Peripheral artery diseases Jakub Honk Kardiologick klinika 2

Peripheral artery diseases Jakub Honěk Kardiologická klinika 2. LF UK a FN Motol

Diagnostic methods Peripheral artery diseases (limb ischemia) ◦ Chronic PAD ◦ Acute limb ischemia Compressive syndromes Vasospastic disorders Specific localization of PAD Vasculitis

Diagnostic methods Medical history, physical examination Measurement of peripheral arterial pressure (+ ABI, TBI) at rest, after exercise Plethysmographic examination Tcp. O 2 Teadmill walking test Color duplex sonography X-ray based methods - DSA, CTA, MRA
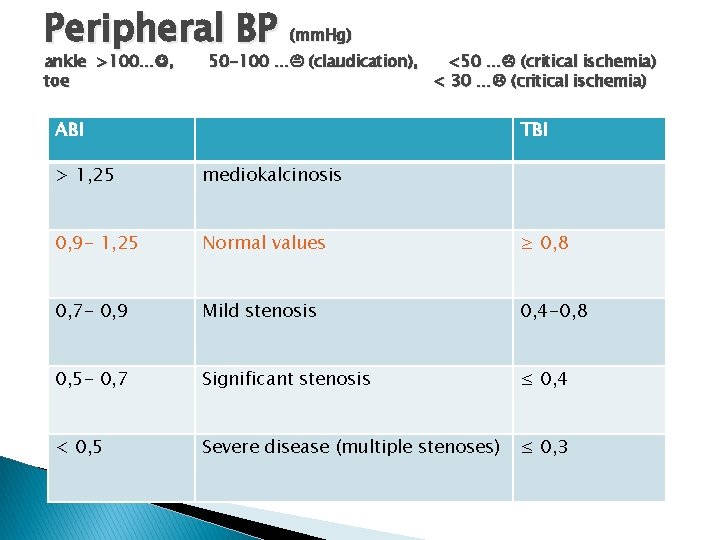
Peripheral BP (mm. Hg) ankle >100… , toe 50 -100 … (claudication), <50 … (critical ischemia) < 30 … (critical ischemia) ABI TBI > 1, 25 mediokalcinosis 0, 9 - 1, 25 Normal values ≥ 0, 8 0, 7 - 0, 9 Mild stenosis 0, 4 -0, 8 0, 5 - 0, 7 Significant stenosis ≤ 0, 4 < 0, 5 Severe disease (multiple stenoses) ≤ 0, 3

tcp. O 2 Testing peripheral skin perfusion on the capillary level; testing skin nutrition Closely corresponds to the capillary pressure of O 2 → To determine the degree of perfusion (ischemia), evaluate the effectiveness of revascularization, determine amputation line, predict effect of hyperbaric oxygen therapy

tcp. O 2 (transkutánní měření parciálního tlaku kyslíku ve tkáni) tcp. O 2 > 50 mm. Hg normal > 30 mm. Hg satisfactory > 20 mm. Hg prediction of healing of amputation stump < 10 mm. Hg critical ischemia
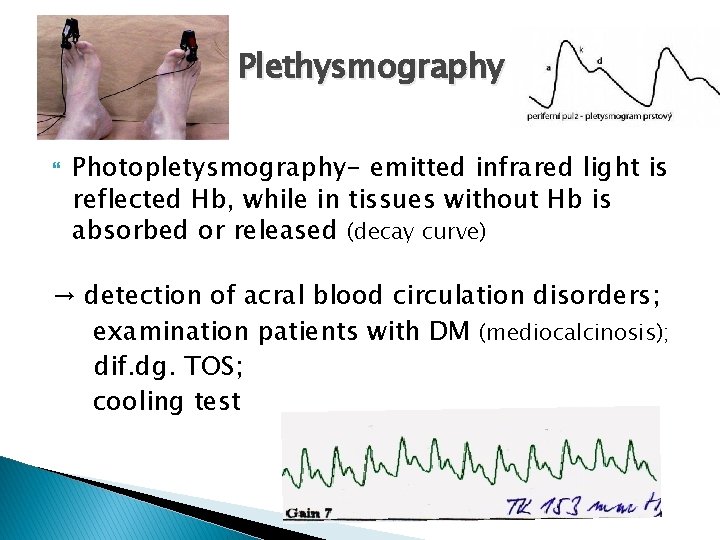
Plethysmography Photopletysmography- emitted infrared light is reflected Hb, while in tissues without Hb is absorbed or released (decay curve) → detection of acral blood circulation disorders; examination patients with DM (mediocalcinosis); dif. dg. TOS; cooling test
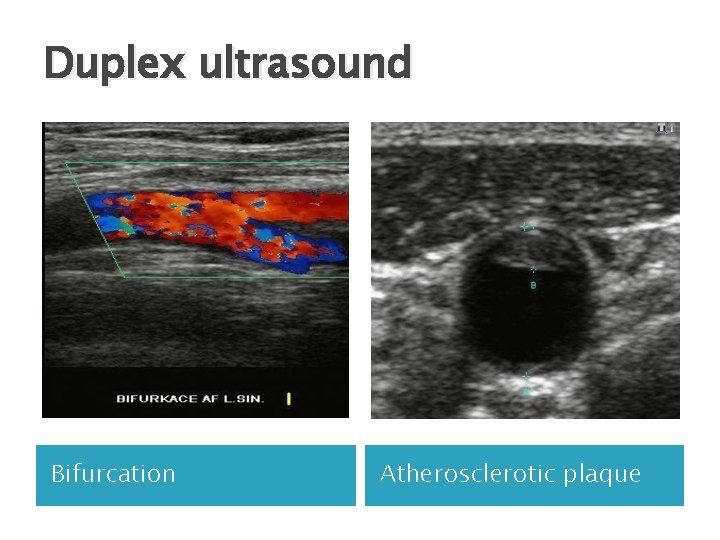
Duplex ultrasound Bifurcation Atherosclerotic plaque
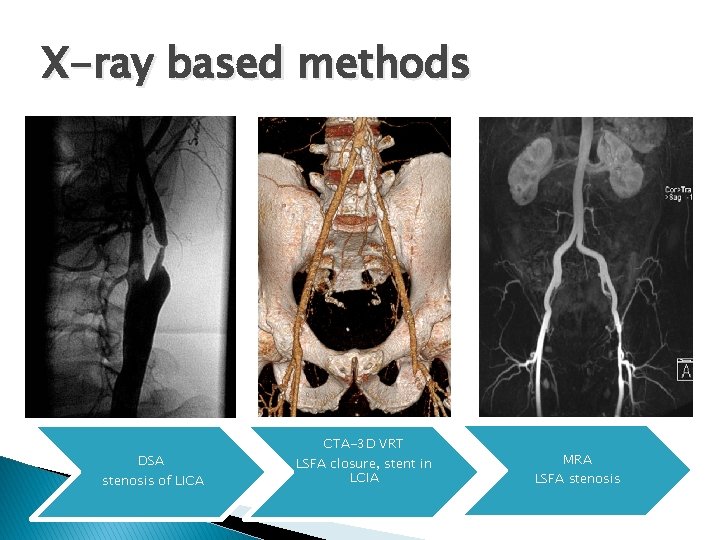
X-ray based methods DSA stenosis of LICA CTA-3 D VRT LSFA closure, stent in LCIA MRA LSFA stenosis

Peripheral artery diseases (PAD) � Peripheral artery disease (PAD) generally refers to a disorder that obstructs the blood supply to the lower or upper extremities � 90 -95 % atherosclerosis � 5 -10% thrombosis, embolism, vasculitis, fibromuscular dysplasia, entrapment Impcact on quality of life + mortality (cardiovascular) > 50% patients with PAD at the same time suffer from coronary atherosclerosis, 15 -40% and carotid atherosclerosis
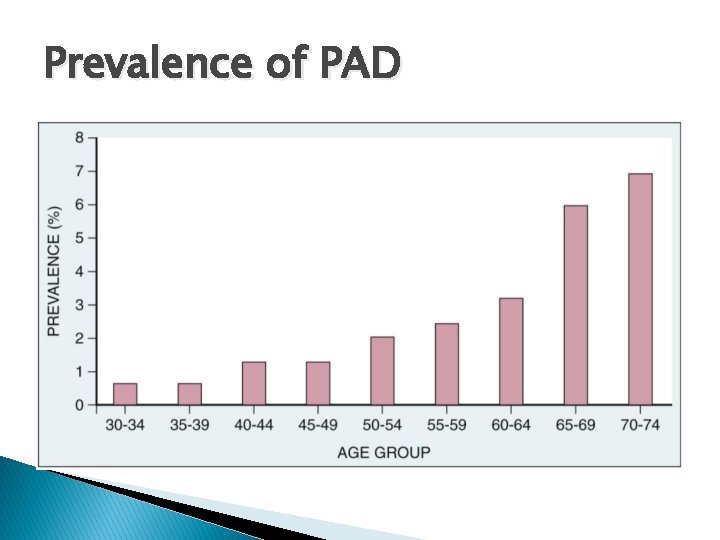
Prevalence of PAD

Modifiable risk factors (atherosclerosis) Cigarette smoking Dyslipidemia Diabetes Arterial hypertension

Less frequent causes of PAD • • • • Coarctation of the aorta Vasculitides Tromboangiitis obliterans (Buergers disease) Peripheral embolisation from various origins Entrapment sy AP Cystic adventitial degeneration AP fibromuscular dysplasia Iliac artery endofibrosis of cyclists Primary vascular tumors Compression (tumors etc. ) Vascular trauma Iatrogenic vascular disease (percutaneous and surgical procedures) Irradiation arterial disease
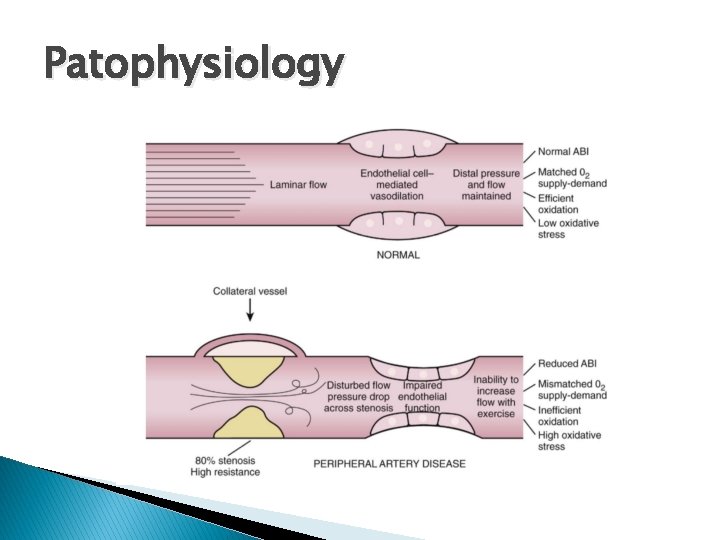
Patophysiology

Symptoms Chronic disease ◦ Claudication – muscle ischemia ◦ Site of stenosis correlates with site of pain ◦ intermittent claudication – on exertion Critical limb ischemia ◦ Acute vs. chronic ◦ Limb/life threatening disease ◦ paresthesia, pain at rest
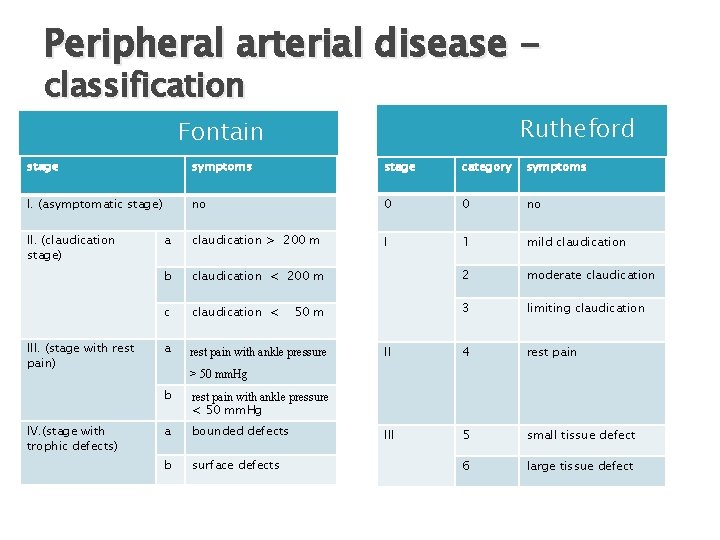
Peripheral arterial disease classification Rutheford Fontain stage symptoms stage category symptoms I. (asymptomatic stage) no 0 0 no a claudication > 200 m I 1 mild claudication b claudication < 200 m 2 moderate claudication c claudication < 3 limiting claudication a rest pain with ankle pressure II 4 rest pain III 5 small tissue defect 6 large tissue defect II. (claudication stage) III. (stage with rest pain) IV. (stage with trophic defects) 50 m > 50 mm. Hg b rest pain with ankle pressure < 50 mm. Hg a bounded defects b surface defects

Intermittent claudication Metabolic demands of muscle not met during exercise ◦ ◦ Higher demand (muscle work) Flow limitation (pressure gradient) Impaired vasomotion Steal syndrome Pain one level bellow stenosis Tredmill test – determines walking capacity, ABI after exercise (pain + 25% decrease in ABI confirms diagnosis)

Chronic critical limb ischemia Persistent pain at rest requiring analgesics and continuing > 2 weeks Trophic defects or gangrene of the toes or feet Associated ankle systolic pressure < 50 mm. Hg Systolic pressure on the thumb < 30 mm. Hg Tcp. O 2 in the ischemic area < 10 mm. Hg

Acute limb ischemia ← 70 -80% embolic closure (sudden PAD) ← 30 -20% thrombotic occlusion (mostly thrombus on ruptured plaque - acute worsening of existing PAD) Clinical picture- incomplete X complete ischemic sy (6 Ps) Pain Paleness Pulselessness Paresthesias Paralysis Prostration

Treatment of acute limb ischemia i. v. Heparin, i. v. analgesics → urgent revascularization (DSA) Surgical embolectomy- pelvic arteries, arm and forearm arteries Endovascular therapy- LTL, thrombus aspiration, mechanical revascularization Combination of both

Treatment of chronic PAD Cardiovascular mortality prevention ◦ antiplatelet drugs (ASA) ◦ risk factor modification (statins!, antihypertensives…) ◦ Lifestyle changes, exercise Qo. L improvement – control of claudications ◦ Vasocative agents (cilostazol 2 x 100 mg, naftidrofuryl 3 x 200 mg) ◦ Few clinical data supporting effectivity of vasoactive drugs ◦ Prostanoids – critical limb ischemia ◦ Exercise ◦ Revascularization

Treatment of chronic PAD Methods of revascularization ◦ Endovascular (percutaneous, invasive) PTA (DEB; BMS, DES); stentgrafts; SIR; thrombolysis ◦ surgery bypass, endarterectomy, amputation Stimulation of angiogenesis Lumbar sympathectomy (stem cells) ? ?
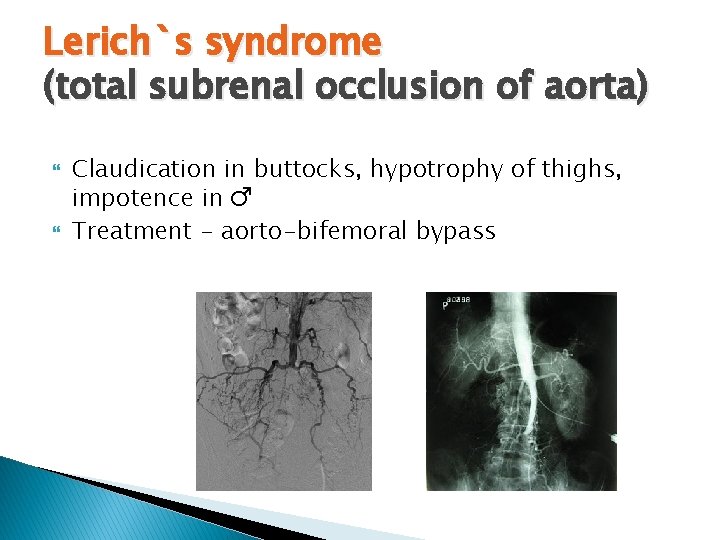
Lerich`s syndrome (total subrenal occlusion of aorta) Claudication in buttocks, hypotrophy of thighs, impotence in ♂ Treatment - aorto-bifemoral bypass

Compressive syndromes compression of arteries, veins, nerves (or all 3 systems) – - anatomical structures (costoclavicular sy) - anatomical anomalies (cervical rib) - different course (medial course of a. poplitea)
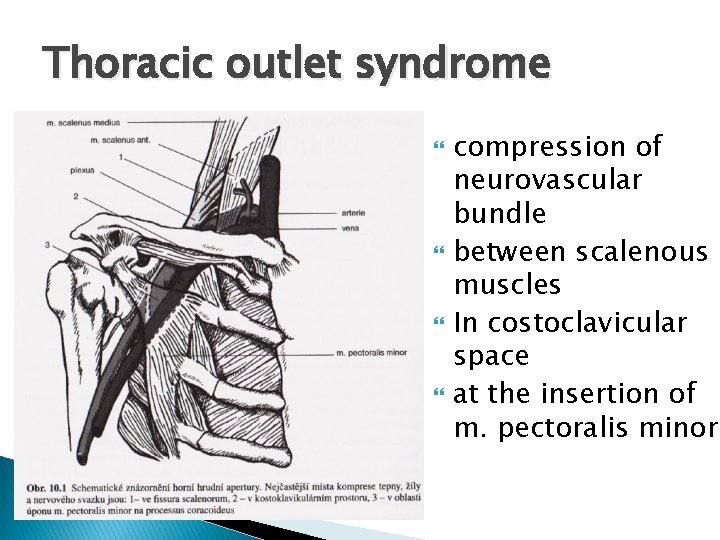
Thoracic outlet syndrome compression of neurovascular bundle between scalenous muscles In costoclavicular space at the insertion of m. pectoralis minor

Thoracic outlet syndrome symptomatology - neurogenic 95% - arterial 3 -5% - venous 2% symptoms- carrying an umbrella, washing windows, painting walls, driving… Therapy - rehabilitation→ improvements up to 70% within a few months - surgical (resection of the first rib) in severe disability
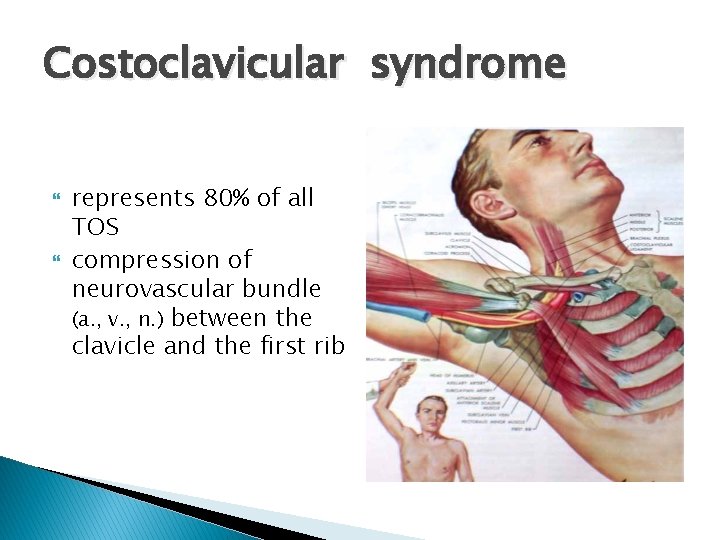
Costoclavicular syndrome represents 80% of all TOS compression of neurovascular bundle (a. , v. , n. ) between the clavicle and the first rib
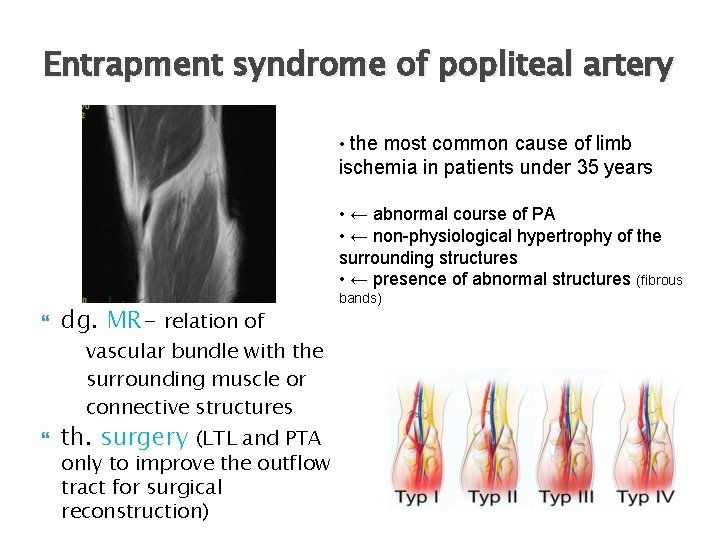
Entrapment syndrome of popliteal artery • the most common cause of limb ischemia in patients under 35 years • ← abnormal course of PA • ← non-physiological hypertrophy of the surrounding structures • ← presence of abnormal structures (fibrous dg. MR- relation of vascular bundle with the surrounding muscle or connective structures th. surgery (LTL and PTA only to improve the outflow tract for surgical reconstruction) bands)

Specific localization of PAD Visceral ischemia Carotid artery disease Renal arteries

Vasospastic disorders • • • Usually reversible localized narrowing of small arteries primary disorders do not lead to trophic changes Raynauds phenomenon • Primary: morbus Raynaud- etiology is not clearly known, suspected failure of regulation at the level of the terminal vascular bed • Secondary: Raynaud´s syndrome – secondary to another underlying disease

Raynaud's phenomenon • • • 1 st phase: ischemia → morbidly pale fingers, paresthesia, 5 -60 min. 2 nd phase: stasis of blood in the capillaries and veins → cyanosis 3 rd phase: reactive hyperemia → reddening

Primary Raynaud's syndrome paroxysmal character, symmetrically, except thumb • women 5 x more often than men • ♀ between puberty and 30 years old, after pregnancy or menopause problems often disappear •

Secondary Raynaud's syndrome Connective tissue disorders ◦ SLE, RA, sclerodermia… PAD ◦ Buergers disease, atherosclerosis, TOS… Drugs Occupational diseases ◦ Vibration – drilling, cold exposure Malignancy Other causes

Take home messages PAD – occlusive diseases of peripheral (limb) arteries 90% atherosclerosis (modfiable risk factors – smoking!, CV mortality) Imaging – DUS, CT (MR), angiography Chronic PAD (claudication, crtitical limb ischemia) vs. Acute limb ischemia Treatment – CV risk modification + revascularization (endovascular, surgical) Many other disorders (vasculitides, compression sy. , vasospastic disorders…)
- Slides: 34