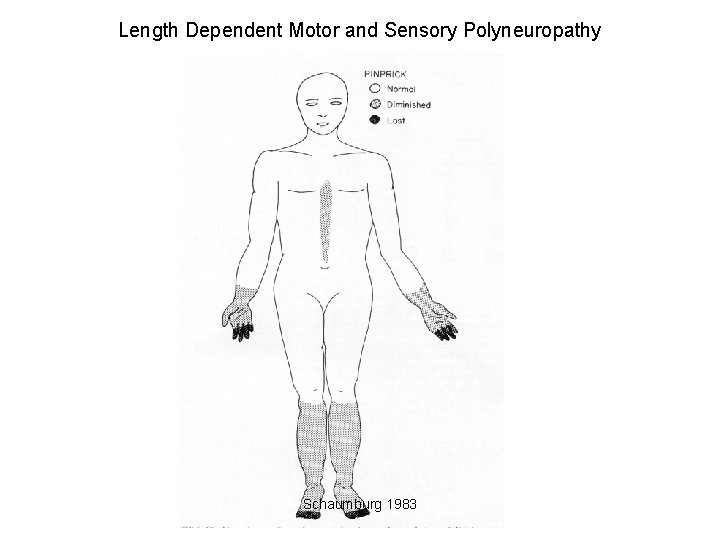
Length Dependent Motor and Sensory Polyneuropathy Schaumburg 1983

Peripheral Neuropathy Etiologies • Diabetes mellitus • Alcohol Abuse • Nutritional: Deficiency of B 1, B 6, B 12, malabsorption syndromes • Uremia • Vasculitis • Genetic/Inherited • Inflammatory • Toxic – Industrial agents – Therapeutic agents

Diabetes Compelling Facts • 7 -8 % of U. S. population (23. 6 million) • 8. 9 million unaware of diagnosis • Total annual economic cost (1997) $98 billion – $44 billion direct medical and treatment – $54 billion indirect costs (disability and mortality) • 7 th leading cause of death • High prevalence in Afro-Americans, Hispanics, Native Americans

Diabetic Neuropathy Prevalence • >60% of diabetics-signs/electrodiagnostic evidence of polyneuropathy (depressed ankle reflexes, absent or diminished distal nerve amplitudes) • 25%- neuropathic pain which can be severely disabling • Majority of Type II diabetics are symptomatic or have signs of neuropathy at diagnosis
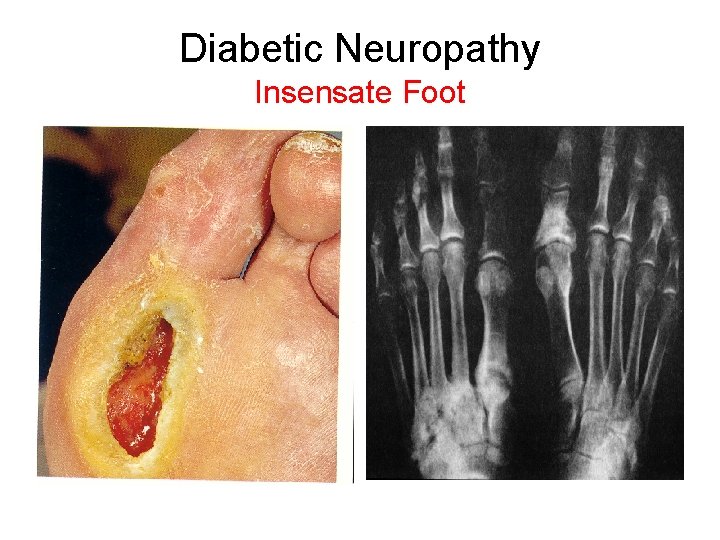
Diabetic Neuropathy Insensate Foot
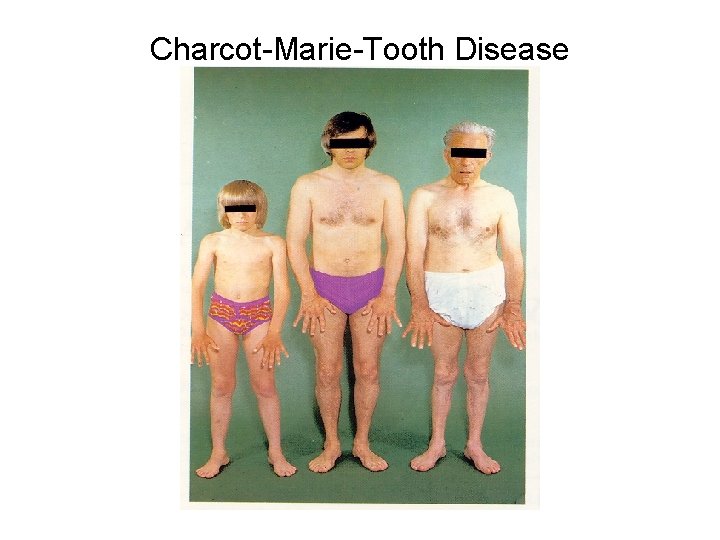
Charcot-Marie-Tooth Disease
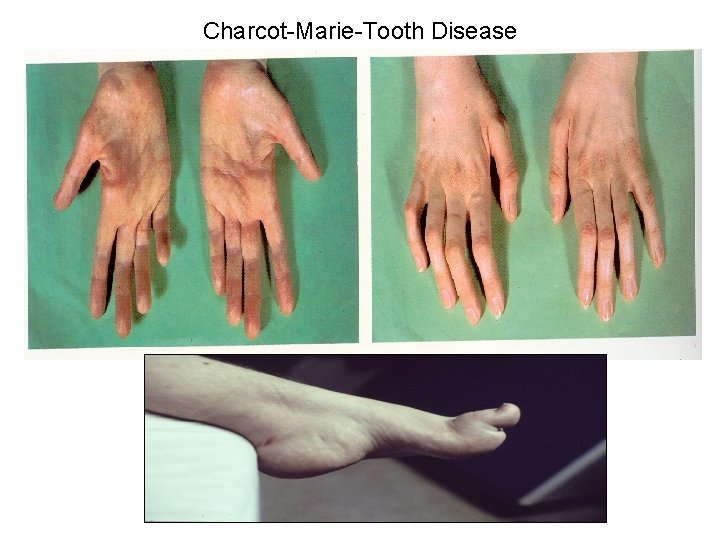
Charcot-Marie-Tooth Disease

Polyneuropathy B 12 (Cobalamin) deficiency • Neurologic manifestations: – Large-fiber sensory loss – Corticospinal tract involvement • EMG reveals a polyneuropathy • Serum levels of B 12 below 100 pg/ml diagnostic, between 100 and 200 pg/ml suggestive • Elevated methylmalonic acid level more sensitive than B 12 level. • Shilling’s test rarely done anymore • Treatment may not reverse all symptoms

Guillain-Barre(-Strohl) Syndrome Clinical Features • Ascending, symmetric, subacute (days) polyneuropathyweakness/paresthesias • About 1/3 require mechanical ventilation • Parainfectious: C. jejuni, M. pneumoniae, CMV, EBV, HIV, Hep A, others • Loss of DTRs • CSF: albumino-cytologic dissociation • Treatment: supportive, PEx, IVIG

Diagnostic Criteria Typical Guillain-Barré Syndrome • Clinical features: – – Weakness that is approximately symmetric in all the limbs Paresthesias in the feet and hands Areflexia or hyporeflexia in all limbs by 1 week Progression of these three features over several days to 1 month • Laboratory abnormalities that confirm the diagnosis: – Elevated CSF protein concentration (more than 45 mg/d. L) within 3 weeks from onset – Abnormalities on electrophysiologic studies

Polyneuropathy Initial Evaluation • • CBC Comprehensive Metabolic Profile Fasting blood sugar Glucose tolerance test (if needed) Vitamin B 12 ESR SPEP Nerve Conduction Studies and EMG
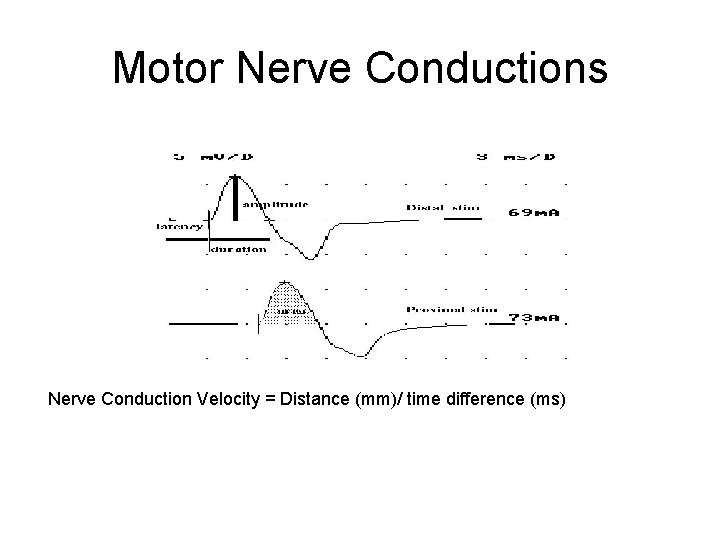
Motor Nerve Conductions Nerve Conduction Velocity = Distance (mm)/ time difference (ms)

Summary • • • Definition of Peripheral Neuropathy Common Mononeuropathies Polyneuropathy-emphasis on diabetes Evaluation of polyneuropathy Nerve conduction studies.
- Slides: 22